Abstract
Purpose
Lifestyle factors such as smoking, alcohol, body weight, physical activity, and diet quality have been associated with the risk of pancreatic cancer. However, studies of their combined association in women are limited.
Methods
Data on smoking habits, alcohol intake, diet composition, recreational physical activity, body weight, and waist circumference, obtained at recruitment for 136,945 postmenopausal women (aged 50–79 years) participating in the Women’s Health Initiative study, were categorized separately, with higher scores for each variable assigned to the categories representing healthier behaviors. The combined healthy lifestyle index (HLI) score, created by summing the scores for each risk factor, was grouped into quartiles. We used multivariable-adjusted Cox regression to estimate hazard ratios (HR) and 95% confidence intervals (CI) for pancreatic cancer risk in association with the HLI.
Results
Over an average follow-up period of approximately 16.0 years, 1,119 incident cases of pancreatic cancer were ascertained. Compared to women in the lowest HLI quartile, those in the upper quartiles (qt) had a reduced risk of pancreatic cancer (multivariable-adjusted HRqt3rd 0.83, 95% CI 0.74–0.99; and HRqt4th 0.74, 95% CI 0.62–0.88, respectively, p trend = 0.001). Use of waist circumference instead of BMI in the HLI score yielded similar results. Among women who were either non-diabetic or non-smokers, high HLI was also associated with reduced risk (HRqt4th 0.78, 95% CI 0.65–0.85 and HRqt4th 0.80, 95% CI 0.66–0.97, respectively). Stratification by BMI categories (18.5− < 25.0, 25.0− < 30.0 and > 30.0 kg/m2) showed similar results in all groups.
Conclusions
Our findings suggest that in postmenopausal women, a healthy lifestyle is associated with reduced risk of pancreatic cancer.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pancreatic ductal adenocarcinoma is the 7th most common type of cancer in the US and the 14th worldwide [1, 2]. In its early stages, the disease is often asymptomatic, so that in the majority of cases, detection and diagnosis occur at an advanced stage, when resection and treatment options are limited [3, 4], resulting in a high fatality rate associated with this malignancy [2]. Increasing age, family history, diabetes, and chronic pancreatitis are major contributors to pancreatic cancer incidence [5, 6]. In addition, several potentially modifiable risk factors such as tobacco smoking, obesity, heavy alcohol consumption, and certain dietary patterns have also been linked to increased pancreatic cancer occurrence [6, 7].
Tobacco smoking has been consistently linked with pancreatic cancer, with increased risk in current smokers, in former smokers up to 20 years after quitting [8, 9], and in those exposed to second-hand smoke [10]. Obesity and overweight in childhood and throughout adulthood have been associated with increased risk of pancreatic precancerous lesions [11] and pancreatic cancer [12]. Dietary patterns, including relatively high intake of red and processed meat, fat, and sugar, have been linked to elevated risk of pancreatic cancer in some studies [13,14,15], while there are indications that whole-plant foods may inhibit pancreatic carcinogenesis and reduce the risk of pancreatic cancer [16, 17]. Despite some inconsistencies, several prospective cohort studies have found a positive dose-dependent association between alcohol intake, particularly distilled spirits such as liquor, and increased risk of pancreatic cancer [18]. The association between physical activity and pancreatic cancer has been the focus of several case–control and cohort studies, which have shown a potential protective effects of physical activity if practiced consistently over time [19]. Both the International Agency for Research on Cancer and the World Cancer Research Fund (WCRF)/American Institute for Cancer Research (AICR) have identified these factors as targets to improve primary prevention and reduce the burden of pancreatic cancer [20]. A study focused on the population attributable fraction (PAF) of pancreatic cancer based on nationally representative data on exposures and outcome prevalence estimated a PAF for pancreatic cancer of approximately 25% due to these modifiable risk factors, in the US population [21]. Similar estimates were found in the analysis of two distinct cohorts with a total of 140,000 individuals with detailed information on these factors and pancreatic cancer occurrence [22].
The healthy lifestyle index (HLI) is a composite score which combines information on body mass index (BMI), smoking, alcohol intake, diet quality, and physical activity and has been linked to the incidence of and mortality from several chronic diseases including cardiovascular disease and some types of cancer, as well as to life expectancy and quality of life [23,24,25,26,27]. However, only two studies have used a combined index score of these modifiable risk factors to assess the impact of a healthy lifestyle on the risk of pancreatic cancer [28, 29]. Therefore, given the paucity of studies to date, we evaluated the association of this lifestyle-related composite index with risk of pancreatic cancer in the Women’s Health Initiative (WHI) cohort.
Methods
The WHI study is a large prospective study designed to advance understanding of the determinants of major chronic disease in postmenopausal women. The study includes 161,808 postmenopausal women aged 50–79 at enrollment, representing major racial/ethnic groups recruited from the general population at 40 clinical centers throughout the United States between 1993 and 1998. The WHI comprises an observational component and 4 overlapping clinical trials, including 2 hormone therapy trials, a dietary modification trial, and a calcium plus vitamin D supplementation trial. Details of the selection criteria, study design, and trial interventions have been extensively reported [30, 31]. The original WHI study was completed in 2005 and was followed by two extension studies (2005–2010 and 2010–2020) with the purpose of gathering additional outcome information. Regular contact (through visits, phone calls, or mailings) with participants occurred throughout the follow-up period to oversee the study participation and the occurrence of health-related outcomes. The study was approved by institutional review boards at all 40 clinical centers and at the coordinating center. All participants in the WHI gave written-informed consent.
Exposure information and covariates
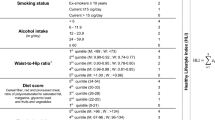
Information on demographic, health and reproductive characteristics, medication use, and lifestyle factors was collected at enrollment. Selection and categorization of the variables included in the HLI was based on WCRF/AIRC recommendation and on previous studies in this cohort [24, 32]. Dietary intake was assessed using a validated food frequency questionnaire administrated at the baseline examination [33] and was used to calculate the Alternate Healthy Eating Index (AHEI-2010), a diet quality index previously used by this and other studies [34, 35]. The AHEI is a composite score based on the intake of vegetables, fruit, nuts and soy protein, red and processed meat, trans fat, the ratio of polyunsaturated to saturated fat, and multivitamin use, with higher score values assigned to more healthy dietary habits [36]. The total AHEI-2010 score was categorized into quintiles. A self-administered questionnaire on frequency and duration of mild, moderate, and vigorous intensity recreational physical activity was completed at baseline by all study participants. A metabolic equivalent (MET) value was assigned to each category of physical activity, and the total weekly MET hours of activity was computed by multiplying the MET of each category by the duration (hours) and then summing the values (MET hours/week (h/wk)) [37]; quintiles of MET-h/wk were created. Smoking status was categorized based on smoking history and cigarette amount (never, former ≤ 15 pack years (number of packs of cigarettes smoked per day by the number of years the person had smoked), former > 15 pack years, current ≤ 15 pack years, and current > 15 pack years). Alcohol intake was calculated from the food frequency questionnaire for beer, wine, and liquor, converted to total grams (g) (12.8 g of ethanol for 360 ml (12 oz) of regular beer, 11.3 g for 360 ml (12 oz) of light beer, 11.0 g for 120 ml (4 oz) of wine, and 14.0 g for 45 ml (1.5 oz) of liquor) and categorized as < 6.0, 6.0– < 12.0, 12.0– < 24.0, 24.0– < 60.0, and ≥ 60.0 g a day (g/d). Measurements of weight (kg), height (cm), and waist circumference (cm) were obtained at baseline by trained personal. BMI was computed as measured weight divided by the square of height (kg/m2) and categorized into three groups (normal, 18.5– < 25.0; overweight, 25.0– < 30.0; and obese ≥ 30.0 kg/m2); women with a BMI < 18.5 kg/m2 were excluded, to reduce the likelihood of reverse causality due to an effect of pancreatic cancer on BMI. Waist circumference was categorized into three groups (< 80 cm, 80– < 88 cm, and ≥ 88 cm).
The combined HLI score included diet quality, level of physical activity, smoking, alcohol intake, and either body mass index or, alternatively, waist circumference, as a marker of abdominal obesity [38]. A description of each component of the HLI and the HLIWST (which included waist circumference instead of BMI) and their distribution is presented in Supplementary Table 1. The total HLI score ranged from 0 to 18 with the highest score representing the healthiest combination of factors (highest quintiles of AHEI and level of physical activity, never smoked, < 6 g/d of alcohol consumption, and normal BMI, or waist circumference < 80 cm).
Information on education, race and ethnicity, marital status, total non-alcohol energy intake, history of type 2 diabetes, history of pancreatitis, and use of hormone replacement therapy was collected at baseline. Type 2 diabetes status was updated throughout the follow-up based on information collected at each visit or via phone contact regarding receipt of a diagnosis of diabetes, use of oral glucose lowering medications or insulin, report of diabetes-related diet and exercise modifications, and hospitalization due to diabetes complications [39].
Analytic sample
For the present study, we included all participants in the observational and clinical trial components, except women randomized to the dietary intervention arm (n = 19,541) of the dietary modification trial, as well as those missing follow-up information (n = 450). In addition, we excluded underweight women (BMI < 18.5 kg/m2, n = 1,328). Some of the participants had missing data on various components of the HLI and HLIWST (Supplementary Table 1), leaving a total of 136,945 women with complete data on the HLI and 139,556 on the HLIWST.
Case ascertainment
Information of cancer occurrence was collected every 6 to 12 months by mailed or telephone questionnaires. Self-reported cancer cases were verified by centralized review of medical records and pathology reports when a biopsy or resection were available [40]. Final adjudication and histology coding were used to identify primary pancreatic adenocarcinoma cases using the National Cancer Institute’s Surveillance, Epidemiology, and End Results coding system (including codes C25.0–C25.3 and C25.7–C25.9—International Classification of Diseases for Oncology (ICD)-2, and ICD-O-3 histology codes: 8000, 8010, 8021, 8140, 8144, 8150, 8240, 8246, 8260, 8323, 8440, 8470, 8480, 8481, 8490, 8500, 8503, 8560, 8570, 8800, and 8801).
Statistical analysis
The study population was categorized into quartiles of the HLI score based on its distribution among non-cases. Descriptive statistical analyses were conducted to compare the study population baseline characteristics by HLI quartiles using Wilcoxon rank-sum tests for continuous variables and χ2 tests for categorical variables. Cox-proportional hazards models were used to estimate hazard ratios (HR) and 95% confidence intervals (CI) for the associations between the HLI quartiles and risk of pancreatic cancer using the lowest quartile as referent group; a similar approach was used for analyses based on the HLIwst. Follow-up time was used as the timescale and was calculated from the date of study entry until the date of cancer diagnosis for the cases, and until the date of death (as reported during the study follow-up and confirmed using the Vital Status from the National Death Index), withdrawal from the study, loss to follow-up, or the end of follow-up (02/28/2020) for the non-cases. No violation of the proportional hazards assumption for HLI quartiles was found on the basis of examination of Schoenfeld residuals (p value = 0.08). To test for linear trend in the risk of pancreatic cancer across the quartiles of the HLI or HLIwst, the quartile levels were included in the model as an ordinal variable and Wald test p values were reported. To evaluate whether HLIwst provided similar results to those obtained using BMI in the HLI, we compared the HR estimates associated with increments of 1 standard deviation of the HLI and HLIWST. Selection of the variables included in the multivariable model was based on their association with pancreatic cancer and whether these factors acted as confounders by altering the estimates of association for the main exposure by more than 10%. The models were adjusted for education, race/ethnicity, marital status, total non-alcohol energy intake, hormone replacement therapy, participation in the calcium and vitamin D trial, the dietary modification trial (no-intervention arm only), and/or the hormone replacement therapy trials, diabetes status and use of diabetes medications, and history of pancreatitis. In addition, when the HLIwst score was used, height was also included in the model.
We conducted several additional analyses. First, we conducted a sensitivity analysis excluding women with less than two years of follow-up to reduce the possibility of an effect of an undiagnosed pancreatic cancer on risk factors such as BMI and waist circumference. Second, type 2 diabetes is an established risk factor for pancreatic cancer [41] and is often associated with elevated BMI [42], and a diet high in fat and low in whole grain, fruits, and vegetables [43]. Therefore, we carried out analyses excluding women with type 2 diabetes to test whether the association between HLI and pancreatic cancer was mainly driven by diabetes. All diabetes-free women at baseline (n = 135,264) were included in this analysis and censored at the time they reported having diabetes, if their diabetes status changed [44]. Third, analyses were also conducted excluding women who were current smokers at baseline (n = 6,733). Fourth, to test if the association between HLI and pancreatic cancer was modified by BMI level, we carried out analyses stratified by BMI categories using HRTWST quartiles. The p value for the interaction term between HLIWST quartiles and BMI categories was obtained by comparing the likelihood ratio of the full regression model, including the cross-product of the HLIWST and BMI terms, versus the reduced model without this term. Finally, we evaluated the association of the individual components of HLI with risk of pancreatic cancer by removing one component at a time from the composite score and adjusting for it in the model. Women with missing values for any of the HLI components were excluded from the main analysis, but they were included in the analyses of the individual components for which they did not have missing values.
The analyses were conducted using STATA version 17 (Stata Corp LP, College Station, TX). All p values were two sided.
Results
Over an average follow-up period of 16.2 years (standard deviation, 7.0 years), a total of 1,119 confirmed cases of incident pancreatic cancer were ascertained among women with complete information on all the HLI components and 1,141 cases were ascertained among women with complete information on HLIWST. Baseline characteristics examined by HLI quartiles showed that women with higher HLI scores were more likely to be older, to be White, to have a higher level of education, to be married or in a marriage-like relationship, to be enrolled in the observational study component of WHI, and to have a lower total non-alcohol energy intake, and that they were less likely to have diabetes and to take diabetes medication at baseline (Table 1).
Compared to women in the lowest quartile of the HLI, those in the upper quartiles had lower risk of pancreatic cancer (multivariable-adjusted HRqt3rd 0.83, 95% CI 0.74–0.99; and HRqt4th 0.74, 95% CI 0.62–0.88, respectively, p trend = 0.001). There was an 11% reduction in risk of pancreatic cancer per standard deviation increase in the HLI (SD = 2.9 HLI) (HR 0.89, 95% CI 0.84–0.95) (Table 2). Excluding women with less than two years of follow-up from the analysis did not change the risk estimates (HRqt4th 0.73, 95% CI 0.60–0.84). Use of waist circumference instead of BMI in the HLI score yielded similar results, with a lower risk of pancreatic cancer for those in the higher HLIWST quartiles compared to the lowest quartile (HRqt2nd 0.84, 95% CI 0.70–0.99; HRqt3rd 0.80, 95% CI 0.68–0.95; and HRqt4th 0.72, 95% CI 0.61–0.85, respectively, p trend = 0.001), and a similar reduction in risk associated with a one SD (3.0 HLI WST) increment (HR 0.91, 95% CI 0.85–0.99) (Table 2). A total of 20,994 (15.5%) women developed type 2 diabetes over an average period of 6.1 years. Analysis restricted to women who remained diabetes-free during the follow-up period yielded similar results (HRqt4th 0.78, 95% CI 0.64–0.95). Also, the results were similar when the analysis was restricted to non-current smokers (HRqt4th 0.80, 95% CI 0.66–0.97).
Analyses stratified by categories of BMI showed that among women with normal BMI, a relatively high HLIWST was associated with a reduced risk of pancreatic cancer (HRqt4th 0.65, 95% CI 0.47–0.90), while among overweight and obese women, there was also a reduction in risk, although the confidence intervals included an HR of one, presumably due to the smaller sample size in these two strata. No overall effect modification by BMI on the association of HLIWST quartiles with pancreatic cancer risk was observed (p value for interaction term = 0.739) (Table 3).
Additional analyses in which each lifestyle component was excluded in turn from the overall HLI score showed that compared to women in the lowest quartile of HLI, those in the uppermost quartile had a significantly reduced risk of pancreatic cancer independently of the component excluded (Table 4).
Discussion
In this large multicenter population-based study of postmenopausal women, we found that a healthy lifestyle index, represented by having a normal BMI or a waist circumference less than 80 cm, no cigarette smoking, low alcohol intake, undertaking at least moderate levels of physical activity, and a diet rich in vegetables, fruits, nuts, and low in red meat, trans fat, and with a high polyunsaturated to saturated fat ratio, was associated with a reduced risk of pancreatic cancer over an average follow-up period of 16 years. The results were similar regardless of whether we used the HLI or the HLIWST scores, and when the analysis was restricted to non-diabetics, non-smokers, and women with normal BMI (Table 4).
Several epidemiological studies have examined the association between modifiable risk factors and the risk of pancreatic cancer, although only two studies have evaluated a combined healthy lifestyle score. A study conducted in the National Institutes of Health-AARP Diet and Health study cohort of approximately 450,000 participants (41.5% women), aged 50–71, used dichotomized scores (healthy behavior no/yes) for each of the 5 factors. Over a follow-up period of approximately 7 years, a total of 1,057 cases (382 in women) of pancreatic cancer were identified. The study showed that compared to the lowest score (0–1 points), the highest composite score (4–5) was associated with a reduction in pancreatic cancer risk (HR 0.48, 95% CI 0.37–0.63 in men, and HR 0.64, 95% CI 0.45–0.91 and in women) [28]. A second study used data from approximately 400,000 participants (age range of 35–70 years) in the European Prospective Investigation into Cancer and Nutrition and constructed a HLI using dose-dependent scores (0–4) to quantify the level of smoking status, alcohol intake, waist-to-hip ratio, and diet based on the intake of cereal fiber, vegetables and fruits, red and processed meat, polyunsaturated to saturated fat ratio, trans fat, and glycemic load [29]. Over 15 years of follow-up, a total of 1,113 cases of pancreatic cancer (634 in women) were diagnosed, and an inverse association was found between the highest HLI score (> 15 points) and risk of pancreatic cancer (HR 0.79, 95% CI 0.73–0.86, using as the reference group the second lowest HLI category (5–9 points)). Among women, each 1 standard deviation increment in the HLI score was associated with a 21% reduction in the risk of pancreatic cancer (HR 0.79, 95% CI 0.73–0.86). The results of our study are in line with those of previous studies, indicating that a healthy lifestyle score based on several modifiable factors is associated with reduced risk of pancreatic cancer.
There is a complex relationship between type 2 diabetes and pancreatic cancer. Diabetes of long duration (> 3 years) is a major risk factor for pancreatic cancer [45] and is associated with a 50–150% increased risk. However, evidence suggests that for individuals who received a diabetes diagnosis less than two years before the diagnosis of pancreatic cancer, a reverse temporal relationship between these two diseases might have occurred [46]. In the present study, we showed for the first time that a healthy lifestyle is associated with a lower risk of pancreatic cancer among non-diabetic women. Information on type 2 diabetes was available at baseline and throughout the study follow-up and was used to define time-at-risk for participants who developed diabetes subsequent to the baseline exam. This approach reduced the possibility that the observed lower risk of pancreatic cancer in women with high healthy lifestyle index was due to the association of HLI with type 2 diabetes [27]. Additional studies are needed to confirm whether a healthy lifestyle may lower the risk of pancreatic cancer in women without diabetes over a prolonged period. There were too few cases of pancreatic cancer among diabetic women to allow us to examine the association between HLI and pancreatic cancer in this sub-group. As with non-diabetics, a healthy lifestyle was associated with a reduction in risk of pancreatic cancer among women who were non-smokers. Cigarette smoking is an established risk factor for pancreatic cancer and is estimated to account for approximately 20–25% of cases [45]. In the WHI cohort, only 7% of participants were current smokers. In analyses stratified by BMI categories, we showed that among women with normal BMI, there was a statistically significant inverse association between the HLI upper quartile and pancreatic cancer risk, while in overweight and obese women, the results were not significant. These findings may be due to small sample sizes within the higher BMI categories. The results obtained with the exclusion of each individual component in turn from the HLI composite score showed that the protective effect of high HLI does not depend upon one particular factor but rather on the combination of multiple lifestyle components. However, we recognize that characteristics such as smoking and high BMI may have a stronger association than the other components of the HLI with this outcome.
The present study, the largest with respect to the number of participating women and the number of incident pancreatic cancer cases, was based on a well characterized cohort with detailed information on risk factors, a prospective design, and an average follow-up period of 16 years. The relative higher incidence rate of pancreatic cancer observed in this cohort compared to other studies [28, 29] was likely due to the higher median age of this cohort at enrollment and the extended duration of follow-up. Objective anthropometric measurements were obtained during the study baseline exam for all participants, while previous studies relied on self-reported data in part or in full [28, 29]. Cancer cases were confirmed centrally by trained physicians according to standard guidelines. The healthy lifestyle index was based on a multilevel risk score, which allowed us to evaluate the association of HLI with the outcome in a dose-dependent manner. Although the estimates of association were adjusted for several risk factors, we cannot exclude the possibility of residual confounding. Furthermore, we did not have repeated measurements of lifestyle factors throughout follow-up, which would have allowed for better characterization and control for lifestyle factors changes.
In conclusion, we found that in this cohort of postmenopausal women, a relatively high healthy lifestyle index is associated with reduced risk of pancreatic cancer over a follow-up period of more than a decade. Pancreatic cancer remains one of the deadliest types of malignancy in the United States and worldwide. The results of our study suggest that promoting smoking cessation and limiting alcohol consumption, along with undertaking regular physical activity, consuming a healthy diet rich in fruits, vegetables, and whole grains and low in saturated and trans fats, and maintaining a healthy body weight, may be important steps to lower the risk of this lethal cancer.
Data availability
Data are available through the WHI online resource, https://www.whi.org/researchers/data/Pages/Home.aspx, and the WHI remains funded indefinitely through BioLINCC, https://biolincc.nhlbi.nih.gov/studies/whi_ctos/.
Change history
26 July 2023
A Correction to this paper has been published: https://doi.org/10.1007/s10552-023-01754-3
References
Siegel RL, Miller KD, Jemal A (2020) Cancer statistics, 2020. CA Cancer J Clin 70:7–30. https://doi.org/10.3322/caac.21590
McGuigan A, Kelly P, Turkington RC, Jones C, Coleman HG, McCain RS (2018) Pancreatic cancer: A review of clinical diagnosis, epidemiology, treatment and outcomes. World J Gastroenterol 24:4846–4861. https://doi.org/10.3748/wjg.v24.i43.4846
Kleeff J, Korc M, Apte M, La Vecchia C, Johnson CD, Biankin AV et al (2016) Pancreatic cancer. Nat Rev Dis Primers 2:16022. https://doi.org/10.1038/nrdp.2016.22
Ducreux M, Seufferlein T, Van Laethem JL, Laurent-Puig P, Smolenschi C, Malka D et al (2019) Systemic treatment of pancreatic cancer revisited. Semin Oncol 46:28–38. https://doi.org/10.1053/j.seminoncol.2018.12.003
The global, regional, and national burden of pancreatic cancer and its attributable risk factors in 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet Gastroenterol Hepatol. 4(2019) 934–947. https://doi.org/10.1016/s2468-1253(19)30347-4.
Maisonneuve P, Lowenfels AB (2015) Risk factors for pancreatic cancer: a summary review of meta-analytical studies. Int J Epidemiol 44:186–198. https://doi.org/10.1093/ije/dyu240
Midha S, Chawla S, Garg PK (2016) Modifiable and non-modifiable risk factors for pancreatic cancer: a review. Cancer Lett 381:269–277. https://doi.org/10.1016/j.canlet.2016.07.022
Koyanagi YN, Ito H, Matsuo K, Sugawara Y, Hidaka A, Sawada N et al (2019) Smoking and pancreatic cancer incidence: a pooled analysis of 10 population-based cohort studies in Japan. Cancer Epidemiol Biomarkers Prev 28:1370–1378. https://doi.org/10.1158/1055-9965.Epi-18-1327
Cigarette smoking and pancreatic cancer: an analysis from the International Pancreatic Cancer Case-Control Consortium (Panc4). Ann Oncol. 23(2012) 2773. https://doi.org/10.1093/annonc/mds491.
Chuang SC, Gallo V, Michaud D, Overvad K, Tjønneland A, Clavel-Chapelon F et al (2011) Exposure to environmental tobacco smoke in childhood and incidence of cancer in adulthood in never smokers in the European Prospective Investigation into Cancer and Nutrition. Cancer Causes Control 22:487–494. https://doi.org/10.1007/s10552-010-9723-2
Rebours V, Gaujoux S, d’Assignies G, Sauvanet A, Ruszniewski P, Lévy P et al (2015) Obesity and fatty pancreatic infiltration are risk factors for pancreatic precancerous lesions (PanIN). Clin Cancer Res 21:3522–3528. https://doi.org/10.1158/1078-0432.Ccr-14-2385
Berrington de Gonzalez A, Sweetland S, Spencer E (2003) A meta-analysis of obesity and the risk of pancreatic cancer. Br J Cancer 89:519–523. https://doi.org/10.1038/sj.bjc.6601140
Casari I, Falasca M (2015) Diet and Pancreatic Cancer Prevention. Cancers (Basel) 7:2309–2317. https://doi.org/10.3390/cancers7040892
Hine RJ, Srivastava S, Milner JA, Ross SA (2003) Nutritional links to plausible mechanisms underlying pancreatic cancer: a conference report. Pancreas 27:356–366. https://doi.org/10.1097/00006676-200311000-00014
Nöthlings U, Wilkens LR, Murphy SP, Hankin JH, Henderson BE, Kolonel LN (2005) Meat and fat intake as risk factors for pancreatic cancer: the multiethnic cohort study. J Natl Cancer Inst 97:1458–1465. https://doi.org/10.1093/jnci/dji292
Harris DM, Srihari P, Go VLW (2011) Pancreatic Cancer Prevention and the 2010 Dietary Guidelines for Americans. 40:641–643. https://doi.org/10.1097/MPA.0b013e3182203e3c
Zheng J, Guinter MA, Merchant AT, Wirth MD, Zhang J, Stolzenberg-Solomon RZ et al (2017) Dietary patterns and risk of pancreatic cancer: a systematic review. Nutr Rev 75:883–908. https://doi.org/10.1093/nutrit/nux038
Wang YT, Gou YW, Jin WW, Xiao M, Fang HY (2016) Association between alcohol intake and the risk of pancreatic cancer: a dose-response meta-analysis of cohort studies. BMC Cancer 16:212. https://doi.org/10.1186/s12885-016-2241-1
Behrens G, Jochem C, Schmid D, Keimling M, Ricci C, Leitzmann MF (2015) Physical activity and risk of pancreatic cancer: a systematic review and meta-analysis. Eur J Epidemiol 30:279–298. https://doi.org/10.1007/s10654-015-0014-9
Maisonneuve P (2019) Epidemiology and burden of pancreatic cancer. Presse Med 48:e113–e123. https://doi.org/10.1016/j.lpm.2019.02.030
Islami F, Goding Sauer A, Miller KD, Siegel RL, Fedewa SA, Jacobs EJ et al (2018) Proportion and number of cancer cases and deaths attributable to potentially modifiable risk factors in the United States. CA Cancer J Clin 68:31–54. https://doi.org/10.3322/caac.21440
Song M, Giovannucci E (2020) Preventable incidence of carcinoma associated with adiposity, alcohol and physical inactivity according to smoking status in the United States. Int J Cancer 146:2960–2967. https://doi.org/10.1002/ijc.32602
Ghosn B, Benisi-Kohansal S, Ebrahimpour-Koujan S, Azadbakht L, Esmaillzadeh A (2020) Association between healthy lifestyle score and breast cancer. Nutr J 19:4. https://doi.org/10.1186/s12937-020-0520-9
Arthur R, Brasky TM, Crane TE, Felix AS, Kaunitz AM, Shadyab AH et al (2019) Associations of a healthy lifestyle index with the risks of endometrial and ovarian cancer among women in the women’s health initiative study. Am J Epidemiol 188:261–273. https://doi.org/10.1093/aje/kwy249
Dartois L, Fagherazzi G, Boutron-Ruault MC, Mesrine S, Clavel-Chapelon F (2014) Association between five lifestyle habits and cancer risk: results from the E3N cohort. Cancer Prev Res (Phila) 7:516–525. https://doi.org/10.1158/1940-6207.Capr-13-0325
Barbaresko J, Rienks J, Nöthlings U (2018) Lifestyle indices and cardiovascular disease risk: a meta-analysis. Am J Prev Med 55:555–564. https://doi.org/10.1016/j.amepre.2018.04.046
Li Y, Schoufour J, Wang DD, Dhana K, Pan A, Liu X et al (2020) Healthy lifestyle and life expectancy free of cancer, cardiovascular disease, and type 2 diabetes: prospective cohort study. BMJ 368:l6669. https://doi.org/10.1136/bmj.l6669
Jiao L, Mitrou PN, Reedy J, Graubard BI, Hollenbeck AR, Schatzkin A et al (2009) A combined healthy lifestyle score and risk of pancreatic cancer in a large cohort study. Arch Intern Med 169:764–770. https://doi.org/10.1001/archinternmed.2009.46
Naudin S, Viallon V, Hashim D, Freisling H, Jenab M, Weiderpass E et al (2020) Healthy lifestyle and the risk of pancreatic cancer in the EPIC study. Eur J Epidemiol 35:975–986. https://doi.org/10.1007/s10654-019-00559-6
(1998) Design of the Women's Health Initiative clinical trial and observational study. The Women's Health Initiative Study Group. Control Clin Trials. 19:61–109. https://doi.org/10.1016/s0197-2456(97)00078-0.
Langer RD, White E, Lewis CE, Kotchen JM, Hendrix SL, Trevisan M (2003) The Women’s Health Initiative Observational Study: baseline characteristics of participants and reliability of baseline measures. Ann Epidemiol 13:S107–S121. https://doi.org/10.1016/s1047-2797(03)00047-4
Arthur R, Wassertheil-Smoller S, Manson JE, Luo J, Snetselaar L, Hastert T et al (2018) The combined association of modifiable risk factors with breast cancer risk in the women’s health initiative. Cancer Prev Res (Phila) 11:317–326. https://doi.org/10.1158/1940-6207.Capr-17-0347
Patterson RE, Kristal AR, Tinker LF, Carter RA, Bolton MP, Agurs-Collins T (1999) Measurement characteristics of the Women’s Health Initiative food frequency questionnaire. Ann Epidemiol 9:178–187. https://doi.org/10.1016/s1047-2797(98)00055-6
Belin RJ, Greenland P, Allison M, Martin L, Shikany JM, Larson J et al (2011) Diet quality and the risk of cardiovascular disease: the Women’s Health Initiative (WHI). Am J Clin Nutr 94:49–57. https://doi.org/10.3945/ajcn.110.011221
McCullough ML, Feskanich D, Stampfer MJ, Giovannucci EL, Rimm EB, Hu FB et al (2002) Diet quality and major chronic disease risk in men and women: moving toward improved dietary guidance. Am J Clin Nutr 76:1261–1271. https://doi.org/10.1093/ajcn/76.6.1261
Chiuve SE, Fung TT, Rimm EB, Hu FB, McCullough ML, Wang M et al (2012) Alternative dietary indices both strongly predict risk of chronic disease. J Nutr 142:1009–1018. https://doi.org/10.3945/jn.111.157222
Ainsworth BE, Haskell WL, Leon AS, Jacobs DR Jr, Montoye HJ, Sallis JF et al (1993) Compendium of physical activities: classification of energy costs of human physical activities. Med Sci Sports Exerc 25:71–80. https://doi.org/10.1249/00005768-199301000-00011
Aune D, Greenwood DC, Chan DS, Vieira R, Vieira AR, Navarro Rosenblatt DA et al (2012) Body mass index, abdominal fatness and pancreatic cancer risk: a systematic review and non-linear dose-response meta-analysis of prospective studies. Ann Oncol 23:843–852. https://doi.org/10.1093/annonc/mdr398
Liu S, Tinker L, Song Y, Rifai N, Bonds DE, Cook NR et al (2007) A prospective study of inflammatory cytokines and diabetes mellitus in a multiethnic cohort of postmenopausal women. Arch Intern Med 167:1676–1685. https://doi.org/10.1001/archinte.167.15.1676
Curb JD, McTiernan A, Heckbert SR, Kooperberg C, Stanford J, Nevitt M et al (2003) Outcomes ascertainment and adjudication methods in the Women’s Health Initiative. Ann Epidemiol 13:S122–S128. https://doi.org/10.1016/s1047-2797(03)00048-6
Everhart J, Wright D (1995) Diabetes mellitus as a risk factor for pancreatic cancer. A meta-analysis. JAMA 273:1605–1609
Eibl G, Cruz-Monserrate Z, Korc M, Petrov MS, Goodarzi MO, Fisher WE et al (2018) Diabetes mellitus and obesity as risk factors for pancreatic cancer. J Acad Nutr Diet 118:555–567. https://doi.org/10.1016/j.jand.2017.07.005
Toi PL, Anothaisintawee T, Chaikledkaew U, Briones JR, Reutrakul S, Thakkinstian A (2020) Preventive role of diet interventions and dietary factors in type 2 diabetes mellitus: an umbrella review. Nutrients. https://doi.org/10.3390/nu12092722
Jin Q, Hart PA, Shi N, Joseph JJ, Donneyong M, Conwell DL et al (2021) Dietary patterns of insulinemia, inflammation and glycemia, and pancreatic cancer risk: findings from the women’s health initiative. Cancer Epidemiol Biomarkers Prev 30:1229–1240. https://doi.org/10.1158/1055-9965.Epi-20-1478
Klein AP (2021) Pancreatic cancer epidemiology: understanding the role of lifestyle and inherited risk factors. Nat Rev Gastroenterol Hepatol 18:493–502. https://doi.org/10.1038/s41575-021-00457-x
Andersen DK, Korc M, Petersen GM, Eibl G, Li D, Rickels MR et al (2017) Diabetes, pancreatogenic diabetes, and pancreatic cancer. Diabetes 66:1103–1110. https://doi.org/10.2337/db16-1477
Acknowledgments
We thank the Women's Health Initiative investigators, staff, and the trial participants for their outstanding dedication and commitment. Program Office: (National Heart, Lung, and Blood Institute, Bethesda, MD) Jacques Roscoe, Shari Ludlum, Dale Burden, Joan McGowan, Leslie Ford, and Nancy Geller. Clinical Coordinating Center: (Fred Hutchinson Cancer Research Center, Seattle, WA) Garnet Anderson, Ross Prentice, Andrea LaCroix, and Charles Kopperberg). Investigators and Academic Centers: (Brigham and Women's Hospital, Harvard Medical School, Boston, MA) JoAnn E, Manson; (MedStar Health Research Institute/Howard University, Washington, DC) Barbara V Howard; (Stanford Prevention Research Center, Stanford, CA) Marcia L. Stefanick; (The Ohio State University, Columbus, OH) Rebecca Jackson; (University of Arizona, Tucson/Phoenix, AZ) Cynthia A. Thompson; (University at Buffalo, Buffalo, NY) Jean Wactawski-Wende; (University of Florida, Gainesville/Jacksonville, FL) Marian Limacher; (University of Iowa, Iowa City/Davenport, IA) Robert Wallace; (University of Pittsburgh, Pittsburgh, PA) Lewis Kuller; (City of Hope Comprehensive Cancer Center, Duarte, CA) Rowan T. Chlebowski; (Wake Forest University School of Medicine, Winston–Salem, NC) Sally Shumaker. Women's Health Initiative Memory Study: (Wake Forest University School of Medicine, Winston Salem, NC) Sally Shumaker. A full list of all the investigators who have contributed to Women's Health Initiative science appears at https://www.whi.org/researchers/Documents%20%20Write%20a%20Paper/WHI%20Investigator%20Long%20List.pdf
Funding
This work was supported by Women’s Health Initiative. The WHI program is funded by the National Heart, Lung, and Blood Institute, National Institutes of Health, U.S. Department of Health and Human Services through contracts HHSN268201600018C, HHSN268201600001C, HHSN268201600002C, HHSN268201600003C, and HHSN268201600004C.
Author information
Authors and Affiliations
Contributions
Conceptualization—TER. Data curation, formal analysis, and investigation RP. Methodology—RP: writing—original draft—RP, TER. Writing—rewriting and editing—all authors.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures in the study were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki Declaration and its later amendments. The study was approved by institutional review boards at all 40 clinical centers and at the coordinating center.
Informed consent
All participants in the WHI gave written-informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: The co-author has been revised.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Peila, R., Coday, M., Crane, T.E. et al. Healthy lifestyle index and risk of pancreatic cancer in the Women’s Health Initiative. Cancer Causes Control 33, 737–747 (2022). https://doi.org/10.1007/s10552-022-01558-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-022-01558-x