Abstract
In this study, we aimed to estimate the association between social support and healthcare utilization among older Mexican adults. We conducted a prospective study with 4027 older adults aged 65–74 in rural areas in seven Mexican states. Data were collected at baseline (2007) and 14 months later (2009). Healthcare utilization was defined as number of visits to a physician for preventive or curative purposes in the last 6 months. Multidimensional social support was operationalized into two components: structural (living arrangements, marital status and network size) and functional (perceived availability of support; and perceived support across emotional, instrumental, economic and information domains). Mixed-effects regression models were used to estimate the probability of healthcare use and to examine the association between social support and the number of visits to a physician. Results showed that perceived availability of social support was associated with the probability of visits to a physician (OR 1.44; p < .01). Meanwhile, the following domains of functional component of social support were associated with the probability of visits to a physician: instrumental (OR 1.55; p < .01), economic (OR 1.19; p = .03) and informational (OR 1.39; p < .01); and also with the number of visits to a physician: instrumental (eβ = 1.27; p < .01), economic (eβ = 1.14; p = .01) and informational (eβ = 1.12; p < .10). Our findings suggest that a significant association exists between social support, measured from a multidimensional viewpoint, and healthcare utilization, in which greater social support was related to a greater extent of use of health services.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The association between social support and diverse health outcomes has been widely studied in the literature (Cohen and Syme 1985; House et al. 1988; Holt-Lunstad et al. 2010). Findings suggest that social support is associated not only with mortality in fact, decreasing the probability of dying (Holt-Lunstad et al. 2010; Holt-Lunstad and Smith 2012) and a number of physical health indicators (Holt-Lunstad et al. 2007; Uchino 2009), but also with mental health indicators (Reinhardt et al. 2006) and even with genetic markers (Uchino et al. 2012). The role of social support has also been explored with regard to healthcare indicators, such as adherence to treatment (DiMatteo 2004) and healthcare utilization (Penning 1995).
Among the several approaches that have been used to analyze the healthcare utilization, one of the most supported is the Andersen and Newman model (Andersen and Aday 1978; Auslander and Litwin 1990), which conceptualizes healthcare utilization as a function of: predisposing factors such as age, gender, marital status and previous health conditions; enabling factors that either encourage or inhibit utilization, such as availability of resources and/or social support, awareness of available services and place of residence; and need-related factors, such as the presence of a chronic or acute condition, disability and perception of health status. According to this model, whether need translates into service use depends, among other things, on the availability of social support.
At least two complementary empirical definitions have been used to analyze the relationship between social support and health. One refers to the structural component of social support, which involves social participation and belonging to social networks (Rodriguez-Artalejo et al. 2006); the other refers to its functional aspect, including different types of interpersonal transactions (Piferi and Lawler 2006) that are commonly operationalized as received and perceived support (Lyyra and Heikkinen 2006). Further broken into types, support has been characterized as instrumental and emotional (Reblin and Uchino 2008).
Regarding the specific association between social support and healthcare utilization, it has remained largely unexplored and is presently under scrutiny, partly due to the necessity of more robust studies (longitudinal) and more broad definitions of the social support (Melchiorre et al. 2013). This debate is important because of its implications for daily healthcare practices and the formulation of public policy. Additionally, the use of health services assumes a special significance for the older adult population, given its vulnerability to frequent health conditions requiring opportune medical care (Cordato et al. 2005). The objective of this study was to determine whether availability of social support in a sample of rural older adults is associated with use of healthcare services.
Methods
Our analyses drew on longitudinal data from an impact evaluation study that was conducted in 2007 on the 70 y más Footnote 1 non-contributory pension program to estimate its effects on various economic and health indicators. The evaluation was carried out under a prospective study of 6000 older adults aged 65–74, who were living in rural areas in seven Mexican states. It included a baseline measurement in 2007, with a 91% (n = 5465) response rate, and one follow-up measurement in 2009. Participants were interviewed at home by trained personnel working for the National Institute of Public Health in Mexico. Data collected featured the following socio-demographic characteristics: education, lifestyle, physical and mental health, nutrition and healthcare utilization. The details of the study have been published elsewhere (Salinas-Rodriguez et al. 2014). The 70 y más impact evaluation study was approved by the Research and Ethics Committees of the National Institute of Public Health, with participants receiving a detailed explanation of the study procedures and signing an informed consent form prior to data collection.
Analytical sample
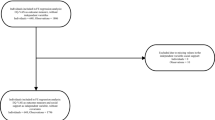
The analytical sample included those older adults who were able to provide complete information on the study variables at the baseline and follow-up measurement. Of the 5465 eligible participants, 343 with cognitive impairment which was determined using the Mini-Mental State Examination—MMSE—developed by Folstein et al. (1975), and who did not have a caregiver, along with 928 with incomplete information on the study variables, were excluded from the study. The final sample of 4194 older adults providing complete information represented 76.7% of the original basal sample. At follow-up, we excluded 298 subjects who had acquired cognitive impairment, 97 who had died, 165 who were no longer traceable and 416 who were unable to provide complete information on the study variables. Differences between the final sample and excluded participants occurred in a number of analytical variables, for instance, the latter had smaller networks (p < .01) and reported less social support availability (p < .01) at baseline. In terms of covariates, they included more females (p < .01), more illiterates (p < .01), fewer salary workers (p < .05), higher prevalence of disability in the basic activities of daily living (ADL) (p < .01) and instrumental activities of daily living (IADL) and a greater prevalence of depressive symptoms (p < .05).
Outcomes
Data collected on number of visits to a physician were used as indicator of healthcare utilization. Healthcare utilization was considered where participants reported having visited a physician for preventive or curative purposes in the last 6 months; also they were asked how many visits they had made in that period. This definition led to two operational indicators of the outcome variable. First, a dichotomous variable was defined and coded as 1 if the participant visits a physician, and second, a count variable was defined as the number of visits to a physician.
Exposure variables
In line with various operational definitions in the literature (Piferi and Lawler 2006; Rodriguez-Artalejo et al. 2006), the association between social support and healthcare utilization was analyzed according to several indicators of the structural and functional components of social support.
Structural indicators of social support included: living arrangements (older adult lived alone = 1, otherwise = 0) and marital status (married/cohabiting = 1, otherwise = 0). The children of the older adults were also considered using three variables combining their number and place of residence, namely: children who lived in the home of the older adult, had migrated internally or had migrated abroad (mainly to the USA). Finally, adopted as a count variable, network size was investigated with the following question: “How many close friends or neighbors do you currently have? (That is, persons with whom you feel comfortable and can talk about private matters, persons who can help you in some way).”
The functional component of social support was analyzed in terms of availability of economic support received as well as the types of support received. These variables were operationalized as follows: (a) Economic availability of support received was operationalized using the following question: “If for some reason you were to need a small amount of money (enough to pay for your expenses at home for a week), do you know anyone, or do you have any close relatives you could turn to for help?” (yes = 1); and (b) Types of support received. To evaluate the types of support received, we used the two following questions: (1) “Please mention the most important people from whom you receive support currently”, and (2) “Of people who mentioned, what support/help received from him/her?” For this last question, the response options were: Instrumental support (food, clothing, medicine and transportation), Emotional support (advice and company), Economic support and Informational support (concerning problems with health, nutrition, income and healthcare services). With these data, four dichotomous indicators were defined (received support = 1, otherwise = 0) for the four types of support.
Covariates
As covariates, the following variables were used: age, gender, literacy and ethnicity (indigenous = 1). Disability was defined using performance in ADLs (walking, bathing, eating, going to bed and using the bathroom) and IADLs (preparing own meals, shopping, taking medication, handling money, getting outside the home and doing housework). For each one, a dichotomous variable was defined (at least one difficulty = 1). Comorbidities were measured by asking participants whether they had been diagnosed by a physician as suffering from hypertension, diabetes, dyslipidemia, myocardial infarction, angina pectoris, heart disease, stroke, chronic lung disease, osteoporosis or cancer. Depressive symptoms were assessed using the 15-item version of the Geriatric Depression Scale (GDS) (Sheikh et al. 1991) with a dummy variable indicating whether respondents showed significant mild depressive symptoms (GDS ≥ 6). Self-perception of health was obtained and treated as a dichotomous variable (good/very good = 1). Having a paid job, being beneficiary of 70 y más program and having health insurance were also used. Also, data on the localities where the older adults resided were used. The socioeconomic status of localities was calculated according to the deprivation index of the National Population Council of Mexico, which features concepts such as illiteracy rates, housing conditions and income (CONAPO 2007).The index is continuous, with higher values denoting greater marginalization levels. Lastly, access to healthcare services was examined in terms of the transportation time (calculated in min) between the localities where the older adult resides and the nearest health facilities, adjusting this distance by taking into account the orographic conditions (topographic relief) of the land.
Statistical analysis
The association between social support and healthcare utilization was estimated using mixed-effects regression models with the aim of taking into account the correlation among repeated measures. Also, and due to the longitudinal structure of our data, the specification of the regression models included, as outcome variable, the use of health services at follow-up (either dichotomous or as a count) conditioned on the baseline measurement of the outcome and on covariates (both time-stationary and time-varying). Since we have two operational definitions of the outcome variable (dichotomous and count), we applied two separate regression models as described below.
First, in the case of dichotomous response variable (yes/no to healthcare utilization), mixed-effects logistic regression model was used and odds ratios (OR) were reported. Second, in the case of count variables (number of physician visits), mixed-effects zero-inflated negative binomial regression model (ZINB) was used and exponentiated coefficients were reported. These models were used to analyze the association of both structural and functional social support, with the likelihood of seeking healthcare and the number of visits to a physician.
In the specific case of the count variable (number of visits to a physician), ZINB was used to account for data heterogeneity resulting from the presence of extra zeros observed in the outcome. For this class of models, the presence of extra zeros means that a large number of zeros were observed, more than expected for a conventional Poisson model. In our case, a Poisson model will predict 2241 zeros, while the number observed was 4839. In fact, for outcome variables such as the number of visits to a physician, it is common to observe a high percentage of observations with values equal to zero (Salinas-Rodriguez et al. 2009).
Another feature of the ZIBN model is to assume that the excess zeros are generated by a separate process from the count values and that the excess zeros can be modeled independently. Thus, the model is composed by two equations: In the first equation, the probability of observing zeros is modeled, and in the second equation, the mean number of the count variable is modeled. In our case, the equation to predict zeros included data on gender, ethnicity, disability, number of chronic diseases, paid job, health insurance and transportation time to the outpatient or inpatient healthcare facility.
Lastly, differences were considered statistically significant if p < .05 and marginally significant if .05 < p < .10. The final models were evaluated in terms of collinearity, goodness of fit and residuals. Analyses were performed using STATA software 13.1 (StataCorp LP College Station, Texas).
Results
Table 1 presents the distribution of the indicators of healthcare utilization and social support in its structural and functional variants at baseline. 40.3% of respondents reported having sought healthcare in the last 6 months, with an average of 1.3 (SD = 2.3) visits to physician.
Concerning the structural component of social support, it was found that the average network size amounted to 4.5 individuals, and 7.7% of participants lived alone, while 60.9% were either married or cohabited. With regard to the functional component, a high percentage (88.8%) of respondents reported having available support. The principal type of support reported was economic (32.2%), followed by emotional (27.9%), instrumental (24.1%) and, lastly, informational support (5.2%).
Table 2 presents the results of the random-effects models used to examine the association between social support and healthcare utilization. The structural support indicators (living arrangements, marital status and network size) yielded no association with healthcare utilization or the average number of physician visits in the last 6 months, with the exception of the indicator that identified the number of children who have migrated internally, which was associated with the probability of visit to a physician (OR 1.04, p < .05), and with the mean number of visits (eβ = 1.02, p < .05). Conversely, the functional support indicators revealed that support availability favored the likelihood of seeking healthcare (OR 1.44, p < .01). Three types of support (instrumental, economic and informational) correlated significantly with both the probability of seeking healthcare (OR 1.55, p < .01; OR 1.19, p = .03; and OR 1.39, p < .01, respectively) and the average number of physician visits reported (eβ = 1.27, p < .01; eβ = 1.14, p = .01; and eβ = 1.12, p < .10, also, respectively). On the other hand, emotional support was not associated with any of the indicators related to the use of health services.
Sensitivity analysis
In this study, we used regression models with the inclusion of a random effect with the aim to exploit the advantage of having longitudinal data; however, it is well known that this approach has not the ability to control for unobserved variables that are constant over time, and hence, its results may have some bias (Allison 2009). One alternative approach is to adjust the same models but with the inclusion of a fixed effect instead. In Table 3, we show the results of the models with fixed effects. In general, we obtained similar results to those generated for the models with random effects, except for the variable number of children who have migrated to the USA, that now is associated with the probability of visit to a physician (OR 1.03, p < .10).
Discussion
This study investigated whether availability of multidimensional social support (split into its structural and functional components) was associated with healthcare utilization in a sample of Mexican older adults. Longitudinal data were used to determine the probability of utilization (users versus non-users) and the volume or total number of visits made to physician.
Although various studies have examined the relationship between social support and healthcare utilization in the older adult population, no conclusive evidence has been provided as yet. Some authors indicate that utilization is only marginally influenced, while others sustain that it is encouraged by social support (Andersen and Newman 1973; Coulton and Frost 1982; Penning 1995; Edelbrock et al. 2003; Melchiorre et al. 2013).
Our findings suggest that availability of support favors healthcare utilization. More specifically, our results can be interpreted according to the Andersen and Newman model (Andersen and Aday 1978; Auslander and Litwin 1990), which conceptualizes healthcare utilization as a function of: predisposing factors; enabling factors; and need-related factors. Under this model, the crossover from need to healthcare utilization depends, among others, on the availability of social support. Our findings suggest that this hypothesis was corroborated.
However, the nature and exact extent of the impact that social support produces on healthcare utilization are not totally clear. Research has moved in two directions. Some findings suggest that the use of health services (formal) declines as support networks (informal) contract (Bass and Noelker 1987), while others affirm that it intensifies where information is available from informal social support networks (particularly those made up of family members) (Arling 1985; Bass and Noelker 1987). Our results indicate that receiving information support increases both the likelihood of utilizing healthcare services and the total number of physician visits attended, thus evincing the importance of counting on this type of assistance.
More strikingly, however, our results demonstrate that utilization is associated not only with information availability, but also with other types of social support examined, instrumental and economic included. The literature has already established a clear nexus between instrumental support and healthcare utilization (Penning 1995), arguing that the use of healthcare not only depends on having information, but is also encouraged by the presence of individuals who can offer instrumental support (e.g., transportation to the physician’s office or hospital). Our study incorporated economic support as an enabling condition and found that it increases healthcare utilization. Its relevance is probably attributable to the importance of having the required economic resources—apart from available information—to reach a physician and even purchase medicine or pay for clinical laboratory tests. This hypothesis warrants a more detailed analysis in subsequent studies.
Our study also found that an indicator of living arrangement (children who have migrated internally) was associated with both the likelihood of use and the number of visits to a physician. There is scarce evidence about this association; however, one study with Mexican population reported that households having US migrants had greater use of health services than households without migrants (Salgado de Snyder et al. 2010). In that sense, we could hypothesize that our observed association shares a similar explanation, namely, that households with migrants have more economic resources which allow them a more intense use of health services. In addition to this economic interpretation, an alternative explanation is still possible, particularly that older adults with migrant children experience a greater degree of loneliness, and this feeling makes them more prone to use the health services, where they are likely to find the friendship and/or company of other older adults who also attend the same health services unit. Nevertheless, this association should be examined specifically in future studies.
Also, it is important to note that our study sample was composed of older adults that reside in rural communities, so this fact has several direct implications for the interpretation of our results. First, what it is known is that in rural areas the access to healthcare services is already reduced and even more in older adult population (González-González et al. 2011). Second, circumstances such as difficulty in managing required procedures for utilizing healthcare services represent a major barrier for older adults, particularly in rural populations (Wong and Díaz 2007). And third, factors such as scarce economic resources and long traveling to the nearest clinics represent additional barriers for this rural population regarding the use of health services (Fang et al. 2014).
However, in our study, we did not find a significant association between transportation time and health service use, in spite of the great variability observed in the transportation time and even the evidence suggesting the travel time to a healthcare provider can adversely affect a person’s ability to access that provider, especially among those needing specialty care (Chan et al. 2006). We hypothesize that other health-related variables (disability and morbidity) had greater power to explain the variability observed in the use of health services than the distance to the health clinics as it has been reported in rural older adults population (Salinas et al. 2010). Even so, it is necessary to deeply explore the urban–rural differences in health services utilization among older adults, especially using longitudinal data.
Our study has two strengths. Firstly, it was built on longitudinal data, whereas previous studies on healthcare utilization by older adults—even those specifically dealing with social support (Penning 1995)—have relied on cross-sectional data (Salinas et al. 2010; González-González et al. 2011). Secondly, and more importantly, it examined social support in detail according to various components, not a single aggregate measure, thus recognizing the multidimensional nature of the construct (Penning 1995; Uchino et al. 2012).
It must be acknowledged, however, that the study was unable to identify the quality of support received, an element which would provide crucial information for analyzing social support and its connection to health in general and healthcare utilization in particular (Uchino et al. 2012). This is important, as determining the quality of support would permit exploring its ties with healthcare utilization even more thoroughly. For instance, our results showed that instrumental support boosted the number of visits to physician, but did not indicate whether the availability of more or better instrumental support would have increased or reduced the number of physician visits.
This poses a major problem in analyzing the association between social support and healthcare utilization, since it remains initially unclear whether the use of healthcare services is actually beneficial. If older adults pursue healthcare because they are ill, and it helps them to keep their condition under control and maintain their health, then using such services is beneficial. But if older adults pursue healthcare because the services obtained are insufficient or fail to keep their condition in check, then the role of social support as a determinant is not as beneficial as one might expect. Future studies will be needed to recognize and analyze this potentially contradictory effect of social support, with the view of proposing possible explanations.
Our study was subject to other limitations that should be noted. Firstly, potential selection bias may have resulted from differences between the analytical sample and excluded older adults. It is a known fact that prospective studies with older people are open to losses at follow-up measurements (Van Beijsterveldt et al. 2002; Matthews et al. 2004), since the occurrence of deceased and untraceable participants often results in differences between sample and excluded subjects. In our case, the analytical sample proved healthier and better-off socioeconomically than those excluded. Therefore, healthcare utilization may have been underestimated, insofar as chronic illnesses and disability require greater medical care. And secondly, the results of our study cannot be generalized, as the sample was circumscribed to seven Mexican states and is therefore not representative of either all Mexican older adults, even rural older adults. Likewise, with the study sample comprising older adults aged 65–74 years, results must be interpreted cautiously, in that they apply exclusively to the younger sector of the old population.
In conclusion, our findings suggest that a significant association exists between social support, measured from a multidimensional viewpoint, and healthcare utilization. In particular, social support is associated with a greater likelihood of use and also with a greater number of doctor visits.
Notes
The 70 y más program, which provides older adults with unconditional cash transfers of US$40 per month, has evolved significantly since its inception. Originally run in rural communities of <2500 inhabitants and exclusively for individuals aged 70 and above, the program has moved forward with the new government in office. From 2011, it has expanded to poor urban communities of >2500 inhabitants, has lowered the age of its beneficiaries to ≥65 years (the name of the program is now Pension Program for Older Adults) and has increased the amount of the cash transfers to US$44 per month.
References
Allison P (2009) Fixed effects regression models. Sage Publications, Thousand Oaks
Andersen R, Aday LA (1978) Access to medical care in the U.S.: realized and potential. Med Care 16:533–546
Andersen R, Newman JF (1973) Societal and individual determinants of medical care utilization in the United States. Milbank Mem Fund Q Health Soc 51:95–124. doi:10.2307/3349613
Arling G (1985) Interaction effects in a multivariate model of physician visits by older people. Med Care 23:361–371
Auslander GK, Litwin H (1990) Social support networks and formal help seeking: differences between applicants to social services and a nonapplicant sample. J Gerontol 45:S112–S119. doi:10.1093/geronj/45.3.S112
Bass DM, Noelker LS (1987) The influence of family caregivers on elder’s use of in-home services: an expanded conceptual framework. J Health Soc Behav 28:184–196. doi:10.2307/2137131
Chan L, Hart L, Goodman D (2006) Geographic access to health care for rural medicare beneficiaries. J Rural Health 22:140–146
Cohen S, Syme SL (1985) Social support and health. Academic Press Inc, New York
CONAPO (Consejo Nacional de Población) (2007) Índice de marginación a nivel localidad 2005. Consejo Nacional de Poblacion, México, D. F
Cordato NJ, Saha S, Price MA (2005) Geriatric interventions: the evidence base for comprehensive health care services for older people. Aust Health Rev 29:151–156
Coulton C, Frost AK (1982) Use of social and health services by the elderly. J Health Soc Behav 23:330–339. doi:10.2307/2136491
DiMatteo MR (2004) Social support and patient adherence to medical treatment: a meta-analysis. Health Psychol 23:207–218. doi:10.1037/0278-6133.23.2.207
Edelbrock D, Waite LM, Broe GA et al (2003) The relation between unpaid support and the use of formal health services: the Sydney older persons study. Australas J Ageing 22:2–8
Fang P, Han S, Zhao L et al (2014) What limits the utilization of health services among the rural population in the Dabie mountains-evidence from Hubei province, China? BMC Health Serv Res. doi:10.1186/1472-6963-14-379
Folstein M, Folstein S, McHugh P (1975) “Mini-mental state”: a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12:189–198
González-González C, Sánchez-García S, Juárez-Cedillo T et al (2011) Health care utilization in the elderly Mexican population: expenditures and determinants. BMC Public Health 11:192. doi:10.1186/1471-2458-11-192
Holt-Lunstad J, Smith TB (2012) Social relationships and mortality. Soc Personal Psychol Compass 6:41–53. doi:10.1111/j.1751-9004.2011.00406.x
Holt-Lunstad J, Uchino BN, Smith TW, Hicks A (2007) On the importance of relationship quality: the impact of ambivalence in friendships on cardiovascular functioning. Ann Behav Med 33:278–290. doi:10.1007/BF02879910
Holt-Lunstad J, Smith TB, Layton JB (2010) Social relationships and mortality risk: a meta-analytic review. PLoS Med. doi:10.1371/journal.pmed.1000316
House JS, Landis KR, Umberson D (1988) Social relationships and health. Science 241:540–545. doi:10.1126/science.3399889
Lyyra T-M, Heikkinen R-L (2006) Perceived social support and mortality in older people. J Gerontol B Psychol Sci Soc Sci 61:S147–S152
Matthews FE, Chatfield M, Freeman C et al. (2004) Attrition and bias in the MRC cognitive function and ageing study: an epidemiological investigation. BMC Public Health 4:12. doi:10.1186/1471-2458-4-12
Melchiorre MG, Chiatti C, Lamura G et al. (2013) Social support, socio-economic status, health and abuse among older people in seven European countries. PLoS ONE. doi:10.1371/journal.pone.0054856
Penning M (1995) Health, social support, and the utilization of health-services among older adults. J Gerontol B Psychol Sci Soc Sci 50:S330–S339
Piferi RL, Lawler KA (2006) Social support and ambulatory blood pressure: an examination of both receiving and giving. Int J Psychophysiol 62:328–336. doi:10.1016/j.ijpsycho.2006.06.002
Reblin M, Uchino BN (2008) Social and emotional support and its implication for health. Curr Opin Psychiatry 21:201–205. doi:10.1097/YCO.0b013e3282f3ad89
Reinhardt JP, Boerner K, Horowitz A (2006) Good to have but not to use: differential impact of perceived and received support on well-being. J Soc Pers Relat 23:117–129. doi:10.1177/0265407506060182
Rodriguez-Artalejo F, Guallar-Castillon P, Herrera MC et al (2006) Social network as a predictor of hospital readmission and mortality among older patients with heart failure. J Card Fail 12:621–627
Salgado de Snyder VN, González-Vázquez T, Infante-Xibille C et al. (2010) Servicios de salud en la Mixteca: utilización y condición de afiliación en hogares de migrantes y no-migrantes a EU. Salud Publica Mex 52:424–431. doi:10.1590/S0036-36342010000500010
Salinas JJ, Al Snih S, Markides K et al (2010) The rural-urban divide: health services utilization among older Mexicans in Mexico. J Rural Health 26:333–341. doi:10.1111/j.1748-0361.2010.00297.x
Salinas-Rodriguez A, Manrique-Espinoza B, Sosa-Rubi SG (2009) Statistical analysis for count data: use of healthcare services applications. Salud Publica Mex 51:397–406
Salinas-Rodriguez A, Torres-Pereda M, Manrique-Espinoza B et al (2014) Impact of the non-contributory social pension program 70 y mas on older adults’ mental well-being. PLoS ONE 9:e113085. doi:10.1371/journal.pone.0113085
Sheikh JI, Yesavage JA, Brooks JO 3rd et al (1991) Proposed factor structure of the Geriatric depression scale. Int Psychogeriatr 3:23–28
Uchino BN (2009) What a lifespan approach might tell us about why distinct measures of social support have differential links to physical health. J Soc Pers Relat 26:53–62. doi:10.1177/0265407509105521
Uchino BN, Cawthon RM, Smith TW et al. (2012) Social relationships and health: is feeling positive, negative, or both (ambivalent) about your social ties related to telomeres? Health Psychol 31:789–796. doi:10.1037/a0026836
Van Beijsterveldt CEM, Van Boxtel MPJ, Bosma H et al. (2002) Predictors of attrition in a longitudinal cognitive aging study: the maastricht aging study (MAAS). J Clin Epidemiol 55:216–223. doi:10.1016/S0895-4356(01)00473-5
Wong R, Díaz JJ (2007) Health care utilization among older Mexicans: health and socioeconomic inequalities. Salud Publica Mex. doi:10.1590/S0036-36342007001000010
Acknowledgements
This project is based on data from an impact evaluation, which was funded by the Mexican Ministry of Social Development. The elaboration of this study results required additional work by the authors. The authors have received no funding for this article. The contents of this publication do not represent the official position of the Mexican Ministry of Social Development.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Responsible editor: D.J.H. Deeg.
Rights and permissions
About this article
Cite this article
Salinas-Rodríguez, A., Moreno-Tamayo, K., Hernández-Serrato, M. et al. Multidimensional social support is associated with healthcare utilization among older Mexican adults. Eur J Ageing 15, 77–85 (2018). https://doi.org/10.1007/s10433-017-0428-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10433-017-0428-1