Abstract
The objective of the present study is to assess the influence of extent of resection (EoR), use of intraoperative imaging, and awake surgery on health-related quality of life (HRQoL) in high-grade glioma (HGG) patients in a prospective multicenter study. We analyzed 170 surgeries of patients suffering from a HGG. During the first year after resection, HRQoL was evaluated using the European Organization of Research and Treatment of Cancer Core Questionnaire C30 and Brain Neoplasm 20 questionnaires. We assessed the influence of EoR; awake surgery; and use of 5-aminolevulinic acid (5-ALA), intraoperative MRI (iMRI), and their combination on sum scores for function and symptoms as well as several neurological single items. In mixed-model analyses, adjustments for age, Karnofsky performance status (KPS), and eloquent location were performed. In the mixed model, EoR generally did not significantly influence HRQoL (p = 0.10). Yet, patients receiving subtotal resection (STR) vs. patients with biopsy showed significantly better QoL and role and cognitive functions (p = 0.04, p = 0.02, and p < 0.01, respectively). The combination of iMRI and 5-ALA reached the highest EoR (95%) followed by iMRI alone (94%), 5-ALA alone (74%), and no imaging (73%). Thereby, neurological symptoms were lowest and functioning score highest after combined use of iMRI and 5-ALA, without reaching significance (p = 0.59). Despite lower scores in emotional function (59 vs. 46, p = 0.24), no significant impact of awake surgery on HRQoL was found (p = 0.70). In HGG patients, STR compared to biopsy was significantly associated with better HRQoL and fewer neurological symptoms in this series. An escalated use of intraoperative imaging increased EoR with stable or slightly better HRQoL and fewer neurological symptoms. Based on HRQoL, awake surgery was a well-tolerated and safe method in our series.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
High-grade gliomas (HGGs) are malignant primary brain tumors with an incidence of 3–4/100,000 inhabitants per year, representing 5% of all solid tumors in adults. Despite being a rare disease compared to other malignant neoplasms such as bronchial or breast cancer, gliomas are known for their rapid, invasive growth, and subsequent significant symptoms such as focal neurological deficits, neurocognitive disorders, and seizures as signs of increased intracranial pressure and infiltration of surrounding tissue. Even though survival of HGG is quite short with a mean overall survival (OS) between 12 and 18 months for glioblastoma (GB) and about 41 months for anaplastic astrocytoma, individual survival can be heterogeneous depending on various factors [1–3]. It is therefore inevitable that quality of life be considered by balancing different treatment options to achieve a livable outcome for each individual patient.
Patient-reported outcome (PRO) measures are the most effective way of directly measuring patients’ well-being and health status [4]. As one of the most common PRO measures, health-related quality of life (HRQoL) has become a frequent secondary outcome measure in randomized clinical trials [5].
According to the literature, the extent of resection (EoR) and volume of the tumor remnant have a crucial impact on survival in HGG [2]. The prognosis for HGG has improved over the last 20 years, not least due to new intraoperative imaging techniques allowing more radical resections before administration of adjuvant treatment. Level 1 evidence exists showing that the use of intraoperative MRI (iMRI) and 5-aminolevulinic (5-ALA) acid fluorescence improves EoR and survival in HGG patients [6, 7]. On the other hand, curative resections are impossible due to the infiltrative growth of tumor cells in HGG, and increasing the EoR might increase neurological deficits, as has been shown for eloquent lesions in the early years of 5-ALA application [8]. Furthermore, a more radical surgery might lead to subtle deficits that remain subclinical but still affect patients’ subjective HRQoL regarding social or role functioning [9, 10]. Thus, it is important to analyze HRQoL in addition to persistent neurological deficits to not only extend a patient’s life, but also to maintain a good quality of life as perceived by the patient him/herself. Further, HRQoL might be impaired by the surgical procedure itself; e.g., for awake surgeries, there are reports of increased distress or even symptoms of posttraumatic stress disorder [11, 12].
Given this background, the objective of this study was to assess the impact of the EoR, intraoperative imaging, and awake surgery on HGG patients’ HRQoL. We aimed to compare HRQoL after varying degrees of resection (biopsy only vs. subtotal (STR) vs. gross total (GTR) resections). In addition to assessing the impact of using different intraoperative imaging techniques (iMRI, 5-ALA, neuronavigation only), we also aim to assess progressive approaches like supramaximal resections using a combined imaging approach of iMRI and 5-ALA as well as awake surgery on HRQoL.
Methods
Study design
We used a prospective multicenter cross-sectional design to allow for an assessment of different surgical methods in an unselected patient cohort. Concerning intraoperative imaging, we concentrated on iMRI and 5-ALA, as those are the only methods with level 1 evidence to increase the EoR and survival in GB [53, 55].
Setting
The current assessment was performed as part of the “ERASMUS” trial (clinical trial ID: NCT02728024). Between June 2013 and June 2016, we recruited 427 patients for the ERASMUS trial in the following four institutions: University of Ulm (Oncology, Ulm and Neurosurgery, Günzburg,), University Medical Centre Mainz (Neurosurgery), Katharinenhospital Stuttgart (Neurosurgery), and the Ludwigsburg Hospital (Department of Neurology and Neurosurgery). As part of the ERASMUS trial, glioma patients were interviewed cross-sectionally during their postoperative routine outpatient visits, usually every 3 to 6 months and prior to surgery as part of routine preoperative inpatient admission. From the collected data, we selected the patients’ first available follow-up information after surgery to assess their postoperative HRQoL for the current analysis.
Participants and study size
Inclusion criteria were age >18 years, diagnosis of a HGG, surgery to survey time of no more than 12 months, ability to give informed consent, adequate knowledge of German language, and no global aphasia. Patients who were unable to be interviewed or fill in the questionnaire by themselves or with assistance were excluded.
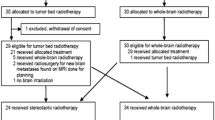
As shown in Fig. 1, 162 patients finally matched the inclusion criteria for the present assessment, yielding 170 surgeries/cases with respective postoperative assessment to be evaluated in the mixed models. The median time of assessment for the current study was 4 months after surgery, with a maximum of 1 year after surgery.
Bias
We used a standardized clinical and radiological assessment protocol in all participating centers. As part of this protocol, the patients’ HRQoL was assessed prior to consultation with an oncologist to avoid a negative bias due to temporary distress caused by patients’ knowledge of the radiological progress. Statistically, we controlled for repeated measures and for the preoperative HRQoL level to minimize influence of progressive disease and individual HRQoL variation.
Assessed variables
Health-related quality of life
To assess HRQoL, we used the validated and well-established European Organization of Research and Treatment of Cancer Core Questionnaire C30 (EORTC QLQ-C30) [3, 13] with its brain cancer-specific module Brain Neoplasm 20 (BN20) (EORTC QLQ-BN20) [14]. Concerning missing values, the standard procedure as recommended by the EORTC QLQ C30 manual was performed: If at least half of the items contributing to the subscore were present, a mean score for these was used so that it is algebraically equivalent to using all items.
We evaluated all functioning scores. Neurological deficits (motor dysfunction, visual disorder, communication deficit, seizures, and weakness of legs) were additionally assessed as single items because they represent very common symptoms in brain tumor patients with a large impact on daily living. Global health status (GHS) and QoL were evaluated separately as single items.
Previous findings show that global assessment of HRQoL is difficult using several single scores as in the classical EORTC scoring system. Hence, we calculated sum scores per Hinz et al. [15, 16]. Accordingly, three sum scores were calculated including all functioning items (functioning score), all symptom items (symptom score), and a total score of all 30 items in the EORTC QLQ-C30 questionnaire. In the event of any missing values in the QLQ-C30 questionnaire, the patient’s data were not used for calculating sum scores. In the total score and functioning score, high values represent a good condition, while a greater symptom score correlates with a higher symptom burden and hence poorer condition.
Clinical variables
As part of the prospective study protocol, the following clinical data were recorded: postoperative Karnofsky performance status (KPS), age, gender, histological diagnosis, WHO grading, eloquent and main localization, time of diagnosis, EoR, intraoperative imaging, and awake surgeries. The EoR was classified into three different groups. Gross total resection (GTR) was defined as complete resection of contrast-enhanced tumor on early postoperative imaging (MRI). The biopsy group was defined as patients undergoing scheduled open or stereotactic biopsies. All other patients were summarized in “subtotal resection” (STR). Intraoperative imaging was only analyzed in cases with intended GTR and was divided into four different subgroups: no imaging, 5-ALA, iMRI, and iMRI and 5-ALA.
Statistical analysis
For statistical analyses, we used a general linear mixed model (GLMM) with the independent/explanatory variables EoR and awake surgery (model 1) as well as intraoperative imaging (model 2) and the dependent variables from EORTC QLQ-C30/BN20 questionnaire. We fitted the GLMM with a random intercept and used the Satterthwaite method to find the denominator degrees of freedom. This model was utilized to account for correlated outcomes within patients. A clinical/hypothesis-driven approach was applied to compose the model. We decided to categorize age >=70 years and KPS <70 as potential risk factors for diminished quality of life as they are common cutoff values in clinical decision making. Adjustment for KPS, age of the patient, eloquent location, and preoperative EORTC QLQ-C30/BN20 values were performed. We controlled for repeated measurements in eight patients with recurrent surgeries. Separate models for the EoR (model 1) and intraoperative imaging (model 2) were calculated since they influence one another. Additionally, in model 2, only patients with intended GTR were included. We tested for fixed effects and calculated least square means. Further, we performed pairwise comparisons for categorical explanatory variables with more than two levels fitting the GLMM. We did not adjust for multiple testing since we performed an exploratory assessment.
We tested for significant differences in the EoR depending on the intraoperative imaging technique used with chi-squared tests.
To analyze our collected data, we used the statistical software IBM SPSS Statistics 21 (IBM Corp. 2012, Armonk, NY, USA) and SAS 9.4 (SAS Institute Inc., 2013, Cary, NC, USA).
Results
Patient and surgery characteristics
The characteristics of patients at the time of assessment are illustrated in Table 1. The characteristics of the surgeries are found in Table 2.
General mixed-model assessments
Impact of Karnofsky performance status on HRQoL (models 1 and 2)
With regard to KPS, we found a significant association with patients’ HRQoL. Patients with a postoperative KPS above or equal to 70 showed a significantly better total score (model 1, 45.6 vs. 64.4, p < 0.001; model 2, 50.2 vs. 72.3, p = 0.003) and functioning score (model 1, 32.8 vs. 61.1, p < 0.001; model 2, 37.1 vs. 68.3, p < 0.001), with a simultaneous reduced symptom burden in the mixed model (model 1, 38.8 vs. 30.2, p = 0.02; model 2, 35.7 vs. 21.3, p = 0.02). Evaluating the EORTC scores, physical (model 1, 25.2 vs. 64.7, p < 0.001; model 2, 31.4 vs. 68.7, p < 0.001), role (model 1, 14.9 vs. 54.5, p < 0.001; model 2, 41.3 vs. 67.6, p = 0.02), emotional (model 1, 44.4 vs. 58.6, p = 0.01; model 2, 41.9 vs. 62.8, p = 0.02), and social (model 1, 30.8 vs. 61.7, p < 0.001; model 2, 41.4 vs. 75.6, p = 0.003) functioning items were significantly higher, and they suffered less from visual disorders (model 1, 34.7 vs. 15.2, p < 0.001; model 2, 34.0 vs. 4.8, p < 0.001), motor dysfunction (model 1, 55.2 vs. 28.6, p < 0.001; model 2, 44.3 vs. 13.5, p < 0.001), and weakness of the legs (model 1, 50.3 vs. 31.0, p = 0.01; model 2, 42.7 vs. 16.2, p = 0.01) compared to patients with a KPS below 70 in both mixed models.
Impact of patients’ age on HRQoL (models 1 and 2)
Social functioning was significantly higher in patients ≤70 years of age (model 2, 40.2 vs. 76.7, p = 0.002). In the mixed model adjusted for intraoperative imaging (model 2), patients >70 years of age reported motor dysfunction more often (model 2, 37.9 vs. 19.9, p = 0.05). Apart from this, in the mixed-model assessment, we did not find any significant differences based on patient age.
Impact of eloquent location on HRQoL (models 1 and 2)
Eloquent location was significantly associated with HRQoL. In particular, GHS (model 2, 4.4 vs. 3.8, p = 0.02), QoL (model 2, 4.8 vs. 3.8, p < 0.001), role (model 2, 67.9 vs. 40.9, p < 0.001), cognitive (model 2, 62.9 vs. 48.7, p = 0.04), and social functioning (model 1, 53.1 vs. 39.4, p = 0.02; model 2, 67.2 vs. 49.8, p = 0.02) and the sum score for functioning outcome (model 2, 56.9 vs. 48.5, p < 0.001) were lower if the tumor location was eloquent. Further, we found significantly higher levels of motor dysfunction (model 2, 23.4 vs. 34.5, p < 0.001), communication deficit (model 1, 29.1 vs. 48.1, p < 0.001; model 2, 17.3 vs. 41.6, p < 0.001), and weakness of the legs (model 2, 22.4 vs. 36.4, p = 0.04) in this subgroup. Except for social functioning and communication deficit, significant differences were only seen in model 2.
Impact of the EoR on quality of life (model 1)
Table 3 shows a detailed assessment of estimated means in model 1. One hundred seventy cases were included in the respective analysis. Figure 2 shows estimated means of sum scores for GTR, STR, and biopsy. Concerning the sum scores, we found no significant differences between GTR, STR, and biopsy. Nonetheless, the total score for biopsy showed lowest values compared to both, GTR and STR.
a Estimated mean of summary scores with mixed-model calculation for the extent of resection according to Hinz et al. [15] GTR gross total resection, STR subtotal resection. b Estimated mean of summary scores with mixed-model calculation for the extent of resection according to Hinz et al. [15] GTR gross total resection), STR subtotal resection
We found a significant influence of the EoR on role and cognitive functioning (p = 0.03; p = 0.04) Post hoc assessment showed that the difference between STR and biopsy was significant for these two scores (p = 0.02, p = 0.01) and for quality of life (p = 0.04). Weakness of the legs was significantly lower in GTR and STR compared to biopsy in post hoc tests (p = 0.03; p = 0.02).
Influence of awake surgery on quality of life (model 1)
We compared patients after awake surgery (n = 18) with patients after general anesthesia (n = 152) in model 1. Evaluating sum scores, we did not see significant differences between the two groups (Fig. 3, Table 3). Assessing functioning and symptom scores, patients undergoing awake surgery reported seizures significantly more often (p = 0.04). No other significant findings were seen in this model (Table 3).
Impact of intraoperative imaging on quality of life (model 2)
We compared the impact of intraoperative imaging methods in cases with an intended GTR (n = 101). Table 2 shows the distribution of the imaging techniques used. The rate of GTR by type of applied imaging technique is shown in Table 4. The highest rates were found for iMRI alone and combined use of iMRI and 5-ALA (94; 95%) compared to no imaging (73%) and 5-ALA (74%). For the combined use of iMRI and 5-ALA, the rate of achieved GTR was significantly improved compared to no intraoperative imaging.
The impact of intraoperative imaging on HRQoL was assessed in model 2. One hundred one cases were entered into the model (Table 3). Sum scores showed no significant disparities between the different modalities. Nonetheless, we saw a general upward trend in functioning and total score while escalating intraoperative imaging from no imaging to 5-ALA and iMRI up to a combination of both (Fig. 4). Correspondingly, symptom score was worst after surgeries without the use of intraoperative imaging (Table 5).
a Estimated mean of summary scores with mixed-model calculation for intraoperative imaging according to Hinz et al. [15] 5-ALA 5-aminolevulinic acid, iMRI intraoperative magnetic resonance imaging. b Estimated mean of summary scores with mixed-model calculation for intraoperative imaging according to Hinz et al. [15] 5-ALA 5-aminolevulinic acid, iMRI intraoperative magnetic resonance imaging
Assessing functioning and symptom scores, visual disorder was significantly influenced by intraoperative imaging (p = 0.04). In post hoc assessments, the combined use of 5-ALA and iMRI showed significantly less visual disorder than no imaging (p < 0.01) or 5-ALA (p = 0.04). All other scores showed no significant difference. In general, the highest estimated mean scores for functioning and the lowest for symptoms were found using iMRI alone or combined with 5-ALA (Table 3).
Discussion
Patients suffering from a HGG show distinctly lower HRQoL than the general population, irrespective of any therapy [17]. Considering this fact, patients’ postoperative HRQoL should be in our focus to the same extent as OS. In surgical decision making for patients suffering from a HGG, we must balance the risks and benefits for the patient. Deterioration in HRQoL may negatively influence OS and progression-free survival (PFS) [18], leading to psychological distress and increased requests for supportive care [19].
Generic HRQoL measures like the short-form health survey questionnaire (SF-36) or the EuroQol-5D allow for a comparison between several groups of cancer patients, e.g., the HRQoL of patients with breast cancer vs. patients with prostate cancer. Disease-specific questionnaires (e.g., EORTC QLQ BN20 for brain tumors) have been validated to assess disease-specific symptoms and concerns. Measurement of global HRQoL in disease-specific questionnaires may seem comparable to results obtained with generic measures, but the disease-specific scores provide a better assessment of symptom burden tailored to the respective cancer type [20]. Thus, for our series, we used a disease-specific, well-established questionnaire: the EORTC QLQ-C30/BN20.
In GB, deciding between STR and biopsy can be controversial based on the present literature [2, 21]. Therefore, we evaluated the impact of the EoR on HRQoL. We further focused on intraoperative imaging in an unselected multicenter cohort. To the best of our knowledge, for the first time, we provide data on HRQoL after resection with a combined iMRI and 5-ALA imaging approach and for patients after awake surgery.
Influential variables
In our series, HRQoL was mostly dependent on KPS. Patients with a KPS above or equal to 70 suffered from neurological symptoms significantly less often and maintained good functioning, global health, and QoL compared to patients with a KPS below 70. This is in accordance with prior publications [22].
Both our models did not show significant associations between HRQoL and patient age, as shown previously in a pooled analysis of the EORTC concerning age in cancer patients in general [23].
Previous publications showed no general association of HRQoL and laterality [24]. We observed a significant negative association of eloquent location with global QoL, functioning scores, and neurological symptoms like motor dysfunction, communication deficit, and weakness of the legs.
Impact of the EoR on patients’ QoL
Interestingly, patients in our series receiving biopsy showed worse HRQoL compared to those receiving GTR or STR—adjusted for KPS and age. As well, QoL, role, and cognitive functioning were significantly lower following biopsy, and these patients suffered significantly from more weakness of the legs. By adjusting for age, KPS, and eloquent location in the mixed model, we controlled for the major clinical selection bias between the STR and biopsy groups. Thus, we conclude a most likely clinical relevant association of STR compared to biopsy for several relevant aspects of HRQoL. By further comparing GTR to STR, no crucial disparities were observed. While the impact of a STR vs. a biopsy on survival is viewed controversially by some authors [21], our data on HRQoL support the approach of a maximal safe resection, even if it is subtotal. A STR may reduce pressure and edema-related symptoms compared to a biopsy, potentially leading to a higher HRQoL.
Impact of intraoperative imaging on quality of life
To the best of our knowledge, there is so far only one published study in which the influence of intraoperative imaging on HRQoL was analyzed [25]. No alteration by use of intraoperative ultrasound and neuronavigation was observed in this previous analysis. Consequently, our assessment of the impact of iMRI, 5-ALA, and especially the combination of both methods provides the first prospective multicenter data on this topic. We analyzed the influence of intraoperative imaging only in patients with primarily intended GTR. We confirmed the previously published results, showing that the highest rate of GTR is achieved with a combined imaging approach using iMRI and 5-ALA, followed by iMRI and 5-ALA alone [6, 7, 13]. The impact of the imaging technique used on the EoR was not the focus of the current trial. No final conclusion can be drawn about the impact of 5-ALA alone or in a combined use with iMRI. Previously reported data on the EoR without intraoperative imaging are similar to our series [6], while the GTR rates using 5-ALA vary between 65 and 89% [7, 26]. Previous volumetric data on the combined use of 5-ALA and iMRI (99.7%) show a significant difference in the EoR compared to iMRI (97%) alone [13].
Concerning sum scores, in the mixed-model assessment, there was no significant association of intraoperative imaging on HRQoL. We found a general tendency towards increased total and functioning score and a reduced symptom burden with ‘escalation’ of intraoperative imaging, yet without reaching significant levels. In the brain tumor-specific module, our patients reported significantly fewer visual disorders after application of the combined use of iMRI and 5-ALA compared to the sole use of 5-ALA or no imaging.
Our results show an important new finding: a potentially better, or at least no decrease, PRO after an escalation of intraoperative imaging methods. Additional control might lead to higher safety levels during resection. Especially, given the novel data on the significant positive impact of supramaximal resection on survival in patients harboring a GB, a positive or at least not a negative influence of increased resection is very important for clinical decision making [27]. It must be stated that use of intraoperative neurophysiological monitoring is part of the standard surgical procedure in all centers taking part in this study. From the authors’ point of view, the use of intraoperative monitoring is crucial when using intraoperative imaging, especially in procedures with intended supramaximal resection.
Impact of awake surgery on quality of life
To the best of our knowledge, this is the first prospective analysis evaluating the impact of awake surgery on HRQoL compared to surgery under general anesthesia. Interestingly, we observed neither significant positive nor negative associations in sum scores. Analyzing the functioning and symptom scores, we also could not verify differences, except for seizures, which were reported significantly more often after awake surgery. A selection bias is most likely the reason for this finding, as tumor location usually is more prone to serve as the epileptogenic focus in this subgroup. Posttraumatic stress disorder (PSD) is a controversially discussed topic in earlier publications [11, 12, 28]. Even though we did not assess PSD directly, we can state that our data showed no significant differences in emotional functioning or a decrease in QoL. However, the results are based on a careful selection of patients suitable for awake surgery in each participating center. Due to this selection bias, no general conclusion can be drawn about a potential benefit of awake surgery compared to surgery under general anesthesia for eloquent tumors.
Limitations
Our study has the following limitations due to the applied cross-sectional, observational study design: Analysis of clinical data, e.g., estimation of the EoR, as well as the intended EoR (STR, biopsy, GTR), might be biased by local specialists or methods. Although an assessment protocol was used in all institutions, no central review was performed. Concerning intraoperative imaging methods, randomization was not possible since not all imaging techniques were available in all centers. Due to the cross-sectional design, follow-up varies between patients. Thus, the potential influence of progressive disease or a potential bias of low preoperative QoL scores could not be adjusted for in all patients. Our results are limited by the heterogeneity of the study population based on diagnosis and different adjuvant treatment regimes. Due to the limited samples size, we cannot control for potential confounding variables at the time of assessment, e.g., ongoing chemotherapy, progressive disease, and severe medical conditions. We used an exploratory approach to data assessment. Thus, we did not account for cumulating alpha error.
Patients in very poor condition were primarily excluded based on the study’s selection criteria, so an additional selection bias exists. We did not assess the number of patients who refused to take part in the study or patients that were unable to be followed up further due to progressive disease. Further, patients with primary lower KPS tend to drop out earlier from studies, resulting in a relatively higher mean HRQoL in later states of disease [29]. This bias will also be found in our series. The calculated sum scores per Hinz et al. [15] do not include BN20 scores, which mainly assess neurological symptoms. Thus, greater differences in neurological symptoms as seen in biopsy patients or after no use of intraoperative imaging might not be reflected in the sum scores. Finally, our patient cohort was quite heterogeneous, and the overall number of cases was too small to make final statements about small subgroups, e.g., patients with awake surgeries.
The clinical impact of the HRQoL assessment results must be interpreted keeping in mind the minimal clinically important difference (MID) of the scores. These scores are disease specific and EORTC QLQ C30 subscore specific. In general, for brain tumor patients, a difference of around 10 points is considered as the MID [30, 31]. Thus, in our series, all significant findings reached the MID. Yet, we did not account for potential response shift phenomena. This may lead to an increase or decrease of the MID based on whether a positive or negative effect is found for the patient, leading to a subjective recalibration, reprioritization, and reconceptualization of the patient’s internal standards [32]. As in most contemporary research on HRQoL, we cannot control for this effect based on our study design. Additional tests would be needed [33], which could be an important aspect for future research.
Interpretation and generalizability
Being based on the cross-sectional cohort of HGG patients of four German neurooncological centers, we find our data to be representative for many centers worldwide using contemporary treatment approaches. Due to the previously mentioned limitations, especially response shift phenomena and a general selection bias for patients with a higher KPS, causality should not be deduced. Yet, our results can be interpreted as significant associations important for clinical practice.
We found a significantly positive association of STR compared to biopsy for several relevant factors of HRQoL. Hence, our data support existing literature favoring an STR over a biopsy, if the KPS is equal to or above 70.
Despite there being no significant difference between STR and GTR concerning HRQoL, we found a potential association of better outcome after an escalation of intraoperative imaging methods, with best results for a combined imaging approach using iMRI and 5-ALA. Given potential limitations, at least no decrease of HRQoL or increase of reported neurological deficits was found.
In our series, awake surgery seems to be a well-tolerated, safe method for tumor resection in eloquent areas which did not negatively affect patients’ HRQoL in general or result in specific emotional dysfunctions.
Conclusion
In HGG patients, STR compared to biopsy was significantly associated with better HRQoL and fewer neurological symptoms in this series. An escalated use of intraoperative imaging increased the EoR with stable or slightly better HRQoL and fewer neurological symptoms. Based on HRQoL, awake surgery was a well-tolerated and safe method in our series.
References
DeAngelis LM (2001) Brain tumors. N Engl J Med 344:114–123. doi:10.1056/NEJM200101113440207
Marko NF, Weil RJ, Schroeder JL, Lang FF, Suki D, Sawaya RE (2014) Extent of resection of glioblastoma revisited: personalized survival modeling facilitates more accurate survival prediction and supports a maximum-safe-resection approach to surgery. J Clin Oncol Off J Am Soc Clin Oncol 32:774–782. doi:10.1200/jco.2013.51.8886
Ostrom QT, Bauchet L, Davis FG, Deltour I, Fisher JL, Langer CE, Pekmezci M, Schwartzbaum JA, Turner MC, Walsh KM, Wrensch MR, Barnholtz-Sloan JS (2014) The epidemiology of glioma in adults: a “state of the science” review. Neuro-Oncology 16:896–913. doi:10.1093/neuonc/nou087
Calvert M, Brundage M, Jacobsen PB, Schünemann HJ, Efficace F (2013) The CONSORT patient-reported outcome (PRO) extension: implications for clinical trials and practice. Health Qual Life Outcomes 11:184. doi:10.1186/1477-7525-11-184
Sanders C, Egger M, Donovan J, Tallon D, Frankel S (1998) Reporting on quality of life in randomised controlled trials: bibliographic study. BMJ (Clinical research ed) 317:1191–1194
Senft C, Bink A, Franz K, Vatter H, Gasser T, Seifert V (2011) Intraoperative MRI guidance and extent of resection in glioma surgery: a randomised, controlled trial. The Lancet Oncology 12:997–1003. doi:10.1016/s1470-2045(11)70196-6
Stummer W, Pichlmeier U, Meinel T, Wiestler OD, Zanella F, Reulen H-J (2006) Fluorescence-guided surgery with 5-aminolevulinic acid for resection of malignant glioma: a randomised controlled multicentre phase III trial. The Lancet Oncology 7:392–401. doi:10.1016/s1470-2045(06)70665-9
Stummer W, Tonn J-C, Mehdorn HM, Nestler U, Franz K, Goetz C, Bink A, Pichlmeier U (2011) Counterbalancing risks and gains from extended resections in malignant glioma surgery: a supplemental analysis from the randomized 5-aminolevulinic acid glioma resection study. J Neurosurg 114:613–623. doi:10.3171/2010.3.JNS097
Hoffermann M, Bruckmann L, Mahdy Ali K, Zaar K, Avian A, von Campe G (2017) Pre- and postoperative neurocognitive deficits in brain tumor patients assessed by a computer based screening test. J Clin Neurosci 36:31–36. doi:10.1016/j.jocn.2016.10.030
Wolf J, Campos B, Bruckner T, Vogt L, Unterberg A, Ahmadi R (2016) Evaluation of neuropsychological outcome and “quality of life” after glioma surgery. Langenbeck’s Arch Surg 401:541–549. doi:10.1007/s00423-016-1403-6
Milian M, Luerding R, Ploppa A, Decker K, Psaras T, Tatagiba M, Gharabaghi A, Feigl GC (2013) “Imagine your neighbor mows the lawn”: a pilot study of psychological sequelae due to awake craniotomy: clinical article. J Neurosurg 118:1288–1295. doi:10.3171/2013.2.JNS121254
Milian M, Tatagiba M, Feigl GC (2014) Patient response to awake craniotomy—a summary overview. Acta Neurochir 156:1063–1070. doi:10.1007/s00701-014-2038-4
Coburger J, Hagel V, Wirtz CR, Konig R (2015) Surgery for glioblastoma: impact of the combined use of 5-aminolevulinic acid and intraoperative MRI on extent of resection and survival. PLoS One 10:e0131872. doi:10.1371/journal.pone.0131872
Taphoorn MJ, Claassens L, Aaronson NK, Coens C, Mauer M, Osoba D, Stupp R, Mirimanoff RO, van den Bent MJ, Bottomley A, Group EQoL, and Brain Cancer N, Radiotherapy G (2010) An international validation study of the EORTC brain cancer module (EORTC QLQ-BN20) for assessing health-related quality of life and symptoms in brain cancer patients. Eur J Cancer 46(6):1033–1040
Hinz A, Einenkel J, Briest S, Stolzenburg JU, Papsdorf K, Singer S (2012) Is it useful to calculate sum scores of the quality of life questionnaire EORTC QLQ-C30? European Journal of Cancer Care 21:677–683. doi:10.1111/j.1365-2354.2012.01367.x
Hinz A, Mehnert A, Degi C, Reissmann DR, Schotte D, Schulte T (2015) The relationship between global and specific components of quality of life, assessed with the EORTC QLQ-C30 in a sample of 2019 cancer patients. European Journal of Cancer Care. doi:10.1111/ecc.12416
Schwarz R, Hinz A (2001) Reference data for the quality of life questionnaire EORTC QLQ-C30 in the general German population. European Journal of Cancer (Oxford, England: 1990) 37:1345–1351 doi: S0959804900004470
Mauer M, Stupp R, Taphoorn MJ, Coens C, Osoba D, Marosi C, Wong R, de Witte O, Cairncross JG, Efficace F, Mirimanoff RO, Forsyth P, van den Bent MJ, Weller M, Bottomley A (2007) The prognostic value of health-related quality-of-life data in predicting survival in glioblastoma cancer patients: results from an international randomised phase III EORTC Brain Tumour and Radiation Oncology Groups, and NCIC Clinical Trials Group study. Br J Cancer 97:302–307
Hickmann AK, Hechtner M, Nadji-Ohl M, Janko M, Reuter AK, Kohlmann K, Haug M, Gruninger S, Deininger M, Ganslandt O, Konig J, Wirtz CR, Coburger J, Renovanz M (2016) Evaluating patients for psychosocial distress and supportive care needs based on health-related quality of life in primary brain tumors: a prospective multicenter analysis of patients with gliomas in an outpatient setting. J Neuro-Oncol. doi:10.1007/s11060-016-2280-0
Maratia S, Cedillo S, Rejas J (2016) Assessing health-related quality of life in patients with breast cancer: a systematic and standardized comparison of available instruments using the EMPRO tool. Qual Life Res Int J Qual Life Asp Treat Care Rehab 25:2467–2480. doi:10.1007/s11136-016-1284-8
Kreth FW, Thon N, Simon M, Westphal M, Schackert G, Nikkhah G, Hentschel B, Reifenberger G, Pietsch T, Weller M, Tonn JC, German Glioma N (2013) Gross total but not incomplete resection of glioblastoma prolongs survival in the era of radiochemotherapy. Annals of Oncology: Official Journal of the European Society for Medical Oncology 24:3117–3123. doi:10.1093/annonc/mdt388
Osoba D, Aaronson NK, Muller M, Sneeuw K, Hsu MA, Yung WK, Brada M, Newlands E (1996) The development and psychometric validation of a brain cancer quality-of-life questionnaire for use in combination with general cancer-specific questionnaires. Qual Life Res Int J Qual Life Asp Treat Care Rehab 5:139–150
Quinten C, Coens C, Ghislain I, Zikos E, Sprangers MA, Ringash J, Martinelli F, Ediebah DE, Maringwa J, Reeve BB, Greimel E, King MT, Bjordal K, Flechtner HH, Schmucker-Von Koch J, Taphoorn MJ, Weis J, Wildiers H, Velikova G, Bottomley A, Probe GEC (2015) The effects of age on health-related quality of life in cancer populations: a pooled analysis of randomized controlled trials using the European Organisation for Research and Treatment of Cancer (EORTC) QLQ-C30 involving 6024 cancer patients. European Journal of Cancer (Oxford, England: 1990) 51:2808–2819. doi:10.1016/j.ejca.2015.08.027
Drewes CSL, Jakola AS, Solheim O (2016) Quality of life in patients with intracranial tumors: does tumor laterality matter? J Neurosurg 125:1400–1407. doi:10.3171/2015.12.JNS152252
Jakola AS, Unsgård G, Solheim O (2011) Quality of life in patients with intracranial gliomas: the impact of modern image-guided surgery. J Neurosurg 114:1622–1630. doi:10.3171/2011.1.JNS101657
Schucht P, Beck J, Abu-Isa J, Andereggen L, Murek M, Seidel K, Stieglitz L, Raabe A (2012) Gross total resection rates in contemporary glioblastoma surgery: results of an institutional protocol combining 5-aminolevulinic acid intraoperative fluorescence imaging and brain mapping. Neurosurgery 71:927–936
Li YM, Suki D, Hess K, Sawaya R (2016) The influence of maximum safe resection of glioblastoma on survival in 1229 patients: can we do better than gross-total resection? J Neurosurg 124:977–988. doi:10.3171/2015.5.jns142087
Goebel S, Nabavi A, Schubert S, Mehdorn HM (2010) Patient perception of combined awake brain tumor surgery and intraoperative 1.5-T magnetic resonance imaging: the Kiel experience. Neurosurgery 67:594–600 . doi:10.1227/01.NEU.0000374870.46963.BBdiscussion 600
Singer S, Danker H, Guntinas-Lichius O, Oeken J, Pabst F, Schock J, Vogel HJ, Meister EF, Wulke C, Dietz A (2014) Quality of life before and after total laryngectomy: results of a multicenter prospective cohort study. Head & neck 36:359–368. doi:10.1002/hed.23305
Maringwa J, Quinten C, King M, Ringash J, Osoba D, Coens C, Martinelli F, Reeve BB, Gotay C, Greimel E, Flechtner H, Cleeland CS, Schmucker-Von Koch J, Weis J, Van Den Bent MJ, Stupp R, Taphoorn MJ, Bottomley A (2011) Minimal clinically meaningful differences for the EORTC QLQ-C30 and EORTC QLQ-BN20 scales in brain cancer patients. Annals of Oncology: Official Journal of the European Society for Medical Oncology / ESMO 22:2107–2112. doi:10.1093/annonc/mdq726
Osoba D, Rodrigues G, Myles J, Zee B, Pater J (1998) Interpreting the significance of changes in health-related quality-of-life scores. J Clin Oncol Off J Am Soc Clin Oncol 16:139–144. doi:10.1200/jco.1998.16.1.139
Schwartz CE, Andresen EM, Nosek MA, Krahn GL (2007) Response shift theory: important implications for measuring quality of life in people with disability. Arch Phys Med Rehabil 88:529–536. doi:10.1016/j.apmr.2006.12.032
Ousmen A, Conroy T, Guillemin F, Velten M, Jolly D, Mercier M, Causeret S, Cuisenier J, Graesslin O, Hamidou Z, Bonnetain F, Anota A (2016) Impact of the occurrence of a response shift on the determination of the minimal important difference in a health-related quality of life score over time. Health Qual Life Outcomes 14:167. doi:10.1186/s12955-016-0569-5
Acknowledgements
The authors thank Sonja Grüninger, Monika Deininger, Güler Savas, Christa Topp, Heike Lahr, Doro Maurer, Linda Messing, and Larissa Reitzug for their reliable cooperation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Statement of human rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Nickel, K., Renovanz, M., König, J. et al. The patients’ view: impact of the extent of resection, intraoperative imaging, and awake surgery on health-related quality of life in high-grade glioma patients—results of a multicenter cross-sectional study. Neurosurg Rev 41, 207–219 (2018). https://doi.org/10.1007/s10143-017-0836-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-017-0836-x