Abstract
Myocardial ischemia/reperfusion (I/R) injury is a serious threat to the health of people around the world. Recent evidence has indicated that high-mobility group box-1 (HMGB1) is involved in I/R-induced inflammation, and inflammation can cause necroptosis of cells. Interestingly, dexmedetomidine (DEX) has anti-inflammatory properties. Therefore, we speculated that DEX preconditioning may suppress H/R-induced necroptosis by inhibiting expression of HMGB1 in cardiomyocytes. We found that hypoxia/reoxygenation (H/R) significantly increased cellular damage, as measured by cell viability (100 ± 3.26% vs. 53.33 ± 3.29, p < 0.01), CK-MB (1 vs. 3.25 ± 0.26, p < 0.01), cTnI (1 vs. 2.69 ± 0.31, p < 0.01), inflammation as indicated by TNF-α (1 ± 0.09 vs. 2.57 ± 0.12, p < 0.01), IL-1β (1 ± 0.33 vs. 3.87 ± 0.41, p < 0.01) and IL-6 (1 ± 0.36 vs. 3.60 ± 0.45, p < 0.01), and necroptosis, which were accompanied by significantly increased protein levels of HMGB1. These changes [cellular damage as measured by cell viability (53.33 ± 3.29% vs. 67.59 ± 2.69%, p < 0.01), CK-MB (3.25 ± 0.26 vs. 2.27 ± 0.22, p < 0.01), cTnI (2.69 ± 0.31 vs. 1.90 ± 0.25, p < 0.01), inflammation as indicated by TNF-α (2.57 ± 0.12 vs. 1.75 ± 0.15, p < 0.01), IL-1β (3.87 ± 0.41 vs. 2.09 ± 0.36, p < 0.01) and IL-6 (3.60 ± 0.45 vs. 2.21 ± 0.39, p < 0.01), and necroptosis proteins] were inhibited by DEX preconditioning. We also found that silencing expression of HMGB1 reinforced the protective effects of DEX preconditioning and overexpression of HMGB1 counteracted the protective effects of DEX preconditioning. Thus, we concluded that DEX preconditioning inhibits H/R-induced necroptosis by inhibiting expression of HMGB1 in cardiomyocytes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Acute myocardial infarction (AMI) is the leading cause of morbidity and mortality worldwide. Currently, the optimal strategy for treating AMI is to restore blood perfusion, but recovered blood flow often leads to accumulation of oxygen-free radicals and inflammatory mediators, which results in + ischemia/reperfusion (I/R) injury [1, 2]. During ischemia, loss of blood flow deprives tissue of oxygen and essential metabolites, and excessive inflammatory mediators generated following restoration of blood flow cause further reperfusion injury [3]. Therefore, suppression of inflammation is widely accepted as a therapeutic strategy to mitigate I/R injury [3, 4].
High-mobility group box-1 (HMGB1) is an architectural chromatin-binding factor involved in maintenance of the nucleosome structure and regulation of gene transcription [5]. It exhibits cytokine activity when released into the extracellular space from immune and non-immune cells in response to various stimuli [6]. Extracellular HMGB1 contributes to the pathogenesis of numerous chronic inflammatory and autoimmune diseases, including trauma and ischemia. Emerging evidence indicates that HMGB1 promotes I/R-induced inflammation that can in turn exacerbate I/R injury [7, 8]. However, the mechanism by which HMGB1 regulates I/R injury is not fully understood. In addition, some studies have revealed that dasatinib-induced cardiotoxicity acts via inducing HMGB1-mediated necroptosis in cardiomyocytes, indicating a viable strategy to prevent dasatinib-induced cardiotoxicity. These findings imply that HMGB1 mediates necroptosis. However, the mechanisms and relationships between HMGB1 and necroptosis in myocardial I/R injury are unclear.
Necrosis, which is considered to be a toxic process through which a cell is a passive agent and independent of energy, is often referred as necroptosis and regulated by receptor interacting protein kinase 1 (RIPK1), RIPK3, and mixed lineage kinase domain-like protein (MLKL) that have been recognized to play an important role in I/R injury and are considered to be candidate targets for therapeutic intervention [9]. Xu et al. revealed that dasatinib-induced cardiotoxicity induces HMGB1-mediated necroptosis in cardiomyocytes [10]. Furthermore, emerging evidence indicates that I/R-induced inflammation is closely related to necroptosis, which is a promising therapeutic target [11]. However, the regulation of HMGB1 by drugs is currently unclear and whether HMGB1-related inflammation can induce necroptosis remains to be explored in myocardial I/R diseases.
Dexmedetomidine (DEX) is a selective α2 adrenergic receptor agonist that has sedative, analgesic, and anxiolytic properties [12]. It has been confirmed that DEX preconditioning significantly inhibits I/R-induced inflammation in myocardial cells, thereby enhancing myocardial protection [13]. These data indicate that DEX has anti-inflammatory properties in myocardial I/R diseases. Furthermore, some studies have confirmed that DEX treatment significantly inhibits the expression of HMGB1 [14, 15]. However, the relationships between DEX, HMGB1, and I/R-induced necroptosis remain largely unclear in myocardial I/R injury. Therefore, we speculated that DEX preconditioning may suppress H/R-induced necroptosis by inhibiting expression of HMGB1 in cardiomyocytes.
Methods and Materials
Reagents and Antibodies
Reagents used in experiments were as follows: Dulbecco’s modified Eagle’s medium (DMEM), fetal bovine serum (FBS), penicillin, streptomycin, trypsin-EDTA (GIBCO Laboratories, Grand Island, New York, USA), and DEX (Sigma, St. Louis, MO, USA). Antibodies used in experiments were as follows: anti-β-actin (sc-47778; Santa Cruz Biotechnology, USA), anti-HMGB1 antibody (50599-2-Ig, Proteintech, China), anti-RIPK1 antibody (17519-1-AP, Proteintech), anti-RIPK3 (17563-1-AP, Proteintech), and anti-MLKL (21066-1-AP, Proteintech). Assay kits used in experiments were as follows: cell counting kit-8 (CCK-8) (CK04; Shanghai Tongren, China), rat creatine kinase-MB (CK-MB) ELISA kit (CSB-E14403r, cusabio, China), rat cardiac troponin I (cTnI) ELISA kit (CSB-E08594r, cusabio), rat TNF-α ELISA kit (CSB-E11987r, cusabio), rat IL-6 ELISA kit (CSB-E04640r, cusabio), and rat IL-1β ELISA kit (CSB-E08055r, cusabio).
Cell Culture
H9C2 embryonic rat heart-derived (ventricular) cells (myoblasts) from the ATCC, at passages 5–10, were used in this study. H9C2 cells were cultured in DMEM supplemented with 10% FBS, 100 U/mL penicillin, and 100 mg/mL streptomycin at 37 °C with 5% CO2.
Cell Hypoxia/Reoxygenation (H/R) Model
A hypoxic environment was induced in a humidified and closed plastic vessel. The cells were placed into the hypoxic vessel filled with a mixture of 95% N2 and 5% CO2 for 5 min and subjected to hypoxia for 6 h at 37 °C and then reoxygenated for 4 h by culture in a cell incubator. As shown in Fig. 1, the cells were assigned to the following groups: normal control (C) group that did not undergo H/R and were always cultured in normal medium with 10% FBS and H/R group and 1 μM dexmedetomidine preconditioning (H/R + DEX) group that was cultured in glucose- and serum-free medium during hypoxia, which was replaced with fresh DMEM with 10% FBS and reoxygenated for 4 h at 37 °C.
Ischemia-reperfusion (I/R) cell models and cellular hypoxia-reoxygenation (H/R) schematics. H9C2 cells were exposed to H/R with or without DEX preconditioning. The hypoxic environment was a moist closed plastic vessel aerated with a 95% N2 and 5% CO2 mixture for 5 min before sealed. Cultures were divided into three groups: an untreated control group (C), an H/R untreated group (H/R), and DEX pretreatment group (H/R + DEX)
HMGB1 Knockdown by siRNA
Cells were seeded at 8 h before virus infection. The original medium was then replaced with 2 ml fresh medium containing 6 μg/ml polybrene, and an appropriate amount of lentiviral suspension was added, followed by incubation at 37 °C for 24 h. The lentivirus-containing medium was then replaced with fresh medium. The effect of lentiviral infection was initially observed under a fluorescence microscope and verified by western blotting.
Cell Viability Measured by CCK-8 and Cell Damage Measured by LDH Assays
The reagents in the CCK assay are activated by dehydrogenase in the mitochondria and then produce a highly water soluble, orange methyl product in the presence of an electron coupling agent. The OD value was measured at a wavelength of 450 mM, which indirectly reflected the viability of the cells. Briefly, reagents and samples were prepared according to the manufacturers’ instructions of the assay kits, and we followed the methods of Deng et al. [16].
Assessment of CK-MB, cTnI, TNF-α, IL-1β, and IL-6
Releases of TNF-α, IL-1β, and IL-6, markers of inflammation, increase significantly during I/R injury. CK-MB, cTnI, TNF-α, IL-1β, and IL-6 were detected in culture supernatants by enzyme-linked immunosorbent assays. Briefly, reagents, samples, and standards were prepared according to the manufacturers’ instructions, and we followed the methods of Deng et al. [17].
Western Blotting of RIPK1, RIPK3, MLKL, and HMGB1
At the end of reoxygenation, cells were harvested and centrifuged at 850×g for 5 min at 4 °C. After removing the supernatant, a protease inhibitor was added, and the cells were lysed on ice for 30 min. After centrifugation at 12000×g for 10 min at 4 °C, the supernatant was mixed with an equal volume of loading buffer and heated at 100 °C for 10 min. The protein sample was subjected to electrophoresis, membrane transferred, blocked, exposure to primary and secondary antibodies, and finally analyzed quantitatively. We followed the methods of Muller et al. [18].
Data Analysis and Statistics
All data are presented as the mean ± SD. All statistics were analyzed using SPSS 13.0 software (SPSS, Chicago, IL, USA). Group mean differences were compared by one-way ANOVA with Bonferroni’s correction for pairwise comparisons. Correlations between variables were assessed by Spearman’s coefficient. Differences of p < 0.05 were considered as statistically significant.
Results
DEX Preconditioning Significantly Improves H/R-Induced Cell Injury and Inflammation
We conducted experiments to determine whether H/R caused cell damage and inflammation. As shown in Fig. 2, H/R significantly increased the levels of CK-MB (p < 0.01) (Fig. 2b) and cTnI (p < 0.01) (Fig. 2c), and releases of TNF-α (p < 0.01) (Fig. 2d), IL-1β (p < 0.01) (Fig. 2e), and IL-6 (p < 0.01) (Fig. 2f), but significantly decreased cell viability (Fig. 2a) (p < 0.01). The H/R-induced cell injury and inflammation were drastically attenuated by 1 μM DEX preconditioning (p < 0.01).
DEX preconditioning significantly improved H/R-induced cell injury and inflammation. a Cell viability measured by CCK-8. b The release of CK-MB. c The release of cTnI. d The release of TNF-α. e The release of IL-1β. f The release of IL-6. Mean ± SD are from five different experiments. Single asterisk refers to p < 0.05 and double asterisks refer to p < 0.01
DEX Preconditioning Significantly Improves H/R-Induced Necroptosis
Many studies have confirmed that I/R-induced inflammation is involved in necroptosis. However, the effect of DEX preconditioning on necroptosis is unclear. As shown in Fig. 3, H/R significantly increased the protein levels of RIPK1 (p < 0.01) (Fig. 3b), RIPK3 (p < 0.01) (Fig. 3c), MLKL (p < 0.01) (Fig. 3d), and HMGB1 (p < 0.01) (Fig. 3e), and the above indicators were significantly ameliorated by 1 μM DEX preconditioning.
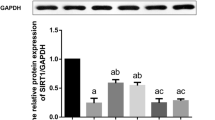
DEX preconditioning significantly improved H/R-induced necroptosis. a Representative images of protein expression. b RIPK1 protein expression. c RIPK3 protein expression. d MIKL protein expression. e HMGB1 protein expression. Mean ± SD are from five different experiments. Single asterisk refers to p < 0.05 and double asterisks refer to p < 0.01
Silencing Expression of HMGB1 Reinforces the Protective Effects of DEX Preconditioning Against H/R-Induced Cellular Damage and Inflammation
Previous evidence suggests that HMGB1 protein is involved in H/R-induced cellular damage and inflammation, but how they are affected by DEX is unknown. To examine the role of HMGB1 in improving I/R injury by DEX preconditioning, we performed lentiviral infection to silence HMGB1 expression and then observed H/R-induced cellular damage and inflammation. As shown in Fig. 4, compared with the H/R group, HMGB1 siRNA or/and DEX preconditioning significantly decreased the levels of CK-MB (p < 0.01) (Fig. 4b) and cTnI (p < 0.01) (Fig. 4c), and releases of TNF-α (p < 0.01) (Fig. 4d), IL-1β (p < 0.01) (Fig. 4e), and IL-6 (p < 0.01) (Fig. 4f) but significantly increased cell viability (p < 0.01) (Fig. 4a). Compared with HMGB1 siRNA treatment alone or DEX preconditioning alone under H/R, combined treatment of HMGB1 siRNA and DEX preconditioning had better protective effects against H/R-induced cellular damage and inflammation (p < 0.01).
Interfering expression of HMGB1 reinforces the protective effects of DEX preconditioning against H/R-induced cellular damage and inflammation. a Cell viability measured by CCK-8. b The release of CK-MB. c The release of cTnI. d The release of TNF-α. e The release of IL-1β. f The release of IL-6. Mean ± SD are from five different experiments. Single asterisk refers to p < 0.05 and double asterisks refer to p < 0.01
Silencing Expression of HMGB1 Reinforces the Protective Effects of DEX Preconditioning Against H/R-Induced Necroptosis
We performed lentiviral infection to silence HMGB1 expression and then observed the relationship between HMGB1 protein expression and the protective effects of DEX preconditioning against H/R-induced necroptosis. As shown in Fig. 5, H/R significantly increased the protein levels of RIPK1 (p < 0.01) (Fig. 5b), RIPK3 (p < 0.01) (Fig. 5c), MLKL (p < 0.01) (Fig. 5d), and HMGB1 (p < 0.01) (Fig. 5e). The trends of the above indicators were effectively reversed by DEX preconditioning or HMGB1 siRNA treatment. Compared with the H/R + DEX group, the protein levels of RIPK1 (p < 0.01) (Fig. 5b), RIPK3 (p < 0.01) (Fig. 5c), MLKL (p < 0.01) (Fig. 5d), and HMGB1 (p < 0.01) (Fig. 5e) in the H/R + DEX + siRNA group were decreased significantly. Therefore, DEX preconditioning effectively ameliorated H/R-induced necroptosis that was effectively enhanced by HMGB1 siRNA.
Interfering expression of HMGB1 reinforces the protective effects of DEX preconditioning against H/R-induced necroptosis. a Representative images of protein expression. b RIPK1 protein expression. c RIPK3 protein expression. d MIKL protein expression. e HMGB1 protein expression. Mean ± SD are from five different experiments. Single asterisk refers to p < 0.05 and double asterisks refer to p < 0.01
Overexpression of HMGB1 Counteracts the Protective Effects of DEX Preconditioning against H/R-Induced Cellular Damage and Inflammation
To confirm the role of HMGB1 in the effects of DEX preconditioning against H/R-induced cellular damage and inflammation, we overexpressed HMGB1 to observe its effects. As shown in Fig. 6, H/R-induced cellular damage and inflammation were significantly increased by overexpression of HMGB1 but decreased by DEX preconditioning. In addition, compared with the H/R + DEX + OE group, CK-MB (p < 0.01) (Fig. 6b), cTnI (p < 0.01) (Fig. 6c), and releases of TNF-α (p < 0.01) (Fig. 6d), IL-1β (p < 0.01) (Fig. 6e), and IL-6 (p < 0.01) (Fig. 6f) were decreased significantly, but cell viability was increased significantly (p < 0.01) (Fig. 6a) in H/R + DEX group.
Overexpression of HMGB1 countermands the protective effects of DEX preconditioning against H/R-induced cellular damage and inflammation. a Cell viability measured by CCK-8. b The release of CK-MB. c The release of cTnI. d The release of TNF-α. e The release of IL-1β. f The release of IL-6. Mean ± SD are from five different experiments. Single asterisk refers to p < 0.05 and double asterisks refer to p < 0.01
Overexpression of HMGB1 Counteracts the Protective Effects of DEX Preconditioning Against H/R-Induced Necroptosis
As shown in Fig. 7, compared with the H/R + DEX + OE group, the protein levels of RIPK1, RIPK3, and MLKL in the H/R + DEX group were significantly decreased, which were accompanied by a significant increase in the protein level of HMGB1. Therefore, overexpression of HMGB1 counteracted the protective effects of DEX preconditioning against H/R-induced necroptosis.
Overexpression of HMGB1 countermands the protective effects of DEX preconditioning against H/R-induced necroptosis. a Representative images of protein expression. b RIPK1 protein expression. c RIPK3 protein expression. d MIKL protein expression. e HMGB1 protein expression. Mean ± SD are from five different experiments. Single asterisk refers to p < 0.05 and double asterisks refer to p < 0.01
Discussion
The findings of the current study showed that DEX preconditioning protected cardiomyocytes against H/R injury by inhibiting inflammation-mediated necroptosis through downregulation of HMGB1. During either H/R or DEX preconditioning, the expression of HMGB1 was correlated with necroptosis proteins. Therefore, we established a relationship between HMGB1 and necroptosis in myocardial H/R and confirmed associations between DEX preconditioning and necroptosis in myocardial H/R injury.
Some recent studies have shown the effects of HMGB1 in I/R injury [19, 20]. For example, Tong et al. revealed that short-term pretreatment with celastrol protects against myocardial I/R injury by suppressing myocardial apoptosis, the inflammatory response, and oxidative stress via PI3K/Akt pathway activation and HMGB1 inhibition [21]. Furthermore, Zhang et al. confirmed that DEX preconditioning reduces myocardial I/R injury in part by attenuating inflammation, which may be attributed to downregulation of the HMGB1-TLR4-MyD88-NF-κB signaling pathway by α2-adrenergic receptor activation [22]. These studies suggest that HMGB1 may be involved in I/R-induced inflammation and that DEX may have the ability to regulate HMGB1 expression, which was conformed in our study. We confirmed a relationship between HMGB1 and necroptosis in myocardial H/R and the association between DEX preconditioning and necroptosis in myocardial H/R injury. Recently, it has been found that DEX, which is a potent α2-adrenergic receptor agonist, has eightfold higher affinity than clonidine and significantly decreases the inflammation of cardiomyocytes while exerting a sedative effect for clinical anesthesia. In general, inflammation is beneficial and the automatic defense response, but excessive release of inflammatory factors during reperfusion is often considered to aggravate cardiomyocyte ischemic injury. HMGB1 is closely related to inflammation in myocardial I/R injury. In addition, HMGB1-induced necroptosis is a major form of myocardial cell injury. Therefore, DEX improves myocardial cell inflammation and necroptosis by inhibiting the expression of HMGB1, indicating multiple forms of cell death in myocardial I/R injury. Although, how these different forms of cell death are linked together and how they are regulated in myocardial I/R injury require further research.
However, we also found that some studies are worth us to learn and think and to further improve. Sun et al. confirmed that DEX protects against I/R-induced cardiac functional and histological changes, inflammation, and oxidative stress by activating the AMPK/PI3K/Akt/eNOS pathway [23]. In addition, Chen et al. found that NOD−, LRR−, and CARD− containing 5 (NLRC5)−/− mice show significantly stronger histological damage, inflammatory responses, oxidative stress, and apoptosis after I/R compared with WT mice [24]. Deng et al. confirmed that propofol counteracts cardiomyocyte H/R injury by attenuating mitochondrial damage and improving mitochondrial biogenesis through upregulating Cav-3 during hyperglycemia [17]. Although we observed different forms of cell death, whether DEX can also improve I/R injury in diabetic patients through HMGB1 is an interesting research direction, as they have a high probability of developing I/R disease that is closely related to inflammation. We can also compare the difference between DEX and propofol in I/R injury. In addition, there are many emerging forms of cell death such as autophagy [25], ferroptosis [18], and pyroptosis [26]. In particular, pyroptosis is closely related to inflammasomes. However, our study only explored the relationship between inflammation and necroptosis and did not include other emerging forms of cell death. Thus, there are some limitations in our study. We only examined how DEX preconditioning improved I/R-induced inflammation, but the association between oxidative stress and DEX preconditioning also needs exploration. In addition, we did not study the signaling pathway in I/R-induced inflammation and necroptosis ameliorated by DEX preconditioning. Our experimental results also require validation in vivo in animal experiments, which will be performed in a subsequent study.
References
Koeppen M, Lee JW, Seo SW, Brodsky KS, Kreth S, Yang IV, et al. Hypoxia-inducible factor 2-alpha-dependent induction of amphiregulin dampens myocardial ischemia-reperfusion injury. Nat Commun. 2018;9:816.
Kawai H, Chaudhry F, Shekhar A, Petrov A, Nakahara T, Tanimoto T, Kim D, Chen J, Lebeche D, Blankenberg FG, et al. Molecular imaging of apoptosis in ischemia reperfusion injury with radiolabeled Duramycin targeting phosphatidylethanolamine: Effective Target Uptake and Reduced Nontarget Organ Radiation Burden. JACC Cardiovasc Imaging. 2018.
Ferrari RS, Andrade CF. Oxidative stress and lung ischemia-reperfusion injury. Oxidative Med Cell Longev. 2015;2015:590987.
Chorawala MR, Prakash P, Doddapattar P, Jain M, Dhanesha N, Chauhan AK. Deletion of extra domain a of fibronectin reduces acute myocardial ischaemia/reperfusion injury in hyperlipidaemic mice by limiting thrombo-inflammation. Thromb Haemost. 2018;118:1450–60.
Roberta A, Vicentino R, Carneiro VC, Carneiro VC, Allonso D, Guilherme R, et al. Emerging role of HMGB1 in the pathogenesis of schistosomiasis liver fibrosis. Front Immunol. 2018;9:1979.
Sekiguchi F, Domoto R, Nakashima K, Yamasoba D, Yamanishi H, Tsubota M, et al. Paclitaxel-induced HMGB1 release from macrophages and its implication for peripheral neuropathy in mice: evidence for a neuroimmune crosstalk. Neuropharmacology. 2018;141:201–13.
Loukili N, Rosenblatt-Velin N, Li J, Clerc S, Pacher P, Feihl F, et al. Peroxynitrite induces HMGB1 release by cardiac cells in vitro and HMGB1 upregulation in the infarcted myocardium in vivo. Cardiovasc Res. 2011;89:586–94.
Andrassy M, Volz HC, Igwe JC, Funke B, Eichberger SN, Kaya Z, et al. High-mobility group Box-1 in ischemia-reperfusion injury of the heart. Circulation. 2008;117:3216–26.
In EJ, Lee Y, Koppula S, Kim TY, Han JH, Lee KH, et al. Identification and characterization of NTB451 as a potential inhibitor of necroptosis. Molecules. 2018;23.
Xu Z, Jin Y, Yan H, Gao Z, Xu B, Yang B, et al. High-mobility group box 1 protein-mediated necroptosis contributes to dasatinib-induced cardiotoxicity. Toxicol Lett. 2018;296:39–47.
Galluzzi L, Kepp O, Chan FK, Kroemer G. Necroptosis: mechanisms and relevance to disease. Annu Rev Pathol. 2017;12:103–30.
Abdel-Ghaffar HS, Kamal SM, El Sherif FA, Mohamed SA. Comparison of nebulised dexmedetomidine, ketamine, or midazolam for premedication in preschool children undergoing bone marrow biopsy. Br J Anaesth. 2018;121:445–52.
Peng K, Qiu Y, Li J, Zhang ZC, Ji FH. Dexmedetomidine attenuates hypoxia/reoxygenation injury in primary neonatal rat cardiomyocytes. Exp Ther Med. 2017;14:689–95.
Zhang JJ, Peng K, Zhang J, Meng XW, Ji FH. Dexmedetomidine preconditioning may attenuate myocardial ischemia/reperfusion injury by down-regulating the HMGB1-TLR4-MyD88-NF-small ka, CyrillicB signaling pathway. PLoS One. 2017;12:e0172006.
Meng L, Li L, Lu S, Li K, Su Z, Wang Y, et al. The protective effect of dexmedetomidine on LPS-induced acute lung injury through the HMGB1-mediated TLR4/NF-kappaB and PI3K/Akt/mTOR pathways. Mol Immunol. 2018;94:7–17.
Deng F, Wang S, Cai S, Hu Z, Xu R, Wang J, et al. Inhibition of caveolae contributes to propofol preconditioning-suppressed microvesicles release and cell injury by hypoxia-reoxygenation. Oxidative Med Cell Longev. 2017;2017:3542149.
Deng F, Wang S, Zhang L, Xie X, Cai S, Li H, et al. Propofol through upregulating caveolin-3 attenuates post-hypoxic mitochondrial damage and cell death in H9C2 cardiomyocytes during hyperglycemia. Cell Physiol Biochem. 2017;44:279–92.
Muller T, Dewitz C, Schmitz J, Schroder AS, Brasen JH, Stockwell BR, et al. Necroptosis and ferroptosis are alternative cell death pathways that operate in acute kidney failure. Cell Mol Life Sci. 2017;74:3631–45.
McDonald KA, Huang H, Tohme S, Loughran P, Ferrero K, Billiar T, et al. Toll-like receptor 4 (TLR4) antagonist eritoran tetrasodium attenuates liver ischemia and reperfusion injury through inhibition of high-mobility group box protein B1 (HMGB1) signaling. Mol Med. 2015;20:639–48.
Mersmann J, Iskandar F, Latsch K, Habeck K, Sprunck V, Zimmermann R, et al. Attenuation of myocardial injury by HMGB1 blockade during ischemia/reperfusion is toll-like receptor 2-dependent. Mediat Inflamm. 2013;2013:174168.
Tong S, Zhang L, Joseph J, Jiang X. Celastrol pretreatment attenuates rat myocardial ischemia/ reperfusion injury by inhibiting high mobility group box 1 protein expression via the PI3K/Akt pathway. Biochem Biophys Res Commun. 2018;497:843–9.
Sun HJ, Lu Y, Wang HW, Zhang H, Wang SR, Xu WY, et al. Activation of endocannabinoid receptor 2 as a mechanism of propofol pretreatment-induced cardioprotection against ischemia-reperfusion injury in rats. Oxidative Med Cell Longev. 2017;2017:2186383.
Sun Y, Jiang C, Jiang J, Qiu L. Dexmedetomidine protects mice against myocardium ischaemic/reperfusion injury by activating an AMPK/PI3K/Akt/eNOS pathway. Clin Exp Pharmacol Physiol. 2017;44:946–53.
Chen Z, Ding T, Ma CG. Dexmedetomidine (DEX) protects against hepatic ischemia/reperfusion (I/R) injury by suppressing inflammation and oxidative stress in NLRC5 deficient mice. Biochem Biophys Res Commun. 2017;493:1143–50.
Nishida K, Otsu K. Autophagy during cardiac remodeling. J Mol Cell Cardiol. 2016;95:11–8.
Frank D, Vince JE. Pyroptosis versus necroptosis: similarities, differences, and crosstalk. Cell Death Differ. 2018.
Acknowledgments
We thank M. Arico from Liwen Bianji, Edanz Group China (www.liwenbianji.cn/ac), for editing the English text of a draft of this manuscript.
Funding
This study was supported by Taihe Hospital Science and Technology Project in 2018 to Dr. Chen, Jingyi (grant numbers: 2018JJXM046).
Author information
Authors and Affiliations
Contributions
Jingyi Chen conceived and designed the project. Jingyi Chen performed the experiments with the help of Zhenzhen Jiang, Xing Zhou, Xingxing Sun, Jianwei Cao, Yongpan Liu, and Xianyu Wang. Jingyi Chen wrote the manuscript. All authors discussed the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interests.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed Consent
This article does not contain any studies with human participants performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, J., Jiang, Z., Zhou, X. et al. Dexmedetomidine Preconditioning Protects Cardiomyocytes Against Hypoxia/Reoxygenation-Induced Necroptosis by Inhibiting HMGB1-Mediated Inflammation. Cardiovasc Drugs Ther 33, 45–54 (2019). https://doi.org/10.1007/s10557-019-06857-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10557-019-06857-1