Abstract
Slaughtering sick poultry is a risk factor for human infection with highly pathogenic avian influenza and is a common practice in Bangladesh. This paper describes human exposures to poultry during slaughtering process and the customs and rituals influencing these practices in two Bangladeshi rural communities. In 2009, we conducted 30 observations to observe slaughtering practices and 110 in-depth and short interviews and 36 group discussions to explore reasons behind those practices. The villagers reported slaughtering 103 poultry, including 20 sick poultry during 2 months. During different stages of slaughtering, humans, the environment, healthy poultry, and other animals were exposed to poultry blood and body parts. Women performed most of the slaughtering tasks, including evisceration. Defeathering required the most time and involved several persons. During festivals, ceremonies, and rituals, many people gathered and participated in the slaughtering of poultry. Exposure to poultry slaughtering created numerous opportunities for potential avian influenza transmission. Strategies that can be further tested to determine if they reduce the risk of transmission include skinning the carcasses of sick poultry, using hot water for defeathering and cleaning, using a bucket to contain slaughtering blood and carcass, burying the offal and encouraging handwashing.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction and Purpose
Highly pathogenic avian influenza (HPAI) is a public health concern, especially in Asia. Among the HPAI viruses, H5N1 is of particular concern because of its transmissibility to humans (Van Kerkhove et al. 2011) and high case fatality (WHO 2013). One risk factor for human infection is close contact with infected sick or dead birds (Areechokchai et al. 2006; Dinh et al. 2006; Zhou et al. 2009). Laboratory-confirmed human H5N1 case-patients have often reported slaughtering poultry prior to illness (Van Kerkhove et al. 2011). Slaughtering, defeathering, or preparing sick poultry for cooking have been implicated as potential risk factors for infection (Abdel-Ghafar et al. 2008; Van Kerkhove 2012). Transmission of avian influenza to humans risks human coinfection with human and avian influenza. Reassortment of the segmented RNA from two different influenza strains in a co-infected host can lead to emergence of a dangerous novel virus with pandemic potential (Jackson et al. 2009).
HPAI has become endemic in poultry in Bangladesh with an increase in outbreaks during December–March (Loth et al. 2010). As of April 2013, 2.7 million poultry have been culled or died in 549 H5 outbreaks (OIE 2013). In Bangladesh, poultry raising plays an important role in food security and the economy. In 2007, poultry contributed 40% of the total meat production in Bangladesh (Dolberg 2008). Poultry raising also makes a crucial contribution to the nutrition and income of rural families, however, their daily practices and low biosecurity expose them to avian influenza infection (Sultana et al. 2012a).
Seven human cases of avian influenza A (H5N1) infection have been identified in Bangladesh (WHO 2013). All cases were reported to have exposure to slaughtering poultry prior to illness. The first case was a child whose mother attended after slaughtering a chicken at home (Brooks et al. 2009). Chickens were slaughtered, defeathered, and skinned inside the second case’s home seven days prior to the case-patient’s illness. The mother of the third case touched him while cooking a chicken (Chakraborty 2011). The fourth, fifth, and sixth cases were live bird market workers (IEDCR 2012a, b) involved in poultry slaughtering (Rimi et al. 2013) and the last case was reported to have direct contact with the meat of a sick poultry during cooking (Rahman et al. 2013).
Slaughtering sick poultry is a common practice in many communities around the world (Padmawatia and Nichter 2008) including in rural Bangladesh (UNICEF Bangladesh 2007; Sultana et al. 2012b). The Government of Bangladesh disseminated a set of 10-step messages to promote awareness and prevent avian influenza infection nationwide, including messages to avoid slaughtering infected poultry (Government of Bangladesh 2007). A subsequent qualitative study reported low awareness about avian influenza and Government prevention messages and sick poultry slaughtering as a common practice among Bangladeshi backyard poultry raisers (Sultana et al. 2012b). Such findings suggest that there is a need for an in-depth understanding of poultry slaughtering practices in order to inform the development of practical and culturally acceptable interventions to reduce the risk of avian influenza transmission to humans. We describe human exposure to poultry during the slaughtering and the influence of customs and rituals on these practices in two rural Bangladeshi communities to identify specific practices that might be modified to avoid human exposure of avian influenza.
Methods
Study Period and Settings
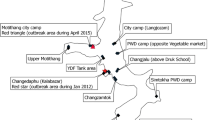
A team of three anthropologists and two sociologists from icddr,b collected data from June to August, 2009. The team collected data from two rural villages in Rajshahi and Chittagong, districts from northwest and southeast Bangladesh (Fig. 1). Being qualitative by nature, this study is designed with comparatively smaller sample size purposively selected to obtain an in-depth understanding of the issue from the perspective of the study population and did not aim to achieve statistical representativeness. Villages were chosen because of their small size, accessibility, and being typical in the region in terms of demographic and geographic characteristics, i.e., agriculture as the main occupation, inhabitant with Muslim majority and located in floodplains.
Data Collection
To obtain in-depth understanding, we used a focused ethnographic approach (Pelto and Pelto 1997) which has been widely used in public health research to holistically study specific issues among a limited number of people of a single culture within a specific time period (Gove and Pelto 1994; Padmawatia and Nichter 2008).
The team lived in two villages and observed 30 events of poultry slaughtering in their natural setting. They conducted 110 in-depth and short interviews and 36 informal group discussions in Bengali with community members, mainly women, to explore reasons for slaughtering poultry and villagers’ explanation behind different tasks during the process. The team took field notes to record the observations. The discussions were recorded using audio recorders and field notes. Our team recorded poultry as sick if villagers judged poultry to be sick. Villagers considered poultry sick when these stopped eating, defecated lime-like feces, or appeared lethargic or agitated.
Data Analysis
The team completed the field notes every day after data collection and transcribed the recorded data verbatim in Bengali. They identified emerging themes from the findings relevant to the study objectives and summarized the data. Translation was not conducted until the data were presented in the manuscript because the first author is a native Bengali speaker.
Ethics
The team obtained informed consent before conducting interviews, group discussions, and visual documentation. The Ethical Review Committee of International Centre for Diarrhoeal Disease Research, Bangladesh reviewed and approved the study protocol.
Results
Demographics
The age of the informants ranged from 18 to 100 years (median 38 years). There were 114 households (73% Muslim and 23% Hindu) in Rajshahi and 138 households (100% Muslim) in Chittagong. The majority of population had primary or no formal education (74% (n = 466) in Rajshahi, 66% (n = 737) in Chittagong). In Rajshahi, 59% households reported monthly income BDT ≤ 5,000 (US$ 64.18) compared to 37% Chittagong households. Twenty-one percent Rajshahi households reported monthly income between BDT 5,001 and 10,000 (US$ 64.19–128.35) compared to 44% Chittagong households. Villagers collected water from tube-wells shared among several households for drinking and from rivers, ponds, and ditches for other purposes.
The majority of households irrespective of religion raised backyard poultry for egg and meat production (92% (n = 114) in Rajshahi, 88% (n = 138) in Chittagong). These poultry were indigenous breeds with less than 50 free-range chickens, ducks, and/or geese per flock reared around the family’s domicile. In Chittagong, two families had small commercial farms of broiler chickens with less than 1,000 poultry. These broiler chickens were commercially raised indoor for meat production. Awareness about avian influenza was low among these communities and few villagers knew about “bird flu” or any of its signs or transmission.
Consumption of Poultry During Study Period
Although most residents raised poultry primarily for egg production, villagers did slaughter poultry for consumption and for specific events. Sometimes they slaughtered home-raised backyard poultry and sometimes they slaughtered broiler chickens purchased alive from local markets or farms. During the two study months, villagers slaughtered 103 poultry (Table 1); 56 poultry in 27 households in Rajshahi, and 47 poultry in 24 households in Chittagong.
Villagers slaughtered and consumed their sick poultry when they could not sell them. Since Islam prohibits eating animals that die of natural causes (Regenstein and Regenstein 2003), villagers tried to slaughter sick poultry before these died. In fear of losing poultry, some villagers slaughtered their healthy poultry when they heard about high mortality in a neighbor’s flock. When a flock of broiler chickens became sick, the owner slaughtered some chickens for household consumption and sold some of the living sick chickens to other villagers.
Slaughtering Process
The team observed the slaughtering and processing of 33 poultry in 30 events, including five of sick poultry. Three of these 30 events included slaughtering of two poultry. We divided the slaughtering process into three steps: killing the poultry, defeathering, and cutting meat. We found differences between the slaughtering of sick and healthy poultry which we described below.
Killing the Poultry
Killing took less than a minute, was conducted in the corner of yards and involved two persons (Table 2). Villagers reported preferring that men of the household kill the poultry. Women and children killed poultry or held poultry during killing when men were absent. Chanting religious verses while killing poultry was a prerequisite for both Muslims and Hindus. Since villagers killed sick poultry hurriedly before these died, women were more likely to be available to kill sick poultry at the place where the free-ranging poultry was found, such as on the roadside, beside ponds, or near kitchens. In four of the five observed killing of sick poultry, women either killed or held the poultry during killing. In Chittagong, the nearby community of fishermen collected dead poultry for consumption from villagers’ houses or from bodies of water where they had been discarded. Below is an excerpt from the observation note to describe the killing process.
The woman held the chicken with both hands while standing in a corner of the yard. Her female neighbor held the head of the chicken in one hand and cut its throat with a traditional sharp curved instrument (haisha or boti) held in her other hand. The woman continued to hold the chicken for some time to let the blood drip on the ground and then dropped the chicken on the ground. The chicken flapped around on the ground for approximately one minute, and as it flapped, blood splattered on the hands, bodies and clothing of the women and on the ground. The neighbor pumped the handle of the tube-well with her bloody hands before rinsing them off. The woman’s niece carried the carcass to the kitchen while blood dripped along the way. The blood remained in the yard for several hours before soaking into the ground.
Villagers rarely used soap (Table 2). Rinsing hands and slaughtering tools with tube-well water or stored water from a pot was common, but usually blood stains remained visible. The persons who held the poultry did not typically rinse their hands. The team observed backyard poultry pecking at the blood. In Chittagong, villagers were more likely to pour water on the yard to wash the blood off the ground compared with Rajshahi (Table 3). Villagers’ explained that they cleaned the blood to avoid disease among poultry, because blood looked bad and stepping on blood might cause harm to others, especially pregnant women.
Defeathering
Villagers usually defeathered carcass, since they ate the skin. Only in two events, they skinned the carcass along with the feathers because they did not want to eat the skin. Defeathering was conducted within the yard and inside the kitchen and involved more than one person (mean 3, range 1–6) and required an average 54 min per event (range 20–150 min) (Table 2). Although two poultry were defeathered during this time in the three of the 30 events, there was more than one person performing the defeathering task simultaneously. Typically women and children family members and neighbors assisted in defeathering and most did not wash their hands after defeathering. Fewer neighbors or relatives were involved in the defeathering in Chittagong, as Chittagong was more socially conservative and women typically remained indoors. In Rajshahi, women defeathered poultry in the yards.
There were differences in defeathering practices between the two sites. Rajshahi villagers first plucked the large feathers keeping the carcass on a large fresh leaf or plastic sack and then scorched the skin to burn the small feathers. After scorching and plucking the small feathers, they washed and scrubbed the carcass in the nearest tube-well or water body because they considered the scorched residues as “dirty.” They stored all the big feathers of backyard poultry in a bag to sell for the production of pillows and dusters in the capital. Using hot water for defeathering was an occasional practice in Rajshahi but a typical one in Chittagong. Chittagong villagers scalded the carcass in a cooking pot or bowl using hot water to ease plucking. They stored a few feathers to use as ear picks and discarded the rest as there were no local vendors to buy feathers. They frequently performed other household tasks during or after defeathering without washing their hands. Below is a description of the defeathering process.
The guest woman and four children (aged approximately 5–6 years) defeathered the carcasses keeping it on a plastic sack on the ground in a corner of the yard beside the pond. A lot of feathers were floating in the air and the place was very windy. The children played with feathers and one playfully touched his eyes with a feather. The woman’s sister lit a fire with jute-sticks and the women held the legs and wings as they scorched the carcasses on the fire. They placed the scorched carcasses on the sack and removed the skin of the legs. The children plucked small feathers by pinching them off with their fingernails. They rinsed their hands with a little water after plucking the feathers and then ate breakfast. A flock of backyard chickens scavenged where the carcasses were defeathered and ate the feathers.
Cutting Meat
This step includes skinning, eviscerating, cutting meat into pieces, and disposing of waste. It required an average of 18 min per event (range 5–30) and in both study sites, one woman performed these tasks (Table 2). Children often touched or played with poultry meat during the cutting.
After defeathering, the women skinned the carcass and cut the skin into pieces with a boti on a banana leaf. Then she cut off the head, legs and wings and then cut open the chest and abdomen. She pulled out the viscera, separated the liver, gizzard and heart, and discarded the rest. She cut the gizzard and peeled off the inner layer of the gizzard. The viscera ruptured and the liquid spilled on the ground and stained her dress.
Villagers cut off and discarded the parts of sick poultry that appeared abnormal; for example, the liver when it was discolored or the gizzard when it had a lump. Some informants reported that some villagers cooked and ate the cleaned intestines. They used the same slaughtering tools for cutting vegetables, onions, and banana leafs without washing them (Table 3).
After cutting, villagers rinsed the meat 2–3 times in a bowl or pot with tube-well or pond water and cooked the meat. Occasionally (8/30), they kept the meat in a food pot for several hours to cook later. Villagers killed sick poultry during the night if these were about to die and then they waited to process and cook the poultry the following morning. Villagers cooked poultry thoroughly. Pink meat was never visible after cooking in any of our observations.
Villagers dumped the offal (including parts of the intestines, pancreas, gallbladder, and bursa) and feathers in nearby bushes, cultivation land, or the same body of water that they used for cooking, bathing, and washing poultry carcass or utensils (Table 3). In five events, they buried the offal. Dogs, crows, and backyard poultry ate the offal and feathers immediately after those were dumped. They also fed offal and feathers to their backyard poultry and dumped offal in the ditch so that ducks and fishes could eat them. A few informants preferred to dump offal from sick poultry in bodies of water far away from their houses rather than in a nearby ditch because they feared that their healthy poultry might get ill by eating the offal. They discarded the water used for defeathering or washing meat by the tube-well or in the yard. Since there was no water drainage system in yards, the discarded water gradually soaked into the ground or evaporated.
The woman gave the gizzard to her daughter and the girl washed it in the pond. After cutting, the woman dumped the banana leaf, offal and the feathers in the ditch behind the kitchen. The dog ate the offal and a duckling ate the intestines.
Villagers never took any personal protective measure when handling poultry, such as covering their mouth or nose or eyes or by using gloves. They did not wash their hands after the process because they considered their hands washed once they washed the meat. Although most households owned soap, handwashing with soap was never observed in Chittagong (Table 2).
Influence of Customs and Rituals on Poultry Slaughtering Practices
On all festival days, villagers considered poultry as “good food.” Villagers slaughtered poultry during religious festivals, rituals, and ceremonies at births, weddings and deaths, and visits by guests. Of the total poultry slaughtered in Chittagong during the study period, 28% was slaughtered during the 2-day period of the Islamic festival Shab-e-Barat (Table 1). During such occasions, neighbors, and relatives gathered and participated in the slaughtering. In Rajshahi, villagers invited married daughters, their in-laws, and relatives and treated them with poultry as an expression of hospitality during mango–jackfruit season (May–July) and date palm sap season in winter (mid-October–mid-March).
During religious festivals, villagers preferred that religious leaders slaughter their poultry. In Rajshahi, during the biggest annual Islamic festival, Eid, many households sent their children with poultry to the mosque so that the religious leader (Imam) could slaughter their poultry. Chittagong fishermen observed Monsha Puja, a religious festival when ducks were slaughtered. Many people came to the temple throughout the day to have their ducks blessed with a prayer (mantra) and then slaughtered at the temple. Other than killing poultry in the yard or compound of the mosque or temple, the rest of the slaughtering process was similar to that of households.
Villagers also slaughtered poultry as a sacrifice for specific prayers, such as recovery from disease or a crisis. One way of practicing such sacrifice was donating poultry to a shrine (mazaar) or mosque. A number of persons, including the shrine workers, the persons who brought the poultry and visitors, slaughtered and cooked the poultry at the shrine and consumed it together. In Rajshahi, one Muslim household slaughtered a rooster and then poured the blood in the betel leaf garden for good luck.
Discussion
The practice of slaughtering and processing poultry in these rural communities exposed villagers, healthy poultry, wild birds, and animals to potentially contaminated body parts and fluids of the slaughtered poultry that could transmit avian influenza. Evisceration exposed villagers directly to intestinal contents and defeathering exposed several persons to the slaughtered poultry for a prolonged period of time. These slaughtering practices also soiled grounds, bodies of water, and bushes with body parts and fluid. The customs and rituals of these communities influenced the occurrence and process of poultry slaughtering and created opportunities for spread of infection through community participation.
During the different stages of the slaughtering process in these communities, transmission of avian influenza to humans was plausible through direct and indirect contact with airborne droplets of respiratory secretions, small particle aerosols, blood, and intestinal contents (Rabinowitz et al. 2010). Since villagers handled poultry without covering their nose, eyes, or mouth while killing, defeathering, and cutting, transmission could occur through inoculation of aerosols into the upper respiratory tract, oral mucosa, or conjunctivae (Rabinowitz et al. 2010). Villagers’ practice of evisceration and preparing the intestine for consumption are particularly risky, since viral particles are produced in large numbers by the poultry gastrointestinal tract (Webster et al. 1978). Defeathering, the lengthiest stage of the process, might also pose risk through creating aerosol and increasing chances of inhalation of the virus, as high viral load has been recorded in feather pulp (Busquets et al. 2010). In Azerbaijan, defeathering a dead swan after a massive swan die-off was associated with exposure to H5N1 among infected case-patients (Gilsdorf et al. 2006). During the process, hands, cloths, utensils, or surfaces became contaminated with poultry blood, feces, or secretions and were not cleaned thoroughly which could facilitate transmission as influenza virus can survive on hands for up to 5 min after transfer from environmental surfaces (Bean et al. 1982).
Soiling of the environment with poultry blood and body parts increased the risk of potential transmission of avian influenza. Since avian influenza virus can survive for 24–48 h on contaminated hard, nonporous surfaces and up to 8–12 h on porous surfaces (Bean et al. 1982) and in water under certain circumstances (WHO 2006b), the environment could be a potential pathway for infection in these communities (Horm et al. 2012). Potentially contaminated environments have been identified as a risk factor for human infection (Cavailler et al. 2010; Vong et al. 2009). Waterfowl, the natural reservoir for influenza viruses, also shared the water bodies where the slaughtering waste was dumped. Crows and domestic animals such as cats and dogs that scavenged for waste or blood could become infected (Maas et al. 2007; Islam et al. 2011). The practice of feeding slaughtering remnants to other backyard poultry has been identified as a risk factor for H5N1 infection among backyard chickens in Bangladesh (Biswas et al. 2009).
Differences in contact patterns with poultry may cause differences in risk for exposure among persons of different age and gender. In rural Cambodia, males were identified to have higher risk of H5N1 exposure than women because males were involved in poultry slaughtering, removing internal organs, and licking wounds of fighting cocks (Van Kerkhove et al. 2008). In our study villages, women and children were involved in all steps of the slaughtering process and women carried out the majority of the activities, especially evisceration and defeathering. In many countries, the majority of avian influenza cases have been females (Gilsdorf et al. 2006; Oner et al. 2006; Zhou et al. 2009; Fasina et al. 2010; Kandeel et al. 2010; Van Kerkhove et al. 2011). Several outbreaks in different countries reported that children accounted for a large number of cases (Areechokchai et al. 2006; Dinh et al. 2006; Oner et al. 2006; WHO 2006a; Fasina et al. 2010).
Several studies have described behavior related to avian influenza in different countries. Barennes et al. (2010) reported the presence of outbreaks did not influence the behavior in Laos. Manabe et al. (2012) reported higher rates of unsafe behaviors, including selling remainder poultry after die-off, throwing carcasses in bodies of water, eating dead poultry, and not wearing gloves while slaughtering, among the participants who lived in a community where H5N1 cases have been reported in Vietnam. People in many countries (Food and Agriculture Organization 2008; Manabe et al. 2012; Paul et al. 2013) often adopt strategies, including quickly slaughtering poultry, to limit financial losses during disease occurrence, which increases their risk of contracting avian influenza. Financial concern also influences Bangladeshi backyard poultry raisers to adopt slaughtering sick poultry (Sultana et al. 2012b). Taken together these data suggests that the attitudes and practices among rural backyard poultry raisers in Bangladesh are typical of rural backyard poultry raisers in the region. The new findings from our study highlight the specific behaviors around slaughtering sick poultry that may represent one of the highest risk opportunities for transmission.
Slaughtering poultry is central to many customs, rituals, and beliefs of many communities around the world (Aklilu et al. 2008; Liu 2008; Padmawatia and Nichter 2008). Poultry consumption increases during certain socio-cultural events (Aklilu et al. 2007; Gondwe and Wollny 2007). As part of such occasions in our study villages, people gathered at households or mosque and shrine, and participated in poultry slaughtering that exposed multiple persons to blood or body parts and so heightened the risk of potential spread of infection to the community. Villagers’ seasonal slaughtering coincides with the season (December–March) when avian influenza outbreaks in poultry reached their peak during the last three years in Bangladesh (Loth et al. 2010). Understanding the link between particular communities’ culture, custom, and seasonality of the slaughtering practices is important to develop culturally compelling interventions to reduce exposure to potential risk for avian influenza in Bangladesh. This information can also be useful to implement interventions targeting particular times and places for demonstrations of safe slaughtering practices.
We intended to collect information about all the poultry slaughtering events that occurred during our data collection period but might have missed a number of events in the initial days, before the study team developed rapport with the villagers. Nevertheless, the team collected data until they repeatedly received similar information; hence the data was sufficiently saturated. Since this study was only conducted in two villages; they may not be representative of Bangladesh as a whole. We view these practices as typical, however, since another study found similar practices in other villages (Sultana et al. 2012b) and there were only few differences between our two study sites despite large geographical distance. A more sophisticated thematic analysis related to cultural issues could provide insights which could be useful to develop interventions. This research provides information on cultural issues related to slaughtering practices, which can be a basis for future research where thematic analysis may provide new direction to recommend and develop interventions.
Conclusion
Although international recommendations discourage home slaughtering of sick poultry (WHO 2007), villagers in rural Bangladesh are unlikely to stop this practice as it is central to household livelihood (Sultana et al. 2012a). Communication campaigns that included general preventive messages on raising poultry more safely in different countries resulted in minimal or no positive change in behavior (Food and Agriculture Organization 2008; Van Kerkhove et al. 2009; Barennes et al. 2010; Manabe et al. 2011, 2012; Paul et al. 2013). Specific messages on reducing risk during slaughtering or environmental cleaning can be incorporated in interventions and evaluated for effectiveness. This study provides information about the context of such practice which can be used to develop potential safe home slaughtering recommendations. Developing recommendations that poultry raisers would be willing and able to implement and would reduce risk is an important research priority. Generic recommendations that could be explored and piloted in these contexts include using a bucket to contain blood, carcass, offal, skin, feathers, and waste water and burying the bucket content to reduce potential environmental contamination. As personal protection measure, handwashing should be promoted. For the slaughtering of sick poultry, a more restrictive set of recommendations could be explored and piloted along with generic recommendations. Hot water could be used to decontaminate the bucket at the end of the process. Since avian influenza virus is susceptible to temperature (WHO 2007), hot water may decontaminate the bucket and slaughtering tools more effectively and using hot water for defeathering sick poultry may help to reduce the virus from the surface of the carcass and reduce flying of feather, which can harbor the virus. Skinning sick poultry along with feathers instead of defeathering may also reduce the exposure from defeathering process. Further research should develop and evaluate interventions during this high risk process in at risk communities.
References
Abdel-Ghafar AN, Chotpitayasunondh T, Gao Z, Hayden FG, Nguyen DH, de Jong MD, et al. (2008). Update on avian influenza A (H5N1) virus infection in humans. N Engl J Med 358:261-273.
Aklilu HA, Almekinders CJ, Udo HM, and Van der Zijpp AJ (2007). Village poultry consumption and marketing in relation to gender, religious festivals and market access. Tropical Animal Health and Production 39:165-177.
Aklilu HA, Udo HMJ, Almekinders CJM, and Van der Zijpp AJ (2008). How resource poor households value and access poultry: Village poultry keeping in Tigray, Ethiopia. Agricultural Systems 96:175-183.
Areechokchai D, Jiraphongsa C, Laosiritaworn Y, Hanshaoworakul W, O’Reilly M (2006) Investigation of avian influenza (H5N1) outbreak in humans—Thailand, 2004. Global Epidemiology 55:3–6.
Barennes H, Harimanana AN, Lorvongseng S, Ongkhammy S, and Chu C (2010). Paradoxical risk perception and behaviours related to Avian Flu outbreak and education campaign, Laos. BMC Infectious Diseases 10:294.
Bean B, Moore BM, Sterner B, Peterson LR, Gerding DN, and Balfour HH, Jr. (1982). Survival of influenza viruses on environmental surfaces. Journal of Infectious Diseases 146:47-51.
Biswas PK, Christensen JP, Ahmed SS, Das A, Rahman MH, Barua H, et al. (2009) Risk for infection with highly pathogenic avian influenza virus (H5N1) in backyard chickens, Bangladesh. Emerging Infectious Diseases 15:1931–1936. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=19961672.
Brooks WA, Alamgir AS, Sultana R, Islam MS, Rahman M, Fry AM, et al. (2009). Avian influenza virus A (H5N1), detected through routine surveillance, in child, Bangladesh. Emerging Infectious Diseases 15:1311-1313.
Busquets N, Abad FX, Alba A, Dolz R, Allepuz A, Rivas R, et al. (2010). Persistence of highly pathogenic avian influenza virus (H7N1) in infected chickens: feather as a suitable sample for diagnosis. Journal of General Virology 91:2307-2313.
Cavailler P, Chu S, Ly S, Garcia JM, Hado Q, Bergeri I, et al. (2010) Seroprevalence of anti-H5 antibody in rural Cambodia, 2007. Journal of Clinical Virology 48:123-126.
Chakraborty A (2011). Outbreak of mild respiratory disease caused by H5N1 and H9N2 infections among young children in Dhaka, Bangladesh, 2011 Health and Science Bulletin 9:5-12.
Dinh PN, Long HT, Tien NT, Hien NT, Mai le TQ, Phong le H, et al. (2006). Risk factors for human infection with avian influenza A H5N1, Vietnam, 2004. Emerging Infectious Diseases 12:1841-1847.
Dolberg F (2008) Poultry sector country review: Bangladesh. Rome: Food and Agriculture Organization of the United Nations.
Fasina FO, Ifende VI, and Ajibade AA (2010). Avian influenza A(H5N1) in humans: lessons from Egypt. Euro Surveill 15:19473.
Food and Agriculture Organization (2008) Rural Livelihood and Biosecurity of Smallholder Poultry Producers and Poultry Value Chain. Rome: FAO. http://www.commdev.org/userfiles/Smallholder%20biosecurity%20in%20Poultry%20Value%20Chain.pdf. Accessed August 24, 2013.
Gilsdorf A, Boxall N, Gasimov V, Agayev I, Mammadzade F, Ursu P, et al. (2006). Two clusters of human infection with influenza A/H5N1 virus in the Republic of Azerbaijan, February-March 2006. Euro Surveill 11:122-126.
Gondwe TN, and Wollny CB (2007). Local chicken production system in Malawi: household flock structure, dynamics, management and health. Tropical Animal Health and Production 39:103-113.
Gove S, and Pelto GH (1994). Focused ethnographic studies in the WHO Programme for the Control of Acute Respiratory Infections. Medical Anthropology 15:409-424.
Government of Bangladesh (2007) Bird Flu: What You Need to Know and Do. http://www.mofl.gov.bd/bird_flu.aspx. Accessed August 24, 2013.
Horm SV, Gutierrez RA, Sorn S, and Buchy P (2012). Environment: a potential source of animal and human infection with influenza A (H5N1) virus. Influenza Other Respi Viruses 6:442-448.
IEDCR (2012a) Fifth and Sixth H5N1 Human Case in Bangladesh. http://www.iedcr.org/pdf/files/influenza/Fifth_and_Sixth_H5N1.pdf. Accessed September 20, 2013.
IEDCR (2012b) Fourth H5N1 Human Case in Bangladesh. http://www.iedcr.org/pdf/files/influenza/Fourth-H5N1-human-case-in-Bangladesh.pdf. Accessed September 20, 2013.
Islam MR, Haque ME, Giasuddin M, Chowdhury EH, Samad MA, Parvin R, et al. (2011). New Introduction of Clade 2.3.2.1 Avian Influenza Virus (H5N1) into Bangladesh. Transbound Emerg Dis 59: 460-463.
Jackson S, Van Hoeven N, Chen LM, Maines TR, Cox NJ, Katz JM, et al. (2009). Reassortment between avian H5N1 and human H3N2 influenza viruses in ferrets: a public health risk assessment. J Virol 83:8131-8140.
Kandeel A, Manoncourt S, Abd el Kareem E, Mohamed Ahmed AN, El-Refaie S, Essmat H, et al. (2010). Zoonotic transmission of avian influenza virus (H5N1), Egypt, 2006-2009. Emerging Infectious Diseases 16:1101-1107.
Liu T (2008). Custom, taste and science: raising chickens in the Pearl River Delta Region, South China. Anthropology & Medicine 15:7-18.
Loth L, Gilbert M, Osmani MG, Kalam AM, and Xiao X (2010). Risk factors and clusters of Highly Pathogenic Avian Influenza H5N1 outbreaks in Bangladesh. Prev Vet Med 96:104-113.
Maas R, Tacken M, Ruuls L, Koch G, van Rooij E, and Stockhofe-Zurwieden N (2007). Avian influenza (H5N1) susceptibility and receptors in dogs. Emerging Infectious Diseases 13:1219-1221.
Manabe T, Pham TP, Vu VC, Takasaki J, Dinh TT, Nguyen TM, et al. (2011). Impact of educational intervention concerning awareness and behaviors relating to avian influenza (H5N1) in a high-risk population in Vietnam. PLoS One 6:e23711.
Manabe T, Tran TH, Doan ML, Do TH, Pham TP, Dinh TT, et al. (2012). Knowledge, attitudes, practices and emotional reactions among residents of avian influenza (H5N1) hit communities in Vietnam. PLoS One 7:e47560.
OIE (2013) Update on Highly Pathogenic Avian Influenza in Animals (Type H5 and H7). Follow-up Report 42. http://www.oie.int/wahis_2/public%5C..%5Ctemp%5Creports/en_fup_0000013335_20130430_165153.pdf. Accessed August 24, 2013.
Oner AF, Bay A, Arslan S, Akdeniz H, Sahin HA, Cesur Y, et al. (2006). Avian influenza A (H5N1) infection in eastern Turkey in 2006. N Engl J Med 355:2179-2185.
Padmawatia S, and Nichter M (2008). Community response to avian flu in Central Java, Indonesia. Anthropology & Medicine 15:31-51.
Paul M, Baritaux V, Wongnarkpet S, Poolkhet C, Thanapongtharm W, Roger F, et al. (2013). Practices associated with Highly Pathogenic Avian Influenza spread in traditional poultry marketing chains: Social and economic perspectives. Acta Trop 126:43-53.
Pelto PJ, and Pelto GH (1997). Studying knowledge, culture, and behavior in applied medical anthropology. Medical Anthropology Quarterly 11:147-163.
Rabinowitz P, Perdue M, and Mumford E (2010). Contact variables for exposure to avian influenza H5N1 virus at the human-animal interface. Zoonoses Public Health 57:227-238.
Rahman MW, Gurley ES, Islam MS, Aleem MA, Salimuzzaman M, Sharif AR, et al. (2013) The first reported fatal pediatric case of H5N1 with atypical symptoms, Bangladesh. In: Options for the Control of Influenza VIII Conference, Cape Town, South Africa.
Regenstein JM CM, Regenstein CE (2003). The kosher and halal food laws. Comprehensive Reviews in Food Science and Food Safety 2:111-127.
Rimi NA, Sultana R, Khan S, Nasreen S, Puri A, Alamgir ASM, et al. (2013) Biosecurity conditions and biosafety practices in the live bird markets of Dhaka city, Bangladesh, 2012. In: Options for the Control of Influenza VIII conference, Cape Town, South Africa.
Sultana R, Nahar N, Rimi NA, Azad S, Islam MS, Gurley ES, et al. (2012a). Backyard poultry raising in Bangladesh: a valued resource for the villagers and a setting for zoonotic transmission of avian influenza. A qualitative study. Rural Remote Health 12:1927.
Sultana R, Rimi NA, Azad S, Islam MS, Khan MS, Gurley ES, et al. (2012b). Bangladeshi backyard poultry raisers’ perceptions and practices related to zoonotic transmission of avian influenza. J Infect Dev Ctries 6:156-165.
UNICEF Bangladesh (2007) Avian Influenza Knowledge, Attitude and Practice (KAP) Survey among the General Public and Poultry Farmers in Bangladesh. Dhaka: UNICEF Bangladesh.
Van Kerkhove MD (2012). Poultry Movement and Sustained HPAI Risk in Cambodia. In: Health and Animal Agriculture in Developing Countries, Van Kerkhove MD, editor, pp. 233–263. New York: Springer.
Van Kerkhove MD, Ly S, Holl D, Guitian J, Mangtani P, Ghani AC, et al. (2008). Frequency and patterns of contact with domestic poultry and potential risk of H5N1 transmission to humans living in rural Cambodia. Influenza Other Respi Viruses 2:155-163.
Van Kerkhove MD, Ly S, Guitian J, Holl D, San S, Mangtani P, et al. (2009). Changes in poultry handling behavior and poultry mortality reporting among rural Cambodians in areas affected by HPAI/H5N1. PLoS One 4:e6466.
Van Kerkhove MD, Mumford E, Mounts AW, Bresee J, Ly S, Bridges CB, et al. (2011). Highly pathogenic avian influenza (H5N1): pathways of exposure at the animal-human interface, a systematic review. PLoS One 6:e14582.
Vong S, Ly S, Van Kerkhove MD, Achenbach J, Holl D, Buchy P, et al. (2009). Risk factors associated with subclinical human infection with avian influenza A (H5N1) virus-Cambodia, 2006. J Infect Dis 199:1744-1752.
Webster RG, Yakhno M, Hinshaw VS, Bean WJ, and Murti KG (1978). Intestinal influenza: replication and characterization of influenza viruses in ducks. Virology 84:268-278.
WHO (2006a) Human Cases of Influenza A (H5N1) Infection in Eastern Turkey, December 2005–January 2006. Geneva: WHO. http://www.who.int/wer/2006/wer8143.pdf.
WHO (2006b) Review of Latest Available Evidence on Potential Transmission of Avian Influenza (H5N1) Through Water and Sewage and Ways to Reduce the Risks to Human Health. Geneva: WHO.
WHO (2007) Avian Influenza: Food Safety Issues. Geneva: WHO. http://www.who.int/foodsafety/micro/avian/en/index1.html. Accessed March 1, 2012.
WHO (2013) Cumulative Number of Confirmed Human Cases of Avian Influenza A/(H5N1). Geneva: WHO. http://www.who.int/influenza/human_animal_interface/H5N1_cumulative_table_archives/en/index.html. Accessed September 20, 2013.
Zhou L, Liao Q, Dong L, Huai Y, Bai T, Xiang N, et al. (2009). Risk factors for human illness with avian influenza A (H5N1) virus infection in China. J Infect Dis 199:1726-1734.
Acknowledgments
This research was funded by the Centers of Disease Control and Prevention (CDC) under the agreement of CoAg Grant 5-U51-CI000298. icddr,b acknowledges the commitment of CDC to its research efforts with gratitude. We are grateful to our study participants for their time and invaluable information. We thank Marufa Hasin, Afroza Khanam Roza, and Md. Zahidur Rahman for their valuable contribution in data collection, Shamim Azad for his contribution to data organizing and Kamal Hossain for preparing the map. We also thank Dorothy Southern for her guidance in writing and Andrea Mikolon, Najmul Haider, and Meghan Scott for reviewing the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rimi, N.A., Sultana, R., Ishtiak-Ahmed, K. et al. Poultry Slaughtering Practices in Rural Communities of Bangladesh and Risk of Avian Influenza Transmission: A Qualitative Study. EcoHealth 11, 83–93 (2014). https://doi.org/10.1007/s10393-013-0885-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10393-013-0885-8