Abstract
Patient and regimen persistence in HIV-infected drug users are largely unknown. We evaluated patterns of medication non-persistence among HIV-infected drug users enrolled in a prospective, 6-month randomized controlled trial of directly administered antiretroviral therapy (DAART). Medication-taking behavior was assessed via direct observation and MEMS data. Of 74 participants who initiated DAART, 59 (80%) subjects were non-persistent with medication for 3 or more consecutive days. Thirty-one participants (42%) had 2 or more episodes of non-persistence. Higher depressive symptoms were strongly associated with non-persistence episodes of ≥ 3 days (AOR: 17.4, P = 0.02) and ≥ 7 days AOR: 5.4, P = 0.04). High addiction severity (AOR 3.2, P = 0.03) was correlated with non-persistence ≥ 7 days, and injection drug use (AOR: 15.2, P = 0.02) with recurrence of non-persistence ≥ 3 days. Time to regimen change was shorter for NNRTI-based regimens compared to PI-based ones (HR: 3.0, P = 0.03). There was no significant association between patterns of patient non-persistence and virological outcomes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Adherence to antiretroviral medications has been critical to improving health outcomes and preventing the development of drug resistance among HIV-infected individuals [1, 2]. Recent studies have demonstrated that the correlations between adherence, drug resistance, virological failure and other health outcomes are more complicated than once conceptualized. Rather, evidence suggests that improved adherence and drug resistance are not directly correlated and many other factors contribute to this relationship [3–6].
Medication persistence has been studied in the treatment of many chronic diseases. It has been used to assess the amount of time that a patient remains on chronic drug therapy as well as the time to discontinuation of therapy, even if temporarily. As with all chronic diseases, including HIV/AIDS, prescribed medications should be prescribed continuously over a lifetime. Generally, persistence is defined as “the duration of time from initiation to discontinuation of therapy” that must include a pre-specified limit on the number of days allowed between when medications are stopped and restarted, considered the “permissible gap” [7]. The permissible gap is the maximum allowable period until when patients could go without a dose and not experience suboptimal outcomes. Once a patient has exceeded the permissible gap, he or she is classified as being non-persistent. As is the case with a lifetime of expected continuous treatment, patients may inadvertently start and stop several times, resulting in repeated episodes of non-persistence.
Several studies have demonstrated low rates of treatment persistence and the associated negative health consequences for a number of medical conditions. In stroke patients, for example, 44.8% were persistent using a 30-day permissible gap criterion, and persistence with antiplatelet medication therapy was found to be significantly associated with delayed time to recurrent stroke hospitalization [8]. In treatment of rheumatoid arthritis, medication persistence was strongly correlated with favorable clinical and laboratory outcomes [9]. Low treatment persistence was observed among elderly patients prescribed statins, with 26% of patients taking their regimens optimally after 5 years [10]. In patients with ischemic heart disease, medication persistence with statins was associated with a lower risk of death, with 19% reduction in risk of death with each additional year of treatment [11]. Thus, non-persistence has been associated with negative health consequences for a number of medical conditions.
The concept of persistence was recently adopted as an innovative new way to assess medication-taking behavior for HIV treatment, with an emphasis on the continuity of therapy of both the regimen as well as for the patient [12]. In short, patient persistence measures the duration of a continuous therapy not exceeding a permissible gap, and is expressed specifically as time with measurements in days, weeks, or months. In contrast, adherence measures the frequency of times that a patient takes the medications as prescribed within a defined period of time, and is frequently measured as a percentage. Both persistence and adherence may be represented as a binary variable (i.e. adherent versus non-adherent and persistent versus non-persistent) in statistical analyses when validated constructs that are associated with treatment outcomes are known. In addition, the term regimen persistence was also created to define the duration between the initiation and discontinuation of a specified combination of antiretroviral medications as agreed upon by the patient and healthcare provider.
An increasing number of investigations suggest that in addition to adherence, patient persistence is important to optimize virological suppression and prevent the development of drug resistance. Retrospective studies have demonstrated that treatment interruptions longer than 2–4 days as well as repeated gaps lasting longer than 48 h are correlated with drug resistance development and treatment failure with some antiretroviral regimens [13–16]. This indicates that the permissible gap may be as short as 2 days, and that the frequency of gaps may be a factor in suboptimal outcomes. The importance of continuous therapy for the successful treatment of HIV has been confirmed by randomized controlled studies of scheduled treatment interruptions [17, 18].
Unstructured treatment interruptions of antiretroviral therapy are common among patients with HIV. One systematic review reported the proportion of patients interrupting treatment to be 23% for a median of 150 days, with recurrent interruptions of up to six episodes per person [19]. Drug toxicity, adverse events, side effects and treatment costs were the most frequently reported reasons for interruptions. The majority of patients who interrupt HIV treatment, however, only do so briefly, as they experience a rapid decline in CD4 count and increases in viral load soon after discontinuation. This contrasts significantly with the management of many other chronic diseases, where the interruption of therapy may not result in adverse consequences until weeks or months later. The result is a prolonged gap in treatment, which many consider to be equivalent to the indefinite discontinuation of therapy. On the other hand, brief interruptions in HIV treatment that exceed the permissible gap can be more accurately considered as episodes of non-persistence than complete discontinuation of therapy because of the brevity and frequency of gaps.
In particular, active drug users are at an increased risk of non-persistence as well as non-adherence [20–23] and are more likely to have poorer treatment HIV outcomes [21, 24]. One strategy that has been successful in increasing adherence and improving treatment outcomes in this vulnerable population is directly administered antiretroviral therapy (DAART) [25–27].
In the present study, we examined patterns of medication persistence among HIV-infected drug users participating in DAART as well as patient and medication characteristics associated with non-persistence. We also described recurrent episodes of non-persistence to assess how often patients stop medications beyond a permissible gap and have investigated the relationship between persistence and HIV treatment outcomes.
Methods
Study Design
The study design, primary outcomes [20, 25], and elements of the DAART intervention [28] have been described previously. Briefly, a 6-month, randomized controlled trial of DAART versus self-administered therapy (SAT) was conducted among 141 drug users. Participants were recruited from all of the HIV clinics in New Haven, Connecticut. Entry criteria included: (1) being HIV seropositive; (2) being eligible for and/or being prescribed antiretroviral medications; (3) residing within the city of New Haven; (4) active use of heroin and/or cocaine in the previous 6 months; and (5) receiving no more than a twice-daily regimen. Following informed consent, eligible participants were randomized 2:1 to DAART or self-administered therapy.
DAART participants received their antiretroviral medications at a mobile health unit that traveled to four New Haven inner city neighborhoods on weekdays [28]. All medication doses were placed in small plastic bags in a medication bottle with a Medication Electronic Monitoring System (MEMS) Version 6 Smart Cap (Aardex). A trained outreach worker observed one daily dose; all other doses were provided for the patient to take later, with a reminder from a beeper. Weekend doses were dispensed on Fridays and each patient had up to 3 days of an emergency supply of antiretroviral medications that were stored in the MEMS bottle.
In this study, only those participants who were randomized to and initiated DAART were included in the analysis.
Description of Co-Variates
Virologic success at 6 months for this predominantly antiretroviral-experienced population was defined a priori as having achieved an HIV-1 RNA level reduction of at least 1.0 log10 copies/ml or an HIV-1 RNA level < 400 copies/ml at 6 months. Missing values were imputed as virological failure.
Persistence was calculated using a combination of daily DAART observations and MEMS event data during the 6-month period of DAART. Subjects were considered to be on treatment for a given day if either there was: (1) an observed DAART dose or (2) a MEMS event. Missed DAART appointments due to hospitalization or imprisonment were corrected from verifiable clinical records of medication administration in these institutions.
Patient persistence and regimen persistence were defined as described previously [12]. Non-persistence was defined for three thresholds at any point during the 6-month intervention period: (1) ≥ 3 days (missing more than 2 consecutive days of antiretroviral medications); (2) ≥ 5 days; and (3) ≥ 7 days. Once a participant met the defined threshold gap, he or she was considered to be non-persistent. To determine the recurrence and true extent of non-persistence, all interruptions in treatment exceeding the proposed permissible gaps were considered to be non-persistent episodes. Recurrent non-persistence was defined as having more than one non-persistent episode, defined as gaps ≥ 3 days, within the 180-day observation period of the study. Time to patient non-persistence was defined as the number of days to the 1st day of a pre-defined first episode of non-persistence. Patients who were lost to follow-up were considered non-persistent from day of DAART discontinuation to day 180 of observation.
Regimen non-persistence was defined as any change in any component of the initial antiretroviral medication regimen. Time to regimen non-persistence was measured as the number of days between DAART initiation and regimen modification.
Baseline interviews assessed an array of psychosocial, demographic, and drug use characteristics. Addiction severity was assessed using binary outcomes (high severity if score ≥ 6) using the 10-item Drug Abuse Screening Test (DAST-10), a self-report measure of problematic substance use, widely used for clinical screening and research [29]. The Center for Epidemiological Studies Depression Scale (CES-D) [30], a 20-item self-report scale to measure depressive symptomatology, is highly correlated with having major depression when scores are ≥ 16. Participants’ attitudes towards DAART were also surveyed. Self-efficacy, which measures one’s sense of control over his life circumstances, was assessed using the Self-Efficacy Form [31]. Interviews were administered by non-clinical research assistants in research settings, but also included hospitals, prisons and drug-treatment settings if necessary. Heavy drinking was defined as more than two drinks per day for men and more than 1 per day for women on average. Heavy cocaine use was defined as use for more than 5 days per month. The following baseline demographic and psychosocial characteristics were included in analysis: age, gender, race, homelessness, education, heavy drinking, any cocaine use, heavy cocaine use, injection drug use, drug abuse severity, CES-D score, social support, self-efficacy, confidence that one can take medications as prescribed, preference for assistance with medication-taking, and willingness to travel for DAART. In addition, frequency of dosing, pill burden, and baseline viral load were included in analysis.
Statistical Analysis
All statistical analyses were performed using Stata SE (version 10.1, Stata Corp, TX, USA). Crude odds ratios were calculated using bivariate logistic regression. Univariate variables with a P-value < 0.10 were included in the multivariate logistic regression modeling, which were used to calculate adjusted odds ratios. Firth’s penalized-likelihood logistic regression was used for bivariate analyses when complete separation occurred [32]. Time to regimen non-persistence, stratified by the antiretroviral therapy based on the 1st day of DAART, was plotted as Kaplan–Meier curves, and a hazard ratio was calculated using Cox proportional-hazards regression.
Results
Patterns of Patient Non-Persistence
Of the 74 participants who initiated DAART, 15 (20%) were completely persistent, not missing 3 or more days, during the 6-month intervention period. The patterns of non-persistence are described in Table 1. Among the 59 (80%) participants who were non-persistent for ≥ 3 days, the mean and median numbers of non-persistence episodes were 2.66 [standard error (SE): ± 0.42] and 1.0 [interquartile range (IQR) 1–3], respectively. The mean and median lengths of non-persistence gaps were 15.0 (SE: ± 2.08) and 4.0 (IQR 3–6) days, respectively. Kaplan–Meier estimates for the time to first non-persistence gap, stratified by length of treatment lapses in therapy, are presented in Fig. 1.
Time to patient non-persistence among DAART subjects, stratified by the length of non-persistence. A subject was categorized as “non-persistence ≥ 3 days” if he missed 3 or more consecutive days of antiretroviral medications at any point during the DAART intervention period. Non-persistence ≥ 5 days and non-persistence ≥ 7 days were defined similarly. Each Kaplan–Meier failure curve represents the same population of subjects (N = 74)
Factors Associated with Patient Non-Persistence
Demographic, psychosocial, and medication characteristics along with other factors thought to be associated with patient non-persistence are presented in Table 2. Having higher depressive symptomatology (CES-D ≥ 16) was significantly associated with non-persistence ≥ 3 days (AOR = 17.4; 95% CI 1.5–204.1, P = 0.02). Similarly, univariate analyses for non-persistence ≥ 7 days were significantly associated with having higher depressive symptoms (OR = 7.2; 95% CI 1.5–35.7, P = 0.02) and having high addiction severity (OR = 3.9; 95% CI 1.5–10.2, P < 0.01). The statistical significance for these outcomes was preserved in multivariable analysis for both having increased depressive symptoms (AOR = 5.4; 95% CI 1.1–27.5, P = 0.04) and higher addiction severity (AOR = 3.2; 95% CI (1.1–9.2, P = 0.03). No other factors were significantly associated with non-persistence ≥ 3 or ≥ 7 days. Non-persistence ≥ 5 days was not significantly associated with any identified covariates.
Of the 59 DAART participants who had any type of predefined non-persistence, 31 (52.5%) had two or more episodes of non-persistence (Table 2). Univariate analyses showed statistically significant associations with injection drug use (OR = 7.1; 95% CI 1.4–36.9, P = 0.02), low self-efficacy (OR = 0.3; 95% CI 0.1–0.9, P = 0.03), and high-confidence in taking medications as prescribed (OR = 0.3; 95% CI 0.01–0.80, P = 0.02) with medication non-persistence. In multivariate analysis, only injection drug use (AOR = 15.2; 95% CI 1.8–129.1, P = 0.02) was significantly associated with recurrent non-persistence. Compared to once-daily dosing, twice daily dosing had a trend towards an increased risk of recurrent non-persistence (AOR = 6.3, 95% CI 1.0–40.0, P = 0.05).
Correlates of Virological Success
In univariate linear analysis, there was no statistically significant association between virological success and non-persistence (data not shown).
Regimen Non-Persistence
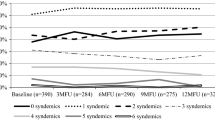
Among the 74 DAART participants, 20 (26%) subjects modified their antiretroviral regimen during the 6-month intervention period and were thereby defined as having regimen non-persistence. Of the demographic and psychosocial characteristics, only low social support (AOR = 2.9; 95% CI 1.0–8.4, P < 0.05) was statistically associated with regimen non-persistence. Kaplan-Meier estimates for the time to regimen non-persistence, stratified by the antiretroviral therapy backbone on the 1st day of DAART, are presented in Fig. 2. Time to regimen non-persistence was significantly shorter for NNRTI-based regimen compared to a PI-based regimen (HR = 3.0; 95% CI 1.1–7.9; P = 0.03). No significant relationship between regimen non-persistence and patient non-persistence was observed.
Time to regimen non-persistence among DAART subjects, stratified by the antiretroviral therapy backbone on the 1st day of DAART (N = 74). Regimen non-persistence was defined as any change in antiretroviral medication during the intervention period of the study. The P-value was calculated with Cox proportional-hazards regression. (Legend: NNRTI non-nucleoside reverse transcriptase inhibitors, PI protease inhibitor)
Discussion
To our knowledge, this study is the only one to examine non-persistence among subjects enrolled in a directly administered antiretroviral therapy program. We report a high rate of patient non-persistence among HIV-infected drug users receiving modified DAART, where weekend dosing was not observed, but recorded using MEMS cap data. Among 74 subjects, 59 (80%) were non-persistent with therapy for 3 or more consecutive days, and 33 subjects (45%) for ≥ 7 consecutive days. Thirty-one patients (42%) had more than one episode of non-persistence lasting ≥ 3 days.
These rates of medication non-persistence are higher than previously reported among diverse population within cohorts, but not specifically among drug-using populations. In a Swiss cohort study, in which adherence was measured through self-report, only 5.8% of patients had non-persistence longer than 24 h [33]. In a prospective study in Uganda, 23% of patients admitted on questionnaires to more than 4 days of treatment interruption [14]. In a French study of 71 patients, including only 12 IDUs, 19 (27%) subjects experienced more than one episode of non-persistence lasting 48 h or more [16]. In a Spanish study, in which 48% of patients were IDUs, 43% of patients per self-report had non-persistence lasting more than 3 days [13].
Several factors may be contributing to the high rate of non-persistence reported in this paper. First, our sample includes only active drug users and drug users have been demonstrated to have problematic adherence to therapy [21, 22]. This study also confirms that drug use, even in the setting of an evidence-based adherence intervention, is associated with problematic non-persistence. Since persistence and adherence are interrelated, and influenced by a number of socioeconomic, clinical, and medication characteristics [12], it is not surprising that this patient population had a high rate of non-persistence.
Second, patient persistence data obtained through self-report may unrealistically underestimate the true frequency and length of non-persistent events, despite some studies suggesting adherence patterns can be accurately reported [34]. Unlike other studies, medication-taking behavior was measured through a combination of direct observation and MEMS caps in this study. This methodology produced detailed and objective data, thereby increasing sensitivity of detecting non-persistence events and reducing patients’ social desirability response bias. In another study in which MEMS was used to assess non-persistence, a similarly high rate of patient non-persistence was observed; among 97 non-drug using subjects, 65% of patients had a treatment interruption lasting more than 3 or more days [15].
Third, transportation issues or inconvenience of traveling to receive DAART may have contributed to a higher than usual rate of non-persistence. We have previously demonstrated, however, that patients randomized to DAART were more adherent to therapy and more successful at virologic suppression than those who self-administered their antiretroviral therapy [20, 25]. Therefore, although possible, it is unlikely that DAART has contributed significantly to the high rate of non-persistence.
In this study, we did not find a significant association between patterns of patient non-persistence and virologic success, which is contrary to findings reported in previous studies. In the Spanish study with a median follow-up of 8.3 years, patients with non-persistence longer than 3 days were at a higher risk of treatment failure (adjusted related hazard 1.39; 95% CI 1.04–1.85) [13]. In the Ugandan study, 13% of patients who had a non-persistent episode ≥ 3 days had developed drug resistance, in contrast to no one with continuous treatment (P = 0.047) [15]. Finally, among patients on an NNRTI-based regimen who were followed for a median of 29 months, those with at least two episodes of non-persistence lasting ≥ 3 days were at a higher risk of developing virologic failure (adjusted hazard ratio 3.3; P = 0.011), and resistance to NNRTI (hazard ratio 22.5; P < 0.0001) [16].
Failure to find an association between non-persistence and virologic success in this study may be attributed to several factors. First, the small sample size likely resulted in an inadequate power to avoid a Type II error. Second, both persistence and virologic outcome data were limited to 6 months of intervention, and it is possible that this period may have been insufficiently long enough to detect a statistically significant association, in contrast to other studies in which patients were followed for years. Third, the impact of non-persistence on virologic outcomes is likely different depending on a patient’s antiretroviral regimen. Because of a low genetic barrier to resistance development as well as long half-lives of NNRTI’s, it is hypothesized that longer term non-persistence may have a greater negative impact on patients on an NNRTI-based regimen than those on a PI-based one; however, short treatment gaps may favor NNRTI-based regimens due to their longer half lives [5]. A high proportion (60%) of patients on a PI-based regimen in this cohort may have required a greater power to detect a statistically significant association between non-persistence and virologic outcomes.
In analysis of factors associated with non-persistence, high levels of addiction severity were associated with an increased risk of non-persistence of 7 days or more. Additionally, patients actively injecting drugs were more like to have multiple episodes of non-persistence. This study is the first to confirm the association of active drug use and severity on non-persistence in patients receiving DAART.
Previous studies have reported that active drug users are at an increased risk of treatment interruptions [23], non-adherence [24], and poor HIV treatment outcomes [21, 22]. Our findings that patients with high levels of addiction severity and active use are at an increased risk of non-persistence and recurrent episodes of treatment gaps are consistent with existing literature, and therefore not surprising. Because of the grave impact active drug use has on adherence, persistence, and HIV outcomes, a substance dependence treatment program must be considered as an integral part of HIV treatment for active drug users. Buprenorphine/naloxone integrated into HIV treatment settings has shown promising results, and was associated with improved HIV treatment outcomes among opioid-dependent patients infected with HIV, especially those treated for longer durations [35].
HIV-infected patients with substance use disorders frequently have an underlying psychiatric disorder [36, 37]. Since depression has been linked to decreased adherence and shorter survival as well as increased treatment interruptions [38], it is not surprising that patients with higher levels of depressive symptoms were less persistent with therapy. Incorporation of effective pharmacotherapy and counseling, as has been shown among homeless persons with HIV [39], in addition to treatment of active drug use, would benefit patients triply diagnosed with HIV, substance use, and depression.
Finally, PI-based regimens were associated with increased regimen persistence compared to NNRTI-based regimens. This finding is also inconsistent with existing literature that NNRTI-based regimens tend to be more persistent than PI-based, triple-NRTI-based, or triple-class regimens [40–43]. One explanation for these results is that among drug users with high rates of non-adherence and non-persistence, PI-based regimens may yield favorable treatment outcomes due to the shorter half-lives and higher genetic barrier to resistance development of PIs compared to NNRTIs; however, due to unavailability of data on reasons explaining regimen non-persistence (i.e. regimen modification), we cannot determine if this is in fact the case in this study.
There are several important limitations to this study. The study population was small, restricted to a single inner-city community, and studied among those who received antiretroviral therapy via direct observation. This limits the generalizability of these findings. Furthermore, the analyses presented here were not part of preplanned analyses comparing randomized groups. As such, the inferences made here must be considered as tentative and hypothesis-generating rather than definitive. Patients who dropped out were considered non-persistent for the remaining duration of the study, although it is possible that they resumed or continued therapy in a non-research setting. Finally, pill-pocketing or non-adherence to MEMS caps instructions, and associated bias in persistence data cannot be excluded.
Further prospective studies are therefore needed to better understand both patient and regimen persistence, factors associated with them, and their impact on HIV treatment outcomes.
References
Altice FL, Friedland GH. The era of adherence to HIV therapy. Ann Intern Med. 1998;129(6):503–5.
Montaner JSG, Reiss P, Cooper D, et al. A randomized, double-blind trial comparing combinations of nevirapine, didanosine, and zidovudine for HIV-infected patients. JAMA. 1998;279(12):930–7.
Bangsberg DR, Charlebois ED, Grant RM, et al. High levels of adherence do not prevent accumulation of HIV drug resistance mutations. AIDS. 2003;17(13):1925–32.
Bangsberg DR, Moss AR, Deeks SG. Paradoxes of adherence and drug resistance to HIV antiretroviral therapy. J Antimicrob Chemother. 2004;53(5):696–9.
Parienti JJ, Das-Douglas M, Massari V, et al. Not all missed doses are the same: sustained NNRTI treatment interruptions predict HIV rebound at low-to-moderate adherence levels. PLoS One. 2008;3(7):e2783.
Parienti JJ, Ragland K, Lucht F, et al. Average adherence to boosted protease inhibitor therapy, rather than the pattern of missed doses, as a predictor of HIV RNA replication. Clin Infect Dis. 2010;50(8):1192–7.
Cramer JA, Roy A. Medication compliance and persistence: terminology and definitions. Value Health. 2008;11(1):44–7.
Burke JP, Sander S, Shah H, Zarotsky V, Henk H. Impact of persistence with antiplatelet therapy on recurrent ischemic stroke and predictors of nonpersistence among ischemic stroke survivors. Curr Med Res Opin. 2010;26(5):1023–30.
Contreras-Yanez I, Cabiedes J, Villa AR, Rull-Gabayet M, Pascual-Ramos V. Persistence on therapy is a major determinant of patient-, physician- and laboratory- reported outcomes in recent-onset rheumatoid arthritis patients. Clin Exp Rheumatol. 2010;28(5):748–51.
Benner JS, Glynn RJ, Mogun H, Neumann PJ, Weinstein MC, Avorn J. Long-term persistence in use of statin therapy in elderly patients. Jama. 2002;288(4):455–61.
Hippisley-Cox J, Coupland C. Effect of statins on the mortality of patients with ischaemic heart disease: population based cohort study with nested case-control analysis. Heart. 2006;92(6):752–8.
Bae JW, Guyer W, Grimm K, Altice FL. Medication persistence in the treatment of HIV infection: a review of the literature and implications for future clinical care and research. AIDS. 2011;25(3):279–90.
Knobel H, Urbina O, Gonzalez A, et al. Impact of different patterns of nonadherence on the outcome of highly active antiretroviral therapy in patients with long-term follow-up. HIV Med. 2009;10(6):364–9.
Spacek LA, Shihab HM, Kamya MR, et al. Response to antiretroviral therapy in HIV-infected patients attending a public, urban clinic in Kampala, Uganda. Clin Infect Dis. 2006;42(2):252–9.
Oyugi JH, Byakika-Tusiime J, Ragland K, et al. Treatment interruptions predict resistance in HIV-positive individuals purchasing fixed-dose combination antiretroviral therapy in Kampala, Uganda. AIDS. 2007;21(8):965–71.
Parienti JJ, Massari V, Descamps D, et al. Predictors of virologic failure and resistance in HIV-infected patients treated with nevirapine- or efavirenz-based antiretroviral therapy. Clin Infect Dis. 2004;38(9):1311–6.
Ananworanich J, Nuesch R, Le Braz M, et al. Failures of 1 week on, 1 week off antiretroviral therapies in a randomized trial. AIDS. 2003;17(15):F33–7.
El-Sadr WM, Lundgren JD, Neaton JD, et al. CD4 + count-guided interruption of antiretroviral treatment. N Engl J Med. 2006;355(22):2283–96.
Kranzer K, Ford N. Unstructured treatment interruption of antiretroviral therapy in clinical practice: a systematic review. Trop Med Int Health. 2011. doi:10.1111/j.1365-3156.2011.02828.x.
Maru DS, Bruce RD, Walton M, et al. Initiation, adherence, and retention in a randomized controlled trial of directly administered antiretroviral therapy. AIDS Behav. 2008;12(2):284–93.
Lucas GM, Cheever LW, Chaisson RE, Moore RD. Detrimental effects of continued illicit drug use on the treatment of HIV-1 infection. J Acquir Immune Defic Syndr. 2001;27(3):251–9.
Lucas GM, Gebo KA, Chaisson RE, Moore RD. Longitudinal assessment of the effects of drug and alcohol abuse on HIV-1 treatment outcomes in an urban clinic. AIDS. 2002;16(5):767–74.
Kavasery R, Galai N, Astemborski J, et al. Nonstructured treatment interruptions among injection drug users in Baltimore, MD. J Acquir Immune Defic Syndr. 2009;50(4):360–6.
Arnsten JH, Demas PA, Grant RW, et al. Impact of active drug use on antiretroviral therapy adherence and viral suppression in HIV-infected drug users. J Gen Intern Med. 2002;17(5):377–81.
Altice FL, Maru DS, Bruce RD, Springer SA, Friedland GH. Superiority of directly administered antiretroviral therapy over self-administered therapy among HIV-infected drug users: a prospective, randomized, controlled trial. Clin Infect Dis. 2007;45(6):770–8.
Macalino GE, Hogan JW, Mitty JA, et al. A randomized clinical trial of community-based directly observed therapy as an adherence intervention for HAART among substance users. AIDS. 2007;21(11):1473–7.
Berg KM, Litwin A, Li X, Heo M, Arnsten JH. Directly observed antiretroviral therapy improves adherence and viral load in drug users attending methadone maintenance clinics: a randomized controlled trial. Drug Alcohol Depend. 2011;113(2–3):192–9.
Altice FL, Mezger JA, Hodges J. Developing a directly administered antiretroviral therapy intervention for HIV-infected drug users: implications for program replication. Clin Infect Dis. 2004;38(Suppl 5(s5)):S376–87.
Yudko E, Lozhkina O, Fouts A. A comprehensive review of the psychometric properties of the Drug Abuse Screening Test. J Subst Abuse Treat. 2007;32(2):189–98.
Radloff LS. The CES-D Scale. Applied psychological measurement. 1977;1(3):385–401.
Huba GJ, Melchior, LA, Staff of the Measurement Group, and HRSA/HAB’s SPNS Cooperative agreement steering committee Module 64: self-efficacy form 1996; http://www.TheMeasurementGroup.com. Accessed July 7 2011.
Heinze G, Schemper M. A solution to the problem of separation in logistic regression. Statist Med. 2002;21(16):2409–19.
Glass TR, De Geest S, Weber R, et al. Correlates of self-reported nonadherence to antiretroviral therapy in HIV-infected patients: the Swiss HIV Cohort Study. J Acquir Immune Defic Syndr. 2006;41(3):385–92.
Knobel H, Alonso J, Casado JL, et al. Validation of a simplified medication adherence questionnaire in a large cohort of HIV-infected patients: the GEEMA Study. AIDS. 2002;16(4):605–13.
Altice FL, Bruce RD, Lucas GM, et al. HIV treatment outcomes among HIV-infected, opioid-dependent patients receiving buprenorphine/naloxone treatment within HIV clinical care settings: results from a multisite study. J Acquir Immune Defic Syndr. 2011;56:S22–32.
Zahari MM, Bae WH, Zainal NZ, Habil H, Kamarulzaman A, Altice FL. Psychiatric and substance abuse comorbidity among HIV seropositive and HIV seronegative prisoners in Malaysia. Am J Drug Alcohol Abuse. 2010;36(1):31–8.
Altice FL, Kamarulzaman A, Soriano VV, Schechter M, Friedland GH. Treatment of medical, psychiatric, and substance-use comorbidities in people infected with HIV who use drugs. Lancet. 2010;376(9738):367–87.
Lima VD, Geller J, Bangsberg DR, et al. The effect of adherence on the association between depressive symptoms and mortality among HIV-infected individuals first initiating HAART. AIDS. 2007;21(9):1175–83.
Tsai AC, Weiser SD, Petersen ML, Ragland K, Kushel MB, Bangsberg DR. A marginal structural model to estimate the causal effect of antidepressant medication treatment on viral suppression among homeless and marginally housed persons with HIV. Arch Gen Psychiatry. 2010;67(12):1282–90.
Braithwaite RS, Kozal MJ, Chang CC, et al. Adherence, virological and immunological outcomes for HIV-infected veterans starting combination antiretroviral therapies. AIDS. 2007;21(12):1579–89.
MacArthur RD, Novak RM, Peng G. A comparison of three highly active antiretroviral treatment strategies consisting of non-nucleoside reverse transcriptase inhibitors, protease inhibitors, or both in the presence of nucleoside reverse transcriptase inhibitors as initial therapy (CPCRA 058 FIRST Study): a long-term randomised trial. Lancet. 2006;368(9553):2125–35.
Springer SA, Friedland GH, Doros G, Pesanti E, Altice FL. Antiretroviral treatment regimen outcomes among HIV-infected prisoners. HIV Clin Trials. 2007;8(4):205–12.
Willig JH, Abroms S, Westfall AO, et al. Increased regimen durability in the era of once-daily fixed-dose combination antiretroviral therapy. AIDS. 2008;22(15):1951–60.
Acknowledgments
The authors would like to acknowledge the National Institutes on Drug Abuse (R01 DA13805) for funding this study and career development award for FLA (K24 DA 0170720). DSRM is a Global Health Equity Fellow at Brigham and Women’s Hospital. The funding sources played no role in the design of the study, data collection, analysis or interpretation of results or in the writing of the report. We would like to thank Paula Dellamura for administrative support. Most importantly, we would like to thank the research staff and the study participants who dedicated time and energy to make this research possible. Without their help, this research would not have been possible.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ing, E.C., Bae, J.W., Maru, D.SR. et al. Medication Persistence of HIV-infected Drug Users on Directly Administered Antiretroviral Therapy. AIDS Behav 17, 113–121 (2013). https://doi.org/10.1007/s10461-011-0082-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-011-0082-0