Abstract
Liquid chromatography tandem mass spectrometry (LC–MS/MS), especially triple-quadrupole mass spectrometry, has become an attractive alternative method to ligand binding assays for therapeutic monoclonal antibody quantification in biological samples, but the use of an internal standard with infliximab LC–MS/MS assays has not been reported yet. In this study, an improved LC–MS/MS method for quantification of infliximab in human serum was developed and validated. A surrogate peptide was used as a representative of infliximab which was cleaved for the quantification of infliximab based on LC–MS/MS assay. A stable isotope-labeled signature peptide was used as the internal standard (IS). The results showed linearity in the range of 0.39–100 μg mL−1; the lower limit of quantification (LLOQ), and the lower limit of detection were 0.39 and 0.0975 μg mL−1, respectively. The quality control (QC) data showed that the within-run, between-run precision (%RSD) and accuracy (%RE) conformed to the acceptance criteria of ±15 % for calibration standards and QCs (±20 % at the LLOQ). Other validation parameters including selectivity, methanol precipitation efficiency, serum matrix effect, stability, and auto-sampler carry-over were also evaluated. This improved LC–MS/MS method might be a promising LC–MS-based methodology for pharmacokinetic studies of other recombinant monoclonal antibodies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Inflammatory disease is a great threat to human health, and tumor necrosis factor alpha (TNF-α) plays a critical role in the development of a variety of inflammatory diseases [1]. The TNF-α inhibitor has now become a dominant therapeutic drug for the current treatment of various inflammatory diseases. Infliximab, as the first FDA approved anti-TNF-α antibody, has been clinically used since the mid-1990s [2, 3]. It is a chimeric monoclonal antibody with murine variable regions and human constant regions, and its molecular weight is about 149 kDa [4]. Studies showed that infliximab displayed a good effect on patients with active Crohn’s Disease, Pediatric Crohn’s Disease, Ulcerative Colitis, Pediatric Ulcerative Colitis, Rheumatoid Arthritis, Ankylosing Spondylitis, Psoriatic Arthritis, Plaque Psoriasis, and Pouchitis [5–14]. Besides, it was proved that the treatment of infliximab was safe and well tolerated in patients who had advanced cancer [15].
However, there are still some problems with the infliximab therapy. Different patients exhibited different clinical responses following initiation of infliximab therapies, and there is compelling evidence that many patients failed to respond to this kind of anti-TNF-α therapy because of the inadequate drug level in blood or the formation of anti-drug antibodies [7, 16–18]. Therefore, accurate monitoring of serum infliximab drug and anti-drug antibody levels has great significance to these therapies. First, the measurement of infliximab through concentration may be useful for individual dosage adjustment and can contribute to the modifying of therapeutic decision for patients. Second, therapeutic drug monitoring of infliximab in patients would improve the control of disease activity [19]. In addition, it conformed to the development of the therapeutic drug monitoring (TDM). TDM is a new branch of medicine formed in the past 20 years, which focused on quantitatively analyzing concentrations of drugs and metabolites for biological sample (including Blood, urine, saliva, and so on) and exploring the safety margin of blood drug concentration through a variety of modern testing methods; furthermore, it can also calculate the optimal dose and dosing intervals by applying various drug dynamics method to achieve individualized dosing regimen, more safe, effective, and economical drug use [20].
In the process of preclinical and clinical pharmacokinetic studies, immunoassays have been chosen as the analytical technique for quantifying proteins in biological fluids, such as ELISA (enzyme-linked immune-sorbent assay) [21] and RIA [22]. Stable isotope standards and capture by anti-peptide antibodies (SISCAPA) approach, similarly to ELISA, are another strategy for quantifying antibodies that combines stable isotope standards and were captured by anti-peptide antibodies [23]. In addition, ELC [24] and HMSA [25] approaches have also been used for detecting the antibody concentration in serum. Although these techniques have shown great utility, they still have several known flaws including poor concordance between assays and interferences [26–28]. For example, ELISA is most widely used for serum concentrations determination for its exceptional sensitivity and high throughput. However, this kind of antibody-based method suffers from some issues, such as insufficient dynamic range, finite detection limit, cross-reactivity, long development time, and high variability [29–31]. As a result, it does not meet the requirement for modern TDM and pharmacokinetic studies. Therefore, it is necessary to develop a more rapid and accurate method for the determination of blood drug concentration in pharmacokinetic study of antibody drugs.
The LC–MS/MS-based techniques, which are considered as the “gold standard” for small molecule drugs and biomarkers in the pharmaceutical industry, are recently gaining increasing interest in the detection of large molecular drugs from complicated biological matrices due to their unique advantages over traditional immune-analytical methods, such as rapid assay development, high selectivity, good accuracy, and precision and ability to detect degradation products and post-translational modifications (PTMs) [32, 33]. Furthermore, the facile translatability across multiple biologic matrices, when taken as a whole, enables a more rapid translation from nonclinical to clinical application with minimal method optimization [34–37]. Most of the examples of protein quantification using LC–MS/MS are based on the selection of a surrogate peptide from enzymatic digests of the protein of interest and stable isotope-labeled IS (SIL-IS) synthesis [38]. The use of SIL-IS is able to ensure precise relative quantification of the targeted peptide [39]. In addition to SIL-IS, the differential dimethyl labeling method could also been used in an ultra-performance liquid chromatography tandem mass spectrometry (UPLC–MS/MS) method for absolute quantification of a therapeutic monoclonal antibody [40]. Although several methods, for instance, ELISA and HMSA [41], have been applied to infliximab estimation, no method has been reported for simultaneous quantitation using LC–MS/MS at present, to our best knowledge.
In this paper, a method for quantifying infliximab in human serum was developed and validated. The sample preparation was adapted from a former study [42]. The total serum proteins were first denatured, reduced, alkylated, and digested by trypsin, and then directly analyzed by LC–MS/MS for the quantitation of the peptides selected from the infliximab. After screening, a unique peptide was chosen from the tryptic peptides for LC–MS/MS quantitation. This LC–MS/MS method was fully validated according to regulatory guidelines [43–45] and was successfully applied to analyzing some blood samples from phase I clinical trial; thus, it might be a promising LC/MS-based methodology for pharmacokinetic studies of other recombinant monoclonal antibodies.
Materials and Methods
Chemicals and Materials
Infliximab (molecular weight ~149 kDa) was expressed by our laboratory; methanol (MeOH, HPLC grade) and acetonitrile (ACN, LC/MS grade) were purchased from Fisher Scientific (USA); sodium iodide (NaI, purity ≥99.5 %) and fibrinopeptide (GFP, HPLC grade, purity ≥99.5 %) were all purchased from Sigma–Aldrich (St. Louis, MO). Dithiothreitol (DTT), iodoacetamide (MIA), and formic acid (FA, MS grade) were obtained from Fluka (GER). High-purity nitrogen (purity >99.9 %) was purchased from Shanghai YiZhi Cold Engineering System Co., LTD; high-purity argon (purity >99.9 %) was purchased from Shanghai MAO Love Purifying Gas Co., LTD. Trypsin was made from our laboratory, and human serum was obtained from phase I clinical trial (CMAB008RA I).
Preparation of Stock and Standard Solutions
The stock solution of infliximab was prepared by dissolving in human serum to give a final concentration of 200 μg mL−1, and the stock solution of IS was dissolved in H2O/ACN/FA (9: 1: 0.05) to reach a concentration of 222.82 μg mL−1. The working calibration standard solutions were freshly prepared on each day of the analysis by serial dilutions of the stock solution of infliximab with lots of control human serum, and the working QC solutions with concentrations of 1.0, 9.0, 80, and 100 μg mL−1 were also prepared in the same manner with working calibration standard solutions. The working solutions of IS (0.4456 μg mL−1) were freshly prepared on each day by dilution of the corresponding stock solution with Milli-Q water. 100 mM DTT was prepared by 100 mM ammonium bicarbonate from 1 M DTT mother liquor, and 100 mM MIA was diluted with 100 mM ammonium bicarbonate by 2.9 M MIA mother liquor.
Sample Preparation
The concentration of 200 μg mL−1 samples was made from pipetting infliximab into human serum, and then different concentration levels of samples (100, 50, 25, 12.5, 6.25, 3.13, 1.56, 0.78, 0.39, 0.195 μg mL−1) were prepared from the 200 μg mL−1 samples by serial dilutions with human serum. Following that, total serum proteins were precipitated with 100 μL of methanol, and the mixtures were vortexed for 2 min and then centrifuged at 17,000g for 20 min. The supernatant was removed, and the retained protein pellet was resuspended with 50 μL 100 mM ammonium bicarbonate (pH 8.0) by vigorously vortexing for 2 min until a uniform white protein suspension was obtained. The denatured protein solution was further reduced with 10 μL of 100 mM DTT at 60 °C for 60 min. After cooling the samples at room temperature, 25 μL of 100 mM MIA was added to each sample, and the samples were incubated in the dark for 30 min at 30 °C. The sample digestion was initiated by adding 25 μL of 8 mg mL−1 trypsin (prepared in water) and incubating at 50 °C in a preheated dry bath for 60 min. The digestion reaction was then quenched by adding 25 μL of 10 % FA/H2O solution. The final tryptic digest was centrifuged at 17,000g for 20 min, and the supernatant (~130 μL) was transferred to a clean EP tube for LC–MS/MS analysis.
LC–MS Setup for Signature Peptide Identification Procedure and Quantitative Analysis
The LC–MS/MS system used for the selection of signature peptide from infliximab consisted of a UPLC with an external column oven connected to a G2S-Q-ToF (Waters, Milford, MA). In the UPLC system, mobile phases were as follows: A (10 % ACN: 89 % H2O: 1 % FA); C (ACN); and D (H2O). An ACQUITY UPLC BEH 300 C18 1.7 μm 2.1 × 100 mm column (Waters, Milford, MA) was used, and the linear gradient was 1–36 % C in 80 min, 105 min in total. The flow rate was 0.2 mL min−1, and the injection volume was 10 μL. Data were obtained with positive ionization (ESI), and the acquisition range was 150–2,000 Da. The ion source setup was presented as follows: capillary voltage, 3.0 kV; the desolvation temperature, 350 °C; the source temperature, 120 °C; and the desolvation gas flow, 800 L h−1. The system was controlled by MassLynx 4.1 (Waters, Milford, MA), and the data analysis was performed with BiopharmaLynx1.3.3.
The quantitative analysis was performed on an ultra-performance liquid chromatography (UPLC)-MS/MS system which consisted of an ACQUITY UPLC®I-Class System (Waters, Milford, MA) equipped with a reliance unit (conditioned stacker and auto-sampler) coupled to a Xevo® TQ-S Quantum ultra triple-quadrupole mass spectrometer from Waters (Milford, MA) equipped with H-ESI, and positive-ion multiple reaction monitoring (MRM) mode was used. The column in application was ACQUITY UPLC BEH 130 C18 1.7 μm 2.1 × 150 mm (Waters, Milford, MA). The mobile phases were 0.1 % FA in water (mobile phase A) and 0.1 % FA in ACN (mobile phase B). The LC gradient program was 1–20 % B for 6.5 min, and total run time was 13 min. The flow rate was 0.3 mL min−1, and the column temperature was 60 °C; the auto-sampler temperature was set at 4 °C. Data acquisition was performed with MassLynx 4.1 (Waters, Milford, MA). Triple-quadrupole mass spectrometer Source parameters were as follows: ion spray voltage, 2.5 kV; Cone voltage, 25 V; source temperature, 500 °C; desolvation gas flow, 800 L h−1; and collision energy, 20 eV. Mass-dependent MRM ion transitions and triple-quadrupole parameters for the target peptide and its SIL-ISs were optimized.
Optimization of Sample Processing Procedures
Comparison of Two Kinds of Precipitants
For removing some endogenous substances (phospholipids, peptide, etc.) prior to trypsin digestion and reduce the interference from the serum matrix to analytic peptide, the step of protein denaturation and precipitation was essential. Here, we compared the precipitation efficiency of two water-miscible organic solvents (MeOH and ACN).
Optimization of Enzyme Digestion Conditions
For the optimization of enzyme digestion conditions, three digestion parameters were investigated including protein-to-trypsin ratio, digestion time, and digestion temperature. In the protein to trypsin ratio experiment, the amount of trypsin was varied so that the ratio between the substrate (total serum proteins) and the digestion enzyme could be altered. As to the effect of incubation time and temperature on digestion efficiency, samples were digested in serum for different times and at various temperatures, respectively.
Method Validation
The LC–MS/MS assay validation involved detecting several key parameters to establish credibility in assay performance including selectivity, accuracy, precision, carry-over, stability, spike recovery as well as the matrix effect. All the sample analysis was conducted according to current regulatory guidelines for macromolecular proteins. The infliximab calibration curve, including a zero standard containing no infliximab spike, was analyzed in duplicate. QC samples fortified with infliximab to specific final concentrations in normal human serum were tested in 6 replicates at each of the spiked infliximab levels in 3 separate batches running on different days. In addition, the stability of samples at different conditions (the analytic peptide in matrix at room temperature for 36 h or three freeze–thaw cycles from −20 °C to room temperature, the processed sample at room temperature for 2 days or at 4 °C for 3 days) were tested, respectively, by 6 replicates in three QCs levels (LQC, MQC, HQC). In addition, we evaluated the stability of IS in the stock solution (10 % ACN: 89.5 % H2O: 0.5 % FA) and working solution (H2O). The peptide SINSATHYAESVK was used as the primary peptide for quantification purposes, and all results shown were based on this peptide. The acceptance criteria of ±15 % for calibration standards and QCs (±20 % at the LLOQ) were applied.
Quantitative Analysis of Clinical Samples
Human serum samples were collected from phase I clinical trial with a single-low-dose (1 mg kg−1) group of the four subjects injected with infliximab. The samples were frozen and stored at −80 °C until analysis. The same set of PK study samples was analyzed by ELISA (ELISA method are supplied in Electronic Supplementary Material) and LC–MS/MS methods.
This study was approved by the Ethical Committee on Clinical Investigation, Xi Jing Hospital and was performed in accordance with the declaration of Helsinki and its amendments.
Results and Discussion
Identification of Signature Peptides of Infliximab
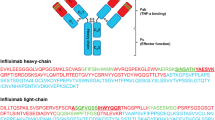
For most proteins larger than 10 kDa, there is no straightforward method to separate them from biological matrices except for immuno-capture [33]. Antibodies are too heavy globular proteins (near 149 kDa) to be directly quantified using standard LC–MS assays. Nevertheless, it is possible to detect unique marker peptides which could present the antibodies. Therefore, for the quantification of the mAb, identifying potential signature peptides is of great important. We first predicted the surrogate peptides by using the silico trypsin digestion [PeptideMass, http://web.expasy.org/peptide_mass/], and then compared the amino acid sequences between human serum proteins and infliximab through BLAST [http://blast.ncbi.nlm.nih.gov/Blast.cgi] and UniProt/Swissprot to exclude peptides present in the plasma proteome [37, 42]. Two surrogate peptides (DILLTQSPAILSVSPGER and SINSATHYAESVK) were selected: the first one is in the framework region (FR) of rat and the other one is located in the complementarity determining region (CDR). In addition, to further confirm, the two surrogate peptides were unique in human serum, and tryptic digestion of the infliximab within human serum and blank serum were conducted, and then we analyzed and compared the peptide map by Q-TOF in 100 min LC gradient. However, only the unique peptide SINSATHYAESVK (HC-T7) showed high sensitivity and specificity (Fig. 1).
Though two candidate peptides (SINSATHYAESVK and DILLTQSPAILSVSPGER) were found from the variable region of infliximab, only the peptide SINSATHYAESVK was unique (Fig. 1a), while some interference peaks were observed in the blank sample with regard to the peptide DILLTQSPAILSVSPGER (Fig. 1b). In addition, the peptide (SINSATHYAESVK) is located in the CDR of the heavy-chain variable region (VH) of infliximab, which is on the surface of the three-dimensional structure and easily accessible to trypsin for digestion. Therefore, the peptide SINSATHYAESVK was chosen as the signature peptide for further quantification study.
IS Labeling Strategy and IS Analysis by LC–MS/MS
Finding a suitable IS is another challenge encountered in the quantification of infliximab in human serum. In previous studies, isotope-labeled protein standards have been successfully used as a kind of strategy for the quantification of mAbs [46]. However, these standards are too expensive and time consuming. A well-designed IS strategy is critical for the successful development of an LC–MS-based protein quantification assay. As variations, which may be introduced in any step in the workflow including sample processing, liquid chromatography, and ionization, could be tracked and compensated by a good IS. The pros and cons of different IS strategies have been briefly discussed [33]. For example, the stable isotope-labeled signature peptide is very straightforward, and it is often easy to synthesize at low cost. However, one of its major drawbacks is that it cannot correct for variations in enzymatic digestion or any other sample processing steps prior to the digestion. Therefore, it may cause serious quantification bias [46, 47]. An alternative IS designed to cover the variations in enzymatic digestion step is the stable isotope-labeled extended signature peptide, which has extra amino acid sequences containing protease digestion sites flanking both sides of the signature peptide [48]. These extended SIL-ISs are added during the sample digestion step to go through the digestion process; therefore, variations in digestion efficiency are expected to be corrected to some extent. The digestion sites in this type of IS are often more accessible than those in target proteins; thus, the digestion kinetics of the target proteins could not be tracked. In our study, the peptide SKSINSATHYAESVK, which contains two additional amino acids (SK) and a protease digestion site at the N-terminal, was selected as a template for the IS. The isotope peptide (SINSA(A → A13C315N)THYAESVK)-labeled [13C315N]-Ala provided a 4 Da shift in mass.
Optimization of Sample Processing Procedures
Comparison of Two Kinds of Precipitants
The step of protein denaturation and precipitation could remove some endogenous substances (phospholipids, peptide, etc.) before trypsin digestion and reduce the interference from the serum matrix. We evaluated the precipitation efficiency of two water-miscible organic solvents (MeOH and ACN) by comparing the peak area of the analytic peptide. The result (Fig. 2a) indicated that the precipitation efficiency of MeOH was better than that of ACN.
Optimization of precipitants and enzyme digestion conditions. a Comparison of denaturation and precipitation effect with two kinds of precipitation agents (methanol and acetonitrile). b Protein-to-trypsin ratio optimization. Four digestion ratios (5:1, 10:1, 20:1, 50:1) were investigated for samples digested for 1 h with trypsin at 50 °C. c, d Effect of incubation time and temperature on digestion efficiency. Samples were digested in serum for 0.5, 0.75, 1, 2, 3, and 4 h with trypsin at 37 and 50 °C, respectively; the protein-to-trypsin ratio was 10:1. All the samples (b, c, d) were spiked with 0.7 μM infliximab and 0.28 μM IS in human serum. Digestion efficiencies were calculated from the normalized averaged peak areas (n = 3) obtained from the MRM chromatograms of the native SINSATHYAESVK peptide (originated from spiked infliximab, MRM transition: 469.6 → 603.8) and the corresponding isotope-labeled analog (SKSINSATHYAESVK, 471.0 → 605.9)
Optimization of Enzyme Digestion Conditions
In order to optimize the digestion conditions, three parameters were investigated: protein-to-trypsin ratio, digestion time, and digestion temperature. In one experiment, the amount of trypsin was varied so that the ratio between the substrate (total serum proteins) and the digestion enzyme could be altered. Four digestion ratios (5:1, 10:1, 20:1, 50:1) were investigated (Fig. 2b). Digestion efficiency was calculated from the normalized averaged peak area ratios (n = 3) obtained from the MRM chromatograms of the native SINSATHYAESVK peptide (originating from spiked infliximab, MRM transition: 469.6 → 603.8) and the corresponding isotope-labeled analog (SKSINSATHYAESVK, 471.0 → 605.9).
According to the data shown in Fig. 2b, there is no significant difference between the protein-to-trypsin ratio 5:1 and 10:1. And the trypsin efficiencies were significantly decreased at ratios above 10. Therefore, the protein-to-trypsin ratio 10:1 was chosen as the best enzyme digestion ratio.
In addition, the digestion time and digestion temperature were evaluated. The protein-to-trypsin ratio was constant (10:1) while the digestion time and temperature varied. Aliquots were taken after certain digestion times as well as temperatures [0.5, 0.75, 1, 2, 3, 4 h; 37, 50 °C]. Digestion efficiency was again calculated from the normalized averaged peak area ratios (n = 6) of the unique peptide SINSATHYAESVK and the corresponding isotope-labeled analog SKSINSATHYAESVK (Fig. 2c, d).
When samples were incubated at 50 °C, the digestion efficiency in 0.5 h was lower than that in 0.75 h. With the increasing reaction time, the efficiency was not significantly changed. However, the enzyme efficiency increased with the increasing reaction time from 0.5 to 4 h at 37 °C. And the highest efficiency at 37 °C for 4 h was close to that at 50 °C for 4 h. To ensure the infliximab being digested completely, we should better choose the digestion time of 1 h at 50 °C. Meanwhile, the enzyme digestion efficiencies under conditions of 1 h at 37 °C and 1 h at 50 °C were also compared. The result showed that peak area ratio at the condition of 50 °C, 1 h was higher than that of 37 °C, 1 h (P < 0.05).
After all, the enzymatic reaction was completed in 1 h by high protein-to-trypsin ratio (10:1, w/w) and high temperature (50 °C). Increasing the amount of trypsin did not increase responses of the peptide and the enzyme reaction condition at 50 °C for 1 h was better than that at 37 °C for 1 h.
Optimization of MRM Transitions and Parameters
The quantitation analysis was performed with Xevo®TQ-S Quantum ultra triple-quadrupole mass spectrometer operating in positive-ion MRM mode. So we first selected the relatively high abundance of MRM transitions (shown in Fig. 3; Table S1, Electronic Supplementary Material) of the signature peptide and IS derived by high-resolution mass spectrometry for quantitative detection.
MRM transitions of the signature peptide and peptide-IS monitored as a function of time. a LC–MS/MS chromatograms of the signature peptide in human serum sample and blank human serum sample [703.8(2+) > 934.5(1+, y8), 703.8(2+) > 173.1(1+, b1), 469.6(3+) > 603.8(2+, y11)]. b LC–MS/MS chromatograms of the peptide-IS in human serum sample and blank human serum sample [471.0(3+) > 465.094(2+, y8), 471.0(3+) > 548.893(2+, y10), 471.0(3+) > 605.907(2+, y11)]
There were no interferences in blank control for quantitative detection of signature peptide by the three MRM transitions. And the transition of 469.6(3+) > 603.8(2+, y11) which had the highest peak area was selected as the quantitation transition. Similarly, no interferences in blank control were observed for the IS. The transition of 471.0(3+) > 605.907(2+, y11) had the highest sensitivity; therefore, it was chosen for quantitation analysis. Then, the mass-dependent MRM ion transitions and triple-quadrupole parameters for the target peptide and its SIL-ISs were optimized (Table 1).
Method Validation
Linearity and LLOQ
A typical calibration curve was established during assay qualification for infliximab in human serum. According to the linear regression analysis of peak area arrived from ten different concentrations (range from 0.39 to 100 μg mL−1), the correlation coefficient (r) was 0.9961 for peptide of infliximab during the method validation. The lower limit of quantitation (LLOQ) for the analytic peptide was 0.39 μg mL−1 (S/N = 66), and the LOD was 0.0975 μg mL−1. From six repeat stitches, the RSD was within 11 % for LLOQ and less than 5 % for other concentrations. This indicated linearity of the detector response can be used as a function of the standard calibration curve.
Selectivity
To ensure that this analytical method can differentiate and quantify the infliximab in the presence of other components in the serum sample, the selectivity of signature peptide and IS in human serum obtained from six sources were tested. All samples were detected at the LLOQ in the absence of interfering components in the chromatograms for the signature peptide and IS, Fig. 4 and Fig. S1 (Electronic Supplementary Material), which demonstrated its high selectivity in human serum.
Representative chromatograms of the signature peptide and peptide-IS at the LLOQ level. Significant analytic peaks were observed in the LLOQ samples: 0.39 μg mL−1 for signature peptide (a1), 0.22 μg mL−1 for the IS (a’1). No interference peaks were observed in the corresponding blank samples: a0 and a’0
Precision and Accuracy
The accuracy (%RE) and precision (%RSD) information of the within-run and between-run for the QCs are presented in Table 2 and shown in Fig. S2; all the results passed the acceptance criteria. The within-run and between-run precision values were within 12 and 15 %, respectively, and the accuracy values were within ±15 % for all the QCs samples.
Recovery and Matrix Effect
The methanol precipitation recovery and serum matrix effect of target peptide from human serum were determined at low, medium, and high concentrations (1, 9, and 80 μg mL−1), results shown in Table 3. The methanol precipitation recovery rates were calculated from the peak area in human serum samples spiked with the infliximab before and after the processing step. The recoveries of denaturation and precipitation were 92.18 % at 1 μg mL−1 and ~100 % at 9 and 80 μg mL−1, respectively. The recoveries of trypsin digestion were above 95 % at the three concentration levels. The recoveries after trypsin digestion were greater than 80 % for all the samples, which might be attributed to sample loss during the centrifugation and transferring of the supernatant. In order to assess the serum matrix effect, the response of infliximab spiked in the human serum was compared with that in water as control. The processing steps after methanol precipitation were all the same (serum sample was precipitated by methanol while water sample was not treated). The mean values of matrix effect rate at the concentrations of 1, 9, and 80 μg mL−1 in human serum were all above 50 %. These results indicated that the serum matrix had a great influence on the quantification of analytic peptide. However, the matrix effect did not affect the accuracy and precision of the results for they were well compensated by the IS we used during the sample processing and analysis.
Carry-over
According to relevant laws and regulations, carry-over should be addressed and minimized during method development. In our study, carry-over was assessed by injecting blank sample directly after a high QC (80 μg mL−1) sample and calibration standard at the upper limit of quantification (100 μg mL−1). Six replicates were tested. Carry-over was calculated by comparing the response of peptide and IS in blank sample with that of high QC sample and highest concentration of calibration standard. The results showed that the carry-over was less than 20 % of the LLOQ for the significant peptide and 5 % for the IS. Therefore, it would not affect accuracy and precision during the assay validation.
Stability
Evaluation of stability should be carried out to ensure that every step taken during sample preparation and sample analysis, as well as the storage conditions used do not affect the concentration of the analytes. Here, we, respectively, evaluated the stability of several situations including the IS in the stock solution (10 % ACN: 89.5 % H2O: 0.5 % FA) and working solution (H2O), the infliximab in human serum at room temperature for 36 h, the analytes in the matrix after three freeze–thaw cycles from −20 °C to room temperature, and the processed sample at room temperature for 2 days and at 4 °C for 3 days.
In order to evaluate the stability of IS, the same IS sample was diluted by the stock solution (10 % ACN: 89.5 % H2O: 0.5 % FA) and working solution (H2O), respectively, and stored at 4 °C for 3 days. We found that the IS was relatively stable in the stock solution (10 % ACN: 89.5 % H2O: 0.5 % FA) but not in the working solution (H2O). It is speculated that the nonspecific adsorption had happened to the peptide-IS in H2O. Therefore, we recommended using the 10 % ACN: 89.5 % H2O: 0.5 % FA as stock solution and configure the working solution when needed. The other stability results are shown in Table 4.
The stability of infliximab in human serum was demonstrated by comparing the mean measured concentrations and predicted QC concentrations. The stability of unique peptide in processed samples was confirmed by comparing the stored and processed QCs against the freshly prepared standards. All the data information passed the criteria, indicating that the unprocessed and processed samples in different conditions were all stable and providing additional confidence and evidence for the analytical procedure.
Comparison Between ELISA and LC–MS/MS for PK Study of Infliximab
We analyzed samples from phase I clinical trial with a single-low-dose (1 mg kg−1) group of the four subjects injected with infliximab drug by ELISA and LC–MS/MS assays. The average concentration to the time after infusion detected by ELISA ranged from 0.15 to 24.34 μg mL−1, with which the results from LC–MS/MS had good consistency in the whole range, seen in Fig. 5; Fig. S3 (Electronic Supplementary Material).
Conclusion
A simple, sensitive, specific, and precise LC–MS/MS assay has been developed and validated for quantitation of infliximab by using isotope-labeled signature peptide as IS in this study. This assay was fully validated to meet the requirements of the US Food and Drug Administration (FDA) and successfully applied to the quantification of our infliximab in some clinical samples by comparing with ELISA. The sample processing procedures were optimized including two kinds of precipitants and the protein digestion conditions. The isotope-labeled signature peptide as IS was able to calibrate for variations in the whole process of the method. In addition, this LC–MS/MS assay can reduce method development time, and the resources required for multiple candidates in different biological matrices during the preclinical stages when specific LBA reagents are not available. Therefore, we believe that this LC–MS/MS method could helpful to the development of the modern TDM, and it can be used as a method model for pharmacokinetic studies of other recombinant monoclonal antibodies.
References
Balkwill F (2009) Nat Rev Cancer 9:361–371
Elliott MJ, Maini R, Feldmann M, Long-Fox A, Charles P, Bijl J, Woody J (1994) Lancet 344:1125–1127
Van Dullemen H, Van Deventer S, Hommes D, Bijl H, Jansen J, Tytgat G (1995) Gastroenterology 109:129–135
Knight DM, Trinh H, Le J, Siegel S, Shealy D, McDonough M, Scallon B, Moore MA, Vilcek J, Daddona P (1993) Mol Immunol 30:1443–1453
Martínez-Borra J, López-Larrea C, González S, Fuentes D, Dieguez A, Deschamps EM, Perez-Pariente J, López-Vázquez A, de Francisco R, Rodrigo L (2002) Am J Gastroenterol 97:2350–2356
Targan SR, Hanauer SB, van Deventer SJ, Mayer L, Present DH, Braakman T, DeWoody KL, Schaible TF, Rutgeerts PJ (1997) New Engl J Med 337:1029–1036
Hanauer SB, Feagan BG, Lichtenstein GR, Mayer LF, Schreiber S, Colombel JF, Rachmilewitz D, Wolf DC, Olson A, Bao W (2002) Lancet 359:1541–1549
Present DH, Rutgeerts P, Targan S, Hanauer SB, Mayer L, Van Hogezand R, Podolsky DK, Sands BE, Braakman T, DeWoody KL (1999) New Engl J Med 340:1398–1405
Chey WY (2001) Inflamm Bowel Dis 7:S30–S33
Järnerot G, Hertervig E, Friis-Liby I, Blomquist L, Karlén P, Grännö C, Vilien M, Ström M, Danielsson Å, Verbaan H (2005) Gastroenterology 128:1805–1811
Maini SR (2004) Rheum Dis Clin N Am 30:329–347
Braun J, Brandt J, Listing J, Zink A, Alten R, Golder W, Gromnica-lhle E, Kellner H, Krause A, Schneider M (2002) Lancet 359:1187–1193
Chaudhari U, Romano P, Mulcahy L, Dooley L, Baker D, Gottlieb A (2001) Lancet 357:1842–1847
Zippi M, Cassieri C, Avallone EV, Pica R (2013) World J Clin Cases 1:191
Brown E, Charles K, Hoare S, Rye R, Jodrell D, Aird R, Vora R, Prabhakar U, Nakada M, Corringham R (2008) Ann Oncol 19:1340–1346
Gisbert JP, Panés J (2009) Am J Gastroenterol 104:760–767
Miheller P, Kiss LS, Lorinczy K, Lakatos PL (2012) Expert Opin Biol Ther 12:179–192
Regueiro M, Siemanowski B, Kip KE, Plevy S (2007) Inflamm Bowel Dis 13:1093–1099
Mulleman D, Méric J-C, Paintaud G, Ducourau E, Magdelaine-Beuzelin C, Valat J-P, Goupille P, GICC CNdlRSU (2009) Arthritis Res Ther 11(6):R178
Dasgupta A (2008) Introduction to therapeutic drug monitoring. In: Dasgupta A (ed) Handbook of drug monitoring methods. Springer, pp 1–39
Baert F, Noman M, Vermeire S, Van Assche G, D’Haens G, Carbonez A, Rutgeerts P (2003) New Engl J Med 348:601–608
Aarden L, Ruuls SR, Wolbink G (2008) Curr Opin Immunol 20:431–435
Anderson NL, Anderson NG, Haines LR, Hardie DB, Olafson RW, Pearson TW (2004) J Proteome Res 3:235–244
Vande Casteele N, Buurman D, Sturkenboom M, Kleibeuker J, Vermeire S, Rispens T, Kleij D, Gils A, Dijkstra G (2012) Aliment Pharm Therap 36:765–771
Wang S-L, Hauenstein S, Ohrmund L, Shringarpure R, Salbato J, Reddy R, McCowen K, Shah S, Lockton S, Chuang E (2013) J Pharm Biomed Anal 78:39–44
Rawlins ML, Roberts WL (2004) Clin Chem 50:2338–2344
Mongia SK, Rawlins ML, Owen WE, Roberts WL (2006) Am J Clin Pathol 125:921–927
La’ulu SL, Roberts WL (2007) Am J Clin Pathol 127:436–440
Palandra J, Finelli A, Zhu M, Masferrer J, Neubert H (2013) Anal Chem 85:5522–5529
Rotmensch S, Cole LA (2000) Lancet 355:712–715
Morgan BR, Tarter TH (2001) J Urol 166:2311–2312
Ciccimaro E, Blair IA (2010) Bioanalysis 2:311–341
Zhang SW, Jian W (2014) Rev Anal Chem 33:31–47
Becker JO, Hoofnagle AN (2012) Bioanalysis 4:281–290
Hilger M, Bonaldi T, Gnad F, Mann M (2009) Mol Cell Proteomics 8:1908–1920
Dephoure N, Zhou C, Villén J, Beausoleil SA, Bakalarski CE, Elledge SJ, Gygi SP (2008) Proc Natl Acad Sci USA 105:10762–10767
Heudi O, Barteau S, Zimmer D, Schmidt J, Bill K, Lehmann N, Bauer C, Kretz O (2008) Anal Chem 80:4200–4207
Desiderio DM, Kai M (1983) Biol Mass Spectrom 10:471–479
Kennedy JJ, Abbatiello SE, Kim K, Yan P, Whiteaker JR, Lin C, Kim JS, Zhang Y, Wang X, Ivey RG (2013) Nat Methods 11:149–155
Ji C, Sadagopan N, Zhang Y, Lepsy C (2009) Anal Chem 81:9321–9328
Steenholdt C, Bendtzen K, Brynskov J, Ainsworth MA (2014) Am J Gastroenterol 109:1055–1064
Jiang H, Zeng J, Titsch C, Voronin K, Akinsanya B, Luo L, Shen H, Desai DD, Allentoff A , Aubry A-Fo (2013) Anal Chem 85:9859–9867
FDA (2001) Guidance for industry: bioanalytical method validation, pp 1–21
Zimmer D (2014) Bioanalysis 6:13–19
Khanna R, Sattin B, Afif W, Benchimol E, Bernard EJ, Bitton A, Bressler B, Fedorak R, Ghosh S, Greenberg G (2013) Aliment Pharm Therap 38:447–459
Li H, Ortiz R, Tran L, Hall M, Spahr C, Walker K, Laudemann J, Miller S, Salimi-Moosavi H, Lee JW (2012) Anal Chem 84:1267–1273
Brun V, Dupuis A, Adrait A, Marcellin M, Thomas D, Vandenesch F, Garin J (2007) Mol Cell Protemics 6:2139–2149
Beynon RJ, Doherty MK, Pratt JM, Gaskell SJ (2005) Nat Methods 2:587–589
Acknowledgments
We thank Waters Company Laboratories for cooperation with us. This work was supported by grants from the Natural Science Foundation of China (81330061), Ministry of Science and Technology of China (973 projects 2010CB833605 and 863 projects 2014AA021004), State Key Project for New Drug Development (2013ZX09101021; 2013ZX09401303), Shanghai Commission of Science and Technology (Key Laboratory and Projects 13DZ1930100), and Shanghai Excellent technical leader (13XD1424000).
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
X. Peng, B. Liu, Y. Li were contributed equally to this work.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Peng, X., Liu, B., Li, Y. et al. Development and Validation of LC–MS/MS Method for the Quantitation of Infliximab in Human Serum. Chromatographia 78, 521–531 (2015). https://doi.org/10.1007/s10337-015-2866-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10337-015-2866-2