Abstract
The objective of this study was to investigate, whether the naturally occurring polyphenol resveratrol (Res) enhances the anti-tumor activities of the chemotherapeutic agent oxaliplatin (Ox) in a cell culture model of colorectal cancer, also with regard to a possible inflammatory response and cytotoxic side-effects. Res and Ox in combination synergistically inhibit cell growth of Caco-2 cells, which seems to be due to the induction of different modes of cell death and further leads to an altered cytokine profile of cocultured macrophages. Moreover, combinatorial treatment does not affect non-transformed cells as severe cytotoxicity is not detected in human foreskin fibroblasts and platelets.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Colorectal carcinoma is one of the most prevalent human cancers in the world [1], and is frequently diagnosed at late stages that require chemotherapeutic treatment. In standard chemotherapy, oxaliplatin (Ox), a platinum coordination complex is especially approved for the treatment of metastatic colorectal carcinoma in combination with fluoropyrimidines [2, 3]. However, successful therapeutic outcome is often limited due to related side effects, targeting mainly the hematopoietic system, the peripheral nerves and the gastrointestinal tract, as well as the development of therapy resistance [2]. Thus, the concept of chemosensitization, e.g. by integrating chemopreventive agents to radio- or chemotherapeutic regimens, provides an innovative anticancer strategy. Among potential chemosensitizers, numerous phytochemicals might be promising agents for enhancing anti-tumor treatments, due to their wide range of biological and pharmacological effects together with the lack of toxicity in different in vitro and in vivo models [4]. Resveratrol (Res), a polyphenolic compound present in various food sources including red wine, peanuts and grapes [5], demonstrated potent chemopreventive and chemotherapeutic properties in different tumor models, which can mainly be explained by its activities on cell cycle control or apoptosis induction [6, 7].
Apoptosis is morphologically defined by chromatin condensation, nuclear fragmentation, shrinkage of the cytoplasm, blebbing of the plasma membrane and formation of apoptotic bodies [8]. This physiological cell death is energy-dependent and usually, but not exclusively, associated with caspase activation [9] and mitochondrial membrane permeabilization [10]. Cells undergoing apoptosis are rapidly and specifically recognized and removed by phagocytes such as macrophages or immature dendritic cells [11]. This process is generally considered to be immunologically silent due to the release of anti-inflammatory mediators and the suppression of local inflammation [12].
In contrast, necrosis is induced by external insults and is morphologically characterized by an increase in cell volume leading to the early rupture of the plasma membrane, consequently leading to the release of cytosolic, organelle, and nuclear components into the surrounding tissue [13]. Unlike apoptosis, necrosis is considered to be immunologically active at all times, because of the sudden release of so-called danger signals such as ATP or high mobility group box 1, which elicit inflammation by activating toll like receptors or the inflammasome in myeloid cells [14]. Besides, necrotic cells are able to induce the expression of genes that are involved in inflammatory responses [15].
Here, we investigated whether the polyphenol Res is able to enhance anti-tumor effects of the chemotherapy drug Ox in colorectal cancer cells, with special regard to the induction of different modes of cell death. We further determined, whether this treatment option may cause an immunogenic response by performing coculture experiments with human monocyte-derived macrophages. Finally, we tried to exclude cytotoxic effects on non-transformed fibroblastic cells and human platelets.
Materials and methods
Cell culture and materials
Caco-2 cells were kept in Dulbecco’s modified-Eagle’s medium (DMEM), supplemented with 10 % fetal calf serum (FCS), 1 % penicillin/streptomycin, 1 % sodium pyruvate and 1 % nonessential amino acids. Human foreskin fibroblasts (HFFs) were cultured in DMEM/Ham’s F-12 medium supplemented with 10 % FCS and 1 % penicillin/streptomycin. Both cell lines were maintained at 37 °C in an atmosphere of 95 % air and 5 % CO2. The cells were passaged weekly using Dulbecco’s phosphate-buffered saline (PBS) containing 0.1 % trypsin and 1 % ethylendiaminetetraacetic acid (EDTA). Cells were screened for possible contamination with mycoplasma at monthly intervals. For stock solutions Res (Sigma-Aldrich, Germany) was dissolved in dimethylsulfoxide (DMSO) at a concentration of 100 mM and Ox (Sigma-Aldrich, Germany) was dissolved in water at a concentration of 10 mM. Stocks were further dissolved in cell culture medium for achieving the required concentrations used in experimental settings. DMEM, DMEM/Ham’s F-12 medium, DMSO, sodium pyruvate solution, penicillin and streptomycin stock solutions were all obtained from PAA Laboratories GmbH. When synergistic effects were analyzed, the cells were pre-treated with Res for 24 h.
Cell proliferation assay
The effects on cellular DNA synthesis of cells was assessed using a cell proliferation ELISA kit (Roche Diagnostics, Germany). This assay is a colorimetric immunoassay for quantification of cell proliferation based on the measurement of bromodeoxyuridine (BrdU) incorporation during DNA synthesis, and is a non-radioactive alternative to the [3H]-thymidine incorporation assay. Cells were grown in 96-well culture dishes (103 cells/well), incubated with Res and/or Ox for 24 h, and then labeled with BrdU for further 4 h. Incorporated BrdU was measured colorimetrically.
Combination index (CI)
To assess the drug interactions of Res and Ox, we used the CI method defined by median-effect analysis of Chou and Talalay [16]. The fractional inhibitory concentration was calculated by dividing the concentration of the drug in the combination at half maximal inhibitory concentration (IC50) by the IC50 of the individual drug.
In this equation, the sum of the dose of Res and the dose of Ox give 50 % inhibition of cell growth. CI <1 indicates a synergistic effect; CI = 1, additive effect; and CI >1, antagonistic effect [17].
Determination of ATP level
Caco-2 cells were grown in 96 well culture dishes (103 cells/well) and allowed to grow overnight. Cell Viability Assay Kit (ApoSENSOR™, BioVision, CA, USA) was used according to the manufacturer’s instructions following a 6–24 h exposure to the substances. The assay utilizes luciferase to catalyze the formation of light from ATP and luciferin, which can be measured luminometrically. Decrease in ATP levels was determined by comparing the results with the level of untreated cells (control).
Determination of DNA fragmentation
Caco-2 cells were seeded in 96-well culture dishes; 24 h after plating, cells were stimulated with substances for 24 h. Cytoplasmic histone associated DNA fragments, as a marker of apoptosis, in control and treated cells were quantified using a commercially available ELISA kit (Roche Diagnostics, Germany).
Caspase-3 activity assay
Caco-2 cells, grown in six-well plates, were stimulated with substances at 80 % confluency. Fluorometric immunosorbent enzyme assay (Roche Diagnostics, Germany) was used according to the manufacturer’s instructions. Subsequent to the test, protein concentrations were measured for adaption of caspase activity.
SDS-polyacrylamide gel electrophoresis and immunoblot analysis
Caco-2 cells were seeded in 80 cm2 flasks; 24 h after plating, cells were incubated with substances for 6 or 24 h. Western blot analysis were performed as described previously [18]. The blots were incubated overnight at 4 °C in 5 % skimmed milk with a 1:1,000 dilution of primary antibodies for poly[ADP-ribose] polymerase, PARP (from Cell Signaling, MA, USA) or survivin (from Santa Cruz Biotechnology, Germany). The secondary, horseradish peroxidase-conjugated, antibody (Santa Cruz Biotechnology, Germany) was diluted at 1:5,000 and incubated with the membrane for another 60 min in skimmed milk. After chemoluminescence reaction (ECL, Amersham Pharmacia Biotech, Austria), bands were detected after exposure to Hyperfilm-MP (Amersham International plc, UK). Blots were reprobed with β-actin antibody (Santa Cruz Biotechnologies, Germany).
Mitochondrial membrane potential (ΔΨ m) analysis
Caco-2 cells were seeded into six-well culture plates at a density of 1 × 106 cells/well and allowed to grow overnight. Cells were stained with JC-1, as a component of the JC-1 mitochondrial membrane potential assay kit (Cayman Chemical Company, MI, USA) following a 6 and 24 h exposure to the substances. JC-1 is a lipophilic, cationic dye that can selectively enter into mitochondria and reversibly change colour from green to red as the membrane potential increases. Changes in ΔΨ m were finally assessed by microfluorimetry analysis using TECAN SpectraFluor Plus (TECAN Austria GmbH, Grödig, Austria) and indicated as changes of red/green ratio.
Annexin V-FITC/PI double labeled flow cytometry
To discriminate between apoptotic and necrotic cell subpopulations simultaneous staining with Annexin V-FITC (fluorescein isothiocyanate) and propidium iodide (PI) was performed. Cells incubated with the drugs for 5 and 24 h were harvested with accutase for 30 min. After centrifugation, cells were resuspended in 100 μl binding buffer mixed with 5 μl Annexin V-FITC (ImmunoTools, Friesoythe, Germany) and 5 µl PI and then incubated in dark for 10 min at 4 °C. Fluorescence was measured with a flow cytometer (FACSCanto; BD Biosciences).
Cytotoxicity
Cytotoxicity was analyzed by measuring lactate dehydrogenase (LDH) released from HFF cells and human platelets, incubated with substances for 24 h, using a commercially available kit [cytotoxicity detection kit (LDH), Roche Diagnostics, Germany]. Triton X-100 (2 %) was used as a positive control.
Cell isolation and culture
Human monocytes were isolated as described [19]. In brief, monocytes were isolated from buffy coats (DRK-Blutspendedienst Baden-Württemberg-Hessen, Institut für Transfusionsmedizin und Immunhämatologie, Frankfurt am Main, Frankfurt, Germany) using Ficoll–Hypaque gradients (PAA Laboratories, Karlsruhe, Germany). Peripheral blood mononuclear cells were washed twice with PBS and were allowed to adhere to culture dishes (Primaria 3072, Becton–Dickinson, Lincoln Park, NJ) for 1 h at 37 °C. Nonadherent cells were removed. Monocytes were then differentiated into macrophages with RPMI 1640 containing 10 % AB-positive human serum (PAA Laboratories) for 7 days or more.
Purified platelets were resuspended in serum-free DMEM containing 1 % penicillin/streptomycin, 1 % sodium pyruvate and 1 % nonessential amino acids, seeded in 80 cm2 flasks and immediately treated with substances. After 24 h, LDH release in the supernatant was analyzed as described above.
Co-culture experiments
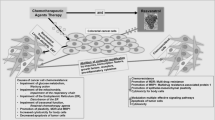
Primary human monocyte-derived macrophages were seeded in 100 mm tissue culture plates. After differentiation, supernatants of Res/Ox-treated tumor cells (conditioned medium) were added, and cocultures were maintained for 24 h. After analysis of the cytokine pattern (described in the following section), the conditioned macrophage medium/macrophage supernatant was further applied to Caco-2 cells, grown in 96-well culture dishes (103 cells/well) overnight, to investigate possible cell growth inhibitory and cytotoxic effects after 24 h of treatment (see overview in Fig. 4).
Quantification of cytokines
Cytokine measurements were performed essentially as described previously [20]. To quantify cytokines in cell culture supernatants of macrophages, we performed FACS analysis using the BD Cytometric Bead Array (CBA) System Human Inflammation Kit to determine interleukin (IL)-10, tumor necrosis factor-α (TNF-α), IL-8 and IL-1β. Samples were analyzed with the FACSCanto (BD Biosciences) flow cytometer and processed with BD Biosciences FCAP software.
Statistics
All statistical analyses were performed using GraphPad Instat 4.01 (San Diego, CA, USA). The data are expressed as means ± SE of at least three independent experiments. Results were analyzed either by Student’s t test or by ANOVA, when more than two groups were compared. When significant, multiple comparisons were done with the Tukey test. A p value <0.05 was considered to be significant.
Results
Synergistic antiproliferative effects of Res and Ox on tumor cells
We tried to explore a possible chemosensitizing capability of Res in Caco-2 colon cancer cells and our first results quickly revealed Res-induced potentiation of cell growth inhibition mediated by Ox (Fig. 1a–c; ***p < 0.001), which was more-than-additive as indicated by CI analysis (CI = 0.51, for details see “Materials and methods” section).
Synergistic antiproliferative effects of resveratrol and oxaliplatin on tumor cells. Inhibition of cell proliferation of Caco-2 by 24 h exposure to Res (a) and Ox (b) alone. Values represent mean ± SE (n = 8); *p < 0.05, **p < 0.01, ***p < 0.001 versus control. The IC50s for Res and Ox in Caco-2 cells were 75 µM (a) and 5.58 µM (b), respectively. c The combined effects of concurrent treatment with Res and Ox on Caco-2 cells. Cell proliferation was measured by BrdU incorporation after 24 h of incubation. According to the CI method of Chou and Talalay [16], a CI of 0.51 could be calculated which indicates synergism (see “Materials and methods” section). Values represent mean ± SE (n = 3); *p < 0.05, **p < 0.01, ***p < 0.001 versus control
Intracellular effects of Res/Ox-treatment in Caco-2 cells related to apoptotic cell death
Cell-growth inhibitory effects of Res/Ox on tumor cells were accompanied by different hallmarks of apoptosis. First experiments could demonstrate that the intrinsic apoptotic pathway seems to play a major role in apoptosis-inducing properties of Res as shown in Fig. 2a, where Res alone already significantly caused depolarization of the mitochondrial membrane potential (***p < 0.001), which could not be further enhanced after combinatorial treatment. Additionally, as shown in Fig. 2b, the effector caspase-3, which is one of the key proteases in the apoptotic pathway, was also induced by Res (100 µM). This effect could be significantly enhanced by co-stimulation with Res and Ox (***p < 0.001), which is in agreement with the observed cleavage of PARP (Fig. 2c; ***p < 0.001), a classical substrate for activated caspase-3. Proteolysis of PARP usually is an indicator for early apoptotic events. Survivin, a member of the inhibitor of apoptosis protein (IAP) family, which is commonly expressed in human tumor cell lines, was shown to bind caspase-3 and inhibit caspase activity and cells death [21]. In contrast to previous studies [22, 23], we could observe at least a slight induction of survivin protein levels after incubation with Ox (1 µM) in Caco-2 cells, which was significantly reduced, when cells were co-treated with Res (***p < 0.001; Fig. 2d).
Intracellular effects of Res/Ox-treatment in Caco-2 cells related to apoptotic cell death. a Loss of mitochondrial membrane potential (ΔΨ m) in Caco-2 cells exposed to Res and Ox, alone or in combination, after 6 and 24 h of treatment. Results represent means of three experiments, ***p < 0.001. b Effects of Res, Ox, their combination and staurosporine on activation of caspase-3 in Caco-2 cells after 24 h of exposure. Results are expressed as the percentage of control. Values represent mean ± SE (n = 4); *p < 0.05, ***p < 0.001. c Western blot analysis of PARP cleavage using whole cell extracts from Caco-2 cells exposed to Res and Ox, separately or in combination, a representative immunoblot of three independent experiments is shown. The bar graph presents densitometric analysis of the cleaved PARP/PARP ratio both normalized to β-actin [mean ± SE (n = 3)]. d Western blot analysis of survivin using whole cell extracts from Caco-2 cells exposed to Res and/or Ox for 24 h. A representative immunoblot of three independent experiments is shown. The bar graph presents densitometric analysis of the western blot images normalized to β-actin [mean ± SE (n = 3); **p < 0.01]
Possible induction of different modes of cell death with increasing concentrations of Res/Ox
As DNA cleavage is the major hallmark for apoptosis, we further quantified histone-complexed DNA fragments in Caco-2 after 24 h of treatment. Res (50–100 µM) in contrast to Ox (1 µM) thereby led to an increase of cytoplasmic histone-associated DNA fragments, an effect which could be significantly enhanced, when the drugs were used in combination (Fig. 3a; ***p < 0.001 vs. Ox).
Possible induction of different modes of cell death with increasing concentrations of Res/Ox. a Quantification of cytoplasmic histone associated DNA after 24 h of incubation with the test compounds. Values represent mean ± SE (n = 4); **p < 0.01, ***p < 0.001. b Intracellular content of ATP in control (untreated), Res- and/or Ox- as well as staurosporine (0.5 µg/ml)-treated cells. Caco-2 cells were incubated with the test substances for 6–24 h. Results are expressed as the percentage of control. Values represent mean ± SE (n = 4); *p < 0.05, **p < 0.01, ***p < 0.001 versus control. c, d Effects of Res and Ox, alone and in combination, on Annexin V-FITC or PI labeling of cells after 5 and 24 h of incubation. Cells were analysed by flow cytometry as described in “Materials and methods” section. The percentage of apoptotic (c) and necrotic (d) cells versus control as a result of the FACS analysis is presented by bar graphs. Values represent mean ± SE (n = 4), quantifying a minimum of 10,000 cells per treatment (*p < 0.05, **p < 0.01, ***p < 0.001)
In Fig. 3b, changes in the intracellular ATP/ADP ratio were analyzed. Although, decreasing ATP and increasing ADP levels are generally found in apoptotic cells, cells will rather undergo necrosis when intracellular ATP levels fall below a critical threshold [24]. We could demonstrate that incubation with Res (50–100 µM) and Ox (1 µM) resulted in a significant dose-, and partially time-dependent reduction of intracellular ATP (***p < 0.001). After 6 h the combined treatment even exceeds the effects induced by the positive control staurosporine (0.5 µg/ml), a well-known inducer of apoptosis [25].
To distinguish between different modes of cell death, Caco-2 cells treated with Res (50–100 µM), Ox (1 µM) alone and in combination for 5 and 24 h, were analyzed by Annexin V-FITC/PI labelling and flow cytometry. The degree of apoptosis thereby was quantitatively expressed as a percentage of the Annexin V-FITC-positive but PI-negative cells, while necrosis or late apoptosis was quantitatively expressed as a percentage of PI-positive or Annexin V-FITC/PI double-stained cells. Analysis after 5 h was chosen in order to differentiate between primary and secondary necrosis. Interestingly at this time point, Annexin V-FITC positive but also PI-positive cells could be measured indicating direct necrotizing effects of Res and Ox (Fig. 3c, d). Even though the population of apoptotic cells in the co-treated cells were still significantly increased after 24 h (**p < 0.01), overall apoptotic events seemed to decline, particularly in Res (50–100 µM)- as well as Ox (1 µM)-treated cells (Fig. 3c), compared to the 5 h-treatment. Rather, at this time point, a distinct population of PI-stained cells could be observed, so that a mixture of cells undergoing rapid primary as well as secondary necrosis/late apoptosis can be assumed (Fig. 3c, d).
Conditioned medium of Caco-2 cells causes an alteration of the cytokine profile in human macrophages
To examine direct or indirect effects of Res/Ox-treatment on immune cells, human primary macrophages were either incubated with conditioned medium of treated tumor cells or directly with Res (100 µM), Ox (1 µM) or the combination of both for 24 h, which was followed by measurement of cytokine TNF-α, IL-10, IL-8 and IL-1β release (for treatment procedure see overview in Fig. 4).
As indicated in Fig. 5 treatment with the supernatants of Res- or Ox-treated Caco-2-cells leads to a significantly elevated release of the pro-inflammatory cytokines TNF-α (Fig. 5a; *p < 0.05) and IL-8 (Fig. 5c; ***p < 0.001) from human macrophages. Even though supernatants of Res/Ox-treated Caco-2 cells show a slight tendency to counteract release of TNF-α and IL-8 from macrophages cocultured with supernatants of solely Ox (1 µM)-treated Caco-2 cells, this combination still provoked a marked increase in TNF-α (*p < 0.05) and IL-8 (***p < 0.001) production compared to control macrophages. When macrophages were directly treated with Res, Ox or the combination of both, no impact on overall TNF-α and IL-8 production or release could be observed. In the case of IL-1β coculture experiments hardly affect the amount of the excreted cytokine. Here, rather the direct treatment with Res and Ox at least shows the tendency to induce IL-1β production and release from macrophages (Fig. 5b). Most importantly, release of the cytokine IL-10 by macrophages from Ox-treated cocultures was increased, compared to control macrophages, an effect which could be significantly abolished when macrophages were stimulated with Res/Ox-treated Caco-2 supernatants (Fig. 5d; **p < 0.01). Inhibitory effects of Res on IL-10 release could also be observed upon direct stimulation of macrophages (**p < 0.01).
Conditioned medium of Caco-2 cells causes an alteration of the cytokine profile in human macrophages. a–d Caco-2 cells were treated with Res [100 µM], Ox [1 µM] or their combination. After 24 h of drug exposure, supernatants (conditioned medium) were collected and human monocyte-derived macrophages were incubated with conditioned Caco-2 medium for further 24 h. Alternatively, macrophages were stimulated directly with substances. Quantification of the cytokines a TNF-α, b IL-1β, c IL-8 and d IL-10 was performed by FACS analysis with BD Cytometric Bead Array Flex Sets as described in “Materials and methods” section. Data are presented as the mean ± SE from six independent experiments. Differences between supernatants from control macrophages and cocultures marked with an asterisk are statistically significant (*p < 0.05, **p < 0.01, ***p < 0.001)
Apoptotic/necrotic tumor cells enhance macrophage cytotoxicity against vital tumor cells
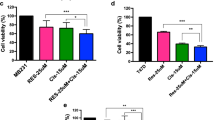
To investigate the effects of conditioned macrophage medium on tumor growth, we treated Caco-2 cells with the supernatant of cocultured macrophages (for details see overview in Fig. 4) and measured cell proliferation as well as LDH release after 24 h of stimulation. As indicated in Fig. 6, cell growth inhibition (***p < 0.001, a) as well as lysis (***p < 0.001, b) of Caco-2 cells were significantly enhanced, especially upon combined treatment.
Apoptotic/necrotic tumor cells enhance macrophage cytotoxicity against vital tumor cells. Effects of conditioned macrophage medium on Caco-2 cells after 24 h of incubation were measured by BrdU incorporation (a) and LDH release/cytotoxicity (b). Results are expressed as the percentage of control. Values represent mean ± SE (n = 4); **p < 0.01, ***p < 0.001
Treatment does not cause cytotoxicity in non-transformed cells
Responding to the question whether Res and Ox cause severe toxicity in normal tissue cells, we further treated human platelets (Fig. 7a) and foreskin fibroblasts (Fig. 7b) with both compounds for 24 h and quantified LDH-release. In this experimental setting neither Res or Ox alone nor their combination caused any effects. As expected Res was found to inhibit cell growth of human fibroblasts in a dose-dependent manner, an effect which was also reported by other authors [26]. However, in contrast to Caco-2 tumor cells, growth inhibitory effects on fibroblasts were not further enhanced when Res was combined with Ox (Fig. 7c).
Treatment does not cause cytotoxicity in non-transformed cells. a Human platelets and b non-transformed human foreskin fibroblasts were treated with Res (50–100 µM) and Ox (1 µM) alone or in combination for 24 h and LDH-release as a marker of direct cytotoxicity was quantified. Values represent mean ± SE (n = 3), ***p < 0.001 versus control. c The effects of combined treatment with Res and Ox on cell growth of non-transformed human foreskin fibroblasts. Values represent mean ± SE (n = 4), ***p < 0.001 versus control
Discussion
Ox is a third generation platinum-based drug, which is typically administered in combination with different other drugs as part of specific cancer-treatment regimens, e.g. Ox plus 5-fluorouracil (5-FU) and leucovorin (referred to as FOLFOX), Ox plus capecitabine (XELOX) or Ox plus cetuximab (CAPOX). Although Ox-based combination regimens show improved clinical efficacy, successful therapeutic outcome is often limited due to high toxicity as well as the development of multi-drug resistance [2, 27, 28]. Lowering the doses of these cytotoxic agents and combining it with chemopreventive drugs hence may be a new therapeutic strategy not only to decrease the toxicity but also to increase the efficacy of conventional chemotherapy, especially against tumors that are particularly difficult to treat. Res represents one of the promising dietary phytochemicals with chemopreventive and chemotherapeutic potential (3,5,4′-trihydroxystilbene) [29, 30], and was already examined in various studies to determine possible chemosensitizing properties when combined with established cancer treatments [31, 32] in which some modes of action could already be identified. Res apparently enhances antitumor therapies by modulating cell signalling pathways [33, 34] and cell cycle regulators [35, 36] and by inducing apoptotic pathways [37, 38]. Res further seems to counteract mechanisms of multidrug resistance by regulating the expression levels of membrane efflux pumps [39, 40] and members of the cytochrome E450 superfamily of enzymes [41, 42] thereby directly modulating intracellular drug metabolism and bioavailability.
In our model we could observe a significant increase of Ox antitumor efficacy even at low concentrations when cells were pretreated with Res. At least some of these effects are related to the induction of apoptosis, since regulation of typical apoptotic indicators could be observed, like depolarization of the mitochondrial membrane potential, caspase-3-activation and PARP cleavage which reflect the synergistic properties of Res and Ox. We further found a distinct reduction of intracellular protein levels of anti-apoptotic survivin, a structurally unique member of the IAPs family that is potentially involved in both control of cell division and inhibition of apoptosis [43] by direct/indirect inhibition of effector caspases [44]. Recently, it has been described as being selectively expressed at high levels in most human cancers and is related to clinical progression and poor prognosis [45, 46]. Furthermore, several anti-cancer agents [47, 48] as well as irradiation [49] show an upregulation of survivin in different tumor models, which seems to be related to treatment resistance. Hence, it has been proposed that survivin may serve as a chemo- or radioresistance factor and that modulation of survivin could target a key control point in resistance development [50].
Noting the facts that many cancers have defective apoptosis machinery or acquire apoptosis resistance during therapy [51], or the finding that apoptosis may be reversed in cancer cells [52], it is reasonable to consider whether activating alternative cell death pathways, such as necrosis, may be another important strategy for cancer therapy [53]. Unlike apoptosis, which is considered immunosuppressive, therapy-induced necrotic cell death initiates an immune response [13]. This inflammatory response may help to recruit cytotoxic immune cells to the tumor site, thereby increasing the efficacy of the chemotherapeutic drugs. Also Ox itself was shown to induce a potent immune response, which partly determines its therapeutic efficacy in cancer patients [54]. Thus, beside the tumor cells themselves, also the tumor microenvironment strongly contributes to tumor surveillance [55]. Tumor-associated macrophages (TAMs) for example are the major tumor cell infiltrates [56], which fulfil diverse functions to promote tumor growth, invasion and angiogenesis [57–59]. Thus, high numbers of intratumoral TAMs often correlate with a poor survival prognosis for patients with solid human tumors [60]. This pro-tumoricidal activity is attributable to a shift towards an anti-inflammatory M2 macrophage phenotype [56, 61], typically reflected by the production of IL-4, IL-13 or IL-10 cytokines [56, 62]. In contrast, the rather pro-inflammatory M1 phenotype is characterized by the production of superoxide (O2 −), TNF-α, IL-1β and IL-6 [62]. Since M2 macrophages reduce the expression of cytotoxic mediators and thus enhance tumor progression, reprogramming M2 towards a M1 phenotype might be beneficial with regards to cancer therapy [63]. Only little research was done by now focusing on modulatory activities of Res on macrophage functions, predominantly analyzing effects on inflammatory cytokine release, whereby Res was generally found to block pro-inflammatory responses from activated macrophages [64, 65]. This is in contrast to our findings, where we could observe changes in the cytokine profile which might reflect a polarization towards the anti-tumorigenic and rather pro-inflammatory M1-phenotype when macrophages were treated either with conditioned Caco-2 medium or directly with the combination of Res and Ox. Consequently, under in vivo conditions, two different strategies are possible by which human macrophages might become polarized by Res- and Ox treatment, either by direct stimulation and or indirectly by signals provided from tumor cells undergoing different modes of cell death. While apoptotic tumor cells were generally reported to suppress macrophage cytotoxicity directed against tumor cells, exposure to necrotized tumor cells rather causes pronounced stimulation of macrophage antitumor activity [66]. This is in accordance with our findings that the conditioned medium of macrophages cocultured with the rather necrotic tumor cell population leads to cell growth inhibition and LDH release when again transferred to tumor cells and this also correlates well with the observed reduction of IL-10 production in macrophages, since IL-10 typically suppresses the cytotoxic potential of macrophages [67], e.g. by inducing regulatory T cells [68, 69]. Finally, the cytotoxic and synergistic properties of Res/Ox-combinatorial treatment seem to be selective for tumor cells, since none of these effects could be observed in non-transformed cells, which might be favorable with regard to possible side-effects.
As discussed here, the immune response against dying tumor cells can play a major role in determining therapeutic success. If tumor cell death occurs in a potentially immunogenic fashion and if the immune system is capable of perceiving this immunogenicity, a potent innate and cognate immune response raised against dying cancer cells can contribute to the control and elimination of residual cancer cells. Our findings demonstrate for the first time that the polyphenol Res is capable of amplifying Ox-induced cell growth inhibition in colon cancer cells supposedly via induction of different modes of cell death. As a result of the apoptotic and necrotic effects of Res and Ox, immunosuppressive potential in macrophages is prevented, which renders them potently tumoricidal. These preliminary in vitro data therefore suggest that Res might not only be a possible candidate for chemoprevention, but also for chemotherapy options. Further mechanistic studies, in vivo animal models and most importantly human clinical trials are therefore needed to respond to the question whether the observed in vitro effects are also translatable to clinical applications.
Abbreviations
- BrdU:
-
Bromodeoxyuridine
- CI:
-
Combination index
- DMEM:
-
Dulbecco’s modified-Eagle’s medium
- DMSO:
-
Dimethylsulfoxide
- EDTA:
-
Ethylendiaminetetraacetic acid
- FCS:
-
Fetal calf serum
- FITC:
-
Fluorescein isothiocyanate
- 5-FU:
-
5-Fluorouracil
- HFF:
-
Human foreskin fibroblasts
- IAPs:
-
Inhibitor of apoptosis proteins
- IC50 :
-
Half maximal inhibitory concentration
- IL:
-
Interleukine
- LDH:
-
Lactate dehydrogenase
- Ox:
-
Oxaliplatin
- PARP:
-
Poly[ADP-ribose] polymerase
- PI:
-
Propidium iodide
- Res:
-
Resveratrol
- TAMs:
-
Tumor associated macrophages
- TNF-α:
-
Tumor necrosis factor-α
References
Siegel R, Naishadham D, Jemal A (2012) Cancer statistics, 2012. CA Cancer J Clin 62:10–29
Alcindor T, Beauger N (2011) Oxaliplatin: a review in the era of molecularly targeted therapy. Curr Oncol 18:18–25
Graham MA, Lockwood GF, Greenslade D, Brienza S, Bayssas M, Gamelin E (2000) Clinical pharmacokinetics of oxaliplatin: a critical review. Clin Cancer Res 6:1205–1218
Sarkar FH, Li Y (2006) Using chemopreventive agents to enhance the efficacy of cancer therapy. Cancer Res 66:3347–3350
Takaoka M (1939) Resveratrol, a new phenolic compound, from Veratrum grandiflorum. Nippon Kagaku Kaishi 60:1090–1100
Delmas D, Solary E, Latruffe N (2011) Resveratrol, a phytochemical inducer of multiple cell death pathways: apoptosis, autophagy and mitotic catastrophe. Curr Med Chem 18:1100–1121
Ulrich S, Wolter F, Stein JM (2005) Molecular mechanisms of the chemopreventive effects of resveratrol and its analogs in carcinogenesis. Mol Nutr Food Res 49:452–461
Kerr JF, Wyllie AH, Currie AR (1972) Apoptosis: a basic biological phenomenon with wide-ranging implications in tissue kinetics. Br J Cancer 26:239–257
Kroemer G, Martin SJ (2005) Caspase-independent cell death. Nat Med 11:725–730
Kroemer G, Galluzzi L, Brenner C (2007) Mitochondrial membrane permeabilization in cell death. Physiol Rev 87:99–163
Savill J, Dransfield I, Gregory C, Haslett C (2002) A blast from the past: clearance of apoptotic cells regulates immune responses. Nat Rev Immunol 2:965–975
Kono H, Rock KL (2008) How dying cells alert the immune system to danger. Nat Rev Immunol 8:279–289
Savill J, Fadok V (2000) Corpse clearance defines the meaning of cell death. Nature 407:784–788
Zitvogel L, Kepp O, Kroemer G (2010) Decoding cell death signals in inflammation and immunity. Cell 140:798–804
Basu S, Binder RJ, Suto R, Anderson KM, Srivastava PK (2000) Necrotic but not apoptotic cell death releases heat shock proteins, which deliver a partial maturation signal to dendritic cells and activate the NF-kappa B pathway. Int Immunol 12:1539–1546
Chou TC, Talalay P (1984) Quantitative analysis of dose–effect relationships: the combined effects of multiple drugs or enzyme inhibitors. Adv Enzym Regul 22:27–55
Carnesecchi S, Langley K, Exinger F, Gosse F, Raul F (2002) Geraniol, a component of plant essential oils, sensitizes human colonic cancer cells to 5-Fluorouracil treatment. J Pharmacol Exp Ther 301:625–630
Kaminski BM, Loitsch SM, Ochs MJ, Reuter KC, Steinhilber D, Stein J, Ulrich S (2010) Isothiocyanate sulforaphane inhibits protooncogenic ornithine decarboxylase activity in colorectal cancer cells via induction of the TGF-beta/Smad signaling pathway. Mol Nutr Food Res 54:1486–1496
Von Knethen AA, Brune B (2001) Delayed activation of PPARgamma by LPS and IFN-gamma attenuates the oxidative burst in macrophages. FASEB J 15:535–544
Weigert A, Tzieply N, von Knethen A, Johann AM, Schmidt H, Geisslinger G, Brune B (2007) Tumor cell apoptosis polarizes macrophages role of sphingosine-1-phosphate. Mol Biol Cell 18:3810–3819
Tamm I, Wang Y, Sausville E, Scudiero DA, Vigna N, Oltersdorf T, Reed JC (1998) IAP-family protein survivin inhibits caspase activity and apoptosis induced by Fas (CD95), Bax, caspases, and anticancer drugs. Cancer Res 58:5315–5320
Fujie Y, Yamamoto H, Ngan CY, Takagi A, Hayashi T, Suzuki R, Ezumi K, Takemasa I, Ikeda M, Sekimoto M, Matsuura N, Monden M (2005) Oxaliplatin, a potent inhibitor of survivin, enhances paclitaxel-induced apoptosis and mitotic catastrophe in colon cancer cells. Jpn J Clin Oncol 35:453–463
Khan Z, Khan N, Tiwari RP, Patro IK, Prasad GB, Bisen PS (2010) Down-regulation of survivin by oxaliplatin diminishes radioresistance of head and neck squamous carcinoma cells. Radiother Oncol 96:267–273
Eguchi Y, Shimizu S, Tsujimoto Y (1997) Intracellular ATP levels determine cell death fate by apoptosis or necrosis. Cancer Res 57:1835–1840
Wang XQ, Xiao AY, Sheline C, Hyrc K, Yang A, Goldberg MP, Choi DW, Yu SP (2003) Apoptotic insults impair Na+, K+-ATPase activity as a mechanism of neuronal death mediated by concurrent ATP deficiency and oxidant stress. J Cell Sci 116:2099–2110
Faragher RG, Burton DG, Majecha P, Fong NS, Davis T, Sheerin A, Ostler EL (2011) Resveratrol, but not dihydroresveratrol, induces premature senescence in primary human fibroblasts. Age (Dordr) 33:555–564
Capdevila J, Elez E, Peralta S, Macarulla T, Ramos FJ, Tabernero J (2008) Oxaliplatin-based chemotherapy in the management of colorectal cancer. Expert Rev Anticancer Ther 8:1223–1236
Rixe O, Ortuzar W, Alvarez M, Parker R, Reed E, Paull K, Fojo T (1996) Oxaliplatin, tetraplatin, cisplatin, and carboplatin: spectrum of activity in drug-resistant cell lines and in the cell lines of the National Cancer Institute’s Anticancer Drug Screen panel. Biochem Pharmacol 52:1855–1865
Smoliga JM, Baur JA, Hausenblas HA (2011) Resveratrol and health—a comprehensive review of human clinical trials. Mol Nutr Food Res 55:1129–1141
Vang O, Ahmad N, Baile CA, Baur JA, Brown K, Csiszar A, Das DK, Delmas D, Gottfried C, Lin HY, Ma QY, Mukhopadhyay P, Nalini N, Pezzuto JM, Richard T, Shukla Y, Surh YJ, Szekeres T, Szkudelski T, Walle T, Wu JM (2011) What is new for an old molecule? Systematic review and recommendations on the use of resveratrol. PLoS ONE 6:e19881
Kaminski BM, Steinhilber D, Stein JM, Ulrich S (2012) Phytochemicals resveratrol and sulforaphane as potential agents for enhancing the anti-tumor activities of conventional cancer therapies. Curr Pharm Biotechnol 13:137–146
Vinod BS, Maliekal TT, Anto RJ (2013) Phytochemicals as chemosensitizers: from molecular mechanism to clinical significance. Antioxid Redox Signal 18(11):1307–1348
El-Mowafy AM, El-Mesery ME, Salem HA, Al-Gayyar MM, Darweish MM (2010) Prominent chemopreventive and chemoenhancing effects for resveratrol: unraveling molecular targets and the role of C-reactive protein. Chemotherapy 56:60–65
Mao QQ, Bai Y, Lin YW, Zheng XY, Qin J, Yang K, Xie LP (2010) Resveratrol confers resistance against taxol via induction of cell cycle arrest in human cancer cell lines. Mol Nutr Food Res 54(11):1574–1584 (Epub ahead of print)
Harikumar KB, Kunnumakkara AB, Sethi G, Diagaradjane P, Anand P, Pandey MK, Gelovani J, Krishnan S, Guha S, Aggarwal BB (2010) Resveratrol, a multitargeted agent, can enhance antitumor activity of gemcitabine in vitro and in orthotopic mouse model of human pancreatic cancer. Int J Cancer 127:257–268
Colin D, Gimazane A, Lizard G, Izard JC, Solary E, Latruffe N, Delmas D (2009) Effects of resveratrol analogs on cell cycle progression, cell cycle associated proteins and 5fluoro-uracil sensitivity in human derived colon cancer cells. Int J Cancer 124:2780–2788
Jazirehi AR, Bonavida B (2004) Resveratrol modifies the expression of apoptotic regulatory proteins and sensitizes non-Hodgkin’s lymphoma and multiple myeloma cell lines to paclitaxel-induced apoptosis. Mol Cancer Ther 3:71–84
Chan JY, Phoo MS, Clement MV, Pervaiz S, Lee SC (2008) Resveratrol displays converse dose-related effects on 5-fluorouracil-evoked colon cancer cell apoptosis: the roles of caspase-6 and p53. Cancer Biol Ther 7:1305–1312
Kweon SH, Song JH, Kim TS (2010) Resveratrol-mediated reversal of doxorubicin resistance in acute myeloid leukemia cells via downregulation of MRP1 expression. Biochem Biophys Res Commun 395:104–110
Nabekura T, Kamiyama S, Kitagawa S (2005) Effects of dietary chemopreventive phytochemicals on P-glycoprotein function. Biochem Biophys Res Commun 327:866–870
Choi JS, Choi BC, Kang KW (2009) Effect of resveratrol on the pharmacokinetics of oral and intravenous nicardipine in rats: possible role of P-glycoprotein inhibition by resveratrol. Pharmazie 64:49–52
Frampton GA, Lazcano EA, Li H, Mohamad A, Demorrow S (2010) Resveratrol enhances the sensitivity of cholangiocarcinoma to chemotherapeutic agents. Lab Investig 90:1325–1338
LaCasse EC, Baird S, Korneluk RG, MacKenzie AE (1998) The inhibitors of apoptosis (IAPs) and their emerging role in cancer. Oncogene 17:3247–3259
Shin S, Sung BJ, Cho YS, Kim HJ, Ha NC, Hwang JI, Chung CW, Jung YK, Oh BH (2001) An anti-apoptotic protein human survivin is a direct inhibitor of caspase-3 and -7. Biochemistry 40:1117–1123
Altieri DC (2003) Validating survivin as a cancer therapeutic target. Nat Rev Cancer 3:46–54
Rodel F, Sprenger T, Kaina B, Liersch T, Rodel C, Fulda S, Hehlgans S (2012) Survivin as a prognostic/predictive marker and molecular target in cancer therapy. Curr Med Chem 19:3679–3688
Chao JI, Kuo PC, Hsu TS (2004) Down-regulation of survivin in nitric oxide-induced cell growth inhibition and apoptosis of the human lung carcinoma cells. J Biol Chem 279:20267–20276
Wall NR, O’Connor DS, Plescia J, Pommier Y, Altieri DC (2003) Suppression of survivin phosphorylation on Thr34 by flavopiridol enhances tumor cell apoptosis. Cancer Res 63:230–235
Rodel C, Haas J, Groth A, Grabenbauer GG, Sauer R, Rodel F (2003) Spontaneous and radiation-induced apoptosis in colorectal carcinoma cells with different intrinsic radiosensitivities: survivin as a radioresistance factor. Int J Radiat Oncol Biol Phys 55:1341–1347
Goyal L (2001) Cell death inhibition: keeping caspases in check. Cell 104:805–808
Igney FH, Krammer PH (2002) Death and anti-death: tumour resistance to apoptosis. Nat Rev Cancer 2:277–288
Tang HL, Yuen KL, Tang HM, Fung MC (2009) Reversibility of apoptosis in cancer cells. Br J Cancer 100:118–122
Ricci MS, Zong WX (2006) Chemotherapeutic approaches for targeting cell death pathways. Oncologist 11:342–357
Tesniere A, Schlemmer F, Boige V, Kepp O, Martins I, Ghiringhelli F, Aymeric L, Michaud M, Apetoh L, Barault L, Mendiboure J, Pignon JP, Jooste V, van Endert P, Ducreux M, Zitvogel L, Piard F, Kroemer G (2010) Immunogenic death of colon cancer cells treated with oxaliplatin. Oncogene 29:482–491
Schreiber RD, Old LJ, Smyth MJ (2011) Cancer immunoediting: integrating immunity’s roles in cancer suppression and promotion. Science 331:1565–1570
Mantovani A, Sozzani S, Locati M, Allavena P, Sica A (2002) Macrophage polarization: tumor-associated macrophages as a paradigm for polarized M2 mononuclear phagocytes. Trends Immunol 23:549–555
Lewis C, Murdoch C (2005) Macrophage responses to hypoxia: implications for tumor progression and anti-cancer therapies. Am J Pathol 167:627–635
Condeelis J, Pollard JW (2006) Macrophages: obligate partners for tumor cell migration, invasion, and metastasis. Cell 124:263–266
Crowther M, Brown NJ, Bishop ET, Lewis CE (2001) Microenvironmental influence on macrophage regulation of angiogenesis in wounds and malignant tumors. J Leukoc Biol 70:478–490
Bingle L, Brown NJ, Lewis CE (2002) The role of tumour-associated macrophages in tumour progression: implications for new anticancer therapies. J Pathol 196:254–265
Mantovani A, Allavena P, Sica A (2004) Tumour-associated macrophages as a prototypic type II polarised phagocyte population: role in tumour progression. Eur J Cancer 40:1660–1667
Gordon S (2003) Alternative activation of macrophages. Nat Rev Immunol 3:23–35
Sica A, Schioppa T, Mantovani A, Allavena P (2006) Tumour-associated macrophages are a distinct M2 polarised population promoting tumour progression: potential targets of anti-cancer therapy. Eur J Cancer 42:717–727
Chung EY, Kim BH, Hong JT, Lee CK, Ahn B, Nam SY, Han SB, Kim Y (2011) Resveratrol down-regulates interferon-gamma-inducible inflammatory genes in macrophages: molecular mechanism via decreased STAT-1 activation. J Nutr Biochem 22:902–909
Chuang CC, Martinez K, Xie G, Kennedy A, Bumrungpert A, Overman A, Jia W, McIntosh MK (2010) Quercetin is equally or more effective than resveratrol in attenuating tumor necrosis factor-{alpha}-mediated inflammation and insulin resistance in primary human adipocytes. Am J Clin Nutr 92:1511–1521
Reiter I, Krammer B, Schwamberger G (1999) Cutting edge: differential effect of apoptotic versus necrotic tumor cells on macrophage antitumor activities. J Immunol 163:1730–1732
Hagemann T, Lawrence T, McNeish I, Charles KA, Kulbe H, Thompson RG, Robinson SC, Balkwill FR (2008) “Re-educating” tumor-associated macrophages by targeting NF-kappaB. J Exp Med 205:1261–1268
Mantovani A, Allavena P, Sica A, Balkwill F (2008) Cancer-related inflammation. Nature 454:436–444
van Dongen M, Savage ND, Jordanova ES, Briaire-de Bruijn IH, Walburg KV, Ottenhoff TH, Hogendoorn PC, van der Burg SH, van der Burg SH, Gelderblom H, van Hall T (2010) Anti-inflammatory M2 type macrophages characterize metastasized and tyrosine kinase inhibitor-treated gastrointestinal stromal tumors. Int J Cancer 127:899–909
Acknowledgments
This work was supported by Graduate Scholarship Grants from the DFG to Bettina M. Kaminski and from the “Stiftung Polytechnische Gesellschaft Frankfurt am Main” to Maria-Christina Scherzberg. Bettina M. Kaminski was a member of the Frankfurt International Research Graduate School for Translational Biomedicine (FIRST), Frankfurt am Main. The authors thank Astrid Brüggerhoff for excellent technical assistance.
Conflict of interest
The authors have declared no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kaminski, B.M., Weigert, A., Scherzberg, MC. et al. Resveratrol-induced potentiation of the antitumor effects of oxaliplatin is accompanied by an altered cytokine profile of human monocyte-derived macrophages. Apoptosis 19, 1136–1147 (2014). https://doi.org/10.1007/s10495-014-0988-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10495-014-0988-x