Abstract
Injection drug use has been the leading route of HIV transmission in Iran. We assessed HIV prevalence, risk behaviors, and uptake of prevention services among people who inject drugs (PWID) in Iran between 2010 and 2020. We also examined the individual and environmental determinants of HIV among PWID. PWID were recruited in major cities across the country in three national bio-behavioral surveillance surveys in 2010, 2014, and 2020. Participants were tested for HIV and interviewed using a behavioral questionnaire. Between 2010 and 2020, the prevalence of HIV (15.1% to 3.5%), receptive needle sharing (25.2% to 3.9%) and unprotected sex (79.4% to 65.2%) decreased. Moreover, uptake of free needle/syringe increased (57.4% to 87.9%), while uptake of free condoms remained relatively stable across the surveys (34.3% to 32.6%). Multivariable analysis for the 2020 survey showed that a history of homelessness, incarceration, and a longer injection career significantly increased the odds of HIV seropositivity. During the past decade, HIV prevalence and drug- and sexual-related risk behaviors decreased among Iranian PWID. However, individual and structural determinants continue to drive HIV among this population. HIV prevention, diagnosis, and treatment among marginalized PWID with a history of homelessness or incarceration and those who inject drugs for a longer period, should be further prioritized in HIV care planning and resource allocation in Iran.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
People who inject drugs (PWID) are at an elevated risk of acquiring and transmitting HIV through needle/syringe sharing and unprotected sex [1, 2]. A global systematic review in 2017 estimated the population size of PWID as ~ 15.6 million, 17.8% of whom were living with HIV [3]. Another systematic review estimated that 23.9% of PWID had recently engaged in receptive needle/syringe sharing, with PWID in the Middle East and North Africa (MENA) ranking first (33.5%) globally [4]. In MENA, PWID, with an estimated population size of ~ 626,000, account for most HIV new infections in the region [5, 6]. HIV prevalence among PWID in MENA overall ranges from 10 to 15% [5].
Iran has an estimated 208,000 PWID who bear the highest prevalence of HIV among all its key populations at risk of HIV [7,8,9]. Although the proportion of sexual transmission of HIV has been increasing in recent years (e.g., around 37% of the identified HIV new cases have been infected through unprotected sex) [10, 11], injection drug use has remained the primary mode of HIV transmission in Iran during the past few decades [12]. A recent meta-analysis estimated the pooled HIV prevalence among PWID in Iran to be 14.3% before 2007 and 9.7% afterwards [13]. Despite PWID’s relatively adequate knowledge about HIV prevention, high-risk sexual and injection behaviors are frequent [9, 14].
In response to concerns regarding prevalent high-risk behaviors and the spread of HIV, targeting key affected populations, including PWID, has been one of the main focuses of the HIV surveillance system in Iran. This surveillance system has contributed to assessing the burden of disease, developing, targeting, and evaluating interventions, as well as monitoring harm reduction efforts over time [15]. Since the rise of the HIV epidemic among PWID in the late 1990s, Iran’s drug policy has shifted from a criminalization approach that criminalized any drug use to a more medicalized approach, and an extensive network of drug treatment and harm reduction services have been established [16]. Iran has also developed harm reduction programs tailored for PWID during the past ten years, including needle and syringe programs (NSP), opioid agonist therapy (OAT), educational programs, and HIV testing. These services are available through drop-in centers, voluntary counseling and testing centers, outreach care provision, and mobile harm reduction centers [17, 18]. Although evaluating changes in PWID’s behaviors is of utmost importance, few small-scale studies have tried to examine HIV prevalence, HIV-related risk behaviors, and harm reduction uptake among PWID in Iran. Moreover, studies with sufficient statistical power and robust survey methodologies quantifying HIV-associated risk factors are lacking. In this study, we aimed to assess changes in HIV prevalence, risk behaviors, and harm reduction utilization of PWID in Iran using the extensive bio-behavioral data collected from 2010 to 2020. We also examined the individual and environmental determinants of HIV seropositivity in 2020 to help inform potential interventions and resource allocation activities.
Methods
Setting and Sampling
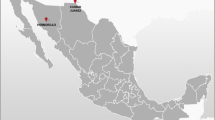
This study leveraged data from three national bio-behavioral surveillance surveys of Iranian PWID from 2010 to 2020. The surveys have been previously described [9, 19, 20]. In brief, the surveys were conducted in diverse cities representing different geographical regions across the country (Fig. 1). We recruited 2546 and 2399 PWID using a convenience sampling method from harm reduction facilities (e.g., drop-in centers, shelters, addiction treatment centers) catered towards PWID as well as through outreach efforts in both 2010 and 2014 surveys. In the 2020 survey (July 2019 to March 2020), 2684 PWID were recruited using a respondent-driven sampling (RDS) approach. RDS is a recruitment method based on long-chain peer referrals to identify and recruit a diverse representation of PWID [21]. The sampling method in 2020 was modified based on the feedback from the Ministry of Health and Medical Education (MoHME) and the need for improving the rigor and quality of HIV surveillance surveys in Iran.
The selection of the facilities in 2010 and 2014 was informed by the presumed level of HIV prevalence in PWID in the previous survey round in 2008, and input from the MoHME’s HIV experts regarding the logistical and capacity constraints of the facilities. The recruitment of participants in 2020 was consistent with the RDS methodology and started with a non-random selection of seeds. Three referral coupons—valid for 3 weeks—were provided for each seed, and participants were trained to use them to recruit up to three peers. This process was repeated with succeeding recruits until the targeted sample size was reached.
Eligibility criteria in all studies were (i) ≥ 18 years of age at the time of the study; (ii) self-reporting illegal drug injection in the previous year; (iii) Iranian citizenship; (iv) residing in the surveyed cities, and (v) providing a valid referral coupon consistent with the study methodology in the 2020 survey. Participants received a monetary incentive for the interview and HIV test in all three surveys and additional incentives for every successful peer referral in the 2020 survey.
Behavioral Data Collection and HIV Testing
A group of trained staff collected the data using a standard behavioral questionnaire and through face-to-face interviews in a private room at each study site. The study questionnaire consisted of sections on demographic characteristics, drug use and injection-related behaviors, sexual practices, history of substance use treatment, and other utilization of harm reduction services. After providing verbal consent and completing the interview, participants received HIV pre-test counselling and consenting PWID were tested for HIV. As rapid HIV testing was unavailable during the 2010 and 2014 surveys, HIV serostatus was estimated using the dried blood spot (DBS) technique. DBS samples were assessed for HIV antibodies by ELISA using a bioMérieux Vironostika Uni-Form II Ag/Ab kit. All positive samples and 10% of the negative samples were rechecked by a Bio-Rad Genscreen Plus HIV Ag-Ab kit. In the 2020 survey, HIV testing was performed by SD-Bioline, South Korea rapid test, and if reactive, confirmed by Unigold HIV rapid test.
Variables
The primary outcome across all surveys was HIV seropositivity status (positive or negative). We examined correlates of HIV with socio-demographic, structural, and injection-related variables. Socio-demographic variables included age at interview (< 30, or ≥ 30 years old), sex (male or female), educational level (≤ high school or > high school), marital status (single, currently married or divorced/widowed), and employment (having a permanent job, having a temporary job or unemployed). Environmental and structural variables included homelessness (never, yes, before the last 12 months or yes, within the last 12 months) and incarceration history (never, yes, before the last 12 months or yes, within the last 12 months). Individual-related variables included age at first drug use (< 15, 15–19, 20–24 or ≥ 25 years old), length of injecting career (< 5, 5–10 or > 10 years), primary drug injected (opioids or stimulants), daily injection (yes or no), public injecting (yes or no), receptive needle/syringes sharing (yes or no), and unprotected sex (yes or no). Harm reduction service usage variables also included receipt of free needles/syringes (yes or no), free condoms (yes or no), and being on OAT (yes or no). All behavioral variables referred to activities in recent months unless otherwise specified. However, the definition of recent differed across the surveys for certain variables (i.e., daily injection, public injecting, and receptive needle/syringes sharing), varying from last month to the last 12 months.
Statistical Analysis
We calculated and reported descriptive statistics and frequencies along with 95% confidence intervals (CI) for HIV prevalence, socio-demographic characteristics, risk behaviors, and harm reduction service utilization in all three surveys. HIV prevalence was compared across subgroups of independent variables using the χ2 test. Bivariable and multivariable logistic regression models were built to identify the significant correlates of HIV seropositivity among PWID for the survey in 2020. The inclusion of individual and environmental risk factors for HIV in the multivariable analysis was guided by the HIV risk environment framework [22, 23]. We constructed the multivariable regression model in four stages [20, 24]. The first multivariable model was performed for socio-demographic variables. The second model included environmental variables, including homelessness and incarceration history. In the third model, we conducted a multivariable model for individual risk factors. Variables with a significant p-value in each model were included in the final multivariable regression model. Stata v.15 (StataCorp, College Station, Texas, USA) was used to analyze the data, and p-values < 0.05 were considered statistically significant throughout. Given the lack of consensus on the validity of weighted regression models, unweighted regression models were performed to avoid error rate, have better coverage, increase accuracy, and avoid biased results arising from the RDS weighted analyses [25]. The RDS unweighted regression has been supported by the growing body of literature [26, 27]. Despite this, we also reported RDS-adjusted estimates for HIV prevalence, overall and in subgroups of PWID recruited in the 2020 survey, which considered network size and homophily within networks. RDS-adjusted estimates for HIV prevalence were calculated in RDS-Analyst.
Ethical Considerations
Ethical issues included the guarantee of the participants’ confidentiality using anonymous questionnaires and obtaining verbal informed consent for both biological and behavioral data collection procedures. Participants’ refusal to take part in the study did not affect their access to healthcare services in any manner. The survey protocols were reviewed and approved by the Kerman University of Medical Sciences ethics committee (Ethics Codes: IR.KMU.REC.597, IR.KMU.REC.93.205, and IR.KMU.REC.1397.573; IR.NIMAD.REC.1398.029).
Results
HIV Prevalence
After removal of missing data on the outcome measure, the analytic sample included 2,349 participants in 2010, 2,307 in 2014, and 2,684 in 2020. Overall, HIV prevalence was 15.1% (95% CI 13.6, 16.6) in 2010, 9.3% (95% CI 8.1, 10.5) in 2014, and 3.5% (95% CI 2.9, 4.3) in 2020 (Fig. 2).
Participants Characteristics and Risk Behaviors Over Time
Participants in the 2010 survey were younger than those in the 2014 and 2020 surveys (mean age = 34.5, 36.8, and 40.2, respectively). While most PWID were male across surveys, the proportion of female participants slightly increased (2.2%, 2.5%, and 3.3%). The proportion of participants with divorced/widowed marital status (21.8%, 24.7%, and 38.3%), and a permanent job (2.2%, 14.8%, and 17.8%) also increased. The prevalence of 10+ years of injecting career (30.4%, 45.6%; and 49.4%), injecting opioids as the primary drug (74.2% and 77.9%), daily injection (26.3% and 50.5%), and public injecting (32.6%, 26.9%, and 69.6%) increased. However, the proportion of participants who reported receptive needle/syringe sharing (25.2%, 10.4%, and 3.9%), unprotected sex (79.4%, 67.9%, and 65.2%), and a history of incarceration decreased (78.2%, 76.5%, and 66.1%). While an increase was observed in the uptake of free needles/syringes (68.8%, 57.4%, and 87.9%), uptake of free condoms remained stable across the surveys (34.3%, 36.1%, and 32.6%), and a downward trend was observed for PWID who reported being on OAT (35.6%, 37.6%, and 25.0%) (Table 1).
Factor Associated with HIV
In 2010, HIV prevalence was significantly higher among PWID who were ≥ 30 years (17.5% vs. 10.1%; χ2 = 22.770, p = 0.023), had ≤ high school education (15.6% vs. 4.5%; χ2 = 9.724, p = 0.013), been ever incarcerated (16.5% vs. 9.3%; χ2 = 16.272, p = 0.014), injected drugs for 10+ years (21.7% vs. 10.3% for < 5 years; χ2 = 39.622, p = 0.011), not engaged in unprotected sex in the last year (20.8% vs. 11.1%; χ2 = 17.755, p = 0.005), and received free condoms (17.8% vs. 13.6%; χ2 = 7.295, p = 0.030). In 2014, HIV prevalence was significantly higher among PWID who were older than 30 years (10.5% vs. 4.7%; χ2 = 15.164, p < 0.001), were female compared to males (24.1% vs. 8.9%; χ2 = 15.459, p < 0.001), were single compared to married (13.9% vs. 4.3%; χ2 = 53.713, p < 0.001), had a temporary job compared to permanent job (10.8% vs. 3.8%; χ2 = 15.275, p < 0.001), been ever incarcerated (10.1% vs. 6.6%; χ2 = 5.989, p = 0.014), initiated drug use between 15 to 19 years old (11.0% vs. 5.5% for ≥ 25 years; χ2 = 9.563, p = 0.023), injected drugs for 10+ years (14.4% vs. 2.2% for < 5 years; χ2 = 65.593, p < 0.001), primarily injected opiates in the last month (10.2% vs. 5.5%; χ2 = 8.802, p = 0.003), reported daily injection in the last month (14.1% vs. 7.7%; χ2 = 21.482, p < 0.001), reported receptive needle/syringe sharing in the last month (18.1% vs. 8.4%; χ2 = 23.394, p < 0.001), received free needles/syringes in the last year (10.1% vs. 7.3%; χ2 = 5.433, p = 0.020), and were on OAT (11.3% vs. 8.1%; χ2 = 6.379, p = 0.012) (Table 2).
In 2020, HIV prevalence was significantly higher among PWID who were older than 30 years (3.9% vs. 1.0%; χ2 = 6.258, p = 0.012), experienced homelessness (5.7% vs. 2.2% for never experienced homelessness; χ2 = 12.160, p = 0.002), been incarcerated before the previous year (4.7% vs. 1.3% for never incarcerated; χ2 = 18.844, p < 0.001), injected for 10+ years (5.6% vs. 1.2% for < 5 years; χ2 = 34.773, p < 0.001), and not engaged in unprotected sex in the last 3 months (4.8% vs. 2.6%; χ2 = 6.222, p = 0.013) (Table 3). The final multivariable logistic regression model for the 2020 survey showed that HIV seropositivity was significantly associated with homelessness (AOR 2.10, 95% CI 1.11, 3.95; p = 0.021), incarceration (AOR 2.66, 95% CI 1.33, 5.32; p = 0.006), and having a longer injecting career (AOR 3.27, 95% CI 1.50, 7.14; p = 0.003) (Table 4).
Discussion
Our results suggest that the prevalence of HIV has declined among PWID recruited in the three consecutive bio-behavioral surveillance surveys in Iran. A decline was also observed in the prevalence of receptive needle/syringe sharing and unprotected sex. There was also an increase in uptake of free needles/syringes. However, the proportion of those who reported daily injection and public injecting has increased. Our final multivariable analysis based on the 2020 survey showed that homelessness, incarceration, and longer injecting careers were significantly associated with HIV seropositivity.
The decline in HIV prevalence could be associated with several factors and should be interpreted with caution. While we employed comparable eligibility criteria and recruited participants from the same harm reduction facilities across the surveys, PWID were recruited using a convenience sampling method in 2010 and 2014 and RDS in 2020, leading to potentially heterogeneous populations being recruited in different rounds. Although a decline in HIV prevalence may suggest a decrease in HIV incidence among PWID in Iran [28], it could also be partly associated with the high mortality rate among people living with HIV in Iran. Indeed, data from the National HIV/AIDS Case Registry System suggests that the survival rate of people living with HIV was 67% for 10 years, and by June 2016, 25.1% of registered people living with HIV had died due to AIDS-related diseases [29]. While the availability of antiretroviral therapy has increased in recent years, its coverage is insufficient (e.g., only 25% of people living with HIV in Iran had received antiretroviral therapy by the end of 2019) [30].
The decline in HIV prevalence could also be partly related to the expansion of HIV-related harm reduction programs across the country. During the last 10 years, Iran has implemented diverse harm reduction programs for PWID, and the coverage of prevention programs has expanded over time. These harm reduction programs include NSP, OAT, behavioral counseling for PWID and their sexual partners, and HIV testing and counseling [17, 31]. Our results showed that while receptive needle/syringe sharing has decreased over time, uptake of free-of-charge needles/syringes has increased from 57% to 87%. Reduction in the prevalence of HIV and risk behaviors which is coincident with increased harm reduction services utilization, have also been reported in other international settings [32, 33]. However, adequate availability of harm reduction services is only part of the wider risk environment framework that helps reduce HIV acquisition risk and lower HIV new infections [23, 24].
Despite the expansion of harm reduction interventions across Iran and increased uptake of services among PWID in the past decade, several limitations exist and need to be addressed. First, despite the increasing number of female PWID, they are disproportionately under-represented in harm reduction service provision in Iran. Studies suggest that while women include almost 10% of people who use drugs in Iran, the proportion of female and male individuals who use the addiction treatment services in Iran is 1 in 17 [17, 34]. The high level of stigma and male-dominant treatment services have been proposed as potential contributors to the lower representation of females in these treatment services [35, 36]. While women-only drug treatment and harm reduction services have been developed to address women’s specific needs, these centers are primarily located in Tehran, the country’s capital, and women face multiple barriers to entering treatment and using these services [37, 38]. The expansion and development of these services is required to address female PWID’s specific needs and implement other strategies to effectively reach and engage women in HIV prevention and drug treatment programs. Second, the increasing prevalence of public injecting in the past decade calls for novel and innovative interventions (e.g., supervised injection facilities) to be introduced to care provision to help reduce high-risk injection practices [39]. The integration of this service into Iran’s harm reduction programs is indeed supported by a high willingness of Iranian PWID to use the service and could help reduce harms among PWID [20].
Our multivariable analysis showed that the length of injecting career and environmental adversities, such as incarceration and homelessness experienced by PWID increased the odds of HIV seropositivity. The link between the duration of injecting and increased odds of HIV indicates how cumulative exposures to high-risk practices or exposures makes PWID more vulnerable to HIV acquisition [40, 41]. The association of HIV with incarceration and homelessness has also been supported by a body of international evidence. For example, a global systematic review associated incarceration with an 81% greater risk of HIV acquisition among PWID and highlighted the importance of decriminalizing drugs [42]. Additionally, it is estimated that in comparison to PWID with stable housing, homeless or unstably housed PWID are 1.5 times more likely to acquire HIV [43]. Indeed, PWID experiencing homelessness experience multiple adversities [43,44,45], such as unemployment, food insecurity, and incarceration. They are also more likely to be involved in high-risk injection and sexual behaviors, and therefore, less likely to access and utilize harm reduction services [43, 46]. Addressing homelessness among PWID is a complex issue requiring context-specific multi-layered social and political interventions. However, programs such as Housing First, have shown promise in improving health, well-being, social integrations, reduction in drug use, and encounter with the criminal justice system among marginalized PWID in high-income settings and could also be a viable option for low- and middle-income countries, including Iran [47, 48].
Limitations
We acknowledge the limitations of this study. First, behavioral data were collected through face-to-face interviews, which may be subject to social desirability and under-reporting biases. We employed gender-matched experienced interviewers and trained them to help address this concern. Second, participants were not followed up over time, and they were recruited with different sampling strategies; therefore, variation between the studies’ findings could be partly due to divergent selection of PWID subgroups. Third, differences across studies measuring recent timeframe for some behavioral variables could have introduced bias to the findings. Harmonizing the surveillance survey methodologies and using comparable sampling design and questionnaire is recommended. Fourth, although efforts were made to enroll PWID from diverse geographical areas, these samples may not represent PWID in all areas of the country as participants were recruited from the major cities of the most populated provinces. Lastly, the study’s design was cross-sectional, reducing the ability to infer causality from the observed associations.
Conclusion
HIV prevalence and related risk behaviors have declined among PWID in Iran during the past decade. Although the decrease in HIV prevalence and risk behaviors is promising, HIV prevalence remained considerably high among specific subgroups of PWID. There is still plenty of room for improvement to achieve public health goals, such as moving towards no new cases of HIV. Indeed, future HIV outbreaks among PWID in Iran are highly likely and continuous surveillance and investments in HIV prevention and harm reduction programs are warranted. Moreover, since structural factors appear to significantly contribute to HIV acquisition among PWID in Iran, developing upstream interventions aimed at tackling these inequities are strongly recommended.
Data Availability
Data are owned by the MoHME of Iran and are available from the HIV/STI office located at Iran’s MoHME (E-mail: aids@behdasht.gov.ir; Tel: + 98-21-81455055) for researchers who meet the criteria for access to confidential data. The authors of this research were the implementers of the survey and had access to the data with permission obtained from the MoHME’s HIV/STI office.
References
Mathers BM, Degenhardt L, Phillips B, Wiessing L, Hickman M, Strathdee SA, et al. Global epidemiology of injecting drug use and HIV among people who inject drugs: a systematic review. Lancet. 2008;372(9651):1733–45.
Meader N, Semaan S, Halton M, Bhatti H, Chan M, Llewellyn A, et al. An international systematic review and meta-analysis of multisession psychosocial interventions compared with educational or minimal interventions on the HIV sex risk behaviors of people who use drugs. AIDS Behav. 2013;17(6):1963–78.
Degenhardt L, Peacock A, Colledge S, Leung J, Grebely J, Vickerman P, et al. Global prevalence of injecting drug use and sociodemographic characteristics and prevalence of HIV, HBV, and HCV in people who inject drugs: a multistage systematic review. Lancet Glob Health. 2017;5(12):e1192–207.
Tran LT, Peacock A, Colledge S, Memedovic S, Grebely J, Leung J, et al. Injecting risk behaviours amongst people who inject drugs: a global multi-stage systematic review and meta-analysis. Int J Drug Policy. 2020;84:102866.
Mumtaz GR, Weiss HA, Thomas SL, Riome S, Setayesh H, Riedner G, et al. HIV among people who inject drugs in the Middle East and North Africa: systematic review and data synthesis. PLoS Med. 2014;11(6):e1001663.
Mumtaz GR, Awad SF, Feizzadeh A, Weiss HA, Abu-Raddad LJ. HIV incidence among people who inject drugs in the Middle East and North Africa: mathematical modelling analysis. J Int AIDS Soc. 2018;21(3):e25102.
Nikfarjam A, Shokoohi M, Shahesmaeili A, Haghdoost AA, Baneshi MR, Haji-Maghsoudi S, et al. National population size estimation of illicit drug users through the network scale-up method in 2013 in Iran. Int J Drug Policy. 2016;31:147–52.
Haghdoost A, Danesh A, Sharifi H, Shokoohi M, Khajehkazemi R, Mirzazadeh A. HIV Bio-Behavioral Surveillance Survey (BBSS) among people who inject drugs, IR Iran in 2014: project report. Tehran: HIV/STI Surveillance Research Center, and WHO Collaborating Center for HIv Surveillance, Kerman University of Medical Sciences, Kerman, Iran. 2014.
Khajehkazemi R, Osooli M, Sajadi L, Karamouzian M, Sedaghat A, Fahimfar N, et al. HIV prevalence and risk behaviours among people who inject drugs in Iran: the 2010 National Surveillance Survey. Sex Trans Infect. 2013;89(Suppl 3):iii29–32.
Karamouzian M, Madani N, Doroudi F, Haghdoost AA. Improving the quality and quantity of HIV data in the Middle East and North Africa: key challenges and ways forward. Int J Health Policy Manag. 2017;6(2):65.
Ministry of Health and Medical Education. Islamic Republic of Iran, AIDS progress report on monitoring of the United Nations general assembly special session on HIV and AIDS. National AIDS Committee Secretariat. 2015.
Nasirian M, Doroudi F, Gooya MM, Sedaghat A, Haghdoost AA. Modeling of human immunodeficiency virus modes of transmission in Iran. J Res Health Sci. 2012;12(2):81–7.
Rahimi J, Gholami J, Amin-Esmaeili M, Fotouhi A, Rafiemanesh H, Shadloo B, et al. HIV prevalence among people who inject drugs (PWID) and related factors in Iran: a systematic review, meta-analysis and trend analysis. Addiction. 2020;115(4):605–22.
Khajehkazemi R, Haghdoost A, Navadeh S, Setayesh H, Sajadi L, Osooli M, et al. Risk and vulnerability of key populations to HIV infection in Iran; knowledge, attitude and practises of female sex workers, prison inmates and people who inject drugs. Sex Health. 2014;11(6):568–74.
Gökengin D, Doroudi F, Tohme J, Collins B, Madani N. HIV/AIDS: trends in the Middle East and North Africa region. Int J Infect Dis. 2016;44:66–73.
Alam-Mehrjerdi Z, Abdollahi M, Higgs P, Dolan K. Drug use treatment and harm reduction programs in Iran: a unique model of health in the most populated Persian Gulf country. Asian J Psychiatr. 2015;16:78–83.
Ekhtiari H, Noroozi A, Farhoudian A, Radfar SR, Hajebi A, Sefatian S, et al. The evolution of addiction treatment and harm reduction programs in Iran: a chaotic response or a synergistic diversity? Addiction. 2020;115(7):1395–403.
Shokoohi M, Karamouzian M, Osooli M, Sharifi H, Fahimfar N, Haghdoost A, et al. Low HIV testing rate and its correlates among men who inject drugs in Iran. Int J Drug Policy. 2016;32:64–9.
Esmaeili A, Shokoohi M, Danesh A, Sharifi H, Karamouzian M, Haghdoost A, et al. Dual unsafe injection and sexual behaviors for HIV infection among people who inject drugs in Iran. AIDS Behav. 2019;23(6):1594–603.
Khezri M, Karamouzian M, Sharifi H, Ghalekhani N, Tavakoli F, Mehmandoost S, et al. Willingness to utilize supervised injection facilities among people who inject drugs in Iran: Findings from 2020 national HIV bio-behavioral surveillance survey. Int J Drug Policy. 2021;97:103355.
Solomon SS, McFall AM, Lucas GM, Srikrishnan AK, Kumar MS, Anand S, et al. Respondent-driven sampling for identification of HIV-and HCV-infected people who inject drugs and men who have sex with men in India: a cross-sectional, community-based analysis. PLoS Med. 2017;14(11):e1002460.
Rhodes T. Risk environments and drug harms: a social science for harm reduction approach. Amsterdam: Elsevier; 2009. p. 193–201.
Strathdee SA, Hallett TB, Bobrova N, Rhodes T, Booth R, Abdool R, et al. HIV and risk environment for injecting drug users: the past, present, and future. Lancet. 2010;376(9737):268–84.
McAuley A, Palmateer NE, Goldberg DJ, Trayner KM, Shepherd SJ, Gunson RN, et al. Re-emergence of HIV related to injecting drug use despite a comprehensive harm reduction environment: a cross-sectional analysis. Lancet HIV. 2019;6(5):e315–24.
Avery L, Rotondi N, McKnight C, Firestone M, Smylie J, Rotondi M. Unweighted regression models perform better than weighted regression techniques for respondent-driven sampling data: results from a simulation study. BMC Med Res Methodol. 2019;19(1):1–13.
Saleem HT, Likindikoki S, Nonyane BA, Nkya IH, Zhang L, Mbwambo J, et al. Correlates of non-fatal, opioid overdose among women who use opioids in Dar es Salaam, Tanzania. Drug Alcohol Depend. 2021;218:108419.
Friedman J, Syvertsen JL, Bourgois P, Bui A, Beletsky L, Pollini R. Intersectional structural vulnerability to abusive policing among people who inject drugs: a mixed methods assessment in California’s central Valley. Int J Drug Policy. 2021;87:102981.
Sharifi H, Mirzazadeh A, Shokoohi M, Karamouzian M, Khajehkazemi R, Navadeh S, et al. Estimation of HIV incidence and its trend in three key populations in Iran. PLoS ONE. 2018;13(11):e0207681.
Akbari M, Fararouei M, Haghdoost AA, Gouya MM, Kazerooni PA. Survival and associated factors among people living with HIV/AIDS: a 30-year national survey in Iran. J Res Med Sci. 2019;24:5.
Farhoudi B, Ghalekhani N, Afsar Kazerooni P, Namdari Tabar H, Tayeri K, Gouya MM, et al. Cascade of care in people living with HIV in Iran in 2019; how far to reach UNAIDS/WHO targets. AIDS Care. 2021;28:1–7.
Nakhaeizadeh M, Abdolahinia Z, Sharifi H, Mirzazadeh A, Haghdoost AA, Shokoohi M, et al. Opioid agonist therapy uptake among people who inject drugs: the findings of two consecutive bio-behavioral surveillance surveys in Iran. Harm Reduct J. 2020;17(1):1–8.
Makarenko I, Ompad D, Sazonova Y, Saliuk T, DeHovitz J, Gensburg L. Trends in injection risk behaviors among people who inject drugs and the impact of harm reduction programs in Ukraine, 2007–2013. J Urban Health. 2017;94(1):104–14.
Mitsch AJ, Hall HI, Babu AS. Trends in HIV infection among persons who inject drugs: United States and Puerto Rico, 2008–2013. Am J Public Health. 2016;106(12):2194–201.
Iran Drug Control Headquarters. Iran Drug Control Headquarter Year Book of 1394: Tehran: Drug Control Headquarter Publications; 2015.
Rahimi Movaghar A, Malayerikhah Langroodi Z, Delbarpour Ahmadi S, Amin EM. A qualitative study of specific needs of women for treatment of addiction. Iran J Psychiatry Clin Psychol. 2011;17(2):116–25.
Karamouzian M, Mirzazadeh A, Rawat A, Shokoohi M, Haghdoost AA, Sedaghat A, et al. Injection drug use among female sex workers in Iran: findings from a nationwide bio-behavioural survey. Int J Drug Policy. 2017;44:86–91.
Alam-Mehrjerdi Z, Daneshmand R, Samiei M, Samadi R, Abdollahi M, Dolan K. Women-only drug treatment services and needs in Iran: the first review of current literature. DARU J Pharm Sci. 2016;24(1):1–9.
Tavakoli F, Khezri M, Tam M, Bazrafshan A, Sharifi H, Shokoohi M. Injection and non-injection drug use among female sex workers in Iran: a systematic review and meta-analysis. Drug Alcohol Depend. 2021;221:108655.
Kennedy MC, Karamouzian M, Kerr T. Public health and public order outcomes associated with supervised drug consumption facilities: a systematic review. Curr HIV/AIDS Rep. 2017;14(5):161–83.
Kakchapati S, Maharjan M, Rawal BB, Dixit SM. Social determinants and risk behaviors associated with prevalent Hepatitis C and HIV/HCV co-infection among male injection drug users in Nepal. Arch Public Health. 2017;75(1):1–10.
Kermode M, Nuken A, Medhi GK, Akoijam BS, Sharma HU, Mahanta J. High burden of hepatitis C & HIV co-infection among people who inject drugs in Manipur, Northeast India. Indian J Med Res. 2016;143(3):348.
Stone J, Fraser H, Lim AG, Walker JG, Ward Z, MacGregor L, et al. Incarceration history and risk of HIV and hepatitis C virus acquisition among people who inject drugs: a systematic review and meta-analysis. Lancet Infect Dis. 2018;18(12):1397–409.
Arum C, Fraser H, Artenie AA, Bivegete S, Trickey A, Alary M, et al. Homelessness, unstable housing, and risk of HIV and hepatitis C virus acquisition among people who inject drugs: a systematic review and meta-analysis. Lancet Public Health. 2021;6(5):e309–23.
Topp L, Iversen J, Baldry E, Maher L. Housing instability among people who inject drugs: results from the Australian needle and syringe program survey. J Urban Health. 2013;90(4):699–716.
Linton SL, Celentano DD, Kirk GD, Mehta SH. The longitudinal association between homelessness, injection drug use, and injection-related risk behavior among persons with a history of injection drug use in Baltimore, MD. Drug Alcohol Depend. 2013;132(3):457–65.
Havens JR, Latkin CA, Pu M, Cornelius LJ, Bishai D, Huettner S, et al. Predictors of opiate agonist treatment retention among injection drug users referred from a needle exchange program. J Subst Abuse Treat. 2009;36(3):306–12.
Bretherton J, Pleace N. Housing first in England: an evaluation of nine services. 2015.
Woodhall-Melnik JR, Dunn JR. A systematic review of outcomes associated with participation in Housing First programs. Hous Stud. 2016;31(3):287–304.
Acknowledgements
We are thankful to the study participants for their time and participation in the surveys, and all the research staff and stakeholders at national and provincial levels for their assistance to the survey’s preparation and implementation. MK is supported by a Banting Postdoctoral Fellowship.
Funding
The project was supported by the Center for Communicable Disease Control and Prevention of Iran’s MoHME, and National Institute for Medical Research Development (NIMAD 973382). The authors received no funding for this specific paper.
Author information
Authors and Affiliations
Contributions
HSH, MKH, MSH, AM, MK, and AAH conceptualized the study and developed the study conception and design. Material preparation and data collection were performed by HSH, AAH, PAK, NG, FT, GM, SM, and MKH. HSH and MK supervised the study implementation and data collection. MKH performed the data analysis and drafted the manuscript. All authors reviewed and revised the initial draft and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
PAK was the head of HIV/STI office at Iran's MoHME during the last round of the bio-behavioural surveillance survey. Other authors confirm they have no potential conflicts of interest to declare.
Ethical Approval
Ethical issues included the guarantee of the participants’ confidentiality using anonymous questionnaires tools and obtaining verbal informed consent for both biological and behavioral data collection procedures. Participants’ refusal to take part in the study did not affect their access to healthcare services in any manner. The survey protocols were reviewed and approved by the Kerman University of Medical Sciences ethics committee (Ethics Codes: IR.KMU.REC.597, IR.KMU.REC.93.205, and IR.KMU.REC.1397.573; IR.NIMAD.REC.1398.029).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Khezri, M., Shokoohi, M., Mirzazadeh, A. et al. HIV Prevalence and Related Behaviors Among People Who Inject Drugs in Iran from 2010 to 2020. AIDS Behav 26, 2831–2843 (2022). https://doi.org/10.1007/s10461-022-03627-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-022-03627-3