Abstract
Melatonin is involved in blood pressure modulation in rats and humans. Some of the effects of melatonin are presumably mediated via two G-protein-coupled receptors (MT1 and MT2), but the distribution of MT1 and MT2 in the cardiovascular system remains to be explored comprehensively. We investigated the expression of both the receptors in the rat aorta on mRNA level by RT-PCR and real time RT-PCR as well as on protein level via western blotting and immunofluorescence microscopy. We verified MT1 mRNA expression in the rat aorta and demonstrated the absence of MT2 mRNA in this vessel type. MT1 receptors were confirmed also at the protein level, and surprisingly they were preferentially localized to the tunica adventitia. Since no daily changes in MT1 mRNA expression were detected, we suppose that the circadian changes in circulating melatonin concentrations are sufficient to mediate circadian effects of melatonin in the aorta. The localization of MT1 in the tunica adventitia suggests an influence of melatonin on vasa vasorum function and signal transduction in the aorta wall.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Melatonin (MEL) is an indolamine produced by the pineal gland and released in a circadian manner, resulting in high circulating levels during the night, and low levels during the day (Waldhauser and Dietzel 1985). MEL is involved in the regulation of a broad scale of physiological processes (Dubocovich and Markowska 2005; Reiter et al. 2007), including blood pressure (BP) modulation. In rats, pinealectomy results in the development of hypertension (Karppanen et al. 1973; Zanoboni et al. 1978) that in turn can be lowered by MEL treatment (Holmes and Sugden 1976). Likewise, MEL reduced BP in spontaneously hypertensive rats (Pechanova et al. 2007), l-NAME (N(G)-nitro-l-arginine-methyl ester)-treated hypertensive rats (Paulis et al. 2010), and in rats hypertensive as a result of high fructose diet (Leibowitz et al. 2008) or due to stress (Xia et al. 2008).
In humans, a hypotensive effect of MEL was shown in healthy men (Arangino et al. 1999) and women (Cagnacci et al. 1997, 1998), as well as in hypertensive male patients (Scheer et al. 2004), hypertensive women without the nighttime decrease (non-dipping) of BP (Cagnacci et al. 2005), patients with nocturnal hypertension (Grossman et al. 2006), or patients with type 1 diabetes mellitus (Cavallo et al. 2004). In addition, decreased MEL levels are associated with non-dipping pattern of BP in hypertensive patients (Jonas et al. 2003; Zeman et al. 2005). Overall, these data suggest hypotensive effects of MEL and its possible therapeutic use in cardiovascular pathologies (Simko and Paulis 2007; Tengattini et al. 2008; Simko and Pechanova 2009), but mechanisms behind the hypotensive effects of MEL are not completely understood.
Presumably, MEL modulates BP at different sites. In addition to not well-characterized central regulatory mechanisms (Paulis and Simko 2007), MEL can modulate directly vascular tone. However, the data testing the influence of MEL on vascular reactivity appear diverse, vessel-specific, and sometimes conflicting (Pozo et al. 2010).
How MEL acts to influence vascular tone at the cellular level is also not fully understood, but several potential mechanisms have been suggested. These include, on the one hand, non-specific mechanisms reflecting the strong antioxidant capacity of MEL and its metabolites (Tan et al. 2007) that may preserve especially endothelial function and structure (Anwar et al. 2001; Pechanova et al. 2007), resulting in vasodilative and hypotensive effects. On the other hand, in mammals, MEL may influence BP also via two subtypes of G-protein-coupled plasma membrane receptors, MT1 and MT2 (Reppert et al. 1994, 1995; Dubocovich et al. 2010).
To understand receptor-mediated vasomodulatory effects of MEL, the study of expression and distribution of MT1 and MT2 receptors in different vessels is needed, since the exact localization of the receptors and their distribution in the vessel wall remain mostly unknown. Using 125I-MEL binding, specific binding sites were detected in rat cerebral arteries and the smooth muscle layer of caudal arteries, while in the same study, aorta, carotid, coronary, mesenteric, or renal arteries lacked binding sites (Viswanathan et al. 1990). By RT-PCR, the MEL binding sites in the tail artery and the cerebral artery were unequivocally identified as being MT1 (Ting et al. 1999; Chucharoen et al. 2003; Masana et al. 2002). Expression of MT2 mRNA was not demonstrated in cerebral arteries (Chucharoen et al. 2003) and remains contradictory in caudal arteries (Ting et al. 1999; Masana et al. 2002).
In the aorta, expression and function of MT1 was attributed to the observed effects of MEL on rat aortic rings in vitro (Lartaud et al. 2007), but the accumulated data remain contradictory. While the expression of MT1 protein had been shown (Benova et al. 2009), demonstration of mRNA expression failed (Chucharoen et al. 2003), and 125I-MEL binding was not observed (Viswanathan et al. 1990). Finally, while MT2 mRNA expression was shown in human aorta (Ekmekcioglu et al. 2003), a study in the rat aorta failed to detect the same (Chucharoen et al. 2003).
The aim of this study was to evaluate the expression of both MEL receptors and possible daily changes in receptor expression in the rat aorta at the mRNA level by RT-PCR using exon-spanning primers according to Ishii et al. (2009) and real-time RT-PCR. To better understand a possible function of MEL in the modulation of the cardiovascular system activity, the receptor localization in the aorta was investigated by immunofluorescence microscopy.
Materials and Methods
Animals
Mature male Wistar rats were obtained from the Institute of Experimental Pharmacology and Toxicology, Dobra Voda, Slovak Republic. The rats received water and food ad libitum, and were kept under a 12:12-h light:dark cycle (lights on at 10:00 a.m.). The experimental protocol was approved by the Ethical Committee for the Care and Use of Laboratory Animals at the Comenius University Bratislava, Slovak Republic.
Tissue Sampling
For mRNA isolation, aortas of 16 male Wistar rats (age 4 months) were used. Half of the aortas were obtained by dissections 2 h before lights on (darktime group, n = 8) and 2 h before lights off (lighttime group, n = 8). Rats were killed by decapitation after CO2 anesthesia, and aortas were quickly removed, snap frozen in liquid nitrogen, and stored at −80°C. For western blot analysis eight male Wistar rats of the same age were used (darktime group, n = 4; lighttime group, n = 4). For immunofluorescence microscopy, four mature male Wistar rats (age 9 months), were killed during the daytime, and aortas were quickly removed. The thoracic part of each aorta was fixated in HOPE® solution (DCS, Hamburg, Germany) and embedded in paraffin for sectioning. As positive controls for the PCR experiments, rat brain and eye samples were used, since the expression of both MT1 and MT2 mRNA in these organs is well documented in rat (Ishii et al. 2009; Sallinen et al. 2005; Fujieda et al. 1999, 2003).
RNA Isolation and Reverse Transcription
Total RNA was isolated using PeqGOLD® TriFast™ reagent (Peqlab, Erlangen, Germany) according to the manufacturer’s instructions and was subsequently checked for integrity by agarose gel-electrophoresis, and quantified using a NanoDrop™ 1000 (Nanodrop, Wilmington, USA) spectrophotometer. RNA was subjected to reverse transcription using the High Capacity cDNA Reverse Transcription Kit with RNase Inhibitor (Applied Biosystems, Carlsbad, CA, USA), according to the manufacturer’s instructions.
RT-PCR
The RT-PCRs for β-actin, MT1, and MT2 were performed using recombinant Taq-polymerase (Fermentas, St. Leon-Rot, Germany) by the methods and primers as described in Ishii et al. (2009) with the following modifications: RT-PCR for β-actin (resulting in a 496-bp product) was carried out using cDNA corresponding to 50 ng RNA using 22 cycles, while RT-PCR for MT1 (resulting in a 316-bp product) was carried out using cDNA corresponding to 400 ng RNA using 40 cycles. To amplify MT2, a nested PCR was performed. The outer PCR primers were designed from the published mRNA sequence for rat MT2 (Ishii et al. 2009) (NCBI Reference Sequence NM_053676.1): forward primer 5′-TAG CAC TTG CTG GGC GGG GA-3′, reverse primer 5′-AGG CTC GGT GGT AGG TCG CA-3′ (resulting in a 540-bp product). The reaction mixture contained 0.2 mM dNTPs, 0.2 μM forward primer, 0.2 μM reverse primer, 1.5 mM MgCl2, and 1 U Taq-Polymerase per reaction. The following temperature program was used: initial denaturation at 95°C for 3 min, 40 cycles of 95°C for 1 min, 57°C for 1 min, 72°C for 1 min, and then final extension at 72°C for 10 min. The PCR was performed using cDNA corresponding to 400 ng RNA. 1 μl of the reaction product was used as template for the inner PCR which was performed using the methods and primers as described in Ishii et al. (2009), but with 20 cycles and an annealing temperature of 57°C. The inner PCR resulted in a 390-bp product. Negative controls were used in all the reactions, which were treated exactly like the samples, but containing water instead of cDNA. To ensure that the observed amplicons resulted only from reversely transcribed mRNA, samples with non-reversely transcribed RNA were included in the PCR setup as well (-RT samples). The PCR products were analyzed by gel-eletrophoresis using 1.5–2.0% agarose gels containing 0.05% ethidiumbromide. For sequencing, bands were excised from the gel, the PCR products were extracted and purified using the QIAquick® Gel Extraction Kit (Qiagen, Hilden, Germany) according to the manufacturer’s instructions, and sequenced using MWG Eurofins Operon (Ebersberg, Germany).
Real Time RT-PCR
Real time RT-PCR was performed using Taq-Man® gene expression assays for rat MT1 (62618 G10) normalized against β-actin (4352340E−0805007) on a StepOnePlus™ real time PCR system (all Applied Biosystems, USA). cDNA corresponding to 100 ng RNA was used in triplicates in 20 μl reactions. Negative controls containing water instead of cDNA were included as well.
Western Blotting
Samples were homogenized in 0.3 M sucrose, 20 mM Tris (pH 7.0) supplemented with a protease inhibitor cocktail (4-[2-aminoethyl]benzenesulfonyl-fluoride, pepstatin A, E-64, bestatin, leupeptin, aprotinin; Sigma, Saint Louis, MO, USA), and subsequently centrifuged twice for 10 min at 3,500×g and once for 11 min at 12,000×g. Protein concentrations in the supernatants were measured (Lowry et al. 1951). Aliquots containing 40 μg of total protein were denatured in loading buffer (10 mM Tris–HCl, 4% SDS, 20% glycerol, 0.05% coomassie brilliant blue, and 4% 2-mercaptoethanol) at 95°C for 5 min. Proteins were separated by SDS-PAGE using 12% gels and transferred to nitrocellulose membranes (Hybond-ECL, Amersham, UK). To block nonspecific binding, membranes were incubated in Tris-Buffered Saline (TBS) containing 1.2% Tween-20 and 5% nonfat dry milk (blocking buffer) overnight at 4°C. A goat antibody directed against MT1 (MEL-1A-R (R-18); sc-13186; Santa Cruz Biotechnology Inc., Santa Cruz, CA, USA), diluted at 1:500 in blocking buffer was used as a primary antibody, and a horseradish peroxidase-conjugated donkey anti-goat IgG (sc-2033; Santa Cruz Biotechnology Inc., Santa Cruz, CA, USA, dilution 1:1,000 in blocking buffer) was applied as a secondary antibody, each for 1 h at room temperature. Immunoreactive proteins were visualized with the enhanced chemiluminiscence detection system (ECL, Amersham, UK). Expression of glyceraldehyde-3-phosphate dehydrogenase (GAPDH) was used as internal control (primary antibody: anti-GAPDH, 1:1,000, Chemicon, Temecula, CA, USA; secondary antibody: anti-mouse IgG, HRP-linked antibody, 1:1,000, Cell Signaling, Danvers, MA, USA). The results of the western blot analysis were scanned and individual bands were evaluated densitometrically using Quantity One software (Bio-Rad, Hercules, CA, USA) to assess the expression level (arbitrary units) of MT1 protein in relation to GAPDH in individual samples.
Immunofluorescence Microscopy
Paraffin-sections (4 μm) were de-paraffined and rehydrated according to HOPE® manufacturer’s instructions, and antigen retrieval was performed by incubation for 15 min in steaming hot 10 mM citrate buffer, pH 6. Afterward, the sections were incubated in blocking buffer, consisting of 5% goat serum (Jackson Immuno Research, Newmarket, UK) in phosphate buffered saline, pH 7.4 (PBS) containing 0.05% saponin for 1 h. The sections were then stained using rabbit anti-MT1 (Abbiotech, San Diego, CA, USA; 250761), diluted 1:10 in blocking buffer, as primary antibody (overnight) and goat anti-rabbit AlexaFluor 647 (Invitrogen molecular probes, Carlsbad, CA, USA; A21244), diluted at 1:1,000 in blocking buffer, as secondary antibody (1 h). Finally, nuclei were labeled with 4′,6-diamidino-2-phenylindole, dihydrochloride (DAPI; Roche, Penzberg, Germany). The sections were mounted in Mowiol (Sigma–Aldrich, St. Louis, MO, USA). After drying, all the stained sections were photographed with identical exposure times using an automated AxioImager Z1 epifluorescence microscope (Zeiss, Oberkochen, Germany), equipped with TissueFAXS-motorized stage and software (TissueGnostics GmbH, Vienna, Austria) using an EC-Plan Neofluar 20×/0.5 objective (Zeiss).
Results
MT1 mRNA and Protein are Expressed in the Rat Aorta
To verify synthesis of MT1 mRNA in the rat aorta, PCR amplification of cDNA prepared from 16 frozen specimens was performed according to Ishii et al. (2009) with some modifications detailed in the method section. In order to study variations in the daily expression, half of the aortas were collected 2 h before lights on (darktime group, D1–D8), and the other half of the aortas were collected 2 h before lights off (lighttime group, L1–L8). The successful amplification of β-actin (496 bp) proved correct reverse transcription (Fig. 1a, upper panel). Bands of the expected length for MT1 (316 bp) could be detected in all but one (L2, lighttime group) aortic samples using 40 cycles of PCR amplification (Fig. 1a, lower panel). A positive control (eye) was investigated as well, exhibiting a strong band at the expected length (not shown). To confirm their identity, the alleged bands for MT1 were purified and sequenced. Sequence analysis showed 100% identity of the amplicons to nucleotides 169–484 of the published Rattus norvegicus MEL receptor 1a (MTNR1A) mRNA sequence (NCBI Reference Sequence NM_053676.1, data not shown).
RT-PCR analysis of MT1 mRNA expression in rat aortas collected during light (L1–L8) or dark (D1–D8) with a difference of 12 h. a Total RNA isolated from aortas was subjected to RT-PCR using specific primers for β-actin (upper panel, 496 bp) and MT1 (lower panel, 316 bp) cDNAs. Negative controls (Neg, water instead of cDNA) and -RT samples (RNA instead of cDNA) are included. b Real time quantitative RT-PCR analysis was performed using the MT1 and β-actin gene-specific primers as described in Materials and Methods. A positive control (eye) was included. Gene expression of MT1 in each aortic sample was normalized with the respective expression of β-actin mRNA and is shown as ∆CT value. Values are mean ± SEM for three replicates of each aorta. c Mean expression levels of MT1 in the lighttime (n = 8) and darktime (n = 8) groups of aortas
The levels of MT1 varied in intensity to a quite high degree throughout the lighttime and darktime sample range. Overall, the bands in the daytime group appeared slightly less intense than those in the nighttime group, and especially D7 and D8 (both of the darkttime group) exhibited quite strong bands (Fig. 1a, lower panel). To verify any quantitative difference in MT1 mRNA expression levels between aortas from lighttime and darktime groups, a real-time RT-PCR experiment was subsequently performed. A positive control (eye) showed the highest expression of MT1 (CT value 32), while the CT values for MT1 in the aortas were high (35–38), indicating generally low expression of MT1 mRNA in the aortas. The calculation of ∆CT values based on the mean β-actin CT values demonstrated that the amount of MT1 expression varied strongly among the individual samples (Fig. 1b). Analysis of the mean expression levels showed no significant difference in MT1 mRNA expression between the lighttime and the darktime groups (Fig. 1c).
Western blotting of the MT1 in the rat aorta samples (n = 4 for lighttime and 4 for darktime) revealed an immunoreactive protein at approximately 60 kDa (Fig. 2), which correlates to a glycosylated form of the MT1 receptor (Brydon et al. 1999). As seen at the mRNA level, protein expression of MT1 varied among the individual aorta samples. For quantification of protein expression, densitometric analysis of the MT1 protein expression was performed and normalized to the respective GAPDH expression in the individual samples. Mean MT1 protein expression in the lighttime group was not significantly different from MT1 protein expression in the darktime group (Fig. 2).
Western blot analysis of MT1-expression in rat aortas. Homogenates from four samples (40 μg per lane) of the lighttime and four samples of the darktime group from rat aortas were subjected to western blot analysis using the anti-MT1-receptor-antibody (upper panel) or an anti-GAPDH-antibody (lower panel) as described in the Materials and Methods section. The immunoreactive band representing MT1 is located at approximately 60 kDa. A densitometric analysis of the mean expression levels of MT1 normalized to GAPDH expression in the lighttime group versus the darktime is shown
Expression of MT2 mRNA in Rat Aortas
To analyze MT2 mRNA expression in rat aortas, a nested RT-PCR was performed on the rat aorta samples (n = 3 for lighttime and 3 for darktime) as well as rat eye and rat brain, the latter two used as positive controls. Amplification occurred only in the two positive controls, where, the bands were very intense and at the expected length of 390 bp (Fig. 3). Correct amplification of MT2 in the positive controls was confirmed by sequencing. 100% identity of the amplicons to nucleotides 60–450 of the published R. norvegicus MEL receptor 2a (MTNR1B) mRNA sequence (NCBI Reference Sequence: NM_001100641.1) was found (data not shown). No bands were visible in the aorta samples (Fig. 3) leading to the conclusion that MT2 mRNA is not expressed in the rat aorta.
Nested RT-PCR analysis of MT2 mRNA expression in 6 rat aortas collected at light (L, n = 3) or dark (D, n = 3). Total RNA isolated from aortas was subjected to two subsequent RT-PCR reactions using specific outer primers (product length of 540 bp, data not shown) and inner primers (product length of 390 bp) for MT1 cDNAs. Two positive controls (brain and eye) and a negative control (Neg, water instead of cDNA) were included
Localization of MT1 Protein in the Rat Aorta by Immunofluorescence Microscopy
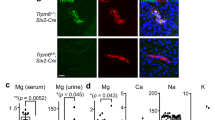
Finally, we investigated the localization of MT1 on paraffin sections of rat aortas by immunofluorescence microscopy. An anti-MT1 primary and an AlexaFluor647-conjugated secondary antibody were used for localization of MT1, nuclei were identified by DAPI staining. Specificity of the antibodies was tested on paraffin sections of brain that is known to express high levels of MT1, and region-specific staining was observed (manuscript in preparation). In the rat aorta, a staining was primarily visible in the tunica adventitia. To a lesser extent, cells of the tunica media and tunica intima were also stained (Fig. 4a). Omission of the primary antibody abolished this staining (Fig. 4b).
MT1 protein localization in the rat aorta. Paraffin-embedded sections from aortic tissue were stained for MT1 using a specific primary and an AlexaFluor647-conjugated secondary antibody (white staining) and analyzed by immunofluorescence microscopy. Nuclei were stained with DAPI (blue staining). a Aorta section stained for MT1. Arrows indicate staining in the TA and TI. b Negative control (secondary antibody only). TA tunica adventitia (connective tissue), TM tunica media (smooth muscle cells and elastic lamellae), TI tunica intima (endothelium)
Discussion
Our study demonstrates the presence of MT1 mRNA in the rat aorta, and the identity of the amplicon was confirmed by sequencing of the PCR products. Expression of MT1 was additionally confirmed at the protein level by Western blotting. These results extend our previous findings in the rat aorta (Benova et al. 2009) and are in line with the MT1 presence in other blood vessels in rats (Dubocovich and Markowska 2005) and the human aorta (Ekmekcioglu et al. 2001). We confirmed the presence of MT1 mRNA by two different RT-PCR techniques applying two different sets of primers and identified the amplicon by sequencing. Methodological differences, especially different numbers of amplification cycles may explain the discrepancy observed between our result and the results of Chucharoen et al. (2003) who were not able to demonstrate MT1 mRNA in the rat aorta.
In contrast to the distinct expression of MT1 receptors in the rat aorta, we failed to demonstrate the presence of MT2 mRNA in this vessel. The absence of the signal was proven by a nested PCR applying exon spanning self-designed outer primers and inner primers used by Ishii et al. (2009). Positive controls using samples of the brain and eyes proved a massive expression of MT2 in both these neural organs, and the specificity of signals was confirmed by sequencing of PCR products. The presence of MT2 was reported in caudal arteries of rats (Masana et al. 2002) and cardiac arteries and aortas of man (Ekmekcioglu et al. 2001) suggesting important tissue and species differences in this type of MEL receptors whose function is still not well understood.
Localization of MT1 receptors in the adventitia of rat aorta is the most important result of this study. Distribution of MEL receptors in the blood vessel wall has been studied only to a limited extent, although it can elucidate a potential role of MEL in the cardiovascular system. In the rat caudal artery activation of the MT1 receptors was reported to cause vasoconstriction and activation of MT2 receptors vasodilatation (Doolen et al. 1998; Masana et al. 2002). In line with these effects, a predominant localization of both receptors in the tunica media has been shown, where they can constrict or relax the caudal artery and contribute to thermoregulation (Viswanathan et al. 1990). Since no investigations on MT1 localization in the aorta and other large conduit blood vessels were performed, we conducted the present study. Surprisingly, the strongest staining for MT1 in aortas was associated with the tunica adventitia, and we detected only a sparse staining for MEL receptors in the endothelium and the tunica media. Similar results have been reported for cerebral vessels from Alzheimer patients where immunohistochemical staining demonstrated MT1 only in the adventitia (Savaskan et al. 2002).
The absence of MT2 in the aorta and the presence of MT1 only in the adventitia in our study suggest that MEL does not contribute directly to relaxation or contraction of the aorta as was demonstrated for the caudal artery. It seems to be oversimplifying to generalize the vasoconstrictive functions of MT1 and vasodilatating effects MT2 to all blood vessels since this conclusion is based on studies using caudal arteries (Doolen et al. 1998; Masana et al. 2002) that have mainly thermoregulatory function. Therefore, an alternative role of MEL and MEL receptors in the adventitia of the aorta, and possible in other large conduit arteries, should be assumed.
The adventitia of the vessel wall received much less attention compared with the endothelium or media, and was considered to have mainly a supportive function. In addition to matrix proteins the adventitia contains (1) the specialized nerve system consisting of afferent and efferent autonomic nerves, and (2) a specialized network of small capillaries (vasa vasorum) that provide nutrients and oxygen to large conduit arteries (Gingras et al. 2009). Recent findings demonstrate that functional changes within the adventitia and especially its vasa vasorum, contribute substantially to vascular function, including the maintenance of elasticity of large arteries. Function of adventitial vasa vasorum is influenced by daily and seasonal rhythms (Nawrot et al. 2005), and it is very well possible that MEL via its MT1 receptors can transfer information about the environmental cycles to vessels. Moreover, vascular physiology exhibits profound circadian rhythms that may be of significant importance for the progression of vascular diseases (Rudic 2009). Mice with the genetic disruption of clock genes bmal1 and clock exhibited pathological vascular remodeling after vessel ligation (Anea et al. 2009). It is not known if MEL can influence rhythmic expression of clock genes in blood vessels as it was shown in the heart (Zeman et al. 2009). We did not find differences in MT1 mRNA expressions between aortas sampled 2 h before lights on and 2 h before lights off. In these time points, the highest receptor expression in the suprachiasmatic nucleus was reported (Poirel et al. 2002). Since only two points from the whole 24-h cycle were analyzed, we cannot completely exclude possible daily changes in MT1 mRNA expression over the day. However, distinct rhythm in plasma MEL concentrations might be sufficient to keep circadian variation without further amplification at the level of its receptor.
Vascular wall inflammation and increased production of ROS play an important role in the initiation and progression of cardiovascular diseases. It has been traditionally expected that vascular wall inflammation originates in the subendothelial space and increases ROS production in the vessel (Lusis 2000). However, recent experimental data support a new paradigm in which the inflammation is initiated in the adventitial layer and progresses through the media toward the intima (Maiellaro and Taylor 2007; Csanyi et al. 2009). This “outside–in” hypothesis is supported by a relatively high adventitial infiltration of leukocytes, increased vasa vasorum neovascularization, and enhanced production of ROS by adventitial fibroblasts. Moreover, activation and migration of adventitial myofibroblasts into the intima participate in vascular remodeling (Siow and Churchman 2007). There is a positive correlation among the magnitudes of adventitial inflammation, the severity of atherosclerosis and the inflammation progresses from the adventitia to intima (Pagano and Gutterman 2007). Adventitial NADPH oxidase appears to have a major contribution to vascular ROS production (Pagano et al. 1995) and ROS can initiate vascular remodeling (Csanyi et al. 2009). Since MEL has been proven as an effective antioxidant that can protect tissue against ROS (Reiter et al. 2007), this indolamine and its MT1 receptors in the adventitia may have the important role of preventing structural and functional modifications of the arterial wall. MEL can both directly scavenge ROS in the free radical scavenging cascade (Tan et al. 2007) and upregulate antioxidant enzyme expression and activity through receptor-mediated processes (Reiter et al. 2007). Such a protective role of MEL can be especially important in the adventitia, since here it may inhibit inflammation, protect elastic fibers, and influence extracellular matrix production. Recently, a significant improvement in mesenteric artery structure and function was observed in rats treated with MEL (Rezzani et al. 2010), and this effect was independent of blood pressure reduction. Similarly, treatment with exogenous MEL resulted in reduced collagen content in the left ventricle (Simko et al. 2009) and can reduce the myocardial remodeling.
In conclusion, MT1 but not MT2 were found in the rat aorta. The allocation of MT1 mainly to the adventitia suggests that MEL in this vessel does not participate directly in its vasoconstriction or vasodilatation. Since the adventitia recently was found to play an important role in the large conduit vessel function, MEL via MT1 receptor-mediated mechanisms could protect against vessels inflammation and subsequent arterial stiffness and modulate signal transduction via sympathetic nerve endings. We did not find daily changes of MT1 receptor expression in the aorta and speculate that circadian changes of circulating MEL concentrations are sufficient to mediate the reported daily and seasonal changes in adventitia function and protection.
References
Anea CB, Zhang M, Stepp DW, Simkins GB, Reed G, Fulton DJ, Rudic RD (2009) Vascular disease in mice with a dysfunctional circadian clock. Circulation 119:1510–1517
Anwar MM, Meki AR, Rahma HH (2001) Inhibitory effects of melatonin on vascular reactivity: possible role of vasoactive mediators. Comp Biochem Physiol C Toxicol Pharmacol 130:357–367
Arangino S, Cagnacci A, Angiolucci M, Vacca AM, Longu G, Volpe A, Melis GB (1999) Effects of melatonin on vascular reactivity, catecholamine levels, and blood pressure in healthy men. Am J Cardiol 83:1417–1419
Benova M, Herichova I, Stebelova K, Paulis L, Krajcirovicova K, Simko F, Zeman M (2009) Effect of L-NAME-induced hypertension on melatonin receptors and melatonin levels in the pineal gland and the peripheral organs of rats. Hypertens Res 32:242–247
Brydon L, Barrett P, Morgan PJ, Strosberg AD, Jockers R (1999) Investigation of the human Mel 1a melatonin receptor using anti-receptor antibodies. Adv Exp Med Biol 460:215–220
Cagnacci A, Arangino S, Angiolucci M, Maschio E, Longu G, Melis GB (1997) Potentially beneficial cardiovascular effects of melatonin administration in women. J Pineal Res 22:16–19
Cagnacci A, Arangino S, Angiolucci M, Maschio E, Melis GB (1998) Influences of melatonin administration on the circulation of women. Am J Physiol 274:R335–R338
Cagnacci A, Cannoletta M, Renzi A, Baldassari F, Arangino S, Volpe A (2005) Prolonged melatonin administration decreases nocturnal blood pressure in women. Am J Hypertens 18:1614–1618
Cavallo A, Daniels SR, Dolan LM, Bean JA, Khoury JC (2004) Blood pressure-lowering effect of melatonin in type 1 diabetes. J Pineal Res 36:262–266
Chucharoen P, Chetsawang B, Srikiatkhachorn A, Govitrapong P (2003) Melatonin receptor expression in rat cerebral artery. Neurosci Lett 341:259–261
Csanyi G, Taylor WR, Pagano PJ (2009) NOX and inflammation in the vascular adventitia. Free Radic Biol Med 47:1254–1266
Doolen S, Krause DN, Dubocovich ML, Duckles SP (1998) Melatonin mediates two distinct responses in vascular smooth muscle. Eur J Pharmacol 345:67–69
Dubocovich ML, Markowska M (2005) Functional MT1 and MT2 melatonin receptors in mammals. Endocrine 27:101–110
Dubocovich ML, Delagrange P, Krause DN, Sugden D, Cardinali DP, Olcese J (2010) International Union of Basic and Clinical Pharmacology. LXXV. Nomenclature, classification, and pharmacology of G protein-coupled melatonin receptors. Pharmacol Rev 62:343–380
Ekmekcioglu C, Haslmayer P, Philipp C, Mehrabi MR, Glogar HD, Grimm M, Thalhammer T, Marktl W (2001) 24 h variation in the expression of the mt1 melatonin receptor subtype in coronary arteries derived from patients with coronary heart disease. Chronobiol Int 18:973–985
Ekmekcioglu C, Thalhammer T, Humpeler S, Mehrabi MR, Glogar HD, Hölzenbein T, Markovic O, Leibetseder VJ, Strauss-Blasche G, Marktl W (2003) The melatonin receptor subtype MT2 is present in the human cardiovascular system. J Pineal Res 35:40–44
Fujieda H, Hamadanizadeh SA, Wankiewicz E, Pang SF, Brown GM (1999) Expression of mt1 melatonin receptor in rat retina: evidence for multiple cell targets for melatonin. Neuroscience 93:793–799
Fujieda H, Scher J, Lukita-Atmadja W, Brown GM (2003) Gene regulation of melatonin and dopamine receptors during eye development. Neuroscience 120:301–307
Gingras M, Farand P, Safar ME, Plante GE (2009) Adventitia: the vital wall of conduit arteries. J Am Soc Hypertens 3:166–183
Grossman E, Laudon M, Yalcin R, Zengil H, Peleg E, Sharabi Y, Kamari Y, Shen-Orr Z, Zisapel N (2006) Melatonin reduces night blood pressure in patients with nocturnal hypertension. Am J Med 119:898–902
Holmes SW, Sugden D (1976) Proceedings: The effect of melatonin on pinealectomy-induced hypertension in the rat. Br J Pharmacol 56:360P–361P
Ishii H, Tanaka N, Kobayashi M, Kato M, Sakuma Y (2009) Gene structures, biochemical characterization and distribution of rat melatonin receptors. J Physiol Sci 59:37–47
Jonas M, Garfinkel D, Zisapel N, Laudon M, Grossman E (2003) Impaired nocturnal melatonin secretion in non-dipper hypertensive patients. Blood Press 12:19–24
Karppanen H, Airaksinen MM, Sarkimaki I (1973) Effects of rats of pinealectomy and oxypertine on spontaneous locomotor activity and blood pressure during various light schedules. Ann Med Exp Biol Fenn 51:93–103
Lartaud I, Faure S, Tabellion A, Resende AC, Nadaud S, Bagrel D, Capdeville-Atkinson C, Atkinson J (2007) Melatonin counteracts the loss of agonist-evoked contraction of aortic rings induced by incubation. Fundam Clin Pharmacol 21:273–279
Leibowitz A, Peleg E, Sharabi Y, Shabtai Z, Shamiss A, Grossman E (2008) The role of melatonin in the pathogenesis of hypertension in rats with metabolic syndrome. Am J Hypertens 21:348–351
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193:265–275
Lusis AJ (2000) Atherosclerosis. Nature 407:233–241
Maiellaro K, Taylor WR (2007) The role of the adventitia in vascular inflammation. Cardiovasc Res 75:640–648
Masana MI, Doolen S, Ersahin C, Al-Ghoul WM, Duckles SP, Dubocovich ML, Krause DN (2002) MT(2) melatonin receptors are present and functional in rat caudal artery. J Pharmacol Exp Ther 302:1295–1302
Nawrot TS, Staessen JA, Fagard RH, Van Bortel LM, Struijker-Boudier HA (2005) Endothelial function and outdoor temperature. Eur J Epidemiol 20:407–410
Pagano PJ, Gutterman DD (2007) The adventitia: the outs and ins of vascular disease. Cardiovasc Res 75:636–639
Pagano PJ, Ito Y, Tornheim K, Gallop PM, Tauber AI, Cohen RA (1995) An NADPH oxidase superoxide-generating system in the rabbit aorta. Am J Physiol 268:H2274–H2280
Paulis L, Simko F (2007) Blood pressure modulation and cardiovascular protection by melatonin: potential mechanisms behind. Physiol Res 56:671–684
Paulis L, Pechanova O, Zicha J, Liskova S, Celec P, Mullerova M, Kollar J, Behuliak M, Kunes J, Adamcova M, Simko F (2010) Melatonin improves the restoration of endothelium-derived constricting factor signalling and inner diameter in the rat femoral artery after cessation of L-NAME treatment. J Hypertens 2010; Suppl 1:S19-24
Pechanova O, Zicha J, Paulis L, Zenebe W, Dobesova Z, Kojsova S, Jendekova L, Sladkova M, Dovinova I, Simko F, Kunes J (2007) The effect of N-acetylcysteine and melatonin in adult spontaneously hypertensive rats with established hypertension. Eur J Pharmacol 561:129–136
Poirel VJ, Masson-Pévet M, Pevét P, Gauer F (2002) MT1 melatonin receptor mRNA expression exhibits a circadian variation in the rat suprachiasmatic nuclei. Brain Res 946:64–71
Pozo MJ, Gomez-Pinilla PJ, Camello-Almaraz C, Martin-Cano FE, Pascua P, Rol MA, Acuña-Castroviejo D, Camello PJ (2010) Melatonin, a potential therapeutic agent for smooth muscle-related pathological conditions and aging. Curr Med Chem 17:4150–4165
Reiter RJ, Tan DX, Manchester LC, Pilar Terron M, Flores LJ, Koppisepi S (2007) Medical implications of melatonin: receptor-mediated and receptor-independent actions. Adv Med Sci 52:11–28
Reppert SM, Weaver DR, Ebisawa T (1994) Cloning and characterization of a mammalian melatonin receptor that mediates reproductive and circadian responses. Neuron 13:1177–1185
Reppert SM, Godson C, Mahle CD, Weaver DR, Slaugenhaupt SA, Gusella JF (1995) Molecular characterization of a second melatonin receptor expressed in human retina and brain: The Mel1b melatonin receptor. Proc Natl Acad Sci USA 12:8734–8738
Rezzani R, Porteri E, De Ciuceis C, Bonomini F, Rodella LF, Paiardi S, Boari GE, Platto C, Pilu A, Avanzi D, Rizzoni D, Agabiti Rosei E (2010) Effects of melatonin and Pycnogenol on small artery structure and function in spontaneously hypertensive rats. Hypertension 55:1373–1380
Rudic RD (2009) Time is of the essence: vascular implications of the circadian clock. Circulation 120:1714–1721
Sallinen P, Saarela S, Ilves M, Vakkuri O, Leppäluoto J (2005) The expression of MT1 and MT2 melatonin receptor mRNA in several rat tissues. Life Sci 76:1123–1134
Savaskan E, Olivieri G, Meier F, Brydon L, Jockers R, Ravid R, Wirz-Justice A, Müller-Spahn F (2002) Increased melatonin 1a-receptor immunoreactivity in the hippocampus of Alzheimer’s disease patients. J Pineal Res 32:59–62
Scheer FA, Van Montfrans GA, van Someren EJ, Mairuhu G, Buijs RM (2004) Daily nighttime melatonin reduces blood pressure in male patients with essential hypertension. Hypertension 43:192–197
Simko F, Paulis L (2007) Melatonin as a potential antihypertensive treatment. J Pineal Res 42:319–322
Simko F, Pechanova O (2009) Potential roles of melatonin and chronotherapy among the new trends in hypertension treatment. J Pineal Res 47:127–133
Simko F, Pechanova O, Pelouch V, Krajcirovicova K, Mullerova M, Bednarova K, Adamcova M, Paulis L (2009) Effect of melatonin, captopril, spironolactone and simvastatin on blood pressure and left ventricular remodelling in spontaneously hypertensive rats. J Hypertens Suppl 27:S5–S10
Siow RC, Churchman AT (2007) Adventitial growth factor signalling and vascular remodelling: potential of perivascular gene transfer from the outside-in. Cardiovasc Res 75:659–668
Tan DX, Manchester LC, Terron MP, Flores LJ, Reiter RJ (2007) One molecule, many derivatives: a never-ending interaction of melatonin with reactive oxygen and nitrogen species? J Pineal Res 42:28–42
Tengattini S, Reiter RJ, Tan DX, Terron MP, Rodella LF, Rezzani R (2008) Cardiovascular diseases: protective effects of melatonin. J Pineal Res 44:16–25
Ting KN, Blaylock NA, Sugden D, Delagrange P, Scalbert E, Wilson VG (1999) Molecular and pharmacological evidence for MT1 melatonin receptor subtype in the tail artery of juvenile Wistar rats. Br J Pharmacol 127:987–995
Viswanathan M, Laitinen JT, Saavedra JM (1990) Expression of melatonin receptors in arteries involved in thermoregulation. Proc Natl Acad Sci USA 87:6200–6203
Waldhauser F, Dietzel M (1985) Daily and annual rhythms in human melatonin secretion: role in puberty control. Ann N Y Acad Sci 453:205–214
Xia CM, Shao CH, Xin L, Wang YR, Ding CN, Wang J, Shen LL, Li L, Cao YX, Zhu DN (2008) Effects of melatonin on blood pressure in stress-induced hypertension in rats. Clin Exp Pharmacol Physiol 35:1258–1264
Zanoboni A, Forni A, Zanoboni-Muciaccia W, Zanussi C (1978) Effect of pinealectomy on arterial blood pressure and food and water intake in the rat. J Endocrinol Invest 1:125–130
Zeman M, Dulková K, Bada V, Herichová I (2005) Plasma melatonin concentrations in hypertensive patients with the dipping and non-dipping blood pressure profile. Life Sci 76:1795–1803
Zeman M, Szantoova K, Stebelova K, Mravec B, Herichova I (2009) Effect of rhythmic melatonin administration on clock gene expression in the suprachiasmatic nucleus and the heart of hypertensive TGR(mRen2)27 rats. J Hypertens Suppl 27:S21–S26
Acknowledgment
The authors gratefully acknowledge the financial support of the FFG/Austria to IE (Bridge 818094) and Slovak APVV-0214-07 and 0150-10 to MZ.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schepelmann, M., Molcan, L., Uhrova, H. et al. The Presence and Localization of Melatonin Receptors in the Rat Aorta. Cell Mol Neurobiol 31, 1257–1265 (2011). https://doi.org/10.1007/s10571-011-9727-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10571-011-9727-9