Abstract
Aim
This study aims to understand the levels and trends of the utilization of antenatal care services and its determinants in Cambodia.
Subject and methods
The study used the data of most recent rounds of nationally representative Cambodian Demographic Health Surveys (CDHS) during 2000–2010. The data was analysed using IBM SPSS 21.0 software and the analytical approach includes both bivariate and multivariate analyses. Arc GIS 10.1 software was used to show the geographic variation in utilization of the antenatal care services.
Results
The utilization of antenatal care services was found to be low along with wide variation according to socio-economic and regional characteristics. Higher education, exposure to mass media and economic condition of the household were the significant enablers, while higher birth order, bigger household size and rural residence were the major barriers to utilization of the antenatal care services. The majority of the women (79 %) had received antenatal care services from midwives. Women in coastal regions (AOR = 0.58, p < .01) and plateau and mountain regions (AOR = .0.41, p < .01) were significantly less likely to get antenatal care by skilled health providers as compared to those in the plains region.
Conclusion
Tailor-made region-specific programs, in addition to accessible antenatal care services with intensive information for the economically backward and less educated women would enhance the utilization, thereby ensuring better antenatal health in Cambodia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Maternal mortality and morbidity possesses a strong challenge to human development worldwide. About 99 % of the maternal deaths come from developing nations and often is a result of the shameful failure of the health system in these countries (WHO 2005). World Health Organization (WHO) estimates reveal more than half of a million women died due to pregnancy related causes in 2005 (UNICEF 2008). Globally, approximately 80 % of the maternal deaths occur due to causes directly related to pregnancy (Kvale et al. 2005). These deaths are unjust and can be prevented with key health interventions such as the provision of antenatal care (ANC) and medically assisted delivery (Adam et al. 2005; MCcaw-Binns et al. 2007).
Large-scale programmatic interventions over the past two decades led to a decline in maternal mortality rates. The decline however remains slow and uneven, both across and within different countries (Filippi et al. 2006; Lawn et al. 2006; Graham et al. 2004). Several studies and interventions in the past few decades identified three key elements to reduce maternal mortality and improve neonatal health, including (1) family planning, (2) skilled birth attendance for all deliveries, and (3) access to emergency obstetric care for all women with life threatening complications. In addition to this, attendance of skilled health personnel and emergency obstetric care works as a direct prevention to unwanted deaths of women (Freedman et al. 2003; Ronsmans and Graham 2006). Effective access to care during pregnancies and after the deliveries further reduces the chance of complications among women. Therefore, the three components of maternal health services—ANC services, delivery attended by skilled birth attendants and postnatal care—remain a priority in safe motherhood programmes and policies of developing countries.
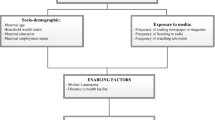
There are many models and theories explaining factors associated with utilization of health care services. Andersen (1968) developed a model of health care utilization (Fig. 1) which looked upon three categories of determinants: (1) predisposing characteristics, i.e. the inclination to utilize health care services; (2) resources found within the family and the community; and (3) need-based characteristics. According to Andersen, an individual’s likelihood to use health services is based on demographics, position within the social structure, and beliefs regarding health services benefits. An individual who believes health services are useful for treatment is likely to use those services, enabling characteristics which includes resources found within the family and the community. Family characteristics such as economic status and the location of residence are important. Community resources incorporate access to health care facilities and the availability of persons for assistance, which includes the third category—the perception of need for health services, whether individual, social, or clinically evaluated perceptions of need (Wolinsky 1988). This model stresses that, besides health belief and community factors, individual and household socio-economic factors strongly influence the utilization of healthcare services.
Andersen’s behavioral model of health services utilization (Wolinsky 1988)
Several studies also suggest that different socio-economic and demographic factors significantly affect utilization of ANC services. There is a strong relationship between birth order and utilization of maternal and child health care services (Elo 1992; Nigussie et al. 2004; Wong et al. 1987; Govindasamy and Ramesh 1997). Having a larger number of children may cause resource constraints, which has been found to be negatively associated with use of maternal and child health care services (Wong et al. 1987; Chakraborty et al. 2003). A larger family also places more demand on a woman’s time thereby limiting her ability to access healthcare (Chakraborty et al. 2003). Research in developing countries has consistently shown maternal schooling to be strongly and positively associated with utilization of maternal health care services (Elo 1992; Nigussie et al. 2004; Chakraborty et al. 2003). The location and quality of available services are also important factors affecting utilization of maternal health care services. For many, lack of transportation, cost of transportation and distance from health facilities serve as mitigating factors to seeking health care. For others, the low quality of services and anticipation of poor behaviour from health staffs are the mitigating factors.
Cambodia, one of the developing countries in South-East Asia is at risk of failing its Millennium Development Goal commitment to reduce the maternal mortality ratio (MMR) to less than 140 deaths per 100,000 live births by 2015 (UN 2010). According to the latest available data, MMR in Cambodia was 206 maternal deaths per 100,000 live births (Ministry of Health 2008). The government of Cambodia took steps to strengthen maternal and child care services as early as in the first and second Five-Year Health Sector Plans—Health Sector Strategic Plan 2003–2007 and 2008–2015.
Cambodia’s National Reproductive Health Program found that despite of high demand of skilled birth attendants (SBA), access continues to be constrained by the cost and distance to appropriate facilities. A continuing trend is observed among young women with higher income using SBAs more frequently, while older and poorer women use traditional birth attendants (TBAs) because they are more familiar to them and are closer to home (Connell 2011). The study in Krong Kep province, Cambodia, demonstrates that the lack of resources, availability of quality services, and distance to health centres in the rural province may be linked to the continued use of traditional birthing practices and medicine (Montesanti 2011). Furthermore, cultural beliefs and practices surrounding pregnancy and childbirth are important not only because of women’s affiliation and identification with their culture, but because such cultural beliefs allow women to make sense of their maternal experiences, and to care for their health when other options of care and treatment are limited by their economic circumstances.
The Ministry of Health (MOH) states that most Cambodians prefer to visit pharmacies and traditional healers for health advice and medicine, especially for sexual and maternal health care to avoid discrimination from health staff. This also includes the use of TBAs to assist in the delivery of babies. This may be reflective of the negative experience that women have in referral hospitals and/or the health centres, along with structural determinants such as transportation and economic barriers for families in the villages (Maternowska 2000). Limited health care staff further impedes the quality and access to care that women receive. On this note, the present study attempts to understand the levels and trends of the utilization of ANC services and its determinants among currently married women in Cambodia.
Methods
Data
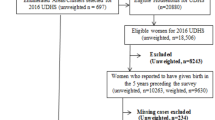
This study used data from three rounds of the Cambodia Demographic and Health Survey (CDHS, 2000, 2005 and 2010) for trend analysis. Currently married women aged 15–49 years of the CDHS-2010 were considered for detailed analysis of differential and determinants of ANC services utilization. The 2010 CDHS was a nationally representative sample survey of 18,754 women and 8,239 men aged 15–49 years. A multistage stratified sampling design was adopted to choose the respondents for the survey. The 2010 CHDS collected information on demography, family planning, maternal mortality, infant and child mortality, women’s healthcare status including ANC, delivery care, postnatal care, breastfeeding, children’s immunization, childhood diseases, and HIV/AIDS.
Statistical analysis
The data was analysed using IBM SPSS 21.0 software and the analytical approach includes both bivariate and multivariate analyses. The bivariate analysis examined the differential in various components of ANC services via different socio-economic variables. Logistic regression was carried out to understand the factors affecting the utilization of ANC services. ArcGIS 10.1 software was used to understand the geographic variation, especially at the provincial level, regarding the utilization of the ANC services.
Outcome variables
Antenatal care was measured using the following three vital indicators:
-
1.
Full antenatal care. Women who had utilized all three components of ANC services—four or more antenatal visits, received two or more tetanus toxic (TT) injections during pregnancy, and took 90+ iron folic acid (IFA) tablets—were considered to have full ANC.
-
2.
Antenatal care by a skilled health provider. Women who had received ANC by a doctor, nurse, or midwife were considered to have ANC by skilled health providers.
-
3.
Components of antenatal checkups. Women who were informed about their signs of pregnancy complications, who had been weighed, whose blood pressure had been measured, urine and blood samples taken, were considered to have various components of an antenatal checkup.
Independent variables
-
1.
Individual factors considered for analysis are—age at birth (less than 20, 20–24, 25–29, 30–34, 35–49 years), women’s education (no education, primary, secondary and higher), women’s occupation (working, not working), birth order (1,2,3–4, 5+), final say on health care (women independently, women with partner, other family members), exposure to mass media (no exposure, partial exposure, high exposure), and education level of the partner (no education, primary, secondary and higher).
-
2.
Household factors included in the analysis are—wealth index (poorest, poorer, middle, richer, richest), number of household members (<= 4, 5+), and religion (Buddhist, others)
-
3.
Contextual factors included in the analysis are—place of residence (urban, rural) and region (Plains region, Tonle Sap region, Coastal region, Plateau and mountain region, Table 1.
Results
Trends of antenatal care services utilization
The data in Fig. 2 reveals the trend in utilization of full ANC, ANC by skilled health provider and ANC by TBA in Cambodia. The results found a steady increase in full ANC from less than 1 % in 2000 to 30 % in 2010. Between 2005 and 2010, an enormous increase had been found in utilization of full ANC, which increased from 7 % to 30 % in 2010. All the components of ANC had also gone up in the 10 years duration. Utilization of 2+ TT injections during pregnancy had doubled in the last 10 years, i.e. from 30 to 60 %, 4+ ANC visits had gone up to 59 % from 7 % and use of 90+ IFA tablets during pregnancy had increased from 1 % in 2000 to 59 % in 2010. During the same period, the ANC by skilled health providers had gone up from 38 to 89 %.
Differentials in utilization of antenatal care services and its components
Utilization of full ANC
Table 2 presents the percentage of women utilizing full ANC services and its components for the most recent live birth in the last 5 years preceding the survey by different social, economic and demographic characteristics. Thirty percent of women had received full ANC. About three in five women (59 %) made four or more ANC visits during their pregnancy. The percentage of women who reported receiving two or more TT injections was 61 % and those who reported consuming more than 90 IFA tablets was 57 %. Utilization of full ANC services was found to be high among women whose age at childbirth was 20–24 years (36 %) as compared to women whose age at childbirth was 35–49 years (20 %). The percentage of women with secondary and higher education (45 %) showed higher utilization of ANC than women with only primary education (27 %) and women with no education (18 %). Similarly, women with more educated partners were found to have higher utilization of full ANC services (39 %) than women without an educated partner.
There was a wide variation among women who had received full ANC by birth order. As the birth order increases from one to five, the utilization of full ANC services decreases from 45 % among women having first birth order to 14 % among women having a birth order of five and more. Exposure to mass media had a positive bearing in utilization of full ANC services. About 35 % women who were fully exposed to different sources of mass media like TV, radio and newspaper received full ANC services as opposed to 18 % of the women without any exposure to mass media. Every second woman from the richest wealth quintiles (50 %) had full ANC services as compared to women from richer (37 %), middle (29 %), poorer (22 %) and poorest (19 %) quintiles. Utilization of full ANC was found highest among women from the Plains region (32 %), followed by women from Tonal Sap region (31 %), Plateau and mountain region (25 %) and Coastal region (23 %).
Figure 3 shows the level of full ANC among women for the most recent birth in the last 5 years preceding the survey at the provincial level. The provinces from the north-eastern parts of the country had the lowest use of full ANC (less than 15 %), whereas Phnom Penh and Banteay Meanchey had the highest percentage (45 % and above) of women receiving full ANC.
Utilization of TT injections
Around 65 % of younger women (aged less than 20 years) reported receiving two or more TT injections as compared to 50 % of the older women aged 35–49 years. A higher percentage of women with birth order one had received two or more TT injections (45 %) than women with higher birth orders. A majority of women from the richest wealth quintile (70 %) were found to have received two or more TT injections as compared to women belonging to richer (66 %), middle (63 %), poorer (58 %) and poorest (51 %) wealth quintiles. The urban rural differential was found prominent with a higher percentage of women from the urban area (70 %) receiving two or more TT injections than women from rural areas (59 %). Around 63 % women from the Plains region had received two or more TT injections followed by women from the Tonle Sap region (59 %), Plateau and mountain region (57 %) and Coastal region (55 %).
The number of ANC visits
Having an educated partner plays a significant role in utilizing ANC services more than four times. It is evident that 72 % of the women whose partners are educated at the secondary and higher levels had visited a facility more than four times for ANC services as compared to 41 % of those women with non-literate partners. Four or more ANC visits had much higher representation among women at the first order of their birth (72 %), as compared to those women who were with their fifth or more birth order (34 %). Additionally, a much higher percentage of Buddhist women (60 %) had gone for four or more ANC visits, compared to the non-Buddhist women (39 %). A higher percentage of women belonging to the richest wealth quintiles (83 %), exposed to mass media (TV, radio, and newspaper, 66 %), having high health care autonomy (62 %), and living in urban areas (80 %) utilized facilities for ANC four or more than four times as compared to their counterparts. Huge regional variation had been found in terms of visiting facilities for ANC four or more times. About 63 % of women from the Plains region and Tonle Sap region had gone for ANC visits four or more times. The corresponding figures were 47 % in both the Coastal region and Plateau and mountain region.
Consumption of 90+ IFA tablets
Wide variations by women according to age at childbirth had been found regarding consumption of 90 and more IFA tablets . About 59 % of women who were less than 20 years of age at childbirth have taken 90+ IFA tablets; however, with increasing age at childbirth beyond 20 years (61 %), the proportion goes down and it was found to be lowest in 48 % of mothers who were 35–49 years of age at childbirth. Results further reveal that, more educated women (72 %) compared to uneducated women (44 %), and women with an educated partner (67 %) compared to having an uneducated partner (40 %) had consumed more than 90 IFA tablets. A higher percentage of women belonging to the richest wealth quintiles (76 %) living in an urban area (74 %) belonging to the Plains region (59 %) had consumed more than 90 IFA tablets compared to their counterparts.
Antenatal care provider
Table 3 explains the ANC providers of women by most recent birth within the last 5 years preceding the survey. Ninety percent of the women had received any ANC services from different health providers. The majority of the women (79 %) preferred to go to midwives for ANC, which was followed by those who preferred to see a doctor (9 %). Higher percentages of younger women (92 %) had received ANC from skilled health providers as compared to older aged women (80 %). The utilization of ANC services from a doctor was high among working women (13 %) compared to those not working (9 %).
A universal ANC care by skilled health providers (96 %) was observed among women with first order birth. Data revealed that 12 % of the women with a first order birth had sought the services from a doctor. The corresponding figure was merely 5 % among women with birth order 5 and more. A higher percentage of women (25 %) had not sought any ANC services for their children of birth order 5 and more, compared to women with birth order one (4 %). A higher percentage of women with secondary education or more had received ANC from a doctor (19 %) compared to women with a primary education (7 %) or no education (4 %). Twenty-two percent of the uneducated women received no ANC at all, with the proportion decreasing to 10 % among women with a primary school education. A higher percentage of women with an educated partner with a secondary or higher level of education had received ANC from skilled health professional (96 %) as compared to women with an uneducated partner (77 %).
Utilizing the assistance of ANC services of skilled health providers showed a gradual increase in women from the poorest to richest (79–99 %) wealth quintiles. There exists wide regional variation in utilization of ANC services according to the type of provider. About 92 % of women from the Plains region had received ANC from skilled health providers. The corresponding figures were 90 % in Tonle Sap region, 87 % in the Coastal region, 77 % in the Plateau and mountain region. As far as ANC from a doctor was concerned, it was used by 14 % women from the Plains region, 8 % of those from Tonle Sap region and merely 2 % of women from both the Coastal region and Plateau and mountain region.
Figure 4 shows the percentage of women who had gone for ANC services from skilled health providers at the provincial level. There exists wide variation in the utilization rate and the lowest percentage of women from north-eastern provinces had received ANC by a skilled health provider. It was evident that less than 65 % of women in north-eastern provinces such as Mondul Kiri and Ratanak Kiri have received ANC from skilled health providers. More than 90 % of the women from the Phnom Penh, Prey Veng, Takeo, Kampong Speu, Battambang, Pailin, Pursat, Svay Rieng, and Siem Reap provinces had received the services from a skilled health provider.
Component of antenatal check-ups
The effectiveness of ANC check-ups for enduring safe motherhood depends in part on the tests and measurements done as well as advice given during the check-up, which is very beneficial in preventing adverse pregnancy outcomes. Table 4 shows the various components of ANC services received by women for their most recent birth in the last 5 years. Eighty percent of the women who had received ANC showed that they were informed about pregnancy-related complications by health providers during their visit. Blood pressure and weight measurements were part of ANC for 91 % of women. Urine and blood sample were taken from 36 and 45 % of the women, respectively during their ANC visit. The percentage distribution of women having various components of ANC varies according to different socio-economic characteristics of the women. With increasing age at childbirth, the reporting of being informed about pregnancy complications by health providers also increases (74 % among women aged <20 vs. 82 % among aged 35–49 during childbirth). However, a relatively higher percentage of the younger women compared to their older counterparts had gone for the other routine tests. For example, 92 % of the women aged below 20 during childbirth had been weighed during the routine ANC check-up compared to 88 % of those aged 35–49 years at the time of childbirth. The corresponding figures were 91 and 87 %, respectively, as far as blood pressure measurement is concerned.
ANC component is also greatly affected by the level of mother’s education. Women with secondary or higher level of education had received all routine tests than less educated women. A higher percentage of the women from the richest quintile were found to have been informed about pregnancy complications and had also utilized the routine check-ups compared to those from the poorest quintile. Again, a higher percentage of women from the Buddhist community, those living in urban area and highly exposed to mass media were informed of pregnancy complications by health providers and had participated more in the routine check-ups during pregnancy compared to their counterparts. Regional variations for various components of ANC are marked. Women residing in the Tonle Sap region had received all components of ANC more often than women from other regions.
Multivariate analysis
In order to understand the adjusted effect of different socio-economic and demographic factors on utilization of full ANC and ANC from skilled health providers, we carried out binary logistic regression. The result from Table 5 shows women’s education, age at childbirth, birth order, economic status of household and religion played a significant role in women going to a skilled health provider for ANC. Education, older age at childbirth, mass media exposure and economic status of household played a positive role on access to a skilled health provider for ANC. For instance, women with secondary or higher education were about three times (AOR = 2.87, p < 0.01) more likely to go for ANC from a skilled health provider than women with no education. The likelihood of ANC from skilled health providers is significantly higher among those aged 20–24 at childbirth than those aged below 20 years (AOR = 1.76, p < 0.01). Women with high mass media exposure had 41 % more chance of going to a skilled health provider for ANC than women without any mass media exposure.
The women from the richest household quintile were four times more likely to use ANC from a skilled health provider than the women from the poorest household quintile. The result shows that with increase in birth order, the access to ANC from a skilled health provider goes down, as women with more than five children are 85 % less likely to go to a skilled health provider for ANC than women with a single child. As compared to the women who were Buddhists, the non-Buddhists were significantly less likely (AOR = 0.54, p < 0.01) to access ANC from a skilled health provider. The women from the Coastal region and Plateau and mountain regions showed less likelihood of selecting a preferred skilled health provider for ANC than those from the Plains region.
Women’s education, older age at childbirth, exposure to mass media, and economic status were positively and significantly associated with utilization of full ANC. Women having primary education (AOR = 1.24, p < 0.05) and secondary or higher education (AOR = 1.50, p < 0.01) were significantly more likely to access full ANC than women with no education. The likelihood of full ANC is significantly higher among those aged 20–24 at childbirth than those aged below 20 years (AOR = 1.33, p < 0.01). Women with high mass media exposure had 23 % more chance of going for full ANC than women without any mass media exposure. Women from richest households were two times more likely to use full ANC than women from poorest households. On the other hand, birth order, place of residence, religion and geographical region showed a significantly negative association with access to full ANC. With increase in birth order, the likelihood of women accessing full ANC declines. The women from rural areas were 33 % less likely to go for full ANC than urban women. Non-Buddhist women were 44 % less likely to go for full ANC than Buddhists. As compared to the women from the Plains region, those from Tonle Sap region were significantly more likely and those from the Coastal region were less likely to use full ANC.
Discussion
The association of individual, household and contextual factors with the utilization of ANC services in Cambodia were assessed in this study. The results of our study showed very strong positive influence of higher household socio-economic status on the use of all components of ANC services. This finding is in conformity with a previous study conducted in a southern Indian state, which reported a positive association between socio-economic status and ANC (Bhatia and Cleland 1995). The study reveals a positive influence of higher education on the use of ANC services. The finding of our study that better educated women were more aware about utilization of ANC services is supported by studies conducted in India, Papua New Guinea, South Asia and Sub-Saharan Africa, Thailand and other countries (Tey and Lai 2013; Navaneetham and Dharmalingam 2002; Raghupathy 1996; Maraga et al. 2011). Partner’s education also playing a similar role in supporting the women’s access to the ANC services (Tey and Lai 2013). The findings that higher maternal age at childbirth leads to higher use of full ANC is in contradiction to many past studies (Regassa 2011; Ali et al. 2010). Some other studies suggested that women in their thirties are more likely to utilize ANC than teenagers (Simkhada et al. 2008). This is perhaps because teenagers are not expecting to become pregnant; thus, they tend to use less ANC in developing countries. Another Indian study found that utilization of all the components of maternal health care was lower among teenage mothers (Datta and Manna 2012). Higher age at childbirth probably comes with more awareness and ability to access the required ANC services and, thus, leads to higher utilization for Cambodian women. The study finds lower use of full ANC in households with more than five members, which is again in contrary to many past studies (Gaur et al. 2014; Matsumura and Gubhaju 2001). The probable reason may be the uniqueness of Cambodian family structure. The extended families might have members from older generations with traditional cultural beliefs and ideas about pregnancy, which can have a negative influence on ANC use by women.
Ethnicity plays a significant role in utilization of ANC services, which is an important finding of our study, where the Buddhist community is in an advantageous position. This finding is supported by another study in Vietnam which indicates that inequity in maternal health care utilization has increased progressively in Vietnam, primarily among ethnic lines (Malqvist et al. 2013). The findings of our study suggest that skilled health providers are having a remarkable effect on the utilization of ANC services. A study conducted in rural India also recorded similar findings (Dilip and Mishra 2009). Findings of previous studies (Govindasamy and Ramesh 1997; Jat et al. 2011; Chakraborty et al. 2003; Ahmed et al. 2010; Zere et al. 2011; Sharif and Singh 2002; Woldemicael 2007; Bashour et al. 2008; Daru et al. 2014) are also in conformity to our findings that women’s educational level, wealth quintile, and place of residence all had a significant positive impact on the utilization of ANC services. Our findings further corroborate the findings of previous studies indicating that better exposure to the media increases the utilization of maternal care services (Govindasamy and Ramesh 1997; Agha and Carton 2011). Geographical variation in utilization of ANC services due to variations in implementation of maternal health care program as well as availability and accessibility between regions is well evident in past studies (Prusty et al. 2015; Singh et al. 2014; Navaneetham and Dharmalingam 2002). The current study found that women from the Coastal and Plateau and mountain regions have a lower proportion of women who utilized full ANC services than the women from the Plains and Tonle Sap regions in Cambodia.
The health care that a woman receives during pregnancy and at the time of delivery is important for the survival and well-being of both the mother and the child. Antenatal care from a trained provider is vital in monitoring the pregnancy and reducing morbidity risk for the mother and child during pregnancy and delivery. There is vast improvement in utilization of maternal health care services in Cambodia in term of the utilization of ANC. This study found an increasing trend in utilization of full ANC services between 2005 and 2010. It is also of importance that a majority of the women were informed of pregnancy complications by health providers during their visit. Routine check-ups at time of pregnancy were also found to be increasing. The study findings are also supported by many studies which argued about an increasing pattern of utilization of health services along with increasing socio-economic conditions. These findings are equally useful in formulating programs and policies to improve maternal health services in the country as a whole.
Although there has been steady improvement in utilization of ANC, the utilization of all components of ANC services is found to be low; and, this is found to be even lower in rural areas and the coastal and mountainous region. It can also be concluded that media has a great role to play as it has a significant influence in access to all the components of ANC found in the study. This study suggests strengthening maternal education related to ANC services in all regions of the country, which will improve use of all the constituents of ANC services. Focus should be on the north-eastern part of the country as it is found to have low utilization of these services. Accessible ANC services with intensive information for the economically underprivileged and less educated women and enhanced awareness for safe motherhood will lead to high utilization of services, thereby ensuring better antenatal health in Cambodia.
References
Adam T, Lim S, Mehta S, Bhutta ZA, Fogstad H et al (2005) Cost effectiveness analysis of strategies for maternal and neonatal health in developing countries. Br Med J 331(7525):1107. doi:10.1136/bmj.331.7525.1107
Agha S, Carton TW (2011) Determinants of institutional delivery in rural Jhang, Pakistan. Int J Equity Health 10(1):31. doi:10.1186/1475-9276-10-31
Ahmed S, Creanga A, Gillespie DG, Tsui AO (2010) Economic status, education and empowerment: implications for maternal health service utilization in developing countries. PLoS ONE 5(6):e11190. doi:10.1371/journal.pone.0011190
Ali A, Osman M, Abbaker AO, Adam I (2010) Use of antenatal care services in Kassala, eastern Sudan. BMC Pregnancy Childbirth 10(1):67
Bashour H, Abdulsalam A, Al-Faisal W, Cheikha S (2008) Patterns and determinants of maternity care in Damascus. Eastern Mediterranean Health J 14(3)
Bhatia JC, Cleland J (1995) Determinants of maternal care in a region of South India. Health Transit Rev 5:127–142
Chakraborty N, Islam MA, Chowdhury RI, Bari W, Akhter HH (2003) Determinants of the use of maternal health services in rural Bangladesh. Health Promot Int 18(4):327–337. doi:10.1093/heapro/dag414
Connell SE (2011) Maternal mortality in Cambodia: efforts to meet the millennium development goal for maternal health. Public Health Thesis paper 198, Georgia State University, Atlanta, GA
Datta M, Manna N (2012) A study on socio-demographic correlates of maternal health care utilization in a rural area of West Bengal, India. GJMEDPH 1(4):7–12
Dilip TR, Mishra US (2009) Social divide in maternal health care use in rural India: the relative impact of education and economic status. In: International Population Conference, IUSSP Marrakech, Morocco. Available: http://iussp2009.princeton.edu/papers/90364. Accessed 25 February 2014
Duru CB, Eke NO, Ifeadike CO, Diwe KC, Uwakwe KA, Nwosu BO, Chineke HN (2014) Antenatal care services utilization among women of reproductive age in urban and rural communities of South East Nigeria: a comparative study. Afrimedic J 5(1):50–58
Elo IT (1992) Utilization of maternal health-care services in Peru: the role of women’s education. Health Transit Rev 2(1):49–69
Filippi V, Ronsmans C, Campbell OM, Graham WJ, MillsA BJ et al (2006) Maternal health in poor countries: the broader context and a call for action. Lancet 368(9546):1535–1541
Freedman L, Wirth M, Waldman R, Chowdhury M, Rosanfield A (2003) Background paper of the task force on child health and maternal health. Millennium Project Commissioned by UN Secretary General and supported by UN Development Group. Available at http://www.unmillenniumproject.org/documents/tf04apr18.pdf. Accessed 25 February 2014
Gaur KL, Gupt P, Kuldeep R, Sharma MC, Gupta R, Manohar RK (2014) Factors associated with antenatal care services utilization and institutional deliveries. IOSR J Dent Med Sci 13(4):96–100
Govindasamy P, Ramesh BM (1997) Maternal education and the utilization of maternal and child health services in India. Working Paper, International Institute for Population Sciences, Mumbai, Macro, Calverton, MD
Graham WJ, Fitzmaurice AE, Bell JS, Cairns JA (2004) The familial technique for linking maternal death with poverty. Lancet 363(9402):23–27
Jat TR, Ng N, San Sebastian M (2011) Factors affecting the use of maternal health services in Madhya Pradesh state of India: a multilevel analysis. Int J Equity Health 10(1):59
Kvale G, Olsen BE, Hinderkar SG, Ulstein M, Bergsjo P (2005) Maternal deaths in developing countries: a preventable tragedy. Norsk Epidemiol 15(2):141–149
Lawn JE, Tinker A, Munjanja SP, Cousens S (2006) Where is maternal and child health now? Lancet 368(9546):1474–1477
Malqvist M, Lincetto O, Du NH, Burgess C, Hoa DTP (2013) Maternal health care utilization in Viet Nam: increasing ethnic inequity. Bull World Health Organ 91(4):254–261
Maraga S, Namosha E, Gouda H, Vallely L, Phuanukoonnon S (2011) Sociodemographic factors associated with maternal health care utilization in Wosera, East Sepik Province, Papua New Guinea. Papua New Guinea Med J 54
Maternowska C (2000) A clinic in conflict: a political economy case study of family planning in Haiti. In: Russell A, Sobo E, Thompson M (eds) Contraception across cultures. Bloomsbury, New York
Matsumura M, Gubhaju B (2001) Women’s status household structure and the utilisation of maternal health services in Nepal. Asia-Pac Popul J 16(1):23–44
MCcaw-Binns A, Lagrenade J, Ashley D (2007) Under-users of antenatal care: a comparison of non-attenders and late attenders for antenatal care with early attenders. Soc Sci Med 40(7):1003–1012
Ministry of Health (2008) Country report on caring and promoting health for mother and child toward healthy next generation in Cambodia, 25 July 2008. Available: http://www.mhlw.go.jp/bunya/kokusaigyomu/asean/asean/kokusai/siryou/dl/h20_cambodia1.pdf. Accessed 25 January 2014
Montesanti S (2011) Cultural perceptions of maternal illness among Khmer women in KrongKep, Cambodia. Vis-à-vis Explor Anthropol 11(1):90–106
Navaneetham K, Dharmalingam A (2002) Utilization of maternal health care services in southern India. Soc Sci Med 55(10):1849–1869
Nigussie M, Haile Mariam D (2004) Mitike, G (2004) Assessment of safe delivery service utilization among women of childbearing age in north Gondar zone, northwest Ethiopia. Ethiop J Health Dev 18(3):145–152
Prusty RK, Gouda J, Pradhan MR (2015) Inequality in the utilization of maternal healthcare services in Odisha, India. Int J Popul Res. Available http://dx.doi.org/10.1155/2015/531485. Accessed 25 May 2015
Raghupathy S (1996) Education and the use of maternal health care in Thailand. Soc Sci Med 43(4):459–471
Regassa N (2011) Antenatal and postnatal care service utilization in southern Ethiopia: a population-based study. Afr Health Sci 11(3):390–397
Ronsmans C, Graham WJ (2006) Maternal mortality: who, when, where and why? Lancet 368:1189–1200
Sharif A, Singh G (2002) Determinants of maternal health care utilization in India: evidence from a recent household survey. Working Paper no. 85, National Council of Applied Economic Research, New Delhi
Simkhada B, Teijlingen ERV, Porter M, Simkhada P (2008) Factors affecting the utilization of antenatal care in developing countries: systematic review of the literature. J Adv Nurs 61(3):244–260
Singh A, Kumar A, Pranjali P (2014). Utilization of maternal healthcare among adolescent mothers in urban India: evidence from DLHS-3. PeerJ 2:e592. Available at https://dx.doi.org/10.7717/peerj.592. Accessed 25 February 2014
Tey NP, Lai SL (2013) Correlates of and barriers to the utilization of health services for delivery in South Asia and Sub-Saharan Africa. Sci World J. doi:10.1155/2013/423403
UNICEF (2008) Progress for Children: A report card on maternal mortality, no. 7 Division of Policy and Planning. http://www.unicef.org/childsurvival/files/Progress_for_Children-No._7_Lo-Res_082008.pdfAccessed. Accessed 25 February 2014
United Nations (2010) Millennium development goal report: Southeast Asia. UN Department of Public Information, New York
Woldemicael G (2007) Do women with higher autonomy seek more maternal and child health-care? Evidence from Ethiopia and Eritrea. Health Care Women Int 31(7):599–620
Wolinsky F (1988) Seeking and using health services. In: The Sociology of health, 2nd edn. Wadsworth, Belmont, CA
Wong EL, Popkin BM, Guilkey DK, Akin JS (1987) Accessibility, quality of care and prenatal care use in the Philippines. Soc Sci Med 24(11):927–944
World Health Organization (2005) World Health Report 2005. Make every mother and child count. WHO, Geneva. Web: http://www.who.int/whr/2005/whr2005_en.pdf.. Accessed 25 February 2014
Zere E, Oluwole D, Kirigia JM, Mwikisa CN, Mbeeli T (2011) Inequities in skilled attendance at birth in Namibia: a decomposition analysis. BMC Pregnancy Childbirth 11(1):34
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Prusty, R.K., Buoy, S., Kumar, P. et al. Factors associated with utilization of antenatal care services in Cambodia. J Public Health 23, 297–310 (2015). https://doi.org/10.1007/s10389-015-0680-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10389-015-0680-9