Abstract
Background
Sex-related differences in the role of androgen have been reported in cardiovascular diseases and angiogenesis. Moreover, androgen receptor (AR) has been causally involved in the homeostasis of human prostate endothelial cells. However, levels of expression, functionality and biological role of AR in male- and female-derived human endothelial cells (ECs) remain poorly characterized. The objectives of this work were (1) to characterize the functional expression of AR in male- and female-derived human umbilical vein endothelial cell (HUVEC), and (2) to specifically analyze the biological effects of DHT, and the role of AR on these effects, in male-derived HUVECs (mHUVECs).
Results
Immunohistochemical analyses of tissue microarrays from benign human tissues confirmed expression of AR in ECs from several androgen-regulated and non-androgen-regulated human organs. Functional expression of AR was validated in vitro in male- and female-derived HUVECs using quantitative RT-PCR, immunoblotting and AR-mediated transcriptional activity assays. Our results indicated that functional expression of AR in male- and female-derived HUVECs was heterogeneous, but not sex dependent. In parallel, we analyzed in depth the biological effects of DHT, and the role of AR on these effects, on proliferation, survival and tube formation capacity in mHUVECs. Our results indicated that DHT did not affect mHUVEC survival; however, DHT stimulated mHUVEC proliferation and suppressed mHUVEC tube formation capacity. While the effect of DHT on proliferation was mediated through AR, the effect of DHT on tube formation did not depend on the presence of a functional AR, but rather depended on the ability of mHUVECs to further metabolize DHT.
Conclusions
(1) Heterogeneous expression of AR in male- and female-derived HUVEC could define the presence of functionally different subpopulations of ECs that may be affected differentially by androgens, which could explain, at least in part, the pleiotropic effects of androgen on vascular biology, and (2) DHT, and metabolites of DHT, generally thought to represent progressively more hydrophilic products along the path to elimination, may have differential roles in modulating the biology of human ECs through AR-dependent and AR-independent mechanisms, respectively.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Androgen receptor (AR) is a ligand-inducible transcription factor, and a member of the steroid–thyroid–retinoid receptor superfamily, that mediates the biological effects of androgens in a wide range of physiological and pathological processes [1]. An increasing body of the literature that demonstrates expression of AR in endothelial cells (ECs) from several human tissues [2–8] suggests a potential role for androgens, acting through AR-mediated processes, in modulation of human EC homoeostasis [9–11]. However, up until now, the biological effects, and the molecular signals/mechanisms, driven by AR in an EC context, still remain poorly characterized.
Androgen signaling plays a key role in several high-incidence and high-prevalence human diseases, such as cardiovascular diseases (CVDs), benign prostate hyperplasia (BPH) and prostate cancer (CaP) [9–11]. Interestingly, in these pathological processes, androgens have been hypothesized to exert their role, at least partially, by modulating EC homeostatic function, presumably acting through AR [8, 12–15]. In the case of CVDs, interaction between androgens and the endothelial cells of the blood vessel wall has been hypothesized based on the following observations: (1) testosterone (T) supplementation inhibits the formation of atheroma in animal models [16], (2) androgen withdrawal is associated with decreased central arterial compliance in humans [17], (3) T is a protective factor against atherosclerosis through immunomodulation of plaque development and stability [18], (4) long-term oral administration of T induces endothelium-dependent and endothelium-independent vaso-relaxation [19], and (5) conversely, men have a higher incidence of cardiovascular disease than women during their reproductive years, with gender differences diminishing after female menopause [20], suggesting that androgens are associated causally with an increased risk of cardiovascular disease in both men [20] and women [21]. As supported by these pieces of evidences, the role of androgens in cardiovascular physiology and physiopathology remains controversial, and therefore, a better understanding of the molecular links between androgen and endothelial cell biology are required in order to unravel the pathogenesis of CVDs.
In androgen-responsive human prostate tissue, withdrawal of androgenic signaling by AR antagonists (e.g., flutamide or bicalutamide) and/or inhibitors of steroid metabolism (e.g., finasteride or dutasteride) inhibited hematuria due to BPH or after prostate surgery [22]. Moreover, two clinical studies [23, 24] in CaP patients have shown that a combination therapy with bicalutamide/goserelin (a gonadotropin-releasing hormone agonist) and dutasteride induced a profound vascular collapse and reduced prostate tissue vascularity. Our group [25] confirmed prostate vascular involution was induced by androgen withdrawal in benign and malignant human prostate tissue transplanted to SCID mice and that this effect was correlated temporally with induction of EC apoptosis. However, the androgen signaling in human prostate ECs requires more in-depth characterization at the mechanisms of action of AR.
Even though an increasing body of the literature documenting the effects of androgens on human vasculature has been developed over the last 10 years, the paradigm of the mechanism of action of androgens on the homeostatic function of human ECs generally is attributed to the effects of androgens being mediated through modulation of other (non-endothelial) cell types in the tissue microenvironment, specially in prostate tissue microenvironment. In this study, the androgen-responsive HUVECs were utilized as model to characterize mechanistically the biological role of androgens, acting through endogenous AR-mediated signaling, in human ECs. Our analysis indicated that expression of AR in HUVECs could define the presence of functionally different subpopulations of EC that may be affected differentially by androgens, and that DHT, and metabolites of DHT, may have differential roles in modulating the biology of human ECs through AR-dependent, and AR-independent, mechanisms, respectively.
Materials and methods
Cell cultures
Primary cultures of HUVECs were isolated from fresh umbilical cords obtained from male and female fetuses according to previously published reports [26, 27]. Human umbilical cords were collected with the approval of the Ethics and Biosafety Committee at Pontifical Catholic University. HUVECs also were obtained commercially from PromoCell (PromoCell, Heidelberg, Germany). All HUVECs were cultured in EC growth media (PromoCell) supplemented with 5 % FBS. LNCaP cells were obtained commercially from ATCC (ATCC, Manassas, VA) and cultured in RPMI-1640 media supplemented with 10 % FBS.
Reverse transcription, PCR and quantitative real-time PCR
Total RNA from primary cultures of HUVEC and LNCaP cell was prepared using the RNAeasy mini-kit (Qiagen, Valencia, CA). Reverse transcription from mRNA was performed using the SuperScript™ III First-Strand kit (Invitrogen, Carlsbad, CA) [25]. Quantitative real-time PCR (QRT-PCR) was performed using power SYBR Green PCR Master Mix (Applied Biosystems, Carlsbad, CA) in the ABI PRISM 7300 system [25]. The cycle conditions were 50 °C for 2 min, 95 °C for 10 min followed by 40 cycles of 95 °C for 15 s and 60 °C for 1 min. Primer sequences for RT-PCR and QRT-PCR are detailed in Supplementary Table 1.
Immunostaining
Immunostaining was performed according to standard procedures [8]. HUVECs were previously stimulated with or without DHT for 24 h. AR (1:100, Santa Cruz Biotechnology, Santa Cruz, CA) and CD31 (Dako, Carpinteria, CA) co-localization analyses were performed using the mouse/rabbit EnVision™ G/2 Double Stain System (Dako) [28]. AR expression was detected using an HRP-conjugated secondary antibody and 3,3-diaminobenzidine tetrahydrochloride as substrate (brown precipitate). CD31 expression was visualized using an alkaline phosphatase-conjugated secondary antibody and Permanent Red as substrate (red precipitate). Immunostaining in the absence of primary antibody provided negative controls.
AR ligand-binding assay
HUVECs were pre-incubated for 24 h in EC growth media supplemented with 5 % charcoal-stripped FBS before binding assays. Total R1881 binding to AR was determined by incubation of cells for 4 h at 37 °C in increasing concentrations of [17∝-methyl-3H]-R1881 (Perkin-Elmer, Waltham, MA) that ranged from 0.01 to 6 nM. Non-specific binding was determined by analysis of total binding in the presence of a 500-fold excess of non-radiolabeled R1881 (Perkin-Elmer) under the same experimental conditions. Specific binding of [3H]-R1881 was calculated by subtraction of the non-specifically bound radioactivity from the total bound radioactivity. The K d value for R1881 was determined using Scatchard analysis [8] (reciprocal of the slope [−1/K d ]) and represents the average of three independent experiments, each performed in triplicate.
AR-mediated luciferase assay
HUVEC and LNCaP cell were incubated for 24 h in EC growth media (HUVEC) or RPMI media (LNCaP), supplemented with 5 % charcoal-stripped FBS. Cells were infected for 3 h with an adenoviral expression vector that encoded either an MMTV promoter- or PSA promoter-driven luciferase reporter (10–20 infectious units/cell) and then stimulated with or without (vehicle, ethanol) DHT for 36 h [8, 29]. Demonstration of inhibition of MMTV-driven luciferase reporter activity by the anti-androgen bicalutamide was achieved by the maintenance of HUVEC cultures in the presence of designated concentrations of bicalutamide throughout the entire duration of the experiment (3-h infection + 36-h incubation).
Flow microfluorimetry
Cell permeabilization was performed using the Caltag Fix and Perm Cell permeabilization kit (Caltag Laboratories, San Francisco, CA). HUVEC were stained immunofluorescently with mouse antihuman CD31 (1:20; Dako) and rabbit antihuman AR (1:100; Santa Cruz Biotechnology) primary antibodies and subsequently with fluorescently labeled species-specific secondary antibodies. Staining was assessed using the FACSCalibur (BD Bioscience with CellQuest software for Macintosh) and analyzed using FCS Express (DeNovo Software, Los Angeles, CA). Briefly, cohorts of cells were deprived of androgen for 24 h (−24 h) or 48 h (−48 h), or were deprived of androgen for 48 h after which androgen (1.0 nM DHT) was re-introduced into the culture media for an additional 24-h period (−48 + 24). As a positive control, cells were treated with serum-free medium for the same intervals of time. Both floating and attached cells were collected from cultures and subjected to CD31 staining, as well as to staining with annexin-V-FITC and propidium iodide (PI) using protocols provided by the manufacturer (BD Biosciences, San Jose, CA).
Immunoblotting
Proteins from cytosol and nuclear cell extracts were isolated using the NE-PER nuclear and cytoplasmic extraction reagents (ThermoFisher Scientific). Cytosol, nuclear and total cell extracts (50 µg of protein) were separated electrophoretically using SDS–polyacrylamide gel electrophoresis (10 % w/v; Bio-Rad Laboratories, Hercules, CA) and the separated proteins transferred to nitrocellulose membranes [8]. Nitrocellulose membranes were incubated with the primary antibodies: anti-AR (1:1000, Santa Cruz Biotechnology), anti-cleaved PARP (1:1000, Cell Signaling, Beverly, MA), anti-caspase-3 (1:500, Cell Signaling), anti-Bcl2 (1:1000, Dako), anti-FXR (1:500, R&D systems, Minneapolis, MN), anti-RXRα (1:500, Santa Cruz Biotechnology), anti-β-actin (1:1000, Santa Cruz Biotechnology), anti-β-tubulin (1:3000, AbCam), anti-Histone H3 (1:1000, Cell Signaling). After this, nitrocellulose membranes were incubated with the corresponding HRP-conjugated anti-mouse or anti-rabbit IgG secondary antibody. Antibody localization was visualized using enhanced chemiluminescence (Pierce Biotechnology).
Microtiter tetrazolium (MTT) and cell counting assays
The effect of DHT on population growth of HUVECs was assessed over a 10-day period using the MTT [3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyl-tetrazolium bromide] method. Cells (5 × 102 cells/well) were inoculated into 96-well plates in 100 µl of medium. The plated cells were allowed to attach overnight, after which the media was replaced with fresh media containing either 1.0 nM DHT, or vehicle (ethanol). Cell growth was determined by the MTT assay on days 0, 1, 3, 5, 7 and 10 after DHT stimulation. For the MTT assay, medium was removed from the wells, and 200 µl of Hepes buffer was added to each well, followed by addition of 50 µl of MTT (2.5 mg/ml in PBS, Sigma-Aldrich, St. Louis, MO). The wells were incubated for 4 h at 37 °C, after which the liquid in the well was aspirated and replaced by 200 µl of dimethyl sulfoxide (Sigma-Aldrich) and 25 µl of Sorensen’s buffer. The optical density was measured at 570 nm using an ELISA reader (EL800, BioTek Instruments, Winooski, VT). For cell counting assays, wells were treated with either 1.0 nM DHT or vehicle, and cell number counted on days 0, 1, 3, 5, 7 or 10 after DHT stimulation. Attached cells were collected by trypsinization and counted using a hemocytometer. Trypan blue dye exclusion was used to determine viable cells.
EC tube formation assay
Matrigel (176 µl, BD Biosciences) was dispensed into wells of a 24-well plate and incubated for 30 min at 37 °C in 5 % CO2 for the Matrigel to solidify [8]. HUVECs were suspended at a density of 100 × 103 cells/ml in 500 µl of EC growth media supplemented with 5 % charcoal-stripped FBS and designated concentrations of DHT (0.01, 0.1, 1, 10 nM). Aliquots of HUVECs (50 × 103 cells) were seeded into wells that contained solidified Matrigel and were incubated for 24 h at 37 °C in 5 % CO2. The effect of DHT on EC tube formation was analyzed by collection of four random digital images per well (4× magnification), and total length of tubular structures was quantified per image using Optimas 6.2 (Media Cybernetics, Bethesda, MD).
Statistical analysis
Statistical evaluation of data was performed using SuperANOVA software (Abacus Concepts, Berkeley, CA). All data differences were considered statistically significant when the p value was <0.05.
Results
AR is expressed in human ECs of multiple organs
Expression of AR in human ECs was validated by immunostaining analyses of microarrays of tissue sections of a diversity of benign human tissues (Fig. 1). AR protein was observed in ECs in brain, endometrium, myometrium, ovary and prostate tissue (Fig. 1a–d, g). However, several benign human tissues, such as thyroid, colon, liver, lung, pancreas, spleen, stomach and kidney, showed no AR immunostaining in ECs (Fig. 1e–g). Within the immunopositive tissues, AR immunostaining was present in ECs of both micro- and macro-vasculatures; however, AR expression at the level of the individual EC was heterogeneous; some ECs showed AR immunostaining, others did not.
AR expression in ECs from benign human tissues. AR expression was analyzed in a tissue microarray containing benign human specimens of brain, breast, colon, endometrium, kidney, liver, lung, myometrium, ovary, pancreas, prostate, skeletal muscle, skin, spleen, stomach, testes, thyroid and tonsil. Expression of AR at the EC level was observed in brain (a), endometrium (b), myometrium (c), ovary (d), prostate and skin (g) (black arrows). However, ECs from stomach (e), thyroid (f), lung, skeletal muscle and kidney (g) showed no expression of AR in ECs. Black bar 50 µm
Functional expression of endogenous AR in female- and male-derived HUVECs does not depend on the sex
Primary cultures of HUVECs isolated from umbilical cords obtained from female and male fetuses were utilized to characterize in vitro the expression and functionality of AR. First, we analyzed the expression of AR protein in female- and male-derived HUVEC cultures that were cultured through 10 consecutive passages after isolation (Fig. 2a). Our results indicated that AR expression was maintained during all these passages in female- and male-derived HUVEC culture (Fig. 2a). Therefore, all subsequent studies in HUVECs were performed using cultures within the first 5 passages. Interestingly, both female and male HUVECs expressed both the 110-kDa full-length AR and a shorter band, around 85 kDa, which might indicate the presence of a short AR variant [30]. Notably, this band was more robust in female than in male HUVEC cultures (Fig. 2a). In parallel, we analyzed expression of AR at the mRNA and protein level in 10 different cultures of female- and male-derived HUVECs (data not shown). In Fig. 2b, c, we show expression of AR mRNA and protein in 4 different male- and 4 different female-derived HUVEC cultures. Our results indicated that expression of AR was variable in both female-derived and male-derived HUVEC cultures. Interestingly, this variability was not related to the gender of the fetus from which HUVECs were obtained (Fig. 2b, c). Functional activity of the endogenous AR in female and male HUVEC was confirmed by measurement of AR-mediated transcriptional activity using an adenoviral MMTV promoter-driven luciferase gene reporter after stimulation with or without DHT for 36 h (Fig. 2d). Our results confirmed that functionality of endogenous AR in female-derived and male-derived HUVECs did not depend on the sex of the HUVEC cultures and it was not correlated with the level of expression of the AR protein. Together, these data indicate that the levels of expression and functionality of AR in HUVECs associated more to a still unexplained inter-donor variability rather than a sex-related variability. In order to pursue with our analysis, and to correlate our results with what we previously observed using human prostate-derived ECs, we decided to focus our study on the expression and functionality of AR in male-derived HUVEC cultures (here after mHUVECs ) (Fig. 3). Expression of AR mRNA and protein, and AR protein translocation to the nucleus after 24 h of DHT stimulation was demonstrated in mHUVECs using RT-PCR (Fig. 3a), immunocytochemistry (Fig. 3b) and immunoblotting (Supplementary Figure 1). Analysis of co-localization of AR and CD31 confirmed expression of AR in ECs (Fig. 3c). Ligand-binding affinity of AR in mHUVECs was analyzed using the radiolabeled synthetic AR agonist/ligand, R1881. Specific binding of R1881 to AR in mHUVECs increased in a dose-dependent manner, and binding saturated above a ligand concentration of 2.0 nM (Fig. 3d). Scatchard transformation of the ligand-binding data resulted in a straight line, indicative of a single ligand-binding site for R1881, with a K d 0.1 nM (Fig. 3e). Functional activity of the endogenous AR in mHUVECs was confirmed by measurement of AR-mediated transcriptional activity using an adenoviral MMTV promoter- or PSA promoter-driven luciferase gene reporter. DHT increased the reporter activity driven by the MMTV promoter fivefold in mHUVECs (Fig. 3f, MMTV). However, DHT did not stimulate expression of the luciferase reporter driven by the epithelial cell-specific PSA promoter (Fig. 3f, PSA). Functionality of the PSA-driven reporter construct was validated using LNCaP cells (Fig. 3f, PSA). The MMTV promoter is promiscuous, and MMTV-driven transcription can be stimulated by nuclear steroid receptors others than AR (i.e., GR and PR) [31]. Consequently, expression of GR and PR nuclear receptors was analyzed in mHUVECs using immunocytochemistry (data not shown). Both nuclear receptors (GR and PR) were expressed in mHUVECs ; however, neither of them translocated to the nucleus after DHT treatment, which suggested that they were not involved in MMTV-driven transcriptional activity. Furthermore, causal participation of AR in the MMTV-driven transcriptional activity in mHUVECs was validated using the anti-androgen bicalutamide. DHT-stimulated, AR-mediated, MMTV-driven luciferase reporter activity was inhibited in a dose-dependent manner by bicalutamide (Fig. 3g).
AR expression and functionality in female- and male-derived HUVECs. a AR protein expression was analyzed using immunoblotting in a female- and a male-derived HUVEC culture, which was cultured through 10 (p1–p10) consecutive passages. β-Actin (actin) was used as loading control, b analysis of AR mRNA expression in 4 different female-derived HUVEC cultures and 4 different male-derived HUVEC cultures using QRT-PCR. LNCaP cells were used as positive control, c the same sets of HUVEC cultures were analyzed for AR protein expression using immunoblotting, d AR-mediated transcriptional activity was analyzed in the same set of female- and male-derived HUVECs infected with an adenoviral MMTV-driven luciferase gene reporter in the absence (vehicle, white bars) and presence (black bars) of 1 nM DHT. AR-mediated transcriptional activity was inhibited by the anti-androgen bicalutamide (gray bars). LNCaP cells were used as positive control
Functional expression of AR in mHUVECs. a AR mRNA expression was analyzed using RT-PCR. LNCaP cells were used as positive control. Std: marker ladder. bp base pair, RT reverse transcription, b AR immunostaining in HUVEC in the absence (vehicle) or presence of 1 nM DHT, c AR and CD31 double immunostaining in HUVEC exposed to 1 nM DHT, d specific [3H]-R1881 binding activity in HUVEC, e scatchard plot of the binding data from graph D, f AR-mediated transcriptional activity in HUVEC infected with adenoviral MMTV- or PSA-driven luciferase gene reporter, g AR-mediated transcriptional activity was inhibited in a dose-dependent manner by the anti-androgen bicalutamide, and h co-expression of AR and CD31 was analyzed in HUVEC using flow cytometry. LNCaP cells were used as positive control for AR expression
As was observed for ECs in multiple benign human tissues in situ (Fig. 1), expression of AR in mHUVECs in vitro was heterogeneous; only a fraction of these cells expressed AR in culture (Fig. 3h). The proportion of AR-expressing male-derived HUVEC was quantitated using flow cytometry to identify cells that co-expressed AR and CD31 (Fig. 3h). The percentage of AR-positive male-derived HUVEC varied according to the cell culture population analyzed, ranging from less than 5 %, to as high as 60 % (Fig. 3h).
Androgens do not affect survival in vitro in male-derived HUVECs
Androgen deprivation was associated with a reduction in microvessel density (MVD), and appearance of apoptotic ECs, in primary xenografts of human benign and malignant prostate tissue [25], which suggested androgen modulated directly EC survival. The role of androgen in EC survival was investigated in vitro in mHUVECs by exposure of cells to 24, or 48 h, of androgen deprivation. As a control of loss/maintenance of AR protein and functionality in the absence of androgen, mHUVECs also were exposed to 48 h of androgen deprivation followed by 24 h of replenishment with exogenous androgen. Quantitative RT-PCR analyses demonstrated no significant variation in the levels of AR mRNA in mHUVECs exposed to androgen deprivation (Fig. 4a). However, AR protein level was diminished consistently in mHUVECs by androgen deprivation, as demonstrated using immunoblotting (Fig. 4b) and immunostaining (Fig. 4c) analyses. Automated image analysis of AR immunostaining was used to quantitate the number of nuclei immunopositive for AR as a percentage of the total nuclei. Statistical evaluation of the data demonstrated the acute removal of androgen resulted in a significant (p < 0.001) decrease (up to ~60 %) in the number of AR immunopositive nuclei (Fig. 4d). Under these conditions, immunoblotting analyses revealed that the level of expression of the pro-apoptotic marker, cleaved PARP, was unaffected by the removal of androgen from mHUVECs (Fig. 4e). The protein level of the pro-apoptotic marker cleaved caspase-3 was slightly decreased, and of the anti-apoptotic marker bcl-2 slightly increased, by androgen deprivation. However, replenishment of androgen (1.0 nM DHT) did not return bcl-2 nor the cleaved-caspase-3 levels to baseline. In parallel, the induction of apoptosis in mHUVECs by androgen deprivation was evaluated using the Annexin V-FITC Apoptosis Detection Kit with flow cytometric analysis (Fig. 4f). Apoptotic cells were defined as Annexin V-FITC positive, PI negative cells (bottom right quadrant of multi-parameter data plot). Only a slight increase in the number of apoptotic mHUVECs was observed after either 24 h (from 1.16 to 1.98 %) or 48 h (from 1.16 to 2.41 %) of androgen deprivation, and this increase was reversed when androgen was replenished (Fig. 4f). As a positive control for induction of apoptosis as detected by immunoblotting and Annexin V-FITC analyses, mHUVECs were exposed to serum starvation for 24 and 48 h. Serum starvation resulted in a robust increase in the number of apoptotic cells, as well as in the expression of cleaved PARP and a decrease in bcl-2 expression at 24 and 48 h (data not shown).
DHT does not affect EC survival in mHUVECs. HUVEC were exposed to 24 or 48 h of androgen deprivation. HUVEC also were exposed to 48 h of androgen deprivation followed by 24 h of replenishment of androgen (1 nM DHT). Control cells were maintained in regular media supplemented with 1 nM DHT. Expression of AR was analyzed using QRT-PCR (a), immunoblotting (b) and immunostaining (c) analyses. d Automated image analysis of the AR immunostaining in HUVECs (*p < 0.001); 10 (×40) independent images were quantified per condition. e Expression of pro-apoptotic (cleaved PARP, cleaved caspase 3) and anti-apoptotic (bcl-2) markers were analyzed using immunoblotting. f Apoptotic levels were confirmed using Annexin-V/PI kit
Androgen modulates proliferation and tube formation capacity in male-derived HUVECs using independent mechanisms
In vitro studies in primary cultures of human prostate ECs indicated that activation of AR by exogenous DHT increased EC proliferation [8]. The effect of androgen on cell growth in mHUVECs was analyzed using the MTT cell proliferation assay of cell number (Fig. 5a) and trypan blue exclusion assay of cell viability (Fig. 5b). mHUVECs were cultured for 1–10 days in the absence (vehicle) or presence of 1.0 nM DHT. Both methodologies independently demonstrated a significant (p < 0.05) increase in mHUVEC growth in the presence of 1.0 nM DHT compared to vehicle (ethanol). The causal role of AR in the induction of EC growth was demonstrated by the capacity of the anti-androgen bicalutamide to block the DHT-activated, AR-mediated growth (Fig. 5c).
Androgen modulates mHUVEC proliferation and tube formation using independent mechanisms. a, b The effect of androgen on HUVEC growth was analyzed by counting viable cells using the trypan blue exclusion method (a) and the MTT cell proliferation assay (b). HUVEC were cultured for 1–10 days in the absence (white circles, vehicle) or presence (black circles, 1 nM DHT) of DHT. c Treatment with bicalutamide confirmed AR-activated EC proliferation. The effect of DHT on endothelial tube formation in Matrigel™ was analyzed in the presence of increasing concentrations of DHT (0.01, 0.1, 1, 10 nM). d Relative tube length was expressed as percentage of the control (white circles, 0 nM), and cell viability was evaluated in parallel using the trypan blue exclusion method (black circles). Effect of DHT on endothelial tube formation was not affected by bicalutamide (e) and not observed when R1881 was used (f, g). *p < 0.05
The effect of androgen on tube formation in Matrigel by mHUVECs was analyzed in the presence of increasing concentrations of androgen (Fig. 5d). DHT significantly decreased, in a dose-dependent manner, the ability of mHUVECs to form tubes in Matrigel. This effect was less pronounced than the effect of DHT on mHUVEC proliferation and was more evident at higher concentrations of DHT (10 nM). In order to confirm/discard the role of AR in the inhibitory action of DHT on tube formation, the effect of bicalutamide on the ability of DHT to inhibit tube formation by mHUVECs was tested (Fig. 5e). Bicalutamide did not revert the inhibitory effect of DHT on tube formation by mHUVECs, which suggested that AR was not involved in mediating this effect. Because higher concentrations of DHT were needed to affect tube formation capacity than to inhibit proliferation by mHUVECs which occurred at concentrations consistent with the K d of DHT for AR (0.1 nM), and considering that AR appeared not to be involved in this effect because bicalumatide did not reverse the inhibition of tube formation, we hypothesized that the inhibition of tube formation was dependent on the ability of mHUVECs to metabolize DHT to other bioactive moieties. To test this hypothesis, R1881, a synthetic, non-metabolizable (Fig. 5f) AR agonist, was utilized to explore whether the inhibition of tube formation was dependent on further bioconversion of DHT into one or more metabolites. R1881 did not reproduce the inhibitory effect of DHT on the ability of mHUVECs to form tubes in Matrigel (Fig. 5g), in contrast to the ability of R1881 to substitute DHT for stimulation of proliferation (data not shown), supporting the hypothesis that further metabolization of DHT is required to produce the molecule(s) that inhibit(s) tube formation in vitro.
DHT could potentially be converted to 3α-androstanediol/androsterone metabolites in male-derived HUVECs
DHT can be metabolized via two different pathways [32] (Fig. 6a). The family of enzymes called 3β-hydroxysteroid dehydrogenase (3β-HSD), of which two members (HSD3β1 and HSD3β2) have been described in human cells, metabolize DHT to 3β-androstanediol (3β-diol). Alternatively, DHT can be metabolized to 3α-androstanediol (3α-diol) and androsterone by the sequential action of two distinct families of enzymes, the 3α-hydroxysteroid dehydrogenase (3α-HSD) and the 17β-hydroxysteroid dehydrogenase (17β-HSD) or to androstanedione and androsterone by the sequential action of 17β-HSD and 3α-HSD (Fig. 6a). Four members of the 3α-HSD family and fourteen members of the 17β-HSD family have been described in human cells [32]. In this study, RT-PCR was utilized to analyze mRNA expression of the two members of the family of enzymes 3β-HSD and select members of the families of 3α-HSD (3α-HSD2, 3α-HSD3, 3α-(20α) HSD) and 17β-HSD (17β-HSD2 and 17β-HSD3) enzymes (Fig. 6b, c). mHUVECs lacked expression of mRNA for both members of the 3β-HSD enzyme family (Fig. 6b). However, mHUVECs expressed mRNA of three members (3α-HSD2, 3α-HSD3, 3α-(20α) HSD) of the 3α-HSD enzyme family (Fig. 6c) and at least one member (17β-HSD2) of the 17β-HSD enzyme family (Fig. 6c). The pattern of expression of enzymes involved in metabolic deactivation of DHT suggests 3α-androstanediol and/or androsterone as candidates for mediation of the effect of androgen on EC tube formation.
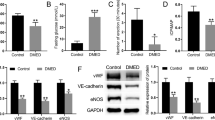
Expression of the enzymes involve in the metabolism of DHT in mHUVECs. a, b Expression of the mRNA for the enzymes HSD3β1 and HSD3β2 was analyzed in HUVEC exposed to vehicle (lanes 1) and 1 nM DHT (lanes 2). LNCaP cells were used as positive control (lanes 3). GAPDH was used as a loading control. a, c Expression of the mRNA for the enzymes 3α-HSD2 (lanes 1, 7, 13), 3α-HSD3 (lanes 2, 8, 14), 3α-(20α) HSD (lanes 3, 9, 15), 17β-HSD2 (lanes 4, 10, 16) and 17β-HSD3 (lanes 5, 11, 17) in HUVEC. GAPDH was used as a loading control (lanes 6, 12, 18). Prostate tissue was used as positive control (lanes 13–18). Expression of the FXR receptor was analyzed using RT-PCR (d) and immunoblotting (e) analyses in HUVEC exposed to vehicle (lanes 1) and 1 nM DHT (lanes 2). HepG2 cells were used as positive control (lanes 3). Expression of RXRα was analyzed using immunoblotting (e). GAPDH and β-actin were used as loading control for RT-PCR and immunoblotting, respectively
Androsterone has been reported to be a ligand capable of activation of the farnesoid X receptor (FXR), a signaling pathway with the potential to modulate EC homeostasis [33–35]. This hypothesis was tested by analysis of the expression of FXR at the mRNA and protein levels in mHUVECs. Neither mRNA (Fig. 6d) nor protein (Fig. 6e) for FXR was expressed in mHUVECs. mRNA isolated from five different donors of mHUVECs (Supp. Figure 2A) was analyzed, demonstrating that inter-patient variability was not responsible for the lack of expression of FXR. Furthermore, the possibility that lack of FXR mRNA in mHUVECs reflected the presence of splicing variants of FXR was excluded through the design of primer sets that covered multiple regions of the FXR coding sequence of the two known human FXR splice variants [36]. None of the variants were expressed in mHUVECs (Supp. Figure 1B). In contrast, expression of the retinoid X receptor alpha (RXRα), a known partner for FXR for production of heterodimers, was detected in mHUVECs (Fig. 6e). Together, these data support the hypothesis that 3α-androstanediol/androstanedione/androsterone might modulate mHUVECs tube formation through a mechanism that does not involve FXR.
Discussion
Over the last two decades, a considerable number of studies have focused on elucidation of the role of androgen on different aspects of vascular biology and atherogenesis. However, the role of androgen as a causal or a protective factor and the importance of the interplay of androgens with estrogens in the etiology and pathogenesis of cardiovascular disease remain controversial [15–21, 37]. Furthermore, while the role of androgen in hormonally sensitive tissues has been explored extensively, the role of circulating androgens in vascular biology in hormonally sensitive tissues, such as prostate tissue, is not understood [12, 13, 23, 25].
Typically, circulating T is the source of androgen that is metabolized in the target tissue to DHT, by the action of the 5α-reductases, or to 17β-estradiol by the action of aromatase (CYP19). Both enzymatic processes occur in ECs [38, 39]; therefore, the net biological effect of T on EC biology may depend on the tissue-specific relative contribution of the activities of both families of enzymes (reductases and aromatase). Based on the fact that DHT is the most bioactive androgen in human cells, having fivefold higher affinity for AR than T [40], and that AR expression in ECs is documented in several human tissues [2–8], in this study we utilized DHT as the source of androgen rather than T, because DHT cannot be aromatized, avoiding the potential for confounding effects mediated through the estrogen receptor in response to the conversion of T to 17β-estradiol.
Previous reports [2–8] of expression of AR in ECs from several human tissues were confirmed in this study. Interestingly, AR-positive ECs were observed both in “classical” and in “non-classical” hormonal target tissues, which suggest an EC-specific role for AR in these tissues. In support of this hypothesis, the present study showed that prostate epithelial cell-specific promoters that are trans-activated by AR, specifically the PSA (Fig. 3f) and probasin (not shown) promoters, were not transactivated by endogenous AR in endothelial cells, suggesting EC-specific roles for AR/co-regulators. Furthermore, the functional characterization of AR in HUVEC in this study demonstrated a dissociation constants (K d ) of AR for DHT around 0.1 nM, consistent with the reported K d for AR in prostate epithelial cells [41], suggesting also an important role for cell-type specific co-regulators of AR-mediated transcription. On this regard, it is important to highlight that the experimentally determined K d predicts a “theoretical” maximum capacity for activation of AR in ECs at concentrations around 1–2 nM DHT. However, some studies [42] that investigated the biological effects of androgen in HUVECs used concentrations of DHT that were far above the predicted range for maximal activation of AR, reaching levels of DHT as high as 400 nM. Using such high concentrations of DHT and claiming that the biological effects are produced by activation of AR, therefore, appear of unknown predictive value.
An interesting observation of this work was the detection of a shorter band (around 85 kDa) for AR. The molecular size of this band was concordant with expression of a shorter AR variant [43], which up until now have been described to be expressed only in prostate cancer cells, in which they have been proposed as a possible explanation for the transition from androgen-sensitive to castration-resistant phenotype [44]. Even though these observations are preliminary, it would be interesting to investigate whether these AR variants may have a physiological role in normal/benign cells, especially endothelial cells, and whether or not these AR variants may show differential expression between male- and female-derived ECs [43–45].
A previous study by Sieveking et al. [42] reported that androgen modulated angiogenesis capacity in HUVECs in a gender-related manner, indicating that AR was expressed at a higher level in male fetus-derived HUVECs compared to female fetus-derived HUVECs. Our study, however, challenged these results indicating that differences in the level of expression of AR in HUVECs were more associated with an inter-donor rather than a gender-related variability. In our study, AR expression and functionality were variable in male- and in female-derived HUVECs, showing male and female HUVEC cultures with high, medium or low levels of expression of AR (Fig. 2b, c). In accordance with our results, a study reported by Yoshida et al. [11, 45] indicated that both male and female AR knockout mice showed impaired revascularization after ischemia. Yoshida et al. [11, 45] attributed their different results, compared to the Sieveking’s study, to the different animal models utilized in both studies [11]. Although our results support Yoshida’s conclusions, they cannot rule out the possibility that this variability might be more associated with difference in the number of AR immunopositive ECs observed in either male or female ECs nor the type of organ involve in each analysis. Our results in mHUVEC (Fig. 3h) indicated that the AR immunopositive cells varied from 0 to up to 60 % between donor and donor, which might explain, at least in part, this controversy.
Even though AR expression and functionality have been studied in great detail in prostate luminal epithelial/epithelial cancer cells, few studies have focused on analysis of the expression and functionality of AR in non-epithelial cell compartments. Our group has a long-standing interest in unraveling the molecular mechanisms associated with the AR function in non-epithelial (endothelial and stromal) prostate cells [8–10, 14, 46–48]. Interestingly, mHUVECs have demonstrated to reproduce most of the biological effects of androgens observed in prostate endothelial cells [8]. Therefore, in this study we concentrated our efforts to unravel the biological effects of androgen, and the role of AR on these effects, in mHUVECs. Our study indicated that DHT had differential effects on multiple on mHUVEC processes: DHT did not affect EC survival; stimulated EC proliferation; and suppressed EC tube formation on Matrigel. From these biological processes, only EC proliferation was modulated directly by activation of AR. Endothelial cell survival has been demonstrated to be affected negatively by androgen deprivation in animal models [12, 23, 24]. Our group demonstrated that apoptosis of human prostate ECs was induced acutely by androgen deprivation in human prostate tissue transplanted to SCID mice [25]. However, whether endothelial cell apoptois was a direct response to androgen deprivation, and the role of perturbation of AR-mediated gene transcription in this process, are questions that remain unanswered. In the current study, androgen deprivation demonstrated no effect on survival of mHUVEC in vitro, in contrast to marked effect on ECs in human prostate xenografts in situ [25]. Considering that both types of ECs express AR, the lack of induction of apoptosis by androgen deprivation in the in vitro studies suggests that androgen deprivation also might activate/deactivate paracrine signaling in the prostate microenvironment that could induce/contribute to EC death in vivo.
In androgen-responsive human prostate tissue, the primary role of AR has been hypothesized to be to drive and maintain differentiation of the secretory luminal epithelial cells. However, in CaP, AR activity has been associated with regulation of cancer epithelial cell growth and/or survival. Mechanistic investigations revealed that AR acts as a master regulator of the G1-S phase transition in CaP epithelial cells. AR-mediated signaling promotes G1 cyclin-dependent kinase (CDK) activity and induces phosphorylation/inactivation of the retinoblastoma tumor suppressor (RB) protein, thereby governing androgen-stimulated proliferation [49]. The current study and our previous studies with primary cultures of human prostate ECs [8] suggest that AR is involved causally in the regulation of human EC proliferation (Fig. 6). Studies by Cai et al. [50] suggested that androgens acting on AR stimulated human aortic EC proliferation through upregulation of VEGF-A, cyclin A and cyclin D. However, the detailed molecular mechanism(s) by which AR regulates proliferation in human ECs is still poorly understood. Interestingly, in vitro, EC proliferation was “activated” by, but not “dependent” on, the presence of an active AR, since EC proliferation was observed, although at a reduced level, in the absence of androgen, as well as in the presence of the anti-androgen bicalutamide. This response could be related to the presence of both AR-expressing and AR-negative compartments in the HUVEC population.
Angiogenesis is an integral part of both normal and pathological processes. The role of androgens in angiogenesis has been considered in some detail in animal and human models, but mostly at the tissue level. In humans, the effect of androgen on tumor angiogenesis has been studied in prostate tissue, with changes in microvessel density correlated with tumor progression both in an androgenic environment and after ADT [13]. Consequently, androgenic effects on tumor angiogenesis have been proposed to be driven largely by indirect mechanisms principally associated with androgen-mediated regulation of VEGF expression by prostate epithelial cells [13], and the subsequent effect on EC survival. Surprisingly, no studies have explored the direct effect of androgen on the angiogenic capacity of human ECs. In order to explore the direct effect of androgen on human EC function, we utilized the tube formation assay, a well-established assay that models the in vitro formation of tubular structures that resembles a capillary network in a three-dimensional architecture. Unexpectedly, DHT decreased the ability of mHUVEC to form tubes on Matrigel, and the effect was not dependent on the presence of an active AR in mHUVECs, but rather depended on the ability of mHUVECs to metabolize further DHT.
DHT can be converted to 3β-androstanediol by the action of the enzyme 3β-hydroxysteroid dehydrogenase [32]. Alternatively, DHT can be metabolized directly to 3α-androstanediol and subsequently androsterone by sequential activity of two families of enzymes: the 3α-hydroxysteroid dehydrogenases and the 17β-hydroxysteroid dehydrogenases, respectively. A role for 3β-androstanediol in regulation of EC homeostasis was discarded based on the lack of expression of the mRNA for any members of the family of 3β-hydroxysteroid dehydrogenases in mHUVEC. Therefore, we initially hypothesized that the DHT metabolite androsterone was a plausible candidate for the DHT metabolite likely to affect tube formation capacity of mHUVEC through activation of the FXR [33, 34]. Consistent with this hypothesis, this study demonstrated that several members of the families of enzymes that participate in the conversion of DHT to androsterone were expressed in mHUVEC. Furthermore, FXR expression was reported in rat pulmonary ECs, where activated FXR leads to down-regulation of endothelin-1 expression [34]. In addition, activated FXR was reported to promote MMP-9-dependent EC motility through regulation of focal adhesion kinase (FAK) activity [51] in human ECs. However, expression of mRNA or protein for FXR was absent in mHUVEC, contrasting with the reports of Bishop-Bailey et al. [33] and He et al. [34] that FXR was expressed broadly in human ECs.
The current study appears to exclude the possibility of androsterone-mediated activation of FXR as a key modulator of endothelial tube formation by mHUVEC. However, more analyses are necessary to clarify whether conversion of DHT to androsterone is responsible for the inhibitory effect of androgen on EC tube formation in vitro. An alternative explanation for our results would posit that 3α-androstanediol is the/a key modulator of angiogenic capacity in mHUVEC. However, further studies are necessary to clarify whether 3α-androstanediol, androstanedione, and/or the further metabolite androsterone are modulators of tube formation capacity and the putative mechanism involved in this effect (Fig. 7).
Schematic representation of the effects of androgen in human ECs. Androgen affects EC homeostasis at multiple levels. DHT stimulates (+) EC proliferation through activation of androgen receptor (AR, red arrows). On the other hand, conversion of DHT to 3α-androstanediol/androsterone (3α-diol/AND) seems to be necessary for androgen to negatively regulate (−) tube formation (3α-diol/AND, blue arrows). Two options for the mechanism of action of 3α-diol/AND are hypothesized in this schema: 1 3α-diol/AND modulates target genes through binding/activation of a putative intracellular receptor and 2 3α-diol/AND needs to be exported outside the cell in order to activate membrane receptors which in turn activate signaling cascades that result in modulation of target gene expression/angiogenic capacity. (Color figure online)
In summary, our analysis supports the following conclusions: (1) expression of AR in human ECs could define presence of functionally different subpopulations of ECs that may be affected differentially by androgens, which could explain, at least in part, the paradigm of the contradictory effects of androgen on vascular biology, and (2) DHT, and metabolites of DHT, generally thought to represent progressively more hydrophilic products along the path to deactivation and elimination, may have differential roles in modulating the biology of human ECs using AR-dependent and AR-independent mechanisms, respectively. This unique observation provides a new paradigm for regulation of endothelial cell homeostasis and opens new avenues of exploration to better understand the role of androgen in human ECs.
References
Laudet V, Hanni C, Coll J, Catzeflis F, Stehelin D (1992) Evolution of the nuclear receptor gene superfamily. EMBO J 11(3):1003–1013
Blauer M, Vaalasti A, Pauli SL, Ylikomi T, Joensuu T, Tuohimaa P (1991) Location of androgen receptor in human skin. J Invest Dermatol 97(2):264–268
Laine M, Blauer M, Ylikomi T, Tuohimaa P, Aitasalo K, Happonen RP, Tenovuo J (1993) Immunohistochemical demonstration of androgen receptors in human salivary glands. Arch Oral Biol 38(4):299–302
Abu EO, Horner A, Kusec V, Triffitt JT, Compston JE (1997) The localization of androgen receptors in human bone. J Clin Endocrinol Metab 82(10):3493–3497
Mantalaris A, Panoskaltsis N, Sakai Y, Bourne P, Chang C, Messing EM, Wu JH (2001) Localization of androgen receptor expression in human bone marrow. J Pathol 193(3):361–366
Schultheiss D, Badalyan R, Pilatz A, Gabouev AI, Schlote N, Wefer J, von Wasielewski R, Mertsching H, Sohn M, Stief CG, Jonas U (2003) Androgen and estrogen receptors in the human corpus cavernosum penis: immunohistochemical and cell culture results. World J Urol 21(5):320–324
Sinha-Hikim I, Taylor WE, Gonzalez-Cadavid NF, Zheng W, Bhasin S (2004) Androgen receptor in human skeletal muscle and cultured muscle satellite cells: up-regulation by androgen treatment. J Clin Endocrinol Metab 89(10):5245–5255
Godoy A, Watts A, Sotomayor P, Montecinos VP, Huss WJ, Onate SA, Smith GJ (2008) Androgen receptor is causally involved in the homeostasis of the human prostate endothelial cell. Endocrinology 149(6):2959–2969. doi:10.1210/en.2007-1078
Godoy AS, Chung I, Montecinos VP, Buttyan R, Johnson CS, Smith GJ (2013) Role of androgen and vitamin D receptors in endothelial cells from benign and malignant human prostate. Am J Physiol Endocrinol Metab 304(11):E1131–E1139. doi:10.1152/ajpendo.00602.2012
Torres-Estay V, Carreno DV, San Francisco IF, Sotomayor P, Godoy AS, Smith GJ (2015) Androgen receptor in human endothelial cells. J Endocrinol 224(3):R131–R137. doi:10.1530/JOE-14-0611
Yoshida S, Ikeda Y, Aihara K (2016) Roles of the androgen–androgen receptor system in vascular angiogenesis. J Atheroscler Thromb 23(3):257–265. doi:10.5551/jat.31047
Buttyan R, Shabsigh A, Perlman H, Colombel M (1999) Regulation of apoptosis in the prostate gland by androgenic steroids. Trends Endocrinol Metab 10(2):47–54
Cheng L, Zhang S, Sweeney CJ, Kao C, Gardner TA, Eble JN (2004) Androgen withdrawal inhibits tumor growth and is associated with decrease in angiogenesis and VEGF expression in androgen-independent CWR22Rv1 human prostate cancer model. Anticancer Res 24(4):2135–2140
Godoy A, Montecinos VP, Gray DR, Sotomayor P, Yau JM, Vethanayagam RR, Singh S, Mohler JL, Smith GJ (2011) Androgen deprivation induces rapid involution and recovery of human prostate vasculature. Am J Physiol Endocrinol Metab 300(2):E263–E275. doi:10.1152/ajpendo.00210.2010
Hougaku H, Fleg JL, Najjar SS, Lakatta EG, Harman SM, Blackman MR, Metter EJ (2006) Relationship between androgenic hormones and arterial stiffness, based on longitudinal hormone measurements. Am J Physiol Endocrinol Metab 290(2):E234–E242
Alexandersen P, Haarbo J, Byrjalsen I, Lawaetz H, Christiansen C (1999) Natural androgens inhibit male atherosclerosis: a study in castrated, cholesterol-fed rabbits. Circ Res 84(7):813–819
Dockery F, Bulpitt CJ, Donaldson M, Fernandez S, Rajkumar C (2003) The relationship between androgens and arterial stiffness in older men. J Am Geriatr Soc 51(11):1627–1632
Malkin CJ, Pugh PJ, Jones RD, Jones TH, Channer KS (2003) Testosterone as a protective factor against atherosclerosis–immunomodulation and influence upon plaque development and stability. J Endocrinol 178(3):373–380
Kang SM, Jang Y, Kim JY, Chung N, Cho SY, Chae JS, Lee JH (2002) Effect of oral administration of testosterone on brachial arterial vasoreactivity in men with coronary artery disease. Am J Cardiol 89(7):862–864
Kalin MF, Zumoff B (1990) Sex hormones and coronary disease: a review of the clinical studies. Steroids 55(8):330–352
Montalcini T, Gorgone G, Gazzaruso C, Sesti G, Perticone F, Pujia A (2007) Endogenous testosterone and endothelial function in postmenopausal women. Coron Artery Dis 18(1):9–13
Oesterling JE (1994) Endocrine therapies for symptomatic benign prostatic hyperplasia. Urology 43(2 Suppl):7–16
Alonzi R, Padhani AR, Taylor NJ, Collins DJ, D’Arcy JA, Stirling JJ, Saunders MI, Hoskin PJ (2011) Antivascular effects of neoadjuvant androgen deprivation for prostate cancer: an in vivo human study using susceptibility and relaxivity dynamic MRI. Int J Radiat Oncol Biol Phys 80(3):721–727
Kravchick S, Cytron S, Mamonov A, Peled R, Linov L (2009) Effect of short-term dutasteride therapy on prostate vascularity in patients with benign prostatic hyperplasia: a pilot study. Urology 73(6):1274–1278
Godoy A, Montecinos VP, Gray DR, Sotomayor P, Yau JM, Vethanayagam RR, Singh S, Mohler JL, Smith GJ (2011) Androgen deprivation induces rapid involution and recovery of human prostate vasculature. Am J Physiol Endocrinol Metab 300(2):E263–E275
Jaffe EA, Nachman RL, Becker CG, Minick CR (1973) Culture of human endothelial cells derived from umbilical veins. Identification by morphologic and immunologic criteria. J Clin Invest 52(11):2745–2756. doi:10.1172/JCI107470
Nachman RL, Jaffe EA (2004) Endothelial cell culture: beginnings of modern vascular biology. J Clin Invest 114(8):1037–1040. doi:10.1172/JCI23284
Sotomayor P, Godoy A, Smith GJ, Huss WJ (2009) Oct4A is expressed by a subpopulation of prostate neuroendocrine cells. Prostate 69(4):401–410
Cano P, Godoy A, Escamilla R, Dhir R, Onate SA (2007) Stromal–epithelial cell interactions and androgen receptor-coregulator recruitment is altered in the tissue microenvironment of prostate cancer. Cancer Res 67(2):511–519
Shafi AA, Putluri V, Arnold JM, Tsouko E, Maity S, Roberts JM, Coarfa C, Frigo DE, Putluri N, Sreekumar A, Weigel NL (2015) Differential regulation of metabolic pathways by androgen receptor (AR) and its constitutively active splice variant, AR-V7, in prostate cancer cells. Oncotarget 6(31):31997–32012. doi:10.18632/oncotarget.5585
von der Ahe D, Janich S, Scheidereit C, Renkawitz R, Schutz G, Beato M (1985) Glucocorticoid and progesterone receptors bind to the same sites in two hormonally regulated promoters. Nature 313(6004):706–709
Hsing AW, Reichardt JK, Stanczyk FZ (2002) Hormones and prostate cancer: current perspectives and future directions. Prostate 52(3):213–235
Bishop-Bailey D, Walsh DT, Warner TD (2004) Expression and activation of the farnesoid X receptor in the vasculature. Proc Natl Acad Sci USA 101(10):3668–3673
He F, Li J, Mu Y, Kuruba R, Ma Z, Wilson A, Alber S, Jiang Y, Stevens T, Watkins S, Pitt B, Xie W, Li S (2006) Downregulation of endothelin-1 by farnesoid X receptor in vascular endothelial cells. Circ Res 98(2):192–199
Wang S, Lai K, Moy FJ, Bhat A, Hartman HB, Evans MJ (2006) The nuclear hormone receptor farnesoid X receptor (FXR) is activated by androsterone. Endocrinology 147(9):4025–4033. doi:10.1210/en.2005-1485
Huber RM, Murphy K, Miao B, Link JR, Cunningham MR, Rupar MJ, Gunyuzlu PL, Haws TF, Kassam A, Powell F, Hollis GF, Young PR, Mukherjee R, Burn TC (2002) Generation of multiple farnesoid-X-receptor isoforms through the use of alternative promoters. Gene 290(1–2):35–43
Lobo RA, Speroff L (1994) International consensus conference on postmenopausal hormone therapy and the cardiovascular system. Fertil Steril 61(4):592–595
Milewich L, Kaimal V, Johnson AR (1987) Steroid 5 alpha-reductase activity in endothelial cells from human umbilical cord vessels. J Steroid Biochem 26(5):561–567
Mukherjee TK, Dinh H, Chaudhuri G, Nathan L (2002) Testosterone attenuates expression of vascular cell adhesion molecule-1 by conversion to estradiol by aromatase in endothelial cells: implications in atherosclerosis. Proc Natl Acad Sci USA 99(6):4055–4060
Feldman BJ, Feldman D (2001) The development of androgen-independent prostate cancer. Nat Rev Cancer 1(1):34–45
Tan J, Sharief Y, Hamil KG, Gregory CW, Zang DY, Sar M, Gumerlock PH, deVere White RW, Pretlow TG, Harris SE, Wilson EM, Mohler JL, French FS (1997) Dehydroepiandrosterone activates mutant androgen receptors expressed in the androgen-dependent human prostate cancer xenograft CWR22 and LNCaP cells. Mol Endocrinol 11(4):450–459
Sieveking DP, Lim P, Chow RW, Dunn LL, Bao S, McGrath KC, Heather AK, Handelsman DJ, Celermajer DS, Ng MK (2010) A sex-specific role for androgens in angiogenesis. J Exp Med 207(2):345–352
Antonarakis ES, Luo J (2015) Prostate cancer: AR splice variant dimerization—clinical implications. Nat Rev Urol 12(8):431–433. doi:10.1038/nrurol.2015.184
Leibrand CR, Price DK, Figg WD (2016) Androgen receptor splice variant 7 (AR-V7) and drug efficacy in castration-resistant prostate cancer: biomarker for treatment selection exclusion or inclusion? Cancer Biol Ther. doi:10.1080/15384047.2016.1156274
Yoshida S, Aihara K, Ikeda Y, Sumitomo-Ueda Y, Uemoto R, Ishikawa K, Ise T, Yagi S, Iwase T, Mouri Y, Sakari M, Matsumoto T, Takeyama K, Akaike M, Matsumoto M, Sata M, Walsh K, Kato S (2013) Androgen receptor promotes sex-independent angiogenesis in response to ischemia and is required for activation of vascular endothelial growth factor receptor signaling. Circulation 128(1):60–71. doi:10.1161/CIRCULATIONAHA.113.001533
Montecinos VP, Godoy A, Hinklin J, Vethanayagam RR, Smith GJ (2012) Primary xenografts of human prostate tissue as a model to study angiogenesis induced by reactive stroma. PLoS One 7(1):e29623. doi:10.1371/journal.pone.0029623
Montecinos VP, Morales CH, Fischer TH, Burns S, San Francisco IF, Godoy AS, Smith GJ (2015) Selective targeting of bioengineered platelets to prostate cancer vasculature: new paradigm for therapeutic modalities. J Cell Mol Med 19(7):1530–1537. doi:10.1111/jcmm.12515
Tanner MJ, Welliver RC Jr, Chen M, Shtutman M, Godoy A, Smith G, Mian BM, Buttyan R (2011) Effects of androgen receptor and androgen on gene expression in prostate stromal fibroblasts and paracrine signaling to prostate cancer cells. PLoS One 6(1):e16027. doi:10.1371/journal.pone.0016027
Balk SP, Knudsen KE (2008) AR, the cell cycle, and prostate cancer. Nucl Recept Signal 6:e001
Cai J, Hong Y, Weng C, Tan C, Imperato-McGinley J, Zhu YS (2011) Androgen stimulates endothelial cell proliferation via an androgen receptor/VEGF/cyclin A-mediated mechanism. Am J Physiol Heart Circ Physiol 300(4):H1210–H1221. doi:10.1152/ajpheart.01210.2010
Das A, Yaqoob U, Mehta D, Shah VH (2009) FXR promotes endothelial cell motility through coordinated regulation of FAK and MMP-9. Arterioscler Thromb Vasc Biol 29(4):562–570
Acknowledgments
This study was supported by the Department of Defense W81XWH-12-1-0341 and FONDECYT Regular (1130051 and 1161115) Grants to A. Godoy and FONDECYT Iniciación (11140255) to P. Sotomayor. V. Torres-Estay was supported by a Ph.D. fellowship from CONICYT. The authors thank Dr. Yusser Olguín from Universidad Andres Bello for the graphic design support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest.
Additional information
Gary J. Smith and Alejandro S. Godoy have contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
10456_2016_9525_MOESM1_ESM.tif
Supplementary Figure 1. Cellular distribution of AR in mHUVECs. mHUVECs were stimulated for 24 h to vehicle (ethanol) or 1 nM dihydrotestosterone (DHT). Nuclear (N) and cytoplasmic (C) cellular extracts were prepared using the NE-PER kit (ThermoFisher Scientific). Membranes and nuclei were probed using antibodies against AR. Histone H3 (nuclear) and β-tubulin (cytoplasmic) were used as loading controls (TIFF 5416 kb)
10456_2016_9525_MOESM2_ESM.tif
Supplementary Fig. 2. FXR expression in mHUVECs. (A) RT-PCR analysis of expression of FXR in HUVECs obtained from 4 different donors and derived from female (lanes 1 and 2) and male (lanes 3 and 4) fetuses. HepG2 cells were used as positive control (lane 5). GAPDH was used as loading control. (B) RT-PCR analysis of expression of FXR directed against four different regions of the FXR gene in HUVECs exposed to vehicle (lanes 1) or 1 nM DHT (lanes 2). HepG2 cells were used as positive control (lanes 3). GAPDH was used as loading control (TIFF 6509 kb)
Rights and permissions
About this article
Cite this article
Torres-Estay, V., Carreño, D.V., Fuenzalida, P. et al. Androgens modulate male-derived endothelial cell homeostasis using androgen receptor-dependent and receptor-independent mechanisms. Angiogenesis 20, 25–38 (2017). https://doi.org/10.1007/s10456-016-9525-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10456-016-9525-6