Abstract
The molecular mechanisms underlying the development of bone metastases in breast cancer remain unclear. Disseminated tumour cells (DTCs) in the bone marrow of breast cancer patients are commonly identified, even in early stage disease, but their potential to initiate metastases is not known. The mechanism whereby DTCs become overt metastatic tumour cells (MTCs) is therefore, an area of considerable interest. This study explored the analysable yield of genetic material from human biopsy samples in order to describe differences in gene expression between DTCs and bone MTCs. Thirteen breast cancer patients with bone metastases underwent a CT-guided bone metastasis biopsy and a bone marrow biopsy. Tumour cells were enriched and gene expression profiling was conducted to identify differentially expressed genes. The analysable yield of sufficient RNA for microarray analysis was 60% from bone metastasis biopsies and 80% from bone marrow biopsies. A signature of 133 candidate genes differentially expressed between DTCs and MTCs was identified. Several genes relevant to breast cancer metastasis to bone (osteopontin, CTGF, parathyroid hormone receptor, EGFR) were significantly overexpressed in MTCs as compared to DTCs. Biopsies of bone metastases and bone marrow rarely yield enough tissue for robust molecular biology studies using clinical samples. The findings obtained however are interesting and seem to overlap with the bone metastasis gene expression signature described in murine xenograft models. Larger biopsy specimens or improved RNA extraction techniques may improve analysable yield and feasibility of these techniques.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Bone metastases are the most common site of metastatic recurrence in breast cancer and are a major cause of morbidity for patients [1]. The underlying molecular mechanisms that govern metastases to bone have not been fully elucidated in humans. Recent work has focused upon the role of DTCs in the bone marrow of breast cancer patients and has demonstrated that DTCs can be found in the bone marrow despite a lack of detectable metastatic growth [2]. Indeed, even though the presence of DTCs in the bone marrow has negative prognostic effect with an increased risk of eventually developing overt metastases [3, 4], only about 50% of breast cancer patients with detectable DTCs experienced relapse after a median follow-up of 10 years [5]. It would appear rational to target DTCs in early breast cancer in order to prevent progression of disease and formation of overt bone metastases.
In this regard, compelling data from bisphosphonate therapy trials in women with early breast cancer have also led to increasing interest in DTCs. Adjuvant studies using the oral bisphosphonate clodronate [6, 7] as well as the recently published ABCSG-12 trial, which administered zoledronic acid [8], have all shown significant improvements in disease-free and relapse-free survival. Furthermore, administration of bisphosphonates led to a reduction in the development of both osseous and non-osseous metastases [8]. In contrast, in the metastatic setting, such survival benefit or reduction in distant metastatic disease has not been observed [9–14]. These findings have generated many hypotheses attempting to explain why the apparent anti-tumour activity of bisphosphonates appears to be selective for women with minimal residual disease (i.e. adjuvant patients) rather than those with established overt bone metastases.
In order to further examine the mechanisms underlying the process of metastasis to bone and to explore why women with minimal residual disease are more likely to benefit from the apparent anti-tumour effects of bisphosphonates, many investigators have focused on both CTCs in blood and DTCs in the bone marrow. Data from two immunocytochemical studies demonstrated statistically significant correlations between these cells, although DTCs were more frequently detectable than CTCs [15, 16]. Consequently, DTCs have become the tissue of choice as a surrogate for minimal residual disease in trials of patients with early breast cancer. In this regard, small trials have been initiated to study the effect of bisphosphonates in patients with DTCs. In the only study to have reported results, all patients (n = 14) receiving bisphosphonates were DTC negative after treatment. In contrast, 4 of 14 patients without bisphosphonate treatment showed DTC persistence [17]. While the characterization of DTCs has been extensively studied [18] and data has been obtained showing potential therapeutic effects of bisphosphonates on DTCs, we are not aware of any studies that have tried to compare these cells with those of established metastases in an attempt to explain this association.
This article describes a study, which explored the analysable yield of genetic material from human biopsy samples needed to describe differences in gene expression between DTCs and established bone metastases and assess the feasibility of these techniques. To the authors’ best knowledge, this is the first description of the use of clinical samples in this setting.
Methods
Patients
Patients with known bone metastases from breast cancer were enrolled in this prospective study regardless of therapeutic regimen or burden of disease. Inclusion criteria included histologically confirmed breast cancer, radiological evidence of at least one bone metastasis, and presence of bone metastases in a site that amenable to CT guided biopsy. The institutional research ethics board of University Health Network, Toronto, Canada approved this study.
Study endpoints
The primary objectives of this study were to quantify the analysable yield of RNA for the purposes of gene expression profiling and the feasibility of using such techniques. Secondary objectives were to describe any gene expression differences between DTCs and cells obtained from established bone metastases.
Specimen collection
CT guided biopsy of a radiologically confirmed bone metastasis was carried out under conscious sedation. Specimens were obtained with a 13-gauge needle yielding two samples with a maximal length of 20 mm. Patients then immediately had both a bone marrow aspiration (10 ml) and trephine biopsy (yielding two cores). A trephine biopsy was carried out using an 11-gauge needle. Tissue from both the targeted bone metastasis samples retrieved under CT guidance as well as the bone marrow trephine biopsies and aspirate specimens were analysed fresh.
Cell enrichment
Malignant cells were enumerated from aspirate and trephine samples by combining red blood cell lysis with an EasySep positive selection immunomagnetic separation kit (StemCell Technologies, Vancouver, BC) targeted to EpCAM. Magnetic nanoparticles were combined to bind to the antibody complex, allowing magnetic separation of antibody-bound malignant cells. This procedure was repeated five times to ensure effective and efficient enumeration. Captured cells were then washed and either snap-frozen in liquid nitrogen for later RNA isolation, or processed immediately. This enrichment technique has been previously validated [19, 20].
RNA extraction and microarray hybridization
CT-guided samples were initially homogenized using a PRO200 micro-homogenizer (Pro Scientific Inc., Oxford, CT) and RNA extracted from the homogenate using Qiagen (Germantown, MD) AllPrep DNA/RNA/Protein extraction kits. RNA from aspirate samples was extracted from immunomagnetically isolated tumor cells using the same extraction kits. RNA concentration was determined using a NanoDrop ND-1000 spectrophotometer (Wilmington, DE). RNA samples were snap-frozen in liquid nitrogen and stored at −80°C prior to transport. RNA quality and concentration were assessed by the Agilent 2100 Bioanalyzer RNA 6000 LapChip (Agilent, Palo Alto, CA). RNA samples were amplified and labelled for microarray analysis using a TargetAmp Nano-g biotin-aRNA labeling kit from Epicentre Biotechnologies (Madison, WI). cRNA samples were hybridized onto Illumina Human Ref-8 v3 bead microarrays (San Diego, CA) following standard protocols.
Microarray data analysis
The scanned Illumina array image data were processed using BeadStudio software (Illumina Inc., San Diego, CA) using background subtraction and Quantile normalization. Reference microarray data of the human body index were downloaded from the Gene Expression Omnibus website (http://www.ncbi.nlm.nih.gov/projects/geo). The downloaded CEL data were processed by GeneChip Operating Software (Affymetrix Inc., Santa Clara, CA). The Probe Logarithmic Intensity Error Estimation method was used to produce a summary value for a probe set using the conservative quantile normalization with the perfect match probe feature intensity minus a corresponding mismatch probe (PM−MM). The normalized intensity values from the two platforms were adjusted using previously described techniques [21].
Normalisation
Quantile normalization was utilized [22] and the model fitted by median polish.
The bone and bone marrow aspirate samples were compared to a reference microarray dataset comprising seven breast tissue samples (two normal breasts and five breast cancers) and five normal bone marrow samples. This technique allowed for the calculation of logarithmic ratios of the two separate datasets.
Pathway analysis
Analysed microarray datasets were uploaded into Ingenuity Pathway Analysis software (Redwood City, CA). Illumina probe identifiers were used to map corresponding genes to biological and cellular functions. Microarray results were used to search for biological pathways with increased or decreased expression in our datasets. Pathways containing two or more genes observed in our datasets were noted and investigated. Particular attention was given to pathways known to be involved in cancer and metastasis.
Validation
Once differences in gene expression were identified, attempts were made to verify these with the use of QT-PCR and by immunohistochemistry. Total RNA was extracted using the Trizol reagent (Invitrogen), and 2 μg were converted into cDNA. Primers were designed using the Primer Express software (Applera Europe, Rotkreuz, Switzerland). Real time PCR was performed using an ABI 7000 Sequence Detection System (Applera Europe), and PCR products were quantified fluorometrically using the SYBR Green Core Reagent kit. Three distinct amplifications were performed in duplicate for each transcript, and mean values were normalized to the mean value of the reference mRNA cyclophilin. Immunohistochemical analysis was carried out on formalin fixed and paraffin embedded samples. Low-molecular weight keratin was assessed by using CAM5.2 (Becton–Dickinson), estrogen receptor was assessed by using Clone 6F11 (Novacastra) and progesterone receptor was determined by using Clone 16PG-312 (Novacastra) antibodies.
Statistical analysis
Significant differences in gene expression between the two tissue types were defined as a Bonferroni corrected, two sided t-test P < 0.01. In analysing the Illumina microarray data comparing CT-guided and bone marrow aspirate samples, a log2 expression ratio of an intensity value to the average signal in all samples for each transcript was calculated. Genes with an average log2 ratio difference >4 (Bonferroni corrected P < 0.01) between the two sample types were considered as differentially expressed. Statistical and data analysis was conducted using Acuity software (Molecular Devices, Sunnyvale, CA).
Results
Thirteen patients were enrolled in the study. Patient demographics and disease characteristics are shown in Table 1. The median time from diagnosis of bone metastases to biopsy was 5.5 months (range 0.5–35.5 months). All patients were hormone receptor positive and had received a median of one prior line of endocrine therapy (range 0–2). Two patients (15.4%) were receiving their first line of cytotoxic chemotherapy in the metastatic setting at the time of biopsy while the other patients had never received palliative chemotherapy. Both patients receiving chemotherapy were being treated with paclitaxel given at a dose of 80 mg/m2 q1 week. Four patients (30.8%) had received radiation therapy for bone pain prior to biopsy and of these two (15.4%) received this treatment to the area from which the CT-guided bone biopsy was taken.
Paired biopsies were obtained from ten patients (77%); in one patient (8%) a radiological metastasis was not evident, precluding image-guided biopsy, while in two patients (15%) the bone marrow biopsy was not acquired either due to procedural problems (significant pain, 8%) or due to inadequate biopsy sampling (8%).
Three samples were obtained from each patient: a CT-guided biopsy of a radiologically confirmed bone metastasis, a standard bone marrow aspirate and a trephine biopsy. Sites for CT-guided biopsies included 7 (70%) from the pelvis (posterior iliac crest and wing), 2 (20%) from the spine (L4 and L5 vertebrae, respectively), and 1 (10%) from the shoulder girdle (right inferior glenoid). All bone marrow biopsies were carried out from the superior inferior iliac spines.
On simple microscopy, 3 patients had malignant cells present in all of their specimens. Three patients had malignant cells present in the CT-guided biopsy but not the bone marrow biopsy, while 3 patients had malignant cells in their bone marrow biopsy, but not in their CT-guided biopsy. One patient did not have any malignant cells found in any specimens. The yield of malignant cells from the CT-guided biopsy was variable and CT-guided biopsies often predominantly contained calcified material with only rare cytokeratin positive tumour cells present (see Fig. 1).
Due to the small number of malignant cells derived from the clinical samples, effective and efficient RNA isolation was difficult. RNA isolation from trephine cores yielded insufficient RNA for microarray analysis. Total RNA extracted from CT-guided samples ranged from 20 to 518 ng, while from aspirate samples total RNA ranged from 57 to 1,413 ng. The quantity of available RNA did not seem to be affected by whether patients received prior treatment with bisphosphonates, although the small sample size of this study makes this association difficult to explore accurately.
Due to the requirements of the Illumina platform for at least 50 ng of RNA, samples consisting of <50 ng were excluded from subsequent microarray analysis. Consequently, 6 CT-guided and 8 marrow aspirate samples were selected for amplification and microarray hybridization. Of these, three patients had paired samples of CT-guided and bone marrow aspirate specimens.
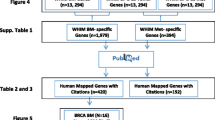
After normalisation, 133 unique genes were identified as significantly differentially expressed between the two sample types. This signature included 83 genes showing increased expression in the metastatic cells as compared to DTCs. Correspondingly, 50 genes were identified as showing decreased expression in the metastatic cells as compared to the DTCs. To further investigate the possible differences in gene expression between the metastatic and disseminated cells, a further analysis was conducted using only samples matched for individual patients (n = 3). Through this method, 161 unique genes were identified as having significant differences in expression. Within this dataset, 104 genes showed increased expression in the metastasis compared to the DTC and 57 genes showed decreased expression. Combining the two datasets revealed 52 unique genes, which were overlapped between the two selected datasets. Of these 52 genes, 30 are showed increased expression in metastatic cells (Table 2) and 22 showed decreased expression (Table 3).
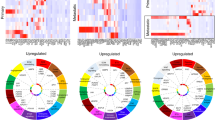
After pathway analysis the differentially expressed genes between DTCs and MTCs were shown to comprise a wide variety of cellular functions, including proliferation, apoptosis, cell cycle and DNA repair. Nine genes were identified as interacting with proteins and pathways involved in the formation of bone metastases from breast cancer (Table 4). All nine of these genes were identified as having increased expression in MTCs as compared to DTCs (Fig. 2).
Attempts at QT-PCR failed as none of the samples contained sufficient RNA for adequate reverse transcription as per platform requirements. Immunohistochemical analyses also proved difficult. Staining using low molecular weight keratin identified tumour cells, but the pattern of staining was variable with some samples appearing much less distinct than usual with mainly membranous staining with associated diffusion into the cytoplasm. Two attempts at staining for TGF-β, OPG and DKK-1 both proved unsuccessful. Of note, a number of samples (n = 4) needed to undergo decalcification, and despite the use of only mildly acidic (pH = 6) decalcification solutions, it is possible that this process had a deleterious effect on antigen preservation.
Discussion
The mechanisms by which minimal residual disease in breast cancer develops into overt metastases are poorly understood. Indeed, it is unclear why only some patients with evidence of isolated DTCs in bone marrow progress to overt metastatic disease. In order to further examine the potential mechanisms underlying these processes, significant research effort is focusing on DTCs in the bone marrow as a surrogate for minimal residual disease. Such methods are touted as allowing for the scientific community to both improve its understanding of the process of metastasis as well as allow for improved targeted drug development.
Central to such research is the ability to validate findings from animal studies with clinical samples. Furthermore, while significant clinical research has focused on the characterisation of DTCs as well as CTCs, ultimately, the most important profile is probably that of the established metastatic deposit. Having already established that there is high patient acceptability to have biopsies of metastases [23, 24], this study set out to explore the feasibility and analysable yield of a program of targeted bone metastasis and bone marrow biopsies in order to study the differences between DTCs and bone metastases. Bone metastases were chosen as the metastatic site in view of this tissue being the most common site of metastatic relapse in breast cancer. In addition, there was an attempt to homogenise tissue types so as to control any unknown confounders associated with tissue sampling and handling that may be associated with the comparison of different tissue types.
Unfortunately, the study did not meet its primary objective of showing adequate feasibility from biopsies of bone and bone marrow. There was a significant deficiency in amount of actual tumour material available for analysis. For instance, despite 13 patients having undergone both guided bone metastasis biopsy and bone marrow aspirate and trephine, only 3 patients (23%) showed evidence of malignant cells in all samples. Even when malignant cells were found, they were often scanty and insufficient for further analysis. Despite the ability to undertake microarray analysis on 60% of guided biopsy samples and 80% of marrow aspirates, none of these had sufficient RNA for the results of this analysis to be validated by QT-PCR. Furthermore, immunohistochemical validation also proved difficult despite attempts to either not decalcify tissue at all, or to decalcify with weakly acidic solutions.
Despite these feasibility issues results did show some interesting findings, which we are not aware of having been previously described using clinical samples and therefore, warrant further study. A number of genes that are differentially expressed between DTCs in the bone marrow and cells from established bone metastases were identified. Within this subset, genes implicated in the formation of osteolytic bone metastases (CTGF, PTHR1, IL11RA) were identified. A number of these genes were previously reported to form a bone metastasis signature in a xenograft model [25]. Of interest, a number of genes involved in angiogenesis (SPP1, AMOT, EPAS1) were also identified as showing differential increased expression in metastases compared to in DTCs. Finally, genes related to growth and proliferation (EGFR, ERBB2, KCNMA1) were also increasingly expressed by metastatic tumour cells. There was very little overlap between highly expressed genes isolated from either DTCs or metastases and those described previously for CTCs [26, 27]. Indeed the only genes identified to overlap between these groups were ERBB2, CCL20 and genes belonging to the IGFBP family. The reasons for this lack of overlap are likely explained by the significant heterogeneity of CTCs both in terms of molecular profile and in terms of clinical outcome [28]. It remains unclear as to whether there is a direct link between CTCs, DTCs and established metastases and therefore it is not surprising that little overlap was found. Finally, there was no significant overlap between genes expressed in either DTCs or metastases and those genes associated with high risk of relapse in ER-positive primary breast tumours [29, 30].
The increasing expression of receptors belonging to the epidermal growth factor (EGF) super-family is an interesting finding especially in view of recent animal data showing that EGF-like ligands stimulate osteoclastogenesis by acting on osteoblastic cells [31]. Despite evidence that this stimulation seemed to be indirect (osteoclasts did not express functional EGF receptors), it did appear to be EGF receptor-dependent. It is therefore possible that tumour cells are the targets of these EGF-like ligands.
It should be emphasised however, that the interpretation of these data should be done with caution especially due to the lack of any validation by either QT-PCR or immunohistochemistry. Furthermore, in the absence of consensus on how to best normalize gene expression data from bone marrow, it could be argued that it may not have been sufficient to simply remove the background expression of bone marrow cells. It may have also been necessary to also remove signals associated with osteoblasts, osteoclasts, osteocytes or other stroma-related cells. Finally, it could be argued that subjecting only the bone marrow aspirate to enrichment using EpCAM-targeted purification could lead to systematic bias and that any difference in gene expression could be affected by the differential sample handling techniques. Nevertheless, the overlap in the data obtained in this study and data derived from xenograft mouse models [25] is encouraging.
Possible explanations for the low analysable yield from both bone and bone marrow biopsies is the quantity of biopsy material obtained as well as the techniques for RNA extraction. In this study, the bone and bone marrow biopsies were undertaken using 13- and 11-gauge needles, respectively each yielding two samples. It is possible that more sufficient quantities of tumour would have been obtained using a larger number of samples or perhaps wider bore needles. In fact, a recent study of long-term bisphosphonate therapy in osteoporosis yielded improved histomorphometric and immunohistochemical data by the use of 7 mm (2-gauge) biopsy needles [32]. It is possible that the use of such biopsy needles in this study would have allowed for improved analysable yield, although whether these techniques are applicable to metastatic biopsies is contentious. Nevertheless, it is clear that greater quantities of tissue are more likely to yield sufficient samples for testing purposes. With regard to RNA extraction, this study utilized the guanidine isothiocyanate technique. Of interest, a recent systematic review concluded that although this technique can yield a higher amount of RNA, the silica-gel column technique may be superior with respect to the reliable generation of an intact RNA and effectively amplified longer products in fresh tissue [33]. Finally, purification of malignant cells from the heterogeneous mix of cells obtained from biopsies may be improved by the use of laser-capture microdissection, with prior immunostaining to aid in malignant cell recognition [34].
In summary, this study has shown that biopsies of bone and bone marrow rarely yield enough tissue for robust molecular biology studies. The findings obtained however are interesting and overlap the bone metastasis gene expression signature described in murine xenograft models. Clearly, improved biopsy techniques yielding greater quantities of tissue as well as improvements in RNA extraction are necessary if such research with clinical samples can be feasible in the future.
Abbreviations
- cDNA:
-
Complimentary deoxyribonucleic acid
- cRNA:
-
Complimentary ribonucleic acid
- CT:
-
Computed tomography
- CTC:
-
Circulating tumour cell
- DNA:
-
Deoxyribonucleic acid
- DTC:
-
Disseminated tumour cell
- EpCAM:
-
Epithelial cell adhesion molecule
- mRNA:
-
Messenger ribonucleic acid
- QT-PCR:
-
Real time quantitative polymerase chain reaction
- RNA:
-
Ribonucleic acid
References
Coleman RE (1997) Skeletal complications of malignancy. Cancer 80:1588–1594
Langer I, Guller U, Koechli OR et al (2007) Association of the presence of bone marrow micrometastases with the sentinel lymph node status in 410 early stage breast cancer patients: results of the swiss multicenter study. Ann Surg Oncol 14:1896–1903
Braun S, Pantel K (2001) Clinical significance of occult metastatic cells in bone marrow of breast cancer patients. Oncologist 6:125–132
Janni W, Hepp F, Rjosk D et al (2001) The fate and prognostic value of occult metastatic cells in the bone marrow of patients with breast carcinoma between primary treatment and recurrence. Cancer 92:46–53
Braun S, Vogl FD, Naume B et al (2005) A pooled analysis of bone marrow micrometastasis in breast cancer. N Engl J Med 353:793–802
Powles T, Paterson A, McCloskey E et al (2006) Reduction in bone relapse and improved survival with oral clodronate for adjuvant treatment of operable breast cancer. Breast Cancer Res 8:1–7
Diel IJ, Jaschke A, Solomayer EF et al (2008) Adjuvant oral clodronate improves the overall survival of primary breast cancer patients with micrometastases to the bone marrow: a long-term follow-up. Ann Oncol 19:2007–2011
Gnant M, Mlineritsch B, Schippinger W et al (2009) Endocrine therapy plus zoledronic acid in premenopausal breast cancer. N Engl J Med 360:679–691
Lipton A, Theriault RL, Hortobagyi GN et al (2000) Pamidronate prevents skeletal complications and is effective palliative treatment in women with breast carcinoma and osteolytic bone metastases: long term follow-up of two randomized, placebo-controlled trials. Cancer 88:1082–1090
Kohno N, Aogi K, Minami H et al (2005) Zoledronic acid significantly reduces skeletal complications compared with placebo in Japanese women with bone metastases from breast cancer: a randomized, placebo-controlled trial. J Clin Oncol 23:3314–3321
Hortobagyi GN, Theriault RL, Lipton A et al (1998) Long-term prevention of skeletal complications of metastatic breast cancer with pamidronate. Protocol 19 Aredia Breast Cancer Study Group. J Clin Oncol 16:2038–2044
Theriault RL, Lipton A, Hortobagyi GN et al (1999) Pamidronate reduces skeletal morbidity in women with advanced breast cancer and lytic bone lesions: a randomized, placebo-controlled trial. Protocol 18 Aredia Breast Cancer Study Group. J Clin Oncol 17:846–854
Conte PF, Latreille J, Mauriac L et al (1996) Delay in progression of bone metastases in breast cancer patients treated with intravenous pamidronate: results from a multinational randomized controlled trial. J Clin Oncol 14:2552–2559
Hultborn R, Gundersen S, Ryden S et al (1999) Efficacy of pamidronate in breast cancer with bone metastases: a randomized, double-blind placebo-controlled multicenter study. Anticancer Res 19:3383–3392
Müller V, Stahmann N, Riethdorf S et al (2005) Circulating tumor cells in breast cancer: correlation to bone marrow micrometastases, heterogeneous response to systemic therapy and low proliferative activity. Clin Cancer Res 11:3678–3685
Pierga JY, Bonneton C, Vincent-Salomon A et al (2004) Clinical significance of immunocytochemical detection of tumor cells using digital microscopy in peripheral blood and bone marrow of breast cancer patients. Clin Cancer Res 10:1392–1400
Rack B, Janni W, Schoberth A et al (2004) Secondary adjuvant therapy with zoledronate in patients with early breast cancer: is there an effect on persisting isolated tumor cells (ITC) in the bone marrow (BM)? Breast Cancer Res Treat 88(Suppl 1):Abstract 6019
Fehm T, Müller V, Alix-Panabières C et al (2008) Micrometastatic spread in breast cancer: detection, molecular characterization and clinical relevance. Breast Cancer Res 10(Suppl 1):S1
Choesmel V, Anract P, Hoifodt H et al (2004) A relevant immunomagnetic assay to detect and characterize epithelial cell adhesion molecule-positive cells in bone marrow from patients with breast carcinoma: Immunomagnetic purification of micrometastases. Cancer 101:693–703
Woelfle U, Breit E, Zafrakas K et al (2005) Bi-specific immunomagnetic enrichment of micrometastatic tumour cell clusters from bone marrow of cancer patients. J Immunol Methods 300:136–145
MAQC Consortium, Shi L, Reid LH et al (2006) The microarray quality control (MAQC) project shows inter- and intraplatform reproducibility of gene expression measurements. Nat Biotechnol 24:1151–1161
Bolstad BM, Irizarry RA, Astrand M et al (2003) A comparison of normalization methods for high density oligonucleotide array data based on variance and bias. Bioinformatics 19:185–193
Amir E, Ooi WS, Simmons C et al (2008) Discordance between receptor status in primary and metastatic breast cancer: an exploratory study of bone and bone marrow biopsies. Clin Oncol (R Coll Radiol) 20:763–768
Simmons C, Miller N, Geddie W et al. (2009) Does confirmatory tumor biopsy alter the management of breast cancer patients with distant metastases? Ann Oncol. doi:10.1093/annonc/mdp028
Kang Y, Siegel PM, Shu W et al (2003) A multigenic program mediating breast cancer metastasis to bone. Cancer Cell 3:537–549
Smirnov DA, Zweitzig DR, Foulk BW et al (2005) Global gene expression profiling of circulating tumor cells. Cancer Res 65:4993–4997
Smirnov DA, Foulk BW, Doyle GV et al (2006) Global gene expression profiling of circulating endothelial cells in patients with metastatic carcinomas. Cancer Res 66:2918–2922
Bertolini F, Mancuso P, Braidotti P, Shaked Y, Kerbel RS (2009) The multiple personality disorder phenotype(s) of circulating endothelial cells in cancer. Biochim Biophys Acta. doi:10.1016/j.bbcan.2009.04.003
van ‘t Veer LJ, Dai H, van de Vijver MJ et al (2002) Gene expression profiling predicts clinical outcome of breast cancer. Nature 415:530–536
Paik S, Shak S, Tang G et al (2004) A multigene assay to predict recurrence of tamoxifen-treated, node-negative breast cancer. N Engl J Med 351:2817–2826
Zhu J, Jia X, Xiao G et al (2007) EGF-like ligands stimulate osteoclastogenesis by regulating expression of osteoclast regulatory factors by osteoblasts: implications for osteolytic bone metastases. J Biol Chem 282:26656–26664
Weinstein RS, Roberson PK, Manolagas SC (2009) Giant osteoclast formation and long-term oral bisphosphonate therapy. N Engl J Med 360:53–62
Muyal JP, Muyal V, Kaistha BP et al (2009) Systematic comparison of RNA extraction techniques from frozen and fresh lung tissues: checkpoint towards gene expression studies. Diagn Pathol 4:9
Fend F, Emmert-Buck MR, Chuaqui R et al (1999) Immuno-LCM: laser capture microdissection of immunostained frozen sections for mRNA analysis. Am J Pathol 154:61–66
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cawthorn, T.R., Amir, E., Broom, R. et al. Mechanisms and pathways of bone metastasis: challenges and pitfalls of performing molecular research on patient samples. Clin Exp Metastasis 26, 935–943 (2009). https://doi.org/10.1007/s10585-009-9284-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10585-009-9284-5