Abstract
Formation of lymphatic capillaries by lymphatic endothelial cells (LECs) occurs both in normal tissues as well as in pathological processes including tumor metastasis. Interleukin-6 (IL-6), a potent pro-inflammatory cytokine, has been shown to be highly elevated in various cancers. IL-6 has also been shown to increase tumor lymphangiogenesis through vascular endothelial growth factor-C (VEGF-C) induction in tumor cells. Although lymphangiogenesis is associated with lymph node metastasis and also resistance to conventional therapy in various cancers, the precise mechanisms of lymphangiogenesis in LECs remain unclear. This study aimed to investigate the signaling cascade involved in IL-6-induced VEGF-C expression in murine LECs (SV-LEC). The VEGF-C mRNA and protein levels were increased in SV-LECs exposed to IL-6. IL-6 time-dependently induced Src phosphorylation and downstream phosphorylation of ERK1/2 and p38MAPK. In contrast, PP2, an inhibitor of Src signaling, abrogated IL-6′s effects on ERK1/2 and p38MAPK phosphorylation. IL-6 exposure also led to increase in VEGF-C promoter-luciferase activity as well as C/EBPβ- and κB-luciferase activities. VEGF-C promoter-, C/EBPβ- and κB-luciferase activities were all suppressed by Src, ERK1/2 or p38MAPK signaling blockades despite presence of IL-6. Finally, C/EBPβ and p65 binding to the VEGF-C promoter region were increased after IL-6 exposure in SV-LECs. Taken together, we report a Src-mediated ERK1/2 and p38MAPK activation resulting in C/EBPβ and p65 binding to the promoter region of VEGF-C, leading to VEGF-C expression in IL-6-exposed SV-LECs.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cancer is an increasingly prevalent health problem and remains a major cause of mortality around the world [1]. The metastatic spread of tumor cells is associated with resistance to conventional therapy and is the leading cause of death for cancer patients. Tumor cells produce a range of growth factors and/or cytokines that promote tumor metastasis by directly or indirectly stimulating angiogenesis and lymphangiogenesis, which is one of the major routes for tumor invasion and metastasis [2, 3]. Inhibiting tumor-induced lymphangiogenesis has been shown to markedly suppress the spread of cancer in animal models [4, 5]. Therefore, the identification of mechanisms underlying tumor lymphangiogenesis is essential for developing new therapeutic strategies in the treatment of cancer.
Chronic inflammation plays a crucial role in human carcinogenesis. Many lines of evidence demonstrated that elevated serum interleukin-6 (IL-6) levels is correlated with poor clinical prognosis in many cancers including lymphoma, head and neck cancer and prostate cancers [6–9]. IL-6 not only plays a central role in cancer-associated inflammation [10], it has also been implicated in the regulation of tumor growth [11–14]. IL-6 exerts its biological activities through IL-6 receptor (IL-6R) and gp130 [15]. When IL-6 binds to mIL-6R, the membrane-bound form of IL-6R, gp130 homodimerizes and forms a functional receptor complex with IL-6 and IL-6R. On the other hand, IL-6 can also bind to the soluble form of IL-6R (sIL-6R) to form an IL-6/sIL-6R complex and act as agonist for cells that express gp130 [16]. The receptor complex formed by IL-6 triggers two main signaling pathways. First is the janus kinases (JAKs)/signal transducer and activator of transcription 3 (STAT3) pathway. In this pathway, active STAT3 translocates to the nucleus and binds to promoter region of target genes, thereby activating transcription. IL-6 can also activate the Ras/extracellular-signal-regulated kinase (ERK) pathway, which activates transcription factors such as NF-IL-6 (CCAAT/enhancer-bindingg protein β, C/EBPβ) [17]. These pathways independently transduce the signal from IL-6 leading to its various biological activities.
Similar to angiogenesis, lymphangiogenesis relies on the regulation of several lymphoangiogenic factors and receptors [18]. Vascular endothelial growth factor-C (VEGF-C) is currently the best-characterized lymphangiogenic factor that acts via VEGF receptor-3 (VEGFR-3). In normal adult tissues, VEGFR-3 expression is largely restricted to the LECs, and its activation is responsible for LEC proliferation, migration, and survival [19, 20]. Tumor cell-derived VEGF-C plays a causal role in lymphangiogenesis and lymphatic metastasis [21–23]. In addition, many studies have also demonstrated that VEGF-C is induced in several types of immune cells and lymphatic capillaries have been shown to proliferate during inflammation [24–26]. IL-6, a typical inflammatory cytokine with various effects on immune cells [27], was recently reported to regulate VEGF-C expression and metastasis in several types of cancer cells, such as oral squamous cell carcinoma [28]. However, little is known about VEGF-C regulation in LECs exposed to IL-6. This study aimed to investigate whether IL-6 regulates VEGF-C expression in LECs. The limitations of studies on lymphangiogenesis and signaling pathways in LECs are the difficulties in the isolation and propagation of LECs from different organs [19, 29, 30]. To overcome these limitations, we selected a “conditionally immortalized” line of murine LECs (SV-LECs) that express SV40 large T and retain their ‘lymphatic’ endothelial characteristics after repeated passages [31, 32]. In this study, we demonstrated that IL-6 activates Src-mediated ERK and p38MAPK signaling cascade, resulting in C/EBPβ and p65 binding to the promoter region of VEGF-C and subsequent VEGF-C expression in SV-LECs.
Materials and methods
Reagents
DMEM, fetal bovine serum (FBS), penicillin, and streptomycin were purchased from Invitrogen (Carlsbad, CA, USA). Normal IgG, rabbit polyclonal antibodies specific for p65 and CEBP/β, and antibodies against FAK phosphorylated at Tyr397 were purchased from Santa Cruz Biotechnology (Santa Cruz, CA, USA). Antibodies against Src phosphorylated at Tyr216, antibodies against ERK1/2 phosphorylated at Thr202/Tyr204, and antibodies against STAT3 phosphorylated at Tyr705 were purchased from Cell Signaling (Beverly, MA, USA). Antibodies against p38MAPK phosphorylated at Thr180/Tyr182, anti-mouse and anti-rabbit IgG conjugated horseradish peroxidase antibodies, and anti-c-Src, anti-p38MAPK, anti-VEGF-C, and anti-α-tubulin antibodies were obtained from GeneTex Inc (Irvine, CA, USA). Recombinant IL-6 and soluble IL6Rα (sIL6R) were purchased from PeproTech (Rocky Hill, NJ, USA). PP2, p38MAPK kinase inhibitor III and ERK activation inhibitor peptide I were bought from Calbiochem (San Diego, CA, USA). Turbofect™ in vitro transfection reagent was purchased from Upstate Biotechnology (Lake Placid, NY, USA). C/EBP reporter construct, p/T81 C/EBP-luc, was kindly provided by Dr. Kjetil Tasken (University of Oslo, Oslo, Norway). κB-Luc, Renilla-luc and Dual-Glo luciferase assay systems were purchased from Promega (Madison, WI, USA). All materials for immunoblotting were purchased from GE Healthcare (Little Chalfont, UK). All other chemicals were obtained from Sigma (St. Louis, MO, USA).
Cell culture
The mouse LEC line SV-LEC was kindly provided by Dr. J.S. Alexander (Shreveport, LA, USA), and was cultured as previously described [31].
Immunoblot analysis
Immunoblot analyses were performed as described previously [33]. Briefly, cells were lysed in an extraction buffer containing 10 mM Tris (pH 7.0), 140 mM NaCl, 2 mM PMSF, 5 mM DTT, 0.5 % NP-40, 0.05 mM pepstatin A, and 0.2 mM leupeptin. Samples of equal amounts of protein were subjected to SDS-PAGE and transferred onto a NC membrane which was then incubated in a TBST buffer containing 5 % non-fat milk. Proteins were visualized by incubating with specific primary antibodies followed by horse radish peroxidase-conjugated secondary antibodies. Immunoreactivity was detected using enhanced chemiluminescence following the manufacturer’s instructions. Quantitative data was obtained using a computing densitometer with Image-Pro Plus image analysis software system (Kodak, Rochester, NY, USA).
Transfection in SV-LECs and dual luciferase reporter assay
SV-LECs (105 cells per well) were transfected with pGL4-VEGF-C-luc-370 (1 μg), κB-luc (1 μg), or CEBP/β-luc (1 μg) plus renilla-luc (0.25 μg) using Turbofect reagent (Upstate Biotechnology, Lake Placid, NY, USA) for 48 h. After transfection, cells with or without treatments were harvested. The luciferase activity was then determined using a Dual-Glo luciferase assay system kit (Promega) according to manufacturer’s instructions, and was normalized on the basis of renilla luciferase activity.
Reverse-transcription polymerase chain reaction (RT-PCR)
Total RNA was isolated from cells using the RNAspin RNA isolation kit (GE Healthcare, Little Chalfont, UK). The RT-PCR was then conducted following the manufacturer’s instructions (Super Script One-Step RT-PCR system, Invitrogen). Primers used for amplification of the VEGF-C and GAPDH fragments were as follows: mouse VEGF-C, sense 5′-AGCCAACAGGGAATTTGATG-3′ and antisense 5′-CACAGCGGCATACTTCTTCA-3′; mouse GAPDH, sense 5′-CCTTCATTGACCTCAACTAC-3′ and antisense 5′-GGAAGGCCATGCCAGTGAGC-3′; and GAPDH was used as the internal control. The PCR was performed with the following conditions: 30 cycles of a 30-s denaturation step at 94 °C, a 30-s annealing step at 56 °C, and a 45-s extension step at 72 °C to amplify survivin and GAPDH cDNA. The amplified fragment sizes for mouse VEGF-C and mouse GAPDH were 239 and 594 bp, respectively. PCR products were run on an agarose gel, stained with ethidium bromide, and visualized by ultraviolet illumination.
Chromatin immunoprecipitation (ChIP) assay
A ChIP assay was performed as described previously [33]. Briefly, cells were cross-linked with 1 % formaldehyde at 37 °C for 10 min and rinsed with ice-cold PBS. Cells were then harvested in SDS lysis buffer, sonicated five times for 15 s each, and centrifuged for 10 min. Supernatants were collected and diluted in ChIP dilution buffer, followed by immunoclearing with gentle rotation with 80 μl protein A-agarose slurry for 1 h at 4 °C. An aliquot of each sample was used as “input” in the PCR analysis. The remainder of the soluble chromatin was incubated at 4 °C overnight with either p65 and CEBP/β antibodies (Santa Cruz Biotechnology), or control IgG (Santa Cruz Biotechnology). Immune complexes were collected by incubation with a 60 μl protein A-agarose slurry for 2 h at 4 °C with a gentle rotation. The complexes were washed sequentially for 5 min in the following three washing buffers: a low salt immune complex washing buffer, a high-salt immune complex washing buffer, and a LiCl immune complex washing buffer. Precipitates were washed two times with Tris–EDTA buffer. The complexes were, then, eluted twice with two 100 μl aliquots of elution buffer. The cross-linked chromatin complex was reversed in the presence of 0.2 M NaCl and heating at 65 °C for 4 h. DNA was purified using GFXTM DNA purification spin columns (GE Healthcare). PCR was performed using PCR Master Mix (Promega, Madison, WI) according to the manufacturer’s protocol. Ten percent of the total purified DNA was used for the PCR in 50 μl reaction mixture. The 170-bp VEGF-C promoter fragment between −198 and −367 (contains putative C/EBP binding sites) was amplified using the primer pair, sense: 5′-cgg gac gag tgg aac atc-3′ and antisense: 5′-agg tac gag cct cac agg aa-3′, in 30 cycles of PCR. The 103-bp VEGF-C promoter fragment between −164 and −62 (contains putative NF-κB binding sites) was amplified using the primer pair, sense: 5′-aga gcc gag ggc aaa agt-3′ and antisense: 5′-gct gag gtc ctc tcc tgg tc-3′, in 30 cycles of PCR. This was done at 95 °C for 30 s, 56 °C for 30 s, and finally 72 °C for 45 s. The PCR products were analyzed by 1.5 % agarose gel electrophoresis
Preparation of VEGF-C promoter-luciferase reporter construct
Mouse genomic DNA from SV-LECs was isolated using the Wizard® Genomic DNA Purification Kit (Promega, Madison, WI, USA) following the manufacturer’s instructions. VEGF-C promoter sequences (−370 to +1) was then amplified from mouse genomic DNA by PCR, using the following primers containing KpnI and BglII restriction sites: forward: 5′-ggtacctcttcgggacgagtggaacat-3′; reverse: 5′-agatcttgtggatggaccgggagca gg-3′. To construct the VEGF-C-luc, the amplified PCR products were digested and ligated into PGL4 vector, which encodes firefly luciferase. The fidelity of the insert was confirmed by DNA sequence analysis. The construct was designed as VEGF-C promoter reporter (pGL4-VEGF-C promoter-luc-370).
Statistical analysis
Results are presented as the mean ± SE from at least three independent experiments. One-way analysis of variance (ANOVA) was followed by the Newman-Keuls test, when appropriate, to determine the statistical significance of the difference between means. A p value of <0.05 was considered statistically significant.
Results
IL-6 induced VEGF-C expression in SV-LECs
It has previously been demonstrated that in addition to extending the half-life of serum IL-6, sIL-6R may form a multimeric signaling complex with IL-6 to activate downstream signal transduction pathways [34–36]. We therefore examined the VEGF-C levels in SV-LECs exposed to IL-6 or IL-6 plus sIL-6R (IL-6/sIL-6R). As shown in Fig. 1a, 24 h treatment with IL-6 (20 ng/ml) significantly increased VEGF-C protein levels by 1.7 ± 0.3-folds (n = 6). IL-6 (20 ng/ml) plus sIL-6R (20 ng/ml) further increased the protein levels of VEGF-C by 3.4 ± 0.7-fold (Fig. 1a). We then determined whether the elevation of VEGF-C protein levels was attributable to an increase in vegf-c mRNA. As shown in Fig. 1b, IL-6 led to elevation of vegf-c mRNA levels. The increase in vegf-c mRNA level was more pronounced when SV-LECs were exposed to both IL-6 and sIL6R. These findings suggest that transcriptional upregulation of vegf-c contributes to IL-6- and IL6/sIL6R-induced VEGF-C expression. In the following experiments, we explored the signaling cascades involved in VEGF-C induction in SV-LECs exposed to IL6/sIL-6R.
IL-6 induces VEGF-C expression in SV-LECs. a Cells were treated with vehicle, IL-6 (20 ng/ml) or IL-6 plus sIL6R (20 ng/ml) for 24 h. After treatment, cells were harvested for assessing the extent of VEGF-C by immunoblotting. Each column represents the mean ± SEM of six independent experiments. *p < 0.05, compared with the control group. b Cells were treated with vehicle, IL-6 (20 ng/ml) or IL-6 plus sIL6-R (20 ng/ml) for 6 h. After treatment, the extent of vegf-c mRNA was analyzed by RT-PCR as described in the “Materials and methods” section. Each column represents the mean ± SEM of five independent experiments. *p < 0.05, compared with the vehicle-treated group. IL-6/sIL-6R: IL-6 plus sIL-6R
IL-6/sIL-6R induced Src, ERK1/2, p38MAPK, STAT3 and FAK phosphorylation in SV-LECs
We next explored the IL-6/sIL-6R-activated signaling pathways in SV-LECs. Src tyrosine kinase, a promising therapeutic cancer target, plays a critical role in cell migration, proliferation, survival, and angiogenesis [37]. Several lines of evidence also indicated that Src signaling is involved in VEGF-C expression in tumor cells [38, 39]. We thus determined whether IL-6/sIL-6R induces Src activation in SV-LECs. IL-6/sIL-6R treatment led to a significant increase in Src phosphorylation in a time-dependent manner (Fig. 2a). The increase in Src phosphorylation was observed to begin at 10 min and then peaked at 30–60 min after treatment. We next determined whether the phosphorylation status of ERK1/2 and p38MAPK are altered in SV-LECs exposed to IL-6/sIL-6R. IL-6/sIL-6R time-dependently induced ERK1/2 (Fig. 2b) and p38MAPK (Fig. 2c) phosphorylation within 120 min of exposure. Since Src can activate STAT3 [40] and FAK [41], we also examined whether STAT3 and/or FAK is activated in IL-6/sIL-6R-stimulated SV-LECs. IL-6/sIL-6R treatment led to an increase in phosphorylation of STAT3, the main downstream molecule of IL-6R-signaling (Fig. 2d). IL-6/sIL-6R also time-dependently induced FAK phosphorylation in SV-LECs (Fig. 2e).
IL-6 induced Src, ERK1/2, p38MAPK, STAT3, and FAK phosphorylation in SV-LECs. Cells were treated with IL-6 plus sIL6R for different time periods as indicated. The phosphorylation status of Src (a), ERK1/2 (b), p38MAPK (c), STAT3 (d) and FAK (e) were then determined by immunoblotting. Each column represents the mean ± SEM of at least four independent experiments. *p < 0.05, compared with the control group
IL-6/sIL-6R induced CCAAT/enhancer-binding protein (C/EBP) and NF-κB activation in SV-LECs
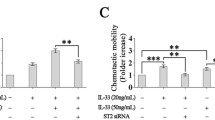
It is conceivable that IL-6/sIL-6R may activate transcription factors, leading to VEGF-C expression in SV-LECs. TFSEARCH analysis (Yutaka Akiyama: “TFSEARCH: Searching Transcription Factor Binding Sites”; http://www.rwcp.or.jp/papia/) [42] indicated that the promoter region between −370 and +1 of the mouse vegf-c gene contains many potential consensus sequences, including those for CCAAT/enhancer-binding protein (C/EBP) and NF-κB. To examine the promoter activity of the 370-bp 5′-flanking sequence of the vegf-c gene, we constructed a VEGF-C promoter reporter plasmid containing the 370 bp promoter region (−370 to +1) of VEGF-C. Treatment of SV-LECs with IL-6 or IL-6/sIL6R for 24 h significantly caused an increase in VEGF-C promoter luciferase activity as determined by reporter assay (Fig. 3A). We also used reporter assays to determine whether IL-6/sIL6R activates C/EBPβ and NF-κB in SV-LECs. As shown in Fig. 3B, cells treated with IL-6/sIL6R for 24 h had significant increases in C/EBPβ- and κB-luciferase activities. To explore whether C/EBPβ and NF-κB subunit p65 are recruited to the endogenous VEGF-C promoter region in response to IL-6/sIL6R, chromatin immunoprecipitation (ChIP) experiments on SV-LECs exposed to IL-6/sIL6R were performed. Primers encompassing the VEGF-C promoter region between −367 and −198 (containing putative C/EBPβ binding sites) and between −164 and −62 (containing putative p65 binding sites) were used. Fig. 3C shows that C/EBPβ (Fig. 3Ca) and p65 (Fig. 3Cb) binding to the VEGF-C promoter region (−367/−198 or −164/−62) were increased after IL-6/sIL6R exposure. The VEGF-C promoter region (-367/-198 or −164/−62) was detected in the cross-linked chromatin sample before immunoprecipitation (bottom panels of Fig. 3Ca and Cb, Input, positive control). These results suggest that IL-6/sIL6R induces the recruitment of C/EBPβ and p65 to the promoter region of the endogenous vegf-c gene, and leads to VEGF-C expression in SV-LECs.
IL-6 induced C/EBPβ and p65 activation in SV-LECs. a Cells were transfected with VEGF-C promoter-luc-370 plus renilla-luc for 48 h. After transfection, SV-LECs were treated with vehicle, IL-6 or IL-6 plus sIL6R for another 24 h. The luciferase activity was then determined as described in the “Materials and methods” section. Each column represents the mean ± SEM of four independent experiments. *p < 0.05, compared with the vehicle-treated group. b Cells were transiently transfected for 48 h with C/EBPβ- or κB-luc plus renilla-luc. After transfection, cells were treated with vehicle or IL-6 plus sIL6R for another 24 h. A luciferase assay was then performed. Data represent the mean ± SEM of at least four independent experiments performed in duplicate (*p < 0.05, compared with the vehicle-treated group). c Cells were incubated with IL-6 plus sIL6R for indicated time periods and the ChIP assay was performed as described in the “Materials and methods” section. Typical traces representative of three independent experiments with similar results are shown. Cells were transfected with C/EBPβ- (d), κB-luc (e) or VEGF-C promoter-luc-370 (f) plus renilla-luc for 48 h. After transfection, SV-LECs were pretreated with p38MAPK inhibitor III (p38MAPK-I, 1 or 3 μM) or ERK activation inhibitor peptide I (ERK-I, 1 or 3 μM) for 30 min, followed by the treatment with IL-6/SIL-6R for another 24 h. The luciferase activity was then determined. Each column represents the mean ± SEM of at least four independent experiments. *p < 0.05, compared with the control group; #p < 0.05, compared to the vehicle-treated group in the presence of IL-6/sIL-6R
ERK1/2 and p38MAPK signaling pathways contribute to IL-6/sIL-6R-induced C/EBPβ and NF-κB activation
We next used p38MAPK inhibitor III (a p38MAPK inhibitor) and ERK1/2 activation inhibitor peptide I (an ERK inhibitor) to block the p38MAPK and ERK1/2 signaling pathways to confirm whether p38MAPK or ERK1/2 signaling contributes to IL-6/sIL-6R-increased C/EBPβ-luciferase and κB-luciferase activities. As shown in Fig. 3D, pretreatment of cells with p38MAPK inhibitor III (p38MAPK-I, 1 or 3 μM) or ERK1/2 activation inhibitor peptide I (ERK-I, 1 or 3 μM) suppressed IL-6/sIL-6R-induced C/EBP-luciferase activity in SV-LECs. Similarly, p38MAPK inhibitor III and ERK1/2 activation inhibitor peptide I also attenuated IL-6/sIL-6R-induced κB-luciferase activity (Fig. 3E). The IL-6/sIL-6R-induced VEGF-C promoter luciferase activities were also significantly inhibited in the presence of p38MAPK inhibitor III or ERK1/2 activation inhibitor peptide I (Fig. 3F). Taken together, these results support the causal role of p38MAPK and ERK1/2 in IL-6/sIL-6R-induced C/EBPβ and NFκB activation, and subsequent VEGF-C expression in SV-LECs.
Src mediated IL-6/sIL-6R-induced ERK1/2, p38MAPK, FAK and STAT3 phosphorylation in SV-LECs
Many studies suggested that Src may act as an upstream regulator of MAPKs including ERK1/2 and p38MAPK [43, 44]. Src was also shown to increase FAK phosphorylation and has been identified as a common signaling pathway stimulated by diverse extracellular stimuli including growth factors for receptor tyrosine kinases [45–47]. We thus used PP2 (a Src-family kinases inhibitor) to block the Src signaling pathway to confirm whether Src contributes to IL-6/sIL-6R-induced phosphorylation of ERK1/2, p38MAPK, and FAK in SV-LECs. As shown in Fig. 4, pretreatment of SV-LECs with PP2 (1 μM) significantly reduced IL-6/sIL-6R-induced ERK1/2 (Fig. 4a), p38MAPK (Fig. 4b), and FAK (Fig. 4c) phosphorylation. Similarly, PP2 at 1 μM is effective in suppressing IL-6/sIL-6R-induced STAT3 phosphorylation (Fig. 4d). Based on these results, we suggest that Src activation may occur upstream of ERK1/2, p38MAPK, FAK or STAT3 signaling in IL-6/sIL-6R-stimulated SV-LECs.
Src contributes to IL-6-induced ERK1/2, p38MAPK, STAT3 and FAK phosphorylation in SV-LECs. Cells were pretreated with vehicle or PP2 (0.1 or 1 μM) for 30 min before treatment with IL-6/sIL-6R for another 30 min. After treatment, cells were then harvested and the phosphorylation status of ERK1/2 (a), p38MAPK (b), FAK (c), and STAT3 (d) were determined by immunoblotting. Each column represents the mean ± SEM of six independent experiments. *p < 0.05, compared with the control group; #p < 0.05, compared with the vehicle-treated group in the presence of IL-6/sIL-6R
Src in IL-6/sIL-6R-induced VEGF-C expression in SV-LECs
To ascertain the linkage between Src signaling and VEGF-C expression downstream of IL-6/sIL-6R, the effects of PP2 on IL-6/sIL-6R-induced VEGF-C expression was determined. As shown in Fig. 5A, PP2 significantly inhibited IL-6/sIL-6R-increased VEGF-C protein levels. In addition, IL-6/sIL-6R induced VEGF-C promoter-luciferase (Fig. 5Ba), C/EBPβ-luciferase (Fig. 5Bb) and κB-luciferase (Fig. 5Bc) activities were also suppressed in the presence of PP2 (Fig. 5B). Furthermore, PP2 attenuated the effects of IL-6/sIL-6R on C/EBPβ (Fig. 5Ca) and p65 (Fig. 5Cb) binding to the VEGF-C promoter region. Together, these findings suggest that Src signaling contribute to IL-6/sIL-6R-induced VEGF-C expression in SV-LECs.
Src contributes to C/EBPβ and NF-κB activation and VEGF-C expression in IL-6-stimulated SV-LECs. A Cells were pretreated with vehicle or PP2 (0.1 or 1 μM) for 30 min before treatment with IL-6/sIL-6R for another 24 h. The extent of VEGF-C was then assessed by immunoblotting. Each column represents the mean ± SEM of five independent experiments. *p < 0.05, compared with the control group; #p < 0.05, compared with the vehicle-treated group in the presence of IL-6/sIL-6R. B Cells were transfected with VEGF-C promoter-luc-370 (a), C/EBPβ- (b) or κB-luc (c) plus renilla-luc for 48 h. After transfection, SV-LECs were pretreated with PP2 (1 μM) for 30 min, followed by the treatment with IL-6/SIL-6R for another 24 h. The luciferase activity was then determined. Each column represents the mean ± SEM of at least three independent experiments. *p < 0.05, compared with the control group; #p < 0.05, compared to the vehicle-treated group in the presence of IL-6/sIL-6R. C Cells were treated with vehicle or PP2 (1 μM) for 30 min followed by the treatment with IL-6/sIL-6R for another 4 h. ChIP assay was then performed as described in the “Materials and methods” section. Typical traces representative of at least three independent experiments with similar results are shown
Discussion
Accumulating data indicate that VEGF-C expression in cancer cells correlates with accelerated tumor progression or unfavorable clinical outcome [28, 48, 49]. VEGF-C is thus proposed as a prospective cancer therapeutic target. It is thought that tumor-derived VEGF-C promotes lymphangiogenesis via VEGF-R3 expressed on the surface of LECs, and facilitates metastatic spread of tumor cells via the lymphatic capillaries [3, 50, 51]. Although growing evidence indicates that VEGF-C plays a causal role in lymphangiogenesis and lymphatic metastasis, little is known about VEGF-C regulation in tumor cells or in LECs. Shinriki et al. [28] recently demonstrated that IL-6, which is elevated in cancer patients, induces VEGF-C expression through PI3 K-Akt cascade in oral squamous cell carcinoma. In the present study, we demonstrated that IL-6 induces VEGF-C expression in LECs. The underlying mechanisms by which IL-6 induced VEGF-C expression may involve the activation of Src, ERK1/2 and p38MAPK. In addition, activation of transcription factors, NF-κB and C/EBPβ, may also contribute to IL-6 actions in inducing VEGF-C expression in LECs.
The molecular mechanism involved in VEGF-C expression by IL-6 in LECs remains unclear. IL-6 plays a critical role in regulating diverse physiological and pathological processes by stimulating downstream signaling events, which include JAK/STAT, PI3 K/Akt and Ras/MAPK pathways [17, 52]. MAPK signaling has also been shown to contribute to a variety of cellular functions in physiology and diseases [53]. Activation of MAPKs is thus postulated to be required in the IL-6-induction of VEGF-C in LECs. In agreement with these observations, we noted that ERK1/2 and p38MAPK signaling blockade by specific inhibitors markedly suppressed VEGF-C promoter luciferase activity in IL-6-stimulated SV-LECs. In addition, IL-6-induced ERK1/2 and p38MAPK phosphorylation and VEGF-C promoter luciferase activity were suppressed in the presence of PP2, s Src family kinases inhibitor, suggesting that Src-mediated ERK1/2 and p38MAPK activation may be causally related to IL-6-induced VEGF-C expression in SV-LECs. On the other hand, although the classical activation pathway of STAT3 is via upstream kinases such as JAK2 that links STAT3 signaling to cytokine receptors [54], STAT3 may also be activated by other kinases including c-Src [55, 56]. We noted in this study that c-Src inhibition using PP2 leads to STAT3 inhibition in SV-LECs exposed to IL-6. PP2 also suppressed IL-6-induced FAK phosphorylation. It is likely that activation of Src by IL-6 may also lead to FAK and STAT3 activation in SV-LECs. Further investigations are needed to clarify whether activation of STAT3 and FAK contributes to VEGF-C expression in SV-LECs after IL-6 exposure.
Transcription factor NF-κB is mainly involved in regulating inflammatory and immune responses in response to extracellular stimuli. NF-κB in vasculature also plays a pathogenic role in various diseases marked by inflammation and abnormal proliferation, including atherosclerosis [57] and aneurysm [58]. NF-κB was also shown to participate in angiogenesis, and increased NF-κB activity has been documented in the vasculature of colorectal and lung carcinoma [59, 60]. Upon activation, NF-κB dissociates from its inhibitory protein IκB-α and translocates from cytosol to the nucleus, where it then binds to related DNA elements (NF-κB response element) and activates its target genes [61]. Previous studies have shown that ERK1/2 and p38MAPK regulate NF-κB in activated vascular endothelial cells [62]. However, the role of NF-κB in the regulation of lymphatic-specific genes was unclear. We showed in this study that IL-6 significantly increased NF-κB activity as determined by reporter assay. A reporter assay further showed that C/EBPβ activity was also elicited by IL-6 in SV-LECs. The IL-6-induced increases in VEGF-C promoter-luciferase, κB-luciferase and C/EBPβ-luciferase activities were attenuated in the presence of Src, ERK1/2 and p38MAPK inhibitors. Moreover, the results from ChIP assay indicated that PP2 attenuated the recruitment of NF-κB subunit p65 and C/EBPβ to the endogenous vegf-c promoter region (−164/−62 and −367/−198) in IL-6-stimulated SV-LECs. Taken together, these results suggest that IL-6 might activate Src signaling to cause ERK1/2 and p38MAPK activation, which in turn, induce NF-κB and C/EBPβ activation and ultimately lead to VEGF-C expression in SV-LECs.
As the promoter region (−370 to +1) of the vegf-c gene also contains Sp1 binding sites, activation of Sp1 is likely to be responsible for the increase in VEGF-C expression in SV-LECs exposed to IL-6. This is supported by the observation that IL-6 induced the activation of ERK1/2 and p38MAPK, two critical upstream regulator of Sp1 [63, 64]. Together, these findings raise the possibility that IL-6 activation of ERK1/2 and p38MAPK signaling cascades may regulate at least three transcription factors in SV-LECs: NF-κB, C/EBPβ and Sp1. The precise mechanisms of IL-6 actions in driving these transcription factors remain to be elucidated. It is likely that these signaling cascades could culminate in the expression of VEGF-C in SV-LECs. Furthermore, several reports have demonstrated the physical and functional interactions between C/EBPβ and NF-κB family members [65, 66] or Sp1 [67]. However, whether C/EBPβ cooperates with p65, Sp1 or other transcription factors in the induction of VEGF-C in IL-6-stimulated SV-LECs requires further investigation.
The essential role of lymphangiogenesis in a multitude of biological and pathological functions makes it promising target for drug development in various diseases. It appears that inhibition of lymphangiogenesis may be beneficial in the context of tumor progression by dampening the metastatic spread of tumor cells [68]. As described above, VEGF-C/VEGFR3 signaling promotes tumor lymphangiogenesis and metastasis [21–23]. VEGF-C/VEGFR3 signaling is thus a potential target for preventing tumor lymphatic metastasis. Preclinical studies have reported that inhibition of VEGF-C/VEGFR3 signaling using soluble VEGFR3 receptors and anti-VEGFR3 antibodies suppressed lymphatic metastasis [69, 70]. Tumor- and LECs-derived VEGF-C is another potential therapeutic target. We demonstrated in this study that Src plays a causal role in IL-6 activation of the ERK/p38MAPK-C/EBPβ and/or NF-κB signaling cascade, leading to VEGF-C expression in SV-LECs. These findings shed light, at least in part, on the mechanisms underlying IL-6-induced VEGF-C expression in LECs. Src signaling has also been shown to contribute to VEGF-C-induced invasion and metastasis in tumor cells [71]. Ischenko et al. demonstrated that inhibition of Src kinase exhibits inhibitory effects on VEGF-C-induced lymphangiogenesis in vitro and in vivo [72]. In agreement with the observations that VEGF-C induction is Src-dependent in tumor cells [38, 39, 72], we showed in this study that Src inhibition also attenuated VEGF-C expression in IL-6-stimulated LECs. In addition, Src plays a crucial role in endothelial cell invasion, migration and tumor angiogenesis [73]. Extrapolating these findings to the clinical scenario, targeting IL-6 and/or its downstream pathways such as Src signaling may prevent LECs-derived VEGF-C activity and tumor lymphatic metastasis. For instance, a humanized anti-IL-6R antibody, tocilizumab, which has been shown to be effective for rheumatoid arthritis [74], was recently reported to reduce IL-6-induced VEGF-C expression, resulting in decrease in oral squamous cell carcinoma-related lymphangiogenesis and metastasis in a mouse model [28]. There is a wealth of literature supporting the role of Src in tumor progression, and currently there are different classes of Src inhibitors such as AZD0530 undergoing clinical trials (http://clinicaltrials.gov). AZM475271, another Src inhibitor, has also been shown to attenuate tumor angiogenesis and lymphangiogenesis [72, 73]. Taken together, these observations suggest that the therapeutic spectrum of these types of drugs such as anti-IL-6/anti-IL-6R-targeted therapies (Ex. Tocilizumab for Rheumatoid Arthritis) and Src inhibitors (Ex. AZD0530, AZM475271 for solid tumors) may be extended to tumor lymphangiogenesis and metastasis prevention. However, further preclinical studies are needed to evaluate the long-term effects of Src inhibitors, or other anti-IL-6/anti-IL-6R-targeted therapies in carcinogenesis settings and other models of lymphatic metastasis. It may also be worthwhile to explore the signaling pathway underlying IL-6-induced VEGF-C expression and lymphangiogenesis for other potential targets for cancer therapy.
References
Chiang AC, Massague J (2008) Molecular basis of metastasis. N Engl J Med 359(26):2814–2823
Achen MG, Stacker SA (2008) Molecular control of lymphatic metastasis. Ann N Y Acad Sci 1131:225–234
Alitalo K, Tammela T, Petrova TV (2005) Lymphangiogenesis in development and human disease. Nature 438(7070):946–953
Caunt M, Mak J, Liang WC, Stawicki S, Pan Q, Tong RK, Kowalski J, Ho C, Reslan HB, Ross J, Berry L, Kasman I, Zlot C, Cheng Z, Le Couter J, Filvaroff EH, Plowman G, Peale F, French D, Carano R, Koch AW, Wu Y, Watts RJ, Tessier-Lavigne M, Bagri A (2008) Blocking neuropilin-2 function inhibits tumor cell metastasis. Cancer Cell 13(4):331–342
Mumprecht V, Detmar M (2009) Lymphangiogenesis and cancer metastasis. J Cell Mol Med 13(8A):1405–1416
Szczepanik AM, Scislo L, Scully T, Walewska E, Siedlar M, Kolodziejczyk P, Lenart M, Rutkowska M, Galas A, Czupryna A, Kulig J (2011) IL-6 serum levels predict postoperative morbidity in gastric cancer patients. Gastric Cancer 14(3):266–273
Kallio JP, Tammela TL, Marttinen AT, Kellokumpu-Lehtinen PL (2001) Soluble immunological parameters and early prognosis of renal cell cancer patients. J Exp Clin Cancer Res 20(4):523–528
Trikha M, Corringham R, Klein B, Rossi JF (2003) Targeted anti-interleukin-6 monoclonal antibody therapy for cancer: a review of the rationale and clinical evidence. Clin Cancer Res 9(13):4653–4665
Hong DS, Angelo LS, Kurzrock R (2007) Interleukin-6 and its receptor in cancer: implications for translational therapeutics. Cancer 110(9):1911–1928
Mantovani A, Allavena P, Sica A, Balkwill F (2008) Cancer-related inflammation. Nature 454(7203):436–444
Ara T, Song L, Shimada H, Keshelava N, Russell HV, Metelitsa LS, Groshen SG, Seeger RC, DeClerck YA (2009) Interleukin-6 in the bone marrow microenvironment promotes the growth and survival of neuroblastoma cells. Cancer Res 69(1):329–337
Duffy SA, Taylor JM, Terrell JE, Islam M, Li Y, Fowler KE, Wolf GT, Teknos TN (2008) Interleukin-6 predicts recurrence and survival among head and neck cancer patients. Cancer 113(4):750–757
Lee YJ, Heo JS, Suh HN, Lee MY, Han HJ (2007) Interleukin-6 stimulates alpha-MG uptake in renal proximal tubule cells: involvement of STAT3, PI3 K/Akt, MAPKs, and NF-kappaB. Am J Physiol Renal Physiol 293(4):F1036–F1046
Smith PC, Hobisch A, Lin DL, Culig Z, Keller ET (2001) Interleukin-6 and prostate cancer progression. Cytokine Growth Factor Rev 12(1):33–40
Hibi M, Murakami M, Saito M, Hirano T, Taga T, Kishimoto T (1990) Molecular cloning and expression of an IL-6 signal transducer, gp130. Cell 63(6):1149–1157
Jones SA, Horiuchi S, Topley N, Yamamoto N, Fuller GM (2001) The soluble interleukin 6 receptor: mechanisms of production and implications in disease. Faseb J 15(1):43–58
Hirano T, Nakajima K, Hibi M (1997) Signaling mechanisms through gp130: a model of the cytokine system. Cytokine Growth Factor Rev 8(4):241–252
Makinen T, Norrmen C, Petrova TV (2007) Molecular mechanisms of lymphatic vascular development. Cell Mol Life Sci 64(15):1915–1929
Makinen T, Veikkola T, Mustjoki S, Karpanen T, Catimel B, Nice EC, Wise L, Mercer A, Kowalski H, Kerjaschki D, Stacker SA, Achen MG, Alitalo K (2001) Isolated lymphatic endothelial cells transduce growth, survival and migratory signals via the VEGF-C/D receptor VEGFR-3. EMBO J 20(17):4762–4773
Veikkola T, Jussila L, Makinen T, Karpanen T, Jeltsch M, Petrova TV, Kubo H, Thurston G, McDonald DM, Achen MG, Stacker SA, Alitalo K (2001) Signalling via vascular endothelial growth factor receptor-3 is sufficient for lymphangiogenesis in transgenic mice. EMBO J 20(6):1223–1231
Karpanen T, Egeblad M, Karkkainen MJ, Kubo H, Yla-Herttuala S, Jaattela M, Alitalo K (2001) Vascular endothelial growth factor C promotes tumor lymphangiogenesis and intralymphatic tumor growth. Cancer Res 61(5):1786–1790
Skobe M, Hawighorst T, Jackson DG, Prevo R, Janes L, Velasco P, Riccardi L, Alitalo K, Claffey K, Detmar M (2001) Induction of tumor lymphangiogenesis by VEGF-C promotes breast cancer metastasis. Nat Med 7(2):192–198
Stacker SA, Caesar C, Baldwin ME, Thornton GE, Williams RA, Prevo R, Jackson DG, Nishikawa S, Kubo H, Achen MG (2001) VEGF-D promotes the metastatic spread of tumor cells via the lymphatics. Nat Med 7(2):186–191
Kataru RP, Jung K, Jang C, Yang H, Schwendener RA, Baik JE, Han SH, Alitalo K, Koh GY (2009) Critical role of CD11b + macrophages and VEGF in inflammatory lymphangiogenesis, antigen clearance, and inflammation resolution. Blood 113(22):5650–5659
Iwata C, Kano MR, Komuro A, Oka M, Kiyono K, Johansson E, Morishita Y, Yashiro M, Hirakawa K, Kaminishi M, Miyazono K (2007) Inhibition of cyclooxygenase-2 suppresses lymph node metastasis via reduction of lymphangiogenesis. Cancer Res 67(21):10181–10189
Brideau G, Makinen MJ, Elamaa H, Tu H, Nilsson G, Alitalo K, Pihlajaniemi T, Heljasvaara R (2007) Endostatin overexpression inhibits lymphangiogenesis and lymph node metastasis in mice. Cancer Res 67(24):11528–11535
Kishimoto T (2005) Interleukin-6: from basic science to medicine—40 years in immunology. Annu Rev Immunol 23:1–21
Shinriki S, Jono H, Ueda M, Ota K, Ota T, Sueyoshi T, Oike Y, Ibusuki M, Hiraki A, Nakayama H, Shinohara M, Ando Y (2011) Interleukin-6 signalling regulates vascular endothelial growth factor-C synthesis and lymphangiogenesis in human oral squamous cell carcinoma. J Pathol 225(1):142–150
Makinen T, Jussila L, Veikkola T, Karpanen T, Kettunen MI, Pulkkanen KJ, Kauppinen R, Jackson DG, Kubo H, Nishikawa S, Yla-Herttuala S, Alitalo K (2001) Inhibition of lymphangiogenesis with resulting lymphedema in transgenic mice expressing soluble VEGF receptor-3. Nat Med 7(2):199–205
Nisato RE, Harrison JA, Buser R, Orci L, Rinsch C, Montesano R, Dupraz P, Pepper MS (2004) Generation and characterization of telomerase-transfected human lymphatic endothelial cells with an extended life span. Am J Pathol 165(1):11–24
Ando T, Jordan P, Joh T, Wang Y, Jennings MH, Houghton J, Alexander JS (2005) Isolation and characterization of a novel mouse lymphatic endothelial cell line: SV-LEC. Lymphat Res Biol 3(3):105–115
Luo Y, Zhou H, Liu L, Shen T, Chen W, Xu B, Han X, Zhang F, Scott RS, Alexander JS, Alam A, Huang S (2011) The fungicide ciclopirox inhibits lymphatic endothelial cell tube formation by suppressing VEGFR-3-mediated ERK signaling pathway. Oncogene 30(18):2098–2107
Hsu YF, Sheu JR, Lin CH, Yang DS, Hsiao G, Ou G, Chiu PT, Huang YH, Kuo WH (1820) Hsu MJ Trichostatin A and sirtinol suppressed survivin expression through AMPK and p38MAPK in HT29 colon cancer cells. Biochim Biophys Acta 2:104–115
Novick D, Rubinstein M (2007) The tale of soluble receptors and binding proteins: from bench to bedside. Cytokine Growth Factor Rev 18(5–6):525–533
Zhang P, Chebath J, Lonai P, Revel M (2004) Enhancement of oligodendrocyte differentiation from murine embryonic stem cells by an activator of gp130 signaling. Stem Cells 22(3):344–354
Patel A, Zhu Y, Kuzhikandathil EV, Banks WA, Siegel A, Zalcman SS (2012) Soluble interleukin-6 receptor induces motor stereotypies and co-localizes with gp130 in regions linked to cortico-striato-thalamo-cortical circuits. PLoS One 7(7):e41623
Yamashita M, Iwama N, Date F, Shibata N, Miki H, Yamauchi K, Sawai T, Sato S, Takahashi T, Ono M (2009) Macrophages participate in lymphangiogenesis in idiopathic diffuse alveolar damage through CCL19-CCR7 signal. Hum Pathol 40(11):1553–1563
Su JL, Shih JY, Yen ML, Jeng YM, Chang CC, Hsieh CY, Wei LH, Yang PC, Kuo ML (2004) Cyclooxygenase-2 induces EP1- and HER-2/Neu-dependent vascular endothelial growth factor-C up-regulation: a novel mechanism of lymphangiogenesis in lung adenocarcinoma. Cancer Res 64(2):554–564
Timoshenko AV, Chakraborty C, Wagner GF, Lala PK (2006) COX-2-mediated stimulation of the lymphangiogenic factor VEGF-C in human breast cancer. Br J Cancer 94(8):1154–1163
Turkson J, Bowman T, Garcia R, Caldenhoven E, De Groot RP, Jove R (1998) Stat3 activation by Src induces specific gene regulation and is required for cell transformation. Mol Cell Biol 18(5):2545–2552
Calalb MB, Polte TR, Hanks SK (1995) Tyrosine phosphorylation of focal adhesion kinase at sites in the catalytic domain regulates kinase activity: a role for Src family kinases. Mol Cell Biol 15(2):954–963
Heinemeyer T, Wingender E, Reuter I, Hermjakob H, Kel AE, Kel OV, Ignatieva EV, Ananko EA, Podkolodnaya OA, Kolpakov FA, Podkolodny NL, Kolchanov NA (1998) Databases on transcriptional regulation: TRANSFAC, TRRD and COMPEL. Nucleic Acids Res 26(1):362–367
Mukundan L, Milhorn DM, Matta B, Suttles J (2004) CD40-mediated activation of vascular smooth muscle cell chemokine production through a Src-initiated, MAPK-dependent pathway. Cell Signal 16(3):375–384
Touyz RM, He G, El Mabrouk M, Diep Q, Mardigyan V, Schiffrin EL (2001) Differential activation of extracellular signal-regulated protein kinase 1/2 and p38 mitogen activated-protein kinase by AT1 receptors in vascular smooth muscle cells from Wistar-Kyoto rats and spontaneously hypertensive rats. J Hypertens 19(3 Pt 2):553–559
Abu-Ghazaleh R, Kabir J, Jia H, Lobo M, Zachary I (2001) Src mediates stimulation by vascular endothelial growth factor of the phosphorylation of focal adhesion kinase at tyrosine 861, and migration and anti-apoptosis in endothelial cells. Biochem J 360(Pt 1):255–264
Min J, Reznichenko M, Poythress RH, Gallant CM, Vetterkind S, Li Y, Morgan KG (2012) Src modulates contractile vascular smooth muscle function via regulation of focal adhesions. J Cell Physiol 227(11):3585–3592
Thamilselvan V, Craig DH, Basson MD (2007) FAK association with multiple signal proteins mediates pressure-induced colon cancer cell adhesion via a Src-dependent PI3 K/Akt pathway. Faseb J 21(8):1730–1741
Gu Y, Qi X, Guo S (2008) Lymphangiogenesis induced by VEGF-C and VEGF-D promotes metastasis and a poor outcome in breast carcinoma: a retrospective study of 61 cases. Clin Exp Metastasis 25(7):717–725
Yamashita T, Uramoto H, Onitsuka T, Ono K, Baba T, So T, Takenoyama M, Hanagiri T, Oyama T, Yasumoto K (2010) Association between lymphangiogenesis-/micrometastasis- and adhesion-related molecules in resected stage I NSCLC. Lung Cancer 70(3):320–328
Hoshida T, Isaka N, Hagendoorn J, di Tomaso E, Chen YL, Pytowski B, Fukumura D, Padera TP, Jain RK (2006) Imaging steps of lymphatic metastasis reveals that vascular endothelial growth factor-C increases metastasis by increasing delivery of cancer cells to lymph nodes: therapeutic implications. Cancer Res 66(16):8065–8075
Saharinen P, Tammela T, Karkkainen MJ, Alitalo K (2004) Lymphatic vasculature: development, molecular regulation and role in tumor metastasis and inflammation. Trends Immunol 25(7):387–395
Mihara M, Hashizume M, Yoshida H, Suzuki M, Shiina M (2012) IL-6/IL-6 receptor system and its role in physiological and pathological conditions. Clin Sci 122(4):143–159
Johnson GL, Lapadat R (2002) Mitogen-activated protein kinase pathways mediated by ERK, JNK, and p38 protein kinases. Science 298(5600):1911–1912
Yu H, Pardoll D, Jove R (2009) STATs in cancer inflammation and immunity: a leading role for STAT3. Nat Rev Cancer 9(11):798–809
Olayioye MA, Beuvink I, Horsch K, Daly JM, Hynes NE (1999) ErbB receptor-induced activation of stat transcription factors is mediated by Src tyrosine kinases. J Biol Chem 274(24):17209–17218
Silva CM (2004) Role of STATs as downstream signal transducers in Src family kinase-mediated tumorigenesis. Oncogene 23(48):8017–8023
De Martin R, Hoeth M, Hofer-Warbinek R, Schmid JA (2000) The transcription factor NF-kappa B and the regulation of vascular cell function. Arterioscler Thromb Vasc Biol 20(11):E83–E88
Aoki T, Kataoka H, Shimamura M, Nakagami H, Wakayama K, Moriwaki T, Ishibashi R, Nozaki K, Morishita R, Hashimoto N (2007) NF-kappaB is a key mediator of cerebral aneurysm formation. Circulation 116(24):2830–2840
DeBusk LM, Massion PP, Lin PC (2008) IkappaB kinase-alpha regulates endothelial cell motility and tumor angiogenesis. Cancer Res 68(24):10223–10228
Sakamoto K, Maeda S, Hikiba Y, Nakagawa H, Hayakawa Y, Shibata W, Yanai A, Ogura K, Omata M (2009) Constitutive NF-kappaB activation in colorectal carcinoma plays a key role in angiogenesis, promoting tumor growth. Clin Cancer Res 15(7):2248–2258
Karin M (2006) Nuclear factor-kappaB in cancer development and progression. Nature 441(7092):431–436
Nizamutdinova IT, Oh HM, Min YN, Park SH, Lee MJ, Kim JS, Yean MH, Kang SS, Kim YS, Chang KC, Kim HJ (2007) Paeonol suppresses intercellular adhesion molecule-1 expression in tumor necrosis factor-alpha-stimulated human umbilical vein endothelial cells by blocking p38, ERK and nuclear factor-kappaB signaling pathways. Int Immunopharmacol 7(3):343–350
Barbier D, Garcia-Verdugo I, Pothlichet J, Khazen R, Descamps D, Rousseau K, Thornton D, Si-Tahar M, Touqui L, Chignard M, Sallenave JM (2012) Influenza A induces the major secreted airway mucin MUC5AC in a protease-EGFR-ERK-Sp1 dependent pathway. Am J Respir Cell Mol Biol 47(2):149–157
Lin HH, Lai SC, Chau LY (2011) Heme oxygenase-1/carbon monoxide induces vascular endothelial growth factor expression via p38 kinase-dependent activation of Sp1. J Biol Chem 286(5):3829–3838
Kinoshita S, Akira S, Kishimoto T (1992) A member of the C/EBP family, NF-IL6 beta, forms a heterodimer and transcriptionally synergizes with NF-IL6. Proc Natl Acad Sci USA 89(4):1473–1476
LeClair KP, Blanar MA, Sharp PA (1992) The p50 subunit of NF-kappa B associates with the NF-IL6 transcription factor. Proc Natl Acad Sci USA 89(17):8145–8149
Goldhar AS, Duan R, Ginsburg E, Vonderhaar BK (2011) Progesterone induces expression of the prolactin receptor gene through cooperative action of Sp1 and C/EBP. Mol Cell Endocrinol 335(2):148–157
Duong T, Koopman P, Francois M (2012) Tumor lymphangiogenesis as a potential therapeutic target. J Oncol 2012:204946
Lin J, Lalani AS, Harding TC, Gonzalez M, Wu WW, Luan B, Tu GH, Koprivnikar K, VanRoey MJ, He Y, Alitalo K, Jooss K (2005) Inhibition of lymphogenous metastasis using adeno-associated virus-mediated gene transfer of a soluble VEGFR-3 decoy receptor. Cancer Res 65(15):6901–6909
Roberts N, Kloos B, Cassella M, Podgrabinska S, Persaud K, Wu Y, Pytowski B, Skobe M (2006) Inhibition of VEGFR-3 activation with the antagonistic antibody more potently suppresses lymph node and distant metastases than inactivation of VEGFR-2. Cancer Res 66(5):2650–2657
Su JL, Yang PC, Shih JY, Yang CY, Wei LH, Hsieh CY, Chou CH, Jeng YM, Wang MY, Chang KJ, Hung MC, Kuo ML (2006) The VEGF-C/Flt-4 axis promotes invasion and metastasis of cancer cells. Cancer Cell 9(3):209–223
Ischenko I, Seeliger H, Camaj P, Kleespies A, Guba M, Eichhorn ME, Jauch KW, Bruns CJ (2010) Src tyrosine kinase inhibition suppresses lymphangiogenesis in vitro and in vivo. Curr Cancer Drug Targets 10(5):546–553
Ischenko I, Guba M, Yezhelyev M, Papyan A, Schmid G, Green T, Fennell M, Jauch KW, Bruns CJ (2007) Effect of Src kinase inhibition on metastasis and tumor angiogenesis in human pancreatic cancer. Angiogenesis 10(3):167–182
Mima T, Nishimoto N (2009) Clinical value of blocking IL-6 receptor. Curr Opin Rheumatol 21(3):224–230
Acknowledgments
We would like to thank Dr. Kjetil Tasken for the kind gift of the p/T81 C/EBP-luc reporter construct and Dr. J.S. Alexander (Shreveport, LA, USA) for the kind gift of the mouse LEC line SV-LEC. This work was supported by grant from the National Science Council of Taiwan [NSC98-2320-B-038-007]; Grant [100TMU-WFH-01-4] from the Taipei Medical University-Wan Fang Hospital, Taipei, Taiwan; and Grant [LSH-2012-04] from the Landseed Hospital, Taoyuan, Taiwan.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
Yu-Han Huang and Hung-Yu Yang have contributed equally to this study.
Rights and permissions
About this article
Cite this article
Huang, YH., Yang, HY., Hsu, YF. et al. Src contributes to IL6-induced vascular endothelial growth factor-C expression in lymphatic endothelial cells. Angiogenesis 17, 407–418 (2014). https://doi.org/10.1007/s10456-013-9386-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10456-013-9386-1