Abstract
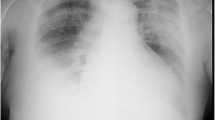
We report a case of fulminant septicemia with Bacillus cereus resistant to carbapenem. A 33-year-old man was suffering from febrile neutropenia (FN) on day 15 after the start of remission-induction therapy for biphenotypic acute leukemia under gut decontamination with polymyxin B and nystatin. Meropenem, a carbapenem, was administered according to the guideline for FN. Two days later (on day 17), he complained of severe abdominal pain, lost consciousness, went into sudden cardiopulmonary arrest, and died. Autopsy showed multiple spots of hemorrhage and necrosis caused by bacterial plaque in the brain, lungs, and liver. B. cereus was isolated from a blood sample obtained in the morning on day 17 and it was after his death that the isolated B. cereus was revealed to be resistant to carbapenem. B. cereus obtained from blood samples has been reported to be usually sensitive to carbapenem and also to vancomycin, new quinolones, and clindamycin. If B. cereus resistant to carbapem increases, our method of gut decontamination with polymyxin B and nystatin may have to be changed to one containing a new quinolone for the prevention of septicemia. Careful watching to determine whether B. cereus resistant to carbapem increases may be also important for empiric therapy, because carbapenem is often selected as the initial therapy for FN in patients with severe neutropenia.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Akiyama N, Mitani K, Tanaka Y, Hanazono Y, Motoi N, Zarkovic M, et al. Fulminant septicemic syndrome of Bacillus cereus in a leukemic patient. Internal Medicine 1997;36:221–6.
Musa MO, Al Douri M, Khan S, Shafi T, Al Humaidh A, Al Rasheed AM. Fulminant septicaemic syndrome of Bacillus cereus: three case reports. J Infect 1999;39:154–6.
de Almeida SM, Teive HA, Brandi I, Nabhan SK, Werneck LC, Bittencourt MA, et al. Fatal Bacillus cereus meningitis without inflammatory reaction in cerebral spinal fluid after bone marrow transplantation. Transplantation 2003;76:1533–4.
Frankard J, Li R, Taccone F, Struelens MJ, Jacobs F, Kentos A. Bacillus cereus pneumonia in a patient with acute lymphoblastic leukemia. Eur J Clin Microbiol Infect Dis 2004;23:725–8.
Haase R, Sauer H, Dagwadordsch U, Foell J, Lieser U. Successful treatment of Bacillus cereus meningitis following allogeneic stem cell transplantation. Pediatr Transplant 2005;9:338–41.
Kobayashi K, Kami M, Ikeda M, Kishi Y, Murashige N, Tanosaki R, et al. Fulminant septicemia caused by Bacillus cereus following reduced-intensity umbilical cord blood transplantation. Haematologica 2005;90:11–2.
Ozkocaman V, Ozcelik T, Ali R, Ozkalemkas F, Ozkan A, Ozakin C, et al. Bacillus spp. among hospitalized patients with haematological malignancies: clinical features, epidemics and outcomes. J Hosp Infect 2006;64:169–76.
Kuwabara H, Kawano T, Tanaka M, Kobayashi S, Okabe G, Maruta A, et al. Cord blood transplantation after successful treatment of brain abscess caused by Bacillus cereus in a patient with acute myeloid leukemia. Rinsho Ketsueki 2006;47:1463–8.
Yoshida H, Moriyama Y, Tatekawa T, Tominaga N, Teshima H, Hiraoka A, et al. Two cases of acute myelogenous leukemia with Bacillus cereus bacteremia resulting in fatal intracranial hemorrhage. Rinsho Ketsueki 1993;34:1568–72.
Masaoka T. Evidence-based recommendations for antimicrobial use in febrile neutropenia in Japan: executive summary. Clin Infect Dis 2004;39(Suppl 1):S49–52.
Zinner SH. Changing epidemiology of infections in patients with neutropenia and cancer: emphasis on gram-positive and resistant bacteria. Clin Infect Dis 1999;29:490–4.
Gaur AH, Shenep JL. The expanding spectrum of disease caused by Bacillus cereus. Pediatr Infect Dis J 2001;20:533–4.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Kiyomizu, K., Yagi, T., Yoshida, H. et al. Fulminant septicemia of Bacillus cereus resistant to carbapenem in a patient with biphenotypic acute leukemia. J Infect Chemother 14, 361–367 (2008). https://doi.org/10.1007/s10156-008-0627-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10156-008-0627-y