Abstract
Few studies have sought to understand factors influencing uptake and continuation of pre-exposure prophylaxis (PrEP) among young adults in sub-Saharan Africa in the context of population-based delivery of open-label PrEP. To address this gap, this qualitative study was implemented within the SEARCH study (NCT#01864603) in Kenya and Uganda, which achieved near-universal HIV testing, and offered PrEP in 16 intervention communities beginning in 2016–2017. Focus group discussions (8 groups, n = 88 participants) and in-depth interviews (n = 23) with young adults who initiated or declined PrEP were conducted in five communities, to explore PrEP-related beliefs and attitudes, HIV risk perceptions, motivations for uptake and continuation, and experiences. Grounded theoretical methods were used to analyze data. Young people felt personally vulnerable to HIV, but perceived the severity of HIV to be low, due to the success of antiretroviral therapy (ART): daily pill-taking was more threatening than the disease itself. Motivations for PrEP were highly gendered: young men viewed PrEP as a vehicle for safely pursuing multiple partners, while young women saw PrEP as a means to control risks in the context of engagement in transactional sex and limited agency to negotiate condom use and partner testing. Rumors, HIV/ART-related stigma, and desire for “proof” of efficacy militated against uptake, and many women required partners’ permission to take PrEP. Uptake was motivated by high perceived HIV risk, and beliefs that PrEP use supported life goals. PrEP was often discontinued due to dissolution of partnerships/changing risk, unsupportive partners/peers, or early side effects/pill burden. Despite high perceived risks and interest, PrEP was received with moral ambivalence because of its associations with HIV/ART and stigmatized behaviors. Delivery models that promote youth access, frame messaging on wellness and goals, and foster partner and peer support, may facilitate uptake among young people.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Sub-Saharan Africa has a burgeoning population of young people [1,2,3] who bear a disproportionate burden of new HIV infections globally [4]. Oral pre-exposure prophylaxis (PrEP) with tenofovir disoproxil fumarate/emtricitabine (TDF/FTC) is highly effective [5, 6] and is recommended in global guidelines for preventing HIV acquisition [7, 8]. PrEP programs are now rapidly expanding in eastern and southern Africa [9], with a particular emphasis on groups among the most vulnerable to HIV acquisition in the region, including adolescent girls and young women [10, 11], female sex workers [12,13,14], and serodifferent couples [15, 16].
Several early implementation and demonstration studies have revealed suboptimal PrEP uptake [17, 18] and continuation [19,20,21] among young adults, with most data reported from studies among young women. Barriers to PrEP uptake and continuation among young persons in clinical trials and implementation studies have included forms of HIV- and antiretroviral therapy (ART)-related stigma, lack of partner support, rumors about PrEP effectiveness, perceived or experienced side effects, pill size or other attributes, and fear of the burden of daily pill-taking [22,23,24,25,26]. Adolescents and young adults, moreover, are less inclined than older persons to pursue preventive health services and more inclined toward risk-taking, given their still-developing executive functioning and decision-making processes [27]. Thus, to meet their needs, PrEP programs must consider individual, interpersonal, structural, and developmental barriers to uptake among youth.
Despite a substantial number of PrEP studies enrolling young women, few open-label studies have offered PrEP to young heterosexual men [28], a group increasingly recognized as pivotal to prevention efforts, both for their own health and to prevent ongoing HIV transmission [29]. Barriers to PrEP use among young men are likely to differ from those for young women and, to our knowledge, have not yet been reported.
Data are still limited to inform an understanding of the perceptions of PrEP among young adults in the context of a community-wide, population-based approach with a universal offer of PrEP (rather than PrEP targeted to specific sub-populations). Moreover, further research is needed to understand demand for PrEP among young heterosexual men. The Sustainable East Africa Research in Community Health (SEARCH) study, an HIV test-and-treat trial of over 320,000 persons in rural Kenya and Uganda, achieved near-universal HIV testing and met the UNAIDS 90–90-90 targets [30]. In 2016–2017, SEARCH began implementing a population-level PrEP intervention [31] prior to the national PrEP rollout in Kenya and Uganda. Within SEARCH, we conducted a qualitative study to deepen understanding of PrEP demand and early uptake among young women and men.
Methods
PrEP Eligibility and Implementation
PrEP implementation in SEARCH (NCT#01864603) began in June 2016 through June 2017 with 2–4-week community sensitization efforts, followed by HIV testing via community health campaigns (CHCs) and home-based testing for non-attendees [32]. During CHCs, community members received group education on PrEP upon arrival to the health campaign. Enhanced HIV post-test counseling on PrEP was provided to HIV-uninfected individuals (≥ 15 years) at elevated risk of HIV acquisition, based on self-identified risk, serodifferent partnership, or a region-specific risk score [33]. All individuals ≥ 15 years who met eligibility criteria (negative HIV-antibody testing performed by SEARCH within past four weeks, no known Hepatitis B infection, and no symptoms of acute HIV) could elect to initiate PrEP; no specific demographic risk groups were targeted apart from serodifferent couples. PrEP initiators were offered same-day or rapid PrEP start. PrEP initiation occurred on-site at CHCs or at nearby health facilities. Transportation was provided to clinics for the PrEP initiation visit but no other incentives for participation were given. After providing written informed consent, participants were given daily oral PrEP (tenofovir disoproxil fumarate 300 mg with emtricitabine 200 mg or lamivudine 150 mg) free of charge. Follow-up visits were scheduled at weeks 4, 12, 24, and every 12 weeks thereafter for up to 144 weeks. Visits occurred at local health facilities, participants’ homes, or other community-based locations of the participant’s choice (such as a trading center or beach).
Study Design
A qualitative study embedded within the SEARCH trial was conducted to explore understandings of PrEP, and to elucidate factors influential of demand, decisions around PrEP uptake or non-initiation, and adherence and discontinuation in population subgroups at elevated HIV risk, in the context of population-based PrEP implementation. Focus group discussions (FGDs) and in-depth interviews (IDIs) with selected populations of interest (youth, members of serodifferent couples, health care providers, and PrEP-eligible adults who accepted or declined offers of PrEP) were conducted in five of 16 communities where PrEP was introduced: a Lake Victoria island community and an inland community at the lakeshore in Kenya, two communities in eastern Uganda, and one in southwestern Uganda. This article focuses on results obtained from baseline data collected from adolescents and young adults, including FGDs with youth (15–24 years), and IDIs with young adults (up to age 35) who were PrEP-eligible. Data were collected from September 2016-September 2017, with focus groups conducted within 3 to 4 weeks and interviews within 10 months after CHCs to allow time for participants to initiate and experience PrEP usage.
Sampling
Eight FGDs (4 male, 4 female groups) were conducted, each with 8–12 participants between the ages of 15 and 24 years, purposively selected and recruited during CHCs conducted in the five SEARCH intervention arm communities in the early months of PrEP implementation. Team members approached CHC attendees who appeared to be young; those who confirmed verbally that they were under age 24 were introduced to the study and invited to attend the FGD. Informed consent procedures were administered prior to the start of each FGD. Team members sought to recruit at each CHC a sample that was composed for balance by age grouping to comprise adequate numbers of teens and young adults. The sample for FGDs included 56 female and 32 male successfully-recruited participants (total n = 88), who were not asked their HIV status, nor about their experience with PrEP, during ascertainment of eligibility and recruitment.
The data collected via in-depth interviews for this analysis were derived from interviews with n = 23 HIV-uninfected individuals who were less than 35 years old, within a larger gender-balanced cohort composed of n = 32 individuals who initiated PrEP (n = 16) and who declined PrEP (n = 16). This cohort was systematically sampled and recruited from a randomly-generated list of PrEP-eligible individuals in each of the five communities, balanced to include those who self-identified as at risk for HIV and those identified by the region-specific risk score. From this larger IDI cohort of adults who were offered PrEP and either initiated or declined it, there were 23 IDIs conducted with young adults. Among these, there were 13 PrEP initiators and 10 PrEP decliners, and 9 women and 14 men, with a median age of 24 years (range 17–35); 12 (52%) were unmarried.
Data Collection
A team of six researchers, who were native speakers of local languages in the study regions (Lusoga, Lugwere, Ateso, Runyankole, and Dholuo) and were trained in qualitative research methods, collected data in participants’ preferred local language, then translated and transcribed audio recordings into English. In-depth semi-structured FGD and IDI guides were translated from English to the local languages, then back-translated to ensure content validity. Interviewers were matched to participants by gender. Semi-structured FGD and IDI guides explored domains of inquiry that we hypothesized to potentially influence PrEP uptake and continuation, drawing upon salient theories and frameworks for understanding health behavior change (e.g. Social Cognitive Theory, the Theory of Planned Behavior [34] and the AIDS Risk Reduction Model [35]), for understanding how social norms change (e.g. Persuasion and Social Influence [36] and Diffusion of Innovations [37]), and for understanding the influence of HIV-related stigma [38] and gender [39] on sexual and social behaviors. These domains of inquiry, structured socio-ecologically, included individual-level beliefs, attitudes, and understandings of PrEP; perceptions of HIV risk; social norms related to gender, sexuality, PrEP, and HIV (especially among peers), including forms of HIV-related stigma, and other potential barriers to and facilitators of PrEP uptake including structural factors in communities and the health system (examples of questions from the guides are shown in Supplementary Table 1). The semi-structured guides for IDIs and FGDs were designed to elicit discussion in these domains but also permit participants to discuss other, unanticipated topics that were salient to the overall purposes of the research.
FGDs were conducted during the first year of PrEP implementation at local community venues and lasted about two hours. Participants were given numbered nametags to enhance confidentiality, and referred to one another by number in the discussions excerpted here (i.e., “P1”, “P2”). IDIs were conducted at participants’ home or another preferred location, at a median of five months (range 4–10) after HIV testing and offer of PrEP during community-wide HIV testing, and lasted 40–90 min. Written informed consent was obtained for all data collection. FGD and IDI participants received transport reimbursements but no other incentives for participation.
Data Analysis
The research team engaged in analysis included the six Kenyan/Ugandan researchers and a U.S.-based team of study manager, clinician-scientist engaged in SEARCH PrEP implementation, and the lead investigator. Audio recordings of FGDs and IDIs were transcribed, translated into English, and deductively and inductively coded by the research team, drawing upon constructivist grounded theoretical approaches [40]. An initial coding framework was developed based on the theory-informed domains of inquiry for FGD and IDI guides. The framework was iteratively refined by the research team during data collection, following review and discussion of emergent findings, including examination of deviant cases, contradictions and inconsistencies.
Ethical Approvals
The study was approved by the institutional review boards of Makerere University, the Uganda National Council of Science and Technology, the Kenya Medical Research Institute, and the University of California, San Francisco.
Results
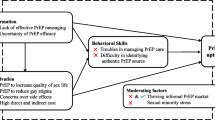
Across diverse models of health behavior change [41, 42], including those specifically concerned with HIV [35, 43], elements thought to be fundamental to the adoption of a new (and especially difficult) behavior or technology include perceived severity of the illness (HIV), as well as perceived personal susceptibility or risk of acquiring it. Appraisals of the difficulty of taking on a new behavior, and of its benefits and potential consequences, normative influences within one’s spheres of intimate partnerships and peer groups, and structural factors all contribute to decision-making related to health behaviors including PrEP use. Evidence for these domains of potential influence on PrEP uptake was ample in the narratives discussed below (with additional evidence presented in Supplementary Tables 2–4).
Perceived Severity of HIV, in Context of ART Rollout
At the time of PrEP rollout in SEARCH communities, nearly all community members (> 90%) had knowledge of their HIV status after population-based testing [32]. Widespread use of ART was perceived to have made people living with HIV healthy and able to work, and to have prolonged their lives. Young people had heard stories about the devastating early days of the epidemic, and some said they were emotionally less affected than their elders were by the trauma of HIV/AIDS. As a young man in Kenya commented, “I don’t think this generation has seen a real HIV positive victim […] a real thin and sick person. We are belittling HIV because we have not witnessed a real victim.” Thus, the perceived severity of HIV disease was low among many young people, who attributed this to the success of ART. Two young men in a FGD in eastern Uganda commented:
Because ARVs [antiretroviral medications, i.e., ART] are available, some youth now days do not see HIV/AIDS as a serious disease, just because they know there is ARVs. Some youths say, “even if I contract HIV I will go to [the] health center and start taking ARVs.”
Youths in this community are not at all scared of contracting HIV. For girls, they are mostly scared about pregnancy and the boys are only scared of being imprisoned for having impregnated a girl.
Young women also reported that HIV was no longer feared, and that pregnancy and other health concerns predominated, as one young woman in a Kenya island FGD noted: “The greatest risk that affects the current young woman is about the pregnancy. They say taking HIV drugs is like drinking water, because it is an easy task to do. What most of the people fear most nowadays is the cancer other than HIV.” Yet, while many young people felt that their peers perceived HIV disease to be not as serious as pregnancy or cancer, and made light of treatment, when discussing themselves and their own motivations, fewer expressed that taking daily ART medications would be easy. On the contrary, many said that their biggest fear related to HIV infection was that it would result in the burden of a life-long daily treatment regimen, as illustrated in this comment of a Kenyan man who had recently started PrEP (age 31):
There is no one who is afraid of HIV along this lakeshore. They say that it is like malaria and that it is not a disease. They only fear cancer.
[Interviewer: How about for you personally?]
I fear it… They say that once you get infected and start on ART you cannot stop for the rest of your life… The fact is that once I start taking ART medication I have to do so each and every day for the rest of my life, and if I stop, I will face problems. Once you start, you become a slave of these drugs.
Gendered Perceptions of HIV Risk
Young men and women in this setting expressed feeling at high personal risk of HIV infection, and were curious about and interested in PrEP. The narratives surrounding HIV risks and interest in PrEP were highly gendered; thus, these findings among young men and women are discussed in turn. First, young men expressed feeling vulnerable to acquiring HIV because of both their own sex drive and also pressure from women to exchange money for sex. As the following excerpt of a discussion among young men in Kenya shows, they were keenly aware of how sexual networks fuel HIV transmission, and rueful about their vulnerability as the age-mates of sexual partners likely to be infected by older men, their wealthier competitors for sex:
P2: Men, we tend to love the female young ladies for sex. They also have other older men whose financial status is somehow stable. I end up sleeping with her not taking into account that she may have some other men elsewhere […] I have a school-going girlfriend who at the same time befriends some boda boda [motorcycle taxi] guy who transports her to school for free. We end up being in the chain of many men, versus one girl, which increases our HIV risk.
P4: What P2 has said is very true […] The other scenario is that I have cash to win a lady and P1 has more cash to win the same lady, and at the end of the day it will be cash talking, hence HIV infection.
P3: […] As men we stand at risk because we share the same ladies, who love money. Men on the other hand are over-practicing their social life, where they want to hook every girl within their vicinity.
P6: […] One of the things that subjects us to HIV infection is that the adults have turned to the young girls who are our age-mates—they see them as their most appealing sexual partners.
The enthusiasm for PrEP expressed by young men was compatible with their participation in a normative form of masculinity that valorized sexual conquest. PrEP was seen as a vehicle for reducing risk while pursuing opportunities for sex without condoms, which were widely disliked. This sentiment expressed by a young man in eastern Uganda was typical: “Most of us youths have a tendency of forgetting to use a condom when we are going to have sex. But if I have swallowed these drugs, even when I forget to put on a condom I will already be protected from contracting HIV.”
Yet, discussions among young men about their own sexual risk-taking also revealed an emotional vulnerability underlying the bravado. Young men admitted to having multiple partners as a form of emotional ‘insurance’, because they did not expect their female partners to be faithful, as illustrated in this comment of a young Kenyan man: “As young men, faithfulness is hard to practice simply because we may have one girl whom we feel to love so much, only to realize at the end that she has another man elsewhere. This also makes us to look for others to be safe.”
Among young women, discussions mirrored the observations of young men about sexual behavior and vulnerabilities to HIV infection among youth in the communities. Young women felt particularly vulnerable to HIV because of their partners’ high risk sexual behavior (frequent partner change and multiple and concurrent partnerships with other women), as well as polygamy being common in the study communities. As one young woman commented in a discussion among young women in a Kenyan island community, to much laughter, “I don’t understand how men were created. They are like Bluetooth, in the sense that they only connect to those within their radius.[… laughter…] You may leave just for a short journey; you will get phone calls that your guy brought P2 to the house.”
In the same discussion in Kenya, young women, like young men, reported that due to poverty and the inability of parents or partners to provide for many of their basic needs, many turned to transactional sex with older men for subsistence. They also both laughed about and discussed in a critical way their reliance on transactional sex for consumption, and to maintain a certain standard of living.
P1: Ladies have varied demands like sanitary pads […] and some parents are not able to support, the best they can tell you is, “my daughter I have no money— you can even use a piece of blanket as a sanitary pad.” […] a young lady will automatically look for other ways of getting that sanitary pad […] will give in to anybody called a man who approaches her, with a mentality that the man will provide what she is missing, and at the end of the day, infection will follow.
P4: The truth is that we don’t have faithful ladies. You get a guy who cannot even meet your saloon expenses, you think of a nice shoes… he does not have anything to support. I will then have to have him just as a toy and move with those who can provide for me. As ladies we believe in money– and by the way we cannot survive without money– the moment I get one who can meet my needs, I will have to be faithful to him. But for one who always complains to be having no money, what do I do with a poor man and what reason do I have to be faithful to him? Who is he to me after all? [long laughter].
In the context of sex with casual partners, condom use was rare, and rarer still with regular partners. While young women discussed their agency in some domains—to choose partners, and negotiate transactional sex exchanges— they also recounted difficulty controlling their partners’ condom use, even after having negotiated it. As a young Ugandan woman said, “What I see, you can find a man, he entices you, you tell him to put on a condom, and then you find that he has later removed it.”
Moreover, young women reported difficulty discussing HIV risk or HIV testing with their partners. They feared that requesting HIV testing would lead to conflict. When asked by an interviewer about whether she felt it was possible to discuss HIV risks with her partner, a young woman in Kenya (a PrEP decliner, age 21), said,
No! […] the men will not allow you to start on that topic, because the minute you bring it up the next sentence is, “so you don’t trust me” […] That may make him feel insecure, and you can be dumped just because of that issue. To save the relationship, you don’t talk about HIV. If I get a boyfriend I find it hard telling him about HIV testing because I fear his reaction afterwards. I may only ask about the HIV status, and once he has told me that he is negative, then I am just okay with that.
Given that many young women were uncertain about their partners’ HIV status and were unable to consistently use condoms, PrEP was seen as a potential option for reducing HIV risk. This comment from a young woman in Kenya was typical of those supportive of PrEP: “Since your partner is not an angel and I may not be sure of his other movements, it would be prudent to use PrEP.” Yet during the time these data were collected, PrEP was still unfamiliar to most, as illustrated in the narratives presented in the next section.
Misconceptions, Fears, and a Need for ‘Social Proof’
National PrEP rollout was at very early stages in Kenya and Uganda at the time the SEARCH PrEP intervention started, and there were no prior information campaigns about PrEP in most communities before SEARCH sensitization activities. Over the first several months of SEARCH PrEP implementation, many community members were unfamiliar with PrEP and rumors and misconceptions were common. Because open-label PrEP was offered as a study drug and a consent form was required, some questioned whether PrEP had previously been tested, or if it was safe and effective. Young people expressed having fears of the known potential side effects of PrEP (such as renal toxicity), as well as rumored effects such as reduced libido, infertility, or fatigue/weakening of the body. Many participants felt that they needed more information about the proven effectiveness of PrEP before they would take it, as illustrated in the following excerpts:
If it is said that it is still being researched on, then some people may shy from taking it. It needs to be communicated that the drug has been approved and it is working. About side effects, they need to be told that each drug has side effects; even Panadol has side effects.
- Kenya-Inland, male, 22, PrEP decliner
What we worry about PrEP is that is it probably a test drug. You see for every drug to be introduced, it has to be tested first. So they might be testing the drug on Ugandans and it is likely that you people might not even know about the side effects of the drugs. You see [he] is taking those drugs, if he does not get infected with HIV in these three months; that that is when I will be sure that the drugs really work.
- Uganda-Southwest, male adolescent FGD
Some youth wanted social proof that PrEP ‘works’ (per Cialdini’s conceptions of persuasion in marketing, we rely on others’ signaling of correct behavior, in ambiguous situations [44]), and this meant not only receiving counseling from providers on PrEP, but the testimony of peers supporting the efficacy of PrEP. The opportunity for vicarious efficacy [42] of successful PrEP use among socially-similar peers (per Bandura’s social learning theory) could help persuade young people that they too, could take PrEP and benefit from it. However, given the novelty of PrEP, many did not yet know others who were taking PrEP. A young woman in Kenya said, “I would love to use it to protect me from HIV, but my worry is that I have never seen anybody who has benefited from PrEP.”
HIV-Related Stigma
Stigma related to HIV and ART also militated against PrEP uptake. Because the blue PrEP pills were recognized by many to be part of HIV treatment regimens, some feared that taking PrEP would lead others to assume that they had HIV. Men, in particular, also feared being seen accessing PrEP at the same health centers where HIV care was provided. Some participants requested separate clinic days or entrances to avoid the risk of appearing to be HIV-positive:
For me what I want you to help us about, majority of us fear to go to the health center. If it is possible you can always designate a day and come and distribute [PrEP] to the people. Yes, some of us may go to the health center. However, majority of the people here do not want to go to the health center.
- Uganda-East, male, 31, PrEP initiator
Some individuals who declined PrEP chose to abstain from sex or undergo frequent HIV testing with their partners. Particularly among participants who believed in abstinence, there were some concerns that PrEP could increase ‘promiscuity’ in the community:
As a born-again Christian I thought that [PrEP] was one way that was going to make promiscuity be on the rise because when people learn that it prevents HIV up to 99% they will not be afraid to have sex with anyone.
- Kenya-Island, male, 26, PrEP decliner
P5: It is not good to talk about PrEP [Laughter].
[Facilitator: That is her view! We need to respect everyone’s view.]
P7: I also think that PrEP should not be promoted, because it will encourage young girls to have reckless sex.
- Uganda-Southwest, female adolescent FGD
Moral prohibitions against sex among young people led to some youth feeling they could not ask providers for PrEP, as reflected in this comment, from a young man in southwestern Uganda, to the FGD facilitator: “There are certain things I may be scared to talk to you about but then comfortable talking to a fellow youth about it. I will not be comfortable telling you I have a girlfriend and so I want to take PrEP to protect myself, because I know you may consider this as bad given my age. I will fear to talk to you about it, and as a result I will opt to go and have sex with this girl without using PrEP.”
Some thought that providers were offering PrEP as a clandestine way to treat HIV without telling individuals that they were infected. This led many to avoid taking up PrEP, but not all: as a man in eastern Uganda (a PrEP initiator, age 31) reported, “I was like, ‘are these people trying to hide the truth from me, but I have the virus, and so they are trying to trick me around so they may start me on ARVs unknowingly?’ I actually told the man who gave me the results, ‘please, don’t fear to tell me the truth. If I have the virus, you tell me the truth.”.
Interference with Conceptions of Healthiness and Sexual Freedom
For many young people, the prospect of taking daily medications while otherwise healthy was daunting. Medications were perceived to be what older people, and sick people take, thus fundamentally challenged a self-conception and identity of youth and healthiness. As a young woman in Kenya commented, “How do you start taking drugs and yet you are not sick?” Moreover, the need to take PrEP daily and the study’s recommendation to take PrEP for several weeks prior to achieving fully protective drug levels were met with concern by youth. Many thought that this would require them to plan ahead for sex, or wait to have sex (both of which were felt to be unrealistic expectations):
PrEP is good, but the frequency of taking it is a concern. I live here in the island and my boyfriend is just a doorstep away. I cannot schedule to have sex with him in the next 28 days waiting to complete the PrEP dose. Once a lady has tasted sex, she would want to have it frequently without restrictions [… laughter…].
- Kenya-Island, female FGD
Compounding these concerns, confusion about PrEP dosing were common early in the implementation of PrEP, as providers struggled with messaging and communications surrounding the concepts of ‘seasonality’ and ‘risk window’. Young people in communities absorbed messages that led them to conclude that PrEP use required stringent control over the scheduling of sex, which was daunting. As a young Kenyan woman commented, “Youth say that they cannot use PrEP, because there is no way you can organize for a date in the next 28 days while on drugs, and another 28 days after the act. They therefore claim that PrEP deserves the married people and not them.”
Structural Barriers to PrEP Uptake
Young people who lived with their parents or were attending school faced additional barriers to starting PrEP; they desired that more information about PrEP be provided to their parents. As one young Ugandan woman said: “Educate our parents about PrEP! I can accept PrEP, and then my mother stops me from taking it.” In addition, those who were attending school outside the community were unable to initiate or continue PrEP while at school, given that PrEP was only offered within study communities.
They found me at home, and then they told me, ‘if you feel that you can’t protect yourself from HIV, if you can’t abstain, the important thing to do is for you to come and we give you these drugs.’ I told her, ‘if I get time, I will come by so that I get the drugs.’ But at the time, I was going back to school, so I didn’t get the time…. Now that I have a boyfriend and yet I don’t trust him that much, I thought to myself that I have to get those drugs, use them and prevent myself from getting infected with HIV.
- Uganda-Southwest, female, 23, PrEP decliner
Others felt that the distance needed to travel to health centers was prohibitive:
Many people in this community know that HIV/AIDS is real but many of them fear to go and test. Some of them know that they are HIV negative but they fail to go and get PrEP because of the long distance they have to move. We think there is need for health workers to help us in delivering these drugs to people or even to find a place nearby where they can put those drugs to help people access them very easily just like they did with condoms.
- Uganda-East, male, 22, PrEP decliner
Early Experiences of PrEP Initiators
The findings above summarize the major themes emerging from interviews and discussions surrounding both motivations for potential PrEP use and the barriers to starting PrEP among youth. Here, we review findings from interviews with individuals who actually started PrEP, in order to understand the factors that differentiated PrEP initiators from others, and the circumstances that led to many early adopters of PrEP to discontinue use.
Participants who initiated PrEP reported a variety of motivations for their decision to take up PrEP use. These included distrust of partners’ sexual behavior and not knowing partners’ HIV status, their own multiple or concurrent sexual partnerships, their lack of agency to control or negotiate condom use, and the HIV-related illness or death of a former partner or family member. In most cases, a precondition to this decision was belief in the effectiveness of PrEP. Most PrEP inititators believed strongly in the efficacy of PrEP, and reported feeling relieved and well-protected from HIV while they were taking PrEP, as illustrated in the following excerpts:
I feel really comfortable knowing that chances of HIV risk are minimal […] Nothing [will make me stop taking PrEP] unless there is something new on it but the way it is currently nothing can make me stop taking it […] I think PrEP is good and I will encourage people to use it because I have experienced it.
- Kenya-Inland, male, 24, PrEP initiator
I thought of it as something that will protect my life. I first got a shock— ‘Really? There is a drug that prevents HIV?’ […] I was very happy about it because my husband can’t stick to one woman, yet I don’t want to get infected. I felt so happy, because I knew that now that it has come, it will help many people. You see, for most women, HIV is brought to us by our husbands.
- Uganda-Southwest, female, 17, PrEP initiator
However, even after starting PrEP, some participants remained uncertain of the effectiveness of PrEP, and used repeat HIV testing to confirm that PrEP worked. A young woman in southwest Uganda (age 17) told us, “You see, people were saying that, ‘we are going to take these drugs, but what if they cause the HIV in themselves?’ So, when the drugs got finished, my heart said to me, ‘go and see if you have caused the virus to yourself’. I didn’t know if it was directing me well or misleading me. So when I tested, I found out that I am not infected.”
In addition to protecting against their own sexual risks or fears of partners’ behaviors, some said that choosing to start PrEP meant they were taking a step to achieving their life goals, such as completing schooling or having a family. This comment of a young man in southwest Uganda (age 21) typified this sentiment: “The risk I have is that if get infected with HIV, I will fail to fulfill my dreams. Because you may have a desire to do something, like to care for yourself or your family […] I want to complete my studies when I am ok. Secondly, I want to have a family—that is admired by people. When I see my baby and his or her mother safe, I feel so happy because nothing will worry me.”
Many participants reported that discussions with their partners either facilitated or hindered their use of PrEP. Whereas men were able to initiate PrEP without discussing it first with their partners, some women said they needed to seek permission from their partners to take PrEP. Among participants with partners who were HIV-negative, some reported their partners were supportive of PrEP use, while others said partners were suspicious of why PrEP would be needed if both partners were negative, and believed its use would lead to infidelity. As one young woman in Kenya said: “You will not tell him that you are using PrEP because he will not agree to it: ‘why are you taking PrEP and yet I am the one you consider your boyfriend?’” The tension of needing PrEP due to mistrust of one’s partner (or due to having other partners) was difficult for some participants to navigate:
I asked my wife, ‘where is that bottle?’ She said, ‘what is it for?’ […] ‘what are you sick of?’ I explained to her the way I was explained to. I told her, ‘this is not a drug for HIV positive people; it is a drug to protect me from HIV.’ She said, ‘Do you still hope that you can sleep around?’ I told her … ‘But if I used PrEP, given the way they have taught me, even if I was to be taken up I can be sure to be safe.’ She told me, ‘I have thrown them away and you will never see them again.’
- Uganda-Southwest, male, 25, PrEP initiator
Other partners were more supportive of PrEP use and in some cases both partners elected to take PrEP together to protect each other. In addition, social support from other family members or peers facilitated PrEP initiation, particularly when participants were not able to disclose PrEP use to their partners:
Before going to the clinic I talked to another sister of mine telling her that “I am going to take PrEP… if it can prevent HIV I am going to take it.” […] she said “in fact PrEP is not available in [my village]. Had it been available in [my village] I would have enrolled too”. She was very supportive of me.
- Kenya-Inland, female 24, PrEP initiator
Factors Leading to Continuation or Discontinuation
Many PrEP initiators stopped or took a break from PrEP use for a variety of reasons. Some reported early side effects of PrEP use, such as headaches, nausea, and fatigue, and a few participants stopped PrEP due to an inability to manage these side effects; for example, a 24 year old southwest Ugandan woman told us, “I started using PrEP but stopped after two months. I stopped because I was experiencing headaches. Interviewer: Did you talk with anyone about this decision? I told my husband about it.” Participants who were in contact with health care providers and received counseling and early management of side effects, and who learned strategies to minimize them, were more able to continue taking PrEP:
When I started taking PrEP I did not feel so well. I felt dizzy and I had diarrhea for about one week […] I also experienced fatigue […] There is one provider who paid me a visit here at home. I explained to him and he told me that the side effects were expected […] They told us that in case we had any questions we were free to call or visit the clinic at any time.
- Kenya-Island, male, 24, PrEP initiator
Several participants reported that their relationships had ended and that, without a current partner, they were not at risk of acquiring HIV. Given that participants were interviewed less than one year after starting PrEP (at a median of 5 months after PrEP initiation), and that all reported HIV risk at PrEP initiation, there was a relatively rapid formation and dissolution of partnerships among study participants, and thus an evolving HIV risk context.
I used to have [a partner] but when I told him that we go to the clinic for HIV testing, he refused, so I abandoned him.[…] You see they told us that after some time, you can discontinue taking [PrEP], so I looked at my condition, am not at risk of getting infected with HIV […] maybe I will find another man and I will start the drugs again.
- Uganda-Southwest, female, 26, PrEP initiator
Other participants stopped PrEP due to unsupportive partners or needing to hide PrEP use from partners. For example, a 25-year old southwest Ugandan man described his wife who, feeling that he was using PrEP in order to be promiscuous, told him, ‘I have thrown them [PrEP pills] away and you will never see them again.” Others who had stopped using PrEP discussed being stigmatized by friends: a man in eastern Uganda (age 31), said, “They [friends] thought that I am HIV positive because they knew these drugs were being given to HIV positive people. Secondly, they said, ‘since you have started using PrEP you are now going to go immoral and start sleeping around.” Still others stopped PrEP because of no longer feeling at risk of HIV because of learning their partners’ HIV status after testing, or because of other life events, such as travel outside the community: “At that time, I was ready to enroll in PrEP, but because of time I couldn’t be enrolled. I arrived very late when they were leaving,” said a 35-year old southwest Ugandan man not on PrEP. A 24 year old woman also in southwest Uganda who had discontinued PrEP said, “After completing one bottle, I traveled to take care of my sick sister. I did not carry the drugs with me, and after missing taking PrEP for some time, I asked myself, ‘Can I continue from where I left?’, but I just stopped.” Some men decided to alternate between condom use and PrEP as HIV prevention options and planned to use PrEP during different periods of risk over time.
Finally, given the novelty of PrEP, some PrEP initiators suggested that more time is needed for PrEP to be accepted in communities and that ongoing education and messaging were needed to foster acceptance. As a Kenyan man commented (age 31, PrEP initiator), “Before PrEP came, we were told that male circumcision also helped reduce the chances of HIV infection. It took a long time for me to change and accept to be circumcised. People do not change easily but with time they do. Just keep talking about PrEP and people will eventually accept it.”
Discussion
This study among young women and men in rural communities in Kenya and Uganda is one of the first to describe factors affecting decision-making surrounding PrEP uptake among young adults in the context of a population-based approach and universal offer of PrEP in community-based settings. It is also among the first to shed light on the experiences with the use of open-label PrEP in sub-Saharan Africa [28] among young men, and young married persons with HIV-negative or status-unknown partners. This is in contrast to most other studies in the literature to date, which have been conducted among those enrolled with intention to start PrEP [45] and in highly targeted populations such as people in serodifferent partnerships [16, 45,46,47], female sex workers [12,13,14], and MSM [24]. Thus, our findings provide insights into demand for PrEP and potential early barriers to PrEP uptake and continuation as rolled out in national programs.
In this high HIV prevalence setting in rural eastern Africa, where high levels of HIV testing and ART coverage were recently achieved, young men and women reported feeling personally vulnerable to HIV acquisition, even as HIV disease itself is less feared than it once was. Many adolescents and young adults in this setting were conversant with epidemiological concepts of sexual networks, if not the scientific vocabulary for such concepts; they engaged in critical discussions about the reasons for the continued transmission of HIV in their communities and their own contributions to it, pointing often to poverty and gender inequities. Many were enthusiastic about the possibilities of PrEP for reducing risks, in the context of their concurrent, frequently changing, and transactional partnerships.
Yet, despite high levels of curiosity and interest due to perceptions of high personal HIV risk among youth, there were numerous barriers to PrEP uptake in the population. More threatening than HIV disease itself was the prospect of engaging in the health care system and with regimens of daily medications: the fear of having to take ART every day was a powerful motivator to staying uninfected. But to start PrEP, for many, also posed a threat to self-concepts of healthiness, and also required a future orientation and discipline that was especially challenging in the cognitive developmental stages of adolescence and young adulthood in the study population.
In addition, this study was conducted early in the national rollout of PrEP in Kenya and Uganda, and numerous barriers to PrEP uptake related to its novelty. Despite intensive efforts to provide community sensitization, group-based education on PrEP during community-wide HIV testing, and individualized counseling for those at elevated risk, PrEP was perceived as an ‘unproven’ biomedical technology. Knowledge of PrEP was not yet widespread, nor were there many opportunities for social learning [42] (i.e. vicarious efficacy for PrEP initiation, and opportunities for rumors to be dispelled) because so few young people in communities were successfully taking PrEP at the time these data were collected. Thus, the findings represent an early stage of the ‘diffusion of innovation’ [37] of PrEP, in which these factors, along with forms of HIV (and ART)-related stigma that manifested in particular in partners’ non-acceptance of PrEP, worked to limit PrEP uptake.
The rumors and misunderstandings that initially circulated in communities related to PrEP and its proper usage, and to the motives of researchers, reduced over time as the SEARCH study refined and reinforced its messaging and mobilization efforts and introduced PrEP ‘ambassadors’. Yet, these rumors and disbelief in the effectiveness of PrEP are consistent with prior research on other products in placebo-controlled studies prior to known effectiveness [22, 48, 49]. Limited knowledge of PrEP, disbelief in efficacy, and rumors are now being reported in other PrEP open-label studies prior to widespread rollout, such as among female sex workers in South Africa [26]. Findings of this study suggest that that given the novelty of PrEP as an ARV-based prevention option, more work is needed to enhance education and messaging campaigns as PrEP is newly introduced into communities. Our findings suggest that extended efforts are needed to introduce PrEP at a community level and to support young people as they consider PrEP use, discuss PrEP with their partners, and navigate PrEP use as partnerships change, in order to facilitate the diffusion of this important HIV prevention technology.
The findings presented here confirm prior research suggesting that perceptions of the severity of HIV disease have been changing as access to effective treatment has rapidly expanded. In the context of widespread knowledge that HIV treatment was available to keep people alive and healthy, the perceived risk of HIV acquisition, while high, was not as salient for youth as were other, more pressing, concerns, such as economic constraints, pregnancy, and cancer. Prior work by members of our group and others has revealed reduced concern about HIV risk with expansion of ART use in fishing communities western Kenya [50] and Rakai, Uganda [51].
Our results also extend prior research showing that understandings of the concept of “risk” are varied, and that diverse measures and data collection methods used can lead to discordant findings even within the same study populations. Several studies using quantitative survey research methods have found low reported HIV risk perception among young women, and a discrepancy between self-reported and objective measures of risk [11, 52, 53]. In SEARCH, our finding that worries about HIV risk among IDI and FGD participants were common contrasts with quantitative survey findings from the parent SEARCH study, in which fewer than half of persons eligible for PrEP reported that they perceived themselves to be at risk of HIV [31]. It is possible that the qualitative data collection methods used in this study– interviews which were conversational in tone and permitted rapport-building between interviewers and participants, and focus group discussions in which participants could freely discuss fears with others in similar circumstances and shared social identities– provided a more comfortable context for individuals to disclose a potentially stigmatizing perception of HIV risk than was possible in survey research encounters.
Perceptions of HIV risk were highly gendered: young men in our study (who were either single or in marriages with HIV-negative or status-unknown spouses) perceived their risks of HIV to mostly stem from their own behaviors, and therefore under their more direct control; they were enthusiastic about PrEP as a vehicle for safely pursuing sex with multiple partners. Young women, who had little control over partner behaviors and felt pressure to engage in transactional and condomless sex, viewed PrEP as a means to assert control over sexual risks. This confirms prior research findings from placebo-controlled and open-label PrEP studies that have found that young women were predominantly worried about their partners’ behaviors as the source of their HIV risk [23, 54]. Future research should explore whether these gendered, nuanced understandings of HIV risk– and whether or not one attributes ‘culpability’ for that risk to oneself or another– are accounted for in survey measures of HIV risk perceptions, and if not, how such measurement can be improved.
Our findings on HIV risk perception suggest that understanding both individual worries about HIV, other health and life priorities, and broader community perceptions of HIV will be important when offering and discussing PrEP with young adults. There have been recent calls to focus on ‘protection’ or ‘wellness’ framing when offering PrEP [55, 56], and this approach, combined with a focus on the goals and priorities of young adults, may facilitate adoption of HIV prevention approaches. Theories of social and health behavior in any case would suggest that a focus on a report of ‘risk’ elicited for the purposes of identifying individuals for whom PrEP is appropriate, could have limited utility without also considering other factors that influence the adoption of a novel health-related behavior, including, of course, the perceived severity of HIV disease. In contexts where HIV disease itself is becoming less feared, it is even more important that the perceived burden of prevention (e.g. daily PrEP pills) be lighter than the demands of treatment (e.g. a daily ART pill regimen); long-acting formulations of PrEP along with post-exposure prophylaxis (PEP) are urgently needed for youth in these settings.
Yet, in contradiction to findings suggesting that perceived severity of HIV disease is declining, HIV-related stigma and the associations of PrEP with ART nevertheless appeared to inhibit PrEP uptake among some youth in this study, confirming findings of prior research among young women and serodifferent couples. Prior studies have also reported beliefs that PrEP was being offered as a way to covertly give ART to those with HIV [45], and that anticipated stigma related to PrEP use and ART [23, 24, 26, 45, 57] militates against uptake. There are gender dimensions to HIV-related stigma, as men in particular said that their avoidance of health facilities, in part due to HIV-related stigma, was a barrier to PrEP use; men in this study, as in prior studies, often felt that health facilities catered to women or were ‘women’s spaces’ [58, 59]. Moreover, we found that (particularly for men who were working), the distance and time to attend clinic were perceived as prohibitive. Our results indicate that future studies offering PrEP to young men should acknowledge the context of their desire to pursue partnerships and should also explore the use of male-friendly spaces and service delivery strategies to make PrEP more accessible and appealing.
Finally, on a more pragmatic level, others have found, as did we, that the physical characteristics and size of the PrEP pills lead some to avoid PrEP use [19, 24, 57], that perceived or experienced side effects also militate against PrEP use [22, 24, 45, 57], and that counseling on anticipated side effects and assistance with managing side effects are important to foster PrEP continuation [24].
Several factors facilitated the uptake and continuation of PrEP: initiators viewed it as supporting their plans to pursue and achieve life goals (such as completing schooling and having a family) while protecting themselves from HIV. The population of early adopters of PrEP in SEARCH communities tended to be older, male, and in discordant relationships [31], and these qualitative findings help to explain those patterns: PrEP initiators perceived themselves to be at high risk of HIV because of their own or their partners’ behaviors; many had a ‘mature’ life outlook or future orientation; and gender inequities meant that men more than women had the agency to decide to take up PrEP without first having to obtain a partner’s permission. We found that discussions with peers, family members, and occasionally partners facilitated PrEP initiation and adherence among young women, as has been previously documented [23]. We also found that repeated negative HIV tests reinforced ongoing PrEP use for both men and women, as in prior studies among young women and members of serodifferent couples [25, 60].
The importance of partner influence cannot be overstated, particularly for women, but also for men. While numerous studies have explored the influence of male partners on women’s decision-making around HIV prevention products [61, 62] and have reported on the challenge of discussing PrEP use with partners [25], few studies have explored female partners’ influence on men’s PrEP use. Similar to prior studies, we found that women often had to seek permission from partners to take PrEP and that some women hid their use of PrEP [57]. However, navigating discussions with partners around PrEP use was challenging for both men and women. Although many men felt empowered to initiate PrEP without first discussing with their partners, some reported that their partners were non-supportive or distrustful of PrEP, leading to conflict within their relationships, a finding also reported among Kenyan MSM in a prior study [24]. Participants struggled with how to explain PrEP use to their HIV-negative primary partners, as its use implied either having concurrent partners or not trusting one’s partner and led to suspicion and conflict; few participants reported testing for HIV with their partners or discussing HIV testing or condom use. Our findings suggest that PrEP programs should support strategies for frequent HIV testing among PrEP users and their partners (including couples testing where feasible) and should support PrEP users in navigating discussions about PrEP use with their partners, particularly in the context of concordant negative relationships.
In this qualitative study population, as in the larger SEARCH study, PrEP was often discontinued; the principal reasons participants gave for their decision to stop PrEP were dissolution of partnerships and a changing perception of risk; unsupportive partners or peers; and early side effects and perceived pill burden. Some young adults who were interested in using PrEP also experienced structural barriers to PrEP continuation, such as school attendance, which made it difficult to initiate PrEP and be seen for follow-up visits. In line with our recent study that distance to clinic predicted lower PrEP uptake and retention [63], some people requested other delivery approaches or separate clinics for PrEP. Yet, despite our supportive delivery model with community- and clinic-based delivery options [64], many young people did not continue using PrEP.
In addition to highlighting challenges with discussing PrEP with partners, our data also revealed relatively rapidly evolving relationship contexts among our participants, particularly those young persons who were unmarried. Several participants chose to start PrEP while in a relationship and then chose to stop using it when that relationship ended. The concept of “seasons of risk” has been proposed for PrEP previously [65]. Our findings suggest that for young people, these seasons may be perceived as relatively brief and may be difficult to anticipate. Particularly for unmarried young people, many felt that they could not predict when they would have sex or plan for sex and could not start PrEP in advance. Discussions also revealed that some young people rejected PrEP because of messaging that several weeks of dosing were needed to achieve protective PrEP drug levels (and perceived this messaging to mean that abstinence from sex or condoms use were required). Our study, which began in 2016, recommended 28 days of PrEP use prior to fully protective drug levels given scientific debate about this threshold for vaginal exposure [66, 67]. Even with a lower threshold of 7 days to protection (which has since been recommended in Kenya guidelines) [68], some young people may find this level of required planning for sex untenable. During the study, we refined our messaging to focus less on time to achieve protection and more on consistent PrEP use. Nonetheless, further work is needed to refine messaging around time to protection from PrEP and the length of seasons of PrEP use in a way that makes sense to and fits within the lives and priorities of young adults.
There are several strengths of this study. We were able to interview individuals who were offered but declined to initiate PrEP, whereas most prior studies have only interviewed individuals who enrolled in a PrEP study and intended to initiate PrEP. In addition, no incentives were offered for study participation apart from initial transport to clinic for PrEP initiation. The study is also strengthened by the rigor of our interpretive approach (involving local research team members in the analysis process) and heterogeneous settings that strengthen applicability of findings to other rural eastern African settings. However, limitations to this research should be noted: data are cross-sectional, and collected in evolving contexts over the first year of PrEP implementation. In addition, because few adolescents (15–17 years of age) initiated PrEP, in part due to requirements for parental consent, we primarily interviewed PrEP initiators and decliners who were ages 18 and above. Thus this study’s finding are more useful for understanding the attitudes, beliefs and experiences of young adults than of adolescents under age 18.
As PrEP implementation expands, additional strategies are needed to enhance community knowledge of PrEP to support PrEP use among young people. PrEP messaging, counseling, and delivery models should address the diverse motivations and needs of young people. In addition, it will be critical to acknowledge that, for many young people, HIV prevention is less salient than life goals and other health and economic priorities. For young adults who desire “proof” of PrEP efficacy via testimonials, peers could play an essential role. Work is also needed to design strategies to support young people’s communication about PrEP with partners, parents, and peers. As PrEP rollout continues throughout eastern Africa, models to provide PrEP in the context of young peoples’ life priorities will be essential to achieving HIV prevention goals.
References
Birx D. PEPFAR & HIV prevention: locations and populations. HIV Research for Prevention (HIVR4P). Chicago, IL; 2016.
Canning D, Raja S, Yazbeck AS, eds. Africa’s demographic transition: dividend or disaster? Africa Development Forum Series. Washington, DC: World Bank; 2015.
Strathdee SA. State of the global HIV pandemic: where are we now? In: International AIDS conference, Durban, South Africa; 2016. [Abstract TUPL0102]
UNAIDS. Miles to go: closing gaps, breaking barriers, righting injustices. Geneva, Switzerland; 2018.
Thigpen MC, Kebaabetswe PM, Paxton LA, Smith DK, Rose CE, Segolodi TM, et al. Antiretroviral preexposure prophylaxis for heterosexual HIV transmission in Botswana. N Engl J Med. 2012;367(5):423–34.
Baeten JM, Donnell D, Ndase P, Mugo NR, Campbell JD, Wangisi J, et al. Antiretroviral prophylaxis for HIV prevention in heterosexual men and women. N Engl J Med. 2012;367(5):399–410.
World Health Organization. Consolidated guidelines on the use of antiretroviral drugs for treating and preventing HIV infection. 2nd ed. Geneva, Switzerland; 2016.
World Health Organization. WHO technical brief: preventing HIV during pregnancy and breastfeeding in the context of pre-exposure prophylaxis (PrEP). Geneva, Switzerland; 2017.
AVAC. Ongoing and planned PrEP demonstration and implementation studies. https://www.avac.org/resource/ongoing-and-planned-prep-demonstration-and-implementation-studies.
Delany-Moretlwe S, Chersich M, Harvey S, Stangl A, Baron D, Columbini M, et al. Empowerment clubs did not increase PrEP continuation among adolescent girls and young women in South Africa and Tanzania—Results from the EMPOWER randomised trial. In: International AIDS conference, Amsterdam, Netherlands; 2018.
Celum C, Delany-Moretlwe S, Hosek S, Dye BJ, Bekker LG, Mgodi N, et al. Risk behavior, perception, and reasons for PrEP among young African women in HPTN 082. In: Conference on retroviruses and opportunistic infections, Boston, MA; 2018.
Eakle R, Gomez GB, Naicker N, Bothma R, Mbogua J, Cabrera Escobar MA, et al. HIV pre-exposure prophylaxis and early antiretroviral treatment among female sex workers in South Africa: Results from a prospective observational demonstration project. PLoS Med. 2017;14(11):e1002444.
Mboup A, Behanzin L, Guedou FA, Nassirou G, Goma-Matsetse E, Giguere K, et al. Early antiretroviral therapy and daily pre-exposure prophylaxis for HIV prevention among female sex workers in Cotonou, Benin: a proscpective observational demonstration study. J Int AIDS Soc. 2018;21:e25208.
Cowan FM, Davey C, Fearon E, Mushati P, Dirawo J, Chabata S, et al. Targeted combination prevention to support female sex workers in Zimbabwe accessing and adhering to antiretrovirals for treatment and prevention of HIV (SAPPH-IRe): a cluster-randomised trial. Lancet HIV. 2018;5(8):e417–e426426.
Mugwanya KK, Irungu E, Bukusi E, Mugo NR, Odoyo J, Wamoni E, et al. Scale up of PrEP integrated in public health HIV care clinics: a protocol for a stepped-wedge cluster-randomized rollout in Kenya. Implem Sci. 2018;13(1):118.
Baeten JM, Heffron R, Kidoguchi L, Mugo NR, Katabira E, Bukusi EA, et al. Integrated delivery of antiretroviral treatment and pre-exposure prophylaxis to HIV-1-serodiscordant couples: a prospective implementation study in Kenya and Uganda. PLoS Med. 2016;13(8):e1002099.
Oluoch L, Mugo N, Roxby A, Wald A, Selke S, Magaret A, et al. Low uptake of preexposure prophylaxis among Kenyan adolescent girls at risk of HIV. In: Conference on retroviruses and opportunistic infections, Seattle, WA; 2019.
Kigozi B, Nabukalu D, Kigozi G, Nordenstedt H, Ekström A, Strömdahl S, et al. Preexposure prophylaxis: acceptability and retention in southwestern Uganda. In: Conference on retroviruses and opportunistic infections, Seattle, WA; 2019.
Kyongo J, Kiragu M, Karuga R, Ochieng C, Ngunjiri A, Wachihi C, et al. How long will they take it? Oral pre-exposure prophylaxis (PrEP) retention for female sex workers, men who have sex witih men and young women in a demonstration project in Kenya. In: International AIDS conference, Amsterdam, Netherlands; 2018.
Rousseau-Jemwa E, Bekker L-G, Bukusi EA, Delaney-Moretlwe S, Omollo V, Travill D, et al. Early persistence of HIV pre-exposure prophylaxis (PrEP) in African adolescent girls and young Women (AGYW) from Kenya and South Africa. HIV research for prevention (HIVR4P). Madrid, Spain; 2018.
Celum C, Mgodi N, Bekker LG, Hosek S, Donnell D, Anderson P, et al. PrEP adherence and effect of drug level feedback among young African women in HPTN 082. In: 10th IAS conference on HIV science, Mexico City, Mexico; 2019.
Toledo L, McLellan-Lemal E, Henderson FL, Kebaabetswe PM. Knowledge, attitudes, and experiences of HIV pre-exposure prophylaxis (PrEP) trial participants in Botswana. World J AIDS. 2015;5(2):10–20.
Amico KR, Wallace M, Bekker LG, Roux S, Atujuna M, Sebastian E, et al. Experiences with HPTN 067/ADAPT study-provided open-label PrEP among women in cape town: facilitators and barriers within a mutuality framework. AIDS Behav. 2016;21(5):1361–75.
Van der Elst EM, Mbogua J, Operario D, Mutua G, Kuo C, Mugo P, et al. High acceptability of HIV pre-exposure prophylaxis but challenges in adherence and use: qualitative insights from a phase I trial of intermittent and daily PrEP in at-risk populations in Kenya. AIDS Behav. 2013;17(6):2162–72.
van der Straten A, Stadler J, Montgomery E, Hartmann M, Magazi B, Mathebula F, et al. Women's experiences with oral and vaginal pre-exposure prophylaxis: the VOICE-C qualitative study in Johannesburg, South Africa. PLoS ONE. 2014;9(2):e89118.
Eakle R, Bothma R, Bourne A, Gumede S, Motsosi K, Rees H. "I am still negative": female sex workers' perspectives on uptake and use of daily pre-exposure prophylaxis for HIV prevention in South Africa. PLoS ONE. 2019;14(4):e0212271.
Institute of Medicine and National Research Council. Investing in the health and well-being of young adults. The National Academies Press, Washington, DC; 2015.
Gill K, Pidwell T, Dietrich J, Gray G, Bennie T, Myer L, et al. A demonstration open label study to assess the acceptability, safety and use of Truvada pre-exposure prophylaxis in healthy, HIV-uninfected adolescents, 15–19 years of age. In: 9th IAS conference on HIV science, Paris, France; 2017.
Adeyeye AO, Stirratt MJ, Burns DN. Engaging men in HIV treatment and prevention. Lancet. 2018;392(10162):2334–5.
Havlir DV, Balzer LB, Charlebois ED, Clark TD, Kwarisiima D, Ayieko J, et al. HIV testing and treatment with the use of a community health approach in rural Africa. N Engl J Med. 2019;381(3):219–29.
Koss CA, Ayieko J, Mwangwa F, Owaraganise A, Kwarisiima D, Balzer LB, et al. Early adopters of human immunodeficiency virus preexposure prophylaxis in a population-based combination prevention study in rural Kenya and Uganda. Clin Infect Dis. 2018;67(12):1853–60.
Chamie G, Clark TD, Kabami J, Kadede K, Ssemmondo E, Steinfeld R, et al. A hybrid mobile approach for population-wide HIV testing in rural east Africa: an observational study. Lancet HIV. 2016;3(3):e111–e119.
Zheng W, Balzer L, van der Laan M, Petersen M, SEARCH Collaboration. Constrained binary classification using ensemble learning: an application to cost-efficient targeted PrEP strategies. Stat Med. 2018;37(2):261–79.
Ajzen I. From intentions to actions: a theory of planned behavior. In: Kuhl J, Beckmann J, editors. Action-control: from cognition to behavior. Berlin, Germany: Springer; 1985. p. 11–39.
Catania JA, Kegeles SM, Coates TJ. Towards an understanding of risk behavior—an AIDS risk reduction model (ARRM). Health Educ Quart. 1990;17(1):53–72.
Wood W. Attitude change: persuasion and social influence. Annu Rev Psychol. 2000;51:539–70.
Rogers EM. Diffusion of innovations. 5th ed. New York, NY: Free Press, A Division of Simon & Schuster, Inc; 2003.
Parker R, Aggleton P. HIV and AIDS-related stigma and discrimination: a conceptual framework and implications for action. Soc Sci Med. 2003;57(1):13–24.
Connell RW. Gender and power: society, the person, and sexual politics. Stanford, CA: Stanford University Press; 1987.
Charmaz K. Constructing grounded theory. 2nd ed. Thousand Oaks, CA: Sage Publications, Inc.; 2014.
Fishbein M, Ajzen I. Belief, attitude, intention and behavior: an introduction to theory and research. Reading, MA: Addison-Wesley; 1975.
Bandura A. Social foundations of thought and action: a social cognitive theory. Englewood Cliffs, NJ: Prentice Hall; 1986.
Brown LK, DiClemente RJ, Reynolds LA. HIV prevention for adolescents: utility of the Health Belief Model. AIDS Educ Prev. 1991;3(1):50–9.
Cialdini RB. Influence: the psychology of persuasion, revised edition. New Work: William Morrow and Co., Inc.; 1993.
Patel RC, Stanford-Moore G, Odoyo J, Pyra M, Wakhungu I, Anand K, et al. "Since both of us are using antiretrovirals, we have been supportive to each other": facilitators and barriers of pre-exposure prophylaxis use in heterosexual HIV serodiscordant couples in Kisumu, Kenya. J Int AIDS Soc. 2016;19(1):21134.
Ware NC, Wyatt MA, Haberer JE, Baeten JM, Kintu A, Psaros C, et al. What's love got to do with it? Explaining adherence to oral antiretroviral pre-exposure prophylaxis for HIV-serodiscordant couples. J Acquir Immune Defic Syndr. 2012;59(5):463–8.
Carroll JJ, Ngure K, Heffron R, Curran K, Mugo NR, Baeten JM. Gendered differences in the perceived risks and benefits of oral PrEP among HIV-serodiscordant couples in Kenya. AIDS Care. 2016;28(8):1000–6.
Chitukuta M, Duby Z, Katz A, Nakyanzi T, Reddy K, Palanee-Phillips T, et al. Negative rumours about a vaginal ring for HIV-1 prevention in sub-Saharan Africa. Cult Health Sex. 2019:1–16.
van der Straten A, Stadler J, Luecke E, Laborde N, Hartmann M, Montgomery ET, et al. Perspectives on use of oral and vaginal antiretrovirals for HIV prevention: the VOICE-C qualitative study in Johannesburg, South Africa. J Int AIDS Soc. 2014;17(3 Suppl 2):19146.
Cohen CR, Montandon M, Carrico AW, Shiboski S, Bostrom A, Obure A, et al. Association of attitudes and beliefs towards antiretroviral therapy with HIV-seroprevalence in the general population of Kisumu, Kenya. PLoS ONE. 2009;4(3):e4573.
Mathur S, Romo D, Rasmussen M, Nakyanjo N, Nalugoda F, Santelli JS. Re-focusing HIV prevention messages: a qualitative study in rural Uganda. AIDS Res Ther. 2016;13:37.
Corneli AL, McKenna K, Headley J, Ahmed K, Odhiambo J, Skhosana J, et al. A descriptive analysis of perceptions of HIV risk and worry about acquiring HIV among FEM-PrEP participants who seroconverted in Bondo, Kenya, and Pretoria, South Africa. J Int AIDS Soc. 2014;17(3 Suppl 2):19152.
Price JT, Rosenberg NE, Vansia D, Phanga T, Bhushan NL, Maseko B, et al. Predictors of HIV, HIV risk perception, and HIV worry among adolescent girls and young women in Lilongwe, Malawi. J Acquir Immune Defic Syndr. 2018;77(1):53–63.
Thuo N, Ngure K, Ogello V, Kamolloh K, Burns B, Pyra M, et al. “So that I don’t get infected even if I have sex with someone who is positive:” Factors influencing PrEP uptake among young women in Kenya. HIV Research for Prevention (R4P). Madrid, Spain; 2018.
Haberer JE, Mugo N, Baeten JM, Pyra M, Bukusi E, Bekker LG. PrEP as a lifestyle and investment for adolescent girls and young women in Sub-Saharan Africa. J Int Assoc Provid AIDS Care. 2019;18:2325958219831011.
Amico KR, Bekker LG. Global PrEP roll-out: recommendations for programmatic success. Lancet HIV. 2019;6(2):e137–e140140.
Corneli A, Perry B, McKenna K, Agot K, Ahmed K, Taylor J, et al. Participants' explanations for nonadherence in the FEM-PrEP clinical trial. J Acquir Immune Defic Syndr. 2016;71(4):452–61.
Katirayi L, Chadambuka A, Muchedzi A, Ahimbisibwe A, Musarandega R, Woelk G, et al. Echoes of old HIV paradigms: reassessing the problem of engaging men in HIV testing and treatment through women's perspectives. Reprod Health. 2017;14(1):124.
Dovel K, Yeatman S, Watkins S, Poulin M. Men's heightened risk of AIDS-related death: the legacy of gendered HIV testing and treatment strategies. AIDS. 2015;29(10):1123–5.
Ngure K, Heffron R, Curran K, Vusha S, Ngutu M, Mugo N, et al. I knew I would be safer. Experiences of Kenyan HIV serodiscordant couples soon after pre-exposure prophylaxis (PrEP) initiation. AIDS Patient Care STDS. 2016;30(2):78–83.
Montgomery ET, van der Straten A, Chitukuta M, Reddy K, Woeber K, Atujuna M, et al. Acceptability and use of a dapivirine vaginal ring in a phase III trial. AIDS. 2017;31(8):1159–67.
Montgomery ET, van der Straten A, Stadler J, Hartmann M, Magazi B, Mathebula F, et al. Male partner influence on women's HIV prevention trial participation and use of pre-exposure prophylaxis: the importance of "understanding". AIDS Behav. 2015;19(5):784–93.
Mayer CM, Owaraganise A, Kabami J, Kwarisiima D, Koss CA, Charlebois ED, et al. Distance to clinic is a barrier to PrEP uptake and visit attendance in a community in rural Uganda. J Int AIDS Soc. 2019;22:e25276.
Jewell BL, Ayieko J, Owaraganise A, Mwangwa F, Kwarisiima D, Koss CA, et al. Community delivery increases PrEP uptake and retention in SEARCH study in Uganda and Kenya. In: International AIDS conference, Amsterdam, Netherlands; 2018.
Mugo NR, Ngure K, Kiragu M, Irungu E, Kilonzo N. PrEP for Africa: What we have learnt and what is needed to move to program implementation. Curr Opin HIV/AIDS. 2016;11(1):80–6.
Hendrix CW, Andrade A, Bumpus NN, Kashuba AD, Marzinke MA, Moore A, et al. Dose frequency ranging pharmacokinetic study of tenofovir-emtricitabine after directly observed dosing in healthy volunteers to establish adherence benchmarks (HPTN 066). AIDS Res Hum Retroviruses. 2016;32(1):32–433.
Cottrell ML, Yang KH, Prince HM, Sykes C, White N, Malone S, et al. A translational pharmacology approach to predicting outcomes of preexposure prophylaxis against HIV in men and women using tenofovir disoproxil fumarate with or without emtricitabine. J Infect Dis. 2016;214(1):55–64.
Ministry of Health National AIDS and STI Control Programme. Guidelines on use of antiretroviral drugs for treating and preventing HIV infection in Kenya 2018. Nairobi, Kenya; 2018.
Acknowledgements
We gratefully acknowledge the Ministries of Health of Uganda and Kenya, the SEARCH research team, collaborators and advisory boards, and especially all communities and participants involved. We also wish to thank Prof. Janet Seeley of the London School of Hygiene and Tropical Medicine for her helpful review of an earlier version of this manuscript.
Funding
Research reported in this article was supported by the National Institutes of Health, NIAID under award number UM1AI068636, NCT #01864603 (AIDS Clinical Trial Group, Kuritzkes PI; SEARCH Supplement, Havlir PI) and in part by the Bill and Melinda Gates Foundation and Gilead Sciences. CAK was also supported by funding from the National Institute of Mental Health (K23 MH114760) and the Gilead Research Scholars Program in HIV. The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH, PEPFAR, Bill and Melinda Gates Foundation or Gilead.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Camlin, C.S., Koss, C.A., Getahun, M. et al. Understanding Demand for PrEP and Early Experiences of PrEP Use Among Young Adults in Rural Kenya and Uganda: A Qualitative Study. AIDS Behav 24, 2149–2162 (2020). https://doi.org/10.1007/s10461-020-02780-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-020-02780-x