Abstract
The correlation between right ventricular ejection fraction (RVEF) and tricuspid annular plane systolic excursion (TAPSE) by two-dimensional (2-D) echo has been repeatedly validated, but not by magnetic resonance imaging (MRI) nor in patients with congenital heart disease. We tested whether TAPSE measurements by MRI correlate with RVEF in surgically repaired tetralogy of Fallot (TOF) patients. TAPSE was measured from systolic displacement of the RV-freewall/tricuspid annular plane junction in the apical 4-chamber view in 7 normal subjects and 14 TOF patients. The RV was reconstructed in 3-D from manually traced borders on MR images to compute true EF. Because we previously observed discrepancy between TAPSE and RVEF in the presence of regional dysfunction, we also analyzed RV wall motion in terms of regional stroke volume at 20 short axis slices from apex to tricuspid annulus. RVEF was 52 ± 3% in normal subjects and 41 ± 9% in TOF (P < 0.01). TAPSE correlated weakly (r = 0.50, P < 0.05) with RVEF. TOF patients exhibited increased regional stroke volume from apical portions of the RV and decreased regional stroke volume at the base compared to normal (P < 0.05 at 15 of 20 slices). Regional stroke volume in apical slices correlated inversely with RVEF such that patients with higher apical stroke volume had lower RVEF (P < 0.05). TAPSE is not a reliable measure of RVEF in TOF by MRI. TAPSE may be of limited use in conditions that exhibit abnormal regional contraction.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Evaluation of right ventricular (RV) function through cost efficient two-dimensional (2-D) imaging has been a long-standing challenge in clinical medicine. The complex shape of the RV has precluded accurate estimation of RV volume by 2-D echocardiography using geometric models [1, 2]. More accurate imaging alternatives have been too expensive, time consuming, or invasive for regular clinical use. Consequently, current clinical practice is to comment on RV size as normal or moderately or severely enlarged and to visually assess RV function [3]. These imprecise readings are of limited use in patients where more subtle changes in RV function may significantly alter clinical management regarding use of medications, mechanical ventilation, or surgery [4]. Two-D echocardiographic techniques for estimating RV ejection fraction (EF), chiefly measurement of tricuspid annular plane systolic excursion (TAPSE), have been studied with results demonstrating correlation between TAPSE and RVEF in normal subjects and in patients with coronary artery disease or cardiomyopathy [5, 6]. There is limited study, however, as to the impact of variant RV anatomy on TAPSE [7].
Tetralogy of Fallot (TOF) is the most common cause of cyanotic congenital heart disease and is associated with a high prevalence of pulmonary regurgitation following repair often requiring later pulmonary valve replacement [8–10]. Monitoring RV volume and function is useful for managing these patients. Therefore the present study evaluated the accuracy with which TAPSE by MRI correlates with RVEF in surgically repaired TOF patients.
Methods
Patient population
We studied 14 patients with repaired TOF with wide-open pulmonary regurgitation who underwent MRI for patient care at their institutions. Three patients were studied at the University of Washington (UW), and 11 patients were studied at Texas Children’s Hospital, Houston. All were selected solely by diagnosis without regard to age, clinical history, or severity of pulmonary regurgitation. For comparison, seven normal subjects were imaged by MRI: one at the University of Washington and six at Oregon Health & Science University. All normal subjects reported no history of heart disease or symptoms and demonstrated normal physical exams and electrocardiograms (ECGs). This study was approved by the Human Subjects committee of the UW and all subjects gave informed consent.
MRI imaging
MRI scanning was performed using steady state free procession cine gradient echo sequences, appropriate for the hardware available at each institution. At Texas Children’s Hospital, a Philips 1.5 T NT-Intera scanner (Philips Medical System, Best, The Netherlands) was used with either a five-element phased-array cardiac coil or a standard four-element phased-array body coil. At the University of Washington images were acquired on a 1.5 T Philips Intera system (Philips Medical System, Best, The Netherlands) using a five-element phased-array cardiac coil. MRI at Oregon Health & Science University was performed using a 3 T Intera scanner (Philips Medical Systems) with a phased-array torso coil.
Depending on the system, TR ranged from 3.1 to 3.8 ms, TE ranged from 1.6 to 1.9 ms and a flip angle of 50–60° was used. A total of 8–12 consecutive short axis slices covering both LV and RV were acquired with 6–10 mm slice thickness, 30–50 cm field-of-view depending on patient size, and matrix sizes ranging from 224 × 160 to 256 × 192. In addition long axis slices were obtained in 4-chamber orientation. Additional long axis slices were obtained in some cases to aid in delineating the pulmonary valve for 3D reconstruction of the RV. A parallel imaging technique, sensitivity encoding with an acceleration factor of 2, was employed when possible. Temporal resolution was 30–40 ms acquired in a 3–13 s breath-hold per slice. The MRI data were submitted to the UW for core laboratory analysis using custom software [11].
TAPSE analysis by MRI
TAPSE was measured by marking the junction of RV free wall and tricuspid annulus in the apical 4-chamber view (Fig. 1) [12, 13]. The junction points were converted to 3-D coordinates using image plane location information in the DICOM file. TAPSE was calculated as the 3-D distance between the junction point at end diastole (ED) and end systole (ES).
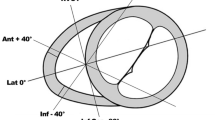
Basal view of traced borders of the right (elongated) and left ventricles (round). The 4-chamber view (black line) was the view that visualized the ventricular apex, crossed the middle of the mitral and tricuspid valves, and crossed the angle of the right ventricular free wall. The aortic and pulmonary valve orifices are also reconstructed
Image analysis for 3D RV reconstruction
True RV volume was measured from 3D reconstructions of the RV. The MRI studies were reviewed and the end systolic (ES) image frames were manually chosen. Global end systole was defined as the most frequently occurring systolic interval and applied to all cardiac cycles. Using custom software [14] the borders of the ventricles and valve orifices and other anatomical landmarks were manually traced and converted to 3D coordinates using MRI image plane coordinates. The papillary muscles and trabeculae were included in the chamber volume to obtain smooth endocardial contours suitable for shape analysis. The tricuspid and mitral annuli were reconstructed in 3D using Fourier series approximations [15]. Points traced from the semilunar valves were fitted to a circle. The RV was reconstructed using the piecewise smooth subdivision surface method, which provides anatomically accurate representation of the 3D shape of a heart ventricle (Fig. 2) [11, 16]. Ventricular volume was computed as the sum of signed volumes of tetrahedra formed by connecting a point in space with each face. The magnitude of intra-observer variability in manually tracing mitral annulus points was 2.2 ± 1.1 mm (n = 83 points). The magnitude of inter observer variability was 2.0 ± 1.3 mm (n = 233 points) [17]. The interobserver variability in measuring left ventricular end diastolic volume is 6.4% (n = 7, standard deviation of the difference expressed as percent of mean) [18]. It takes 2–5 h to trace a 3-D MRI study of the RV or left ventricle (LV) including time for immediate 3-D review of each traced border for compatibility with previously traced borders, checking especially for contact where image planes intersect and for concordance between similar views. This spatial border examination facilitates verification of image planes and border tracing consistency.
Regional function analysis
To measure regional RV function we divided the RV from apex to tricuspid annulus into 20 evenly spaced slices perpendicular to the LV long axis, which was constructed from the centroid of the 3-D reconstruction of the mitral annulus to the most distant point on the LV endocardial surface. The volume of each slice was computed as the product of the area of the slice by the height (Fig. 3). The stroke volume of a slice was determined as the difference between its end diastolic (ED) and ES volumes. Regional RV function was then computed in terms of the percent contribution of each slice to global stroke volume.
Comparison of 2D echocardiogram and MRI
The accuracy of TAPSE measurement from MRI was assessed in 7 subjects who underwent echocardiography on the same day as MRI using freehand 3-D technique as part of another study. Briefly, transthoracic 2-D echocardiograms were acquired using a Terason3000 ultrasound machine (Teracorp, Burlington, MA). During each scan the position and orientation of the transducer were recorded using a magnetic field tracking system (Flock of Birds, Ascension Technology Corp, Burlington, VT). The images and tracking data were stored in linked files on a personal computer to permit off-line 3-D analysis using custom software [14, 15]. Patients were imaged in the left lateral decubitus position on a nonferrous bed during held end-expiration for acquisition of 25 to 36 6-s scans obtained from multiple acoustic windows.
The images were analyzed as for MRI. The borders of the RV, LV, and associated structures were manually traced in multiple views. The location of the 4-chamber view relative to the RV and LV in the echocardiographic data set was compared to the location of this view in the MRI data set to confirm that TAPSE was being measured in the same anatomic location by both modalities (Fig. 1). In addition tricuspid valve leaflet position in the ED and ES frames was compared to verify that TAPSE was measured at the same time points in the cardiac cycle by both modalities.
We did not measure TAPSE by M-mode echo because it only visualizes tricuspid motion in a single 2-D plane.
Statistical analysis
The correlation between TAPSE and RVEF was analyzed using linear regression. The relationship between regional RV function and RVEF was also evaluated using linear regression. Differences between normal subjects and TOF patients were evaluated by t-test. Agreement between echo and MRI measurements of TAPSE was assessed by paired t-test and linear regression analysis.
Results
Patient population
The normal subjects and TOF patients differed in demographics and in RV and LV volume and function (Table 1).
Correlation of TAPSE with RVEF
TAPSE correlated weakly with RVEF (r = 0.50, P < 0.05, Fig. 4). The average value for TAPSE in normal subjects was 24 ± 2 mm, consistent with prior reports [13, 19].
Regional function analysis
Quantitative RV wall motion analysis demonstrated a significant difference in regional contractile patterns with TOF patients exhibiting a higher contribution to global stroke volume from the apical region (P < 0.05 in slices 1–8) compared with normal subjects. TOF patients also had a lower contribution from the basal region (P < 0.05 in slices 14–20). The stroke volume contribution from apical slices 4–7 correlated significantly with RVEF in an inverse relationship such that patients with higher apical contributions had lower RVEF. Conversely, the stroke volume contribution from basal slices 17–19 correlated directly with RVEF (P < 0.05). On multivariate regression analysis, however, TAPSE was a stronger correlate of RVEF than wall motion in any slice (Fig. 5).
Regional function in normal subjects (open squares) and patients with tetralogy of Fallot (closed diamonds) at 20 slices spanning the length of the right ventricle. Regional stroke volume contribution was greater than normal along apical slices and base, but the converse was seen near the base (asterisk, P < 0.05). Crosses indicate slices whose regional function correlated significantly with right ventricular ejection fraction
Agreement of TAPSE between echocardiogram and MRI
The 2D echocardiogram and MRI measurements of TAPSE were similar (17.4 ± 3.1 vs. 17.9 ± 3.3 mm, respectively, P = NS) and agreed with each other (correlation coefficient r = 0.948, P = 0.001, N = 7). The mean difference in TAPSE between imaging modalities was 0.5 ± 1.0 mm.
Discussion
There is great clinical need for non-invasive, economical methods to assess RV systolic function [20]. TAPSE has been shown to correlate highly with RV ejection fraction in normal subjects and patients with ischemic heart disease [5]. The correlation was weaker in patients with ischemic or idiopathic dilated cardiomyopathy [6]. The present observational study demonstrated a much weaker relationship between TAPSE and RVEF measured by MRI in TOF patients. The most likely reason is the altered regional contraction pattern in this population. These results confirm our previous study demonstrating that the relationship between TAPSE and RVEF fails in the presence of regional dysfunction [18].
The altered regional contraction pattern observed in the TOF patients may be attributable to altered muscle fiber orientation. Sanchez-Quintana et al. have reported that TOF patients have a middle layer of circumferential fibers in their RVs that is not present in normal RVs [21]. Such a middle layer is normally present in the LV and contains circumferential fibers that act to reduce ventricular diameter [22]. There is an anatomic correspondence between the increased function in the apical slices observed in the present study and alterations in regional RV shape that we have recently reported [23]. We did not analyze muscle fiber orientation in the present study population. Nevertheless the middle muscle layer could explain both the functional and shape alterations.
Methods for quantitative analysis of 3-D RV wall motion are few. In four studies of normal subjects, arrhythmogenic RV dysplasia, or congenital heart disease, the RV was divided into four circumferential regions, three vertical regions, or 9–12 regions created by subdividing short axis slices [24–27]. The present study presents a simple method for gauging regional RV function. We utilized short axis slices to measure regional function along the RV long axis. However, regional stroke volume could easily be measured in RV subdivisions defined using alternative axes or other approaches. The key is having an anatomically accurate 3-D reconstruction of the RV surface from which to make the regional analysis.
The present study is the first to measure TAPSE using MRI instead of ultrasound. The two modalities have a number of temporal and spatial differences. Image acquisition by MRI is ECG-triggered, whereas the end diastolic and end systolic frames are selected manually in freehand 3-D echo [12, 28]. The 4-chamber view is prescribed with reference to other views by MRI, whereas its identification by ultrasound depends on the skill and experience of the sonographer and frequently varies from the optimal position and orientation [29]. By carefully verifying that the same anatomic plane was visualized by both modalities and that TAPSE was measured at the same time point in the cardiac cycle, we obtained similar results by the two modalities. Our conclusion from this data is that TAPSE and RVEF measurements by MRI do not correlate in adult tetralogy of Fallot patients despite agreement of TAPSE measured by echocardiogram in many the same subjects.
Other investigators have also found only a weak correlation between RVEF and TAPSE when utilizing 3D echo for the RVEF measurement [30, 31]. These studies suggest that TAPSE correlates best with RVEF when measured in 2D, without consideration of the RV’s volume out of the plane of the 4-chamber view. Another consideration is that TAPSE correlates poorly with RVEF in the presence of tricuspid regurgitation [32], and our repaired TOF patients all had at least moderate tricuspid regurgitation.
These studies and our data suggest that the poor correlation of TAPSE and RVEF by MRI in this population may be due to the regional wall motion abnormalities or tricuspid regurgitation in this population rather than imaging modality.
Limitations
Due to constraints of image availability, the study population is smaller than ideal. Additionally, there is heterogeneity in regards to RVEF, age, wall motion abnormalities, and prior cardiac surgeries which may contribute to results obtained.
Conclusions
TAPSE does not correlate with RV systolic function in patients with repaired TOF. Further study of TAPSE in other conditions that alter RV anatomy, wall motion pattern, and/or tricuspid function is warranted. Quantitative analysis of regional RV function can be performed by calculation of percent stroke volume contribution.
References
Helbing WA, Bosch HG, Maliepaard C et al (1995) Comparison of echocardiographic methods with magnetic resonance imaging for assessment of right ventricular function in children. Am J Cardiol 76:589–594
Lorenz CH (2002) Right ventricular anatomy and function in health and disease. In: Manning W, JaP DJ (eds) Cardiovascular magnetic resonance. Churchill Livingstone, New York, pp 283–292
Lang RM, Bierig M, Devereux RB et al (2005) Recommendations for chamber quantification: a report from the American society of echocardiography’s guidelines and standards committee and the chamber quantification writing group, developed in conjunction with the European association of echocardiography, a branch of the European society of echocardiography. J Am Soc Echocardiogr 18:1440–1463
Gatzoulis MA, Webb GD, Daubeney PEF (2003) Adult congenital heart disease. Churchill Livingstone, Edinburgh
Kaul S, Tei C, Hopkins J, Shah P (1984) Assessment of right ventricular function using two-dimensional echocardiography. Am Heart J 107:526–531
Ghio S, Recusani F, Klersy C et al (2000) Prognostic usefulness of the tricuspid annular plane systolic excursion in patients with congestive heart failure secondary to idiopathic or ischemic dilated cardiomyopathy. Am J Cardiol 85:837–842
Therrien J, Henein MY, Li W, Somerville J, Rigby M (2000) Right ventricular long axis function in adults and children with Ebstein’s malformation. Int J Cardiol 73:243–249
Norgaard MA, Lauridsen P, Helvind M, Petterson G (1999) Twenty-to-thirty-seven-year follow-up after repair for tetralogy of Fallot. Eur J CardioThor Surg 16:125–130
Oechslin EN, Harrison DA, Harris L et al (1999) Reoperation in adults with repair of tetralogy of Fallot: indications and outcomes. J Thorac Cardiovasc Surg 118:245–251
Li W, Davlouros PA, Kilner PJ et al (2004) Doppler-echocardiographic assessment of pulmonary regurgitation in adults with repaired tetralogy of Fallot: comparison with cardiovascular magnetic resonance imaging. Am Heart J 147:165–172
Legget ME, Leotta DF, Bolson EL et al (1998) System for quantitative three dimensional echocardiography of the left ventricle based on a magnetic field position and orientation sensing system. IEEE Trans Biomed Eng 45:494–504
Miller D, Farah MG, Liner A, Fox KA, Schluchter MD, Hoit BD (2004) The relation between quantitative right ventricular ejection fraction and indices of tricuspid annular motion and myocardial performance. J Am Soc Echocardiogr 17:443–447
Alam M, Wardell J, Andersson E, Samad BA, Nordlander R (2000) Right ventricular function in patients with first inferior myocardial infarction: assessment by tricuspid annular motion and tricuspid annular velocity. Am Heart J 139:710–715
Sheehan FH, Bolson EL, Martin RW, Bashein G, McDonald JA (1998) Quantitative three dimensional echocardiography: methodology, validation, and clinical applications. 1st International conference on medical image computing and computer-assisted intervention, Springer, Boston, pp 102–109
Legget ME, Bashein G, McDonald JA et al (1998) Three-dimensional measurement of the mitral annulus by multiplane transesophageal echocardiography: in vitro validation and in vivo demonstration. J Am Soc Echocardiogr 11:188–200
Hubka M, Bolson EL, McDonald JA, Martin RW, Munt B, Sheehan FH (2002) Three-dimensional echocardiographic measurement of left and right ventricular mass and volume: in vitro validation. Int J Card Imag 18:111–118
Kaplan SR, Bashein B, Sheehan FH et al (2000) Three-dimensional echocardiographic assessment of annular shape changes in the normal and regurgitant mitral valve. Am Heart J 139:378–387
Smith JL, Bolson EL, Wong SP, Hubka M, Sheehan FH (2003) Three-dimensional assessment of two-dimensional technique for evaluation of right ventricular function by tricuspid annulus motion. Int J Card Imag 19:189–197
Hammarstrom E, Xranne B, Pinto FJ, Puryear J, Popp RL (1991) Tricuspid annular motion. J Am Soc Echocardiogr 4:131–139
Redington AN (2002) Right ventricular function. Cardiol Clin 20:341–349
Sanchez-Quintana D, Anderson RH, Ho SY (1996) Ventricular myoarchitecture in tetralogy of Fallot. Heart 76:280–286
Streeter DD Jr, Hanna WT (1973) Engineering mechanics for successive states in canine left ventricular myocardium: I. Cavity and wall geometry. Circ Res 33:639–655
Sheehan FH, Ge S, Vick GWIII et al (2008) Three-dimensional shape analysis of right ventricular remodeling in repaired tetralogy of Fallot. Am J Cardiol 101:107–113
Tulevski II, Zijta FM, Smeijers AS, Dodge-Khatami A, van der Wall EE, Mulder BJM (2004) Regional and global right ventricular dysfunction in asymptomatic or minimally symptomatic patients with congenitally corrected transposition. Cardiol Young 14:168–174
Menteer J, Weinberg PM, Fogel MA (2005) Quantifying regional right ventricular function in tetralogy of Fallot. J Cardiovasc Mag Res 7:753–761
Klein SS, Graham TPJ, Lorenz CH (1998) Noninvasive delineation of normal right ventricular contractile motion with magnetic resonance imaging myocardial tagging. Ann Biomed Eng 26:756–763
Bomma C, Dal D, Tandri H et al (2005) Regional differences in systolic and diastolic function in arrhythmogenic right ventricular dysplasia/cardiomyopathy using magnetic resonance imaging. Am J Cardiol 95:1507–1511
Hui W, El Rahman MYA, Dsebissowa F et al (2005) Comparison of modified short axis view and apical four chamber view in evaluating right ventricular function after repair of tetralogy of Fallot. Int J Cardiol 105:256–261
King DL, Harrison MR, King DL Jr, Gopal AS, Kwan OL, DeMaria AN (1992) Ultrasound beam orientation during standard two-dimensional imaging: assessment by three-dimensional echocardiography. J Am Soc Echocardiogr 5:569–576
Tamborini G, Brusoni D, Molina JET et al (2008) Feasibility of a new generation three-dimensional echocardiography for right ventricular volumetric and functional measurements. Am J Cardiol 102:499–505
Kjaergaard J, Petersen CL, Kjaer A, Schaadt BK, Oh JK, Hassager C (2006) Evaluation of right ventricular volume and function by 2D and 3D echocardiography compared to MRI. Eur J Echocardiogr 72:430–438
Hsiao S-H, Lin S-K, Wang W-C, Yang S-H, Gin P-L, Liu C-P (2006) Severe tricuspid regurgitation shows significant impact in the relationship among peak systolic tricuspid annular velocity, tricuspid annular plane systolic excursion, and right ventricular ejection fraction. J Am Soc Echocardiogr 19:902–919
Acknowledgments
Supported in part by grants from the John L. Locke, Jr. Charitable Trust and VentriPoint, Inc. (both of Seattle, WA).
Conflict of interest disclosures
Dr. Sheehan is a founder and equity holder in VentriPoint, Inc. The remaining authors have no disclosures of conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Morcos, P., Vick, G.W., Sahn, D.J. et al. Correlation of right ventricular ejection fraction and tricuspid annular plane systolic excursion in tetralogy of Fallot by magnetic resonance imaging. Int J Cardiovasc Imaging 25, 263–270 (2009). https://doi.org/10.1007/s10554-008-9387-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-008-9387-0