Abstract
Background
There is no consensus amongst colorectal surgeons as to whether preoperative exercise is beneficial in the management of colorectal cancer patients. Research has shown higher rates of postoperative complications in patients who are less fit. Agreement needs to be sought on whether improving fitness via exercise should be a part of preoperative care. The Delphi process is an iterative process designed to refine opinions on a subject, until consensus agreement is reached within an expert group.
Methods
We performed a Delphi survey with a group of consultant colorectal surgeons. Statements achieving >80 % agreement were taken as consensus, those achieving >80 % disagreement were removed, and those in between were revised in the following round. The process ended with a group of statements which achieved consensus.
Results
Thirty-two statements were included in the first round of the survey. After three rounds of the survey, 21 statements were accepted as consensus, six statements were rejected, and seven statements did not reach consensus. It was agreed that exercise training should form part of preoperative care and would be supported by surgeons. That suitable programmes pose significant risk to patients was rejected. There was no consensus reached on the strength of current available evidence or whether it would be possible to deliver exercise programmes.
Conclusions
This work is the first to produce a set of statements on which expert consensus opinion has been agreed regarding preoperative exercise in colorectal cancer patients. Future work, informed by this study, will design interventions to produce rapid improvements in fitness before surgery.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
As the population ages, and as diagnostic techniques and healthcare improve, greater numbers of older patients are undergoing surgery for colorectal cancer. Age alone may not be an independent risk factor for poor postoperative recovery, but comorbid health conditions that often accompany ageing increase the risks of surgery for colorectal cancer [1].
Whilst some risk factors for increased postoperative morbidity, e.g. gender [2], cannot be modified, control of concurrent health conditions such as diabetes and chronic obstructive pulmonary disease can be improved preoperatively. Poor cardiorespiratory fitness may also be a risk factor that can be improved before surgery to reduce the risks of postoperative morbidity and mortality.
Although an intuitive assumption, there is now a growing evidence base confirming that increased fitness improves postoperative outcomes [3]. There is also published work showing that exercise prehabilitation in colorectal cancer patients is effective in improving preoperative fitness [4].
However, there is no consensus within surgical teams regarding the benefits of preoperative exercise, which modality of exercise is best, which patient populations would benefit from exercise, the possible risks and how to practically deliver exercise interventions. In the published literature, there is no definitive guidance on preoperative exercise before resection of colorectal cancer.
Enhanced Recovery After Surgery (ERAS) Society guidelines suggest that increasing exercise preoperatively may be of benefit but give no detail on amount, type or duration of exercise [5]. In the general population, there are many published guidelines recommending the amount of exercise to be taken by healthy individuals, but these do not relate specifically to colorectal cancer patients [6]. Changing practice to incorporate preoperative exercise would also require the involvement of stakeholders in developing these exercise programmes.
Delphi methodology is very widely used in health care to establish consensus on clinical issues [7]. The Delphi technique is an iterative process rooted in structured and repeated communication of specific statements that are revised and/or rejected according to expert responses to refine opinion on a topic until a preagreed level of consensus is reached. An expert panel scores a bank of statements relating to the topic on an agree/disagree Likert scale. Scores are accepted or rejected if consensus level is reached, and scores and remaining statements are recirculated either in original form or with revision to encourage consensus. The process is repeated for a given number of iterations, or until all statements have been accepted and consensus established. At the conclusion of a Delphi study, a set of statements agreed upon by an expert panel is produced.
The aim of this study was to establish an expert consensus from consultant colorectal surgeons on the role of preoperative exercise training for surgical patients with colorectal cancer.
Materials and methods
Study type
We conducted a three-round electronic Delphi study using e-mail invitations and a web-based survey tool (Bristol Online Surveys, University of Bristol, http://survey.bris.ac.uk). It was completed between April 2014 and November 2014. The study was granted ethical approval by the University of Nottingham Medical School Ethics Committee (C10042014 SoM MSGEM).
Participants
Currently practicing consultant colorectal surgeons were recruited by an e-mail invitation (“Appendix 1”). Invitations were sent to surgeons from units spread across the UK and working in teaching hospitals and district general hospitals. Those who registered their interest were sent a participant information sheet. Informed consent was obtained from all individual participants included in the study.
Procedure
Via e-mail, participants were invited to score an online survey instrument that considered the nature and form of prehabilitation for colorectal surgery. The survey was organised to consider five broad areas (potential benefits of improved aerobic performance, prehabilitation, intended users, risk management and practical application), and the research team constructed statements to best reflect a range of pertinent issues and topics. Scoring was based on a five-point (strongly agree, agree, neither agree nor disagree, disagree and strongly disagree) Likert scale; free-text boxes enabled participants to make further comment on their scoring and to contextualise their responses.
The survey instrument was scored on three separate occasions with the purpose of establishing consensus upon both general principles and specific aspects of prehabilitation for colorectal cancer surgery. Between scoring rounds, all participants received feedback of whole group responses; this feedback did not identify individual participants or their scores. Following each scoring round, specific statements were revised prior to rescoring to support the process of finding consensus.
At the outset, a score of 80 % (across agree/strongly agree or disagree/strongly disagree categories) was established as a consensus threshold: where 80 % participants agreed the statement was accepted to inform prehabilitation programmes; where 80 % disagreed the statement was rejected; statements where the 80 % threshold is not achieved were revised and rescored. In each round, participants were given 3 weeks to complete the survey with an e-mail reminder at 2 weeks.
Descriptive statistics for responses were generated after each round of scoring, and free-text comments reviewed to inform the development of subsequent rounds. After each round, statements exceeding the 80 % threshold (for agree or disagree) were accepted or rejected and removed from subsequent scoring. When appropriate, statements not removed were revised or reworded in accordance with the free-text comments before being used in the subsequent round. The number of statements lessened in rounds 2 and 3 as statements were accepted or rejected. A final e-mail was sent containing the agreed statements regarding exercise prehabilitation in colorectal cancer surgery patients.
Results
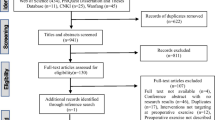
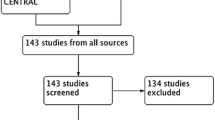
An invitation e-mail was sent to 33 consultant colorectal surgeons. Twenty responded and gave written consent to take part in the study. Responses to the first-round survey were received from 19 of 20 participants; these 19 respondents were sent second-round surveys. One participant did not receive the second-round survey and was withdrawn from the process. Eighteen participants were therefore sent third-round surveys, all of whom responded.
The first-round survey consisted of 32 statements (Table 1). Of these statements, 15 reached the predetermined consensus level of >80 % agreement and were accepted as exceeding the consensus threshold. Experts agreed that “Improved aerobic performance leads to”… improved preoperative cardiorespiratory function and better tolerance of the physiological demands of surgery, that “Exercise training could improve aerobic performance” and that “Exercise training could be used to beneficially improve aerobic performance in”… in patients awaiting elective, laparoscopic, open, malignant and non-malignant surgery and across all age ranges from 40 to those over 80 years old. In this round of statements it was also agreed that “Preoperative exercise training programmes” would be most useful if capable of improving performance within 31 days and if they were designed to provide the greatest gain in fitness in the shortest time frame. Ninety-four percentage of experts agreed that preoperative exercise training programmes would be supported in their own practice.
The statement “Preoperative exercise training programmes are likely to risk respiratory complications” received greater than 80 % disagreement and was removed from the survey. The remaining 16 statements were carried forward into the second-round survey.
At this point, the responses and free-text comments from the first Delphi round were analysed. This led to five questions from the first round being rephrased in an attempt to add clarity to the statements (1e, 2d, 3c, 4a and 4b). Additionally, three of the original first-round statements were divided into two parts each and reworded in order to aid clarity (1f, 2e and 4d). In total, 19 statements were therefore asked in the second-round survey (Table 1).
In the second-round survey, six statements were accepted. The expert panel agreed that “Improved aerobic performance leads to”… improved preoperative muscle strength, mood and wellbeing, and a reduced postoperative time to mobilisation and length of stay in hospital. Consensus was also reached that exercise training should be an aspect of preoperative care, and that exercise training could be used to beneficially improve aerobic performance in patients awaiting urgent (cancer) surgery.
Three statements regarding the risks of preoperative training programmes were rejected by the expert panel (“Preoperative exercise training programmes are likely to risk cardiac/neurological complications if the programme is personally tailored and suitable monitored” and “Musculoskeletal injuries if a low impact (e.g. cycling/swimming) programme is personally tailored and suitably monitored”). Consensus was not reached on the remaining 10 statements (Table 2).
At this point, statements and comments were again reassessed. This resulted in four statements being rephrased for the third round of the survey (1c, 2b, 3b and 5b from the second round). Additionally, two (1d and 1e from the second round) were consolidated and reworded into one statement (“Improved aerobic performance leads to reduced length of postoperative stay in high dependency unit (HDU)/intensive therapy unit (ITU)”). This resulted in nine statements being asked of the expert panel in the third round (Table 3).
During the third round, the two statements “Preoperative exercise programmes should be designed to improve muscle strength only” and “Exercise training could be used to beneficially improve aerobic performance in Patients awaiting emergency surgery within 24 h of admission” were rejected and seven statements did not reach consensus.
In total during the Delphi process, a total of 21 statements achieved the consensus agreement of the expert panel, six statements were rejected by the panel, and consensus was not reached on seven statements (“Appendix 2”).
Discussion
This Delphi study has produced a collection of statements that might inform the future development of prehabilitation programmes for colorectal cancer surgery patients. These statements have been agreed by an expert group of consultant colorectal surgeons and include agreement on the importance and role of exercise prehabilitation. Such consensus and detail has not been defined previously.
Surgeons agreed that improvement in aerobic capacity has many benefits in the perioperative period and that exercise should be part of a preoperative care package. It was agreed that patients undergoing elective and urgent operations for benign and malignant pathology across several age categories could be involved in preoperative exercise programmes. The expert group would globally support such exercise programmes.
The expert group disagreed that exercise should focus on improving muscle strength only and agreed that the emphasis should be on improving aerobic capacity. Previous studies using HIT in older people have shown significant improvements in aerobic capacity in other clinical groups such as lung cancer [8] and chronic cardiac disease patients [9]. The drawback with these studies is that improvement in fitness was seen over 6–12 weeks, whereas improvements in fitness in preoperative colorectal cancer patients would need to be evident in a shorter time frame. The group did not agree that preoperative exercise should be used in patients awaiting emergency surgery (defined as taking place <24 h from admission) due to the very limited time available and the acute nature of emergency surgical pathology. They also disagreed that suitably tailored and monitored exercise programmes pose high risk of complications to participants. In HIT studies on patients with known coronary artery disease, there have been very few adverse events reported [10, 11]. It seems likely that colorectal cancer patients without cardiorespiratory comorbidities would be at any higher risk of complications.
No consensus was reached on whether improved aerobic performance would reduce the need for intraoperative vasoactive drugs or length of postoperative stay in critical care wards. There were several free-text comments made during the survey, indicating that use of vasoactive drugs was outside the expert knowledge of consultant colorectal surgeons which may explain the lack of agreement in either direction. No consensus was reached regarding the improvement in balance or flexibility, with preoperative exercise nor the risks of musculoskeletal complications associated with high-impact exercise.
Interestingly, there was no consensus on whether there was currently good evidence of the benefits of preoperative exercise in colorectal cancer patients or whether this type of exercise programme would be deliverable in healthcare institutions at present. There is limited published work on preoperative exercise in colorectal cancer patients [12], especially in a time frame dictated by the national cancer waiting time limits. This would explain why even expert surgeons in the field are unconvinced by the strength of current published evidence. There is an evidence gap in this area that should be a focus for future work.
Further work also needs to be done on how an exercise programme in this patient group could realistically be set up within the NHS cancer pathway (personnel, facilities, timing etc). There was no consensus found amongst the expert group on how or whether this could be achieved.
A perceived limitation of this work may be the small number of consultant colorectal surgeons recruited to the study; however, it is well documented that although larger numbers of participants in Delphi studies will increase the reliability of group judgment, these improvements with group sizes above 12–15 participants are small [13].
Conclusions
This work has produced the first consensus agreement amongst an expert group of consultant colorectal surgeons on the importance of preoperative exercise in colorectal cancer patients and the benefits that exercise may give. It was agreed that a wide range of patients would benefit from preoperative exercise and that surgeons would support exercise programmes in their own institutions. However, it is clear from our results that more evidence is required to support the introduction of timely preoperative exercise interventions.
References
Wydra J, Kruszewski W, Jasiński W et al (2013) Is age a risk factor of postoperative complications in colorectal cancer? Pol Przegl Chir 85:491–495
Bertelsen CA, Andreasen AH, Jørgensen T, Harling H (2010) Anastomotic leakage after anterior resection for rectal cancer: risk factors. Colorectal Dis 12:37–43
West MA, Parry MG, Lythgoe D et al (2014) Cardiopulmonary exercise testing for the prediction of morbidity risk after rectal cancer surgery. Br J Surg 101:1166–1172
West MA, Loughney L, Lythgoe D et al (2015) Effect of prehabilitation on objectively measured physical fitness after neoadjuvant treatment in preoperative rectal cancer patients: a blinded interventional pilot study. Br J Anaesth 114:244–251
Gustafsson UO, Scott MJ, Schwenk W et al (2012) Guidelines for perioperative care in elective colonic surgery: Enhanced Recovery After Surgery (ERAS®) Society recommendations. Clin Nutr 31:783–800
World Health Organization (2010) Global recommendations on physical activity for health. World Health Organization, Geneva
Wesley V (2009) The Delphi technique: a review. Int J Ther Rehabil 16:69–76
Jones LW, Peddle CJ, Eves ND et al (2007) Effects of presurgical exercise training on cardiorespiratory fitness among patients undergoing thoracic surgery for malignant lung lesions. Cancer 110:590–598
Moholdt TT, Amundsen BH, Rustad LA et al (2009) Aerobic interval training versus continuous moderate exercise after coronary artery bypass surgery: a randomized study of cardiovascular effects and quality of life. Am Heart J 158:1031–1037
Meyer P, Normandin E, Gayda M et al (2012) High-intensity interval exercise in chronic heart failure: protocol optimization. J Card Fail 18:126–133
Guiraud T, Juneau M, Nigam A et al (2010) Optimization of high intensity interval exercise in coronary heart disease. Eur J Appl Physiol 108:733–740
O’Doherty AF, West M, Jack S, Grocott MPW (2013) Preoperative aerobic exercise training in elective intra-cavity surgery: a systematic review. Br J Anaesth 110:679–689
Murphy M, Black N, Lamping D et al (1998) Consensus development methods, and their use in clinical guideline development. Health Technol Assess 2:1–88
Acknowledgments
Thanks to the consultants of the Exercise Prehabilitation in Colorectal Cancer Delphi Study Group who participated in this study. The contributors were Patricia Boorman, Steven Brown, Gordon Buchanan, Nicola Fearnhead, Talvinder Gill, Aileen McKinley, Sarah Mills, Deborah Nicol, Stefan Plusa, Rupert Pullen, Mike Saunders, Humphrey Scott, Baljit Singh, Richard Slater, Bob Steele, Siram Subramonia, Arti Varma, Nicholas Watson and Gethin Williams.
Ethical standard
All procedures performed in this study were in accordance with the ethical standards of the University of Nottingham (UK) and with the 1964 Helsinki declaration and its later amendments.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
None.
Author information
Authors and Affiliations
Consortia
Corresponding author
Appendices
Appendix 1: E-mail invitation to participate in Delphi survey
Dear
I am a surgical research fellow working with Mr Jon Lund and Dr John Williams. We are looking at the benefits of preoperative exercise (“prehabilitation”) for elderly cancer patients prior to their cancer surgery.
Although much is known about the physiological benefits that occur with exercise and there is evidence for the improvement in surgical outcomes for fitter patients, there is no consensus opinion on how this exercise should be delivered in an elderly cancer population.
We are planning a Delphi study to achieve a consensus opinion from colorectal surgeon on the importance of prehabilitation and the practical application of such an exercise programme.
We have written to you as a consultant colorectal surgeon to invite you to take part in the study.
This would require,
-
Your written consent (either signed and returned by post or as an e-signature on a consent form returned by e-mail)
-
Completion of 3 online surveys. Each round will consist of statements to be marked against a Likert scale and the opportunity for further comments. The first survey will contain 40 statements, the second and third survey will contain progressively fewer statements
-
We ask that each survey is returned within the 3 weeks following its distribution. We anticipate that each survey will take approximately 15 min to complete
You will be informed of the consensus findings in a fourth and final e-mail.
The study is anonymous and you will not know who else is taking part.
The survey will be entirely e-mail/internet based.
The Delphi technique is an iterative process that has been used to establish consensus opinion on a variety of topics. After each round the results are anonymised and feedback provided; results are used to inform a subsequent survey instrument for the second round and the process is repeated. Consensus is achieved once >80 % of the expert body agree with a statement, it is then removed from the survey.
It is envisaged that all participants will be acknowledged on publication of this work as members of the Prehabilitation in Colorectal Cancer study group.
We hope that you will be able to help us to develop the body of evidence in this important area of research.
Please let us know if you have any questions about the logistics of the study.
If you are happy to participate please read the attached information sheet and sign and return the consent form. We will be in touch with your password for the survey as soon as the first round opens.
We look forward to hearing from you soon.
Appendix 2: Final results of survey
Statements achieving consensus agreement of the expert group
-
1.
Improved aerobic performance leads to improved preoperative cardiorespiratory function
-
2.
Improved aerobic performance leads to better tolerance of the physiological demands of surgery
-
3.
Improved aerobic performance leads to improved preoperative muscle strength
-
4.
Improved aerobic performance leads to improved preoperative mood and wellbeing
-
5.
Improved aerobic performance leads to reduced postoperative length of stay in hospital
-
6.
Improved aerobic performance leads to reduced postoperative time to mobilise
-
7.
Exercise training could improve aerobic performance
-
8.
Exercise training should be an aspect of preoperative care
-
9.
Preoperative exercise programmes should be designed to improve cardiorespiratory fitness
-
10.
Exercise training could be used to beneficially improve aerobic performance in patients awaiting elective (planned) surgery
-
11.
Exercise training could be used to beneficially improve aerobic performance in patients awaiting urgent (e.g. cancer) surgery
-
12.
Exercise training could be used to beneficially improve aerobic performance in patients between 40 and 60 years old awaiting surgery
-
13.
Exercise training could be used to beneficially improve aerobic performance in patients between 60 and 80 years old awaiting surgery
-
14.
Exercise training could be used to beneficially improve aerobic performance in patients over 80 years old awaiting surgery
-
15.
Exercise training could be used to beneficially improve aerobic performance in patients awaiting laparoscopic surgery
-
16.
Exercise training could be used to beneficially improve aerobic performance in patients awaiting open surgery
-
17.
Exercise training could be used to beneficially improve aerobic performance in patients with benign pathology
-
18.
Exercise training could be used to beneficially improve aerobic performance in patients with malignant pathology
-
19.
Preoperative exercise training programmes would be most useful if they improved aerobic performance within the 31 day time frame allowed for cancer surgery
-
20.
Preoperative exercise training programmes should be designed to give the greatest gain in fitness in the shortest time frame
-
21.
Preoperative exercise training programmes would be supported by you in your own practice.
Statements rejected by the expert group
-
1.
Preoperative exercise programmes should be designed to improve muscle strength only
-
2.
Exercise training could be used to beneficially improve aerobic performance in patients awaiting emergency surgery within 24 h of admission
-
3.
Individually tailored and suitably monitored preoperative exercise training programmes are likely to risk cardiac complications
-
4.
Individually tailored and suitably monitored preoperative exercise training programmes are likely to risk neurological complications
-
5.
Individually tailored and suitably monitored preoperative exercise training programmes are likely to risk respiratory complications
-
6.
Individually tailored and suitably monitored low impact preoperative exercise training programmes are likely to risk musculoskeletal complications.
Statements on which no consensus was achieved among the expert group
-
1.
Improved aerobic performance leads to reduced need for intraoperative vasoactive drugs due to better cardiac performance
-
2.
Improved aerobic performance leads to reduced length of HDU/ITU postoperative stay
-
3.
Preoperative exercise programmes should be designed to improve balance
-
4.
Preoperative exercise programmes should be designed to improve flexibility
-
5.
Individually tailored and suitably monitored high impact preoperative exercise training programmes are likely to risk musculoskeletal complications
-
6.
Preoperative exercise training programmes are already supported by robust evidence of their benefit
-
7.
Preoperative exercise training programmes are deliverable in your hospital.
Rights and permissions
About this article
Cite this article
Boereboom, C.L., Williams, J.P., Leighton, P. et al. Forming a consensus opinion on exercise prehabilitation in elderly colorectal cancer patients: a Delphi study. Tech Coloproctol 19, 347–354 (2015). https://doi.org/10.1007/s10151-015-1317-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-015-1317-2