Abstract
Distal anterior cerebral artery (DACA) aneurysms are rare, accounting for 1–9% of all intracranial aneurysms. Previous systematic reviews have highlighted that given the markedly increased incidence of major complications after endovascular treatment, microsurgical clipping is the more attractive treatment option with generally excellent clinical outcomes. Subcallosal DACA aneurysms constitute a rare subset of these aneurysms, requiring special anatomic considerations—particularly with regard to the approach. The aim of this study is to review the technical nuances of microsurgical treatment of subcallosal DACA aneurysms, including review of contemporary techniques through presentation of a microneurosurgical operative video. This is a retrospective case series and intraoperative microsurgical videos review. Three subcallosal DACA aneurysms were identified via retrospective query of our institutional neurosurgical database from December 2017 to May 2018. Two were female; median age was 74 years (range 70–83); all 3 underwent bifrontal craniotomy via bicoronal skin incision for aneurysm clipping. Aneurysms were located in left pericallosal–callosomarginal artery junction, bifurcation of azygos A2, and pericallosal artery related with azygos A2, and the anterior interhemispheric approach was used in all 3 operations. No acute stroke, hemorrhage, or major complications occurred, and all patients remained neurologically intact at the time of last follow-up (median 3 months, range 1–6). Although DACA aneurysms are rare, they represent an important variant for cerebrovascular neurosurgeons where microsurgical clipping can have better angiographic outcomes than endovascular treatment. Detail-oriented anterior interhemispheric arachnoid dissection through bifrontal craniotomy with its lower margin sitting at the superior orbital rim maximizes safe and effective clipping of subcallosal DACA aneurysms.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Distal anterior cerebral artery (DACA) aneurysms are rare, accounting for 1–9% of all intracranial aneurysms [1]. These lesions can arise at any DACA division, including the orbitofrontal, frontopolar, callosomarginal arteries, as well as more distal segments. Evidence for best treatment practices in these uncommon aneurysms is limited with equivocal results, including a major systematic review published in 2013 that demonstrated a markedly increased complication rate in endovascular treatment of DACA aneurysms—as high as 12% [2]. Of note, although a more recent meta-analysis published in 2017 demonstrated the observed differences in procedure-related morbidity and mortality between microsurgical clipping and endovascular treatment were not statistically significant, it did conclude that angiographic outcomes were significantly improved in microsurgical aneurysm clipping [3]. Correspondingly, clip ligation remains an effective and important treatment option for consideration in many DACA aneurysms. Subcallosal DACA aneurysms further complicate this calculus, as they typically require the anterior interhemispheric approach, necessitating meticulous, long arachnoid dissection through a narrow working corridor, which is further made complex by the rostrum and genu of corpus callosum overlying the aneurysm dome. Correspondingly, the goals of the present study were to report our single-institution series with treatment of 3 subcallosal DACA aneurysms using microsurgical clipping via the anterior interhemispheric approach, and to describe the key steps via operative video to review the technical pearls for successfully executing this challenging but critical microneurosurgical procedure.
Materials and methods
Under institutional review board approval, a retrospective query of an institutional neurosurgical database and review of an intraoperative video was performed. All patients provided documented consent for their images and other clinical information to be reported anonymously in presentation or journal.
Results
From December 2017 to May 2018, three patients underwent microsurgical clipping of subcallosal DACA aneurysms. Two were female; median age was 74 years (range 70–83). All three patients had an unruptured, saccular aneurysm with a median maximal diameter of 7 mm (range 4–7.8). All patients were discharged to home without stroke, hemorrhage, neurological deficits, or major medical morbidities, and were functionally independent at median follow-up of 3 months (range 1–6).
Case histories
Case 1
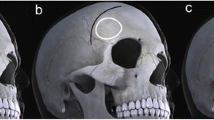
An 83-year-old right-handed female with a history of hypertension and medically stable sarcoidosis was incidentally discovered to harbor a left pericallosal–callosomarginal artery junction aneurysm. Subsequent follow-up magnetic resonance imaging (MRI) and MR angiography revealed enlargement of the aneurysm on two consecutive imaging intervals. The aneurysm had a complex configuration with a bi-lobulated shape and dome/neck ratio of 4.2/3.7 mm, and a maximal diameter of 7.8 mm, as measure on last preoperative computed tomography angiogram (CTA; Fig. 1a). T2-weighted MRI confirmed aneurysm localization just below the genu of the corpus callosum, projecting anteriorly and inferiorly (Fig. 1b). Despite her age, she was functionally independent, medically stable and in good condition for surgery. Intraoperative and postoperative course was uncomplicated, and postoperative CTA demonstrated complete obliteration of the aneurysm (Fig. 1c).
Preoperative images of case 1. Computed tomography angiogram (CTA) with 3D reconstruction demonstrated a bi-lobulated aneurysm in the left pericallosal–callosomarginal artery junction (a). Magnetic resonance imaging (MRI) in T2 sequence showed the aneurysm was located just below the genu of corpus callosum, projecting anteriorly and inferiorly (b). The black arrow shows the aneurysm. Postoperative CTA with 3D reconstruction demonstrated complete obliteration of the aneurysm (c)
Case 2
A 74-year-old right-handed female with a history of hypertension, diabetes mellitus, dyslipidemia, and subclavian artery stenosis on clopidogrel undergoing unrelated medical workup was found to have a snowman-shaped 7 × 5 mm aneurysm at the azygos A2 bifurcation (Fig. 2a). T2-weighted MRI confirmed that the aneurysm projected superiorly from its position beneath the rostrum of the corpus callosum (Fig. 2b). Of further note, a large bleb in the aneurysm was observed to be in line with the projection of the azygos A2 and was correspondingly thought to imply an increased risk of aneurysm rupture and subarachnoid hemorrhage (SAH). Intraoperative and postoperative course was uncomplicated, and postoperative CTA demonstrated complete obliteration of the aneurysm (Fig. 2c).
Preoperative images of case 2. CTA with 3D reconstruction demonstrated an aneurysm with a large bleb in azygos A2 bifurcation (a). MRI in T2 sequence showed the aneurysm projecting superiorly beneath the rostrum of corpus callosum (b). The black arrow shows the aneurysm. Postoperative CTA with 3D reconstruction demonstrated complete obliteration of the aneurysm (c)
Case 3
Magnetic resonance angiogram (MRA) completed for an unrelated medical workup in a 70-year-old right-handed gentleman with a history of hypertension demonstrated a 4 × 2 mm saccular aneurysm of the pericallosal artery, which was associated with an azygos A2 segment (Fig. 3a). T2-weighted MRI confirmed a superiorly projecting aneurysm dome, which was buried in the rostrum of corpus callosum (Fig. 3b). As in case 2, the aneurysm’s projection was noted to be in straight alignment with the azygos A2 and therefore considered to be high risk for rupture and SAH, prompting microsurgical treatment. Intraoperative and postoperative course was uncomplicated, and postoperative CTA demonstrated complete obliteration of the aneurysm (Fig. 3c).
Preoperative images of case 3. Magnetic resonance angiogram (MRA) demonstrated a saccular aneurysm in the pericallosal artery associated with azygos A2 (a). MRI in T2 sequence showed the aneurysm projecting superiorly was buried in the rostrum of corpus callosum (b). The white arrow shows the aneurysm. Postoperative CTA with 3D reconstruction demonstrated complete obliteration of the aneurysm (c)
Operative approach
All 3 patients were treated using the same surgical strategy. In each operation, the patient was positioned supine with their head fixed in the neutral position using three-point pinion fixation. Bilateral lower extremity somatosensory evoked potential (SSEP) was monitored throughout the procedure. A coronal skin incision was made behind the hairline, and a pedicled pericranial flap was elevated for frontal sinus reconstruction during closure. Bilateral temporalis fat pad dissections were completed, allowing maximal inferior exposure beyond the lower margin of the glabella. A bifrontal craniotomy was fashioned, with multiple burr holes placed overlying the sinus and at 3 cm lateral to the midline bilaterally, again allowing for maximal inferior exposure to the level of the superior orbital rim. The bilateral frontal sinuses were demucosalized for postoperative cranialization and protected with iodine-soaked cotton pads intraoperatively. The dura was initially opened on the right side. When a prominent bridging vein running low close to the frontal base was encountered, we selectively opened the dura on the left side to ligate the superior sagittal sinus at its insertion on the crista galli, and cut the falx to allow its retraction superiorly, resulting in a maximized working corridor below the bridging vein.
With the exposure completed, an anterior interhemispheric dissection was carried out in the three-step fashion described by Ito et al. [4] First, the interhemispheric fissure anterior to the genu of corpus callosum was dissected with the operating table maneuvered into a vertex-down head position to expose bilateral pericallosal arteries lying on the genu. Second, reverse Trendelenburg position was applied, allowing for a safer and more comfortable anterior interhemispheric dissection, which was carried inferiorly toward the planum sphenoidale. Third, the operating table was returned to a neutral head position, allowing for dissection of suprachiasmatic cistern and optimal visualization of the proximal A2 segments and/or azygos A2 (Fig. 4a–c).
Schematic drawings of intraoperative concepts of anterior interhemispheric approach by Ito et al. [4] The shaded area demonstrates craniotomy, lower margin of which is at the superior orbital rim. The green arrow shows the projection of operating microscope in each step. First, the genu of corpus callosum and bilateral pericallosal arteries lying just above it are exposed with the patient’s head positioned neutral. In this step, microscope projection is nearly vertical to the floor to maximize effective confrontation to enable flat and wide exposure of the genu (a). In the next step, a reverse Trendelenburg position is applied to allow for dissection of the cingulate and rectal gyri until exposure of the planum sphenoidale. Operating microscope should be projecting forward so that the operator is vertically confronting the anterior skull base (b). Finally, the head position is returned neutral for exposure of proximal A2 segments or azygos A2. Operating microscope projection is modified back to neutral to confront neutrally to A2 (c). Adjustment of patient’s head orientation and operating microscope projection provides more comfort for the operator. Used with permission of Mayo Foundation for Medical Education and Research, all rights reserved
Satisfactory proximal control with safe application of a temporary clip to the parent artery was achieved in every case. For each operation, a single titanium aneurysm clip was initially placed in parallel with the artery and across the neck of the aneurysm. Indocyanine green (ICG) angiography was performed following clip reconstruction to confirm complete occlusion of the aneurysm and uncompromised patency of the parent artery, followed by application of additional clip, as needed. Quantitative vascular flow measurements were assessed prior to and following clip application, using the Doppler ultrasound probe (DVM-4300T, Hadeco, Inc., Kawasaki, Japan). All cases were closed with a watertight dural approximation, which was reinforced using fibrin sealant. The inner table of the frontal sinus was removed to complete the cranialization process and to allow uncompromised covering of the frontal sinus floor using the pedicled pericranial flap. Bifrontal bone flaps were fixed with titanium plates and screws positioned so as to maximize cosmesis, and the scalp was closed over a subgaleal drain (Supplemental digital content 1, Video 1).
Actual surgical video of Case 3 (4 minutes and 28 seconds; 402MB) (MP4 412156 kb)
Postoperative course
All patients underwent postoperative CT and MRI to rule out postoperative hemorrhage or stroke. All patients were encouraged early mobilization from the next day of the surgery. All patients returned to home without neurologic deficit as of last clinical follow-ups at 1, 3, and 6 months postoperatively.
Discussion
DACA aneurysm
DACA aneurysms may arise from any DACA divisions including the frontobasal artery, A2 or A3 trunks, and, rarely, the more distal segments [1]. Within this subset of cerebrovascular lesions, A2 segment aneurysms are the most rare, representing 0.2–1% of all intracranial aneurysms, and 5–22% of all DACA aneurysms [5]. By contrast, A3 segment lesions are the most common, accounting for 2–7% of all intracranial aneurysms, and 69–82% of all DACA aneurysms [5]. Interestingly, the azygos anterior cerebral artery appears to be highly associated with DACA aneurysms, with multiple preceding analyses reporting a prevalence of 3–22% [5]. In our case series, aneurysms were diversely distributed, involving the pericallosal–callosomarginal artery junction, azygos A2 bifurcation, and pericallosal artery related with an azygos A2. Our cohort included fairly elderly patients, and indication for treatment vs. observation was discussed based on the PHASES score [6], and all the three patients carried a rupture risk of more than 4% within 5 years. The most elderly patient (case 1, age 83 years) had growth of her aneurysm on two consecutive follow-up images. She was in excellent health, living independently, and after extensive discussion of the risks and benefits of treatment she elected to proceed with repair of her aneurysm.
Endovascular treatment vs. microsurgical clipping
Although progressive advances in the development of endovascular devices and technique have enabled catheter-based treatments of DACA aneurysms, earlier studies suggested that these lesions were associated with markedly increased rates of major complications, including arterial dissection, intraprocedural rupture, and incomplete occlusion. These findings were initially consolidated via a systematic review and meta-analysis published in 2013 by Sturiale et al., which reported a relatively high overall rate of total/near-total occlusion at 78% during a mean follow-up of 13.47 ± 8.73 months, as well as a high rate of periprocedural complications exceeding 12% [2]. More recently, a subsequent meta-analysis inclusive of a contemporary dataset was published in 2017 which did not reproduce the same significant difference in complications, but perhaps more importantly did identify a dramatic advantage in the primary endpoint of durable occlusion. More specifically, as compared to endovascular modalities, microsurgical clipping was associated with a significantly higher rate of complete aneurysm occlusion at last follow up (97.0% vs. 69.0%, p < 0.0001), as well as significantly lower rates of aneurysm recurrence (2.0% vs. 18.0%, p < 0.0001) and aneurysm rebleeding (0.0% vs. 2.0%, p = 0.029) [3]. Taken together, while endovascular treatment has improved, and a certain cohort of DACA aneurysms with amenable configuration, size, and projection can still be treated with endovascular treatments, and fast recovery is undoubtedly an attractive strong point of endovascular treatment, microsurgical clip reconstruction, on the other hand, remains a safe and effective treatment strategy with higher treatment success rate and lower risk of recurrence in trade-off of a nature of craniotomy and involved recovery from surgery.
Technical details of microsurgical clipping for subcallosal DACA aneurysms
Subcallosal DACA aneurysms are highly unusual subspecies of the more commonplace distal DACA aneurysms, which require an anterior interhemispheric approach (AIH) for clipping. The frontal sinus is often opened, and this results in small but significant increase in risk for several complications, such as cerebrospinal fluid (CSF) leak (with or without associated meningitis), mucocele formation, and anosmia. Nakayama et al. reported in their series of 142 basal interhemispheric approaches for anterior communicating artery aneurysm clipping, an overall rate of frontal sinus violation at 97%, which resulted in CSF rhinorrhea in 4 cases (2.8%), and meningitis in 6 cases (4.2%) [7]. Anosmia similarly occurred in 6 cases (4.2%), although oddly, this did not correlate with reported intraoperative olfactory nerve injury [7].
To avoid such complications, we utilized a vascularized pericranial flap to cover the floor of the frontal sinus after cranialization. Similarly, immediately following the dural opening, we dissected the bilateral olfactory tracts off the interior frontal lobes and fixed the olfactory bulbs to the frontal base prior to the draining of significant CSF, in order to reduce the risk of retraction injury. Intracranially, as has been emphasized by many preceding authors [8,9,10], we adhered strictly to a practice of bridging vein preservation. Numerous techniques have been described to optimize AIH exposure within the limits of bridging vein preservation, including the interfalcine approach described by Fujitsu et al. [11], and the bridging vein rerouting procedure advocated by Ohara et al. [12] In two cases from our case series, no major bridging vein was encountered at the anterior skull base, allowing for an optimal approach; by contrast, in case 2, we achieved an excellent exposure by ligating the anterior superior sagittal sinus, releasing the falx, and retracting it superiorly. We performed a bifrontal craniotomy; however, a smaller craniotomy with unilateral exposure and therefore a smaller incision can be considered in selected cases when preoperative imaging studies convincingly demonstrate that there are no bridging veins that would obstruct a unilateral AIH approach. Admittedly, we prefer the bilateral approach as we do not feel the slightly larger incision or craniotomy increases the overall risk or morbidity of the operation significantly, and allows for the option of primarily approaching the aneurysm through either a right- or left-sided parafalcine trajectory depending on the most favorable venous anatomy.
Another key technical aspect of the AIH we echo from the description by Ito et al. [4] is the importance of adjusting the patient’s head position (and, in tandem, the trajectory of the operating microscope) from vertex-down to vertex-up during the posterior and anterior dissections, and finally vertex-neutral for the approach to the aneurysm dome itself (Fig. 4a–c). In order to further capitalize on the positional advantages afforded by the AIH, we strongly emphasize the importance of a very low craniotomy—particularly when clipping subcallosal DACA aneurysms. In these atypical lesions, the corpus callosum overlies the aneurysm, which effectively limits both the range of potential working corridors for the microscope and the options for clip applier trajectories (and therefore clip and clip-configuration options). The impact of these constraints is particularly critical in subcallosal DACA aneurysms with superior projection (e.g., cases 2 and 3), with a lower lying aneurysm position along the anterior skull base (case 2), or with the rostrum of corpus callosum angled down below the horizontal line (case 3). In these instances, the best available clip applier angle was defined by the lower margin of the craniotomy (Fig. 5); correspondingly, in order to achieve maximal visualization and safe, satisfactory aneurysm clip ligation, the combination of a very low craniotomy extending to the superior margin of the orbit is essential, and optimize through the use of aggressive, temporary Trendelenburg positioning.
Schematic drawing of concept illustrating importance of low craniotomy in subcallosal DACA aneurysm with superior projection, and inferiorly projecting baseline of the rostrum of corpus callosum. The shaded area demonstrates craniotomy, and the arrow indicates the projection of clip applier, which is limited by the lower margin of the craniotomy. © Used with permission of Mayo Foundation for Medical Education and Research, all rights reserved
Conclusion
Although DACA aneurysms are rare, they represent an important variant for cerebrovascular neurosurgeons in which microsurgical clipping can have better angiographic outcomes than endovascular treatment. Clipping of subcallosal DACA aneurysms requires unique microsurgical nuances as the rostrum of the corpus callosum limits the surgical view and working corridor. Detail-oriented anterior interhemispheric arachnoid dissection via a low frontal craniotomy, with its inferior margin sitting at the superior orbital rim, enables maximal visualization as well as safe, durable, and effective clipping of subcallosal DACA aneurysms.
References
Carvi y Nievas MN (2010) The influence of configuration and location of ruptured distal cerebral anterior artery aneurysms on their treatment modality and results: analysis of our casuistry and literature review. Neurol Res 32(1):73–81
Sturiale CL, Brinjikji W, Murad MH, Cloft HJ, Kallmes DF, Lanzino G (2013) Endovascular treatment of distal anterior cerebral artery aneurysms: single-center experience and a systematic review. AJNR Am J Neuroradiol 34(12):2317–2320
Petr O, Coufalova L, Bradac O, Rehwald R, Glodny B, Benes V (2017) Safety and efficacy of surgical and endovascular treatment for distal anterior cerebral artery aneurysms: a systematic review and meta-analysis. World Neurosurg 100:557–566
Ito Z (1982) The microsurgical anterior interhemispheric approach suitably applied to ruptured aneurysms of the anterior communicating artery in the acute stage. Acta Neurochir 63(1–4):85–99
Lehečka M (2009) Distal anterior cerebral artery aneurysms. University of Helsinki, Helsinki
Greving JP, Wermer MJ, Brown RD Jr et al (2014) Development of the PHASES score for prediction of risk of rupture of intracranial aneurysms: a pooled analysis of six prospective cohort studies. Lancet Neurol 13(1):59–66
Nakayama H, Ishikawa T, Yamashita S, Fukui I, Mutoh T, Hikichi K, Yoshioka S, Kawai H, Tamakawa N, Moroi J, Suzuki A, Yasui N (2011) CSF leakage and anosmia in aneurysm clipping of anterior communicating artery by basal interhemispheric approach. No Shinkei Geka 39(3):263–268
Aoki N, Sakai T, Oikawa A, Tsutsumi K (1990) Significance of preserving bridging veins in an interhemispheric approach. Surg Neurol 33(2):159–160
Kubota M, Saeki N, Yamaura A, Ono J, Ozawa Y (2001) Influences of venous involvement on postoperative brain damage following the anterior interhemispheric approach. Acta Neurochir 143(4):321–325 discussion 325-326
Tsutsumi K, Shiokawa Y, Sakai T, Aoki N, Kubota M, Saito I (1991) Venous infarction following the interhemispheric approach in patients with acute subarachnoid hemorrhage. J Neurosurg 74(5):715–719
Fujitsu K, Sekino T, Sakata K, Kawasaki T (1994) Basal interfalcine approach through a frontal sinusotomy with vein and nerve preservation. Technical note. J Neurosurg 80(3):575–579
Ohara K, Inoue T, Ono H, Kiyofuji S, Tamura A, Saito I (2017) Technique for rerouting a bridging vein that hinders the anterior interhemispheric approach: a technical note. Acta Neurochir 159(10):1913–1918
Previous presentation
Components of this study (case presentation) will be presented as a poster at the North American Skull Base Society 29th Annual Meeting, Orlando, FL, February 15–17, 2019.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This is a retrospective investigational study of patients who underwent treatment and does not report on primary research or new protocols. This study was carried out under IRB approval.
Informed consent
All patients provided documented consent for their images and other clinical information to be reported anonymously in presentation or journal.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Kiyofuji, S., Sora, S., Graffeo, C.S. et al. Anterior interhemispheric approach for clipping of subcallosal distal anterior cerebral artery aneurysms: case series and technical notes. Neurosurg Rev 43, 801–806 (2020). https://doi.org/10.1007/s10143-019-01126-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-019-01126-z