Abstract
Circulating leukocyte subtypes and monocyte subsets are independent predictors of cardiovascular events. We hypothesized that an increased leukocyte subtype would predict severe coronary stenosis and extensive plaque involvement. We retrospectively analyzed clinical, laboratory, and coronary CT data in a total of 588 asymptomatic adults (69% men; mean age, 57 ± 9 years) undergoing a general health check-up. Intermediate CD14++CD16+ monocyte count had the strongest association with mixed and calcified plaque scores, whereas the numbers of neutrophils and classical CD14++CD16− monocytes were significantly associated with non-calcified plaque score. Only high CD14++CD16+ monocyte count (>12 cells/μL) significantly predicted extensive plaque involvement [odds ratio 3.16 (95% confidence interval 1.84–5.43), P < 0.001; quartile 4 vs. 1–3] and severe coronary stenosis [3.67 (1.84–7.33), P < 0.001; quartile 4 vs. 1–3] after adjustments for Framingham Risk Score (FRS), metabolic syndrome, and C-reactive protein. The CD14++CD16+ monocyte count, when added to FRS, significantly reclassified 30.4 and 26.7% of the overall and 50.2 and 36.2% of the intermediate-risk population (FRS 6–20%) for predicting extensive plaque involvement and severe coronary stenosis, respectively. Thus, in asymptomatic individuals, intermediate CD14++CD16+ monocyte could independently predict severe CAD and improve risk stratification.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Coronary artery disease (CAD) is a manifestation of complex interactions between circulating leukocytes and the vascular wall [1]. High leukocyte count, monocyte count, neutrophil count, and neutrophil-to-lymphocyte ratio predict increased cardiovascular risk [2–5]. Moreover, monocytes are subdivided into 3 subsets based on the expression of the CD14 and CD16 receptors: classical CD14++CD16−, intermediate CD14++CD16+, and non-classical CD14+CD16++ subsets [6]. They constitute the population of monocytes around 85, 5, and 10%, respectively, in healthy conditions. A preferential increase in certain monocyte subsets, specifically classical or intermediate monocytes [7, 8], also predicts a poor cardiovascular outcome. Despite these associations of leukocyte subtypes with cardiovascular risk, little evidence has been reported about which subtype impact CAD most [3, 9].
Coronary atherosclerosis precedes major coronary events. Coronary computed tomography (CT) angiography can reliably show the manifestations of coronary atherosclerosis, including coronary plaque stenosis, composition, and extent [10]. At the same extent and stenotic severity of coronary plaques, a greater proportion of segments with non-calcified and mixed plaque confer an independent risk above and beyond stenotic severity alone [11]. A few evidence has suggested that coronary non-calcified plaque is associated with CD14+CD16+ monocytes, neutrophils, and the neutrophil-to-lymphocyte ratio in CAD patients [12, 13]. Nevertheless, previous studies were performed in smaller sample sizes, and the associations had not been adjusted for clinical risk factors and other inflammatory markers, such as C-reactive protein (CRP), thus not providing conclusive results. Moreover, most previous studies have investigated the relationship between a single leukocyte subtype and the non-calcified coronary plaque. A broader investigation of the association between coronary plaque subtypes and leukocyte subtypes is warranted. Furthermore, clinical studies investigating the features of circulating monocytes in advanced coronary lesions are lacking. Therefore, in the present study, we aimed to explore the relationships between leukocyte subtypes and coronary plaque composition, extent, and stenosis, and to assess which leukocyte subtype is best associated with severe stenosis and extensive involvement independent of clinical risk factors and inflammatory parameter.
Methods
Study participants
Study participants were consecutively enrolled after undergoing coronary CT angiography as part of a general health check-up protocol at National Taiwan University Hospital from January 2011 to June 2012. Our Ethics Committee approved the study protocol, and informed consent was obtained from all individual participants included in the study. A medical history and a physical examination were taken by a physician in all subjects. The major exclusion criteria were a history of arrhythmia, typical angina or known CAD, serum creatinine level ≥2.0 mg/dL, known hypersensitivity to iodine-based contrast agents, and evidence for an overt inflammatory disease. Structured questionnaires on family history, lifestyle habits, and medical history were administered, and anthropometric measurements, such as body weight, body height, and waist circumference, were recorded. Hypertension was defined as blood pressure ≥140/90 mmHg and/or a history of antihypertensive medication. Diabetes mellitus was defined as a history of diabetes, current medical treatment, or fasting plasma glucose ≥126 mg/dL. Smoking history was classified as current smoker or not. A current smoker was defined as having regularly smoked cigarettes in the year prior to the examination. The definition of metabolic syndrome (MS) was modified according to the National Cholesterol Education Program’s Adult Treatment Panel III criteria, which classifies abdominal obesity as a waistline of 90 cm for men and 80 cm for women. The Framingham Risk Score (FRS) is based on data from a sample of the Framingham Heart studies. The defining risk factors are age, cigarette smoking, blood pressure, total cholesterol, high-density lipoprotein cholesterol, and diabetes. A FRS value <6, 6–20, or >20% indicates a low, intermediate, or high 10-year risk for coronary events [14]. All the biochemical measurements, including glucose, total cholesterol, total triglycerides, low-density lipoprotein cholesterol, and high-density lipoprotein cholesterol, were measured using a Hitachi 7450 automated analyzer (Hitachi, Tokyo, Japan). Hemoglobin A1c levels were measured using a DCA 2000 analyzer (Bayer Diagnostics, Elkhart, IN). Plasma CRP levels were determined using a high-sensitivity immunoturbidimetric assay (Denka Seiken, Tokyo, Japan) on a Hitachi 911 analyzer (Roche Diagnostics, Indianapolis, IN). The coefficients of variation of these measurements were approximately 5%.
Leukocyte subtype analysis
For the leukocyte subtypes studies, 2.7 mL of peripheral venous blood was drawn into ethylenediaminetetraacetate (EDTA) tubes at 8 A.M. after an overnight fast and immediately analyzed. Leukocyte and subtype counts were determined using an automated cell counter (Sysmex XE-5000-Hematology-Analyzer, Tokyo, Japan). For the monocyte subpopulation analysis, 100 µL of EDTA anti-coagulated blood was incubated with monoclonal antibodies against CD14 (fluorescein isothiocyanate-conjugated; BD Bioscience, San Jose, CA, USA) and CD16 (phycoerythrin-Cy5-conjugated; BD Bioscience) for 15 min at room temperature in the dark. Matched isotype antibodies (BD Bioscience) were used as negative controls. Lysing solution (1 mL; BD FACS Lyse, Lysing Solution; Becton Dickinson Germany) was used to lyse the erythrocytes and fix the leukocytes. Cytometric analyses were performed using a flow cytometer (FACSCalibur™; BD Bioscience, Franklin Lakes, NJ, USA), and the results were analyzed using Cell Quest software (BD Bioscience). Monocytes were first gated in a forward scatter/side scatter dot plot. The percentage of CD14+CD16+ monocytes was then measured by the 2-color mean fluorescence intensity within the monocyte gate. CD14++CD16− cells were defined as monocytes that expressed CD14 but not CD16. CD16+ cells were defined as monocytes that expressed CD16 and either high or low levels of CD14. Thus, CD14++CD16+ and CD14+CD16++ cells were analyzed separately (Fig. 1). Monocyte subset counts were calculated by multiplying percentages of gated monocyte subsets with absolute monocyte count obtained from the automated cell counter. The coefficient of variation for absolute monocyte count is 1.9%, and for surface CD14 and CD16 markers are <5%.
Coronary plaque analysis
Subjects without contraindications received propranolol or diltiazem to target a heart rate of ≤65 bpm and 0.4 mg of nitroglycerin sublingually before image acquisition. Cardiac CT angiography was performed using a 256-slice scanner (Brilliance iCT, Philips, Eindhoven, The Netherlands). Initial unenhanced axial CT imaging of the heart was obtained with a prospective ECG trigger for the purpose of coronary artery calcium scoring (Agatston Method). Then, nonionic contrast media (iopromide; 370 mg/mL Ultravist, Bayer HealthCare) was injected using a dual-barrel injector (Stellant D, Medrad). Contrast-enhanced CT imaging was performed to obtain images from the mid-ascending aorta to the diaphragm. When the heart rate was ≤65/min, prospective ECG triggering was used, and images were obtained at 70, 75 and 80% of the cardiac cycle. When the heart rate was >65/min, retrospective ECG gating was used, and images were reconstructed at 40, 45, 55, 70, 75 and 80% of the cardiac cycle. Scanning parameters are 128 × 0.625 mm collimation, 0.27 s tube-rotation time, and 100–120 kV tube-voltage adjusted based on subjects’ BMI. The median radiation dose was 3.0 mSv (interquartile range 2.3–3.7) with the use of prospective ECG triggering and 6.3 mSv (interquartile range 4.2–9.7) with the use of retrospective ECG gating, using the product of the dose-length product and a conversion factor (0.0140 mSv/mGy cm).
The CT angiography imaging analysis was performed by a cardiac radiologist (Lee WJ) who was blinded to the subjects’ clinical information and followed the recommended quantitative stenosis grading in the SCCT Guidelines for the interpretation and reporting of coronary computed tomographic angiography [15]. A 17-segment model of the coronary artery was used for the evaluation and visual semi-quantification of coronary artery plaque. In each coronary artery segment, coronary atherosclerosis was defined as tissue structures >1 mm2 that existed either as (1) calcified plaques with high density compared to the contrast-enhanced vessel lumen, (2) non-calcified plaques with lower density, or (3) mixed plaques (calcified and non-calcified morphologies) [16]. Then, we adopted the segment-involvement score constructed by Min et al. [11] to assess the extent of coronary plaques. The score was calculated as the total number of coronary artery segments exhibiting plaque irrespective of the degree of luminal stenosis within each segment (minimum = 0; maximum = 17). The same method was used to sum segments according to plaque type (isolated calcified plaque, isolated non-calcified plaque, and mixed plaque). The presence of one or more stenoses with a ≥70% reduction in luminal diameter in at least one major epicardial coronary artery or its branches was defined as severe stenosis. The sensitivity, specificity, and accuracy of CT angiography analyzed by Dr. Lee WJ were 85, 100, and 92%, respectively, to detect significantly stenotic lesions (≥50% diameter stenosis), using invasive coronary angiography as the standard of reference for per-segment analysis [17].
Statistical analysis
Sample size was calculated to detect an odds ratio of 2.0 in severe CAD among the two leukocyte subtype groups: lower (quartile 1–3) and higher (quartile 4). Power analysis revealed a minimum of 414 participants in the lower group and 138 in the higher group (total 552) with power 80% at a significance level <0.05 for a two-sided test. Data are presented as the mean ± standard deviation or the median (25–75th percentile), and frequencies are presented as counts (%). The data were tested for normal distribution prior to their utilization in the parametric analysis. The distribution of cardiovascular risk factors was assessed, and differences in group means or proportions were evaluated using Student’s t test or Pearson’s Chi square test, as appropriate. In non-normally distributed variables, differences in group medians were assessed using a nonparametric test. Unadjusted and adjusted partial Spearman’s rank correlations were determined for leukocyte subtypes and coronary plaque scores after adjusting for age and sex (model 1) and FRS, MS, and CRP (model 2). Multivariate logistic regression with Bonferroni correction were used to examine the association between solely leukocyte subtype and the presence of extensive plaque involvement plaque or severe stenosis. Plaques were analyzed on a per-patient level, and initial analysis was unadjusted, and then adjusted for age and sex (model 1), and finally adjusted for FRS, MS, and CRP (model 2). As seven multivariate models were created in this study, using a P value of 0.05, a Bonferroni-adjusted threshold of 0.007 was considered to be significant. Area under the receiver-operating characteristic curve (AUC) analysis, integrated discrimination improvement (IDI) value, and net reclassification improvement (NRI) were used to assess the extent to the leukocyte subtype increased the discriminative performance of CAD prediction. All calculations were performed with SPSS statistical software (SPSS 18.0 version for windows, SPSS, Chicago, IL, USA) and Stata (version 13.1; StataCorp, College Station, TX).
Results
Baseline characteristics
The study population comprised 588 individuals (404 men, 69%) with a mean age of 57 ± 9 years. After the exclusion of 33 (0.3%) coronary segments with insufficient image quality, plaque of any type was shown in 1026 (10%) segments. At least one coronary plaque was identified in 320 subjects (54.4%); 77 subjects (13.1%) had extensive plaque involvement (SIS > 4); 42 subjects (7.1%) had at least one severe coronary stenosis (≥70%). Table 1 summarizes the participants’ characteristics according to coronary plaque, extensive plaque involvement, or severe coronary stenosis. All the coronary heart disease risk factors were significantly different between subjects with and without coronary plaque (P < 0.05). Nearly all the leukocyte subtypes were positively correlated with obesity, blood pressure, smoking, C-reactive protein and Framingham risk score, and negatively correlated with HDL cholesterol (Supplementary Table S1). Specifically, the neutrophil count correlated better with high glucose level, whereas the monocyte count correlated better with low HDL cholesterol. The leukocyte, neutrophil, and monocyte counts as well as the monocyte subset populations were increased in subjects with any coronary plaque. However, the proportions of the monocyte subsets were similar between subjects with and without any coronary plaque. Among the subjects with any coronary plaque, those with extensive involvement or severe stenosis had a worse profile in terms of age, diabetes mellitus, hypertension, MS, FRS, and CRP. Those with extensive involvement or severe stenosis had a higher proportion and number of intermediate CD14++CD16+ monocytes. On the other hand, the leukocyte, neutrophil, and monocyte counts as well as classical CD14++CD16− and non-classical CD14+CD16++ monocyte subset populations were similar between subjects with and without extensive involvement or severe stenosis.
Coronary plaque types, extent, and stenosis
Figure 2 illustrates the three coronary plaque types and the stenosis severity analyzed in our study. The total number of subjects in the cohort with <50, 50–69, and ≥70% stenosis were 214 (36.4%), 64 (10.9%), and 42 (7.1%), respectively. A total of 1026 coronary plaques were found and the most common plaque type was calcified plaque, followed by mixed plaque and then non-calcified plaque (62, 26, and 12%, respectively). Similarly, a total of 530 coronary plaques were found in 77 subjects with extensive plaque involvement and the most common plaque type was calcified plaque, followed by mixed plaque and then non-calcified plaque (60, 30, and 10%, respectively). Besides, a total of 46 coronary plaques with severe stenosis were found in 42 subjects and the most common plaque type was mixed plaque, followed by calcified plaque and then non-calcified plaque (72, 15, and 13%, respectively). Among the subjects with coronary plaques, those with extensive involvement had higher calcium and plaque scores than those without. Those with severe stenosis had a higher score in terms of calcium, total plaque, mixed plaque, and calcified plaque but not non-calcified plaque (Table 1).
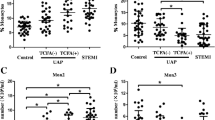
Representative images of coronary CT angiography demonstrating the plaque subtypes and stenosis: non-calcified coronary plaque with >70% stenosis, mixed-calcified plaque with 50% stenosis, calcified coronary plaque with <50% stenosis, and normal coronary artery without plaque. The corresponding proportion of monocyte subsets and count of intermediate CD14++CD16+ monocytes were shown in dot plots
Leukocyte subtypes and coronary plaques
Table 2 presents the correlations between leukocyte subtypes and plaque scores. Calcium score was significantly correlated with all the leukocyte subtypes, especially monocytes and monocyte subsets (Fig. 3). Specifically, the neutrophil count and the classical CD14++CD16− monocyte count correlated better with the non-calcified plaque score, whereas the intermediate CD14++CD16+ monocyte count correlated better with the calcium score, and the total, mixed plaque score, and calcified plaque score. After adjustment for age and sex (model 1), the numbers of neutrophils and classical CD14++CD16− monocytes remained correlated with the non-calcified plaque score, and intermediate CD14++CD16+ monocyte remained correlated with the calcium score and the total, mixed, and calcified plaque scores. Similar results were obtained after adjusting for FRS, MS, and CRP (model 2). By contrast, the neutrophil-to-lymphocyte ratio and non-classical CD14+CD16++ monocyte showed no correlation with the calcium score or any plaque score after adjusting for model 1 or model 2.
Predictors of extensive plaque involvement and severe coronary stenosis
As shown in Table 3, in a univariate analysis, the presence of extensive plaque involvement was significantly associated with neutrophils, monocytes, classical CD14++CD16− monocytes, or intermediate CD14++CD16+ monocytes in the upper quartile. After adjustment for age and sex (model 1) in a multivariate logistic regression analysis, only intermediate CD14++CD16+ monocyte count in the upper quartile (>12 cells/μL) remained an independent predictor for the presence of extensive plaque involvement. Similar results were obtained after adjusting for FRS, MS, and CRP (model 2). On the other hand, in a univariate analysis, the presence of severe coronary stenosis was significantly associated with monocytes and their subset populations in the upper quartile. After adjustment for age and sex (model 1), only intermediate CD14++CD16+ monocyte count in the upper quartile (>12 cells/μL) remained an independent predictor for the presence of severe coronary stenosis. Similar results were obtained after adjusting for FRS, MS, and CRP (model 2).
Predictive value of intermediate CD14++CD16+ monocyte
Table 4 details the incremental discriminative ability of intermediate CD14++CD16+ monocyte parameter. In the analysis the area under the receiver operating characteristic curve for the extensive plaque involvement, the areas under curve for the model with FRS alone was 0.74, which increased significantly with the addition of intermediate CD14++CD16+ monocyte (+0.05; P for improvement = 0.016). A similar magnitude of effect was observed for the severe coronary stenosis (the area increased from 0.72 to 0.81 after intermediate CD14++CD16+ monocyte was added to FRS; P < 0.001). Overall, the absolute IDI for the extensive plaque involvement was 0.03 (P for improvement = 0.003) and 0.03 (P for improvement = 0.018) for the severe coronary stenosis, with categoryless NRIs of 0.54 and 0.68 for the extensive plaque involvement and the severe coronary stenosis, respectively (both P < 0.001). Comparing the predicted and observed data, we found non-significant P values for the Hosmer–Lemeshow statistics in the multiple variable models. Upon examining the reclassification properties of intermediate CD14++CD16+ monocyte, we observed an overall improvement in the net risk stratification of up to 30.4% for predicting extensive plaque involvement and 26.7% for predicting severe coronary stenosis (P < 0.001 for both). For individuals at intermediate risk (FRS 6–20%), the net reclassification was 50.2% for predicting extensive plaque involvement and 36.2% for predicting severe coronary stenosis (P < 0.001 for both) (Tables 5, 6). The improvement was largely driven by reclassifying non-diseased subjects into a lower risk category.
Discussion
To the best of our knowledge, this is the first study to report the relationship among leukocyte subtype, coronary plaque composition, and severe stenosis in a cohort of apparently healthy individuals. The main findings of this study are as follows. First, all the measured leukocyte subtype counts were higher in subjects with any coronary plaque than in those without, but intermediate CD14++CD16+ monocytes were the only leukocyte subtype that was increased in subjects with severe stenosis compared with those with non-severe luminal narrowing. Second, leukocyte subtypes corresponded to different coronary plaque compositions. Neutrophils and classical CD14++CD16− monocytes correlated better with non-calcified plaque, whereas intermediate CD14++CD16+ monocytes correlated better with mixed plaque and calcified plaque. Third, intermediate CD14++CD16+ monocytes were the only leukocyte subtype that was associated with the presence of extensive involvement or severe stenosis independent of the Framingham Risk Score, metabolic syndrome, and C-reactive protein. In apparently healthy adults, addition of flow cytometric measurements of intermediate CD14++CD16+ monocyte significantly improves prediction for severe CAD beyond the predictive ability of a traditional FRS-type risk model. This improvement is mainly the result of net improvement in down-classifying risk in participants who did not have extensive plaque involvement or severe coronary stenosis. This is particularly important when the relative ease of obtaining an intermediate CD14++CD16+ monocyte is compared against radiation exposure and the expense involved in obtaining an individual’s coronary CT angiography.
In the present study, the relationship between coronary plaque morphology and stenosis severity was also investigated, and mixed plaque was most associated with moderate or severe stenosis. Indeed, the major cardiac event rate is significantly higher in patients with noncalcified or mixed plaque than in patients with calcified plaque [18]. Additionally, compared to histology, coronary CT angiography reliably depicts advanced stage coronary mixed plaque with an overall good correlation with stenosis degree [19]. Furthermore, the major determinants of coronary plaques in coronary events are a large plaque burden, a small luminal area and a thin-cap fibroatheroma, which are more frequently observed in mixed plaques than in other plaque types [20]. These observations support evidence that mixed plaques are involved in ischemic cardiovascular disease, particularly major events. Among the leukocyte subtypes, intermediate CD14++CD16+ monocytes correlated best with coronary calcium and mixed plaque severity. This relationship might translate into better discrimination when predicting severe coronary stenosis and extensive plaque involvement.
The reasons for the differences between specific coronary plaque compositions regarding the associated leukocyte subtypes are as yet unknown. Clinically, few studies have performed correlations of leukocyte subtypes with coronary plaque compositions assessed by coronary CT angiography. Kashiwagi et al. advocated it for the first time [12]. They found that an increased level of CD14+CD16+ monocyte subset, but not the total number of monocytes or CRP, is associated with the presence of non-calcified plaques in patients with stable angina pectoris. However, their study described entire CD14+CD16+ populations without referring to either intermediate CD14++CD16+ or non-classical CD14+CD16++ monocytes. Then Nilsson et al. further demonstrated that neutrophil counts are significantly correlated with non-calcified plaques in CAD patients [13]. Nonetheless, they did not measure monocyte subsets, but the lack of association between total number of monocytes, CRP and the presence of non-calcified plaques was also found in their study. By contrast, we found that the monocyte counts and its classical CD14++CD16− monocyte counts were also significantly associated with the non-calcified plaque score, but the correlation coefficients for these factors were lower than that for the neutrophil counts. Experimentally, both neutrophils and monocytes-derived macrophages are present in atherosclerotic plaque lesions [21]. In mice studies, neutrophils contribute to the recruitment of classical monocytes to the arterial wall [22], and neutrophil depletion leads to reduced monocyte/ macrophage counts within aortic wall [23]. Taking together, the previous studies and our data suggest that neutrophils could play a greater role than monocytes in the non-calcified plaque formation.
Our study shows, for the first time, that intermediate CD14++CD16+ monocytes correlated best with the mixed plaque and calcified plaque scores among the leukocyte subtypes. One assumption is that intermediate CD14++CD16+ monocytes promotes the plaque calcification. Indeed, increased numbers of CD14+CD16+ monocytes, including intermediate CD14++CD16+ and/or non-classical CD14+CD16++ subsets, are associated with the production of tumor necrosis factor (TNF)-alpha [24]. TNF-alpha is known as the potent pro-osteochondrogenic cytokine in vitro and contributes to vascular calcification and inflammation [25]. Additionally, CD14+ monocytes, including classical CD14++CD16− and/or intermediate CD14++CD16+ subsets, have a remarkable ability to change their phenotype in response to a wide range of stimuli, and these cells could form an osteogenic monocyte subset [26, 27]. Moreover, activated circulating CD14+ monocytes could induce the osteoblast differentiation of human mesenchymal stem cells and matrix mineralization [28]. These observations support the idea that intermediate CD14++CD16+ monocytes play a key role in the plaque calcification.
Another assumption is that intermediate CD14++CD16+ monocytes repairs the calcified plaques. Intermediate CD14++CD16+ monocytes are found at low frequency in blood, but they are reported to be a predominant type of monocytes expressing Tie-2 (an angiopoietin receptor) and vascular endothelial growth factor (VEGF) receptors, which has been implicated in angiogenesis and reparation [6]. In the advanced human atherosclerotic plaque, microvascular endothelium displays VEGF and angiopoietin 2 much more prominently than does that from early lesions [29]. Hence, the increased number of circulating CD14++CD16+ monocytes would appear to provide advanced plaques more angiogenesis or reparative process to overcome diffusion limitations on oxygen and nutrient supply. In summary, our findings correspond with those from previous studies suggesting that among the leukocyte subtypes, the intermediate CD14++CD16+ monocyte count might be useful for evaluating mixed or calcified plaque progression.
Among patients with any coronary plaque, we observed that an elevated CD14++CD16+ monocyte count may identify patients at increased risk for extensive plaque involvement or severe coronary stenosis. Of note, Ozaki et al. found that intermediate CD14++CD16+ monocytes activated more frequently than classical CD14++CD16− and non-classical CD14+CD16+ monocytes in patients with plaque rupture and thrombus formation assessed by frequency-domain optical coherence tomography [30]. Whether specific interventions to decrease CD14++CD16+ monocyte count could limit plaque extent and stenosis severity should be investigated. For example, recent studies showed that hypertriglyceridemia causes intermediate CD14++CD16+ monocytes adhere to vascular cell adhesion molecule-1 higher efficiency than other subsets, especially in patients with myocardial infarction [31, 32]. Furthermore, lower Apo AI and HDL-C levels are associated with higher intermediate CD14++CD16+ monocyte counts, which predict cardiovascular events in patients with chronic kidney disease [33]. Additionally, statins would not only reduce the plaque volume but also modulate the monocyte counts [34]. Treatment with simvastatin and atorvastatin reduces the proportion of CD16+ monocytes in peripheral blood mononuclear cells, especially intermediate CD14++CD16+ monocytes, in HIV-1-infected subjects [35]. Based on these findings and our study, in subjects with intermediate risk, any plaque, or a non-zero calcium score, an increase in intermediate CD14++CD16+ monocytes may prompt a clinician to prescribe statins or more intensive lifestyle modifications, such as dietary lipids or regular exercise.
There are several limitations to our study. First, we demonstrated that the relationship between leukocyte subtypes and coronary plaque type and stenosis is weak and very limited. Nevertheless, these data have been analyzed with a Bonferroni-adjusted p value, leading to very conservative results in most. Second, racial and ethnic differences may produce altered susceptibilities to various forms of CAD. Only ethnic Chinese individuals who attended voluntary cardiovascular health check-ups were enrolled. Whether our results are applicable to other racial populations is unclear, and a self-selective bias may have existed for subjects who voluntarily submitted to health check-ups. Another limitation is only using a basic flow cytometry gating strategy, we could have missed some CD16+ cells that scatter in the lymphocyte range. Finally, as this was a cross-sectional study, we could only analyze associations between coronary plaques and leukocyte subtypes at one-time point; we cannot draw any functional conclusions regarding these associations during the progression of atherosclerosis in individuals. Thus, our study does not provide a mechanistic explanation for the effects of specific monocyte subsets on the severity of CAD.
Conclusion
Intermediate CD14++CD16+ monocytes predicted the presence of extensive plaque involvement and severe coronary stenosis in asymptomatic individuals from the general population. Whether the intermediate monocyte subset could improve risk stratification needs further research.
References
Stone GW, Maehara A, Lansky AJ, de Bruyne B, Cristea E, Mintz GS, Mehran R, McPherson J, Farhat N, Marso SP, Parise H, Templin B, White R, Zhang Z, Serruys PW, PROSPECT Investigators (2011) A prospective natural-history study of coronary atherosclerosis. N Engl J Med 364:226–235
Madjid M, Awan I, Willerson JT, Casscells SW (2004) Leukocyte count and coronary heart disease: implications for risk assessment. J Am Coll Cardiol 44:1945–1956
Horne BD, Anderson JL, John JM, Weaver A, Bair TL, Jensen KR, Renlund DG, Muhlestein JB, Intermountain Heart Collaborative Study Group (2005) Which white blood cell subtypes predict increased cardiovascular risk? J Am Coll Cardiol 45:1638–1643
Guasti L, Dentali F, Castiglioni L, Maroni L, Marino F, Squizzato A, Ageno W, Gianni M, Gaudio G, Grandi AM, Cosentino M, Venco A (2011) Neutrophils and clinical outcomes in patients with acute coronary syndromes and/or cardiac revascularisation. A systematic review on more than 34,000 subjects. Thromb Haemost 106:591–599
Papa A, Emdin M, Passino C, Michelassi C, Battaglia D, Cocci F (2008) Predictive value of elevated neutrophil-lymphocyte ratio on cardiac mortality in patients with stable coronary artery disease. Clin Chim Acta 395:27–31
Zawada AM, Rogacev KS, Rotter B, Winter P, Marell RR, Fliser D, Heine GH (2011) SuperSAGE evidence for CD14++CD16+ monocytes as a third monocyte subset. Blood 118:e50–e61
Berg KE, Ljungcrantz I, Andersson L, Bryngelsson C, Hedblad B, Fredrikson GN, Nilsson J, Björkbacka H (2012) Elevated CD14++CD16– monocytes predict cardiovascular events. Circ Cardiovasc Genet 5:122–131
Rogacev KS, Cremers B, Zawada AM, Seiler S, Binder N, Ege P, Große-Dunker G, Heisel I, Hornof F, Jeken J, Rebling NM, Ulrich C, Scheller B, Böhm M, Fliser D, Heine GH (2012) CD14++CD16+ monocytes independently predict cardiovascular events: a cohort study of 951 patients referred for elective coronary angiography. J Am Coll Cardiol 60:1512–1520
ó Hartaigh B, Bosch JA, Thomas GN, Lord JM, Pilz S, Loerbroks A, Kleber ME, Grammer TB, Fischer JE, Boehm BO, März W (2012) Which leukocyte subsets predict cardiovascular mortality? From the Ludwigshafen risk and cardiovascular health (LURIC) Study. Atherosclerosis 224:161–169
Dragu R, Kerner A, Gruberg L, Rispler S, Lessick J, Ghersin E, Litmanovich D, Engel A, Beyar R, Roguin A (2008) Angiographically uncertain left main coronary artery narrowings: correlation with multidetector computed tomography and intravascular ultrasound. Int J Cardiovasc Imag 24:557–563
Min JK, Shaw LJ, Devereux RB, Okin PM, Weinsaft JW, Russo DJ, Lippolis NJ, Berman DS, Callister TQ (2007) Prognostic value of multidetector coronary computed tomographic angiography for prediction of all-cause mortality. J Am Coll Cardiol 50:1161–1170
Kashiwagi M, Imanishi T, Tsujioka H, Ikejima H, Kuroi A, Ozaki Y, Ishibashi K, Komukai K, Tanimoto T, Ino Y, Kitabata H, Hirata K, Akasaka T (2010) Association of monocyte subsets with vulnerability characteristics of coronary plaques as assessed by 64-slice multidetector computed tomography in patients with stable angina pectoris. Atherosclerosis 212:171–176
Nilsson L, Wieringa WG, Pundziute G, Gjerde M, Engvall J, Swahn E, Jonasson L (2014) Neutrophil/lymphocyte ratio is associated with non-calcified plaque burden in patients with coronary artery disease. PLoS ONE 9:e108183 doi:10.1371/journal.pone.0108183
Greenland P, Smith SC Jr, Grundy SM (2001) Improving coronary heart disease risk assessment in asymptomatic people: role of traditional risk factors and noninvasive cardiovascular tests. Circulation 104:1863–1867
Leipsic J, Abbara S, Achenbach S, Cury R, Earls JP, Mancini GJ, Nieman K, Pontone G, Raff GL (2014) SCCT guidelines for the interpretation and reporting of coronary CT angiography: a report of the society of cardiovascular computed tomography guidelines committee. J Cardiovasc Comput Tomogr 8:342–358
Hoffmann U, Moselewski F, Cury RC, Ferencik M, Jang IK, Diaz LJ, Abbara S, Brady TJ, Achenbach S (2004) Predictive value of 16-slice multidetector spiral computed tomography to detect significant obstructive coronary artery disease in patients at high risk for coronary artery disease patient-versus segment-based analysis. Circulation 110:2638–2643
Lee BC, Lee WJ, Hsu HC, Chien KL, Shih TT, Chen MF (2011) Using clinical cardiovascular risk scores to predict coronary artery plaque severity and stenosis detected by CT coronary angiography in asymptomatic Chinese subjects. Int J Cardiovasc Imag 27:669–678
Russo V, Zavalloni A, Bacchi Reggiani ML, Buttazzi K, Gostoli V, Bartolini S, Fattori R (2010) Incremental prognostic value of coronary CT angiography in patients with suspected coronary artery disease. Circ Cardiovasc Imag 3:351–359
Dettmer M, Glaser-Gallion N, Stolzmann P, Glaser-Gallion F, Fornaro J, Feuchtner G, Jochum W, Alkadhi H, Wildermuth S, Leschka S (2013) Quantification of coronary artery stenosis with high-resolution CT in comparison with histopathology in an ex vivo study. Eur J Radiol 82:264–269
Pundziute G, Schuijf JD, Jukema JW, Decramer I, Sarno G, Vanhoenacker PK, Reiber JH, Schalij MJ, Wijns W, Bax JJ (2008) Head-to-head comparison of coronary plaque evaluation between multislice computed tomography and intravascular ultrasound radiofrequency data analysis. JACC Cardiovasc Interv 1:176–182
Soehnlein O (2012) Multiple roles for neutrophils in atherosclerosis. Circ Res 110:875–888
Drechsler M, Megens RT, van Zandvoort M, Weber C, Soehnlein O (2010) Hyperlipidemia-triggered neutrophilia promotes early atherosclerosis. Circulation 122:1837–1845
Wantha S, Alard JE, Megens RT, van der Does AM, Döring Y, Drechsler M, Pham CT, Wang MW, Wang JM, Gallo RL, von Hundelshausen P, Lindbom L (2013) Neutrophil-derived cathelicidin promotes adhesion of classical monocytes. Circ Res 112:792–801
Schlitt A, Heine GH, Blankenberg S, Espinola-Klein C, Dopheide JF, Bickel C, Lackner KJ, Iz M, Meyer J, Darius H, Rupprecht HJ (2004) CD14+CD16+ monocytes in coronary artery disease and their relationship to serum TNF-alpha levels. Thromb Haemost 92:419–424
Tintut Y, Patel J, Territo M, Saini T, Parhami F, Demer LL (2002) Monocyte/macrophage regulation of vascular calcification in vitro. Circulation 105:650–655
Collin J, Gössl M, Matsuo Y, Cilluffo RR, Flammer AJ, Loeffler D, Lennon RJ, Simari RD, Spoon DB, Erbel R, Lerman LO, Khosla S, Lerman A (2015) Osteogenic monocytes within the coronary circulation and their association with plaque vulnerability in patients with early atherosclerosis. Int J Cardiol 181:57–64
Fadini GP, Albiero M, Menegazzo L, Boscaro E, Vigili de Kreutzenberg S, Agostini C, Cabrelle A, Binotto G, Rattazzi M, Bertacco E, Bertorelle R, Biasini L, Mion M, Plebani M, Ceolotto G, Angelini A, Castellani C, Menegolo M, Grego F, Dimmeler S, Seeger F, Zeiher A, Tiengo A, Avogaro A (2011) Widespread increase in myeloid calcifying cells contributes to ectopic vascular calcification in type 2 diabetes. Circ Res 108:1112–1121
Guihard P, Danger Y, Brounais B, David E, Brion R, Delecrin J, Richards CD, Chevalier S, Rédini F, Heymann D, Gascan H, Blanchard F (2012) Induction of osteogenesis in mesenchymal stem cells by activated monocytes/ macrophages depends on oncostatin M signaling. Stem Cells 30:762–772
Calvi C, Dentelli P, Pagano M, Rosso A, Pegoraro M, Giunti S, Garbarino G, Camussi G, Pegoraro L, Brizzi MF (2004) Angiopoietin 2 induces cell cycle arrest in endothelial cells: a possible mechanism involved in advanced plaque neovascularization. Arterioscler Thromb Vasc Biol 24:511–518
Ozaki Y, Imanishi T, Teraguchi I, Nishiguchi T, Orii M, Shiono Y, Shimamura K, Ishibashi K, Tanimoto T, Yamano T, Ino Y, Yamaguchi T, Kubo T, Akasaka T (2014) Association between P-selectin glycoprotein ligand-1 and pathogenesis in acute coronary syndrome assessed by optical coherence tomography. Atherosclerosis 233:697–703
Xue D, He X, Zhou C, Xu X, Xu R, Xu N (2013) Correlation between CD14+CD16++ monocytes in peripheral blood and hypertriglyceridemia after allograft renal transplantation. Transplant Proc 45:3279–3283
Foster GA, Gower RM, Stanhope KL, Havel PJ, Simon SI, Armstrong EJ (2013) On-chip phenotypic analysis of inflammatory monocytes in atherogenesis and myocardial infarction. Proc Natl Acad Sci USA 110:13944–13949
Rogacev KS, Zawada AM, Emrich I, Seiler S, Böhm M, Fliser D, Woollard KJ, Heine GH (2014) Lower apo A-I and lower HDL-C levels are associated with higher intermediate CD14++CD16+ monocyte counts that predict cardiovascular events in chronic kidney disease. Arterioscler Thromb Vasc Biol 34:2120–2127
Tani S, Nagao K, Anazawa T, Kawamata H, Furuya S, Takahashi H, Iida K, Matsumoto M, Washio T, Kumabe N, Hirayama A (2009) Association of leukocyte subtype counts with coronary atherosclerotic regression following pravastatin treatment. Am J Cardiol 104:464–469
Yadav A, Betts MR, Collman RG (2016) Statin modulation of monocyte phenotype and function: implications for HIV-1-associated neurocognitive disorders. J Neurovirol 22:584–596
Acknowledgements
This study was funded by the National Taiwan University Hospital (NTUH.100-S1611). The authors appreciate the help of the staff of the Health Management Center at National Taiwan University Hospital and thank Rong Ling Hung for her help in the flow cytometric analyses.
Funding
This study was funded by the National Taiwan University Hospital (NTUH.100-S1611).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lo, SC., Lee, WJ., Chen, CY. et al. Intermediate CD14++CD16+ monocyte predicts severe coronary stenosis and extensive plaque involvement in asymptomatic individuals. Int J Cardiovasc Imaging 33, 1223–1236 (2017). https://doi.org/10.1007/s10554-017-1097-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-017-1097-z