Abstract
Formation of a correctly organised vasculature and subsequently embryonic survival is critically dependent on the dosage and site-specific expression of VEGF. Murine VEGF exists in three common isoforms (viz. 120, 164 and 188 amino acids) having different organ specific distribution levels. Gene knock-in studies show that expression of any of the individual isoforms of VEGF extends survival until birth, although each is associated with distinct organ-specific abnormalities. Comparison of the effects of VEGF isoform expression is complicated by the general lethality of mis-expression, in addition to cumulative effects of adjacent tissues from the inappropriately patterned vasculature. Here we investigate the effects of over-expression of individual VEGFA isoforms from the lens-specific αA-Crystallin promoter and characterise their effects on the vessel morphology of the hyaloid and developing retinal vasculature. Since the hyaloid vasculature is an anatomically distinct, transient vasculature of the eye, comprising 3 cell types (endothelium, pericytes and macrophages) it is possible to more readily interpret the role of individual VEGF-A isoforms in vascular pattern formation in this model. The severity of the vascular phenotype, characterised by a hyperplastic hyaloid at E13.5 and subsequently retinal vascular patterning and ocular defects, is most severe in transgenics over-expressing the more diffusible forms of VEGFA (120 and 164), whereas in VEGFA188 transgenics the hyaloid vascular defects partially resolve post-natally. The results of this study indicate that individual isoforms of VEGFA induce distinct vascular phenotypes in the eye during embryonic development and that their relative doses provide instructive cues for vascular patterning.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The prototypical vascular endothelial growth factor (herein termed VEGFA) is a critical regulator of vasculogenesis, as well as of developmental, physiological and pathological angiogenesis. Loss of a single VEGFA allele in mice is sufficient to result in embryonic death at around E9 [1, 2], demonstrating that embryonic survival is dependent on the dose of VEGFA expressed. In addition to dose, site-specific expression of VEGFA during embryogenesis is crucial to fetal growth and neonatal survival. Gene deletion of VEGFA in areas expressing collagen 2α1 results in embryonic lethality at E10.5 [3], whereas Cre-LoxP mediated gene excision in mice leads to neonatal lethality [4].
Murine VEGFA is expressed in at least three distinct isoforms of 120, 164 and 188 amino acids, which are generated by alternative transcription from a single gene locus [5, 6]. Although VEGFA164 seems to be the predominantly expressed isoform, individual isoforms of VEGFA show an organ specific pattern of distribution during embryonic development [7]. VEGFA120 is diffusible and does not bind heparin, whereas the higher molecular weight isoforms bind heparin with increasing affinity [8, 9] and are tightly bound to basement membranes [10]. Expression of VEGFA120 alone, is sufficient to compensate for the loss of VEGFA164 and 188 during embryonic angiogenesis [11, 12], which indicates some degree of functional redundancy between the isoforms of VEGFA. However, the post-natal mortality due to reduced myocardial vascularisation [11], in addition to perturbations in lung and bone angiogenesis [13] in VEGFA120 knock-in mice implies that higher molecular-weight, heparin-binding VEGFA isoforms are an absolute requirement for appropriate vascular patterning in specific organs during post-natal development [12].
In order to more clearly delineate the functional impact of the major VEGFA isoforms in vascular patterning, we have established three lines of transgenic mice in which individual isoforms of murine VEGFA are expressed from the ocular lens via the αA-Crystallin promoter [14, 15]. The lens is an organ where endogenous VEGFA isoforms are expressed as early as E12.5 and expression levels correlate with both the establishment and early growth of the hyaloid vasculature [16]. As the hyaloid vasculature contains only 3 cell types (i.e. endothelial cells/angioblasts, pericytes and macrophages), this makes it an ideal structure for sequential analysis of morphological changes associated with vascular specific cues emanating from the lens. Specifically, over-expression of individual VEGFA isoforms results in unique vascular malformations in both the hyaloid and retinal vasculature. Here we demonstrate that individual isoforms of VEGFA result in distinctive structures within the embryonic hyaloid vasculature at E13.5, just 1 day after the differentiation of this vascular plexus from precursor cells [16]. This data shows that in permissive environments, individual isoforms of VEGFA determine unique patterns of vascular morphogenesis and that both the dose and organ specific expression of VEGFA isoforms is critical to induce and maintain an appropriate vascular phenotype.
Methods
Generation of transgenic mice
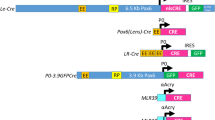
In order to generate equivalent VEGFA isoform transgenics, the cDNA of murine VEGFA120, 164 or 188 isoform coding sequences were individually cloned into CPV2 plasmids [17] in frame with the αA-Crystallin promoter (Fig. 1A). Transgenic mice for each VEGFA isoform were generated by standard methods. Presence of the transgene in genomic DNA was confirmed by both Southern analysis (not shown) using an 857 bp EcoRI–XbaI SV40 polyA fragment excised from the CPV-2 plasmid [17] and PCR analysis (Fig. 1B) with primers specific for the αA-crystallin promoter 5′-CCGAGCTGAGCATAGACATTTTG-3′ and the VEGFA cDNA coding sequence 5′-CTCCAGGGCTTCATCGTTAC-3′. The phenotype of VEGFA transgenic mice was confirmed from at least three independent lines for each of the isoforms of VEGFA examined. Ethical approval for experimental procedures involving animals in this study conformed to institutional and national guidelines.
Production and characterisation of VEGF-A transgenics. (A) VEGFA isoform transgene design. Positions of the oligonucleotide PCR and SV40 polyA cDNA probe are indicated. (B) PCR analysis of transgenic founder DNA samples. Lane 1, HindIII marker; lane 2–4, 10 pg VEGFA plasmids; lane 5, wt; lane 6, VEGFA164 founder; lane 7, VEGFA120 founder; lane 8, VEGFA188 founder. (C) Bright field photomicrographs of an E16.5 VEGFA164 mouse eye hybridised with 35S-labelled SV40 polyA mRNA (i) anti-sense probe (ii) sense control. (D) rt-PCR with VEGFA specific probes of mRNA extracted from P2 lenses. Upper panel: (1) Size marker (2) VEGFA164 (3) VEGFA120 (4) VEGFA188 (5) Wt (6) VEGFA164 plasmid, (7) VEGFA120 plasmid, (8) VEGFA188 plasmid, (9) negative control. Lower panel: (2–5) 18S reference samples. (E) Representative photographs of gross eye phenotypes in (i) wt (ii) 2-month-old VEGFA120 transgenic (iii) A 3-month-old VEGFA164 mouse (arrow = corneal blood vessel) (iv) 2-month-old VEGFA188 mouse
Timed matings between C57Bl6J wild-type female mice and transgenic male founder mice were arranged and embryos (E12.5–E18.5) collected following euthanasia. Samples were fixed in either 2.5% glutaraldehyde in 0.1 M cacodylate buffer for electron microscopy, 10% neutral formal buffered saline for histology, 4% para-formaldehyde in phosphate buffered saline (PBS) for immunohistochemistry or embedded in OCT for cryosectioning. Processing and examination of specimens for scanning or transmission electron microscopy were performed according to standard procedures.
In situ hybridisation
An 845 bp fragment of SV40 pA [17] was used to generate 35S-labelled cRNA probes, with the sense probe serving as a negative control. In situ hybridisation on E16 transgenic eyes was performed as previously described [16] and showed specific localisation of the probe to lens epithelial cells (Fig. 1C).
Determination of VEGFA concentration in lenses
mRNA from pooled P2 lens was prepared and reverse transcribed using an Abgene 1st strand synthesis kit (Advanced Biotechnologies, USA) according to the manufacturers’ instructions. PCRs were performed on 2 μl samples of cDNA using VEGFA specific primers 5′-CTG CTC TCT TGG GTC CAC TGG and 3′ CAC CGC CTT GGC TTG TCA CAT located in exons 1 and 8, respectively [18]. The PCR conditions used were 94°C, 3 min for 1 cycle, then 94°C, 15 s, 60°C, 30 s, 72°C, 1 min for either 21 or 23 cycles. Scanning densitometry was used to semi-quantitatively assess message levels against an 18S internal standard. Lenses from individual P2 mice were pooled and dissociated in lysis buffer as previously described [19]. Soluble VEGFA protein concentrations were determined using a VEGFA specific ELISA kit (R and D Systems Inc., Minneapolis, Minnesota, USA) according to the manufacturers’ instructions.
Immunohistochemistry
Immunohistochemical detection of macrophages using F4/80 antibody (Southern Biotechnology, USA), VEGF (Santa Cruz Biotechnology Inc.: USA), HSPG (Upstate Biotechnology: USA) or α-smooth muscle actin (Sigma, USA) for pericytes was carried out according to the manufacturers’ instructions using the Vectastain (Birlingame, USA), ABC staining method. Negative controls for primary antibodies, in both wild-type and transgenic tissue, was determined by inclusion of the appropriate IgG isotype control; no demonstrable non-specific labelling with the control antibody was seen in any of the tissues examined (not shown). Immunofluorescent staining of endothelium was performed using an undiluted Mec 13/3 hybridoma supernatant (anti-CD31) and Cy3-coupled goat anti-rat secondary antibody on acetone fixed cryosections; counter-staining of nuclei was performed with Hoechst 33342. Photographs were taken with an Axiocam digital camera mounted on a Axiophot (Zeiss) microscope.
Whole mount sample preparation and immunohistochemistry
Eyes were enucleated and fixed in 4% PFA (in PBS) over night. Retinas were dissected and processed for immunofluorescence microscopy as previously described [20]. Briefly, samples were labelled with biotinylated Isolectin B4 (Bandeiraea simplicifolia; Sigma, 20 μg/ml) followed by Alexa 568 conjugated streptavidin (Molecular Probes) and/or double stained with 1:400 dilution of Glial Fibrillary Acidic Protein (GFAP: Sigma) followed by Alexa 488 (Molecular Probes) and subsequently flat-mounted. Photographs were taken with an Axiocam digital camera mounted on a Axiophot (Zeiss) microscope or on an SP5 con-focal microscope (Leica).
Results
VEGFA isoform-specific ocular defects
Semi-quantitative rt-PCR analysis of pooled P2 lens samples showed that the predominant mRNA isoforms in wild-type mice are VEGFA164 and 120. Isoform-specific message levels were raised approximately 6- to 10-fold in transgenic mice (P < 0.05) in comparison to controls (Fig. 1D). Gross ocular phenotypes were indistinguishable between 3 independent lines for each VEGFA transgenic isoform examined. Compared to wild-type eyes (Fig. 1E(i)), adult VEGFA120 mice showed corneal opacity, often with evidence of recent anterior chamber haemorrhage (Fig. 1E(ii)). By 3 months VEGFA120 mice had suffered spontaneous ocular rupture with subsequent lid fusion (Table 1). Adult VEGFA164 mice also had conspicuous intra-ocular bleeding often accompanied by corneal neovascularisation (Fig. 1E(iii)), with eye rupture and lid fusion typically occurring in the fourth month (Table 1), whereas VEGFA188 mice had distinct, bilateral cataracts and mis-shapen globes (Fig. 1E(iv)).
Unique large vessel morphology in VEGFA transgenic mice
The hyaloid vasculature is a discrete cluster of cells on the posterior pole of the lens vesicle in both E12.5 wild-type (Fig. 2a) and VEGFA transgenic (Fig. 2b–d) mice. By E13.5 distinct vascular plexi, the tunica vasculosa lentis (TVL) and arteria hyaloidea propria (AHP) are observed on the lens surface and inner limiting membrane (ILM) in wild-type mice (Fig. 2e). In transgenic mice, vessel hypertrophy is conspicuous (Fig. 2f–h; Table 1). Specifically, in E13.5 VEGFA120 transgenics, the vasculature in the posterior compartment of the eye appears spongy with many CD31 immunoreactive cells, although there is no distinct AHP, TVL or pupillary membrane and there is evidence of anterior chamber haemorrhage (Fig. 2f). In VEGFA164 mice (Fig. 2g), the lens is prolapsed into the anterior chamber, hyperplastic vascular sacs adhere to posterior and anterior lens surfaces, and there is frequent intra-ocular haemorrhage (Table 1). In VEGFA188 transgenics (Fig. 2h), a single hyperplastic vascular sac adheres to the posterior pole of the lens and the AHP is clearly separated from the retinal surface. Immunostaining of E15.5 wild-type eyes with CD31 revealed discrete and regularly spaced capillaries (Fig. 2i). Most noticeably, CD31 immunoreactivity in transgenic eyes follows an isoform-specific distribution, with the greatest numbers of labelled cells in VEGFA120, followed by VEGFA164 and VEGFA188 (c.f. Fig. 2i–l). CD31 immunoreactive cells form a continuous rim around the lens in VEGFA120 eyes (Fig. 2j) and contribute to the structure of a large vascular sac in VEGFA164 mice (Fig. 2k) and a somewhat smaller vascular sac on the posterior pole of the lens in VEGFA188 mice (c.f. Fig. 2l).
Isoform-specific hyperplastic vascular structures in VEGFA transgenic mice. Haematoxylin and Eosin stained paraffin sections from wt and VEGFA transgenic mice. (a) E12.5 wt, (b–d) E12.5 VEGFA transgenics (e) E13.5 wt, showing vessels of the AHP (arrows) and TVL (arrowheads) (f) E13.5 VEGFA120 transgenic; haemorrhage (arrowheads) (g) E13.5 VEGFA164: vascular sacs on the posterior (arrowheads) and anterior (arrows) lens surface (h) E13.5 VEGFA188 transgenic; vascular sac on the posterior lens capsule (arrows) and the AHP (arrowheads) is separated from the retina. CD31 immunostaining of eyes from E15.5 mice (i–l). (i) wt mice; AHP (arrowheads) and TVL capillaries (arrows). (j) VEGFA120; hyperplastic vasculature (arrowheads) and markedly increased CD31 immunoreactivity. (k) VEGFA164; vascular sac (arrows) and numerous CD31 positive cells (arrowhead). (l) VEGFA188; CD31 positive vascular sac on lens surface (arrowheads) and capillaries (arrows)
In wild-type eyes, α-smooth muscle actin (αSMA) immunoreactivity was most often associated with single ablumenal cells in the TVL and AHP (Fig. 3a) and is consistent with identification of these cells as pericytes. αSMA positive cells were abundant in the hyperplastic vasculatures of VEGFA transgenic mice, being juxtaposed to the ablumenal surface of endothelium (Fig. 3b–d). Cells staining with the macrophage specific marker F4/80, termed hyalocytes, were observed from as early as E13.5 in both wild-type (Fig. 3e), VEGFA164 (Fig. 3f) as well as VEGFA120 and 188 transgenic mice (not shown), where they were largely associated with the ablumenal surface of the vasculature. At E18.5, the control (Fig. 3g) and VEGFA120 mice (not shown) had relatively few F4/80 immunoreactive cells on their vessel ablumenal surfaces, whereas in both VEGFA164 (Fig. 3h) and VEGFA188 transgenic mice (not shown) numerous macrophages were identified both ablumenally and within the walls of the hyperplastic vessels.
Increased pericyte and hyalocyte numbers in transgenic hyaloid vasculature. Immunohistochemical detection of αSMA (a–d) and F4/80 (e–h) in paraffin sections from wt and VEGFA transgenic mice. (a) wt: an endothelial cell (arrowhead) in a TVL capillary associated with an αSMA positive cell (arrow). αSMA positive cells (arrows) are on the ablumenal surface of vessels and closely associated with endothelial cells (arrowheads) in VEGFA120 (b) VEGFA164 (c) and VEGFA188 (d) mice. (e) F4/80 labelling (arrows) of hyalocytes in (e) E13.5 wt, (f) E13.5 VEGFA164 transgenic, (g) E18.5 wt and (h) E18.5 VEGFA164 transgenic. Bar = 50 μm (a–d, f–h) and 100 μm (e)
Both matrix-bound and soluble VEGFA levels regulate vessel morphology
The total levels of individual VEGFA protein isoforms in P2 lenses were measured in three independent assays. Levels of soluble VEGFA isoforms detected (mean ± 1 SD) were greatest in VEGFA120 (1216±52 pg/ml; P = 0.003) and next highest in VEGFA164 lenses (600±297 pg/ml; P = 0.016), whereas levels of VEGFA in lenses from VEGFA188 mice (146±52 pg/ml; P = 0.99) were not significantly different from those of wild-type mice (157±69 pg/ml). This result indicated that some of VEGFA188 could be retained in the insoluble fraction. We were unable to resolve this issue by Western blotting, as for each line of transgenic mouse, results of pilot studies indicated that more than 200 lenses from P2 mice would be required to detect sufficient quantities of insoluble VEGFA protein isoforms bound in the lens capsule.
Immunohistochemical detection of heparin sulphate proteoglycan (HSPG; Fig. 4a–c) and VEGFA (Fig. 4d–f) revealed co-localisation in the lens capsule of wild-type mice. HSPG labelling was weak and largely restricted to the lens capsule and periphery of the hyaloid vasculature in VEGFA120 eyes at E15.5 (Fig. 4b), with VEGFA immunostaining most prominent in the lens and surrounding the hyaloid vasculature (Fig. 4e). In VEGFA188 eyes, the weak HSPG staining of the lens capsule and hyaloid vasculature (Fig. 4c) was similar to that observed in wild-type eyes (Fig. 4a), while the distribution of VEGF staining was widespread (Fig. 4f). The similarity in the staining pattern for VEGFA immunohistochemical labelling in the VEGFA120 E15.5 eye compared with wild-type mice (c.f. Fig. 4d and e), is most likely due to an inability of the primary antibody to detect the entirely soluble form of VEGFA.
HSPG/VEGF immunostaining and ultrastructural features of wt and VEGFA transgenic mice. HSPG (a–c) and VEGF immunostaining (d–f) in E15.5 wt (a, d), VEGFA120 (b, e) and VEGFA188 (c, f) transgenic mice. (a) wt HSPG immunostaining in lens capsule (arrow) and hyaloid capillary basement membrane (arrowheads). (b) VEGFA120: weak HSPG staining in the thin lens capsule (arrow) and obvious immunoreactivity around hyperplastic vessels (arrowheads). (c) VEGFA188 transgenic: weak HSPG staining in the thin lens capsule (arrow) and basement membrane surrounding a vascular lacuna (arrowhead). (d) wt VEGFA immunostaining. (e) VEGFA120; VEGF immunostaining in the lens and basement membrane of the hyperplastic lens vasculature (arrow). (f) VEGFA188 transgenic; widespread immunostaining of VEGFA, including lens capsule (arrows). Bar = 50 μm (a–f). (g) SEM of TVL from wt mouse. Bar = 100 μm. (h) E18.5 VEGFA120 transgenic; honeycomb-like vascular plexus (asterisks) separated from the lens. RF = retinal fold. Bar = 100 μm. (i) VEGFA120 transgenic lens capsule (lc) with several non-fused endothelial segments (arrowheads) and accompanying mononuclear cells (arrows); Asterisk = process artefact. Bar = 5 μm. (j) VEGFA164 transgenic; lens cavity (lc), lens fibre cells (lf), capillary membrane (cm) on lens surface, posterior lens mass (plm), containing small diameter vessels (arrows). Bar = 100 μm. (k) E18.5 VEGFA164 transgenic: several loosely organised endothelial cells (arrows) are observed adjacent to the thin lens capsule (arrowhead). Bar = 2 μm. (l) VEGFA188 transgenic: patent vessels (arrows) on the surface of a hyper-fused vascular mass. Bar = 100 μm
Scanning electron microscopic (SEM) analyses of wild-type eyes, revealed a regular, fine network of capillaries ramifying over the lens surface (Fig. 4g). In VEGFA120 eyes, a layered hyaloid vasculature is juxtaposed to the posterior lens surface (Fig. 4h). There is also evidence of failure of endothelial tube formation, as unconnected tube segments are conspicuous on the lens surface (Fig. 4i). In VEGFA164 transgenic mice, the posterior lens capsule is covered by a membrane composed of capillaries (Fig. 4j), which is interspersed with loosely organised endothelial cells (Fig. 4k). The “ablumenal” surface of the hyperplastic vascular structure in VEGFA164 transgenics (posterior lens mass; PLM) consists of a dense mass of cells (Fig. 4j) composed of endothelium (Fig. 2k), α-smooth muscle actin (Fig. 3c) and F4/80 positive cells (Fig. 3h). In VEGFA188 transgenics, the hyperplastic vascular structure is tightly associated with the lens surface and has numerous surface-associated capillaries (Fig. 4l).
Ocular architecture is severely disturbed by VEGFA isoform over-expression
The AHP and TVL vessel plexi are readily observed in wild-type eyes and differentiation of the neural and sensory retinal layers is apparent by E18.5 (Fig. 5a). In neonatal mice (P20), the hyaloid vasculature has regressed completely and the retina has an essentially mature structure (Fig. 5e). Contrastingly, in all VEGF transgenic mice, separation of the vascular plexus into the AHP and TVL is indistinct and there are discrete vascular and ocular pathologies associated with over-expression of each individual isoform (Fig. 5b–d; Table 1). Retinal rosetting and folding, in addition to separation of the inner and outer retinal layers, abnormal lens epithelial cell differentiation, intra-ocular bleeding, corneal hypertrophy and vascularisation are all consistent histological features of eyes from E18.5 VEGFA120 mice (Fig. 5b, Table 1). These pathologies are exacerbated by P20, where there is marked disturbance of the lens architecture and a grossly swollen lens vesicle, resulting in obliteration of the anterior and posterior chambers (Fig. 5f). There is also evidence of traction on the retina, vitreous and sub-retinal haemorrhage and clear signs of corneal thickening (Fig. 5f; Table 1). In all E18.5 VEGFA164 mice, a large vascular lacuna was present on the posterior pole of the lens, there were disorders of lens epithelial cell differentiation and amorphous lens inclusions were also seen (Fig. 5c), which may be associated with failure of lens vesicle closure. Severe lenticular hypertrophy in P20 VEGFA164 mice, results in obliteration of the vitreous. In addition, the abnormal lens abuts the inner surface of the thickened cornea and there is often bleeding into the anterior chamber (Fig. 5g; Table 1). In E18.5 VEGFA188 transgenics (Fig. 5d and Table 1), a considerably milder phenotype than that of \(\hbox{VEGFA}{_{120 \ {\rm and} \ 164}}\) mice is observed (c.f. Fig. 5b and c), consisting of cataract formation and persistent vascular network. By P20, the less severe phenotype in the VEGFA188 transgenic mice is obvious (Fig. 5h).
Severe ocular phenotypes in VEGFA transgenic mice. Haematoxylin and Eosin stained sections from the eyes of E18.5 (a–d) and P20 (e–h) wt and VEGFA transgenic mice. (a) E18.5 wt eye. (b) VEGFA120 eye. Multi-layered vascular plexus (arrowheads), vitreal bleeding (asterisk) and thickened cornea. (c) VEGFA164 mice: flattened vascular plexus (arrows) and haemorrhage (arrowhead), asterisk = lens vesicle. (d) VEGFA188 transgenic mice: vascular sac (arrows) and haemorrhage (asterisk). (e) P20 wt mice. (f) P20 VEGFA120 transgenic: (g) P20 VEGFA164 transgenic: flattened vascular lacuna (arrowhead) and lens haemorrhage (arrows). (h) VEGFA188 mice: partially regressed vascular structure on lens (arrowheads)
Retinal vascular patterning defects in VEGFA transgenic mice
The retinal vasculature of wild-type mice at P7 has an evenly branched pattern with readily recognisable arteries and veins (Fig. 6a). The retinal vasculature of all VEGF-A transgenic mice appeared highly abnormal (Fig. 6b–d), although distinct isoform-specific differences were noted. In VEGFA120 mice (Fig. 6b), vessel duplication was seen, both within the fibre layer and under the inner limiting membrane, producing a multi-layered appearance of the plexus (Fig. 6b). Arterio-venous specification was clearly evident in VEGFA164 and 188 mice (Fig. 6c and d), although in VEGFA164 eyes a deterioration of the regular routing and spacing pattern of arteries and veins (Fig. 6c) was apparent. Reduced numbers of connecting vessels around arterioles in VEGFA164 and 188 eyes was noted (Fig. 6c and d). However, vessel density around veins was sharply increased in both VEGFA164 and 188 eyes (Fig. 6c and d). This pattern was particularly prominent in VEGFA188 retina, leading to an extraordinarily dense appearance of large parts of the plexus and occasional hyper-fusion of vessels into large sacs (Fig. 6d). In order to further understand the role of VEGF-A isoform over-expression in vascular patterning we studied the formation of the primary retinal plexus at P3. In wild-type littermates, an evenly spaced meshwork (Fig. 6e) was observed, whereas in VEGFA120 eyes, intra-retinal sprouts appeared stunted, there were fewer inter-connecting branches and the sprout density along the leading edge was reduced (Fig. 6f). Duplication of the primary retinal plexus observed at P7 in VEGFA120 retinae (Fig. 6b), was also evident at P3 (Fig. 6f). In VEGFA164 eyes, the density of sprouting tips in the newly forming vascular plexus, as well as the calibre of vessels (Fig. 6g), was highly variable. The density of sprouting in VEGFA188 retina was comparable to that of wild-type mice (Fig. 6e), however individual sprouts appeared wider, flattened and displayed numerous filopdia (Fig. 6h). In addition, the broad inter-connecting vessels of the VEGFA164 and 188 plexi were indicative of hyper-fusion (Fig. 6g and h). Dual immunofluorescence stating with GFAP (astrocytes) and BSI-B4 (endothelium), revealed that in littermate control mice, a regularly spaced astrocytic network underlay the advancing retinal vessels (Fig. 7a–c). In VEGF-A120 mice, the density of astocytic processes was greatly reduced and the regular vascular arcade patterning was lost (Fig. 7d), although the endothelium (Fig. 7e) clearly used these cells as a growth template (Fig. 7f). In contrast, the astrocytic network in VEGFA164 mice was extremely dense, with no distinct vascular arcade formation at the leading edge (Fig. 7g–i).
Retinal vascular morphology at P7 (a–d) and P3 (e–h). (a) P7wt retina: arterial (arrows) and venous (arrowheads) profiles. (b) VEGFA 120 retina. (c) In VEGFA164 retina: Arterial (arrows) and venous (arrowheads) connections to the primary plexus are reduced. (d) In VEGFA188 mice at P7: note the marked increase in capillaries connecting to veins (arrowheads) and arteries (arrows). (e) At P3, wt retinal vasculature: sprouts at the leading edge (arrows) are highly polarised. (f) P3 VEGFA120 retina: note, there are few inter-connecting branches and polarised cells at the leading edge (arrowheads). (g) P3 VEGFA164 retina: stunted endothelial sprouts (arrowheads). (h) P3 VEGFA188 retina: flattened, irregular tip-cells with numerous filopodia (arrowheads) and evidence of hyper-fused vessels (asterisks)
Discussion
This study investigates the relationship between lens specific over-expression of individual splice-variants of VEGFA and specific patterning defects in the developing hyaloid and retinal vasculature. VEGFA levels as measured by semi-quantitative rt-PCR are approximately 10-fold higher in transgenic than those of wild-type mice. In VEGFA120 transgenics, tortuous vascular tufts are observed in the vitreous, in addition to marked retinal malformations and haemorrhage. Over-expression of VEGFA164 resulted in fused sac-like hyaloid vasculatures with conspicuous intra-ocular bleeding and ultimately ocular involution; whereas in the case of VEGFA188 transgenics the hyaloid vasculature partially regressed during the neonatal period. The relative severity of the ocular morphology in these transgenic lines is inversely related to the size and ability of the VEGFA isoform to bind heparin sulphate proteoglycans [9]; i.e. in decreasing order of severity (VEGFA120 > VEGFA164)≫ VEGFA188. The levels of VEGFA isoforms are unlikely to be accounted for by transgene copy number differences, as independent lines from each transgenic construct yielded similar protein levels and consistent ocular phenotypes. Similarly, quantitation of protein within P2 lenses, revealed that free VEGFA levels mirrored the severity of the ocular phenotype, being highest in VEGFA120 transgenics (approximately 10 × the levels in wild-type), with intermediate levels in VEGFA164 mice and levels in VEGFA188 not significantly different from wild-type eyes.
Cells expressing VEGF-A usually express all the isoforms simultaneously [21], however, there are specific biases to the isoforms of VEGF-A expressed. For instance, VEGF-A isoform expression varies during blastocyst implantation [22, 23], embryogenesis [7] as well as in the normal adult [24] and may also account for differences in the behaviour of benign and malignant tumours [25–28]. In this study, the \(\hbox{VEGFA}{_{120\&164}}\) isoforms are most abundant in the wild-type lens. VEGFA164 (and its various species homologues) are the predominant isoform in the periods of angioblast migration and organ development during embryogenesis [7] and in the adult [29]. Temporal regulation of VEGFA isoform expression also occurs during mammary gland development in pregnancy and lactation [18], as well as in multi-stage carcinogenesis in mice [29], although the mechanisms responsible for this switching are poorly understood. During embryogenesis, VEGFA levels are tightly regulated, with small reductions, increases or inappropriate expression domains leading to severe, often lethal phenotypes characterised by gross vascular and associated tissue malformations [1–4].
The hyaloid vascular system of the developing eye is a transient vascular network that surrounds and provides nourishment to the developing fetal lens, retina and associated structures [30]. The primary vascular plexus comprising the hyaloid vascular architecture is established by E13, and following remodelling, the structure normally regresses post-natally [31, 32], with retinal and choriocapillaris vasculature maintaining retinal development after birth. Lens epithelial cells (LEC) in various stages of differentiation constitute the only cell type in the lens, and from E15 onwards they form the lens capsule, a thick, heparin-rich basement membrane [33] capable of binding significant quantities of endothelial mitogens [34, 35]. Throughout embryonic development, LEC produce a variety of growth [33, 36] and survival factors [16], which are capable of acting in an autocrine [37, 38] or paracrine manner [17, 39]. As the hyaloid vasculature is juxtaposed to, and is capable of responding to signals from the lens, including human VEGFA165 [15], it is an ideal, non-lethal model system with which to examine the developmental effects of individual VEGFA isoforms on vascular patterning.
Between E12 and E13.5, the murine posterior hyaloid vasculature is fully established and is a completely arterial plexus [31]. The vastly increased numbers of endothelial cells observed surrounding the lenses of transgenic mice at E13.5 are unlikely to be due to precursor proliferation alone as there were no obvious differences in cell numbers noted in this study between transgenic and control mice at E12.5. Quantitative ultrastructural analysis in E13.5 VEGFA188 transgenics revealed a 3-fold increase in the numbers of both endothelial cells and pericytes as compared to wild-type embryos. We therefore conclude that the aberrant vascular structures on the posterior aspect of the E13.5 lens in VEGFA188 mice (as well as in \(\hbox{VEGFA}{_{120\&164}}\) transgenics where endothelial cell numbers were much greater), must have been contributed to by the migration of endothelial precursors towards the increasing concentration of VEGF, similar to that described in VEGFA165 transgenics [15] and during formation of the dorsal aorta [40, 41].
During early ocular development, mesenchymal cells in the developing vitreal compartment migrate to both the lens and retinal surface [30]. Since the morphology of the murine hyaloid is established at E13.5, it is clear that angioblast migration is critical to establish appropriate hyaloid morphology. High regional concentrations of VEGFA120, coupled with a high density of precursors, disrupts normal plexus formation, as no effective concentration gradient exists on either the lens or retinal surface. This situation favours the formation of dilated tortuous vessels, similar to that described in VEGF120/120 knock-in mice [42] and in the chick chorioallantois following administration of VEGFA120 homo-dimer [43]. In contrast, both \(\hbox{VEGFA}{_{164\&188}}\) transgenics are exposed to strong concentration gradients, which are highest on the lens surface, promoting endothelial spreading and capillary formation on the capsule and the formation of large sac-like vessel structures, typical in situations of VEGFA164/165 injection or over-expression [44, 45]. Similarly, long-term administration of VEGFA164 leads to persistence of these aberrant vessels (this study; [15]), whereas conditional, short-term switching in heart and liver of mice results in inappropriately connected sac-like vessels that quickly resolve upon VEGFA164 withdrawal [46]. The spreading of preexisting endothelial precursors over an increased surface area and the formation of large “mother” vessels has been reported in various tissues of adult mice following the injection of adenovirus containing VEGFA165 [47] and in experimental tumours over-expressing this isoform [28]. It is thus possible that spatially defined, temporal expression of high concentrations of VEGFA are critical in the formation of large calibre blood vessels during normal embryonic development. The results of this study also suggest that an intimate association of the vasculature with basement membranes of organ rudiments, such as the lens capsule and the lung [7, 25], is likely to be mediated by the heparin-binding isoforms of VEGFA.
Pericytes, which regulate vessel maturation and survival, probably arise de novo from mesenchymal cells within the developing eye [48]. These cells are conspicuous in the hyperplastic hyaloid vasculature of all three lines of transgenic mice and despite the greatly increased levels of VEGFA, assume their normal locations on the ablumenal surface of the endothelium. Pericytes express VEGFR1&2 and neuropilin 1 [49], are known to proliferate in hypoxic conditions through the flt-1 receptor [50] and following vessel stabilisation become unresponsive to VEGF [51]. These observations are consistent with the contention that pericyte-endothelial cell fates are linked via VEGFA/PDGF-B recruitment [51], possibly mediated by the ability of pericytes to respond to \(\hbox{VEGFA}{_{164\&188}}\) directly [49)] through the flt-1 receptor [50]. In addition, an increasing body of evidence supports the hypothesis that heterotypic cell contact [52], in addition to endothelial cell production of platelet derived growth factor-B [53, 54] mediates the close relationship of pericytes and endothelium in addition to the structural stability of nascent capillaries. F4/80 positive macrophages are also detected in the eyes of wild-type and transgenic mice as soon as a differentiated vasculature is observed at E13.5. In all 3 types of VEGFA isoform transgenic mice, large numbers of F4/80 positive cells are located both external and internal to the vascular lacunae as well as within the structure of the wall, in contrast to the observations of Ash and Overbeek [15], where these cells were not observed until much later in development. While macrophages have been implicated in the programmed regression of the hyaloid vasculature in wild-type mice [55, 56] via the Wnt-3b pathway [57], the role of macrophages within the abnormally structured hyaloid vasculature of VEGFA transgenic mice is unclear, however, it is possible that these cells are responsible for the partial regression of the hyaloid vasculature in post-natal VEGFA188 transgenics.
Murine retinal vascular development begins 7 days later than the hyaloid vasculature at around birth [12, 58]. Retinal vascular expansion toward the optic rim is characterised by classic, branching angiogenesis, with growth and remodelling being determined by time-dependent VEGFA-mediated cues from the underlying astrocytes and matrix [59]. Normally these two plexuses are both morphologically and temporally distinct structures that regulate the growth and differentiation of the lens and retina, respectively. However, in both \(\hbox{VEGFA}{_{164\&188}}\) transgenic mice, the hyaloid vasculature has direct connections with the retinal vasculature, similar to the situation in VEGFA188/188 knock-in mice; whereas both VEGFA120 transgenics (this study) and VEGFA120/120 mice [12] no such inter-connections are observed. The retinal vascular phenotypes in VEGFA120 mice are consistent with the hypothesis that a preponderance of non-heparin-binding [8, 9] VEGFA matrix guidance cues, result in a reduction of plexus patterning and extent. Retinal vasculature from VEGFA120 transgenics is characterised by reduced venous and extremely poor arterial patterning, with few connecting capillaries. This finding is consistent with the suggestion that endothelial cells at the leading edge fail to form connections with neighbouring branches due to the decrease in filopodial extensions [20]. Particularly evident in retinal vessels of VEGFA120 mice are the increased numbers of large calibre vessels, presumably formed by recruitment of nascent endothelial cells [42]. One further possibility that may account for the differences in retinal vascular patterning observed in \(\hbox{VEGFA}{_{164\&188}}\) mice is the distribution of the VEGFA co-receptors neuropilin-1 (NRP-1) only found on arterial endothelial cells [60] and neuropilin-2 (NRP-2) which is venous specific. NRP-1 and NRP-2 form heterodimeric complexes with VEGF-R2 and specifically bind VEGFA165 (and possibly VEGFA188 which also contains the NRP-1 binding domain; [12]), but not VEGFA120 as this isoform lacks the NRP-1 binding domain [61]. The differential binding capabilities of NRP/VEGF-R2 complexes are believed to mediate plexus patterning as these receptors co-localise in areas of neovascularisation [62]. In VEGFA164 transgenics, vessel density around retinal arterioles is reduced and there is significant venular hypertrophy. In contrast to VEGF164/164 knock-in mice, where the retinal vasculature is morphologically indistinct from wild-type and total VEGFA levels are normal [12], greatly increased VEGFA164 levels favour venular hypertrophy, possibly mediated via excess VEGFA deposition in the astrocyte matrix which guides vascular pattern formation [59]. In VEGFA188 mice there is normal arteriolar but markedly increased capillary growth, particularly around venules, similar to the situation described in VEGFA188/188 knock-in mice [12]. As VEGFA188 is strongly membrane bound following secretion, the phenotypes resulting from over-expression of this splice-variant may arise via urokinase-mediated proteolytic cleavage into a shorter molecular weight isoform [63] capable of establishing a local concentration gradient. The numerous filopodia around the tips of leading edge endothelial cells in VEGFA188 transgenics, previously associated with fusion of these cells into large vessels [12, 42], is also consistent with this suggestion. In normal retinal development, the highest VEGF expression levels are detected surrounding the veins and labelling for VEGF protein displays strong deposition around veins [20]. Thus, loading the ILM with heparin-binding isoforms of \(\hbox{VEGFA}{_{164 \ {\rm and} \ 188}}\) or the astrocytic surface in large regions of the retinal plexus, may underlie the hyper-fusion and over-production of venous structures observed in these transgenic mice.
In addition to the ocular vascular malformations described in this study, several distinct pathologies in ocular tissue structure of VEGFA transgenic mice are apparent (Table 1). VEGFA120 results in a significant degree of sub-retinal haemorrhage, probably due to the accompanying retinal traction. The retinal rosetting and detachment from the underlying sclera, characteristic in VEGFA120 transgenics, may be mediated via VEGFR2 found on retinal ganglion cells [64]. In addition, corneal vascularisation is a serious complication of several ocular diseases as well as following corneal transplantation and is only a consistent feature in \(\hbox{VEGFA}{_{120\&164}}\) transgenic mice, perhaps warranting the investigation of the \(\hbox{VEGFA}{_{120\&164}}\) isoforms in the aetiology of these conditions. While the non-vascular malformations (summarised in Table 1) are beyond the scope of the present study, it is clear that both lens (probably indirectly through a tractional disturbance of lens development) and retinal malformations (directly via retinal ganglion cell VEGFR2) can be induced by over-production of VEGFA splice-variants. Retinal rosetting and detachment are common features of retinopathy of prematurity [65], a condition characterised by uncontrolled retinal vascular proliferation [66]. The effects of over-expression of VEGFA splice-variants on vascular leakage presented in this study (Table 1), i.e. that the more labile forms of \(\hbox{VEGFA}{_{120\&164}}\) promote vascular leakage and haemorrhage, is consistent with data describing the effects of transplanted tumour cell lines expressing \(\hbox{VEGF}{_{121,165\&189}}\) (the equivalent human splice-variants) on intra-cerebral associated tumour haemorrhage [45]. In addition, clinical evidence from solid tumours expressing the low molecular weight VEGFA splice-variants reveals severe haemorrhage and a poorer prognosis in these tumours [67].
The results of the present study support the hypotheses that over-expression of specific VEGFA isoforms induces distinct vascular morphologies in both the hyaloid and retinal vasculature. These results have implications for diseases associated with abnormal vascular growth, such as diabetic retinopathy and tumourigenesis. More specifically, VEGFA120 over-expression in murine eyes shows several of the features of the vascular patterning defects in retinopathy of prematurity and \(\hbox{VEGFA}{_{164\&188}}\) transgenics display features consistent with persistent hyperplastic primary vitreous, a human congenital condition in which hyperplastic hyaloid vasculature fails to regress [68]. Failure of the hyaloid vasculature to regress is a ubiquitous finding in congenital cataracts [69] whereas inappropriate retinal vascularisation, which is often associated with increased levels of intra-ocular VEGFA, is recognised as the leading cause of childhood blindness [70].
References
Carmeliet P, Ferreira V, Breier G, Pollefeyt S, Kieckens L, Gertsenstein M, Fahrig M, Vandenhoeck A, Harpal K, Eberhardt C, Declercq C, Pawling J, Moons L, Collen D, Risau W, Nagy A (1996) Abnormal blood vessel development and lethality in embryos lacking a single VEGF allele. Nature 380:435–439
Ferrara N, Carver-Moore K, Chen H, Dowd M, Lu L, O’Shea KS, Powell-Braxton L, Hillan KJ, Moore MW (1996) Heterozygous embryonic lethality induced by targeted inactivation of the VEGF gene. Nature 380:439–442
Haigh JJ, Gerber HP, Ferrara N, Wagner EF (2000) Conditional inactivation of VEGF-A in areas of collagen2a1 expression results in embryonic lethality in the heterozygous state. Development 127:1445–1453
Gerber HP, Hillan KJ, Ryan AM, Kowalski J, Keller GA, Rangell L, Wright BD, Radtke F, Aguet M, Ferrara N (1999) VEGF is required for growth and survival in neonatal mice. Development 126:1149–1159
Ferrara N, Houck K, Jakeman L, Leung DW (1992) Molecular and biological properties of the vascular endothelial growth factor family of proteins. Endocr Rev 13:18–32
Shima DT, Kuroki M, Deutsch U, Ng YS, Adamis AP, D’Amore PA (1996) The mouse gene for vascular endothelial growth factor. Genomic structure, definition of the transcriptional unit, and characterization of transcriptional and post-transcriptional regulatory sequences. J Biol Chem 271:3877–3883
Ng YS, Rohan R, Sunday ME, Demello DE, D’Amore PA (2001) Differential expression of VEGF isoforms in mouse during development and in the adult. Dev Dynam 220:112–121
Park JE, Keller GA, Ferrara N (1993) The vascular endothelial growth factor (VEGF) isoforms: differential deposition into the subepithelial extracellular matrix and bioactivity of extracellular matrix-bound VEGF. Mol Biol Cell 4:1317–1326
Keyt BA, Berleau LT, Nguyen HV, Chen H, Heinsohn H, Vandlen R, Ferrara N (1996) The carboxyl-terminal domain (111–165) of vascular endothelial growth factor is critical for its mitogenic potency. J Biol Chem 271:7788–7795
Forsten KE, Fannon M, Nugent MA (2000) Potential mechanisms for the regulation of growth factor binding by heparin. J Theor Biol 205:215–230
Carmeliet P, Ng YS, Nuyens D, Theilmeier G, Brusselmans K, Cornelissen I, Ehler E, Kakkar VV, Stalmans I, Mattot V, Perriard JC, Dewerchin M, Flameng W, Nagy A, Lupu F, Moons L, Collen D, Damore PA, Shima DT (1999) Impaired myocardial angiogenesis and ischemic cardiomyopathy in mice lacking the vascular endothelial growth factor isoforms VEGF(164) and VEGF(188). Nat Med 5:495–502
Stalmans I, Ng YS, Rohan R, Fruttiger M, Bouche A, Yuce A, Fujisawa H, Hermans B, Shani M, Jansen S, Hicklin D, Anderson DJ, Gardiner T, Hammes HP, Moons L, Dewerchin M, Collen D, Carmeliet P, D’Amore PA (2002) Arteriolar and venular patterning in retinas of mice selectively expressing VEGF isoforms. J Clin Invest 109:327–336
Maes C, Carmeliet P, Moermans K, Stockmans I, Smets N, Collen D, Bouillon R, Carmeliet G (2002) Impaired angiogenesis and endochondral bone formation in mice lacking the vascular endothelial growth factor isoforms VEGF(164) and VEGF(188). Mech Dev 111:61–73
Overbeek PA, Chepelinsky AB, Khillan JS, Piatigorsky J, Westphal H (1985) Lens-specific expression and developmental regulation of the bacterial chloramphenicol acetyltransferase gene driven by the murine alpha A-crystallin promoter in transgenic mice. Proc Natl Acad Sci USA 82:7815–7819
Ash JD, Overbeek PA (2000) Lens-specific VEGF-A expression induces angioblast migration and proliferation and stimulates angiogenic remodeling. Dev Biol 223:383–398
Mitchell CA, Risau W, Drexler HCA (1998) Regression of vessels in the tunica vasculosa lentis is initiated by coordinated endothelial apoptosis: a role for vascular endothelial growth factor as a survival factor for endothelium. Dev Dynam 213:322–333
Reneker LW, Silversides DW, Patel K, Overbeek PA (1995) TGF alpha can act as a chemoattractant to perioptic mesenchymal cells in developing mouse eyes. Development 121:1669–1680
Hovey RC, Goldhar AS, Baffi J, Vonderhaar BK (2001) Transcriptional regulation of vascular endothelial growth factor expression in epithelial and stromal cells during mouse mammary gland development. Mol Endocrinol 15:819–831
Marti HJ, Bernaudin M, Bellail A, Schoch H, Euler M, Petit E, Risau W (2000) Hypoxia-induced vascular endothelial growth factor expression precedes neovascularization after cerebral ischemia. Am J Pathol 156:965–976
Gerhardt H, Golding M, Fruttiger M, Ruhrberg C, Lundkvist A, Abramsson A, Jeltsch M, Mitchell C, Alitalo K, Shima D, Betsholtz C (2003) VEGF guides angiogenic sprouting utilizing endothelial tip cell filopodia. J Cell Biol 161:1163–1177
Kretzler M, Schroppel B, Merkle M, Huber S, Mundel P, Horster M, Schlondorff D (1998) Detection of multiple vascular endothelial growth factor splice isoforms in single glomerular podocytes. Kidney Int 54:S159–S161
Halder JB, Zhao X, Soker S, Paria BC, Klagsbrun M, Das SK, Dey SK (2000) Differential expression of VEGF isoforms and VEGF(164)-specific receptor neuropilin-1 in the mouse uterus suggests a role for VEGF(164) in vascular permeability and angiogenesis during implantation. Genesis 26:213–224
Krussel JS, Behr B, Milki AA, Hirchenhain J, Wen Y, Bielfeld P, Lake Polan M (2001) Vascular endothelial growth factor (VEGF) mRNA splice variants are differentially expressed in human blastocysts. Mol Hum Reprod 7:57–63
Simon M, Grone HJ, Johren O, Kullmer J, Plate KH, Risau W, Fuchs E (1995) Expression of vascular endothelial growth-factor and its receptors in human renal ontogeny and in adult kidney. Am J Physiol Renal Fluid Electrolyte Physiol 37:F240–F250
Cheung N, Wong MP, Yuen ST, Leung SY, Chung LP (1998) Tissue-specific expression pattern of vascular endothelial growth factor isoforms in the malignant transformation of lung and colon. Hum Pathol 29:910–914
Okamoto K, Oshika Y, Fukushima Y, Ohnishi Y, Tokunaga T, Tomii Y, Kijima H, Yamazaki H, Ueyama Y, Tamaoki N, Nakumura M (1999) Xenografts of human solid tumors frequently express cellular-associated isoform of vascular endothelial growth factor (VEGF) 189. Oncol Rep 6:1201–1204
Grunstein J, Masbad JJ, Hickey R, Giordano F, Johnson RS (2000) Isoforms of vascular endothelial growth factor act in a coordinate fashion to recruit and expand tumor vasculature. Mol Cell Biol 20:7282–7291
Yu JL, Rak JW, Klement G, Kerbel RS (2002) Vascular endothelial growth factor isoform expression as a determinant of blood vessel patterning in human melanoma xenografts. Cancer Res 62:1838–1846
Tober KL, Cannon RE, Spalding JW, Oberyszyn TM, Parrett ML, Rackoff AI, Oberyszyn AS, Tennant RW, Robertson FM (1998) Comparative expression of novel vascular endothelial growth factor vascular permeability factor transcripts in skin, papillomas, and carcinomas of v-Ha-ras Tg.AC transgenic mice and FVB/N mice [Full text delivery]. Biochem Biophys Res Commun 247:644–653
Mann IC (1964) The development of the human eye. Grune and Stratton Inc., New York
Balazs EA, Toth LZ, Ozanics V (1980) Cytological studies on the developing vitreous as related to the hyaloid vessel system. Albrecht Von Graefes Archiv fur Klinische und Experimentelle Ophthalmologie 213:71–85
Lang R (1997) Apoptosis in mammalian eye development: lens morphogenesis, vascular regression and immune privilege. Cell Death Differ 4:12–20
de Iongh R, McAvoy JW (1992) Distribution of acidic and basic fibroblast growth factors (FGF) in the foetal rat eye: implications for lens development. Growth Factors 6:159–177
Parmigiani CM, McAvoy JW (1989) A morphometric analysis of the development of the rat lens capsule. Curr Eye Res 8:1271–1277
Davies MJ, Mitchell CA, Maley MAL, Grounds MD, Harvey AR, Plant GW, Wood DJ, Hong Y, Chirila TV (1997) In vitro assessment of the biological activity of basic fibroblast growth factor released from various polymers and biomatrices. J Biomater Appl 12:31–56
Mudhar HS, Pollock RA, Wang C, Stiles CD, Richardson WD (1993) PDGF and its receptors in the developing rodent retina and optic nerve. Development 118:539–552
Robinson ML, Overbeek PA, Verran DJ, Grizzle WE, Stockard CR, Friesel R, Maciag T, Thompson JA (1995) Extracellular FGF-1 acts as a lens differentiation factor in transgenic mice. Development 121:505–514
Lovicu FJ, Overbeek PA (1998) Overlapping effects of different members of the FGF family on lens fiber differentiation in transgenic mice. Development 125:3365–3377
Reneker LW, Overbeek PA (1996) Lens-specific expression of PDGF-A alters lens growth and development. Dev Biol 180:554–565
Cleaver O, Krieg PA (1998) VEGF mediates angioblast migration during development of the dorsal aorta in Xenopus. Development 125:3905–3914
Shoji W, Isogai S, Sato-Maeda M, Obinata M, Kuwada JY (2003) Semaphorin3a1 regulates angioblast migration and vascular development in zebrafish embryos. Development 130:3227–3236
Ruhrberg C, Gerhardt H, Golding M, Watson R, Ioannidou S, Fujisawa H, Betsholtz C, Shima DT (2002) Spatially restricted patterning cues provided by heparin-binding VEGF-A control blood vessel branching morphogenesis. Genes Dev 16:2684–2698
Wilting J, Birkenhager R, Eichmann A, Kurz H, Martiny-Baron G, Marme D, McCarthy JE, Christ B, Weich HA (1996) VEGF121 induces proliferation of vascular endothelial cells and expression of flk-1 without affecting lymphatic vessels of chorioallantoic membrane. Dev Biol 176:76–85
Drake CJ, Little CD (1995) Exogenous vascular endothelial growth factor induces malformed and hyperfused vessels during embryonic neovascularization. Proc Natl Acad Sci USA 92:7657–7661
Cheng SY, Nagane M, Huang HJS, Cavenee WK (1997) Intracerebral tumor-associated hemorrhage caused by overexpression of the vascular endothelial growth factor isoforms VEGF(121) and VEGF(165) but not VEGF(189). Proc Natl Acad Sci USA 94:12081–12087
Dor Y, Djonov V, Abramovitch R, Itin A, Fishman GI, Carmeliet P, Goelman G, Keshet E (2002) Conditional switching of VEGF provides new insights into adult neovascularization and pro-angiogenic therapy. EMBO J 21:1939–1947
Pettersson A, Nagy JA, Brown LF, Sundberg C, Morgan E, Jungles S, Carter R, Krieger JE, Manseau EJ, Harvey VS, Eckelhoefer IA, Feng D, Dvorak AM, Mulligan RC, Dvorak HF (2000) Heterogeneity of the angiogenic response induced in different normal adult tissues by vascular permeability factor/vascular endothelial growth factor. Lab Invest 80:99–115
Beck L Jr, D’Amore PA (1997) Vascular development: cellular and molecular regulation. Faseb J 11:365–373
Ishida A, Murray J, Saito Y, Kanthou C, Benzakour O, Shibuya M, Wijelath ES (2001) Expression of vascular endothelial growth factor receptors in smooth muscle cells. J Cell Physiol 188:359–368
Yamagishi S, Yonekura H, Yamamoto Y, Fujimori H, Sakurai S, Tanaka N, Yamamoto H (1999) Vascular endothelial growth factor acts as a pericyte mitogen under hypoxic conditions. Lab Invest 79:501–509
Benjamin LE, Hemo I, Keshet E (1998) A plasticity window for blood vessel remodelling is defined by pericyte coverage of the preformed endothelial network and is regulated by PDGF- B and VEGF. Development 125:1591–1598
Hirschi KK, Rohovsky SA, Beck LH, Smith SR, D’Amore PA (1999) Endothelial cells modulate the proliferation of mural cell precursors via platelet-derived growth factor-BB and heterotypic cell contact. Circ Res 84:298–305
Lindahl P, Hellstrom M, Kalen M, Betsholtz C (1998) Endothelial-perivascular cell signaling in vascular development: lessons from knockout mice. Curr Opin Lipidol 9:407–411
Lindblom P, Gerhardt H, Liebner S, Abramsson A, Enge M, Hellstrom M, Backstrom G, Fredriksson S, Landegren U, Nystrom HC, Bergstrom G, Dejana E, Ostman A, Lindahl P, Betsholtz C (2003) Endothelial PDGF-B retention is required for proper investment of pericytes in the microvessel wall. Genes Dev 17:1835–1840
Diez-Roux G, Lang RA. (1997) Macrophages induce apoptosis in normal cells in vivo. Development 124:3633–3638
Diez-Roux G, Argilla M, Makarenkova H, Ko K, Lang RA (1999) Macrophages kill capillary cells in G1 phase of the cell cycle during programmed vascular regression. Development 126:2141–2147
Lobov IB, Rao S, Carroll TJ, Vallance JE, Ito M, Ondr JK, Kurup S, Glass DA, Patel MS, Shu W, Morrisey EE, McMahon AP, Karsenty G, Lang RA (2005) WNT7b mediates macrophage-induced programmed cell death in patterning of the vasculature. Nature 437:417–421
Fruttiger M (2002) Development of the mouse retinal vasculature: angiogenesis versus vasculogenesis. Invest Ophthalmol Vis Sci 43:522–527
Stone J, Itin A, Alon T, Pe’er J, Gnessin H, Chan-Ling T, Keshet E (1995) Development of retinal vasculature is mediated by hypoxia-induced vascular endothelial growth factor (VEGF) expression by neuroglia. J Neurosci 15:4738–4747
Klagsbrun M, Takashima S, Mamluk R (2002) The role of neuropilin in vascular and tumor biology. Adv Exp Med Biol 515:33–48
Soker S, Takashima S, Miao HQ, Neufeld G, Klagsbrun M (1998) Neuropilin-1 is expressed by endothelial and tumor cells as an isoform-specific receptor for vascular endothelial growth factor. Cell 92:735–745
Ishihama H, Ohbayashi M, Kurosawa N, Kitsukawa T, Matsuura O, Miyake Y, Muramatsu T (2001) Colocalization of neuropilin-1 and Flk-1 in retinal neovascularization in a mouse model of retinopathy. Invest Ophthalmol Vis Sci 42:1172–1178
Plouet J, Moro F, Bertagnolli S, Coldeboeuf N, Mazarguil H, Clamens S, Bayard F (1997) Extracellular cleavage of the vascular endothelial growth factor 189-amino acid form by urokinase is required for its mitogenic effect. J Biol Chem 272:13390–13396
Ogata N, Yamanaka R, Yamamoto C, Miyashiro M, Kimoto T, Takahashi K, Maruyama K, Uyama M (1998) Expression of vascular endothelial growth factor and its receptor, KDR, following retinal ischemia-reperfusion injury in the rat. Curr Eye Res 17:1087–1096
Stout AU, Stout JT (2003) Retinopathy of prematurity. Pediatr Clin North Am 50:77–87, vi
Alon T, Hemo I, Itin A, Pe’er J, Stone J, Keshet E (1995) Vascular endothelial growth factor acts as a survival factor for newly formed retinal vessels and has implications for retinopathy of prematurity. Nat Med 1:1024–1028
Zhang HT, Scott PA, Morbidelli L, Peak S, Moore J, Turley H, Harris AL, Ziche M, Bicknell R (2000) The 121 amino acid isoform of vascular endothelial growth factor is more strongly tumorigenic than other splice variants in vivo. Br J Cancer 83:63–68
Silbert M, Gurwood AS (2000) Persistent hyperplastic primary vitreous. Clin Eye Vis Care 12:131–137
Mullner-Eidenbock A, Amon M, Moser E, Klebermass N (2004) Persistent fetal vasculature and minimal fetal vascular remnants: a frequent cause of unilateral congenital cataracts. Ophthalmology 111:906–913
Campochiaro PA (2000) Retinal and choroidal neovascularization. J Cell Physiol 184:301–310
Acknowledgements
The authors wish to thank Mrs. M. Mitchell for expert animal care, Dr. Karim Bakri for sample processing, as well as Mr. Trevor Gray and Phillip Hinson for assistance with electron microscopy. We thank G. Breier for VEGF isoform plasmids, P. Overbeek for the CPV2 plasmid as well as L.A.G. Lucas and N.J. Duffin for assistance with microscopy. H. Gerhardt was supported by an EMBO fellowship.
Author information
Authors and Affiliations
Corresponding author
Additional information
Werner Risau: Deceased 13 December 1998
Rights and permissions
About this article
Cite this article
Mitchell, C.A., Rutland, C.S., Walker, M. et al. Unique vascular phenotypes following over-expression of individual VEGFA isoforms from the developing lens. Angiogenesis 9, 209–224 (2006). https://doi.org/10.1007/s10456-006-9056-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10456-006-9056-7