Abstract
Polyinosinic-polycytidylic acid [Poly (I: C)], a ligand for Toll-like receptor (TLR-3), is used as an adjuvant to enhance anti-tumor immunity because of its prominent effects on CD8 T cells and NK cells. Myeloid-derived suppressor cells (MDSCs) are one of the main immunosuppressive factors in cancer, and their abnormal accumulation is correlated with the clinical stage of breast cancer and is an important mechanism of tumor immune evasion. Although Poly (I: C) is thought to have direct anti-tumor activity in different cell lines, its effect on immunosuppressive MDSCs in tumor-bearing animals has not been studied. 4T1-Luc, a metastatic breast cancer mouse cell line, was injected into the left flank of female BALB/c mice. Tumor-bearing mice were treated with i.p. injection of Poly (I: C) or PBS beginning on day 7 after tumor inoculation. WBCs and MDSCs were counted using coulter counter and stained for flow cytometry, respectively. Bioluminescent imaging was used to monitor tumor burden at multiple time points during the course of tumor growth. Poly (I: C) treatment led to a decrease in MDSC frequencies in BM, blood, and tumor compared to saline-treated control mice. Poly (I: C) treatment also abrogated the immunosuppressive function of MDSCs, concomitant with an increase in local T cell response of the immune system in a murine model of breast cancer. Poly (I: C) treatment decreases MDSC frequency and immunosuppressive function in 4T1-tumor-bearing hosts and effectively augments the activity of breast cancer immunotherapy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Polyinosinic-polycytidylic acid (Poly (I: C)) is a synthetic dsRNA analog that is recognized by Toll-like receptor-3 (TLR-3), triggering innate and adaptive immune responses. Based on its ability to enhance immunity, Poly (I: C) has been used as a vaccine adjuvant over the past decade. In recent years, evidence has accumulated that Poly (I: C) can also directly trigger apoptosis in some cell lines [1–3].
Myeloid-derived suppressor cells (MDSCs) are a heterogeneous population of early myeloid and dendritic cells that expand from the bone marrow during tumor progression and have the ability to inhibit both innate and adaptive immunity. As MDSCs are one of the main immunosuppressive factors in breast cancer [4], different therapeutic strategies have been developed to target these cells [5–7]. Preclinical studies using different tumor models [8, 9] have shown a correlation between tumor progression and the numbers of MDSCs. Some publications present conflicting data concerning the effects of TLR agonists on MDSCs [1, 10, 11], however, there is no available information regarding the effect of TLR-3 agonists on MDSC accumulation in the tumor microenvironment. Considering the fact that MDSC levels correlate with clinical breast cancer stage [12, 13], and published reports describe the direct anti-tumor activity of Poly (I: C) on different cell lines [14, 15], we hypothesized that the immune stimulatory effect of Poly (I: C) is mediated through modulation of MDSC function in a murine model of breast cancer. We tested the effect of Poly (I: C) on mice bearing the 4T1 breast cancer cell line. Our results showed a dramatic reduction of absolute numbers of blood and tumor-infiltrating MDSCs and modulation of MDSCs immunosuppressive function.
Materials and methods
Mice
Female BALB/c (age 6–8 weeks) mice were purchased from Jackson laboratories (Bar Harbor, ME) and were housed at the animal research facility of the Winship Cancer Institute. All animal protocols were reviewed and approved by the Institutional Animal Care and Use Committee (IUCAC) Guidelines at the University of Emory (Permit number: A3180-01).
Cell line, tumor inoculation, and treatment
Stably transfected luciferase-expressing 4T1 breast tumor cells were used. The 4T1 mammary carcinoma cell line was maintained as described before [16]. To establish subcutaneous (s.c.) tumors, 1 × 106 cells viable 4T1-Luc cells were injected into 1st left mammary fat pad of female BALB/c mice. Treatment with Poly (I: C) commenced on day 7 after tumor inoculation (when tumors were palpable) at an initial dose of Poly (I: C) of 200 μg/mouse daily for 3 days then 100 μg/mouse beginning on day 10 following tumor inoculation. Control mice were injected with PBS on the same schedule. For in vitro treatment, appropriate amounts of stock solution of Poly (I: C) (200μg in D.W) were added to cell culture media in 24-well plates in serial dilutions to achieve the indicated final concentrations and then incubated with cells for 24 h.
Reagents and antibodies
RPMI 1640, DMEM Hi Glu, FBS, and antibiotics were obtained from Fisher Scientific, Cellgro. Poly (I: C) was purchased from Sigma (St. Louis, MO; lot 27H4009) and dissolved in PBS, and aliquots of 1 mg/ml were preserved at −20° C. The following antibodies were purchased from eBioscience: anti-Gr1 FITC/PE, anti-F4/80 PE/pacific blue, anti Ly6C PE-Cy7, anti Ly6G PE, anti-CD11b APC-Cy7, anti-CD11c APC, anti–CD69 PE-cy7/PE, anti-CD80 PE, anti-CD86 APC, anti SCA-1 PE-Cy7, anti-I-ad PE, anti–CD3 APC, anti-CD4 FITC, anti Apc-Cy7 CD25, anti-CD8 Percp, anti–IFN-γ PE, anti-TNF APC, anti-Granzyme B PE, and isotype antibodies (rat & hamster IgG, IgG2bk, IgG2a isotype control).
Isolation of MDSCs from spleen, blood, and tumors of mice
Mice were euthanized on day 14 and day 21 after tumor inoculation. Harvested tumors were mechanically dissociated into suspensions of individual tumor cells through a 70-μm cellular sieve with a plunger, followed by washing in RPMI medium with 10 % FBS. Cell suspensions were counted and used for flow cytometric analysis or culture. Single cell suspensions of spleen were obtained by mechanical disruption and red cells were removed using ammonium-chloride-potassium chloride lysing buffer. Blood samples were drawn from the tail vein and cheek vein according to IACUC guidelines. Peripheral blood was counted using a Coulter AcT diff Analyzer (Beckman) and analyzed by flow cytometry using lyse no-wash method to maximize the numbers of evaluable leukocytes as we have previously described [16].
Peritoneal cell isolation
Cells were harvested using a published protocol [17]. Briefly 5 ml of ice cold PBS (with 3 % FCS) was injected into the peritoneal cavity of mice using a 27 g hypodermic needle following euthanasia, carefully avoiding contamination with blood and puncturing organs. Collected cells were centrifuged at 1500 rpm for 8 min, counted and stained as described above.
Flow cytometry
For surface staining, single cell suspensions were resuspended in FACS buffer [2 % FBS, 0.1 % NaN3, 2 mM EDTA (ethylene diamine tetra acetic acid) in PBS], lysed and incubated with FCR (CD16/CD32) (2.4G2) (Pharmingen, San Diego, CA) at RT for 10 min to block nonspecific binding of fluorochromes. Staining with relevant Abs directed against surface antigens was performed for 30–45 min on ice. Sytox blue (molecular probes, 100 mM) was used to exclude dead cells in most experiments. The samples were analyzed using a FACS Aria instrument (BD Biosciences, Becton, Dickinson, San Jose, CA), and the data were analyzed using FlowJo software (Tree Star, Ashland, OR). MDSC subunits were counted using the scatter pattern and CD11b positive cells gated for Ly6G and Ly6C for granulocytic MDSCs and monocytic MDSCs and using a high side scatter and F4/80 positive gate for macrophages [16]. For intracellular staining, cells were stained first for surface expression of lineage/differentiation markers (CD80, CD86, SCA-1, I-Ad), then fixed and permeabilized by Cyto Fix/Perm Kit (BD Pharmingen). Identification of Th1 (CD4+, TNF+, IFNγ+) and T CD8+ cytotoxic producing Granzyme was performed following stimulation with plate-bound anti-CD3/CD28 or incubation with PMA and ionomycin. Single cell suspensions of tumor cells and/or spleen were resuspended in media containing 5 pg/ml PMA (sigma-Aldrich) and 5 ng/ml ionomycin (Sigma-Aldrich) or 10 μg/ml purified anti-mouse CD3 plate-bound and 2 μg/ml purified anti-mouse CD28. 1μl/1000 ml Brefeldin A (Golgi plug; BD, San Jose, CA, USA) was added 4–5 h before harvesting for all samples.
Cell sorting
Spleen and tumor suspension were stained with allophycocyanin (APC)-cyanine7 (Cy7)-conjugated anti-CD11b, fluorescein isothiocyanate (FITC)-conjugated Gr-1, and PE-conjugated lineage markers for 20 min at 4 °C and FACS was performed as we have previously described [18].
Bioluminescence imaging (BLI)
4T1 tumor-bearing BALB/c mice were anesthetized with diluted ketamine/xylazine s.c according to Emory IACUC guidelines. Synthetic firefly D-luciferin potassium salt stock solutions (15 mg/ml in PBS) were prepared and injected s.c into anesthetized mice as described [16]. Imaging was performed at two time points in anesthetized mice using an IVIS 100 charge-coupled device imaging system (Xenogen, Alameda, CA, USA). Imaging data were analyzed with Living Image Version 3.2 software. Bioluminescence intensity regions of interest (ROIs) were displayed in photons mode (unit is photons/s), and were compared using the same BLI intensity scale and setting before and after treatment.
Evaluation of reactive oxygen species (ROS) production
Sorted purified CD11b positive, lineage negative splenocytes from tumor-bearing mice were co-cultured with and without Poly (I: C) (20–50 µg/ml) in 24-well plates in culture media. In some experiments, sorted purified splenocytes from tumors recovered from the Poly (I: C)-treated group were co-cultured with and without Poly (I: C) 20μg/ml in culture media. ROS was measured by Cell ROX® Green Reagent (Life Technology). After 24 h, 5μM Cell ROX was added into the culture media and followed by flow cytometry after 30 min incubation at 37 °C. The fluorescence signal was analyzed using the FACS Aria.
Cell protein extraction and Western blot analysis
Cell lysates of sorted purified MDSCs were prepared in 10 X lysis buffer (Cell Signaling Technology). For Western blot analyses, 40-μg samples of protein measured by BCA were subjected to SDS-PAGE on ready to use mini-Protean TGXTM gels (Bio-Rad). Precision-Plus protein kaleidoscope (Bio-Rad) was used as a standard. Separated proteins were transferred onto nitrocellulose membranes by Western blotting. The membranes were blocked with 5 % w/v milk powder in TBST for 1 h at room temperature and probed with primary antibodies against rabbit polyclonal to TLR-3 (1/3000 dilution) (Abcam, MA, US) overnight at 4 °C followed by horseradish peroxidase-conjugated anti-rabbit secondary antibody for 1 h at room temperature (25 °C). Chemiluminescent detection was performed using the substrate Supersignal Westfemto Luminol/Enhancer solution (Thermo scientific). Protein bands of interest were visualized using the ECL detection system followed by exposure to X-ray film.
Statistical analysis
All data are expressed as mean ± standard deviation (SD). Differences between groups were analyzed with Mann–Whitney U test. For survival analyses, Kaplan–Meier analysis by log-rank test was performed. These analyses were performed using GraphPad Prism version 4 (Graph Pad Software, San Diego, CA). Values of p < 0.05 were considered statistically significant.
Results
Suppression of tumor growth correlates with MDSC/tumor-infiltrating lymphocyte (TIL) ratio in tumor microenvironment following Poly (I: C) administration
To investigate the role of Poly (I: C) treatment in controlling tumor growth, we used BALB/c mice bearing luciferase-transfected 4T1 breast cancer cells. 4T1-Luc cells were injected s.c into the 1st left mammary fat pad of BALB/c mice as previously described [16]. Mice were treated with Poly (I: C) or PBS on Days 7 and 10 after tumor cell inoculation, as described in “Materials and methods” section. The day before beginning treatment, mice were imaged (4 mice/group) to establish baseline tumor growth. Mice were then weighed every other day and sacrificed on day 14 (4 days after the second treatment) and imaged to compare with the pre-treatment image (Fig. 1a). Bioluminescence imaging (BLI) revealed a lower tumor burden in the Poly (I: C)-treated group, with 2- to 3-fold greater signal intensity in PBS-treated mice 14 days after tumor cell injection (Fig. 1b, c) (p = 0.012). In line with the greater tumor burden, we found more weight loss in PBS-treated mice compared with Poly (I: C)-treated mice (Fig. 1d) (p = 0.001). Treatment with Poly (I: C) increased overall survival in 4T1-bearing mice, accompanied by a reduction in tumor burden as measured by BLI (Fig. 1e) (p = 0.0217).
Poly (I: C) decreases total flux in parallel with an increase in the myeloid/lymphoid ratio. Groups of BALB/c mice were injected s.c. with 1 × 106 of the 4T1 cell line. a Poly (I: C) was administered by i.p injection on day 7 (200 μg/mouse) and day 10 (100 μg/mouse) after tumor injection of 4T1 cells. b Mice were imaged on day 6 (before treatment) and day 14 (4 days after second injection of Poly (I: C) or PBS). Representative total flux from Poly (I: C)-treated versus PBS-treated mice before and after treatment using the same settings (FOV: 25, binning: medium, f stop: 1, exposure time: 5s). c Total fluxes were assessed by measuring the ROI in tumor-bearing mice after PBS or Poly (I: C) injection. One of three independent experiments is shown. *p < 0.05 (student t test; n = 4 per group). d Percentage of weight loss in both groups. **p < 001. e Treatment with Poly (I: C) increased overall survival (Log-rank (Mantel-Cox) test) *p < 0217
It is well known that both the granulocytic population of CD11b+GR-1+ MDSCs that expresses Ly6G marker and the monocytic phenotype that expresses Ly6C marker have distinct roles in promoting tumor growth. To determine if decreased tumor growth in Poly (I: C)-treated mice was associated with a reduction in tumor-associated MDSC subunits, mice were sacrificed 3 weeks after tumor inoculation (tumor >100 mm3), and analyzed for the quantity of total MDSC subunits in the tumor microenvironment. We found a significant reduction in the numbers of both tumor-infiltrating MDSC subsets (CD11b+Gr-1+, CD11b+, Ly6C+/hi, CD11b+ Ly6G+/hi/int) at two time points (14 and 21 days after tumor inoculation) in Poly (I: C)-treated mice compared with PBS-treated mice). The numbers of Gr-1med CD11b+ cells that express F4/80 (typical of immature macrophages) were significantly decreased after Poly (I: C) treatment compared with that in PBS-treated control mice (Fig. 2a). In line with the decreased frequency of MDSCs and CD11b+Gr-1+ F4/80+ Mϕ in the tumor microenvironment of Poly (I: C)-treated tumor-bearing mice, we found a corresponding increase in the frequency of CD3+ TILs in the tumor microenvironment. In addition, we found a significant correlation between the total flux of tumor and the MDSC/TIL ratio when analyzing different tumor samples (Fig. 2b).
Administration of Poly (I: C) decreases MDSC subunit cell count in tumor-bearing mice compared with PBS-treated tumor-bearing mice. Tumor cells were harvested 3 weeks after tumor inoculation and analyzed for MDSCs. For each sample, flow cytometry analysis was performed as described in “Materials and methods” section. a Representative FACS plots gated on sytox blue (-) cells. Tumor-infiltrating MDSC subsets (CD11b+Gr-1+, CD11b+, Ly6C+/hi, CD11b+ Ly6G+/hi/int) and CD11b+ Gr-1+ F4/80+ macrophages were significantly reduced (3 to 4-fold) after Poly (I: C) treatment compared with control mice. Percentages of designated subsets of CD11b+ Gr-1+/Ly6C+Ly6G+ (left columns from top to bottom) and tumor-associated macrophage (TAM) (CD11b+GR-1+F4/80+) (right columns) in correlation with tumor-infiltrating T cells are shown. b Correlation between total flux and MDSC/TIL ratio from three experiments (Linear regression with best-fit value). Filled square represents Poly (I: C)-treated versus filled circle for PBS-treated mice. Experiments were performed in triplicates. Error bars show mean and SD. (Student t-test; n = 4 per group) p = 0.002; R 2 = 0.7514
Poly (I: C) impacts MDSCs content in peritoneal and BM possibly through TLR3
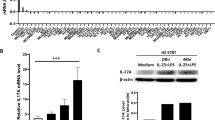
As we and others have previously reported that inoculation with the 4T1 tumor cell line induces expansion of MDSCs in blood [16, 19, 20], we monitored the blood content of MDSCs during tumor growth and after Poly (I: C) treatment. We found that PBS-treated mice had a higher number of CD11b+Gr-1+ cells in the blood compared with Poly (I: C)-treated mice (Supplementary Fig. S1). To test whether the effect of Poly (I: C) on MDSC numbers occurred through direct regulation of MDSC production in the bone marrow, we administered Poly (I: C) once a week for 4 weeks to non-tumor-bearing naïve BALB/c mice and compared immature myeloid cell (IMC) numbers in the bone marrow to age and sex-matched control mice treated with PBS. 24 h after the last injection, peritoneal cells and BM were collected as described in “Materials and methods” section. Our results showed significant reductions in the frequency of CD11b+ GR-1+, Ly6C+ IMCs, and CD11b+ F4/80+ macrophages in the peritoneal fluid of Poly (I: C)-treated non-tumor-bearing mice compared with PBS-treated mice (Fig. 3a). Examination of BM from naïve and tumor-bearing mice showed Poly (I: C) treatment leads to depletion of both IMCs and MDSCs from BM compared with that in PBS-treated control mice (Fig. 3b, c). To demonstrate if the effect of Poly (I: C) is mediated directly through TLR-3 expression on MDSCs, we investigated the expression of TLR-3 in MDSCs. Sorted purified MDSC subunits from splenocytes of B16 tumor bearing mice expressed a high level of TLR3 protein (Fig. 3d).
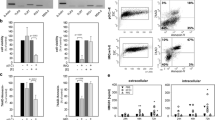
MDSC content in peritoneal cells and BM upon Poly (I: C) administration. Tumor-free mice received Poly (I: C) (200 mg/mice) once a week for 4 weeks. 24 h after the last injection, peritoneal cells were collected as in described in “Materials and methods” section. a Dot plots represent the percentages of IMCs (CD11b+ Gr-1+, Ly6C+) and CD11b+ F4/80+ macrophages in the peritoneal compartment of tumor-free mice. b Comparison of BM-derived IMC and BM-derived MDSC frequencies upon Poly (I: C) treatment. c Graph represents significant difference upon Poly (I: C) treatment for both IMCs and MDSCs; one-way Anova (n = 4 per experiment). One representative example of three individual experiments is shown. d Protein expression of TlR3 by MDSCs. FACS-purified CD11b + Gr-1 + Hi/low cells from the splenocytes of B16-F1 tumor-bearing mice were analyzed for expression of TLR3 following lysis and blotting
Poly (I: C) influences both maturation and suppressive activity of MDSCs
Based upon evidence that Poly (I: C) matures DC [21, 22], we tested whether Poly (I: C) treatment causes maturation of MDSCs in vitro. CD80, CD86, and MHC class II (I-Ad) expression levels were used to evaluate the maturation status of MDSCs [18, 23]. Splenocyte-derived MDSCs from 4T1 tumor-bearing mice were co-cultured with Poly (I: C) (20 μg/ml) overnight. As MDSCs readily lose viability in culture, we used conditioned media from cultured 4T1 cells to increase the survival of sorted MDSCs in culture (data not shown). Our data showed a significant increase in MFI (mean fluorescence index) of maturation markers (MHC II; I-Ad and co-stimulatory molecules CD80 and CD86) on MDSCs following in vitro exposure to Poly (I: C) (Fig. 4a).
Poly (I: C) induces up-regulation of co-stimulatory molecules and modulates suppressive function of MDSCs. Sorted viable CD11b+ lineage negative (CD3, CD4, CD8, Ter119, NK1.1) cells were co-cultured with and without Poly (I: C) for 24 h. a Live-gated CD11b+ FACS-purified splenocyte-derived MDSCs were stained for CD80, CD86, and MHC class II expression. Gray-filled histogram represents staining with an isotype control antibody versus black histogram represents Poly (I: C) treatment. b Sorted purified lineage negative CD11b+ MDSCs were co-cultured with and without Poly (I: C) and ROS measured by flow cytometry. Two-way ANOVA* shows statistically significant differences from control (p < 0.05) from three independent experiments. c Experiments were performed in triplicates. Data represent mean fluorescence index (mean ± SD). d. Sorted tumor-derived MDSCs from 4T1 tumor-bearing mice were cultured in the absence (left) and presence of Poly (I: C) (center) in 96-well plates at a concentration of 2 × 105/mL for 72 h. Cells were harvested and washed with cold staining media and were stained for flow cytometry as described in “Materials and methods” in section. A panel representative of CFSE proliferated cells was analyzed by flow cytometry. SSC side scatter, Lin lineage
In line with the observed maturation, we also measured the effect of Poly (I: C) on the ability of MDSCs to suppress CD4+ T cells through ROS [24]. FACS-purified CD11b+ Gr-1+cells (Fig. 4b) were isolated from the spleens of both PBS- and poly (I: C)-treated groups and co-cultured with and without Poly (I: C). After 24 h, ROS levels in MDSCs from the Poly (I: C)-treated groups were significantly decreased compared with MDSCs from the PBS-treated groups (Fig. 4c). Of note, even when MDSC from Poly (I: C)-treated mice were re-cultured without additional exposure to Poly (I: C), ROS levels remained lower than in PBS-treated mice. We also analyzed the effect of Poly (I: C) on the immunosuppressive activity of MDSCs using proliferation of splenocytes stimulated with anti-CD3/CD28 beads as an in vitro readout, as described [18]. Briefly, (5 × 105) sorted purified splenocyte-derived MDSCs were co-cultured in FBS-supplemented RPMI 1640 in the presence of Poly (I: C) in 24-well flat-bottom plates. Then CFSE-labeled normal spleen cells were stimulated with anti-CD3/CD28 beads for 4–5 days. Our data showed that the addition of Poly (I: C) to co-cultured MDSCs and T cells blocked the ability of MDSCs to inhibit T cell proliferation (Fig. 4d).
Poly (I: C) treatment skews the immune response toward Th1
Since the anti-tumor activity of Th1-polarized T cells expressing IFN-γ and TNF-α is well known [25, 26], we tested whether MDSC levels in the tumor microenvironment correspond with the production of Th1 cytokines by CD4+ T cells [26]. To assess the activation status of CD4+ T cells in our tumor model following Poly (I: C) treatment, T cells were analyzed for cytokine expression. Following in vitro activation with either PMA/ionomycin or plate–bound antibody, CD4+ T cells from the Poly (I: C)-treated group showed an increase in the percentage of TNF-α+/IFN-γ + and CD8+ Granzyme B+ T cells recovered from tumors (Fig. 5a). These data show that the administration of Poly (I: C) to 4T1-tumor-bearing BALB/c mice promotes a Th1 phenotype characterized by IFN-γ and TNF-α up-regulation. In addition, in vitro re-stimulation of splenocytes with anti-CD3/CD28 from the tumor-inoculated and Poly (I: C)-treated group significantly increased the percentage of CD4+ TNF-α+ T cells in the spleen of tumor-bearing mice (Fig. 5b).
Effect of Poly (I: C) treatment on skewing of immune response. Harvested TILs from the tumor at week 3 after tumor inoculation were activated using plate-bound anti-CD3/anti-CD28 or PMA/iono overnight (see “Materials and methods” section). Both groups were analyzed for CD4 + and CD8 + T cell production of IFN-γ, TNFα, and Granzyme B. a Histograms show intracellular expression of TNFα, IFNγ gated on viable CD4 + T cells, and Granzyme B + gated on CD8 + T cells. Experiments were performed in triplicates. b Splenocytes produce more TNF upon treatment. Fresh splenocytes from both groups were cultured and lymphocytes activated with plate-bound anti-CD3/CD28. Histograms represent of TNF-alpha content of activated CD4 + T cells from both groups. Frequency and mean fluorescence index was shown in each graph. Error bars show mean and SD. *p < 0.05, **p < 0.01, (Student t test and two-way ANOVA)
Discussion
Targeting TLR-3 is a promising therapeutic approach for cancer immunotherapy, through direct induction of tumor cell apoptosis leading to improved survival in breast cancer patients [11, 27]. The role of TLR agonists in modulating the immunosuppressive activity of MDSCs in the context of the tumor is controversial. Studies to date have shown that administration of TLR agonists can have direct pro-apoptotic effects on tumors as well as modulating the immunosuppressive activity of tumor-associated MDSCs. In one study, injection of LPS (TLR-4 agonist) and IFN-γ into tumors triggered the generation of immunosuppressive MDSCs and impaired dendritic cell differentiation [28]. The frequent injection of CPG (TLR-9 agonist) led to expansion of MDSCs in tumor-free mice but inhibited the suppressive activity of MDSCs in tumor-bearing mice [1]. Recent published data have shown a suppressive effect of Poly (I: C) on MDSCs in inflammatory conditions [29]. An agonist of TLR-3, Poly (I: C), is currently being tested in human clinical trials as an adjuvant to anti-cancer vaccines and in combination with other therapies [30].
Basic research using animal models of prostate cancer [31] demonstrated that Poly (I: C) treatment reduced tumor volume [32], but the mechanism by which Poly (I: C) limits tumor growth has not been fully explained. Recent published data suggest that Poly (I: C) targets MDSCs, reducing the priming of NK cells, and thus reducing the anti-tumor activity of NK cells against NK-sensitive tumor cells [33]. Thus, since MDSCs are an essential component of the immunosuppressive network induced by tumors [9, 34], we reasoned that Poly (I: C) might stimulate anti-tumor adaptive immunity indirectly by inhibiting the immunosuppressive activity of MDSCs in a murine model of breast cancer. Our data support a new mechanism for the anti-tumor activity of Poly (I: C), namely limiting MDSC generation and MDSC immunosuppressive activity in tumor-bearing mice. Although some data have shown that Poly (I: C) induces a strong anti-tumor response and limited tumor growth in different mouse models [32], direct apoptosis of tumor cells has been considered to be the main mechanism by which Poly (I: C) induces tumor regression [35, 36]. Here we show that treatment with TLR-3 agonist limits MDSC generation and function in tumor-bearing mice. Based upon the effect of Poly (I: C) on MDSC and T cells in vitro, our data are consistent with a mechanism of Poly (I: C) activity by suppression of generation of MDSCs in the BM and accumulation in the tumor microenvironment of 4T1 breast tumor-bearing mice. These new data represent a previously undescribed mechanism of action of Poly (I: C) that supports its use as an adjuvant in future cancer immunotherapy approaches. Contrary to previous reports based on in vitro data [37], our data indicate that MDSC infiltration into the tumor is suppressed by Poly (I: C) in tumor-bearing mice possibly through inhibition of the generation of IMCs in the BM. The decrease in the quantity of MDSCs was paralleled by a significant increase in TILs that produced TNFα, IFN-γ, and Granzyme B. Poly (I: C) treatment also regulated the maturation status of MDSCs, making them more effective in antigen presentation through up-regulation of MHC class II, CD80, and CD86. Decreased numbers of MDSCs in the tumor were accompanied by skewing of cellular anti-tumor immune response toward Th1 in Poly (I: C)-treated mice compared with PBS-treated mice.
Taken together, the data presented here are consistent with two hypotheses for the immunostimulatory activity of Poly (I: C). First is a direct effect of Poly (I: C) on MDSC through TLR-3. Further experiments are needed to confirm the immunostimulatory activity of Poly (I: C) through direct binding of MDSCs using transgenic animals with TLR3 knocked out. A second hypothesis is that Poly (I: C) affects MDSC number and function indirectly by targeting 4T1 tumor cells and reducing tumor burden, thereby causing a decrease in circulating and infiltrating MDSCs and an increase in T cell infiltration.
Based on the data presented here, the cancer immunomodulatory activity of Poly (I: C) may be considered to be mediated by a direct apoptotic effect on tumor cell lines as previously described [3, 6] and an indirect effect through the modulation of MDSC number and function. Considering the role of MDSCs in breast cancer promotion [38] and the possible effect of Poly (I: C) on MDSCs through TLR-3-mediated signaling, this research supports the potential value of Poly (I: C) in breast cancer immunotherapy. Taken together, our results provide further evidence that Poly (I: C) is effective as a potent immune-stimulatory adjuvant that may affect the tumor microenvironment by MDSC modulation.
Abbreviations
- MDSC:
-
Myeloid-derived suppressor cells
- S.C:
-
Subcutaneous
- I.P:
-
Intra peritoneal
- BLI:
-
Bioluminescence intensity
- ROI:
-
Regions of interest
- Luc:
-
Luciferase
- Lin:
-
Lineage
- FACS:
-
Fluorescent activated cell sorting
- IMC:
-
Immature myeloid cell
References
Zoglmeier C, Bauer H, Norenberg D, Wedekind G, Bittner P, Sandholzer N, Rapp M, Anz D, Endres S, Bourquin C (2011) CpG blocks immunosuppression by myeloid-derived suppressor cells in tumor-bearing mice. Clin Cancer Res 17(7):1765–1775
Finke J (2011) MDSC as a mechanism of tumor escape from sunitinib mediated anti-angiogenic. Inter Immunopharmacol 11:856
Nakamura H, Horai Y, Suzuki T, Okada A, Ichinose K, Yamasaki S, Koji T, Kawakami A (2013) TLR3-mediated apoptosis and activation of phosphorylated Akt in the salivary gland epithelial cells of primary Sjogren’s syndrome patients. Rheumatol Int 33(2):441–450
Markowitz J, Wesolowski R, Papenfuss T, Brooks TR, Carson WE 3rd (2013) Myeloid-derived suppressor cells in breast cancer. Breast Cancer Res Treat 140(1):13–21
Harashima N, Inao T, Imamura R, Okano S, Suda T, Harada M (2012) Roles of the PI3 K/Akt pathway and autophagy in TLR3 signaling-induced apoptosis and growth arrest of human prostate cancer cells. Cancer Immunol Immunother 61(5):667–676
Sun R, Zhang Y, Lv Q, Liu B, Jin M, Zhang W, He Q, Deng M, Liu X, Li G et al (2011) Toll-like receptor 3 (TLR3) induces apoptosis via death receptors and mitochondria by up-regulating the transactivating p63 isoform alpha (TAP63alpha). J Biol Chem 286(18):15918–15928
Taura M, Fukuda R, Suico MA, Eguma A, Koga T, Shuto T, Sato T, Morino-Koga S, Kai H (2010) TLR3 induction by anticancer drugs potentiates poly I:C-induced tumor cell apoptosis. Cancer Sci 101(7):1610–1617
Liechtenstein T, Perez-Janices N, Gato M, Caliendo F, Kochan G, Blanco-Luquin I, Van der Jeught K, Arce F, Guerrero-Setas D, Fernandez-Irigoyen J et al (2014) A highly efficient tumor-infiltrating MDSC differentiation system for discovery of anti-neoplastic targets, which circumvents the need for tumor establishment in mice. Oncotarget 5(17):7843–7857
Ghansah T (2012) A novel strategy for modulation of MDSC to enhance cancer immunotherapy. Oncoimmunology 1(6):984–985
Mignot G, Chalmin F, Ladoire S, Rébé C, Ghiringhelli F (2011) Tumor exosome-mediated MDSC activation. Am J pathol 178(3):1403–1405
Green TL, Santos MF, Ejaeidi AA, Craft BS, Lewis RE, Cruse JM (2014) Toll-like receptor (TLR) expression of immune system cells from metastatic breast cancer patients with circulating tumor cells. Exp Mol Pathol 97(1):44–48
Diaz-Montero CM, Salem ML, Nishimura MI, Garrett-Mayer E, Cole DJ, Montero AJ (2009) Increased circulating myeloid-derived suppressor cells correlate with clinical cancer stage, metastatic tumor burden, and doxorubicin-cyclophosphamide chemotherapy. Cancer Immunol Immunother 58(1):49–59
Chi N, Tan Z, Ma K, Bao L, Yun Z (2014) Increased circulating myeloid-derived suppressor cells correlate with cancer stages, interleukin-8 and -6 in prostate cancer. Int J Clin Exp Med 7(10):3181–3192
Salaun B, Coste I, Rissoan MC, Lebecque SJ, Renno T (2006) TLR3 can directly trigger apoptosis in human cancer cells. J Immunol 176(8):4894–4901
Cheng YS, Xu F (2010) Anticancer function of polyinosinic-polycytidylic acid. Cancer Biol Ther 10(12):1219–1223
Forghani P, Khorramizadeh MR, Waller EK (2014) Silibinin inhibits accumulation of myeloid-derived suppressor cells and tumor growth of murine breast cancer. Cancer Med 3(2):215–224
Ray A, Dittel BN (2010) Isolation of mouse peritoneal cavity cells. J Vis Exp 35:1488
Forghani P, Harris W, Giver CR, Mirshafiey A, Galipeau J, Waller EK (2013) Properties of immature myeloid progenitors with nitric-oxide-dependent immunosuppressive activity isolated from bone marrow of tumor-free mice. PLoS ONE 8(7):e64837
Ostrand-Rosenberg S, Sinha P, Chornoguz O, Ecker C (2012) Regulating the suppressors: apoptosis and inflammation govern the survival of tumor-induced myeloid-derived suppressor cells (MDSC). Cancer Immunol Immunother 61(8):1319–1325
Sinha P, Okoro C, Foell D, Freeze HH, Ostrand-Rosenberg S, Srikrishna G (2008) Proinflammatory S100 proteins regulate the accumulation of myeloid-derived suppressor cells. J Immunol 181(7):4666–4675
Fucikova J, Rozkova D, Ulcova H, Budinsky V, Sochorova K, Pokorna K, Bartunkova J, Spisek R (2011) Poly I: C-activated dendritic cells that were generated in Cell Gro for use in cancer immunotherapy trials. J Trans Med 9:223
Verdijk RM, Mutis T, Esendam B, Kamp J, Melief CJ, Brand A, Goulmy E (1999) Polyriboinosinic polyribocytidylic acid (poly(I:C)) induces stable maturation of functionally active human dendritic cells. J Immunol 163(1):57–61
Moller I, Michel K, Frech N, Burger M, Pfeifer D, Frommolt P, Veelken H, Thomas-Kaskel AK (2008) Dendritic cell maturation with poly(I:C)-based versus PGE2-based cytokine combinations results in differential functional characteristics relevant to clinical application. J Immunother 31(5):506–519
Nagaraj S, Nelson A, Youn JI, Cheng P, Quiceno D, Gabrilovich DI (2012) Antigen-specific CD4(+) T cells regulate function of myeloid-derived suppressor cells in cancer via retrograde MHC class II signaling. Cancer Res 72(4):928–938
Kulbe H, Thompson R, Wilson JL, Robinson S, Hagemann T, Fatah R, Gould D, Ayhan A, Balkwill F (2007) The inflammatory cytokine tumor necrosis factor-alpha generates an autocrine tumor-promoting network in epithelial ovarian cancer cells. Cancer Res 67(2):585–592
Charles KA, Kulbe H, Soper R, Escorcio-Correia M, Lawrence T, Schultheis A, Chakravarty P, Thompson RG, Kollias G, Smyth JF et al (2009) The tumor-promoting actions of TNF-alpha involve TNFR1 and IL-17 in ovarian cancer in mice and humans. J Clin Invest 119(10):3011–3023
Salaun B, Zitvogel L, Asselin-Paturel C, Morel Y, Chemin K, Dubois C, Massacrier C, Conforti R, Chenard MP, Sabourin JC et al (2011) TLR3 as a biomarker for the therapeutic efficacy of double-stranded RNA in breast cancer. Cancer Res 71(5):1607–1614
Bunt SK, Clements VK, Hanson EM, Sinha P, Ostrand-Rosenberg S (2009) Inflammation enhances myeloid-derived suppressor cell cross-talk by signaling through Toll-like receptor 4. J Leukoc Biol 85(6):996–1004
Conrad E, Resch TK, Gogesch P, Kalinke U, Bechmann I, Bogdan C, Waibler Z (2014) Protection against RNA-induced liver damage by myeloid cells requires type I interferon and IL-1 receptor antagonist in mice. Hepatology 59(4):1555–1563
Aranda F, Llopiz D, Diaz-Valdes N, Riezu-Boj JI, Bezunartea J, Ruiz M, Martinez M, Durantez M, Mansilla C, Prieto J et al (2011) Adjuvant combination and antigen targeting as a strategy to induce polyfunctional and high-avidity T-cell responses against poorly immunogenic tumors. Cancer Res 71(9):3214–3224
Paone A, Starace D, Galli R, Padula F, De Cesaris P, Filippini A, Ziparo E, Riccioli A (2008) Toll-like receptor 3 triggers apoptosis of human prostate cancer cells through a PKC-alpha-dependent mechanism. Carcinogenesis 29(7):1334–1342
Forte G, Rega A, Morello S, Luciano A, Arra C, Pinto A, Sorrentino R (2012) Polyinosinic-polycytidylic acid limits tumor outgrowth in a mouse model of metastatic lung cancer. J Immunol 188(11):5357–5364
Shime H, Kojima A, Maruyama A, Saito Y, Oshiumi H, Matsumoto M, Seya T (2014) Myeloid-derived suppressor cells confer tumor-suppressive functions on natural killer cells via polyinosinic:polycytidylic acid treatment in mouse tumor models. J Innate Immun 6(3):293–305
Ostrand-Rosenberg S, Sinha P, Beury DW, Clements VK (2012) Cross-talk between myeloid-derived suppressor cells (MDSC), macrophages, and dendritic cells enhances tumor-induced immune suppression. Semin Cancer Biol 22(4):275–281
Dalotto-Moreno T, Croci DO, Cerliani JP, Martinez-Allo VC, Dergan-Dylon S, Mendez-Huergo SP, Stupirski JC, Mazal D, Osinaga E, Toscano MA et al (2013) Targeting galectin-1 overcomes breast cancer-associated immunosuppression and prevents metastatic disease. Cancer Res 73(3):1107–1117
Kovacs-Solyom F, Blasko A, Fajka-Boja R, Katona RL, Vegh L, Novak J, Szebeni GJ, Krenacs L, Uher F, Tubak V et al (2010) Mechanism of tumor cell-induced T-cell apoptosis mediated by galectin-1. Immunol Lett 127(2):108–118
Liu C, Zhang C, Lu H, Cai J, Wang Z, Chen J, Liu F, Wu Z, Liu X, Sun W (2011) Poly(I:C) induce bone marrow precursor cells into myeloid-derived suppressor cells. Mol Cell Biochem 358(1–2):317–323
Danilin S, Merkel AR, Johnson JR, Johnson RW, Edwards JR, Sterling JA (2012) Myeloid-derived suppressor cells expand during breast cancer progression and promote tumor-induced bone destruction. Oncoimmunology 1(9):1484–1494
Acknowledgments
The authors thank Dr. Ragavan Chinnadurai for his guidance; Wayne Harris for his helpful technical assistance in sorting and Christopher Peterson for help in Western blotting. Also author thanks Anthea Hamond for her careful reading and editing of manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors disclose no potential conflicts of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
10549_2015_3508_MOESM1_ESM.tif
Figure. S1. Poly (I: C) treatment decreases the frequency and absolute numbers of MDSCs 4T1 tumor cells were implanted into the 1st left mammary fat pad of female BALB/c mice (1 × 106 cells per mouse, n = 4 per group). Blood samples were obtained on week three after tumor inoculation. (A) Flow cytometry analysis of blood showing mean percentages of MDSCs and CD3+ T cells in Poly (I: C)-treated and PBS-treated tumor-bearing mice vs. non-tumor bearing Poly (I: C)-treated mice. Mean frequencies (±SD) from three separate experiments. (B) Absolute numbers of MDSCs and CD3+ T cells in the blood after tumor inoculation in two groups. Two-way ANOVA* shows statistically significant differences from control (p < 0.05) from three independent experiments.
Rights and permissions
About this article
Cite this article
Forghani, P., Waller, E.K. Poly (I: C) modulates the immunosuppressive activity of myeloid-derived suppressor cells in a murine model of breast cancer. Breast Cancer Res Treat 153, 21–30 (2015). https://doi.org/10.1007/s10549-015-3508-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-015-3508-y