Summary
1. During the course of studies directed to determine the transport of Angiotensin II AT2 receptors in the rat brain, we found that stab wounds to the brain revealed a binding site recognized by the AT2 receptor ligand CGP42112 but not by Angiotensin II.
2. We localized this novel site to macrophages/microglia associated with physical or chemical injuries of the brain.
3. The non-Angiotensin II site was also highly localized to inflammatory lesions of peripheral arteries.
4. In rodent tissues, high binding expression was limited to the spleen and to circulating monocytes. A high-affinity binding site was also characterized in human monocytes.
5. Lack of affinity for many ligands binding to known macrophage receptors indicated the possibility that the non-Angiotensin II CGP42112 binding corresponds to a novel site.
6. CGP42112 enhanced cell attachment to fibronectin and collagen and metalloproteinase-9 secretion from human monocytes incubated in serum-free medium but did not promote cytokine secretion.
7. When added in the presence of lipopolysaccharide, CGP42112 reduced the lipopolysaccharide-stimulated secretion of the pro-inflammatory cytokines TNF-α, IL-1, IL-1 ß, and IL-6, and increased protein kinase A.
8. Molecular modeling revealed that a CGP42112 derivative was selective for the novel macrophage site and did not recognize the Angiotensin II AT2 receptor.
9. These results demonstrate that CGP42112, previously considered as a selective Angiotensin II AT2 ligand, recognizes an additional non-Angiotensin II site different from AT2 receptors.
10. Our observations indicate that CGP42112 or related molecules could be considered of interest as potential anti-inflammatory compounds.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
As a contribution to the Special Issue of Cellular and Molecular Neurobiology dedicated to the memory of Julius Axelrod, I chose to present a Review and Commentary on a series of experiments conducted several years ago in our laboratory. I selected to present these findings because, originated in a failed experiment yielding unexpected results, led us to postulate a hypothesis of potential basic and therapeutic value, and to a re-evaluation of established notions in our field of research. The recognition of new leads as a consequence of unexpected results, especially when they represented a challenge to established assumptions, was essential to the progress and success of Julie's laboratory. I feel he would have enjoyed the progression of the research described here. This was originated on our studies on the function of Angiotensin II (Ang II) in the brain, which we initiated in Julie's laboratory in the early 1980s. Our interpretation of a “failed” experiment led us to discover a novel binding site, recognizing macrophages and activated microglia, and useful as a quantitative marker of neuronal injury. Further, our results reveal unexpected anti-inflammatory properties of a compound previously considered selective for a different receptor type. With this study, we developed a lead compound of potential clinical interest, and we questioned established assumptions of ligand selectivity in our field. We are convinced that, if successful, future experiments based on the findings presented here will reveal further complexity of Ang II and related receptors. In addition, this project will improve our understanding of the actions of Ang II and related compounds, and perhaps result in advances of basic and therapeutic significance.
THE brain angiotensin ii system and angiotensin ii receptor types
Ang II was first described as a hormone of peripheral origin, the active principle of the Renin-Angiotensin System (RAS) (Braun-Menéndez et al., 1940; Page and Helmer, 1940). Through stimulation of specific receptors, Ang II acts as a pro-hypertensive, vasoconstrictor, sodium and water conserving peptide (Page, 1987). Local synthesis of Ang II occurs in many tissues including the brain, where the peptide plays multiple additional important roles (Saavedra et al., 2005), including a role as a pro-inflammatory factor (Saavedra, 1992; Ando et al., 2004; Saavedra, 2005; Zhou et al., 2005).
The development of selective non-peptidic and peptidic ligands allowed the demonstration of two distinct receptor types, the AT1 and AT2 receptors. Both receptor types belonged to the superfamily of seven membrane-spanning G-protein coupled receptors. Although they both bound Ang II with similar high affinity, they only shared 32–34% identity at the amino acid level (de Gasparo et al., 2000). The receptor types were pharmacologically characterized with the use of the AT1 receptor non-peptidic antagonist losartan and derivatives or the AT2 receptor agonist and peptide derivative CGP42112 and the AT2 non-peptidic receptor antagonist PD123199 (de Gasparo et al., 2000). It was first considered that stimulation of AT1 receptors was necessary and sufficient to produce all significant effects of Ang II, while the role of AT2 receptors remained undetermined (de Gasparo et al., 2000).
With quantitative autoradiography with a selective agonist for Ang II receptors, [125I]Sarcosine1-Ang II, ([125I]Sar1-Ang II) we localized Ang II receptors throughout the brain. Specific quantification of AT1 and AT2 receptors was obtained by displacing [125I]Sar1-Ang II binding with ligands considered selective for AT1 or AT2 sites, unlabelled losartan to determine binding to AT1 receptors or unlabelled PD123199 or CGP42112 to determine binding to AT2 receptors (Tsutsumi and Saavedra, 1991a).
We found that AT1 receptors were expressed in many brain areas involved in the regulation of hormone and sympathetic function, in agreement with well-characterized effects of brain Ang II and of circulating Ang II acting centrally (Tsutsumi and Saavedra, 1991a, b, c). Surprisingly, AT2 receptors were present in brain areas involved in sensory and motor functions, and their expression was much higher in the immature rodent brain than in adult animals (Tsutsumi and Saavedra, 1991a, b, c). This suggested that in the brain AT2 receptors could have specific functions, related to the integration of sensory and motor activity and to brain development (Tsutsumi and Saavedra, 1991a)
The discovery of the novel non-angiotensin ii binding site
One of areas of high AT2 receptor expression in the immature rat brain was the inferior olivary complex, which sends ascending climbing fibers to innervate Purkinje cells in the cerebellar cortex (Tsutsumi and Saavedra, 1991a). Because the inferior olive expressed AT2 receptor binding and mRNA, and the cerebellar cortex only AT2 receptor binding and not receptor mRNA (Jöhren et al., 1995a; Jöhren and Saavedra, 1996), we speculated that the AT2 receptors transcribed in inferior olivary neurons could be transported through the ascending climbing fibers. This hypothesis was supported by our finding that chemical lesions of the inferior olive decreased AT2 receptor binding in the cerebellar cortex (Jöhren et al., 1998).
To further test such hypothesis, we attempted to cut the ascending fiber tract in immature rats with the use of a knife, hoping to eliminate AT2 binding in the cerebellar cortex with such a procedure. For these experiments, focused on the role of AT2 receptors, we decided to use [125I]CGP42112 instead of [125I]Sar1-Ang II, to selectively label AT2 receptors, since we believed this compound to be a specific high affinity AT2 receptor ligand (Heemskerk et al., 1993; Heemskerk and Saavedra, 1995). The method consisted in attempting to cut the ascending fiber tract with a Halász knife, followed by a waiting period of one week to allow fiber degeneration, sacrificing the animal and incubating one brain section in the presence of [125I]CGP42112, and a consecutive section with addition of excess unlabelled Ang II, to displace the binding to AT2 receptors (Heemskerk et al., 1993).
In a preliminary experiment, the knife cut was located towards the mid portion of the brain stem, away from the lateral position of the ascending tract, and no changes in AT2 receptor binding were found in the cerebellar cortex. Careful analysis of this failed experiment directed us in a totally different direction. To our surprise, in addition to the inferior olivary and cerebellar AT2 receptors, we detected intense binding at the lesion site (Fig. 1). Even more surprising was the discovery that excess unlabelled Ang II was not able to displace [125I] CGP42112 binding (Fig. 1). We immediately realized that [125I] CGP42112 recognized a non-Ang II site, selectively localized to the brain lesion.
Autoradiogram of [125I]CGP42112 binding to a brainstem lesion. Figure on the left is an autoradiogram of a brainstem section from a rat sacrificed 7 days after a knife lesion to the brainstem, and incubated in the presence of [125I]CGP42112, as described earlier (Heemskerk and Saavedra, 1995). Note that binding is localized to the inferior olivary complex and to the brain lesion. Figure on the right is a consecutive section incubated as above in the presence of unlabelled Ang II. Note that [125I]CGP42112 binding to the inferior olivary complex, representing Ang II AT2 receptors, has been displaced by unlabelled Ang II, and that [125I]CGP42112 binding to the lesion has not been displaced by Ang II, indicating the presence of a non-Ang II binding site.
Characterization of the non-angiotensin ii [125I]CGP42112 binding site
Our findings prompted us to characterize this novel site. To this purpose, we incubated tissue sections with [125I] CGP42112, and consecutive sections, one with addition of unlabelled Ang II, and another with addition of unlabelled CGP42112. The [125I] CGP42112 binding displaced by Ang II corresponded to Ang II AT2 receptors; binding not displaced by Ang II but displaced by unlabelled CGP42112 corresponded to non-Ang II, CGP42112 binding.
We were not able to detect significant levels of non-Ang II [125I] CGP42112 binding anywhere in the normal, non-lesioned brain or in any other organ of untreated rats, except the spleen, where non-Ang II CGP42112 binding was extraordinarily high in the red pulp (Fig. 2), and in the thymus and lung, where non-Ang II CGP42112 binding was very low (de Oliveira et al., 1994). It was of interest that, in addition to the non-Ang II CGP42112 binding, the rat spleen expressed very significant numbers of Ang II AT1 receptors but no AT2 receptors (Tsutsumi et al., 1992) (Fig. 3).
Emulsion autoradiography of [125I]CGP42112 binding in rat spleen. (A) section stained with Hematoxylin-eosin, RP: red pulp, WP: white pulp. (B) dark-field illuminated micrograph with localization of silver grains in the red pulp. Magnification is X 1190. (From de Oliveira et al., 1994, with permission).
Angiotensin II and non-Angiotensin II binding in the rat spleen. Figures represent autoradiograms of consecutive spleen sections incubated in the presence of [125I]CGP42112 (left) or [125I]Sar1-Ang II (right). The upper figure is a consecutive spleen section stained with hematoxylin-eosin. Arrows indicate the red pulp. Note that [125I]CGP42112 binding is displaced by unlabelled CGP42112 only, and not by Ang II, the AT1 receptor antagonist losartan or the AT2 receptor antagonist PD123177, indicating the presence of non-Ang II binding sites. Note that [125I]Sar1-Ang II binding is displaced only by losartan and unlabelled Ang II, and not by unlabelled CGP42112 or PD123177, indicating the presence of Ang II AT1 receptors and not AT2 receptors. (From de Oliveira et al., 1994, with permission).
Our analysis of CGP42112 binding in rat spleen revealed a single binding site with high affinity for [125I] CGP42112, which could not be displaced by unlabelled Ang II or any of the Ang II fragments tested, by Ang II AT1 antagonists or by the Ang II AT2 selective ligand PD123177 (de Oliveira et al., 1994).
Our autoradiographic studies did not allow us to determine the cellular localization of the [125I]CGP42112 binding. Because of the high number of macrophages present in the red pulp of the spleen, we speculated that the novel binding site was located in macrophages. We isolated a macrophage-enriched cellular fraction from the spleen and identified significant non-Ang II CGP42112 binding in this fraction (de Oliveira et al., 1994). We then speculated that [125I]CGP42112 binding could be a specific marker for macrophages, and that CGP42112 or related peptides could contribute to the regulation of macrophage function.
Macrophages express many surface receptors controlling multiple functions including growth, differentiation, activation, recognition and migration. In the spleen, CGP42112 binding could not be displaced by cytokines, growth factors and macrophage activating peptides, indicating the possibility that CGP42112 could bind to a novel macrophage site (de Oliveira et al., 1994).
CHARACTERIZATION OF NON-ANGIOTENSIN II [125I]CGP42112 BINDING AS A MARKER OF NEURONAL INJURY
Because the brain CGP42112 site was highly expressed only after a lesion, and was normally expressed in the spleen, an organ rich in macrophages and in spleen-derived macrophages (de Oliveira et al., 1994) we hypothesized that perhaps this site was expressed after brain lesions as a result of macrophage migration from the circulation and/or in lesion-activated microglia.
We conducted a series of experiments to determine to what extent the novel binding site was expressed in brain lesions. First, we further characterized the novel binding site in healing wounds of the rat brain. Following a stab wound to the cortex, non-Ang II CGP42112 binding was highest 3 days after the lesion, and was localized to macrophages or reactive microglia surrounding the wound (Viswanathan et al., 1994a) (Fig. 4). The time course of binding expression, decreasing to very low levels 10 days after the lesion, was in close agreement the transient appearance of macrophages at the wound site after penetrating injuries of the brain (Giulian et al., 1989). As it was the case in the normal spleen, binding could not be displaced by cytokines, growth factors or macrophage activating peptides, again suggesting the presence of a novel site (Viswanathan et al., 1994a).
Localization of non-Ang II [125I]CGP42112 binding and detection of GFAP and ED-1 immunohistochemistry in rat brain 5 days after injury. (A) Toluidine blue staining of a coronal section of the brain. (B) Consecutive section incubated with [125I]CGP42112 to reveal binding surrounding the knife wound. (C) Consecutive section incubated as above in the presence of unlabelled CGP42112. (D) Consecutive section showing immunocytochemical staining for GFAP, which does not colocalize with binding. (E) Consecutive section showing immunocytochemical staining for ED-1. (F) Negative control; normal goat serum was used instead of primary antisera. Arrowheads (A–F) point to the edges of the lesion. Arrows (A–F) point to the lateral ventricle. Bars (A–F) are 1 mm. G-I: Higher magnification (bar: 2 (.m) of the area surrounding the tip of the lesion. (G) Hematoxylin-eosin staining. (H) Dark-field illumination. (I) Immunocytochemical staining for ED-1. Note that the localization of [125I]CGP42112 binding is associated with positive staining for ED-1 of macrophages/microglia. (From Viswanathan et al., 1994a, with permission).
Autoradiograph of [125I]CGP42112 binding after a MPP+-induced lesion. (A) staining with toluidine blue. (B–F) consecutive sections incubated with [125I]CGP 42112, B: total binding, (C) non-specific binding after incubation in the presence of unlabelled CGP42112, (D) incubated in the presence of unlabelled Ang II, (E) incubated in the presence of losartan, (F) incubated in the presence of PD123177. Note that binding of [125I]CGP42112 to AT2 receptors in the medial geniculate nuclei (MG) and the superior colliculus (SC) marked by arrows, is displaced by Ang II and by PD123177, and that non-Ang II lesion binding, marked by arrowheads, is only displaced by unlabelled CGP42112. Bar is 2 mm. (From Viswanathan et al., 1994, with permission).
Further evidence of an association of non-Ang II CGP 42112 sites with brain injury was found in 1-methyl-4-phenylpyridine (MPP+)-induced lesions of the substantia nigra, which in high doses results not only in cytotoxic damage to dopaminergic neurons in this structure but also in nonspecific damage and necrosis not restricted to this system (Viswanathan et al., 1994b). After a high dose of MPP+, high non-Ang II [125I]CGP42112 binding was localized to the periphery of the lesion, an area with high concentrations of activated microglia and macrophages derived from the peripheral circulation (Fig. 5).
Binding to non-Ang II CGP42112 sites was also expressed in the brain after administration of kainic acid in the lateral ventricle. Binding was expressed early (4 days after administration) in the hippocampus, the primary target for kainic acid neurotoxicity, and later (14 days after the lesion) in the thalamus, amygdala, and piriform cortex, containing terminal fields from the originally damaged hippocampal neurons, as a result of delayed neuronal injury and death. Again, appearance of binding coincided temporally and spatially with the expression of activated microglia and macrophages at the lesion sites as well as with neuronal death at a distance from the lesion, as a consequence of neuronal degeneration (Jöhren et al., 1995b) (Figs. 6 and 7).
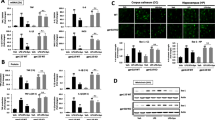
Binding of [125I]CGP 42112 and immunostaining for macrophages/activated microglia in rat hippocampus after kainic acid administration in the lateral ventricle. A1–D1: Staining with cresyl violet. A2–D2: binding of [125I]CGP 42112 in the presence of unlabelled Ang II to reveal non-Ang II binding sites. A3–D3: immunostaining for OX-42 antibody. A4–D4: immunostaining for ED-1 antibody. Figures are 1 day (A1–A4), 4 days (B1–B4) and 14 days (C1–C4) after kainic acid administration. D1–D4: animals received saline instead of kainic acid. Filled arrows point to hippocampal area CA3. Open arrows point to hippocampal area CA1. Scale bar: 0.5 mm. Note the spatial and temporal correspondence of neuronal damage, [125I]CGP 42112 binding and immunostaining of macrophages/microglia. (From Jöhren et al., 1995b, with permission).
Time progression of binding of [125I]CGP 42112 in hippocampus and projection areas after kainic acid administration in the lateral ventricle. A,C,E: 4 days after kainic acid administration. B,D,F: 14 days after kainic acid administration. A,B: non-Ang II CGP 42112 binding. C,D: immunostaining for OX-42. E,F: immunostaining for ED-1. CA3: hippocampal area 3. LD: laterodorsal, MD: mediodorsal and VM: ventromedial thalamus. Amg: amygdala. Pir: piriform cortex. Scale bar: 2 mm. Note the spatial and temporal correspondence of [125I]CGP 42112 binding and immunostaining for macrophages/microglia. Fourteen days after the lesion both [125I]CGP 42112 binding and immunostaining are expressed in brain areas receiving projections from the hippocampus. (From Jöhren et al., 1995a, b, with permission).
These results demonstrated that non-Ang II CGP42112 sites are sensitive markers of different types of neuronal injuries, that these sites localize to activated microglia and macrophages derived from the peripheral circulation, and that the binding expression correlates well with the degree of injury, making the [125I]CGP42112 binding a good marker for the quantitative study of neuronal injury. Our results have been recently confirmed with studies associating the non-Ang II CGP42112 binding with neuronal injury and macrophage infiltration following nodose ganglionectomy in the rat (Roulston et al., 2003, 2004, 2005).
Association of non-angiotensin II [125I]CGP42112 binding with peripheral vascular inflammation
Our observations were not limited to the study of brain lesions. During our studies on the expression and role of Ang II receptor types in peripheral arteries, we focused on the role of AT1 and AT2 receptors after balloon injury of the carotid endothelium. Our objective was to determine if a lesion of the arterial endothelium produced enhanced expression of AT1 receptors, associated to the endothelial lesion and the development of arteriosclerotic plaques, and of AT2 receptors related to the healing process after the injury, effects which could counterbalance those of the AT1 receptor type. Balloon angioplasty indeed enhanced the expression of AT1 receptors in the neointima, the pathological intima growth which follows the endothelial denudation, supporting the hypothesis of a role of this receptor type in endothelial injury (Viswanathan et al., 1992). However, we could not detect AT2 receptor expression in the neointima after the carotid lesion, and this appeared to negate the hypothesis of a protective role of the AT2 receptor type (Viswanathan et al., 1992).
On the light of our findings related to the association of non-Ang II [125I]CGP42112 binding with brain injury and inflammation, we decided to reinvestigate our model of balloon angioplasty, an operation which results, in addition to the endothelial lesion, in a marked inflammatory reaction in the adventitia surrounding the lesion. Our hypothesis was that the novel macrophage receptor would associate with inflammatory lesions not only in the brain but also in the periphery. Indeed, we found high expression of non-Ang II CGP42112 binding in the carotid artery adventitia after balloon catheterization, associated with macrophages in the inflamed tissue surrounding the injured artery (Fig. 8) (Viswanathan et al., 1996).
Expression and characterization of the non-angiotensin II [125I]CGP42112 binding site in human monocytes
While studies in animal populations could generate interest, a robust hypothesis for clinical implications cannot only be based on findings in animal models. Such an hypothesis needs corroboration from preclinical studies in humans. The association of [125I]CGP42112 binding with macrophages and/or activated microglia in lesions of the brain and carotid artery and the high expression of binding in the macrophage-rich spleen and in spleen-derived macrophages prompted us to study the possible presence of non-Ang II CGP42112 binding in human macrophages. We detected membrane-associated, single site, high affinity, specific non-Ang II CGP42112 binding in human peripheral mononuclear cells and, using autoradiography, in human monocyte pellets (Fig. 9) (Egidy et al., 1997). As it was the case with the non-Ang II CGP42112 site in the rat spleen, binding could not be displaced by a number of Ang II fragments, cytokines and growth factors, suggesting the expression of a novel site (Egidy et al., 1997).
Characterization of non-Angiotensin II [125I]CGP42112 binding to human monocytes. (A) displacement of [125I]CGP42112 binding from human monocyte membranes. Data represent percent of [125I]CGP42112 binding inhibited by unlabeled CGP42112 (•) Z-Arg(Pmc)OH (▴) or Ang II (○). Note that binding was displaced by CGP42112 or, with lower affinity, by Z-Arg(Pmc)OH, but not by Ang II. B: displacement of [125I]CGP42112 binding by unlabeled CGP42112 from human monocyte pellet sections. (From Egidy et al., 1997, with permission).
Anti-inflammatory effects of cgp42112 in cultured human monocytes
To establish whether or not such binding could have any physiological significance, we studied the effects of CGP42112 on cultured human monocytes. The results obtained can be summarized as follows. Addition of CGP42112 to human monocytes increased their adhesion to fibronectin and collagen. While CGP42112 alone did not influence cytokine secretion from monocytes, it produced a dose-dependent inhibition of lipopolysaccharide-induced secretion of proinflammatory cytokines such as tumor necrosis factor-α (TNF-α, interleukin-1α (IL-1α, interleukin-1β (IL-1β, and interleukin-6 (IL-6), (Table I) without effect on the anti-inflammatory cytokine interleukin-10 (IL-10). Likewise, CGP42112 produced a significant inhibition of the lipopolysaccharide-induced production of matrix metalloproteinase-9 (MMP-9), probably through a prostaglandin PGE2 pathway (Egidy et al., 1997). The observation that CGP42112 could partially block the stimulating effect of lipopolysaccharide on human monocytes suggested that the non-Ang II [125I]CGP42112 binding site could be considered a receptor, and that CGP42112 could possess important anti-inflammatory properties.
Molecular analysis of the non-angiotensin ii cgp42112 site and discovery of a selective ligand for this binding site
The discovery of the anti-inflammatory properties of CGP42112 renewed our interest in the molecular analysis of the novel site. Since CGP42112 could bind to either AT2 receptors or to the non-Ang II macrophage receptor with high affinity, we attempted to determine the structural requirements of the novel CGP42112 binding site, and compared these with the requirements for binding to the Ang II AT2 receptor. We designed and studied a series of CGP42112 analogs using binding assays to membranes from rat spleen, expressing non-Ang II CGP42112 macrophage receptors but no AT2 receptors, or membranes from rat fetus, expressing AT2 receptors but not non-Ang II CGP42112 macrophage receptors (Ciuffo and Saavedra, 1995).
CGP42112 is a peptide derivative containing a CBZ group [Nic-Tyr-(ε-CBZ (benzyloxycarbonyl)-Arg)Lys-His-Pro-Ile]. The compound is derived from the Ang II C-terminal pentapeptide (Whitebread et al., 1989), with the positively charged, aminopeptidase-sensitive amino terminal replaced by Nic and the Ile5 of Ang II replaced by a Lys linked through its ε amino group to Arg-CBZ. A CGP42112 analog lacking the CBZ group (Nic-Tyr-(Ac-Arg)Lys-His-Pro-OH) and the peptide Nic-Tyr-Lys-His-Ala-His-OH displaced binding to the AT2 receptor selectively, and poorly recognized the non-Ang II macrophage receptor (Ciuffo and Saavedra, 1995). Our studies suggested that the presence and spatial orientation of free carboxyl terminal and CBZ groups were essential determinants for the recognition of the CGP42112 site (Ciuffo and Saavedra, 1995). In agreement with this hypothesis, we found that a non-peptidic CGP42112 analog, Z-Arg(Pmc)OH (NαCBZ-NG-2,2,5,7,8-pentamethylchroman-6sulphonyl-L-Arg), the side chain of CGP42112 substituted on the guanidinium group, selectively recognized the non-Ang II CGP42112 macrophage receptor but not the AT2 receptor. We could prove the specificity of Z-Arg(Pmc)OH for the CGP42112 macrophage receptor when we showed that Z-Arg(Pmc)OH displaced [125I]CGP42112 binding from human monocytes membranes (Fig. 9) (Egidy et al., 1997) and from spleen membranes, expressing the non-Ang II binding sites, but not from fetal rat membranes expressing only AT2 receptors but not the non-Ang II CGP42112 binding site (Fig. 10) (Ciuffo and Saavedra, 1995). We then proposed Z-Arg(Pmc)OH as a lead compound for development of CGP42112 site-selective analogs (Ciuffo and Saavedra, 1995).
Characterization of CGP42112, Z-Arg(Pmc)OH and Angiotensin II displacement of [125I]CGP42112 binding from rat spleen and fetal membranes. Note that both CGP42112 (•–•)and Z-Arg(Pmc)OH (*–*)displace [125I]CGP42112 binding from spleen membranes, expressing the non-Ang II CGP42112 binding sites. Conversely, Z-Arg(Pmc)OH is unable to displace [125I]CGP42112 binding from fetal membranes expressing only AT2 receptors. This indicates that Z-Arg(Pmc)OH is selective for the non-Ang binding site.
Summary and conclusions
Initial (and apparently unsuccessful) studies on the regulation of brain Ang II receptor types lead us to detect the presence of a novel non-Ang II binding site recognized by a peptide derivative of Ang II which until then had been considered a selective Ang II AT2 receptor. The novel site, which for lack of a better name was called “non-Ang II CGP42112 binding site,” undetectable in the normal brain, had a temporal and spatial association with activated microglia and blood derived macrophages following different kinds of direct neuronal injury and neurodegenerative cell death.
Associated with macrophages not only in inflammatory lesions of the brain but also with those of peripheral arteries, and present in circulating human monocytes, the binding was not influenced by many ligands selective for known macrophage receptors, suggesting the possibility of a novel site. Occupation of the site by CGP42112 in human macrophages significantly reduced cytokine stimulation by bacterial lipopolysaccharide, a strong indication of important anti-inflammatory effects. Molecular modeling revealed that compounds could be developed with selective affinity for the non-Ang II macrophage receptor.
Our results demonstrate again that pharmacological selectivity is relative, and that compounds once thought specific for particular receptors may later be found to activate or inhibit additional sites. In the case of Ang II, our results demonstrate further complexity of the Ang II receptors and associated types. These considerations are not exclusively related to the Ang II AT2 receptor type. For example, high levels of non-Ang II binding sites have been reported in the kidney for the “selective” AT1 receptor antagonist losartan (Chancel et al., 1994). That little attention has been paid to such a finding does not diminish its possible implications. For this reason it is useful to consider the possibility of yet to be characterized additional binding sites for “Ang II receptor type” ligands, CGP42112 and losartan (Fig. 11). A better understanding of the physiological interactions between these sites and their degree of homology requires further characterization, purification and cloning of the proposed novel sites. Purification and cloning of the macrophage non-Ang II CGP42112 site could reveal a novel receptor, or simply demonstrate that CGP42112 binds to one of the many receptors selectively expressed in macrophages. The finding of a novel receptor in macrophages will certainly generate the most interest. However, in either case, the discovery that the CGP42112 class of molecules possesses unexpected anti-inflammatory properties indicates the possibility of the development of novel anti-inflammatory therapies, potentially of great clinical interest.
Angiotensin II receptor types, related sites, and their ligands. Note that Angiotensin II binds to two fully characterized receptor types, the AT1 and AT2 receptors. In rodents, AT1 receptors are subdivided into AT1A and AT1B types. Losartan, a proposed selective ligand for AT1 receptors, also binds to a site not fully characterized but not recognized by Angiotensin II, the “losartan binding site.” CGP42112, a proposed selective ligand for AT2 receptors, also binds to the CGP42112 macrophage site described here and not yet fully characterized. Neither losartan nor CGP42112 can be considered “selective” ligands for AT1 or AT2 receptors, respectively.
In the meantime, several important points can be made. CGP42112 is not selective for Ang II AT2 receptors, binds to novel sites in macrophages unrecognized by Ang II, and apparently possesses important anti-inflammatory properties. [125I]CGP42112 binding recognizes microglial activation, macrophage infiltration, neuronal and non-neuronal injury, and binding quantification can be used as a powerful method to evaluate the efficacy of protective, anti-inflammatory compounds. A novel class of anti-inflammatory compounds could be developed following the leads mentioned above. The last point may be of fundamental clinical importance. Inhibition of the macrophage initial response to the bacterial lipopolysaccharide implicates a regulation of the innate immune response, essential as a first step in the response of the organism against infection. Ischemic, chemical and infectious insults to the brain provoke microglial and macrophage activation and recruitment at the sites of injury to regulate neuronal survival, astroglial proliferation and angiogenesis. Microglia plays fundamental roles in neurodegenerative diseases like multiple sclerosis and Alzheimer's disease and is the major brain cell type to be infected with HIV. For these reasons it appears of importance to study and develop novel ligands, such as CGP42112 analogs, that selectively recognize macrophages and activated microglia.
References
Ando, H., Zhou, J., Macova, M., Imboden, H., and Saavedra, J. M. (2004). Angiotensin II AT1 receptor blockade reverses pathological hypertrophy and inflammation in brain microvessels of spontaneously hypertensive rats. Stroke 35:1726–1731.
Chancel, D., Bizet, T., Vandermeersch, S., Pham, P., Levy, B., and Ardaillou, R. (1994). Differential regulation of angiotensin II and losartan binding sites in glomeruli and mesangial cells. Am. J. Physiol. 266:F384–F393.
Braun-Menéndez, E., Fasciolo, J. C., Leloir, L. F., and Muñoz, J. M. (1940). The substance causing renal hypertension. J. Physiol. (Lond.) 98:283–298.
Ciuffo, G. M., and Saavedra, J. M. (1995). Selective peptide and non-peptide ligands differentially bind to angiotensin II AT2 receptor and a non-angiotensin II CGP 42112 binding site. J. Pharmacol. Exp. Ther. 274:1129–1134.
De Gasparo, M., Catt, K. J., Inagami, T., Wright, J. W., and Unger, T. H. (2000). International Union of Pharmacology: XXIII. The angiotensin receptors. Pharmacol. Rev. 52:415–472.
De Oliveira, A. M., Viswanathan, M., Heemskerk, F. M. J., Correa, F. M. A., and Saavedra, J. M. (1994). Specific, non-angiotensin, [125I]CGP 42112 binding sites in rat spleen macrophages. Biochem. Biophys. Res. Com. 200:1049–1058.
Egidy, G., Friedman, J., Viswanathan, M., Wahl, L. M., and Saavedra, J. M. (1997). CGP 42112 partially activates human monocytes and reduces their stimulation by lipopolysaccharides. Am. J. Physiol. 273:C826–C833.
Giulian, D., Chen, J., Ingeman, J. E., George, J. K., and Noponen, M. (1989). The role of mononuclear phagocytes in wound healing after traumatic injury to adult mammalian brain. J. Neurosci. 9:4416–4429.
Heemskerk, F. M. J., and Saavedra, J. M. (1995). Quantitative autoradiography of angiotensin II AT2 receptors with [125I] CGP 42112. Brain Res. 677:29–38.
Heemskerk, F. M. J., Zorad, S., Seltzer, A., and Saavedra, J. M. (1993). Characterization of brain angiotensin II AT2 receptor subtype using [125I] CGP42112A. Neuroreport 4:103–105.
Jöhren, O., Häuser, W., and Saavedra, J. M. (1998). Chemical lesion of the inferior olive reduces [125I]sarcosine1-angiotensin II binding to AT2 receptors in the cerebellar cortex of young rats. Brain Res. 793:176–186.
Jöhren, O., Inagami, T., and Saavedra, J. M. (1995a). AT1A, AT1B, and AT2 angiotensin II receptor subtype gene expression in rat brain. Neuroreport 6:2549–2552.
Jöhren, O., and Saavedra, J. M. (1996). Gene expression of angiotensin II receptor subtypes in the cerebellar cortex of young rats. Neuroreport 7:1349–1352.
Jöhren, O., Viswanathan, M., and Saavedra, J. M. (1995b). Expression of non-angiotensin II [125I]CGP 42112 binding sites on activated microglia after kainic acid induced neurodegeneration. Brain Res. 207:153–161.
Page, I. H. (1987). Hypertension mechanisms. Grune & Stratton. New York, pp. 1–1102.
Page, I. H., and Helmer, O. M. (1940). A crystalline pressor substance (angiotensin) resulting from the reaction between renin and renin activator. J. Exp. Med. 71:29–42.
Roulston, C. L., Lawrence, A. J., Jarrott, B., and Widdop, R. E. (2003). Localization of AT2 receptors in the nucleus of the solitary tract of spontaneously hypertensive and Wistar Kyoto rats using [125I]CGP42112: Upregulation of a non-angiotensin II binding site following unilateral nodose ganglionectomy. Brain Res. 968:139–155.
Roulston, C. L., Lawrence, A. J., Jarrott, B., and Widdop, R. E. (2004). Non-angiotensin II [125I] CGP42112 binding is a sensitive marker of neuronal injury in brainstem following unilateral nodose ganglionectomy: Comparison with markers for activated microglia. Neuroscience 127:753–767.
Roulston, C. L., Lawrence, A. J., Widdop, R. E., and Jarrott, B. (2005). Minocycline treatment attenuates microglia activation and non-angiotensin II [125I]CGP42112 binding in brainstem following nodose ganglionectomy. Neuroscience 135:1241–1253.
Saavedra, J. M. (1992). Brain and pituitary angiotensin. Endocr. Rev. 13:329–380.
Saavedra, J. M. (2005). Brain angiotensin II: New developments, unanswered questions and therapeutic opportunities. Cell. Mol. Neurobiol. 25:485–512.
Saavedra, J. M., Ando, H., Armando, I., Baiardi, G., Bregonzio, C., Juorio, A., and Macova, M. (2005). Anti-stress and anti-anxiety effects of centrally acting angiotensin II AT1 receptor antagonists. Reg. Pept. 128:227–238.
Tsutsumi, K., and Saavedra, J. M. (1991a). Characterization and development of angiotensin II receptor subtypes (AT1 and AT2) in rat brain. Am. J. Physiol. 261:R209–R216.
Tsutsumi, K., and Saavedra, J. M. (1991b). Differential development of angiotensin II receptor subtypes in the rat brain. Endocrinology 128:630–632.
Tsutsumi, K., and Saavedra, J. M. (1991c). Quantitative autoradiography reveals different angiotensin II receptor subtypes in selected rat brain nuclei. J. Neurochem. 56:348–351.
Tsutsumi, K., Strömberg, C., and Saavedra, J. M. (1992). Characterization of angiotensin II receptor subtypes in the rat spleen. Peptides 13:291–296.
Viswanathan, M., de Oliveira, A. M., Correa, F. M. A., and Saavedra, J. M. (1994a). Expression of a novel non-angiotensin II [125I] CGP 42112 binding site in healing wounds of the rat brain. Brain Res. 658:265–270.
Viswanathan, M., de Oliveira, A. M., Wu, R. -M., Chiueh, C. C., and Saavedra, J. M. (1994b). [125I]CGP 42112 reveals a non-angiotensin II binding site in 1-Methyl–4- phenylpyridine (MPP+)-induced brain injury. Cell. Mol. Neurobiol. 14:99–104.
Viswanathan, M., Jöhren, O., de Oliveira, A. M., and Saavedra, J. M. (1996). Increased non-angiotensin II [125I]CGP 42112 binding in rat carotid artery after balloon injury. Peptides 17:695–699.
Viswanathan, M., Strömberg, C., Seltzer, A., and Saavedra, J. M. (1992). Balloon angioplasty enhances the expression of angiotensin II AT1 receptors in neointima of rat aorta. J. Clin. Invest. 909:1707–1712.
Whitebread, S., Mele, M., Kamber, B., and De Gasparo, M. (1989). Preliminary biochemical characterization of two angiotensin II receptor subtypes. Biochem. Biophys. Res. Commun. 163:284–291.
Zhou, J., Ando, H., Macova, M., Dou, J., and Saavedra, J. M. (2005). Angiotensin II AT1 receptor blockade abolishes brain microvascular inflammation and heat shock protein responses in hypertensive rats. J. Cereb. Blood Flow Metab. 25:878–886.
Acknowledgment
This study is supported by the Division of Intramural Research Programs, National Institute of Mental Health, NIH, DHHS.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Saavedra, J.M., Pavel, J. The Discovery of a Novel Macrophage Binding Site. Cell Mol Neurobiol 26, 507–524 (2006). https://doi.org/10.1007/s10571-006-9044-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10571-006-9044-x