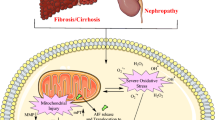
Abstract
Mitochondria are known to be involved in cholestatic liver injury, but the damage and biogenesis of mitochondria in response to the early stage of cholestasis is unknown. A rat model of cholestasis was established by bile duct ligation (BDL), with simultaneous creation of the sham group receiving laparotomy without BDL. A significant decrease of liver peroxisome proliferators-activated receptor γ coactivator-1α, mitochondrial transcriptional factor A (Tfam) and glutathione peroxidase (GPx) mRNA and Tfam protein from 6 to 72 h after BDL was found, which was associated with significant decrease of the glutathione, GPx and catalase activity at 72 h. At 72 h after BDL, mitochondrial DNA copy number reached the lowest level, while caspase 9 and 3 activity, but not caspase 8, Bax, Bcl2, Fas L and Fas–Fas L complex, were upregulated significantly in the liver homogenates of BDL rats. The apoptotic liver cells appeared in large amounts in the rat liver by 72 h after BDL. Our results indicate that transcriptional regulation of the mitochondrial biogenesis is impaired within a few hours after complete bile duct obstruction, resulting in later mitochondrial dysfunction and consequent cholestatic liver injury via the intrinsic apoptosis pathway.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cholestasis constitutes one of the most common and severe liver diseases [1, 2]. Early recognition and diagnosis of the cholestatic liver disorders are critical especially for those resulting from complete obstruction of the extrahepatic bile duct such as biliary atresia [1, 2]. In biliary atresia, liver injury develops quickly and hepatic fibrosis is evident by 2 months of age. The outcome of surgical treatment of biliary atresia is usually poor after 3 months of age, mostly owing to irreversible hepatic fibrosis [3, 4]. The exact pathogenesis of this disorder is unknown. In rats, hepatic fibrosis usually develops by 2–3 weeks after bile duct ligation (BDL) [5, 6]. It is obvious that liver injury develops very early following complete biliary obstruction, probably in minutes or in hours.
Previous studies have implicated free radicals and lipid peroxides in the pathogenesis of longstanding cholestatic liver injury [7, 8]. However, the response of hepatocyte mitochondrial oxidative status and biogenesis to cholestatic liver injury was detected in days or weeks in most of the previous studies when cholestatic liver injury was well-established [9–13]. Increased oxidative damage to mitochondrial DNA (mtDNA) has been reported in other liver injuries such as chronic ethanol ingestion [14, 15] and it may contribute to alterations in the abundance of mitochondria and the mtDNA copy number [9]. These data are consistent with our report that reveals significant oxidative stress and mitochondrial dysfunction in the early stages of biliary atresia, which is associated with a decrease in mtDNA copy number [16].
Mitochondrial biogenesis and mtDNA maintenance depend on coordinated expression of genes in the nucleus and mitochondria [15]. Mitochondrial transcriptional factor A (Tfam) is one of the most important nuclear genes that binds to the sequence promoters within the mitochondrial D-loop region and stimulates transcription from mtDNA [17]. The expression of Tfam is regulated by other transcriptional factors, including peroxisome proliferator-activated receptor γ coactivator-1α (PGC-1α) [18, 19]. Persistent mitochondrial oxidative stress caused by cholestatic liver injury may lead to a decline in mitochondrial respiratory function with decreased mtDNA copy number [9], as manifested in one of our previous studies [16]. Therefore, regulation of mtDNA transcription seems to be an essential step in elucidation of cholestatic liver injury. To cope with increased levels of oxidative stress, the antioxidant capacity of hepatocytes is likely to respond within the first few days of BDL before the decision making of life-and-death of these stressed cells [20]. However, mitochondrial biogenesis in response to oxidative liver injury in the early stage of BDL, with consequent effects on the expression of antioxidative enzymes such as glutathione peroxidase (GPx) and catalase, is virtually unknown.
In this study, we investigated the deregulation of the mitochondrial biogenesis within a few hours after cholestasis, which subsequently led to mitochondrial dysfunction and full-blown cholestatic liver injury in a murine model of extrahepatic bile duct obstruction.
Materials and methods
Animal model
Male Sprague-Dawley rats 250–350 g were purchased from the National Animal Center, the Academia Sinica, Taipei, Taiwan, after weaning. The animals were maintained on standard laboratory rat chow in a 12-h light–dark cycle. The care and use of the laboratory animal strictly followed the protocol, which was approved by the animal ethics committee of the Chang Gung University, Kaohsiung, Taiwan. After anesthesia by intraperitoneal injection of 50 mg/kg ketamine and 50 mg/kg xylazine, the rat received a median laparotomy and the extrahepatic bile duct was identified. The bile duct was double ligated with 4–0 silk sutures to create obstructive jaundice and was designated as BDL. The animals receiving laparotomy without ligation of the bile duct were designated as sham rats. The animals without any operative procedures were designated as normal controls. The rats were then sacrificed at 0.5, 1, 3, 6, 24, 72 h after BDL or sham operation. All the rats received cardiac puncture to obtain blood at the time of sacrifice to assay total bilirubin levels, alanine transaminase (ALT) and aspartate transaminase (AST) activities, determined by a standard autoanalyzer (Hitachi model 7450, Tokyo, Japan). Liver was removed and some of the liver tissues were snap-frozen for messenger RNA (mRNA) and protein determinations, and the remaining were formalin-fixed for histological examinations.
mRNA isolation and real-time QRT-PCR
LightCycler® 480 Real-Time PCR System (Roche Co., Germany) was used to quantify the tissue amount of mRNA. For real-time quantitative reverse transcription-polymerase chain reaction (QRT-PCR), the reagent mixture was prepared according to the protocol provided by the manufacturer (Protech Technology, Taipei, Taiwan). Two micrograms of total RNA extracted from the liver tissue was used to generate cDNA using an oligodeoxynucleotide primer (oligo dT15) following the protocol for transcription (Promega, Madison, WI). PCR was performed on 20 μl in a LightCycler® 480 SYBR Green I Master (Roche Co., Germany) containing 10 nmol forward primers and reverse primers, and approximately 10 ng cDNA was produced. The primer sequences for the study gene and the housekeeping β-actin gene were provided in Table 1. Each sample was tested in duplicate and the mean of the two values was chosen as copy number of the sample. The validation experiments were done in triplicate and amplification efficiencies were validated as indcated in our previous reports [16, 21].
Western blotting analysis
The frozen tissue was homogenized in a buffer then centrifuged at 14,000g. Protein (40 μg) from the supernatant of each sample was separated by SDS–PAGE and transferred to polyvinylidene difluoride membranes for electrophoresis. The membranes were blocked in TBST buffer for 1 h at room temperature after which the blots were incubated with a primary polyclonal rabbit anti-PGC-1α antibody (sc-13067; Santa Cruz Biotech.), polyclonal goat anti-Tfam antibody (sc-23588; Santa Cruz Biotech.), caspase 9 antibody (# 9507; Cell Signaling), caspase 3 antibody (# 9661; Cell Signaling), caspase 8 antibody (# 9748; Cell Signaling), Bax antibody (#2772; Cell Signaling), Bcl2 antibody (#2827; Cell Signaling) followed by a secondary alkaline phosphatase-conjugated anti-IgG antibody (1:5000; Promega). The Western blots were visualized with the Blot AP System (Promega). Alpha-tubulin or β-actin was used as internal control.
Catalase assay
The liver tissue was homogenized and assays were conducted on a Bradford assay (Biorad) automated chemistry analyzer. Catalase activity assay kit (Cayman, Catalog No: 707002) and samples (20 μl) were placed on the instrument and assayed according to the manufacturer’s protocol. The catalase activity level was quantified spectrophotometrically at 540 nm. The results were expressed as nmol/min/ml of protein. Standards and blanks were assayed in duplicate and treated as samples (i.e., not placed in the calibration positions). The average of two measurements was used in subsequent statistical analysis of the data.
Measurement of liver total glutathione (GSH) and reduced GSH to oxidized glutathione (GSSG) ratio
Liver total GSH and GSH/GSSG ratios, the main intracellular detoxifying molecules, were measured using a commercial kit (Glutathione Assay Kit II Cat No. 354103, Calbiochem) according to the manufacturer’s protocol. In short, the assay utilizes a carefully optimized enzymatic recycling method, using glutathione reductase, for the quantification of GSH. The GSH is quantified spectrophotometrically at 405 nm. Quantification of GSSG, exclusive of GSH, is accomplished by first derivatizing GSH with 2-vinylpyridine. Tissue sample (liver) was homogenized on ice using a polytron homogenizer. The solution used for homogenization consisted of 50 mM MES which contains 0.4 M 2-(N-morpholino) ethanesulphonic acid, 0.1 M phosphate, and 2 mM EDTA, pH 6.0 (1 g tissue per 5 ml MES buffer). The total homogenate was centrifuged at 4°C at 10,000g for 15 min to obtain the supernatant for the assay of total GSH and GSSG. Duplicate determinations in 100 μl of tissue homogenate samples collected from all animals were made and the average of two measurements was used in subsequent statistical analysis of the data. The GSH to GSSG ratios were calculated and expressed as GSH/GSSG ratio.
Determination of mtDNA copy number
DNA samples were extracted from rat liver cells. The mtDNA copy numbers were measured by a real-time PCR and corrected by simultaneous measurement of the nuclear DNA. The forward and reverse primers complementary to nuclear β-actin gene were 5′-GAAATCGTGCGTGACATTAAAG-3′ and 5′-ATCGGAACCGCTCATTG-3′ [22]. The forward and reverse primers for mtDNA, which are complementary to the sequence of the mitochondrial ND1 gene, were 5′-ATTCTAGCCACATCAAGTCTTT-3′ and 5′-GGAGGACGGATAAGAGGATAAT-3′. The PCR was performed in a LightCycler® 480 Real-Time PCR System (Roche Co., Germany), using the LightCycler ® 480 SYBR Green I Master (Roche Co., Germany). DNA (10 ng) was mixed with 10 μl SYBR® Green PCR Master Mix containing 10 n mol of forward and reverse primers, in a final volume of 20 μl. The PCR reactions were: initial 50°C 2 min, 95°C 1 min, 40 cycles for denaturation at 95°C for 15 s, annealing at 60°C for 20 s and primer extension at 72°C for 15 s, final 25°C. The threshold cycle number (Ct) values of the β-actin gene and the mitochondrial ND1 gene were determined for each individual quantitative PCR run. Ct values can be used as a measure of the input copy number and Ct value differences used to quantify mtDNA copy number relative to the β-actin gene with the following equation: Relative copy number (R c) = 2∆Ct, where ∆Ct is the Ctβ-actin − CtmtDNA [23]. Each measurement was carried out at least three times and normalized in each experiment against a serial dilution of a control DNA sample. We compared mtDNA copy number in BDL rats to the sham and the normal control. For comparison between groups, logarithmic transformation of data was used since the original values of the relative mtDNA copy number in rat hepatocytes showed a non-normal distribution.
TdT-mediated dUTP biotin nick end labeling (TUNEL)
Immediately after sacrifice, representative sections were cut from the mid-right lobe of the liver in the rat. Sections were obtained from six rats in each group. After formalin fixation, these paraffin-embedded liver sections were stained and evaluated by two pathologists (Huang and Kuo). Double-strand DNA breaks were detected by TUNEL according to the method of our previous study [16] with some modifications. We used ApopTag® plus peroxidase in situ apoptosis detection kit (CHEMICON International, Inc. USA) for TUNEL. Deparaffinized sections were washed with distilled water and treated with protein digestion enzyme for 15 min at 37°C. After washing with three changes of PBS, sections were treated with TdT solution, incubated with 3% hydrogen peroxide for 5 min to block endogenous peroxidase activity, and then treated with peroxidase conjugated antibody for 10 min at room temperature. After washing in PBS, nick end labeling was visualized by immersing reacted sections in 3′,3′-diaminobenzidine solution with 3% hydrogen peroxide and counterstaining with methyl green.
Statistical analysis
Data were expressed as mean ± SD. Comparisons between control and BDL rats were made at each time point. Results were analyzed by the t-test when comparing the BDL groups with sham. P < 0.05 was considered to be statistically significant.
Results
Impairments of liver function of the experimental animals in BDL
BDL resulted in increases in serum total and direct bilirubin levels, as well as AST and ALT (Fig. 1a–d), which progressed with time. The data are consistent with the establishment of cholestatic liver injury.
Increase in serum a total bilirubin and b direct bilirubin levels, as well as c aspartate aminotransferase and d alanine aminotransferase levels in the rats receiving bile duct ligation (BDL) in comparison to the sham rats. All results represent means ± SD of 6 animals, * P < 0.05 when comparing the BDL groups with sham
Cholestasis decreases mRNA and protein expression of mitochondrial biogenesis regulator Tfam
PGC-1α mRNA decreased significantly by 6 h after BDL (Fig. 2a), but the protein levels were not significantly different between groups throughout the study period (data not shown). Tfam mRNA levels decreased significantly by 6 h after BDL (Fig. 2b), and the protein levels also decreased significantly at this time (Fig. 2c, d). Both were persistently lower than the sham control throughout the study period till 72 h.
a The hepatic expression of proliferator-activated receptor γ coactivator-1α (PGC-1α) mRNA in the rats receiving bile duct ligation (BDL) or sham operation. Significant decrease of PGC-1α mRNA is found in the BDL rats from 6 to 72 h after inception of the experiment, in comparison to the sham rats. b The hepatic expression of transcriptional factor A (Tfam) mRNA in the rats receiving BDL or sham operation. Significant decrease of Tfam mRNA is found in the BDL rats from 6 to 72 h after the beginning of the experiment, compared to the sham rats. c and d Western blot analysis reveals significant decrease of Tfam protein from 6 to 72 h in the animals treated with bile duct ligation as compared to the sham group. All results represent means ± SD of six animals, * P < 0.05 when comparing the BDL groups with sham
Regulation of mitochondrial antioxidative enzymes
A transient but significant increase of Mn-superoxide dismutase (MnSOD) mRNA was noted in the rats at 3 h after receiving BDL, which reached a maximum at 6 h, following by a return to a level that was not significant from the sham group, denoted by a decompensation at a later time (Fig. 3a). The glutathione peroxidase (GPx) mRNA levels were significantly down-regulated by 6 h following BDL and persistently lower in the BDL rats than in the sham group throughout the study period (Fig. 3b). Consistent with the above changes, the GPx enzyme (Fig. 3c, d) and catalase enzyme (Fig. 3e) activity in the liver homogenates decreased significantly in the BDL rats compared to that in the sham rats at 72 h. Liver total GSH levels were lower at 72 h after BDL, in comparison to the sham group (111.6 ± 30.3 μM vs. 163.8 ± 17.7 μM, P = 0.008; Fig. 4a). The GSH/GSSG ratio in the liver was lower at 72 h after BDL, compared to that of the sham group (7.5 ± 2.6 vs. 23.9 ± 13.4, P = 0.003; Fig. 4b).
a The liver Mn-superoxide dismutase (MnSOD) mRNA expression is significantly elevated in the rats at 3 h after bile duct ligation (BDL), reaching a maximum at 6 h, following by a return to levels that are not significantly different from the sham group. b The glutathione peroxidase (GPx) mRNA of BDL animals is down regulated from 6 to 72 h when compared to the sham group. c, d Western blot analysis reveals a significant decrease of GPx protein at 72 h after BDL, compared to that of the sham group. e The catalase activity in the liver homogenates decreases significantly at 72 h after BDL, compared to the sham group. All results represent means ± SD of 6 animals, * P < 0.05 when comparing the BDL groups with sham
Mitochondrial DNA copy number decreased and the activity of apoptosis significantly increased at 72 h after bile duct ligation via the intrinsic pathway
The amount of mtDNA copy number, as corrected by the amount of nuclear DNA, varied during the course of the experiment, however it decreased significantly at 72 h in the BDL group, compared to that of the sham control (Fig. 5). Histological evidence of liver cell apoptosis was demonstrated by TUNEL staining of the liver tissue. Liver cell apoptosis was not evident until 72 h after BDL, which revealed significantly increased TUNEL-positive cells in the rat livers of the BDL group, comparing to the sham control as depicted in Fig. 6. The consequence of decreased GPx and catalase activity is apoptotic, as well as necrotic cell death. Furthermore, we measured the caspase 9 and caspase 3, which are the active forms of the caspase family. Interestingly, both caspase 9 (Fig. 7a, b) and caspase 3 (Fig. 7c, d) were augmented significantly by 72 h after BDL, in comparison to the sham control. There were no differences in caspase 8, Bcl2, Bax, Fas L and Fas–Fas L complex between the BDL animals and the sham control (Fig. 7e).
Comparison of mitochondrial DNA (mtDNA) copy number in the rat hepatocyte between groups by relative copy number (R c) = 2∆Ct, where ∆Ct is the Ctβ-actin − CtmtDNA. The mtDNA copy number varies during the course of the experiment, but decreases significantly in the rats receiving bile duct ligation (BDL) than in the sham group at 72 h. All results represent means ± SD of six animals, * P = 0.020 when comparing the BDL groups with sham
TdT-mediated dUTP-biotin nick end-labeling stain in the liver tissue. a At 72 h after bile duct ligation (BDL), remarkable amount of positively staining cells are found in the liver tissue. The staining is mainly in the nucleus of the hepatocytes (arrow) but not in the bile ductular epithelial cells (arrowhead). b Contrary to that of the BDL rats, none of the hepatocytes or the bile ductular epithelial cells (arrowhead) are stained in the sham group. Original magnification: 400×
a and b The caspase 9 protein in the rat liver, measured by Western blotting, increases after bile duct ligaton (BDL), which is significantly higher than the sham control at 72 h of experiment. c and d The caspase 3 protein follows the same trend as that in the capase 9, which is significantly higher at 72 h after BDL, compared to the sham group. e caspase 8, Bcl2, Bax, Fas L and Fas–Fas L complex do not change significantly from 1 to 72 h. All results represent means ± SD of 6 animals, * P < 0.05 when comparing the BDL groups with sham
Discussion
Mitochondria are the sites of oxidative phosphorylation and an essential source of ATP production in most tissues including liver [10]. Mitochondrial biogenesis is a complex process, which involves more than 100 proteins encoded by the nucleus coordinating with the 13 proteins encoded by mtDNA [10]. PGC-1α is a master regulator of the process [18, 19] and Tfam stimulates transcription from mtDNA templates [10]. Induced stress responses may alter the expression of specific nuclear genes to uphold the energy metabolism to rescue the cell [9]. Once beyond the threshold, oxidative damage to mtDNA and other components of the mitochondria may occur in the affected cells, which subsequently lead to apoptosis or necrosis [9]. In our study, we observed significant down-regulation of PGC-1α and Tfam mRNAs and Tfam protein within 6 h after inception of cholestasis. Moreover, the derangement of the transcriptional regulation of mitochondrial biogenesis in the cholestatic rats persists throughout the course of the study.
Cells lacking PGC-1α are hypersensitive to death from oxidative stress caused by H2O2 or paraquat [24]. Mice deficient in PGC-1α will develop excessive neurodegeneration after induction of kainic acid-induced seizures or MPTP that causes Parkinsonism [24]. We find a significant reduction in PGC-1α mRNA (but not in protein levels) after BDL, implying a deficient PGC-1α function in the BDL rats. In the report of Vercauteren et al., the rapid induction of PGC-1-related coactivator mRNA does not require de novo protein synthesis [25]. The decrease of PGC-1α transcript in the BDL rats in association with a decrease of Tfam transcript may predispose the cholestatic liver to dampening oxidative stress.
Tfam is essential for human mtDNA transcription and is also probably a key regulator of mtDNA copy number [26]. The significantly decreased Tfam mRNA and protein in the cholestatic rat liver is coincident with significant decrease of mtDNA copy number and significant increase in the number of apoptotic liver cells. In the heart of the tissue-specific Tfam knockouts, Wang et al. found severe respiratory chain deficiency and massive apoptosis in day 9.5 mouse embryos [27]. The importance of Tfam in the maintenance of mtDNA and mitochondrial respiratory function has also been supported by the observation that decreased Tfam expression and mtDNA copy number in animals with heart failure can be ameliorated by Tfam overexpression as well as the defected mitochondrial complex enzyme activities [28]. A recent report of mitochondrial transcription factor in drosophila development further confirms the importance of these factors in oxidative phosphorylation, mitochondrial ATP synthesis, cell proliferation and apoptosis [29]. These reports support our contention that the early decrease of Tfam mRNA and protein levels in the cholestatic rat liver indicates impairment of mitochondrial biogenesis and maintenance immediately after bile duct obstruction.
The consequent effects of mitochondrial transcriptional deregulation are derangement of oxidative repair enzymes, including MnSOD, GPx and catalase, which convert free radicals into less toxic or nontoxic forms [9]. MnSOD converts superoxide radicals to hydrogen peroxide and molecular oxygen within the mitochondrial matrix and GPx converts hydrogen peroxide into water within mitochondria and the cytosol [9]. Catalase also functions to catalyze the decomposition of hydrogen peroxide to water and oxygen [9]. In our study, the transient increase of MnSOD mRNA expression at 3 h after BDL may indicate a short-term compensatory mechanism to overcome the upcoming load of oxidative stress. However, it is followed by a return of MnSOD transcript to a level not different from the sham control, denoting a decompensation in the later phase. On the contrary, a persistent decrease of GPx mRNA transcript from 6 h and thereafter in the BDL rats indicates failure of the cholestatic liver to generate enough GPx for scavenging of H2O2 and protecting the organelles against damaging effects [30]. Our data is consistent with that of Allen which indicates that the expression levels of GPx decrease during some forms of oxidative damage [31]. In our study, catalase activity and GSH level also show significant a decrease by 72 h when the condition of the BDL rats is worsened. Since GPx and catalase are critical enzymes involved in the process of H2O2 detoxification, decreased production of these enzymes may cause further accumulation of H2O2 which facilitates the well known Fenton’ reaction and leads to the generation of the more hazardous hydroxyl radical further precipitating more tissue oxidative damage [32, 33]. These results indicate an early defective mitochondrial GPx and catalase-dependent defense system in the BDL rats.
Apoptosis is an energy-consuming process [34, 35], which has been reported to be involved in reactive oxygen species (ROS) generation and oxidative damage [36]. Excess ROS generation can lead to cell apoptosis [36]. In studies with radioactively labeled precursors, the half-life of liver mitochondria was estimated to be in the range of 3–10 days [37]. When the capacity of the antioxidant system is compromised, the exposure of tissue cells to higher oxidative stress will result in an increase of defective mitochondria, and thus, a cyclic increase in ROS production and oxidative damage [9]. Once beyond a threshold, mitochondria could drive the cell into an irreversible cell death process [9]. In our study, the mtDNA copy number decreases significantly at 72 h after BDL. This decompensation of mitochondrial biogenesis is associated with a significant increase of levels of caspase 9 and 3 and of apoptotic hepatocytes at 72 h of BDL. Apoptotic cell death can be initiated by either an intrinsic or extrinsic pathway, both of which converge at the activation of caspase-3 [38, 39]. Activation of this executioner enzyme is irreversible, resulting in the cleavage of numerous structural and functional proteins and the internucleosomal cleavage of genomic DNA [38]. Death receptors, especially Fas, are widely expressed via the extrinsic pathway in response to evolutionary pressure to eliminate hepatotropic viruses [40]. To activate the intrinsic pathway, mitochondrial proteins are released from the mitochondrial intermembrane space and lead to the activation of pro-apoptotic proteins such as caspase-9, and consequential apoptosis [38, 39]. We found there to be a failure of activation of caspase-8, Bax, Bcl2, Fas L and Fas–Fas L complex in the early phase of BDL in the rats. This indicates that apoptotic cell death is initiated by an intrinsic pathway in the early stage of cholestatic liver injury.
In conclusion, our results indicate an early transcriptional deregulation of the mitochondria after BDL, which results in derangement of oxidative repair enzymes, and finally apoptosis of the hepatocytes through the intrinsic pathway in the cholestatic rats. Future intervention of the cholestatic liver injury should be aimed at maintenance of the transcriptional regulation of the mitochondrial biogenesis within hours after the inception of cholestasis.
Abbreviations
- BDL:
-
Bile duct ligation
- GPx:
-
Glutathione peroxidase
- GSH:
-
Glutathione
- GSSG:
-
Oxidized glutathione
- mRNA:
-
Messenger RNA
- mtDNA:
-
Mitochondrial DNA
- PGC-1α:
-
Peroxisome proliferators-activated receptor γ coactivator-1α
- QRT-PCR:
-
Real-time quantitative reverse transcriptase-polymerase chain reaction
- Tfam:
-
Mitochondrial transcription factor A
References
Suchy FJ (2003) Clinical problems with developmental anomalies of the biliary tract. Semin Gastrointest Dis 14:156–164
Bezerra JA, Balistreri WF (2001) Cholestatic syndromes of infancy and childhood. Semin Gastrointest Dis 12:54–65
Bates MD, Bucuvalas JC, Alonso MH, Ryckman FC (1998) Biliary atresia: pathogenesis and treatment. Semin Liver Dis 18:281–293. doi:10.1055/s-2007-1007164
Kelly DA, Davenport M (2007) Current management of biliary atresia. Arch Dis Child 92:1132–1135. doi:10.1136/adc.2006.101451
Aykac G, Ozdemirler G, Alptekin N, Arican N, Oz B, Uysal M, Oz H (1989) The hepatic lipid peroxidation, copper and fibrosis in cholestatic rats. Pharmacol Res 21:701–706. doi:10.1016/1043-6618(89)90229-6
Panozzo MP, Basso D, Balint L, Biasin MR, Bonvicini P, Metus P, Infantolino D, Plebani M (1995) Altered lipid peroxidation/glutathione ratio in experimental extrahepatic cholestasis. Clin Exp Pharmacol Physiol 22:266–271. doi:10.1111/j.1440-1681.1995.tb01992.x
Sokol RJ, Devereaux M, Khandwala R, O’Brien K (1993) Evidence for involvement of oxygen free radicals in bile acid toxicity to isolated rat hepatocytes. Hepatology 17:869–881. doi:10.1002/hep.1840170518
Parola M, Leonarduzzi G, Robino G, Albano E, Poli G, Dianzani MU (1996) On the role of lipid peroxidation in the pathogenesis of liver damage induced by long-standing cholestasis. Free Radic Biol Med 20:351–359. doi:10.1016/0891-5849(96)02055-2
Lee HC, Wei YH (2005) Mitochondrial biogenesis and mitochondrial DNA maintenance of mammalian cells under oxidative stress. Int J Biochem Cell Biol 37:822–834. doi:10.1016/j.biocel.2004.09.010
Forestier M, Solioz M, Isbeki F, Talos C, Reichen J, Krahenbuhl S (1997) Hepatic mitochondrial proliferation in rats with secondary biliary cirrhosis: time course and mechanisms. Hepatology 26:386–391. doi:10.1002/hep.510260219
Engin A, Bozkurt BS, Altan N, Memiş L, Bukan N (2003) Nitric oxide-mediated liver injury in the presence of experimental bile duct obstruction. World J Surg 27:253–255. doi:10.1007/s00268-002-6710-0
Chen CH, Nagayama K, Enomoto N, Miyasaka Y, Kurosaki M, Sakamoto N, Maekawa S, Kakinuma S, Ikeda T, Izumi N, Sato C, Watanabe M (2005) Enhancement of mitochondrial gene expression in the liver of primary biliary cirrhosis. Hepatol Res 31:24–30. doi:10.1016/j.hepres.2004.09.007
Kass GE (2006) Mitochondrial involvement in drug-induced hepatic injury. Chem Biol Interact 163:145–159. doi:10.1016/j.cbi.2006.06.007
Saravanan R, Viswanathan P, Pugalendi KV (2006) Protective effect of ursolic acid on ethanol-mediated experimental liver damage in rats. Life Sci 78:713–718. doi:10.1016/j.lfs.2005.05.060
Jeong WI, Park O, Gao B (2008) Abrogation of the antifibrotic effects of natural killer cells/interferon-gamma contributes to alcohol acceleration of liver fibrosis. Gastroenterology 134:248–258. doi:10.1053/j.gastro.2007.09.034
Tiao MM, Lin TK, Kuo FY, Huang CC, Du YY, Chen CL, Chuang JH (2007) Early stage of biliary atresia is associated with significant changes in 8-hydroxydeoxyguanosine and mitochondrial copy number. J Pediatr Gastroenterol Nutr 45:329–334. doi:10.1097/MPG.0b013e3180cc2c0f
Parisi MA, Clayton DA (1991) Similarity of human mitochondrial transcription factor 1 to high mobility group proteins. Science 252:965–969. doi:10.1126/science.2035027
Nisoli E, Clementi E, Moncada S, Carruba MO (2004) Mitochondrial biogenesis as a cellular signaling framework. Biochem Pharmacol 67:1–15. doi:10.1016/j.bcp.2003.10.015
Wu Z, Puigserver P, Andersson U, Zhang C, Adelmant G, Mootha V, Troy A, Cinti S, Lowell B, Scarpulla RC, Spiegelman BM (1999) Mechanisms controlling mitochondrial biogenesis and respiration through the thermogenic coactivator PGC-1. Cell 98:115–124. doi:10.1016/S0092-8674(00)80611-X
Wang G, Shen H, Rajaraman G, Roberts MS, Gong Y, Jiang P, Burczynski F (2007) Expression and antioxidant function of liver fatty acid binding protein in normal and bile-duct ligated rats. Eur J Pharmacol 560:61–68. doi:10.1016/j.ejphar.2007.01.015
Lee CW, Chuang JH, Wang PW, Chang NK, Wang HC, Huang CC, Tiao MM, Lo SK (2006) Effect of glucocorticoid pretreatment on oxidative liver injury and survival in jaundiced rats with endotoxin cholangitis. World J Surg 30:2217–2226. doi:10.1007/s00268-006-0143-0
Diehl AM, Goodman Z, Ishak KG (1988) Alcohol like liver disease in nonalcoholics. A clinical and histologic comparison with alcohol-induced liver injury. Gastroenterology 95:1056–1062
Kim MM, Clinger JD, Masayesva BG, Ha PK, Zahurak ML, Westra WH, Califano JA (2004) Mitochondrial DNA quantity increases with histopathologic grade in premalignant and malignant head and neck lesions. Clin Cancer Res 10:8512–8515. doi:10.1158/1078-0432.CCR-04-0734
Spiegelman BM (2007) Transcriptional control of mitochondrial energy metabolism through the PGC1 coactivators. Novartis Found Symp 287:60–69. doi:10.1002/9780470725207.ch5
Vercauteren K, Pasko RA, Gleyzer N, Marino VM, Scarpulla RC (2006) PGC-1-related coactivator: immediate early expression and characterization of a CREB/NRF-1 binding domain associated with cytochrome c promoter occupancy and respiratory growth. Mol Cell Biol 26:7409–7419. doi:10.1128/MCB.00585-06
Ekstrand MI, Falkenberg M, Rantanen A, Park CB, Gaspari M, Hultenby K, Rustin P, Gustafsson CM, Larsson NG (2004) Mitochondrial transcription factor A regulates mtDNA copy number in mammals. Hum Mol Genet 13:935–944. doi:10.1093/hmg/ddh109
Wang J, Silva JP, Gustafsson CM, Rustin P, Larsson NG (2001) Increased in vivo apoptosis in cells lacking mitochondrial DNA gene expression. Proc Natl Acad Sci USA 98:4038–4043. doi:10.1073/pnas.061038798
Ikeuchi M, Matsusaka H, Kang D, Matsushima S, Ide T, Kubota T, Fujiwara T, Hamasaki N, Takeshita A, Sunagawa K, Tsutsui H (2005) Overexpression of mitochondrial transcription factor a ameliorates mitochondrial deficiencies and cardiac failure after myocardial infarction. Circulation 112:683–690. doi:10.1161/CIRCULATIONAHA.104.524835
Adán C, Matsushima Y, Hernández-Sierra R, Marco-Ferreres R, Fernández-Moreno MA, González-Vioque E, Calleja M, Aragón JJ, Kaguni LS, Garesse R (2008) Mitochondrial transcription factor B2 is essential for metabolic function in Drosophila melanogaster development. J Biol Chem 283:12333–12342. doi:10.1074/jbc.M801342200
Salvi M, Battaglia V, Brunati AM, La Rocca N, Tibaldi E, Pietrangeli P, Marcocci L, Mondovì B, Rossi CA, Toninello A (2007) Catalase takes part in rat liver mitochondria oxidative stress defense. J Biol Chem 282:24407–24415. doi:10.1074/jbc.M701589200
Allen RG, Balin AK (2003) Effects of oxygen on the antioxidant responses of normal and transformed cells. Exp Cell Res 289:307–316. doi:10.1016/S0014-4827(03)00279-9
Aust SD, Morehouse LA, Thomas CE (1985) Role of metals in oxygen radical reactions. J Free Radic Biol Med 1:3–25. doi:10.1016/0748-5514(85)90025-X
Dikalova AE, Kadiiska MB, Mason RP (2001) An in vivo ESR spin-trapping study: free radical generation in rats from formate intoxication–role of the Fenton reaction. Proc Natl Acad Sci USA 98:13549–13553. doi:10.1073/pnas.251091098
Sokol RJ, Devereaux M, Khandwala RA (1991) Effect of dietary lipid and vitamin E on mitochondrial lipid peroxidation and hepatic injury in the bile ductligated rats. J Lipid Res 32:1349–1357
Wasserman DH, Cherrington AD (1991) Hepatic fuel metabolism during muscular work: role and regulation. Am J Physiol 260:E811–E824
Nègre-Salvayre A, Hirtz C, Carrera G, Cazenave R, Troly M, Salvayre R, Pénicaud L, Casteilla L (1997) A role for uncoupling protein-2 as a regulator of mitochondrial hydrogen peroxide generation. FASEB J 11:809–815
Lipsky NG, Pedersen PL (1981) Mitochondrial turnover in animal cells. Half lives of mitochondria and mitochondrial subfractions of rat liver based on (14C)bicarbonate incorporation. J Biol Chem 256:8652–8657
Johnson AL, Bridgham JT (2002) Caspase-mediated apoptosis in the vertebrate ovary. Reproduction 124:19–27. doi:10.1530/rep.0.1240019
Johnson AL, Ratajczak C, Haugen MJ, Liu HK, Woods DC (2007) Tumor necrosis factor-related apoptosis inducing ligand expression and activity in hen granulosa cells. Reproduction 133:609–616. doi:10.1530/REP-06-0287
Guicciardi ME, Gores GJ (2005) Apoptosis: a mechanism of acute and chronic liver injury. Gut 54:1024–1033. doi:10.1136/gut.2004.053850
Acknowledgments
The authors thank Jo B. Harnaha for major contributions to this work. This work was supported by grants (CMRPG850282, CMRPG870451) from the Chang Gung Memorial Hospital, and grant (NSC 96-2314-B-182A-052-MY2) from the National Science Council of the Republic of China, Taiwan.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tiao, MM., Lin, TK., Liou, CW. et al. Early transcriptional deregulation of hepatic mitochondrial biogenesis and its consequent effects on murine cholestatic liver injury. Apoptosis 14, 890–899 (2009). https://doi.org/10.1007/s10495-009-0357-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10495-009-0357-3