Abstract
Since the worldwide approval of lithium therapy in 1970, lithium has been used for its anti-manic, antidepressant, and anti-suicidal effects. The last decade has witnessed the following discoveries about its neuroprotective and neurotrophic properties, yet the therapeutic mechanisms at the cellular level remain not-fully defined. We have undertaken the present study to determine if chronic lithium treatment, at therapeutically relevant concentrations, exerts neurotrophic/neuroprotective effects in the mouse brain in vivo. For this purpose, 10 months aged mice were fed for 3 months on food pellets contained 1 g (L1 group) or 2 g (L2 group) lithium carbonate/kg, resulting in serum concentrations of 0.4 and 0.8 mM, respectively. The evaluation of lipid peroxidation level and the activities of catalase, superoxide-dismutase and glutathione-peroxidase showed that chronic Li administration, at therapeutic doses doesn’t induce oxidative stress in brain tissue. No changes in the expression levels of molecular chaperones, namely, the HSP70, and HSP90 heat shock proteins and the GRP94 glucose-regulated protein were detected. Moreover, this treatment has caused (1) an increase in the relative brain weight (2) a delay in the age induced cerebral glucose impairment (3) an enhancement of the neurogenesis in hippocampus and enthorinal cortex highlighted by silver impregnation. Under these experimental conditions, no modifications were observed in expression levels of GSK3 and of its downstream target β-catenin proteins. These results suggested that chronic Li administration, at therapeutic doses, has a neuroprotective/neurotrophic properties and its therapeutic mechanism doesn’t implicate GSK3 inactivation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lithium was introduced into psychiatry almost half a century ago and remains the most important drug for the treatment and prophylaxis of mania and depression (Goodwin and Jamison 1990; Birch 1991; Post et al. 1992).
Accumulating studies have suggested that lithium is a neuroprotective agent against diverse insults (Nonaka and Chuang 1998). Indeed, increasing evidence suggests that lithium can be used in the treatment of acute brain injuries (e.g., ischemia) and chronic neurodegenerative diseases (e.g., Alzheimer’s disease) (Wada et al. 2005a, b); the downstream mediator molecules of lithium’s effects have been increasingly elucidated, ranging from up-regulation of cell survival molecules (e.g., brain-derived neurotrophic factor and vascular endothelial growth factor) to down regulation of pro-apoptotic activities (e.g., excitotoxicity) (Quiroz et al. 2004; Wada et al. 2005a, b; Marmol 2008). Furthermore, lithium may protect against the cerebral atrophy and neuronal degeneration induced by the neurochemical processes and pathways known to regulate cell death and atrophy after an ischemic event. Lithium-mediated neuroprotective and neurotrophic effects involve mechanisms highly relevant to the post-stroke population including the increased expression of brain-derived neurotrophic factor (BDNF) and Bcl-2, and inhibition of GSK-3β. Lithium-induced increases in human gray matter have been reported and occur within a time frame consistent with the known effects of lithium through increased expression of BDNF, Bcl-2 and GSK-3β inhibition.
Lithium is used in the human therapy in the form of salts, especially the carbonate (Li2CO3) and acetate (LiCH3COO) (Hal and Angelica 2008). The serum (blood) level under therapeutic lithium treatment should not exceed 11.1 mM lithium and must be carefully monitored. Nevertheless, patients on long-term lithium treatment may suffer from severe neurotoxic effects while serum lithium concentrations are normal (Stern 1995).
The combination of the increased use of lithium and its extremely narrow therapeutic window enhances the potential for increased toxicity. The therapeutic serum concentrations are normally about 5.6–8.4 mM (Jaeger 2003).
In a previous study, we have shown that, although its neuroprotective effects, lithium administration by a daily intraperitoneal injection for one month led to transitory and repeated peaks in serum lithium concentrations (of about 1.1 mM) able to generate an oxidative stress and a renal insufficiency (Nciri et al. 2008, 2009). More recently (Nciri et al. 2010), in an attempt to avoid these cyclic variations, lithium was given orally mixed with the food. As therapeutic effects of lithium in man require long-term treatment, mice were treated for more than 3 months with 1 or 2 g of lithium carbonate/kg of food that generated serum lithium concentrations close to therapeutic relevant concentrations in man. This treatment did not led to significant renal insufficiency or oxidative stress which suggests that these treatment conditions are favourable for further research on the lithium neuroprotective properties. Indeed, the present study was designed to determine these properties. Neurotrophic effects were verified by monitoring relative brain weight and brain glucose level. Importance of the oxidative stress was evaluated by measuring in brain tissue the level of lipid peroxidation (TBARS) and activities of catalase (CAT), superoxide-dismutase (SOD) and glutathione-peroxidase (GPX). Expression levels of molecular chaperones, namely, the HSP70 and HSP90 heat shock proteins and the GRP94 glucose-regulated protein were investigated.
In order to define molecular mechanisms underlying lithium action, expression and activity changes of glycogen synthase kinase-3 (GSK-3) were analysed using the measurement of expression levels of both proteins: GSK-3 and its downstream target β-catenin.
Materials and methods
Chemicals reagents
Monoclonal mouse antibodies against HSP72/73 (SPA 820) and against HSP90 (SPA 830), and monoclonal rat antibody against GRP94 (SPA 850) were purchased from StressGen Biotechnologies (Victoria, BC, Canada). Monoclonal mouse antibodies against GSK3 αβ (sc-7291) was purchased from Santa Cruz Biotechnology (Bergheimer, Germany) and monoclonal mouse antibodies against β-catenin was from Sigma-Aldrich. Anti-mouse and anti-rat peroxidase-conjugated antibodies and proteases inhibitors: phenylmethanesulfonyl fluoride (PMSF), N-ethylmaleimide (NEM) and aprotinin were purchased from Sigma-Aldrich (Saint Quentin, France). SuperSignal® West Pico chemiluminescent substrate was from Pierce Biotechnology (USA).
Animals and experimental protocols
Forty-eight Wistar male mice, 10 months old, about 32 g body weight, fed on 15% proteins food pellets (SICO, Sfax, Tunisia) and given normal tap water ad libitum were kept in a breeding farm, at 22°C with a stable hygrometry, under constant photoperiod. Animals were divided into three groups: a control group (C) receiving normal food pellets and two lithium-treated groups, namely, the (L1) group given food pellets containing 1 g lithium carbonate/kg and the (L2) group given food pellets containing 2 g lithium carbonate/kg. After 1 and 3 months, eight animals from each group were sacrificed by rapid decapitation. Blood was collected without anticoagulant, centrifuged (2,000*g) and the collected serum was used for the determination of lithium concentrations. Brains were removed, the weight/body weight ratio × 100 was calculated and expressed as relative organ weight. The organ was then stored at −80°C.
The study was approved by the local ethical committee for animal experimentations at the Sfax University.
Preparation of tissue extracts
About 0.5 g of brain was homogenized in 1 ml NP40-PBS buffer, pH 7.4, containing 0.5% Nonidet P-40, and protease inhibitors (10 mM EDTA, 2 mM PMSF, 5 mM NEM, 4 μg/ml of aprotinin,), then centrifuged for 30 min at 15,000 g at 4°C. The supernatants were stored at −80°C. Protein content concentrations were measured using the Lowry’s method (Lowry et al. 1951).
Biochemical determinations
Serum lithium concentrations were measured by atomic absorption with a flame spectrophotometer (Analyst 400, Perkin-Elmer).
Cerebral glucose was assayed by glucose-oxidase, using a commercial kit (Biomaghreb, Tunisia).
Lipid peroxidation level was evaluated as the amount of ThioBarbituric Acid Reactive Substances (TBARS) as described by Esterbauer (1993). Briefly, 125 μl of supernatant from tissue homogenate were mixed with 125 μl 20% trichloroacetic acid containing 1% butyl-hydroxytoluene in order to precipitate proteins. After centrifugation (1,000*g, 10 min at 4°C), 200 μl of supernatant were mixed with 40 μl 0.6 N HCl and 160 μl of 120 mM thiobarbituric acid in 25 mM Tris buffer (pH 7.4). The mixture was heated at 80°C for 10 min and the optical density of the solution was measured at 530 nm. TBARS concentration was calculated using an extinction coefficient of 156 mM−1 cm−1.
Catalase (CAT) activity was determined at 25°C according to Aebi (1984) by measuring the decrease of H2O2 absorbance at 240 nm for 1 min. Activity was calculated by using an extinction coefficient of 0.043 mM−1 cm−1 and expressed as μmol of H2O2 destroyed/min/mg of protein.
Total (Cu–Zn and Mn) superoxide-dismutase (SOD) activity was determined at 25°C by measuring its ability to inhibit the photoreduction of nitroblue tetrazolium (NBT) into blue formazan (Sun et al. 1988; Durak et al. 1993). The assay was performed in 50 mM PBS (phosphate-buffered saline) (pH 7.4) containing 13 mM methionine, 0.1 mM EDTA, 2 μM riboflavin and 75 μM NBT. Activity was expressed as units/mg protein, one unit being the amount inhibiting the photoreduction of NBT by 50%.
Glutathione-peroxidase (GPX) activity was assayed at 25°C according to Flohe and Gunzler (1984) with some modifications. Activity was measured in 250 μl tissue extract mixed with GSH (final concentration: 0.35 mmol/l). Reaction was started with the addition of H2O2 (0.2 mmol/l). After the reaction was stopped, 5,5′-dithiobis-2-nitrobenzoic acid (DTNB) was added and the absorbance was recorded at 412 nm. The activity was expressed as μmol of GSH oxidized/min/g protein.
Western blot analysis of stress proteins expression
Known amounts of protein per lane (either 20 or 40 μg) from each homogenate were submitted to electrophoresis on 10% SDS-PAGE, and then transferred onto 0.45 μm-pores nitrocellulose membranes. In order to avoid the unspecific binding of antibodies to the nitrocellulose, the membranes were incubated for 1 h at 37°C into a Tris-buffered saline (TBS: 10 mM Tris, 140 mM NaCl, pH 7.4) containing 0.1% Tween 20 (TBST) and 3% non-fatty milk powder. The membranes were then incubated overnight at 4°C in TBST containing the primary antibodies, i.e., anti-HSP72/73, anti-HSP90, anti-GRP94, Anti-GSK-3 and anti β-catenin diluted, respectively, to 1/40,000; 1/40,000; 1/30,000; 1/40,000 and 1/20,000. After washing, blots were incubated for 2 h, in TBST containing 3% dried skimmed milk and peroxidase-conjugated secondary antibodies diluted to 1/80,000 for anti-mouse IgG and 1/30,000 for anti-rat IgG. After washing, immunoreactive bands were detected using the ECL-enhanced chemiluminescence system (Amersham International, UK) and Bio Max light-1 film (Kodak).
Histological analysis
After fixation in Bouin solution, pieces of fixed tissue were embedded into paraffin and cut into 5 μm slices. The sections were stained with Luxol Fast Blue for staining of myelin combined with Bodian for staining of axons.
Statistical analysis
Data were expressed as mean ± standard error to the mean (SEM). Statistical significance was assessed by Student’s t-test. P ≤ 0.05 was considered statistically significant.
Results
Serum lithium concentration
Lithium carbonate treatment at the doses of 1 or 2 g lithium carbonate/kg of food led to serum lithium concentrations in the range of therapeutic values in human reaching, respectively, 0.3 and 0.75 mM after 1 month and 0.42 and 0.8 mM after 3 months of treatment.
Level of lipid peroxidation and antioxidant enzymes activities in brain
Lipid peroxidation levels in brain of lithium-treated mice expressed as TBARS concentrations were not significantly changed compared to controls (Table 1). Besides, no significant variation in activities of CAT, SOD, and GPX was observed during this treatment.
Changes in expression pattern of stress proteins
As shown in Fig. 1 which represents western blots from brain, the anti-HSP70s antibody revealed one band of 73 kDa corresponding to constitutive form of HSP70 protein. The anti-HSP90 revealed a band of about 90 kDa and GRP94 appeared as a single 98 kDa protein band. All the proteins presented in this immunoblot have the same apparent band intensity which suggests that no significant changes in the expression levels of HSP70, HSP90 and GRP94 were observed in brains of control and Li-treated mice.
Immunoblot showing stress protein expression detected with anti-GRP94, anti-HSP90 and anti-HSP70 s antibodies, in brain NP40 extracts from control (C) or lithium treated (L1, L2) mice for 1 and 3 months. Equal amounts of protein (20 μg) were resolved by SDS-PAGE on 10% polyacrylamide gels. There were four mice by experimental condition. Two different blots were performed for each extract and results were pooled
Relative brain weight
A one or a three months treatment with Li2CO3 caused a significant increase in the relative brain weight of the L2 mice (0.75–0.8 mM lithium concentration) compared to controls (C) (P ≤ 0.001), (Fig. 2). However, in the case of L1 mice (0.3–0.42 mM lithium concentration), this increase was not significant in both treatment stages.
Cerebral glucose concentration
As shown in Fig. 3, the cerebral glucose concentration has been decreased in control mice in age related manner. In fact, this concentration has decreased from 0.5 mM for 11 months mice age to reach 0.27 mM when mice have 13 months of age. Besides, lithium carbonate treatment seems to delay glucose impairment in treated mice brains. For example, after 3 months of treatment, cerebral glucose concentrations increased by 115% and 70% compared to C in L1 and L2, respectively.
Histological changes in hippocampus and enthorinal cortex
The examination of histological slides performed on the CA3 (Cornu Ammonis 3) area of hippocampus stained with combined Bodian luxol fast blue colorations has shown an increase of axon diameters and an enhancement of neurites growth in L2 mice compared to C after 3 months of treatment (Fig. 4).
The same staining method used with enthorinal cortex in 3 months treated L2 mice has demonstrated an increase of the myelination density which suggests an enhancement of the neuron network (Fig. 5).
These findings reflect the stimulation of neurogenesis under Li treatment.
Changes in expression of GSK3 protein
The expression levels of the GSK3 αβ in brain of the control (C) and the lithium treated mice (L1, L2) during 1 and 3 months are presented on immunoblot (Fig. 6). The GSK3 α is presented in the form of one band at 51 kDa. Whereas, the GSK3β appeared under two isoforms of 46 and 47 kDa.
Immunoblot showing GSK-3 protein expression in brain NP40-extracts from control (C) or lithium-treated (L1, L2) mice for 1 and 3 months. Equal amounts of protein (20 μg) were resolved by SDS-PAGE on 10% polyacrylamide gels. There were four mice by experimental condition. Two different blots were performed for each extract and results were pooled
No modification of GSK3 protein expression was observed in the brains of Li treated mice (L1, L2) compared to the control (C) after 1 and 3 months of treatment.
Changes in expression of phosphorylated β-catenin protein
β-Catenin is a 94–97 kDa protein regulated by GSK3. GSK-3 is constitutively active in unstimulated cells where it phosphorylates beta-catenin, targeting beta-catenin for rapid degradation. In order to evaluate the effect of lithium on the GSK3 activity, we have examined the expression level of the phosphorylated form of β-catenin protein quantified with antibody which recognized phosphorylated forms in serine 33 and 37.
As shown in Fig. 7, β-catenin (92–97 kDa) was under expressed which suggests that it was little phosphorylated. However, the antibody has immunodetected two major bands of about 45 and 55 kDa corresponding to the β-catenin cleavage products. The expression levels of these phosphorylated forms were comparable between controls (C) and Li treated mice.
Immunoblot showing β-catenin protein expression in brain NP40-extracts from control (C) or lithium-treated (L1, L2) mice for 1 and 3 months. Equal amounts of protein (20 μg) were resolved by SDS-PAGE on 10% polyacrylamide gels. There were four mice by experimental condition. Two different blots were performed for each extract and results were pooled
Discussion
This study was undertaken to evaluate the neuroprotective/neurotrophic effects of chronic lithium administration in mice brain.
Addition of 1 or 2 g of lithium carbonate/kg of food led to lithium serum concentrations reaching, respectively, 0.3 or 0.75 mM after 1 month and 0.42 or 0.8 mM after 3 months, which is in the range of therapeutic doses used in humans.
In previous studies, we have reported that the obtained serum lithium concentrations did not led to significant renal insufficiency or oxidative stress in liver and kidney tissues. This suggests that these treatment conditions are favourable for further research on the lithium neuroprotective properties (Nciri et al. 2010).
In this work, our results have shown that long term lithium carbonate treatment, at therapeutically relevant concentrations, did not induce significant changes in lipid peroxidation (TBARS) level and antioxidant enzymatic activities (CAT, SOD, GPX) Which suggests that Li treatment, in our conditions, hasn’t created toxicity in brains of treated mice. This may be necessary for the neuroprotective effects of this medication. In accordance, we reported previously that, by contrast to kidney and liver, no oxidative stress was observed in brain of mice injected daily by 20, 40, or 80 mg of lithium carbonate per kilogram of body weight for 14 or 28 days (Nciri et al. 2008).
It has been documented that stress proteins were implicated in the beneficial effects of lithium (Hiroi et al. 2005; Ren et al. 2003; Allagui et al. 2009). For that, we have evaluated the expression levels of HSP70, HSP90, and GRP94 in brain extracts of control and treated mice.
No significant changes in the expression levels of these proteins were observed in brains of treated mice compared to control. These results were different from those reported by Xu et al. (2006) which demonstrated that rats pretreatment with a subcutaneous injection of lithium for 2 days enhances neuroprotection by the up-regulation of cytoprotective heat shock proteins HSP70 and GRP78 in the ischemic brain hemisphere. Therefore, the absence of stress proteins induction in our experimental conditions could be explained by the length of treatment (1 and 3 months) and doses of lithium that we have used (0.4–0.8 mM).
Another finding from our research is that the relative brain weight was increased following lithium carbonate treatment in particular in L2 mice having 0.75 and 0.8 mM lithium serum concentration after 1 and 3 months of treatment, respectively, which is in the range of therapeutic doses used in humans. In this context, Manji et al. (2000b) have reported that Brain gray matter volume is significantly increased following 4 weeks of lithium administration at therapeutic levels in manic-depressive illness patients. In agreement with these observations, several lines of clinical evidence suggest that lithium has neurotrophic actions. For example chronic lithium treatment increases the volume of gray matter and the content of N-acetyl-aspartate, a cell survival marker, in bipolar mood disorder patients (Lyoo et al. 2010). Moreover, treatment with this mood-stabilizer suppresses the decrease in the volume of the subgenual pre-frontal cortex found in bipolar patients (Drevets 2001).
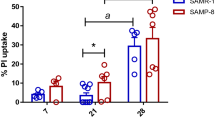
In our results, an increase in the cerebral glucose concentrations of treated mice has also been shown. This suggests an enhancement of glucose uptake and could explain the delay of cerebral glucose impairement in treated mice compared to the controls. These findings are in favour of a neurotrophic effect of long term lithium treatment. Thereby, glucose is the primary source of the energy required for brain activity and it has been strongly implicated in the pathogenesis of a variety of neurodegenerative diseases. In fact, glucose uptake and metabolism are impaired in Alzheimer disease brain and the reduction of cerebral glucose metabolism provides the earliest evidence of an ongoing neurodegenerative disease process (Hoyer 2004; Hunt et al. 2007).
Plenge (1976) has reported that lithium induces increase in brain glucose uptake and stimulates glycolysis. More recently, we have also found that lithium exerts its neuroprotective effect by the enhancement of glucose uptake and glycolysis in SH-SY5Y cells exposed chronically (more than 10 months) to low lithium carbonate dose (0.5 mM) (Nciri et al. in preparation).
The increase of brain weight and the enhancement of cerebral glucose uptake in treated mice suggest that chronic lithium may not only exert robust neuroprotective effects (as has been demonstrated in a variety of preclinical studies), but also exerts neurotrophic effects. In this context, Moore et al. (2000) have found that chronic lithium treatment (4 weeks), at therapeutically relevant concentration (0.8 mM), increases neuronal viability/function in the human brain in vivo, as evidenced by increased central nervous system (CNS) levels of N-acetyl-aspartate in both medication-free bipolar disorder patients and healthy subjects.
Consistent with the robust increases in bcl-2 levels, lithium has been shown to protect neurons from the deleterious effects of a variety of insults both in vitro and in vivo. In fact, chronic (4-week) lithium administration robustly increases the levels of the neuroprotective protein bcl-2 in rat frontal cortex (Chen et al. 1999), in hippocampus and striatum of rodent and human as well as neuronal cells in culture (Chen and Chuang 1999; Manji et al. 1999).
It has been clearly demonstrated that not only does bcl-2 overexpression protect against apoptotic and certain types of necrotic cell death, it can also promote regeneration of axons in the mammalian CNS, leading to the intriguing postulate that bcl-2 acts as a major regulatory switch for a genetic program that controls the growth of CNS axons (Chen et al. 1997).
Lithium has also been reported to stimulate hippocampal neurogenesis in adult rodents (Chen et al. 2000) and is associated with the increase of bcl-2 expression (Manji et al. 2000a). Limbic structures (enthorinal cortex, hippocampus, and amygdala) are essential for the cognitive processes and emotional behavior (Bertrand et al. 2003). The hippocampus is a key component of frontotemporal neural networks involved in memory (McKinnon et al. 2007) and is susceptible to a wide variety of neurologic diseases, including hypoxia–ischemia, epilepsy, Alzheimer disease, or schizophrenia (Insausti and Amaral 2004).
Our results showed that 0.8 mM lithium was able to enhance neurogenesis in hippocampus and enthorinal cortex of L2 mice after 3 months of treatment. This was highlighted by the increase of axon diameters and the enhancement of neurites growth in CA3 area of hippocampus. Furthermore, neuron network was enriched in enthorinal cortex. This enrichment was proved by the increase of myelination density.
The role of lithium as an important agent in neuroprotection and neurogenesis has been documented in human and in animal studies. For example, Chen et al. (2000) demonstrated enhancement of hippocampus neurogenesis in the dentate gyri of Li-treated mice. In a more recent study, Frey et al. (2006) reported that Li increased hippocampus brain-derived neurotrophic factor (BDNF) levels in an animal model of mania. The hippocampus has been implicated as a site for cellular plasticity and Li appears to be involved in this process (Chen and Manji 2006).
Su et al. (2007) have reported that 1 mM lithium induced maximal proliferation and neuronal differentiation of neural progenitor cells (NPCs) in vitro suggesting that lithium increases the neurogenesis of NPCs both in vitro and in vivo possibly via stimulating their production of BDNF. More recently, these authors (Su et al. 2009) have found that 1 mM lithium induced maximal BDNF production, which correlate very well with the finding that 1 mM lithium induced maximal neuronal generation of NPCs. Thereby lithium exerts the promoting effect on neurogenesis by up-regulating expression and release of BDNF, a member of the neurotrophin family which plays a critical role in regulating neuronal development, survival, and plasticity (Huang and Reichardt 2001).
It has been documented that the beneficial effects of lithium, such as mood stabilization, behavioral amelioration, and neurogenesis, are due to the inhibition of glycogen synthase kinase-3β (GSK-3β) by lithium, which promotes β-catenin-dependent transcriptional events (Quiroz et al. 2004; Wada et al. 2005a, b; Marmol 2008; Takahashi-Yanaga and Sasaguri 2007).
GSK-3, a serine/threonine protein kinase, controls multiple aspects of physiological events (e.g., cell membrane signal-to-gene transcription/protein translation, cytoskeletal organization, neuronal polarity, and cell survival/apoptosis) (Wada et al. 2005a, b; Jope and Johnson 2004; Jope et al. 2007; Wada 2009a).
GSK-3α (51 kDa) and GSK-3β (47 kDa) are encoded by different genes, GSK-3β being more enriched in the nervous system. GSK-3 is constitutively active in nonstimulated cells under the basal quiescent state and is inactivated by phosphorylation on Ser21 (GSK-3α) and Ser9 (GSK-3β) (Wada 2009b).
The transcription factor β-catenin is an established marker of glycogen synthase kinase-3 inactivation because cytoplasmic levels are increased by inhibition of the enzyme (Gould et al. 2004). Indeed, β-catenin, when sequentially phosphorylated at Ser45 by casein kinase I, and at Ser33, Ser37, and Thr41 by GSK-3β, undergoes proteasomal degradation; conversely, lithium prevents GSK-3β–catalyzed phosphorylation of β-catenin, enabling β-catenin to accumulate and translocate to the nucleus, where β-catenin facilitates survival gene transcription (Takahashi-Yanaga and Sasaguri 2007; Jope and Johnson 2004).
Gould et al. (2004) have reported that therapeutic serum range (0.5–1.2 mM) of lithium inhibits GSK-3β in vivo. In fact, 9 days of treatment with lithium increased β-catenin protein levels in soluble fractions from the frontal cortex.
While we utilized the same range of serum lithium concentration (0.4–0.8 mM), this treatment was without effect on both GSK-3αβ and phosphorylated β-catenin expression levels in brains of treated mice after 1 and 3 months of treatment. This suggests that lithium has not modified GSK-3 expression and activity in our experimental conditions.
From these findings, it appears that lithium may act via nonidentical mechanisms to exert its action depending on the length of treatment. Thereby, the most extensively studied signaling pathway associated with lithium’s neuroprotective action involves the inactivation of GSK-3β (Hongisto et al. 2003). But this inactivation was usually observed for short-term exposure and for higher concentrations of lithium (more than 1 mM) (Gould and Manji 2005). Thus, we have found that lithium performed its neuroprotective effect without inhibiting GSK-3β in SH-SY5Y cells exposed for long term (more than 10 months) to low lithium carbonate dose (0.5 mM) (Nciri et al. in preparation).
In conclusion, our study suggests that chronic treatment by therapeutic relevant lithium concentrations could favour neuroprotective and neurotrophic effects in mice brains. These effects were proved by the stability of lipid peroxidation level and antioxidant enzymes activities, the absence of modification in stress proteins expression such as HSP70, HSP90, and GRP94, the increase of relative brain weight, the enhancement of brain glucose incorporation, and the stimulation of neurogenesis and neurites growth in the hippocampus and enthorinal cortex of treated mice. Besides, lithium treatment has not modified GSK-3 protein expression and activity suggesting that its neuroprotective/neurotrophic effects were not mediated by GSK-3 inhibition.
References
Aebi H (1984) Catalase in vitro. Methods Enzymol 105:121–126
Allagui MS, Nciri R, Rouhaud MF, Murat JC, Elfeki A, Croute F, Vincent C (2009) Long-term exposure to low lithium concentrations stimulates proliferation, modifies stress protein expression pattern and enhances resistance to oxidative stress in SH-SY5Y cells. Neurochem Res 34(3):453–462
Bertrand E, Lechowicz W, Lewandowska E, Szpak GM, Dymecki J, Kosno-Kruszewska E, Wierzba-Bobrowicz T (2003) Degenerative axonal changes in the hippocampus and amygdala in Parkinson’s disease. Folia Neuropathol 41(4):197–207
Birch NJ (1991) Lithium and the cell: pharmacology and biochemistry. Academic Press, San Diego
Chen RW, Chuang DM (1999) Long term lithium treatment suppresses p53 and Bax expression but increases bcl-2 expression. A prominent role in neuroprotection against excitotoxicity. J Biol Chem 274:6039–6042
Chen G, Manji HK (2006) The extracellular signal-regulated kinase pathway: an emerging promising target for mood stabilizers. Curr Opin Psychiatry 19:313–323
Chen DF, Schneider GE, Martinou JC, Tonegawa S (1997) Bcl-2 promotes regeneration of severed axons in mammalian CNS. Nature 385:434–439
Chen G, Zeng WZ, Jiang L, Yuan PX, Zhao J, Manji HK (1999) The mood stabilizing agents lithium and valproate robustly increase the expression of the neuroprotective protein bcl-2 in the CNS. J Neurochem 72:879–882
Chen G, Rajkowska G, Du F, Seraji-Bozorgzad N, Manji HK (2000) Enhancement of hippocampal neurogenesis by lithium. J Neurochem 75:1729–1734
Drevets WC (2001) Neuroimaging and neuropathological studies of depression: implication for the cognitive-emotional features of mood disorders. Curr Opin Neurobiol 11:240–249
Durak I, Yurtarslanl Z, Canbolat O, Akyol O (1993) A methodological approach to superoxide-dismutase (SOD) activity assay based on inhibition of nitroblue tetrazolium (NBT) reduction. Clin Chim Acta 214:103–104
Esterbauer H (1993) Cytotoxicity and genotoxicity of lipid-oxidation products. Am J Clin Nutr 57:779–785
Flohe L, Gunzler WA (1984) Assays of glutathione peroxidase. Methods Enzymol 105:114–121
Frey BN, Andreazza AC, Cereser KM, Martins MR, Valvassori SS, Reus GZ (2006) Effects of mood stabilizers on hippocampus BDNF levels in an animal model of mania. Life Sci 79:281–286
Goodwin FK, Jamison KR (1990) Manic-depressive illness. Oxford University Press, New York
Gould TD, Manji HK (2005) Glycogen synthase kinase-3: a putative molecular target for lithium mimetic drugs. Neuropsychopharmacology 30:1223–1237
Gould TD, Chen G, Manji HK (2004) In vivo evidence in the brain for lithium inhibition of glycogen synthase kinase-3. Neuropsychopharmacology 29:32–38
Hal A, Angelica VS (2008) Toxicity of lithium to humans and the environment. A literature review. Ecotoxicol Environ Saf 70:349–356
Hiroi T, Wei H, Hough C, Leeds P, Chuang DM (2005) Protracted lithium treatment protects against the ER stress elicited by thapsigargin in rat PC12 cells: roles of intracellular calcium, GRP78 and Bcl-2. Pharmacogenomics J 5:102–111
Hongisto V, Smeds N, Brecht S, Herdegen T, Courtney MJ, Coffey ET (2003) Lithium blocks the c-Jun stress response and protects neurons via its action on glycogen synthase kinase 3. Mol Cell Biol 23:6027–6036
Hoyer S (2004) Causes and consequences of disturbances of cerebral glucose metabolism in sporadic Alzheimer disease: therapeutic implications. Adv Exp Med Biol 541:135–152
Huang EJ, Reichardt LF (2001) Neurotrophins: roles in neuronal development and function. Annu Rev Neurosci 24:677–736
Hunt A, Schönknecht P, Henze M, Seidl U, Haberkorn U, Schröder J (2007) Reduced cerebral glucose metabolism in patients at risk for Alzheimer’s disease. Psychiatr Res-Neuroim 155:147–154
Insausti R, Amaral DG (2004) Hippocampal formation. In: Paxinos G, Mai JK (eds) The human nervous system, 2nd edn. Elsevier Academic Press, Boston, pp 871–914
Jaeger A (2003) Lithium. Medicine, Medicine Publishing Co. Ltd, Oxford, UK, p 58
Jope RS, Johnson GVW (2004) The glamour and gloom of glycogen synthase kinase-3. Trends Biochem Sci 29:95–102
Jope RS, Yuskaitis CJ, Beurel E (2007) Glycogen synthase kinase-3 (GSK-3): inflammation, diseases, and therapeutics. Neurochem Res 32:577–595
Lowry OH, Rosebrouch NJ, Farr AL, Randall RJ (1951) Protein measurement with the folin phenol reagent. J Biol Chem 193:265–275
Lyoo IK, Dager SR, Kim JE, Yoon SJ, Friedman SD, Dunner DL, Renshaw PF (2010) Lithium-induced gray matter volume increase as a neural correlate of treatment response in bipolar disorder: a longitudinal brain imaging study. Neuropsychopharmacology 35:1743–1750
Manji HK, Moore GJ, Chen G (1999) Lithium at 50: have the neuroprotective effects of this unique cation been overlooked. Biol Psychiatry 46:929–940
Manji HK, Moore GJ, Chen G (2000a) Lithium up-regulates the cytoprotective protein Bcl-2 in the CNS in vivo: a role for neurotrophic and neuroprotective effects in manic depressive illness. J Clin Psychiatry 61:82–96
Manji HK, Moore GJ, Chen G (2000b) Clinical and preclinical evidence for the neurotrophic effects of mood stabilizers: implications for the pathophysiology and treatment of manic-depressive illness. Biol Psychiatry 48:740–754
Marmol F (2008) Lithium: bipolar disorder and neurodegenerative diseases. Possible cellular mechanisms of the therapeutic effects of lithium. Prog Neuropsychopharmacol Biol Psychiatry 32:1761–1771
McKinnon MC, Svoboda E, Levine B (2007) The frontal lobes and autobiographical memory. In: Miller BL, Cummings JL (eds) The human frontal lobes functions and disorders, 2nd edn. The Guilford Press, New York, pp 227–248
Moore GJ, Bebchuk JM, Hasanat K, Chen G, Seraji-Bozorgzad N, Wilds IB, Faulk MW, Koch S, Glitz DA, Jolkovsky L, Manji HK (2000) Lithium increases N-acetyl-aspartate in the human brain: in vivo evidence in support of bcl-2’s neurotrophic effects. Biol Psychiatry 48:1–8
Nciri R, Allagui MS, Croute F, Vincent C, Elfeki A (2008) Effects of low doses of Li carbonate injected into mice. Functional changes in kidney seem to be related to the oxidative status. C R Biologies 331:23–31
Nciri R, Allagui MS, Vincent C, Murat JC, Croute F, Elfeki A (2009) The effects of subchronic lithium administration in male Wistar mice on some biochemical parameters. Hum Exp Toxicol 28:641–646
Nciri R, Allagui MS, Vincent C, Murat JC, Croute F, Elfeki A (2010) Chronic lithium administration triggers an over-expression of GRP94 stress protein isoforms in mouse liver. Food Chem Toxicol 48:1638–1643
Nonaka S, Chuang DM (1998) Neuroprotective effects of chronic lithium on focal cerebral ischemia in rats. NeuroReport 9:2018–2084
Plenge P (1976) Acute lithium effects on rat brain glucose metabolism in vivo. Int Pharmacopsychiatr 11:84–92
Post RM, Weiss SRB, Chuang DM (1992) Mechanisms of action of anticonvulsants in affective disorders: comparisons with lithium. J Clin Psychopharmacol 12:23–35
Quiroz JA, Gould TD, Manji HK (2004) Molecular effects of lithium. Mol Interv 4:259–272
Ren M, Senatorov VV, Chen RW, Chuang DM (2003) Postinsult treatment with lithium reduces brain damage and facilitates neurological recovery in a rat ischemia/reperfusion model. Proc Natl Acad Sci USA 100:6210–6215
Stern R (1995) Lithium in the treatment of mood disorders. N Engl J Med 332:127–128
Su H, Chu T, Wu W (2007) Lithium enhances proliferation and neuronal differentiation of neural progenitor cells in vitro and after transplantation into the adult rat spinal cord. Exp Neurol 206:296–307
Su H, Zhang W, Guo J, Guo A, Yuan Q, Wu W (2009) Lithium enhances the neuronal differentiation of neural progenitor cells in vitro and after transplantation into the avulsed ventral horn of adult rats through the secretion of brain-derived neurotrophic factor. J Neurochem 108:1385–1398
Sun Y, Oberley LW, Li Y (1988) A simple method for clinical assay of superoxide dismutase. Clin Chem 34:497–500
Takahashi-Yanaga F, Sasaguri T (2007) The Wnt/β-catenin signaling pathway as a target in drug discovery. J Pharmacol Sci 104:293–302
Wada A (2009a) GSK-3 inhibitors and insulin receptor signaling in health, disease, and therapeutics. Front Biosci 14:1558–1570
Wada A (2009b) Lithium and neuropsychiatric therapeutics: neuroplasticity via glycogen synthase kinase-3β, β-catenin, and neurotrophin cascades. J Pharmacol Sci 110:14–28
Wada A, Yokoo H, Yanagita T, Kobayashi H (2005a) Lithium: potential therapeutics against acute brain injuries and chronic neurodegenerative diseases. J Pharmacol Sci 99:307–321
Wada A, Yokoo H, Yanagita T, Kobayashi H (2005b) New twist on neuronal insulin receptor signaling in health, disease, and therapeutics. J Pharmacol Sci 99:128–143
Xu XH, Zhang HL, Han R, Gu ZL, Qin ZH (2006) Enhancement of neuroprotection and heat shock protein induction by combined prostaglandin A1 and lithium in rodent models of focal ischemia. Brain Res 1102:154–162
Author information
Authors and Affiliations
Corresponding author
Additional information
Riadh Nciri and Mohamed Salah Allagui have equally contributed to this work.
Rights and permissions
About this article
Cite this article
Riadh, N., Allagui, M.S., Bourogaa, E. et al. Neuroprotective and neurotrophic effects of long term lithium treatment in mouse brain. Biometals 24, 747–757 (2011). https://doi.org/10.1007/s10534-011-9433-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10534-011-9433-6