Abstract
Bioaerosols are major air pollutants commonly found both indoors and outdoors. High exposure levels may result in various adverse health outcomes. Laboratories, which are indoor environments carefully designed for specific purposes, may contain high levels of bioaerosols, which may threaten worker’s health, and contaminate experimental results. This study investigated the levels of bioaerosols (i.e., culturable fungi and bacteria, and fungal spores) in laboratories in the Bangkok metropolitan area. Air samples were collected from 14 Class I and one Class II laboratories by using a single-stage impactor and a VersaTrap spore trap cassette. Colonies were counted after 72 h and 48 h of incubation for culturable fungi and bacteria, respectively. Culturable fungi and fungal spores were identified based on their morphological characteristics. Associations between bioaerosols and indoor air parameters and laboratory characteristics were evaluated. The concentrations (mean ± SD) of culturable bacteria, culturable fungi, and fungal spores were 87.0 ± 97.8 CFU/m3, 294.9 ± 376.1 CFU/m3, and 771.8 ± 545.3 spores/m3, respectively. Aspergillus/Penicillium, ascospores, and Cladosporium were common fungal spore taxa in the laboratories. Culturable fungi significantly increased with the number of staff and visible molds, whereas water leaks and culturable fungi significantly increased fungal spore concentrations. Culturable bacteria were positively associated with the numbers of trash bins and − 80 °C freezers. Although bioaerosol concentrations were considerably lower in the studied laboratories, proper indoor air management is still suggested in order to reduce emissions and exposure. This can help workers avoid adverse health outcomes and reduce the chance of experimental contamination.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
Bioaerosols are prevalent in the indoor environment including various forms of cells, toxins, and metabolites generated by microorganisms, arthropods, animals, and plants (Burge 2003; Macher 1999). In addition to other indoor air pollutants such as particulate matter (PM) and volatile organic compounds, bioaerosols are considered health hazards. Exposure to indoor bioaerosols has been proved to cause adverse health outcomes such as respiratory diseases, asthma, decrease in lung function, allergic diseases, and sick building symptoms (Adhikari et al. 2011; Chao et al. 2003; Chen et al. 2011, 2014; Vesper et al. 2013).
In specific occupational environments, workers have higher chances of exposure to bioaerosols. A study conducted in Croatia revealed that exposure to fungi and mites in poultry farms was associated with respiratory and allergic diseases (Rimac et al. 2010). Similar results were reported by a study in Taiwan that discovered that exposure to high fungal levels in mushroom and vegetable farms was significantly associated with decline in lung function among workers (Tarigan et al. 2017). Adverse health outcomes from bioaerosol exposure have also been observed in office environments. A US study conducted in Boston, Massachusetts, demonstrated a positive association between fungal exposure and work-related symptoms, such as upper respiratory and non-specific symptoms (Chao et al. 2003).
In laboratories, especially those specializing in biological work, workers have a relatively high chance of being exposed to bioaerosols. The substances they are expose to include bioaerosols, which may be introduced from outdoors or a contaminated ventilation system, and from handling biological samples (Hwang et al. 2013, 2017). In addition to creating adverse health outcomes, these agents can contaminate work performed in the laboratory. Poor indoor air quality (IAQ) (e.g., low ventilation rate, high humidity, and high temperature) can facilitate the growth of microorganisms (Alves et al. 2016; Balasubramanian et al. 2012; Knudsen et al. 2017). Furthermore, human activity can promote the release and resuspension of these bioaerosols (Adams et al. 2013; Heo et al. 2017).
In this study, we investigated the distributions and characteristics of bioaerosols and IAQ in laboratories in the Bangkok metropolitan area in Thailand. The indoor air parameters and characteristics that may influence bioaerosol concentrations were recorded, and the associations between these parameters were evaluated.
2 Materials and methods
2.1 Study design
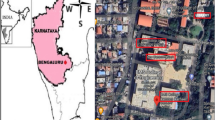
This cross-sectional study was conducted during July and August 2017. Duplicate air samples were collected from university and research institute laboratories. Outdoor air samples were also collected as a reference. The IAQ parameters and laboratory characteristics were recorded concurrently. The associations between bioaerosol levels and IAQ parameters were examined.
2.2 Bioaerosol sampling
2.2.1 Culturable fungi and bacteria
The sampling was performed during the regular practice of each laboratory on a weekday. Sampler was placed on the laboratory bench in the middle of each laboratory. Duplicate air samples were collected from each laboratory using an SKC BioStage impactor for viable fungi and bacteria connected to an air suction pump SKC QuickTake 30 (SKC Inc., PA, USA) with a flow rate of 28.3 L/min for 2 min. Culturable bacteria were collected on Typtic Soy Agar (TSA) and incubated at 30 °C for 48 h. Each colony was counted, and the concentration was reported as colony-forming units per air volume sampled (CFU/m3). Culturable fungi were collected on Malt Extract Agar (MEA) and incubated at room temperature for 72 h. The colonies were counted and also reported as CFU/m3. Fungal colonies were subsequently identified to the level possible by a light microscope (generally to the genus level) based on their morphological characteristics.
2.2.2 Fungal spores
Fungal spores were collected using a VersaTrap spore trap cassette (SKC Inc., PA, USA) connected with an SKC QuickTake 30 with a flow rate of 15 L/min and sampled for 15 min. Samples were stained using phenol–safranin–glycerin jelly, covered with a cover glass, and sealed with clear nail polish (Rogers and Muilenberg 2001). Spores were counted and identified based on their morphological characteristics following the guidelines of the American Academy of Allergy, Asthma and Immunology (Lin et al. 2004; Muilenberg 1999; Smith 2000). The concentration was reported as spores/m3.
2.3 Indoor air parameters
Indoor air parameters were monitored for 30 min in each laboratory concurrently with bioaerosol sampling. Temperature (°C) and relative humidity (RH, %) were monitored using the Air Quality Monitor TES-5322 (TES Electrical Electronic Corp., Taipei, Taiwan). PM with the aerodynamic ≤ 10 and ≤ 2.5 μm (PM10 and PM2.5) was monitored using the DustTrak DRX Aerosol Monitor 8533 (TSI Inc., MN, USA).
2.4 Laboratory characteristics
During the air sampling, personnel in each laboratory were interviewed on laboratory characteristics. Questions included the types of experiments conducted (e.g., biology, chemistry, microbiology), visible mold on the ceiling or walls, number of years the laboratory had been in operation, the number of staff, the number of waste collection bins (both general and biohazard waste), the number of refrigerators and freezers, and the type of ventilation.
2.5 Data analysis
The difference between indoor and outdoor bioaerosol concentrations was tested using the Mann–Whitney U test. Spearman’s correlation coefficient was used to determine the correlations between bioaerosols and IAQ parameters. Univariate regression analysis was used to investigate the association between bioaerosols and each parameter. The parameter with a p value ≤ 0.2 was chosen for further multivariate analysis. A multiple regression model for each bioaerosol taxon was built using general linear model (PROC GLM) in SAS version 9.2 (SAS Institute, Cary, NC, USA). The final regression models included only the variables with p < 0.05. To approximate the normality of bioaerosol distribution, the bioaerosol concentrations were log 10-transformed before the regression analyses.
3 Results
Bioaerosols were collected from 15 laboratories at three universities and one research institute. Most of the laboratories were involved in biological and chemical work and had been operating for 3 months to 20 years. Most biological-related laboratories are Class I laboratories equipped with biological safety cabinet Class II, except laboratory No. D3 which is a Class II laboratory. The chemistry laboratories are Class I equipped with chemical fume hood and no biological sample handling. Only trained personnel were present in the laboratories. General information of each laboratory is presented in Table 1. Bioaerosol concentrations are listed in Table 2. The average concentrations (mean ± SD) of culturable bacteria, culturable fungi, and fungal spores in the laboratories were 87.0 ± 97.8 CFU/m3, 294.9 ± 376.1 CFU/m3, and 771.8 ± 545.3 spores/m3, respectively. Mann–Whitney U test results indicated that the concentrations of indoor bioaerosols were lower than those of outdoor bioaerosols (p < 0.05). The distributions of bioaerosols are illustrated in Fig. 1.
Aspergillus/Penicillium spores were the most abundant fungal spore taxa in the laboratories (40.62%), followed by Cladosporium (30%) and ascospores (17%). In outdoor environment, by contrast, ascospores were the most abundant taxon (30.4%). The percentages of each fungal spore taxon recovered from the air samples both indoors and outdoors are illustrated in Fig. 2. Cladosporium, Aspergillus, and Penicillium were also the most abundant taxa in the culture-based method. However, the concentrations were lower than those of non-sporulating fungi that could not be identified based on morphology (Fig. 3). The levels of fungal spores and culturable fungi between biological and chemical laboratories were not significantly different. However, we observed slightly higher concentrations of Cladosporium spp. in microbiology laboratories compared to others (data not shown). The most prevalent fungal taxa were comparable in biological and chemical laboratories.
Temperature in all laboratories was relatively constant at approximately 24–25 °C, but PM10, PM2.5, and RH varied among laboratories (Table 3). Spearman’s correlation coefficient revealed that indoor culturable fungi and fungal spores were both significantly associated with PM10 with r = 0.582 and 0.565, respectively, whereas other IAQ parameters were not correlated (Table 4).
Table 5 shows the associations between bioaerosols and other variables through multiple regression analysis. After adjustment for the number of operating years, the results indicated that concentrations of bioaerosols were associated with laboratory characteristics rather than environmental parameters. The number of staff and visible mold was positively associated with culturable fungi, whereas the number of − 80 °C freezers and general trash bins was associated with culturable bacteria. Additionally, the fungal spore level was correlated with the concentration of culturable fungi and evidence of water leaks. The coefficients of determination (R2) were 0.72, 0.56, and 0.93 for culturable fungi, culturable bacteria, and fungal spores, respectively.
4 Discussion
Contamination in the laboratories affects both occupants’ health and experimental results. Our study used air impactors to investigate levels of bioaerosols in laboratories in the Bangkok metropolitan area and demonstrated that the concentrations were associated with laboratory characteristics rather than the environmental parameters.
The bioaerosol concentrations varied among the sampling sites. The mean concentrations of culturable fungi and bacteria levels were 294.9 ± 376.1 CFU/m3 and 87.0 ± 97.8 CFU/m3, respectively. Compared with studies conducted in Korea that collected air samples from various types of laboratories, our results revealed lower concentrations of airborne culturable bacteria, but higher concentrations of culturable fungi (Hwang et al. 2013; 2018; Hwang et al. 2011b; Hwang et al. 2017). These differences were potentially caused by the main activities of the sampling sites, because the Korean studies investigated animal laboratories (i.e., mice and rabbits) and biowaste sites which usually contain more waste and release more microorganisms into the air. Studies in Thailand (Luksamijarulkul et al. 2014) and France (Sautour et al. 2009) that collected air samples in the clinical laboratories reported lower airborne bacterial and higher fungal concentrations that resembled the findings of our study. Although their bacterial concentrations were higher than those observed in our study, they were still relatively low because most clinical laboratories regularly disinfect their facilities.
The concentrations in the laboratories we studied were noticeably lower than those in most IAQ studies that sampled bioaerosol levels in residences and other public spaces in various regions (Basilico et al. 2007; Hsu et al. 2011, 2012; Salonen et al. 2015). This difference is clearly the result of the human activities and space management that influence the growth and resuspension of bioaerosols (Heo et al. 2017; Wu et al. 2005). Laboratories are designed for specific purposes, and only laboratory personnel are allowed to enter. Therefore, major bioaerosol contributors are limited to a few potential sources, such as the handling samples, improper laboratory practices, and poor IAQ management. In this study, the concentrations of bioaerosols observed indoors were significantly lower than those observed outdoors in similar studies (Adams et al. 2013; Codina et al. 2008; Haas et al. 2014; Jara et al. 2017). This finding was expected, because the outdoor environment teems with various bioaerosol sources, and no major biological contamination was observed at our sampling sites. However, low outdoor concentrations may be observed during the winter months when the ambient temperature is much lower than that of the indoor (Sautour et al. 2009).
Various fungal spore taxa were observed in laboratory environments in this study. These taxa are commonly observed in normal indoor environments where no water damage is reported (Codina et al. 2008; Gonçalves et al. 2010). Aspergillus/Penicillium, Cladosporium, and ascospores were the most abundant taxa recovered in every sample with large proportions. Unlike studies in the USA and Europe that discovered Alternaria as the most prevalent fungal taxon both indoors and outdoors (Aira et al. 2013; Fernández-Rodríguez et al. 2014; O’Connor et al. 2014; Sabariego et al. 2000; Tang 2009), Alternaria accounted for only 0.16% and 0.24% of indoor and outdoor samples, respectively, in our study. Similar to outdoor air samples, Aspergillus/Penicillium, Cladosporium, and ascospores were the most dominant taxa, but with different proportions. Ascospores were the most abundant taxon outdoors, followed by Aspergillus/Penicillium and Cladosporium. Additionally, we observed a higher proportion of basidiospores (14.6%) in the outdoor samples with more diverse fungal taxa compared to indoor samples. This probably resulted from the more diverse sources of fungi and factors related to the release of spores outdoors, leading to greater fungal diversity (Fernández-Rodríguez et al. 2015; Lymperopoulou et al. 2016; Rathnayake et al. 2017; Sadys et al. 2014). Fungal diversity varies seasonally, and in winter it may become greater indoors than outdoors. However, in Bangkok, outdoor temperatures are higher than indoor temperatures year-round. Hence, this finding may be observed consistently throughout the year (Adams et al. 2013). These fungal spores reflected the observed genera of culturable fungi, because we also noted Cladosporium and non-sporulating fungi most frequently in our samples. These non-sporulating fungi are probably ascomycetes, which usually not produce spores on MEA medium. However, the proportions of the Aspergillus spp. and Penicillium spp. in culturable samples were still lower compared to those observed in spore counts. This discrepancy is probably because a large proportion of Aspergillus spp. and Penicillium spp. are no longer viable and cannot grow on the culture media. Also a number of other fungal genera which have similar spore morphological characteristics may be identified as Aspergillus/Penicillium on spore count samples. It might also in part result from the different sampling flow rates and sampling time for the two samplers, i.e., BioStage and VersaTrap, which could affect the cut off size of fungal spores and fragments, as well as different exposure time. Therefore, the proportions of this group of fungal spores and culturable fungi were discordant.
Our study investigated the correlations between indoor bioaerosols and other environmental parameters (outdoor bioaerosols, temperature, RH, and PM) and initially hypothesized that indoor bioaerosols would be accompanied by outdoor bioaerosols, as in other studies (Gonçalves et al. 2010; Hargreaves et al. 2003; Rajasekar and Balasubramanian 2011). However, according to the Spearman’s correlation analyses, only PM10 was significantly correlated with fungal spores (r = 0.582, p < 0.05). This correlation was not observed in PM2.5, though PM2.5 is a constituent of PM10. Temperature and RH were initially expected to significantly correlate with indoor bioaerosols, but no correlation was observed in our study. This potentially resulted from most laboratories keeping their indoor temperature at approximately 25 °C throughout the day. Therefore, no correlation with temperature was observed.
We further investigated the associations between bioaerosols and other variables by using multiple regressions. We hypothesized that older laboratories should exhibit higher concentrations of bioaerosols. Therefore, we adjusted the age of the laboratory in the final model to avoid this effect and focused on the effects of other variables. After adjustment, the laboratory characteristics remained significant in the final models. The number of staff and visible molds was significantly associated with culturable fungi. The number of occupants and their activities has been proved to influence bioaerosol levels, especially airborne bacteria (Adams et al. 2014; Heo et al. 2017). Visible mold is likewise a critical factor associated with indoor fungal levels and their community (Crawford et al. 2015; Rosenbaum et al. 2010; Sordillo et al. 2010). Visible molds at home are reportedly associated with childhood asthma (Chen et al. 2014; Hwang et al. 2011a; Seo et al. 2014; Vesper et al. 2013). In this study, the ventilation type might also play an important role in bioaerosol levels. However, we did not observe a significant correlation between the ventilation type and bioaerosol levels (data not shown). This is probably because most laboratories (13 out of 15) in our study had the same ventilation type (split type AC), while the other two types had only one laboratory each. The impact of ventilation types should be further evaluated with more sampling sites.
Water leaks can increase the moisture in the air, supporting the growth of fungi in the area of the leak. Fungi can release spores into the environment after absorbing the moisture as well as through air disturbance (Burge and Rogers 2000), resulting in a high concentration of spores in the air. However, in our regression model, we did not observe an association between RH and fungal spores. This is probably because the amount of leaked water was sufficient to increase humidity only in the area of the leak, not in the whole laboratory. In the multiple regression model, the fungal spore level was also determined by the culturable fungal level. Because culturable fungi are a subgroup of total airborne fungal spores, identifying the level of this subgroup can determine the total airborne spores in this environment.
In the case of culturable bacteria, we expected a positive association with the number of staff, as described previously by Heo et al. (2017), but this was not observed in our final regression model. The numbers of − 80 °C freezers and general trash bins in the laboratory were the major predictors of culturable bacteria in this study. These variables reflect the main characteristic of the laboratory, such as the type of experiments, sample storage and handling, and waste collection. These processes may aerosolize bacterial particles, resulting in a high concentration of bacteria. However, the R2 of the model is only 56%. It is likely that other variables that influence bacterial levels were not measured in our study (Adams et al. 2014; Balasubramanian et al. 2012; Hwang et al. 2018). In this part of analysis, we did not further analyze bacterial genera because of limited resources. Detailed bacterial categories may be able to better explain the sources in laboratories.
In this study, we investigated bioaerosol concentrations in laboratories using both culture- and non-culture-based methods. The use of both methods improved our understanding of bioaerosol distributions and characteristics. Because the laboratories were engaged in work, we could not sample for more than 30 min at each location. In addition, we sampled at only a relatively small proportion of laboratories in the Bangkok area. However, our sampling included a variety of types of laboratories, and our sampling sites were dispersed throughout the Bangkok area and in the three major types of city environments: a downtown with high-rise buildings, an urban area with parks, and suburb near major expressways. This should minimize potential bias regarding the spatial variation in bioaerosols.
5 Conclusions
We conducted a cross-sectional study to investigate bioaerosol levels in laboratories in Bangkok, Thailand. Laboratory characteristics (i.e., visible mold; water leak; and the numbers of occupants, freezers, and trash bins) were the main predictors in our study. Average bioaerosol concentrations were lower than the maxima specified in standards and guidelines implemented in many other countries (Balasubramanian et al. 2012; IAQ Information Centre 2003; Heo et al. 2017; Maryam et al. 2015). Although no guidelines for bioaerosol concentrations have been implemented in Thailand, the baseline data gathered by this study will assist in the proper management of IAQ. Periodic inspections are encouraged to keep the laboratories free of major contamination. Additionally, temperature, humidity, and proper ventilation controls are essential for reducing bioaerosol concentrations, although these variables were not significant in our regression analyses. Proper management will help reduce contamination during experiment, reduce occupants’ exposure, and avoid adverse health outcomes.
References
Adams, R. I., Miletto, M., Lindow, S. E., Taylor, J. W., & Bruns, T. D. (2014). Airborne bacterial communities in residences: Similarities and differences with fungi. PLoS ONE, 9(3), e91283.
Adams, R. I., Miletto, M., Taylor, J. W., & Bruns, T. D. (2013). Dispersal in microbes: Fungi in indoor air are dominated by outdoor air and show dispersal limitation at short distances. ISME Journal, 7(7), 1262–1273.
Adhikari, A., Gupta, J., Wilkins, J. R., III, Olds, R. L., Indugula, R., Cho, K. J., et al. (2011). Airborne microorganisms, endotoxin, and (1/3)-b-D-glucan exposure in greenhouses and assessment of respiratory symptoms among workers. Annals of Occupational Hygiene, 55(3), 272–285.
Aira, M.-J., Rodríguez-Rajo, F.-J., Fernández-González, M., Seijo, C., Elvira-Rendueles, B., Abreu, I., et al. (2013). Spatial and temporal distribution of Alternaria spores in the Iberian Peninsula atmosphere, and meteorological relationships: 1993–2009. International Journal of Biometeorology, 57(2), 265–274.
Alves, C., Duarte, M., Ferreira, M., Alves, A., Almeida, A., & Cunha, Â. (2016). Air quality in a school with dampness and mould problems. Air Quality, Atmosphere and Health, 9(2), 107–115.
Balasubramanian, R., Nainar, P., & Rajasekar, A. (2012). Airborne bacteria, fungi, and endotoxin levels in residential microenvironments: A case study. Aerobiologia, 28(3), 375–390.
Basilico, M.d.l. L. Z, Chiericatti, C., Aringoli, E. E., Althaus, R. L., & Basilico, J. C. (2007). Influence of environmental factors on airborne fungi in houses of Santa Fe City, Argentina. Science of the Total Environment, 376(1–3), 143–150.
Burge, H. A. (2003). Bioaerosols and the scientific method. Annals of Allergy, Asthma & Immunology, 91(3), 217–219.
Burge, H. A., & Rogers, C. A. (2000). Outdoor allergens. Environmental Health Perspectives, 108, 653–659.
Chao, H. J., Schwartz, J., Milton, D. K., & Burge, H. A. (2003). The work environment and workers’ health in four large office buildings. Environmental Health Perspectives, 111(9), 1242–1248.
Chen, C.-H., Chao, H. J., Chan, C.-C., Chen, B.-Y., & Guo, Y. L. (2014). Current asthma in schoolchildren is related to fungal spores in classrooms. Chest, 146(1), 123–134.
Chen, B.-Y., Chao, H. J., Chan, C.-C., Lee, C.-T., Wu, H.-P., Cheng, T.-J., et al. (2011). Effects of ambient particulate matter and fungal spores on lung function in schoolchildren. Pediatrics, 127(3), e690–e698.
Codina, R., Fox, R., Lockey, R., DeMarco, P., & Bagg, A. (2008). Typical levels of airborne fungal spores in houses without obvious moisture problems during a rainy season in Florida, USA. Journal of Investigational Allergology and Clinical Immunology, 18(3), 156–162.
Crawford, J. A., Rosenbaum, P. F., Anagnost, S. E., Hunt, A., & Abraham, J. L. (2015). Indicators of airborne fungal concentrations in urban homes: Understanding the conditions that affect indoor fungal exposures. Science of the Total Environment, 517, 113–124.
Fernández-Rodríguez, S., Sadyś, M., Smith, M., Tormo-Molina, R., Skjøth, C. A., Maya-Manzano, J. M., et al. (2015). Potential sources of airborne Alternaria spp. spores in South-west Spain. Science of the Total Environment, 533, 165–176.
Fernández-Rodríguez, S., Tormo-Molina, R., Maya-Manzano, J. M., Silva-Palacios, I., & Gonzalo-Garijo, Á. (2014). Outdoor airborne fungi captured by viable and nonviable methods. Fungal Ecology, 7, 16–26.
Gonçalves, F. L. T., Bauer, H., Cardoso, M. R. A., Pukinskas, S., Matos, D., Melhem, M., et al. (2010). Indoor and outdoor atmospheric fungal spores in the São Paulo metropolitan area (Brazil): Species and numeric concentrations. International Journal of Biometeorology, 54(4), 347–355.
Haas, D., Habib, J., Luxner, J., Galler, H., Zarfel, G., Schlacher, R., et al. (2014). Comparison of background levels of culturable fungal spore concentrations in indoor and outdoor air in southeastern Austria. Atmospheric Environment, 98, 640–647.
Hargreaves, M., Parappukkaran, S., Morawska, L., Hitchins, J., He, C., & Gilbert, D. (2003). A pilot investigation into associations between indoor airborne fungal and non-biological particle concentrations in residential houses in Brisbane, Australia. Science of the Total Environment, 312(1–3), 89–101.
Heo, K. J., Lim, C. E., Kim, H. B., & Lee, B. U. (2017). Effects of human activities on concentrations of culturable bioaerosols in indoor air environments. Journal of Aerosol Science, 104, 58–65.
Hsu, N.-Y., Chen, P.-Y., Chang, H.-W., & Su, H.-J. (2011). Changes in profiles of airborne fungi in flooded homes in southern Taiwan after Typhoon Morakot. Science of the Total Environment, 409, 1677–1682.
Hsu, Y.-C., Kung, P.-Y., Wu, T.-N., & Shen, Y.-H. (2012). Characterization of indoor-air bioaerosols in southern Taiwan. Aerosol and Air Quality Research, 12, 651–661.
Hwang, S., Ko, Y., Park, D., & Yoon, C. (2018). Seasonality in airborne bacterial, fungal, and (1 → 3)-β-D-glucan concentrations in two indoor laboratory animal rooms. Journal of Clinical Pathology, 71(1), 59–66.
Hwang, S. H., Lee, I. M., & Yoon, C. S. (2013). Levels of total airborne bacteria, gram-negative bacteria, and endotoxin according to biosafety levels in Korean biosafety laboratories. Human and Ecological Risk Assessment: An International Journal, 19(6), 1576–1585.
Hwang, B. F., Liu, I. P., & Huang, T. P. (2011a). Molds, parental atopy and pediatric incident asthma. Indoor Air, 21(6), 472–478.
Hwang, S. H., Park, D. U., Ha, K. C., Cho, H. W., & Yoon, C. S. (2011b). Airborne bacteria concentrations and related factors at university laboratories, hospital diagnostic laboratories and a biowaste site. Journal of Clinical Pathology, 64(3), 261–264.
Hwang, S. H., Park, D. U., & Yoon, C. S. (2017). Levels of airborne biological agents and related factors in indoor environments of fish toxicity laboratory. Human and Ecological Risk Assessment: An International Journal, 23(7), 1553–1563.
IAQ Information Centre. (2003). A guide on indoor air quality certification scheme for offices and public places. Environmental Protection Department: The Government of the Hong Kong Special Administrative Region Indoor Air Quality Management Group. http://www.iaq.gov.hk/ Accessed 6 October 2017.
Jara, D., Portnoy, J., Dhar, M., & Barnes, C. (2017). Relation of indoor and outdoor airborne fungal spore levels in the Kansas City metropolitan area. Allergy and Asthma Proceedings, 38(2), 130–135.
Knudsen, S. M., Gunnarsen, L., & Madsen, A. M. (2017). Airborne fungal species associated with mouldy and non-mouldy buildings—Effects of air change rates, humidity, and air velocity. Building and Environment, 122, 161–170.
Lin, Z. Z., Cai, S. F., & Utsugi, W. (2004). An atlas of airborne fungal spores in southern Taiwan. Fengshan: Fengshan Tropical Horticultural Experiment Branch, Taiwan Agricultural Research Institute.
Luksamijarulkul, P., Kiennukul, N., & Vatthanasomboon, P. (2014). Laboratory facility design and microbial indoor air quality in selected hospital laboratories. Southeast Asian Journal of Tropical Medcine and Public Health, 45(3), 746–755.
Lymperopoulou, D. S., Adams, R. I., & Lindow, S. E. (2016). Contribution of vegetation to the microbial composition of nearby outdoor air. Applied and Environmental Microbiology, 82(13), 3822–3833.
Macher, J. (1999). Bioaerosols: Assessment and Control. Cincinnati, OH: ACGIH.
Maryam, Z., Rafiqah Azira, M. R., Noor Faizul Hadry, N., Norhidayah, A., & Mohd Shukri, M. A. (2015). Indoor microbial contamination through water mist aerosol at public restaurants. Jurnal Teknologi (Sciences & Engineering), 77(24), 45–50.
Muilenberg, M. (1999). A practical guide to aeroallergen identification. American College of Allergy and Immunology Annual Meeting, Chicago.
O’Connor, D. J., Sadyś, M., Skjøth, C. A., Healy, D. A., Kennedy, R., & Sodeau, J. R. (2014). Atmospheric concentrations of Alternaria, Cladosporium, Ganoderma and Didymella spores monitored in Cork (Ireland) and Worcester (England) during the summer of 2010. Aerobiologia, 30, 397–411.
Rajasekar, A., & Balasubramanian, R. (2011). Assessment of airborne bacteria and fungi in food courts. Building and Environment, 46, 2081–2087.
Rathnayake, C. M., Metwali, N., Jayarathne, T., Kettler, J., Huang, Y., Thorne, P. S., et al. (2017). Influence of rain on the abundance of bioaerosols in fine and coarse particles. Atmospheric Chemistry and Physics, 17(3), 2459–2475.
Rimac, D., Macan, J., Varnai, V. M., Vucemilo, M., Matkovic´, K., Prester, L., et al. (2010). Exposure to poultry dust and health effects in poultry workers: impact of mould and mite allergens. International Archives of Occupational and Environmental Health, 83, 9–19.
Rogers, C., Muilenberg, M. (2001). Comprehensive guidelines for the operation of Hirst-type suction bioaerosol samplers. The Pan-American Aerobiology Association.
Rosenbaum, P. F., Crawford, J. A., Anagnost, S. E., Wang, C. J. K., Hunt, A., Anbar, R. D., et al. (2010). Indoor airborne fungi and wheeze in the first year of life among a cohort of infants at risk for asthma. Journal of Exposure Science & Environmental Epidemiology, 20, 503–515.
Sabariego, S., Guardia, C. D.d.l, & Alba, F. (2000). The effect of meteorological factors on the daily variation of airborne fungal spores in Granada (southern Spain). International Journal of Biometeorology, 44, 1–5.
Sadys, M., Skjøth, C. A., & Kennedy, R. (2014). Back-trajectories show export of airborne fungal spores (Ganoderma sp.) from forests to agricultural and urban areas in England. Atmospheric Environment, 84, 88–99.
Salonen, H., Duchaine, C., Mazaheri, M., Clifford, S., & Morawska, L. (2015). Airborne culturable fungi in naturally ventilated primary school environments in a subtropical climate. Atmospheric Environment, 106, 412–418.
Sautour, M., Sixt, N., Dalle, F., L’Ollivier, C., Fourquenet, V., Calinon, C., et al. (2009). Profiles and seasonal distribution of airborne fungi in indoor and outdoor environments at a French hospital. Science of the Total Environment, 407(12), 3766–3771.
Seo, S. C., Choung, J., Cehn, B., Lindsley, W. G., & Kim, K. (2014). The level of submicron fungal fragments in homes with asthmatic children. Environmental Research, 131, 71–76.
Smith, E. G. (2000). Sampling and identifying allergenic pollens and molds: An illustrated identification manual for air samplers. San Antonio, TX: Blewstone Press.
Sordillo, J. E., Alwis, U. K., Hoffman, E., Gold, D. R., & Milton, D. K. (2010). Home characteristics as predictors of bacterial and fungal microbial biomarkers in house dust. Environmental Health Perspectives, 119, 189–195.
Tang, J. W. (2009). The effect of environmental parameters on the survival of airborne infectious agents. Journal of the Royal Society, Interface, 6(Suppl 6), S737–S746.
Tarigan, Y. G., Chen, R.-Y., Lin, H.-C., Jung, C.-Y., Kallawicha, K., Chang, T.-P., et al. (2017). Fungal bioaerosol exposure and its effects on the health of mushroom and vegetable farm workers in Taiwan. Aerosol and Air Quality Research, 17(8), 2064–2075.
Vesper, S., Barnes, C., Ciaccio, C. E., Johanns, A., Kennedy, K., Murphy, J. S., et al. (2013). Higher Environmental Relative Moldiness Index (ERMI) values measured in homes of asthmatic children in Boston, Kansas City, and San Diego. Journal of Asthma, 50(2), 155–161.
Wu, P. C., Li, Y. Y., Chiang, C. M., Huang, C. Y., Lee, C. C., Li, F. C., et al. (2005). Changing microbial concentrations are associated with ventilation performance in Taiwan’s air-conditioned office buildings. Indoor Air, 15(1), 19–26.
Acknowledgements
This study was supported by a research grant from the Chulabhorn Graduate Institute, Chulabhorn Royal Academy (Grant No. ET-60-16). The authors would like to thank all participating laboratories and staffs for providing information and accommodating us during our air sampling. We also thank Innovative Instrument Co., Ltd. (Thailand), for providing a particle counter.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kallawicha, K., Chao, H.J. & Kotchasatan, N. Bioaerosol levels and the indoor air quality of laboratories in Bangkok metropolis. Aerobiologia 35, 1–14 (2019). https://doi.org/10.1007/s10453-018-9535-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10453-018-9535-5