Abstract
Introduction
Peroral esophageal myotomy (POEM) is a novel endoscopic treatment for achalasia. It has gained popularity worldwide among surgeons and endoscopists, but no studies have compared peroral endoscopic short with long myotomy for achalasia. We aimed to compare the clinical efficacy and safety between peroral endoscopic shorter and longer myotomy.
Methods
The retrospective study enrolled 129 achalasia patients who underwent POEM from July 2011 to September 2017. Based on the myotomy length (ML), patients were divided into shorter myotomy (SM) group (ML ≤ 7 cm, n = 36) and longer myotomy (LM) group (ML > 7 cm, n = 74). Procedure-related parameters, symptom scores, adverse events and manometric data were compared between two groups.
Results
The mean ML was 6.0 ± 0.6 cm in SM group, and 11.5 ± 3.1 cm in LM group (p < 0.001). The mean operation time was significantly less in SM group than LM group (46.6 ± 18.5 min vs 62.1 ± 25.2 min, p = 0.001). During a mean follow-up period of 28.7 months, treatment success (Eckardt score ≤ 3) was achieved in 94.4% (34/36) of patients in SM group and 91.9% (68/74) in LM group (p = 0.926). There was no statistical difference in the incidence of intraoperative complications (8.4% vs 8.2%, p = 0.823) and reflux rate (8.3% vs. 14.9%, p = 0.510) between two groups.
Conclusions
Peroral endoscopic shorter myotomy is comparable with longer myotomy for treating achalasia with regard to clinical efficacy and has the advantage of shorter procedure time.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Achalasia is an esophageal motility disorder involving failure of the lower esophageal sphincter (LES) to relax, presenting with dysphagia, regurgitation, chest pain, and weight loss [1, 2]. Current treatments include muscle relaxants, endoscopic injection of botulinum toxin, pneumatic balloon dilation, and surgical myotomy [3]. However, these therapies were limited for only short-term efficacy or more invasiveness [4,5,6].
Presently, peroral endoscopic myotomy (POEM) has been developed to treat achalasia as a less invasive therapy. Firstly described by Inoue et al. in 2010, this technique allows for cutting the esophageal circular muscle bundle by creation a submucosal tunnel [7]. So far, a number of studies have demonstrated that POEM could achieve an 82–100% success rate of eliminating dysphagia [8]. A major advantage of POEM is the ability to tailor myotomy length. The mean myotomy length has been reported to range from 8.2 to 14.4 cm [8], and long myotomy (> 10 cm) was applied in most studies [9,10,11,12,13,14,15]. The key of conventional treatments was to disrupt the smooth muscle of LES, thus we hypothesized that shorter myotomy could achieve a similar satisfactory outcome in comparison with longer myotomy. Currently, there are no available studies comparing treatment outcomes between shorter and longer myotomy. In this study, we compared this two myotomy methods in terms of clinical outcomes and safety.
Patients and methods
Patients
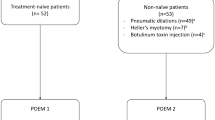
In this retrospective study, the prospectively enrolled patients (n = 129) who underwent POEM for achalasia from July 2011 to September 2017, at Shenzhen Hospital, Southern Medical University and Affiliated Hospital of Southwest Medical University were reviewed. The flowchart of this study is shown in Fig. 1. Achalasia was diagnosed with contrast fluoroscopy, esophagoduodenoscopy (EGD) and high-resolution manometry (HRM). The first 15 cases were excluded to eliminate the effect of learning curve. Four patients were lost in follow-up. Information on patients’ age, gender, symptoms duration, American Society of Anesthesiologists Class (ASA), Eckardt score, Chicago classification [16], LES resting pressure were collected. Data regarding to intraoperative, postoperative and follow-up outcomes between the two groups were compared and analyzed. Written informed consent was obtained from all patients before POEM procedure. This retrospective review was approved by the Institutional Review Board (NFEC-2016-186). All subjects gave written consent and all research was performed in accordance with the Declaration of Helsinki (BMJ 1991; 302: 1994).
POEM procedure
All the POEM procedures were performed by a single endoscopist (Dr. Wei Gong). Patients were fast for 24 h before POEM. POEM was performed under general anesthesia with endotracheal intubation. CO2 insufflation was used during the procedure. The steps of the procedure were described as Inoue et al. (Fig. 2) [7]. Since there is no consensus about optimal myotomy length suggested for achalasia up to date, our endoscopist not only performed routine longer myotomy (esophageal myotomy length > 4 cm, gastric myotomy length 2–3 cm) in most patients but also tried shorter myotomy (esophageal myotomy length < 4 cm, gastric myotomy length 2–3 cm) in the remaining patients. The patients were not randomized in our selection.
Schema of peroral endoscopic shorter myotomy procedure. a, a 2-cm longitudinal incision was made into the mucosa after injection of saline and indigo carmine. b, c, A submucosal tunnel from the esophagus to the gastric cardia was created using a Hybrid knife. c Endoscopic myotomy starts 4 cm below the initial mucosal incision. d Circular muscle bundles were dissected and the shorter myotomy was completed. e After completion of myotomy, the mucosal entry site was closed using hemostatic clips
Postprocedural management
Two days after the procedure, the patients undergo a contrast esophagram to check whether there was no leak. Patients were kept fast for 48 h and started a clear liquid diet, which would be switched to solid diet gradually. Proton pump inhibitors (PPI) were prescribed for 2 weeks.
Definitions and follow-up
The reviewed patients were divided into two groups according to myotomy length: short myotomy group (total myotomy length ≤ 7 cm, n = 36) and long myotomy group (total myotomy length > 7 cm, n = 74). All patients were scheduled to take follow-up visits at 3, 6 months after POEM with EGD, manometry, and Eckardt score, then yearly. Treatment success was defined as symptom relief, based on an Eckardt score lower than 3. Complications included mucosal perforation, pneumothorax, bleeding and gastroesophageal reflux disease (GERD) were recorded.
Statistical analysis
Continuous variables with normal distribution were presented as mean ± standard deviation (SD), and their statistical differences were analyzed with Student t test. Uncontinuous data were presented as median (range), their statistical differences were analyzed with Chi-square test or Fisher’s exact. Kaplan–Meier curves were generated and the log-rank test were used to compare symptom relief between the two groups. A two-sided p value < 0.05 was considered to be statistically significant. Data were analyzed using commercially available statistical software packages SPSS version 18.0 (SPSS Inc., Chicago, IL, USA).
Results
Patient baseline characteristics
The characteristics and clinical data of the two groups are shown in Table 1. There were no significant differences in age, sex, ASA classification or previous interventions. The severity of symptoms, as measured by Eckardt score, was similar for the two groups (7.1 ± 1.6 vs 7.5 ± 1.9, p = 0.195).
Clinical outcome of POEM
POEM was successfully completed in all included patients and no case was converted to surgery. Mean operative time in longer myotomy group was longer than shorter myotomy group (62.1 ± 25.2 min vs 46.6 ± 18.5 min, p = 0.001). Mean submucosal tunnel length was shorter than in longer myotomy group (8.6 ± 1.3 cm vs 15.1 ± 2.9 cm, p < 0.001). There was a significant difference of myotomy length between shorter myotomy group and longer myotomy group [mean total myotomy length: 6.0 ± 0.6 cm (esophageal, 4.0 ± 0.7 cm; gastric, 2.1 ± 0.3 cm) vs 11.5 ± 3.1 cm (esophageal, 8.2 ± 2.7 cm; gastric, 3.2 ± 1.2 cm), p < 0.001] (Table 2). To note, there was one sigmoid-type achalasia patients in each group. For the case in short myotomy group, we made a shorter submucosal tunnel at the distal straight part of esophagus, approximately 5 cm above the GEJ, then extended 2 cm to the cardia with a total length of 7 cm. After that, myotomy was performed successfully with a total length of 5 cm. The whole procedure time was 56 min, which is much shorter than the case treated using conventional longer myotomy (total submucosal tunnel length 16 cm, total myotomy length 14 cm, procedure time 100 min).
Follow-up with Eckardt score was available for all included patients. Treatment success was achieved in 92.7% of all cases (94.4% in shorter myotomy group vs 91.9% in longer myotomy group, p = 0.926) after a mean follow-up period of 28.7 months (range 6–58.8 months) (Table 2, Fig. 3). The mean Eckardt score was improved from 7.1 to 1.3 after POEM treatment in shorter myotomy group (p < 0.001), and from 7.5 to 1.6 in longer myotomy group (p < 0.001).
Follow-up manometry was available in 68/110 cases, 16 cases in shorter myotomy group and 51 cases in longer myotomy group. The reasons for patients who refused follow-up manometry was discomfort related to the procedure or long-distance travel. Mean LES pressure was decreased from 41.8 to 15.9 mmHg after POEM in shorter myotomy group (p < 0.001), and 39.7–13.3 mmHg in longer myotomy group (p < 0.001). The difference in the pressure reduction between the two groups were not statistically significant (reduced pressure: 27.3 ± 13.0 mmHg vs 26.8 ± 15.9 mmHg; p = 0.915).
Complications
There was no difference in procedure-related complications between the two groups such as bleeding and pneumothorax (8.4 vs 8.2%, p = 0.823) (Table 2). The rate of GERD was also similar (8.3% vs. 14.9%, p = 0.510). By EGD, 1 patient in shorter myotomy group was diagnosed with reflux esophagitis classified as grade A according to Los Angeles classification. In longer myotomy group, four patients was diagnosed as grade A reflux esophagitis and two patients was diagnosed as grade B reflux esophagitis.
Discussion
Achalasia is an esophageal motility disorder presented with dysphagia, regurgitation and chest pain with an estimated annual incidence of 1 in 100,000 [1, 17]. In spite of an increasing understanding of its pathophysiology, the etiology of achalasia still remains unknown [18]. All current treatments focus on disruption of LES, with different advantages and drawbacks [19, 20]. Endoscopic botox injection is safe and effective for most patients in short term but symptom relief is observed in only 29% on intermediate follow-up [21]. Endoscopic pneumatic dilation can achieve the efficacy of more than 90% but usually requires serial dilations and the risk of perforation is between 2 and 5% [22,23,24,25]. Laparoscopic Heller myotomy (LHM) allows for a complete disruption of LES and provides the best solution for achalasia, but it usually results in gastroesophageal reflux symptoms and requires antireflux procedure [26]. The recent novel technique of POEM can enable endoscopists to complete a myotomy of esophageal circular muscle fibers across the GEJ and into the stomach through a submucosal tunnel. Pasricha et al. initially described the feasibility of this technique in pig model in 2007 [27], and then Inoue et al. firstly reported the clinical trial of this treatment in human beings [7]. Since then, more than 3000 POEM procedures have been performed worldwide with promising clinical outcomes [28].
To our knowledge, this is the first study comparing clinical outcome between shorter myotomy and longer myotomy in POEM procedure. With regard to the myotomy length in POEM procedure, Inuoe et al. recommended more than 10 cm (average 13 cm) as the standard length [20]. This standard longer myotomy has become an international experience, followed by many endoscopists. Zhou et al. in China (reported mean length of myotomy: 10.2 cm), von Renteln et al. in Germany (reported mean length of myotomy: 12 cm), Costamagna et al. in Italy (reported mean length of myotomy: 10 cm), Chiu et al. in Hong Kong of China (reported mean length of myotomy: 10.8 cm), Minami et al. in Japan (reported mean length of myotomy: 14.4 cm), Neuhaus et al. in Germany (reported mean length of myotomy: 12 cm) applied the longer myotomy to treat achalasia patients with promising clinical outcomes [9,10,11,12,13,14]. However, it has been demonstrated that the length of LES was just 3.2 cm (range 2.4–4.0 cm) based on esophageal manometry in health normal volunteers and achalasia patients [29, 30]. SAGES guidelines for the surgical treatment of esophageal achalasia recommended that surgical myotomy should be at least 4 cm on the esophagus and 1–2 cm on the stomach [31]. Therefore, we managed to use the modified POEM with shorter myotomy (myotomy length ≤ 7 cm) to treat achalasia and achieved similar treatment success compared to longer myotomy but with less procedure time.
It was interesting to find that shorter myotomy of POEM had the same efficacy as standard longer myotomy. Our previous study analyzed the high-resolution manometry data in 36 achalasia patients before and after POEM [32]. It was found that myotomy of the distal esophagus could attenuate the pressurization or spasm in proximal esophagus without myotomy and could assist upper esophageal sphincter relaxation. One possible mechanism is that the myotomy of distal esophagus might have an inhibition reflex on the motility of the proximal esophagus, via the enteral nervous system [33]. Another possible mechanism is reduced proximal venting resistance following distal myotomy, which could facilitate the bolus transit in proximal esophagus. In addition, Ezra et al. analyzed the efficacy of extended proximal esophageal myotomy in POEM, using intraoperational functional lumen imaging probe to assess the distensibility of GEJ [34]. The GEJ distensibility was increased significantly in creating submucosal tunnel and GEJ-myotomy, but not further increased in extended proximal myotomy. It seems that shorter myotomy was enough for the improvement of esophageal physiology and an extended proximal esophageal myotomy was unnecessary.
What is more, shorter myotomy may be more useful and appealing for treating sigmoid-form achalasia. According to our experience, orientation during procedure is a big challenge for this type of achalasia, which means that it is hard to create a straight submucosal tunnel from esophagus to cardia and easy to get lost in the tunnel due to the tortuous esophagus. There were two sigmoid-type achalasia patients in our studies, one in shorter myotomy group, the other in longer myotomy group. We made a shorter submucosal tunnel (7 cm) and myotomy (5 cm) for the case in shorter myotomy group successfully. The procedure time was much shorter than the case in longer myotomy group. To note, disorientation in the submucosal tunnel of sigmoid esophagus may have the risk of injury of the adjacent mucosa, even perforation. Shorter myotomy with a short submucosal tunnel method may have a potential to reduce this risk with similar efficacy, but future trial with large volume are needed to assess the role of shorter myotomy for achalasia with sigmoid esophagus.
Our study has several limitations. First, it is a retrospective study and non-randomized design. Secondly, not all the patients underwent follow-up manometry mainly due to discomfort related to the procedure. Finally, our mean follow-up length was 28.7 months, we cannot comment on the 5-year or 10-year efficacy.
In conclusion, shorter myotomy is comparable with longer myotomy for treating achalasia with regard to short-term clinical efficacy and safety and may have the advantage of shorter procedure time. Further randomized controlled trials are warranted to evaluate the long-term efficacy and safety of these two myotomy approaches in POEM.
Data availability
The data belong to the Department of Gastroenterology, Shenzhen Hospital of Southern Medical University, and Department of Gastroenterology, Affiliated Hospital of Southwest Medical University, and a permission is requested to make it freely available.
References
Richter JE, Boeckxstaens GE. Management of achalasia: surgery or pneumatic dilation. Gut. 2011;60:869–76.
Zaninotto G, Bennett C, Boeckxstaens G, et al. The 2018 ISDE achalasia guidelines. Dis Esophagus. 2018. https://doi.org/10.1093/dote/doy071.
Boeckxstaens GE, Zaninotto G, Richter JE. Achalasia. Lancet. 2014;383:83–93.
Muehldorfer SM, Schneider TH, Hochberger J, et al. Esophageal achalasia: intrasphincteric injection of botulinum toxin A versus balloon dilation. Endoscopy. 1999;31:517–21.
Karamanolis G, Sgouros S, Karatzias G, et al. Long-term outcome of pneumatic dilation in the treatment of achalasia. Am J Gastroenterol. 2005;100:270–4.
Kilic A, Schuchert MJ, Pennathur A, et al. Long-term outcomes of laparoscopic Heller myotomy for achalasia. Surgery. 2009;146:826–31.
Inoue H, Minami H, Kobayashi Y, et al. Peroral endoscopic myotomy (POEM) for esophageal achalasia. Endoscopy. 2010;42:265–71.
NOSCAR POEM White Paper Committee, Stavropoulos SN, Desilets DJ, et al. Per-oral endoscopic myotomy white paper summary. Gastrointest Endosc. 2014;80:1–15.
Zhou P, Yao L, Zhang YQ. Peroral endoscopic myotomy (POEM) for esophageal achalasia: 205 cases report [abstract]. Gastrointest Endosc. 2012;75:AB132–133.
von Renteln D, Inoue H, Minami H, et al. Peroral endoscopic myotomy for the treatment of achalasia: a prospective single center study. Am J Gastroenterol. 2012;107:411–7.
Costamagna G, Marchese M, Familiari P, et al. Peroral endoscopic myotomy (POEM) for oesophageal achalasia: preliminary results in humans. Dig Liver Dis. 2012;44:827–32.
Chiu PW, Wu JC, Teoh AY, et al. Peroral endoscopic myotomy for treatment of achalasia: from bench to bedside (with video). Gastrointest Endosc. 2013;77:29–38.
Minami H, Isomoto H, Yamaguchi N, et al. Peroral endoscopic myotomy for esophageal achalasia: clinical impact of 28 cases. Dig Endosc. 2014;26:43–51.
Charton JP, Schumacher B, Toermer T. Peroral endoscopic myotomy (POEM) for achalasia: pilot case series of a Western referral center. Gastrointest Endosc. 2013;77(supp 5):AB351.
Swanstrom LL, Kurian A, Dunst CM, et al. Long-term outcomes of an endoscopic myotomy for achalasia: the POEM procedure. Ann Surg. 2012;256:659–67.
Bredenoord AJ, Fox M, Kahrilas PJ, et al. Chicago classification criteria of esophageal motility disorders defined in high resolution esophageal pressure topography. Neurogastroenterol Motil. 2012;24(Suppl 1):57–655.
Kashiwagi H, Omura N. Surgical treatment for achalasia: when should it be performed, and for which patients? Gen Thorac Cardiovasc Surg. 2011;59:389–98.
Gockel HR, Schumacher J, Gockel I, et al. Achalasia: will genetic studies provide insights? Hum Genet. 2010;128:353–64.
Ahmed A. Achalasia: what is the best treatment? Ann Afr Med. 2008;7:141–8.
Inoue H, Santi EG, Onimaru M, et al. Submucosal endoscopy: from ESD to POEM and beyond. Gastrointest Endosc Clin N Am. 2014;24:257–64.
Gutschow CA, Töx U, Leers J, et al. Botox, dilation, or myotomy? Clinical outcome of interventional and surgical therapies for achalasia. Langenbecks Arch Surg. 2010;395:1093–9.
Campos GM, Vittinghoff E, Rabl C, et al. Endoscopic and surgical treatments for achalasia: a systematic review and meta-analysis. Ann Surg. 2009;249:45–57.
Zerbib F, Thétiot V, Richy F, et al. Repeated pneumatic dilations as long-term maintenance therapy for esophageal achalasia. Am J Gastroenterol. 2006;101:692–7.
Vaezi MF, Richter JE. Diagnosis and management of achalasia. American College of Gastroenterology Practice Parameter Committee. Am J Gastroenterol. 1999;94:3406–12.
Boeckxstaens GE, Annese V, des Varannes SB, et al. Pneumatic dilation versus laparoscopic Heller’s myotomy for idiopathic achalasia. N Engl J Med. 2011;364:1807–16.
Triadafilopoulos G, Boeckxstaens GE, Gullo R, et al. The Kagoshima consensus on esophageal achalasia. Dis Esophagus. 2012;25:337–48.
Pasricha PJ, Hawari R, Ahmed I, et al. Submucosal endoscopic esophageal myotomy: a novel experimental approach for the treatment of achalasia. Endoscopy. 2007;39:761–4.
Bechara R, Ikeda H, Inoue H. Peroral endoscopic myotomy: an evolving treatment for achalasia. Nat Rev Gastroenterol Hepatol. 2015;12:410–26.
Shi YN, Xiao YL, Chen MH. Normative data of high resolution impedance manometry in the Chinese population. J Gastroenterol Hepatol. 2013;28:1611–5.
Wang J, Tan N, Xiao Y, et al. Safety and efficacy of the modified peroral endoscopic myotomy with shorter myotomy for achalasia patients: a prospective study. Dis Esophagus. 2015;28:720–7.
Stefanidis D, Richardson W, Farrell TM, et al. SAGES guidelines for the surgical treatment of esophageal achalasia. Surg Endosc. 2012;26:296–311.
Ren Y, Tang X, Chen F, et al. Myotomy of distal esophagus influences proximal esophageal contraction and upper esophageal sphincter relaxation in patients with achalasia after peroral endoscopic myotomy. J Neurogastroenterol Motil. 2016;22:78–85.
Wauters L, Van Oudenhove L, Selleslagh M, et al. Balloon dilation of the esophagogastric junction affects lower and upper esophageal sphincter function in achalasia. Neurogastroenterol Motil. 2014;26:69–766.
Teitelbaum EN, Soper NJ, Pandolfino JE, et al. An extended proximal esophageal myotomy is necessary to normalize EGJ distensibility during Heller myotomy for achalasia, but not POEM. Surg Endosc. 2014;28:2840–7.
Acknowledgements
This work was supported by the following financial grants, Doctoral Research Start-up Funding Project of Affiliated Hospital of Southwest Medical University (No. 16229), Beijing Municipal Administration of Hospitals’ Youth Program (No. QML20160903) and Medical Science and Technology Plan Projects of Zhejiang Province (No. 2017196257).
Author information
Ethics declarations
Ethical Statement
This retrospective review was approved by the Institutional Review Board (NFEC-2016-186). All research was performed in accordance with the Declaration of Helsinki (BMJ 1991; 302: 1994).
Conflict of interest
We declared that no conflicts of interest or financial ties to disclose.
Informed consent
All subjects gave written consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Huang, S., Ren, Y., Peng, W. et al. Peroral endoscopic shorter versus longer myotomy for the treatment of achalasia: a comparative retrospective study. Esophagus 17, 477–483 (2020). https://doi.org/10.1007/s10388-020-00739-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10388-020-00739-4