Abstract
The presence of activated macrophages is an important predictor of atherosclerotic plaque rupture. In this study, our aim was to determine the accuracy of 18F- fluorodeoxyglucose (FDG) microPET imaging for quantifying aortic wall macrophage content in a rabbit model of atherosclerosis. Rabbits were divided into a control group and two groups post aortic balloon injury: 6 months high-cholesterol diet (HC); and 3 months HC followed by 3 months low-cholesterol diet plus statin (LCS). In vivo and ex vivo microPET, ex vivo well counting and histological quantification of the atherosclerotic aortas were performed for all groups. Macrophage density was greater in the HC group than the LCS group (5.1 ± 1.4% vs. 0.6 ± 0.7%, P < 0.001) with a trend towards greater macrophage density in LCS compared to controls (P = 0.08). There was a strong correlation across all groups between macrophage density and standardized uptake value (SUV) derived from ex vivo microPET (r = 0.95, P < 0.001) and well counting (r = 0.96, P < 0.001). Ex vivo FDG SUV was significantly different between the three groups (P < 0.001). However, the correlation between in vivo microPET FDG SUV and macrophage density was insignificant (r = 0.16, P = 0.57) with no statistical differences in FDG SUV seen between the three groups. This study confirms that in an animal model of inflamed and non-inflamed atherosclerosis, significant differences in FDG SUV allow differentiation of highly inflamed atherosclerotic aortas from those stabilized by statin therapy and low cholesterol diet and controls.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
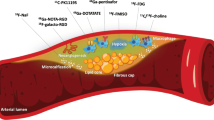
The presence of inflammatory cells, particularly macrophages, in the intimal layer of the arterial wall is a cardinal feature of the vulnerable atherosclerotic plaque [1]. These plaques can rupture and cause clinical events such as unstable angina, myocardial infarction, and stroke [2]. X-ray angiography remains the gold standard imaging modality for assessing atherosclerotic lesions in clinical practice. Although it is an excellent tool for measuring luminal narrowing, it does not provide any information regarding the plaque composition and hence its ability to identify vulnerable plaque and future clinical events is limited. For this reason, alternative imaging techniques are currently being tested, one of the more promising of which is 18F-fluorodeoxyglucose (FDG) positron emission tomography (PET).
18F-fluorodeoxyglucose (FDG) is a glucose analogue that can be non-invasively imaged using PET. Increased FDG uptake in the atherosclerotic artery wall has been shown in man [3–11] and animal imaging studies suggest that plaque macrophages account for most of the FDG uptake [12–16]. For drug efficacy tracking, reproducibility is excellent [17–19] and one study has suggested that FDG uptake could be used to monitor the effects of treatment on plaque macrophage content in vivo [14].
In the present study, dietary manipulation and statin therapy were used to modify plaque macrophage content in a rabbit model of atherosclerosis to determine how accurately FDG uptake quantifies plaque macrophage content. We compared the quantitative accuracy of in vivo small animal PET to both ex vivo PET and gamma well counting, and examined the correlations between each of these methods and plaque histology.
Materials and methods
Animals
Fifteen male New Zealand White (NZW) rabbits weighing 3.4 ± 0.4 kg (mean ± SD; Harlan UK Limited, Bicester, UK) were used for the study which was conducted according to UK Home Office animal welfare guidelines.
The rabbits in the control group (n = 3) were kept on a normal diet for 6 months prior to FDG studies. The non-control rabbits (n = 12) were fed a high cholesterol diet (SDS Diets Services, Essex, UK) consisting of 0.5% cholesterol and 12% peanut oil. 2 weeks after the start of cholesterol feeding all non-control rabbits underwent aortic balloon injury, to facilitate and target the rapid development of atheromatous lesions [20]. The right femoral artery was isolated and a 4F Fogarty embolectomy catheter (Edwards Life Sciences) was introduced via an arteriotomy and advanced 20 cm proximally, equating approximately to the level of the diaphragm. A balloon mounted at the tip of the catheter was then inflated with 2 ml of air, following which the catheter was dragged back to the iliac bifurcation. Cholesterol diet was then maintained in all non-control rabbits for a total of 3 months to encourage the development of macrophage-rich lesions. After 3 months half of the non-control rabbits were returned to a normal diet for 3 months. To ensure maximal resolution of plaque inflammation, the cholesterol-lowering drug, atorvastatin (10 mg/kg/day), was also added to their feed. This rabbit group is henceforth referred to as the LCS group (low cholesterol plus statin). The other non-control rabbits (HC group) were further maintained on the high cholesterol diet for 6 months after balloon injury to ensure a high plaque macrophage content.
PET
The 15 rabbits were imaged with a microPET scanner (Concorde microPET P4, Concorde Microsystems, Knoxville, TN, USA). Once anaesthetized, the rabbits were positioned on the scanning bed with the infra-diaphragmatic aorta in the centre of the field of view. Transmission scans were carried out using a rotating germanium-68 point source for attenuation correction. FDG (150 ± 5.6 MBq, mean ± SD) was injected through an intravenous cannula using a mechanical pump over 1 min. A dynamic 3D emission scan was performed for each rabbit over 110 min (1 × 20, 2 × 15, 8 × 30, 5 × 60, 15 × 120, and 14 × 300 s). Arterial blood samples were taken from a cannula sited in the central ear artery at specified time points during the emission scan. The radioactivity in each plasma sample was then counted in a calibrated scintillation well counter (Harwell Instruments, Didcot, Oxfordshire).
After 110 min of imaging the whole aorta was carefully excised. Surrounding connective tissue was removed and the aorta was then pinned onto a corkboard and replaced in the microPET scanner for ex vivo imaging. This consisted of both emission (15 min) and transmission (11 min) scans.
All PET images were reconstructed using PROMIS 3D filtered backprojection [21] into 0.5 × 0.5 × 0.5 mm voxels. PET data were corrected for randoms, dead time, normalization, attenuation, sensitivity and decay.
Quantification of PET data
Quantification of FDG concentration in the PET images was carried out using the software package Analyze (Biomedical Imaging Resource, Mayo Foundation, USA) by a blinded observer (DI).
For in vivo images, as anatomical imaging was not available both a circular region of interest (ROI) (for the lumen) and an annular ROI (for the aortic wall) were drawn on each transaxial slice of the early blood-pool images (35–80 s after FDG injection) throughout the infra-diaphragmatic aorta. The size of the lumen and aortic wall ROIs was estimated from histological sections of the same animal. Aortic wall time activity curves were calculated for each rabbit.
For ex vivo image analysis, a ROI was placed over the sub-diaphragmatic aorta from the coeliac trunk to the iliac bifurcation. The mean activity concentration in the ROI was then multiplied by the volume of the ROI to give the total activity. Next, total activity was divided by the actual volume of tissue calculated from the weight of the tissue sample, to give a partial volume corrected activity concentration for the balloon injured section of aorta.
Mean standardized uptake values (SUV) were determined by dividing the relevant ROI concentration by the ratio of the injected activity to the body weight. Maximum SUV values were also determined for in vivo microPET. SUV was compared to ROI concentration normalized to the integral of the plasma input function, which we refer to as normalized uptake rate (NUR). For in vivo imaging, SUV and NUR were determined using images acquired between 95 and 110 min post-injection. In addition, for in vivo microPET, Patlak analysis [22] was used on data acquired from 30–110 min post-injection to calculate the FDG influx rate K i .
Ex vivo well counting
Following ex vivo imaging, each aorta was cut transversely into 5 mm segments. Each segment was weighed and the radioactivity in each segment was counted in a gamma well counter (Harwell Instruments, Didcot, Oxfordshire). As above, well counter radioactivity concentration was converted to SUV and NUR.
Histology
After ex vivo well counting, each aorta segment was fixed in formalin followed by a rinse with phosphate buffered saline (PBS). Macrophage and vascular smooth muscle cell (VSMC) densities were calculated by a blinded observer (NF) for each segment by taking three 5 μm sections and double staining for macrophages (RAM 11, Dako) and VSMCs (α actin, Dako). Digital photographs of all immunostained sections were taken using a Nikon digital microscope and the software package, analySIS (Soft Imaging System Ltd, Yorkshire, UK). A color threshold method was employed to estimate the area of macrophage and VSMC positive staining on each section as a percentage of its total area [23]. For each rabbit in the LCS and HC groups, mean macrophage and VSMC density were calculated for the balloon-injured section of aorta. For each rabbit in the control group, mean densities were calculated for the infradiaphragmatic aorta.
Statistical methods
Differences in FDG uptake (SUV, NUR and K i ), macrophage density and VSMC density between the three groups of rabbits were assessed using one-way ANOVA. The strength of correlation between macrophage or VSMC density and ex vivo and in vivo FDG uptake was tested using the Spearman method. P values of <0.05 were considered significant. All calculations were performed using SPSS version 14.0.
Results
Histology
Figure 1 presents the histological data across the three groups. All rabbits in the control group had normal aortic wall with no measurable macrophages. Histology from both the LCS and HC groups confirmed the presence of intimal expansion and hyperplasia affecting the balloon-injured segment of the aorta in all rabbits (Fig. 2). Immunocytochemical evaluation revealed both macrophages and VSMCs within the aortic wall in the balloon-injured segments. However, compared to the LCS group, the rabbits in the HC group had a significantly higher mean macrophage density, (5.1 ± 1.4% vs. 0.6 ± 0.7%, P < 0.001), a lower mean VSMC density (30.4 ± 5.9% vs. 47.4 ± 9.7%, P = 0.001), confirming a morphological difference between the walls in the LCS and HC groups (Fig. 2). No statistical difference was found between VSMC density in LCS and control groups (P = 0.28). The difference between macrophage density in LCS and control groups just failed to reach statistical significance (P = 0.08).
Ex vivo imaging and well counting
Table 1 shows a summary of all the uptake parameters. There are significant differences in FDG uptake values between control, LSC and HC groups for ex vivo microPET and well counting (P = 0.001 and <0.001, respectively).
Figure 2 shows the typical difference in aortic FDG SUV from rabbits in the LCS and HC groups and Fig. 3 shows the variation in FDG uptake and histology along the aorta for a rabbit from the HC group.
Excised aorta and corresponding ex vivo microPET image from one of the rabbits in the HC group. On the right hand side of the figure histological sections from different segments of the aorta are shown for comparison. Note that high and low FDG uptake corresponds to high and low macrophage density, respectively
Figure 4 illustrates the strong correlation noted between ex vivo microPET aortic wall FDG SUV and macrophage density (r = 0.95, P < 0.001). There was also a strong correlation between macrophage density and ex vivo microPET aortic wall FDG NUR (r = 0.92, P < 0.001), and both well counting FDG SUV (r = 0.96, P < 0.001) and FDG NUR (r = 0.95, P < 0.001). SUV and NUR determined by ex vivo microPET and well counting were highly correlated (r = 0.97, P < 0.001 and r = 0.97, P < 0.001, respectively) as indicated in Fig. 5 for SUV, and SUV and NUR were also strongly correlated (r = 0.99, P < 0.001). A significant negative correlation was found between VSMC density and FDG SUV across all groups determined from both ex vivo microPET (r = −0.82, P < 0.001) and well counting (r = −0.83, P < 0.001). Similar correlation values were found for NUR.
In vivo imaging
Examples of in vivo microPET FDG scans from the 3 rabbit groups are shown in Fig. 6. Figure 7 shows the mean aortic FDG SUV in the three groups. Despite the statistically significant differences in mean FDG uptake in ex vivo imaging, no significant differences were found when mean FDG SUV was calculated from in vivo microPET (1.25 ± 0.02 vs. 1.54 ± 0.29 vs. 1.45 ± 0.24 for control, LCS and HC groups respectively, P = 0.27). There were also no inter-group differences found for NUR, nor for group means calculated from maximum values of SUV and NUR. This did not change when Patlak analysis was used to calculate K i in the three groups of rabbits (mean K i for control, LCS and HC groups were 1.9, 2.5, and 1.9 × 10−3, respectively, P = 0.43). As a consequence the correlation between in vivo FDG SUV and macrophage density was poor (r = 0.16, P = 0.57). Table 1 shows a summary of the in vivo microPET data.
Discussion
We have demonstrated increased FDG uptake in the atherosclerotic aortic wall of this experimental model compared to controls. This was confirmed by two different methods of quantification: ex vivo microPET and scintillation well counting. These results substantiate those found in other rabbit atherosclerosis PET studies [13–16]. Additionally, we noted that withdrawal of high cholesterol feeding combined with the administration of a statin reduced FDG uptake to near control levels, despite the presence of substantial fibrous intimal thickening.
18F-fluorodeoxyglucose (FDG) uptake was strongly positively correlated with the degree of macrophage infiltration in the vessel wall. Conversely, there was a negative association between FDG uptake measures and VSMC density, not previously shown in a rabbit model. These correlations indicate that high FDG uptake is associated with a high degree of macrophage infiltration and low VSMC density. These data support the notion that FDG uptake into the arterial wall is likely attributable to accumulation within plaque macrophages, as it has already been shown that FDG accumulates within macrophages more avidly than within other plaque elements [7].
The ex vivo results showed significantly higher FDG uptake in the group of rabbits with highly inflamed aortic atheroma (HC group) compared with controls and also that FDG can distinguish highly inflamed plaques (HC group) from those with lower levels of inflammation (LCS group).
We have demonstrated that microPET can replace well counting for quantification of FDG uptake in the ex vivo aorta. MicroPET has the advantage of higher spatial sampling and hence can more accurately quantify local FDG uptake. In addition, in this study we have used a quantification method NUR, which in theory should provide a more accurate measure of FDG metabolism than SUV as it more accurately normalizes for the delivery of FDG to the tissue. However unlike SUV, it requires the measurement of the plasma input function. The tight correlation found between SUV and NUR (r = 0.99) indicates than NUR can be replaced by SUV with no loss of accuracy. However, blood sampling does allow the calculation of influx rate (K i ), an even more accurate measure of FDG metabolism than NUR. Calculation of K i requires dynamic imaging and therefore is only applicable to in vivo imaging.
In vivo quantification of FDG uptake using the microPET scanner did not mirror the results of our ex vivo study. Uptake measures (SUV, NUR and K i ) did not correlate with the degree of aortic wall macrophage infiltration, and there was no significant difference in FDG uptake seen between the rabbits with highly inflamed aortic wall, those with a low level of inflammation or controls. The reasons for this lie in the limitations of the in vivo data acquisition and analysis. When compared with ex vivo PET, in vivo PET of the aortic wall is subject to a number of limitations: contamination of the wall signal by activity in blood and surrounding tissues, and loss of wall signal (partial volume error); inaccuracy in delineating the vessel wall; higher level of noise which is accentuated by high attenuation correction factors; systematic errors due to scatter and inaccuracies in the attenuation correction; motion of the animal.
The partial volume error will reduce the range of the observed FDG uptake; highly inflamed aortic wall uptake will be reduced and uptake in aortic wall with low inflammation will be increased. To reduce partial volume error, Tawakol et al. [15]. Calculated FDG uptake at 3 h post injection. The slow excretion component of the blood time-activity curves measured in this study had an average half life of 101.2 ± 7.7 min, and hence we estimate that if the data in our study had been acquired at 3 h post injection rather than 2 h, spill-over of signal from the lumen into the aortic wall would have been reduced by approximately 34%. Ideally, rather than delayed acquisition, partial volume error should be reduced using post-acquisition image processing, the feasibility of which has been demonstrated for human atheroma imaging by our group [17]. However, as this method requires accurate ROI placement, the lack of anatomical imaging precluded its use in our current study.
Both CT [13–15] and MR [16] have been used to provide anatomical information in rabbit PET studies for atherosclerosis. In contrast to our in vivo results, two of these studies [15, 16] showed statistically significant correlation between in vivo FDG uptake and macrophage content. The study of Zhang et al. [16]. Used a similar rabbit model to the one used in this study and also a comparable post-injection PET imaging time. Hence, their superior results may be attributed to the availability of anatomical imaging.
The results of Tawakol et al. [15]. In comparison to those of Zhang et al. [16]. Indicate that acquiring data later after injection and reducing blood FDG concentration through glucose administration also improves the in vivo quantification of macrophage content using FDG PET.
Conclusion
This study adds to the evidence that FDG is a suitable tracer for identifying inflammation within atherosclerotic plaque. Our ex vivo results indicate that increased FDG uptake in the atherosclerotic vessel wall can be attributed to macrophage infiltration and that FDG is able to resolve highly inflamed atherosclerotic plaques from those with a low level of inflammation. We have demonstrated that a quantification method that relies on blood sampling (NUR) can be replaced by a method (SUV) that normalizes uptake using only injected activity and weight. Accurate quantification in vivo from PET alone is problematic, especially when the size of the vessel wall is small, such as in the experimental model used in this study.
References
Virmani R, Burke AP, Farb A, Kolodgie FD (2006) Pathology of the vulnerable plaque. J Am Coll Cardiol 47:C13–C18
Davies MJ, Thomas AC (1985) Plaque fissuring—the cause of acute myocardial infarction, sudden ischaemic death, and crescendo angina. Br Heart J 53:363–373
Ben-Haim S, Kupzov E, Tamir A, Israel O (2004) Evaluation of 18F-FDG uptake and arterial wall calcifications using 18F-FDG PET/CT. J Nucl Med 45:1816–1821
Rudd JHF, Warburton EA, Fryer TD, Jones HA, Clark JC, Antoun N, Johnstrom P, Davenport AP, Kirkpatrick PJ, Arch BN, Pickard JD, Weissberg PL (2002) Imaging atherosclerotic plaque inflammation with 18F-fluorodeoxyglucose positron emission tomography. Circulation 105:2708–2711
Davies JR, Rudd JHF, Fryer TD, Graves MJ, Clark JC, Kirkpatrick PJ, Gillard JH, Warburton EA, Weissberg PL (2005) Identification of culprit lesions after transient ischemic attack by combined 18F-fluorodeoxyglucose positron-emission tomography and high-resolution magnetic resonance imaging. Stroke 36:2642–2647
Okane K, Ibaraki M, Toyoshima H, Sugawara S, Takahashi K, Miura S, Shimosegawa E, Kitamur J, Satoh T (2006) 18F-FDG accumulation in atherosclerosis: use of CT and MR co-registration of thoracic and carotid arteries. Eur J Nucl Med Mol Imaging 33:589–594
Tawakol A, Migrino RQ, Bashian GG, Bedri S, Vermylen D, Cury RC, Yates D, LaMuraglia GM, Furie K, Houser S, Gewirtz H, Muller JE, Brady TJ, Fischman AJ (2006) In vivo 18F-Fluorodeoxyglucose positron emission tomography imaging provides a noninvasive measure of carotid plaque inflammation in patients. J Am Coll Cardiol 48:1818–1824
Dunphy MP, Schoder H, Strauss HW (2007) Radionuclide techniques for identifying vulnerable plaque. J Nucl Med 48:1753–1755
Dunphy MP, Freiman A, Larson SM, Strauss HW (2005) Association of vascular 18F-FDG uptake with vascular calcification. J Nucl Med 46:1278–1284
Silvera SS, Aidi HE, Rudd JH, Mani V, Yang L, Farkouh M, Fuster V, Fayad ZA (2009) Multimodality imaging of atherosclerotic plaque activity and composition using FDG-PET/CT and MRI in carotid and femoral arteries. Atherosclerosis. doi:10.1016/j.atherosclerosis.2009.04.023
Rudd JH, Hyafil F, Fayad ZA (2009) Inflammation imaging in atherosclerosis. Arterioscler Thromb Vasc Biol 29:1009–1016
Lederman RJ, Raylman RR, Fisher SJ, Kison PV, San H, Nabel EG, Wahl RL (2001) Detection of atherosclerosis using a novel positron-sensitive probe and 18-fluorodeoxyglucose (FDG). Nucl Med Commun 22:747–753
Ogawa M, Ishino S, Mukai T, Asano D, Teramoto N, Watabe H, Kudomi N, Shiomi M, Magata Y, Iida H, Saji H (2004) 18F-FDG accumulation in athorosclerotic plaques: immunohistochemical and PET imaging study. J Nucl Med 45:1245–1250
Ogawa M, Magata Y, Kato T, Hatano K, Ishino S, Mukai T, Shiomi M, Ito K, Saji H (2006) Application of 18F-FDG PET for monitoring the therapeutic effect of antiiflammatory drugs on stabilization of vulnerable atherosclerotic plaques. J Nucl Med 47:1845–1850
Tawakol A, Migrino RQ, Hoffmann U, Abbara S, Houser S, Gewirtz H, Muller JE, Brady TJ, Fischman AJ (2005) Noninvasive in vivo measurement of vascular inflammation with F-18 fluorodeoxyglucose positron emission tomography. J Nucl Cardiol 12:294–301
Zhang Z, Machac J, Helft G, Worthley SG, Tang C, Zaman AG, Rodriguez OJ, Buchsbaum MS, Fuster V, Badimon JJ (2006) Non-invasive imaging of atherosclerotic plaque macrophage in a rabbit model with F-18 FDG PET: a histopathological correlation. BMC Nucl Med 6:4
Izquierdo-Garcia D, Davies JR, Graves MJ, Rudd JH, Gillard JH, Weissberg PL, Fryer TD, Warburton EA (2009) Comparison of methods for magnetic resonance-guided [18-F]fluorodeoxyglucose positron emission tomography in human carotid arteries. Reproducibility, partial volume correction, and correlation between methods. Stroke 40:86–93
Rudd JH, Myers KS, Bansilal S, Machac J, Pinto CA, Tong C, Rafique A, Hargeaves R, Farkouh M, Fuster V, Fayad ZA (2008) Atherosclerosis inflammation imaging with 18F-FDG PET: carotid, iliac, and femoral uptake reproducibility, quantification methods, and recommendations. J Nucl Med 49:871–878
Rudd JH, Myers KS, Bansilal S, Machac J, Rafique A, Farkouh M, Fuster V, Fayad ZA (2007) 18Fluorodeoxyglucose positron emission tomography imaging of atherosclerotic plaque inflammation is highly reproducible: implications for atherosclerosis therapy trials. J Am Coll Cardiol 50:892–896
Fischman AJ, Lees AM, Lees RS, Barlai-Kovach M, Strauss HW (1987) Accumulation of native and methylated low density lipoproteins by healing rabbit arterial wall. Arteriosclerosis 7:361–366
Kinahan PE, Rogers JG (1989) Analytic 3D image reconstruction using all detected events. IEEE Trans Nucl Sci 36:964–968
Patlak CS, Blasberg RG (1985) Graphical evaluation of blood-to-brain transfer constants from multiple-time uptake data. Generalizations. J Cereb Blood Flow Metab 5:584–590
Lehr HA, van der Loos CM, Teeling P, Gown AM (1999) Complete chromogen separation and analysis in double immunohistochemical stains using Photoshop-based image analysis. J Histochem Cytochem 47:119–126
Acknowledgments
This study was funded by programme grants from the British Heart Foundation. JRD, DI-G, JHFR, JLEB, APD, and PLW are all supported by grants from the British Heart Foundation (FG/03/013 and PS/02/001). EAW receives support from the Cambridge Biomedical Research Centre grant (NIHR). This work was also supported by an equipment grant (microPET) from the HEFCE and Merck Sharp and Dohme, Ltd. We would like to acknowledge the Wolfson Brain Imaging Centre radiochemistry staff for supplying the FDG.
Author information
Authors and Affiliations
Corresponding author
Additional information
The authors John R. Davies and David Izquierdo-Garcia have contributed equally to the study.
Rights and permissions
About this article
Cite this article
Davies, J.R., Izquierdo-Garcia, D., Rudd, J.H.F. et al. FDG–PET can distinguish inflamed from non-inflamed plaque in an animal model of atherosclerosis. Int J Cardiovasc Imaging 26, 41–48 (2010). https://doi.org/10.1007/s10554-009-9506-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-009-9506-6