Abstract
During the past several decades, an increasing incidence of thyroid cancer has been reported in many parts of the world. To date, no study has compared the trends in thyroid cancer incidence across continents. We examined incidence data from cancer incidence in five continents (CI5) over the 30-year period 1973–2002 from 19 populations in the Americas, Asia, Europe, and Oceania. Thyroid cancer rates have increased from 1973–1977 to 1998–2002 for most of the populations except Sweden, in which the incidence rates decreased about 18% for both males and females. The average increase was 48.0% among males and 66.7% among females. More recently, the age-adjusted international thyroid cancer incidence rates from 1998 to 2002 varied 5-fold for males and nearly 10-fold for females by geographic region. Considerable variation in thyroid cancer incidence was present for every continent but Africa, in which the incidence rates were generally low. Our analysis of published CI5 data suggests that thyroid cancer rates increased between 1973 and 2002 in most populations worldwide, and that the increase does not appear to be restricted to a particular region of the world or by the underlying rates of thyroid cancer.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Thyroid cancer is a relatively rare neoplasm worldwide, accounting for approximately 1–5% of all cancers in females and <2% in males [1]. Although the incidence of thyroid cancer is relatively rare, it is the most common endocrine malignancy worldwide [1]. While the international incidence varies considerably, a fairly consistent female-to-male ratio of 3:1 is observed in almost all geographic areas and ethnic groups [1].
During the past several decades, an increasing incidence of thyroid cancer has been reported in some European countries, the United States, and some parts of the China [2–7]; however, no study has provided a comparison of trends in thyroid cancer incidence across continents. The International Agency of Research on Cancer (IARC) has published rates for time periods spanning three decades for 95 registries around the world, enabling the analysis of trends over a relatively longer time period. In order to understand how thyroid cancer incidence has changed over time across different populations and what factors may be responsible for the observed change, we examined incidence data over the 30-year period 1973–2002 from 19 populations in the Americas, Asia, Europe, and Oceania.
Materials and methods
Incidence data
In order to examine the secular trends in the incidence of thyroid cancer, age-standardized (World Population) incidence rates were obtained from Vols. 4–9 of cancer incidence in five continents (CI5). The CI5 volumes include incidence data reported by selected population-based cancer registries covering areas within Asia, Oceania, Africa, Europe, and the Americas. Volumes 4–9 generally provided data for the 5-year periods: 1973–1977, 1978–1982, 1983–1987, 1988–1992, 1993–1997, and 1998–2002. The classification of thyroid cancer was based on ICD-8, ICD-9, and ICD-10 for Vols. 4, 5–8, and 9, respectively. There were no changes in the coding of thyroid cancer among the 8th, 9th, and 10th revisions (193). Incidence rates for different histologic subtypes (follicular, papillary, medullar, anaplastic, and other/unspecified) were abstracted from Vol. 9, as incidence rates for specific subtypes was not provided in the earlier volumes.
Populations were chosen for inclusion in our analysis on the basis of the following criteria: (1) availability of rates in the CI5 for time periods at least, as far back as 1978–1982; (2) an absence of changes in population coverage or of warnings regarding data quality; and (3) a sufficiently large number of registered cases in CI5 Vol. 9 to enable analyses of recent rates by histologic subtype (trends by histologic subtype are not included in our study). Only one registry from each country was selected; if more than one registry met the basic criteria, the registry with the largest population was included in the analysis. A total of 19 populations were selected: four from the Americas, four from Asia, four from Scandinavia, five from elsewhere in Europe and two from Oceania. No African or South Asian populations met all the inclusion criteria. However, five African countries included in CI5 Vol. 9 (Algeria, Setif; Egypt, Gharbiah; Tunisia, Center, Sousse; Uganda, Kyadondo Country; and Zimbabwe, Harrare) and the registry of Mumbai, India, had rates available which allowed for a broader geographic comparison for recent years.
Data analysis
Thyroid cancer incidence is presented overall and by histologic subtype for males and females separately for selected populations for the time period 1998–2002. Trends in age-standardized (world standard) incidence rates were examined for the time periods 1973–1977, 1978–1982,1983–1987, 1988–1992, 1993–1997, and 1998–2002. The percentage change in thyroid cancer rates between 1973–1977 and 1998–2002 was calculated for each population to show the relative change in incidence between these two periods for males and females separately.
Results
The 1998–2002 age-adjusted thyroid cancer incidence rates varied 5-fold for males and nearly 10-fold for females (Table 1), with the highest rates in the US and Israel for males (3.5 per 100,000 for both countries) and for females (10.0 per 100,000 and 12.1 per 100,000, respectively), and the lowest rates in Uganda for males (0.5 per 100,000) and for females (1.5 per 100,000). Neither the highest rates nor the lowest rates were concentrated in one continent for either males or females. Considerable variation in thyroid cancer incidence was present within every continent with the exception of Africa, in which the incidence rates were generally low. Based on the rates from 1998 to 2002, the incidence of papillary was the highest, followed by follicular, medullar and anaplastic subtypes (Figs. 1, 2).
Thyroid cancer rates increased from 1973–1977 to 1998–2002 (Table 1) for most populations. On average, the populations with increasing rates experienced about a 58.1% increase. The average increase was 48.0% among males and 66.7% among females with the largest increase in New South Wales, Australia for both males (177.8%) and females (252.2%). In contrast, the incidence rates decreased for males in Sweden (18.8%) and for females in Norway, Sweden, and Spain (5.8%, 18.2%, and 25.9%, respectively).
The thyroid cancer rates among each population during the 30-year period 1973–2002 are shown in Fig. 2a, b. Fairly consistent increasing trends in rates were apparent for most populations, and positive trends were generally stronger among females. There has been, however, a leveling off for trends in the Scandinavian countries.
Discussion
During the period 1973–2002, the incidence rates of thyroid cancer increased among most populations examined. Thyroid cancer incidence among the 19 populations varied more than 5-fold in both males and females. The variation was mainly attributed to papillary thyroid carcinoma. Despite the wide intercountry variation in age-adjusted incidence rates, a consistent female-to-male ratio of 3:1 is observed within most of the countries included in both the earlier (1973–1977) and later (1998–2002) data (Figs. 3, 4).
It is currently unclear whether the observed increases in thyroid cancer are real or are due to increased diagnosis. The common use of fine needle aspiration technology in the late 1980s in combination with thyroid ultrasound has facilitated the diagnosis of smaller thyroid tumors [8] in areas with access to these technologies. Previously, investigators concluded that the increase in the incidence rates reflects the increased detection of subclinical disease, not an increase in the true occurrence of thyroid cancer due to the increase in microcarcinomas [8]. Since, information on tumor size is not available for majority of the registries, we were unable to assess whether the international incidence rates increased for all sizes of thyroid cancer tumors or mainly in cases with smaller size tumors. However, we observed a substantial percent change from 1988–95 to 1996–2005 in the incidence of thyroid cancer for both smaller size tumors and larger size tumors in the SEER 9 database [9], with a 120.85% increase in thyroid microcarcinomas < 1 cm, and a 56.2% increase for thyroid tumors > 4 cm. This argues against advanced diagnostic techniques or increased attention to small nodules as the only explanation for the observed increasing trend of thyroid cancer.
The histopathologic classification system for thyroid cancer has evolved over time. In 1988, the World Health Organization (WHO) revised its classification when it was recognized that nuclear features (particularly nuclear inclusions and nuclear folds) are more important than architectural patterns in classifying thyroid cancer [10]. As a result, many cancers previously classified as follicular are now categorized as follicular variants of papillary cancer [11]. Although changes in classification could impact the distribution of cases by subtype, this point does not undermine our findings as the total number of cases diagnosed should not be significantly affected.
Most countries have introduced nationwide iodization measures, but there are regional differences in the year iodine supplementation was implemented. In 1990, iodine deficiency affected almost one-third of the world population [12]. Following a resolution adopted by the World Summit for Children in 1990, major programs of iodine supplementation were implemented by the governments of the affected countries. By April 1999, 68% of the affected populations had access to iodized salt. It has been noted that when iodine supplementation occurs in iodine deficient regions, the proportion of papillary thyroid cancers often increases although the overall rates tend to stay the same [13, 14]. According to the World Health Organization, of the countries included in this study with available iodine intake data, Denmark, France, Italy, Australia, New Zealand, and Algeria are reported to be iodine deficient [15].
The differences in thyroid cancer rates, particularly among women, in the Scandinavian countries are notable because similar standards of medical care and reporting in the Scandinavian countries reduce the limitations associated with intercountry comparisons. The age-adjusted incidence rate among women in Finland is over twice that reported in Denmark in both time periods of interest (1973–1977 and 1998–2002). Furthermore, the wide variation in percent change over the past three decades in these countries is striking. This suggests that these populations may be experiencing different levels of environmental exposure to a significant risk factor/set of risk factors.
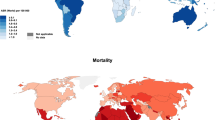
It is also notable that despite the wide intercountry variation in age-adjusted incidence rates, according to the GloboCan 2002 database [16], there is a small variation in sex-specific mortality rates by geographic region. Among females, the current thyroid cancer mortality rates for the European, Oceanic, American, and Asian countries included in this analysis is between 0.2 and 1.0 per 100,000 person-years. Similarly, for males, the range in thyroid cancer mortality rates is from 0.1 to 0.7 per 100,000 person-years. Such consistency in the mortality burden suggests that differences in incidence may be a function of detection methods. However, as thyroid cancer is known to have a high rate of survival, the intercountry consistency in mortality rate may not necessarily be evidence for artificially inflated rates.
There is emerging evidence that PBDEs alter thyroid hormone homeostasis and cause thyroid dysfunction, and may subsequently play a role in the global increase in thyroid tumorigenesis [17]. The use of PBDEs has increased rapidly during the last three decades in the US and other parts of the world, doubling in some areas in less than a decade [18], reaching a global demand of 200,000 tons in 2003 [19]. PBDEs are widely used as flame retardants in polyurethane foam, textiles, and hard plastics used in applications such as carpet pads, furniture, curtains, televisions, computers, and seats in automobiles and airplanes. The impact of these hormone disrupting agents in the etiology of thyroid cancer is of interest, as there is strong animal data and evidence for increasing and widespread global exposure. The European Union banned the use of two PBDEs (Penta- and OctaBDE) in 2004 due to increasing evidence that PBDEs may result in thyroid toxicity, liver toxicity, and neurodevelopmental toxicity, and because PBDEs accumulate in human breast milk [20]. The State of Washington also passed a bill banning the use of PBDEs in 2007 [21]. However, these compounds, like the other previously banned PHAHs (such as PCBs, DDT, and HCB), will remain ubiquitous in the environment due to their stability, persistence, and their ability to bioaccumulate.
It is also notable that despite the wide intercountry variation in age-adjusted incidence rates, a consistent female-to-male ratio of 3:1 is observed within most of the countries included in the international comparison in both the earlier (1973–1977) and later (1998–2002) data. Possible explanations for the disparities between males and females with sporadic thyroid cancers are biological sex differences, differential screening patterns, or gender-specific behavioral differences. One hypothesized mechanism is that increased levels of female hormones during reproductive years, due to pregnancy which increases thyroid stimulating hormone (TSH) levels, potentially lead to thyroid dysplasia and then to cancer [22–25]. Experimental evidence shows that TSH stimulation of the thyroid gland leads to proliferative changes in follicular cells including hypertrophy and hyperplasia, as well as ultimately neoplasia in rodents [26]. Our results confirm the previously observed gender disparity and support the need for future research in this area.
In summary, our analysis of published CI5 data suggests that thyroid cancer rates increased between 1973 and 2002 in most populations worldwide, for males and females, and that the increase does not appear to be restricted to a particular region of the world or by the underlying rates of thyroid cancer. There is also some indication that the rates may be leveling off in some populations. The worldwide increase in thyroid cancer incidence may be due to changes in the prevalence of important risk factors; epidemiologic investigations describing between population differences and within population trends in the prevalence of suspected risk factors may yield important insights into the causes of the widespread increase in thyroid cancer.
References
Curado MP, Edwards B, Shin HR, Storm H, Ferlay J, Heanue M, Boyle P (eds) (2007) Cancer incidence in five continents, vol IX. IARC Scientific Publications, Lyon, IARC, p 160
Akslen LA, Haldorsen T, Thoresen SO, Glattre E (1993) Incidence pattern of thyroid cancer in Norway: influence of birth cohort and time period. Int J Cancer 53:183–187. doi:10.1002/ijc.2910530202
Colonna M, Grosclaude P, Remontet L et al (2002) Incidence of thyroid cancer in adults recorded by French cancer registries (1978–1997). Eur J Cancer 38:1762–1768. doi:10.1016/S0959-8049(02)00110-7
Dos Santos Silva I, Swerdlow AJ (1993) Thyroid cancer epidemiology in England and Wales: time trends and geographical distribution. Br J Cancer 67:330–340
Montanaro F, Pury P, Bordoni A, Lutz JM (2006) Unexpected additional increase in the incidence of thyroid cancer among a recent birth cohort in Switzerland. Eur J Cancer Prev 15:178–186. doi:10.1097/01.cej.0000197450.94980.36
Pettersson B, Adami HO, Wilander E, Coleman MP (1991) Trends in thyroid cancer incidence in Sweden, 1958–1981, by histopathologic type. Int J Cancer 48:28–33
Qian B, He M, Dong S, Wang J, Chen K (2005) Incidence and mortality of thyroid cancers in Tianjin from 1981 to 2001. Chin J Endocrinol Metab 21:432–434
Davies L, Welch HG (2006) Increasing incidence of thyroid cancer in the United States, 1973–2002. JAMA 295:2164–2167. doi:10.1001/jama.295.18.2164
Surveillance, Epidemiology, and End Results (SEER) Program (November 2007 submission). Public-use database (1973–2005). National Cancer Institute DCCPS, Suveillance Research Program, Cancer Statistics Branch, Released April 2008, based on the November 2007 submission
World Health Organization (1998) In: Hedinger CWE, Sobin LH (eds) Histological typing of thyroid tumours, 2nd edn. Springer, Berlin
LiVolsi VA, Asa SL (1994) The demise of follicular carcinoma of the thyroid gland. Thyroid 4:233–236
Delange F, Lecomte P (2003) Iodine supplementation: benefits outweigh risk. Drug Saf 22:89–95. doi:10.2165/00002018-200022020-00001
Harach HR (2003) Sporadic versus familial medullary thyroid microcarcinoma. Am J Surg Pathol 27:136–137. doi:10.1097/00000478-200301000-00016
Huszno B, Szybinski Z, Przybylik-Mazurek E, Stachura J, Trofimiuk M, Buziak-Bereza M, Gollowski F, Pantoflinski J (2003) Incidence of thyroid cancer in the selected areas of iodine deficiency in Poland. J Endocrinol Invest 26:57–62
World Health Organization (2004). In: de Benoist B, Andersson M, Egli I, Takkouche B, Allen H (eds). Iodine status worldwide: WHO global database on iodine deficiency. Department of Nutrition for Health and Development. World Health Organization, Geneva
Ferlay J, Bray F, Pisani P, Parkin DM (2004) GLOBOCAN 2002: cancer incidence, mortality and prevalence worldwide. IARC CancerBase No. 5. Version 2.0. IARC Press, Lyon
Zhang Y, Guo G, Han X, Zhu C, Kilfoy BA, Zhu Y, Boyle P, Zheng T (2008) Do polybrominated diphenyl ethers (PBDEs) increase the risk of thyroid cancer? Biosci Hypothesis 1:195–199. doi:10.1016/j.bihy.2008.06.003
Schecter A, Päpke O, Tung KC, Joseph J, Harris TR, Dahlgren J (2005) Polybrominated diphenyl ether flame retardants in the U.S. population: current levels, temporal trends, and comparison with dioxins, dibenzofurans, and polychlorinated biphenyls. J Occup Environ Med 47(3):199–211. doi:10.1097/01.jom.0000158704.27536.d2 Mar
Guvenius DM, Aronsson A, Ekman-Ordeberg G, Bergman A, Noren K (2003) Human prenatal and postnatal exposure to polybrominated diphenyl ethers, polychlorinated biphenyls, polychlorobiphenylols, and pentachlorophenol. Environ Health Perspect 111:1235–1241
Directive 2003/11/EC of the European Parliament and of the Council of 6 February 2003 amending for the 24th time Council Directive 76/769/EEC relating to restrictions on the marketing and use of certain dangerous substances and preparations (pentabromodiphenyl ether, octabromodiphenylether). http://eur-x.europa.eu/LexUriServ/site/en/oj/2003/l_042/l_04220030215en00450046.pdf
“Chemical ban puts industry on the defensive.” State of Washington bans use of PBDEs. http://seattlepi.nwsource.com/local/311845_pbdes17.html
Memon A, Darif M, Al-Saleh K, Suresh A (2002) Epidemiology of reproductive and hormonal factors in thyroid cancer: evidence from a case–control study in the Middle East. Int J Cancer 97:82–89. doi:10.1002/ijc.1573
Negri E, Dal Maso L, Ron E et al (1999) A pooled analysis of case-control studies of thyroid cancer. II. Menstrual and reproductive factors. Cancer Causes Control 10:143–155. doi:10.1023/A:1008880429862
Zivaljevic V, Vlajinac H, Jankovic R et al (2003) Case–control study of female thyroid cancer—menstrual, reproductive and hormonal factors. Eur J Cancer Prev 12:63–66. doi:10.1097/00008469-200302000-00010
Goodman MT, Kolonel LN, Wilkens LR (1992) The association of body size, reproductive factors and thyroid cancer. Br J Cancer 66:1180–1184
Smith P, Williams ED, Wynford-Thomas D (1987) In vitro demonstration of a TSH-specific growth desensitising mechanism in rat thyroid epithelium. Mol Cell Endocrinol 51:51–58. doi:10.1016/0303-7207(87)90118-3
Acknowledgment
This research was supported by the National Institutes of Health training grant TU2CA105666 and National Institutes of Health Fogarty training grant 2043TW007864-01.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kilfoy, B.A., Zheng, T., Holford, T.R. et al. International patterns and trends in thyroid cancer incidence, 1973–2002. Cancer Causes Control 20, 525–531 (2009). https://doi.org/10.1007/s10552-008-9260-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-008-9260-4