Abstract
The success of microvascular decompression (MVD) depends on the permanent and complete transposition of the offending vessels. This paper describes the stitched sling retraction techniques for treating trigeminal neuralgia (TN), hemifacial spasm (HFS), and glossopharyngeal neuralgia (GPN), focusing on the stitching point for slinging the offending artery in the appropriate direction. Between January 2007 and March 2009, 28 patients with TN, 5 patients with HFS, and 3 patients with GPN underwent MVD with a sling retraction technique. In cases of TN, MVD was performed using the infratentorial lateral supracerebellar approach, and the offending superior cerebellar artery was superomedially transposed with a sling stitched to the tentorium cerebelli. In cases of HFS, MVD was performed using the lateral suboccipital infrafloccular approach, and the offending vertebral artery was superolaterally transposed with a sling stitched to the petrous dura. In cases of GPN, MVD was performed using the transcondylar fossa approach, in which the posterior inferior cerebellar artery was inferolaterally mobilized with a sling secured to the jugular tubercle. No patient suffered recurrence in the follow-up period. For the sling retraction technique to be performed successfully, it is important for a stitch to be placed at a suitable site to sling the offending vessel in the intended direction. An appropriate surgical approach must be used to obtain a sufficient operative field for performing the stitching procedures safely.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Trigeminal neuralgia (TN), hemifacial spasm (HFS), and glossopharyngeal neuralgia (GPN) are caused by vascular compression at the root entry or exit zone of the cranial nerves. Microvascular decompression (MVD) performed via the lateral suboccipital approach is now the preferred method for treating these cranial nerve compression syndromes. MVD was introduced in the late 1960s and was largely popularized by Jannetta and colleagues [3, 8, 9, 18]. Since Jannetta’s original description, there have been several developments in the procedures and techniques, particularly in methods of keeping the offending vessel away from the nerve. In recent years, a variety of sling retraction techniques have been reported for securing vascular transposition [2, 5, 17, 19, 20, 24, 29, 30]. We have also utilized the stitched sling retraction technique to secure the transposition of the offending arteries [12]. However, few reports have systematically described the details of the optimal stitching point for effective transposition of the offending artery. In this paper, we introduce and describe surgical procedures and techniques for treating TN, HFS, and GPN with the stitched sling retraction method. We particularly focus on the stitching point for slinging the offending vessel in the appropriate direction and the surgical approach for obtaining a sufficient operative field from an anatomical viewpoint.
Patients and methods
Patient population
Between January 2007 and March 2009, 33 patients with TN, 36 patients with HFS, and 3 patients with GPN underwent MVD at our institution. Among them, the stitched sling retraction technique was employed in 28 patients (85%) with TN, 5 patients (14%) with HFS, and 3 patients (100%) with GPN.
Surgical procedures and stitching methods
We have adopted three different MVD approaches to treat the three main cranial nerve compression syndromes: (1) the infratentorial lateral supracerebellar approach for TN, (2) the lateral suboccipital infrafloccular approach for HFS, and (3) the transcondylar fossa approach for GPN. The details of these three approaches have been described in previous publications [7, 13, 14].
Trigeminal neuralgia
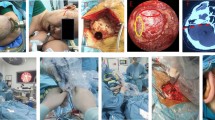
In cases of TN, the stitched sling retraction technique was employed to mobilize the superior cerebellar artery (SCA) and/or the anterior inferior cerebellar artery (AICA). We found that the SCA coursed medial to the trigeminal nerve and compressed the nerve from the superomedial side (Fig. 1a). To treat the condition, therefore, the SCA was transposed in a superomedial direction to free the compressed trigeminal nerve. Meticulous arachnoid dissection was performed to fully mobilize the SCA. We stitched 5–0 thread to the tentorium cerebelli to transpose the SCA superomedially, then passed it around the SCA, and knotted it to make a sling, ensuring that the vessel was not kinked (Fig. 1b). We placed the stitch at the center of the tentorium and used a long sling to transpose the SCA because the tentorial arteries and sinuses are located near the tentorial edge and in the dorsomedial part of the tentorium (Fig. 2). This helps to avoid hemorrhage from the tentorium and to perform the procedure in a shallow operative field. In the cases of compression of the AICA, the artery was transposed in the caudolateral direction because the AICA coursed caudal to the trigeminal nerve and compressed the nerve from the caudolateral side (Fig. 1a). We placed a stitch to the petrous dura (Fig. 3) to transpose the AICA inferolaterally (Fig. 1b). The petrous dura on the suprameatal tubercle is occasionally so thin that care should be taken not to tear the dura mater. Figure 4 demonstrates the intraoperative photographs of MVD for right TN.
Schematic drawings of MVD for TN caused by the SCA and AICA. a The SCA compresses the trigeminal nerve from the superomedial side, and the AICA compresses the nerve from the caudal side. b The SCA is transposed superomedially with a sling stitched to the tentorium cerebelli. The AICA is transposed caudolaterally with a sling secured to the petrous dura. SPV superior petrosal vein
Hemifacial spasm
In cases of HFS, we used the sling retraction technique to mobilize the offending vertebral artery (VA). The VA compressed the nerve from the ventral side. We made a stitch to the petrous dura near the jugular foramen (Fig. 3) and transposed the VA superolaterally away from the root exit zone of the facial nerve. Following this procedure, if necessary the ordinary prosthesis insertion with Teflon felt was added to dislocate the PICA or AICA. To inspect the root exit zone, the direction of view of the microscope should be turned to the brainstem side (Fig. 5a). To facilitate surgical access, it is important to expose sufficiently the inferolateral limit of the surgical field. On the other hand, to make a stitch to the petrous dura, the axis of view of the microscope should be turned to the petrous bone side (Fig. 5b). Therefore, the medial border of the surgical field should be enlarged. Figure 6 demonstrates the intraoperative photographs of MVD for left HFS.
Schematic drawings of MVD for HFS, caused by the PICA concomitantly with the VA. a The root exit zone (REZ) of the facial nerve is compressed by the PICA originating from the ectatic VA. b The VA is transposed superolaterally by a sling anchored to the petrous dura near the jugular foramen. Following this procedure, the ordinary prosthesis insertion with Teflon felt is added to dislocate the PICA. Ch Pl choroid plexus
Glossopharyngeal neuralgia
In cases of GPN, a loop of the PICA protruded into the supraolivary fossette and compressed the glossopharyngeal and vagal nerves from the caudal side (Fig. 7a). Therefore, the offending PICA was transposed caudally to free the compressed nerve. We made a stitch to the dura mater on the jugular tubercle (Fig. 3) and transposed the offending PICA inferolaterally (Fig. 7b). Figure 8 demonstrates the intraoperative photographs of MVD for left GPN.
Schematic drawings of MVD for GPN caused by the PICA. a The loop of PICA compresses the root of the glossopharyngeal nerve in the supraolivary fossette. b The loop of PICA is pulled out from the supraolivary fossette and repositioned inferolaterally by a sling stitched to the dura mater on the jugular tubercle
Results
The demographics of the patients are summarized in Table 1.
Trigeminal neuralgia
Among the 28 patients with TN treated using the stitched sling retraction technique, the SCA was involved in 23 patients, the AICA in 1 patient, and the SCA and AICA were both involved in 4 patients. In 5 of the 33 patients undergoing MVD, the sling retraction technique was not employed: four patients exhibited no arterial compression and one patient had short perforators from the SCA to the brainstem. An excellent outcome (complete pain relief without medication) was obtained in 24 of 28 (86%) patients, and a good outcome (no or mild pain controlled with low-dose medication) was observed in the remaining four patients (14%). No recurrence was observed during postoperative follow-up periods of between 8 and 30 months. Complications were observed in four patients: One patient developed transient cerebellar ataxia due to venous infarction, and three patients showed cerebrospinal fluid leakage.
Hemifacial spasm
Among the five HFS patients treated with the stitched sling retraction technique, the VA alone was involved in one patient, the VA and AICA together in two patients, and the VA and PICA were involved together in two patients. All patients showed a complete resolution of their spasm and experienced no complications. Although the longest follow-up period was only 24 months, no patient suffered recurrence.
Glossopharyngeal neuralgia
In all three cases of GPN, the PICA alone was implicated. All patients recovered immediately after surgery. One patient suffered mild hoarseness. No recurrences were observed and each patient experienced complete relief during the 12, 18, and 29 months, respectively.
Discussion
Trigeminal neuralgia
Jannetta described an interposition technique that involved the insertion of a Teflon felt to keep the offending vessel off the nerve [1, 18]. However, long-term follow-up studies revealed that the efficacy of MVD for TN gradually decreased over time because of recurrence. The incidence of recurrence of TN has been reported to vary from between 3% and 30% [17]. The pathogenesis of recurrence in cases treated using the interposition method includes adhesions between the prosthesis–nerve complex [4] and inflammatory responses such as granuloma [23]. Thus, an ideal method should maintain a permanent separation between the nerve and the offending vessel, without any contact with the nerve itself [25, 30]. The transposition method may be more suitable than the interposition method for achieving this goal. Some authors have reported the use of a transposition method using adhesive glue [25]. Though an adhesive glue transposition technique is relatively easy to perform, the use of glue involves several problems, including adhesive strength, viral and prion disease transmission, and adhesion to the trigeminal nerve, which is considered to cause recurrence [21]. The technique of vascular transposition using a sling retraction was originally developed by Fukushima [5], and a variety of sling retraction techniques involving offending arteries have subsequently been reported using aneurysm clips [2], Gore-tex tape [29], or fascia strips [20]. To accomplish the sling retraction method successfully, an appropriate surgical approach must be used to obtain a sufficient operative field for placing a stitch at a suitable site and performing the stitching procedures safely.
We have utilized the infratentorial lateral supracerebellar approach for MVD in the treatment of TN [13]. The SCA, which is the most frequent offending vessel involved in TN, courses above the trigeminal nerve making a downward loop and compresses the nerve from the superior, superomedial or medial side [6, 13, 31]. Therefore, it is reasonable to transpose the SCA superomedially with a sling stitched to the tentorium cerebelli. This procedure can be facilitated using the infratentorial lateral supracerebellar approach. Moreover, the stitching procedure is both relatively easy and safe because the working space on the tentorial cerebellar surface obtained through this approach is sufficiently wide and is far from the seventh and eighth cranial nerves and the superior petrosal vein. Though some authors placed a stitch at the lateral part of the tentorium and repositioned the SCA superiorly [19, 20], unexpected bleeding can occur because tentorial sinuses are located in this area [16].
Hemifacial spasm
In cases of HFS, we employed a sling retraction technique to mobilize the VA. For dislocation of the AICA or PICA, however, we used the interposition method with Teflon felt because of difficulties in transposing these vessels due to the presence of short perforators in most cases. Compared with TN, the recurrence rate for HFS following the interposition method with Teflon felt is low, ranging from 1% to 10% [22, 26]. The main cause of recurrence of HFS is not attributed to adhesion. Rather, inadequate cushion effect of offending vessels is thought to be a frequent causative factor in HFS recurrence [26, 32]. The interposition method is sometimes insufficient to buffer a large pulsatile force caused by the VA; thus, we prefer the stitched sling retraction method for mobilizing the VA. We have also found Teflon sponges between the VA and brainstem useful to avoid excessive stress on the arterial wall. To obtain an adequate working space, a wide opening of the cerebellopontine fissure is essential. This can be facilitated using the lateral suboccipital infrafloccular approach.
Glossopharyngeal neuralgia
In cases of GPN, we have applied the transcondylar fossa approach [10, 14], in which the posterior part of the jugular tubercle is extradurally removed without injuring the atlanto-occipital joint [15]. This approach provides sufficient visualization of the entire course of the cisternal portion of the ninth and tenth cranial nerves with a slight retraction of the cerebellum and clearly shows its relationships with nearby arteries such as the PICA or VA. There have been only a few reports on the use of the sling retraction technique for the treatment of GPN. Sampson et al. repositioned the offending artery superolaterally with a Teflon sling that was attached to the petrous dura between the internal auditory meatus and jugular foramen [27]. We consider that inferior displacement of the vessel is more reasonable because the vessel usually arises from below and ventral to the nerves. The transcondylar fossa approach provides wide exposure of dura mater on the jugular tubercle; therefore, it is not difficult to reposition the offending artery in a caudal direction with this approach. Thus, the stitched sling retraction method through this approach seems to be the most suitable for MVD for GPN.
As a limitation, the sample size is not large enough for strong conclusion. The majority of previous reports insisting efficacy of the sling retraction method include a small number of patients, and data regarding the long-term outcome comparing the interposition method versus the sling retraction method are very limited [30]. Our method cannot apply to some cases in which short perforators originate from the offending artery, and the stitching points may not be generalized to every case due to individual variations. Nonetheless, it is clinically useful to understand the principle of the optimal stitching point because the anatomical relationships between the cranial nerves and the cerebellar arteries are similar in the majority of the cases. Recently, three-dimensional computer graphics with image fusion have been applied to preoperative simulation of MVD [11, 28]. With improvements in the software and the quality of the source images, this may become a powerful tool in the planning of the stitching points.
In summary, the stitched sling retraction method can be a safe and effective treatment for cranial nerve compression syndromes. It is vital to select the most suitable surgical approach and stitching point based on the surgical anatomy. Further evaluation in large series of patients with longer follow-up period is needed to assess the efficacy and safety of this method.
References
Ammar A, Lagenaur C, Jannetta P (1990) Neural tissue compatibility of Teflon as implant material for microvascular decompression. Neurosurg Rev 13:299–303
Attabib N, Kaufmann A (2007) Use of fenestrated aneurysm clips in microvascular decompression surgery. J Neurosurg 106:929–931
Barker FG 2nd, Jannetta PJ, Bissonette DJ, Larkins MV, Jho HD (1996) The long-term outcome of microvascular decompression for trigeminal neuralgia. N Engl J Med 334:1077–1083
Fujimaki T, Hoya K, Sasaki T, Kirino T (1996) Recurrent trigeminal neuralgia caused by an inserted prosthesis: report of two cases. Acta Neurochir (Wein) 138:1307–1310
Fukushima T (1982) Posterior cranial fossa microvascular decompression (Jannetta method) for trigeminal neuralgia and facial spasm (in Japanese). No Shinkei Geka 10:1257–1261
Hardy DG, Rhoton AL Jr (1978) Microsurgical relationships of the superior cerebellar artery and the trigeminal nerve. J Neurosurg 49:669–678
Hitotsumatsu T, Matsushima T, Inoue T (2003) Microvascular decompression for treatment of trigeminal neuralgia, hemifacial spasm and glossopharyngeal neuralgia: three surgical approach variations. Neurosurgery 53:1436–1443
Jannetta PJ (1967) Arterial compression of the trigeminal nerve at the pons in patients with trigeminal neuralgia. J Neurosurg 26(Suppl 1):159–162
Jannetta PJ (1977) Observations on the etiology of trigeminal neuralgia, hemifacial spasm, acoustic nerve dysfunction and glossopharyngeal neuralgia: definitive microsurgical treatment and results in 117 patients. Neurochirurgia (Stuttg) 20:145–154
Kawashima M, Matsushima T, Inoue T, Mineta T, Masuoka J, Hirakawa N (2010) Microvascular decompression for glossopharyngeal neuralgia through the transcondylar fossa (supracondylar trans-jugular tubercle) approach. Neurosurgery 66(6 Suppl Operative):275–280
Kin T, Oyama H, Kamada K, Aoki S, Ohtomo K, Saito N (2009) Prediction of surgical view of neurovascular decompression using interactive computer graphics. Neurosurgery 65:121–128
Matsushima T (2006) Microsurgical anatomy and surgery of the posterior fossa (in Japanese). SciMed, Tokyo
Matsushima T, Fukui M, Suzuki S, Rhoton AL Jr (1989) The microsurgical anatomy of the infratentorial lateral supracerebellar approach to the trigeminal nerve for tic douloureux. Neurosurgery 24:890–895
Matsushima T, Goto Y, Natori Y, Matsukado K, Fukui M (2000) Surgical treatment of glossopharyngeal neuralgia as vascular compression syndrome via transcondylar fossa (supracondylar transjugular tubercle) approach. Acta Neurochir 142:1359–1363
Matsushima T, Natori Y, Katsuta T, Ikezaki K, Fukui M, Rhoton AL Jr (1998) Microsurgical anatomy for lateral approaches to the foramen magnum with special reference to transcondylar fossa (supracondylar transjugular tubercle) approach. Skull Base Surg 8:119–125
Matsushima T, Suzuki SO, Fukui M, Rhoton AL Jr, de Oliveira E, Ono M (1989) Microsurgical anatomy of the tentorial sinuses. J Neurosurg 71:923–928
Matsushima T, Yamaguchi T, Inoue TK, Matsukado K, Fukui M (2000) Recurrent trigeminal neuralgia after microvascular decompression using an interposing technique: Teflon felt adhesion and the sling retraction technique. Acta Neurochir (Wien) 142:557–561
McLaughlin MR, Jannetta PJ, Clyde BL, Subach BR, Comey CH, Resnick DK (1999) Microvascular decompression of cranial nerves: lessons learned after 4400 operations. J Neurosurg 90:1–8
Melvill RL, Baxter BL (1996) A tentorial sling in microvascular decompression for trigeminal neuralgia. Technical note. J Neurosurg 84:127–128
Mitsos AP, Georgakoulias N, Lafazanos SA, Konstantinou EA (2008) The “hanging technique” of vascular transposition in microvascular decompression for trigeminal neuralgia: technical report of four cases. Neurosurg Rev 31:327–330
Ohta M, Komatsu F, Abe H, Sakamoto S, Tsugu H, Oshiro S, Fukushima T (2008) Complication caused by use of fibrin glue in vessel transposition for trigeminal neuralgia. Case report. Neurol Med Chir (Tokyo) 48:30–32
Payner TD, Tew JM Jr (1996) Recurrence of hemifacial spasm after microvascular decompression. Neurosurgery 38:686–690
Premsagar IC, Moss T, Coakham HB (1997) Teflon-induced granuloma following treatment of trigeminal neuralgia by microvascular decompression. J Neurosurg 87:454–457
Rawlinson JN, Coakham HB (1988) The treatment of hemifacial spasm by sling retraction. Br J Neurosurg 2:173–178
Ryu H, Yamamoto S (2000) A simple technique for neurovascular decompression for the cranial nerves. Br J Neurosurg 14:132–134
Samii M, Gunther T, Iaconetta G, Muehling M, Vorkapic P, Samii A (2002) Microvascular decompression to treat hemifacial spasm: long-term results for a consecutive series of 143 patients. Neurosurgery 50:712–719
Sampson JH, Grossi PM, Asaoka K, Fukushima T (2004) Microvascular decompression for glossopharyngeal neuralgia: long-term effectiveness and complication avoidance. Neurosurgery 54:884–889
Satoh T, Onoda K, Date I (2007) Preoperative simulation for microvascular decompression in patients with idiopathic trigeminal neuralgia: visualization with three-dimensional magnetic resonance cisternogram and angiogram fusion imaging. Neurosurgery 60:104–113
Shigeno T, Kumai J, Endo M, Oya S, Hotta S (2002) Snare technique of vascular transposition for microvascular decompression. Technical note. Neurol Med Chir (Tokyo) 42:184–190
Sindou M, Leston JM, Decullier E, Chapuis F (2008) Microvascular decompression for trigeminal neuralgia: the importance of a noncompressive technique—Kaplan–Meier analysis in a consecutive series of 330 patients. Neurosurgery 63(ONS Suppl 2):341–351
Ueda F, Suzuki M, Fujinaga Y, Kadoya M, Takashima T (1999) In vivo anatomical analysis of arterial contact with trigeminal nerve: detection with three-dimensional spoiled grass imaging. Br J Radiol 72:838–845
Yamaki T, Hashi K, Niwa J, Tanabe S, Nakagawa T, Nakamura T, Ueda T, Tsuruno T (1992) Results of reoperation for failed microvascular decompression. Acta Neurochir (Wien) 115:1–7
Author information
Authors and Affiliations
Corresponding author
Additional information
Comments
Alessandro Ducati, Turin, Italy
In this useful paper about microvascular decompression, the authors describe in detail the technique to transpose the offending vessel by means of a sling retraction stitched to the dura. They put the attention both to the most effective direction to retract the vessel and to the safest location in the dura to place a stitch, avoiding venous lakes that may cause dangerous bleedings. The case presentation is very effective; the figures are clear and illustrative; the discussion of the literature is complete. I found this work useful for experienced surgeons, to reevaluate the technique of microvascular decompression, using the transposition of the vessel instead of the interposition of foreign material between the nerve and the vessel, and useful for beginners as well because the anatomical detail of this presentation is so accurate that “drive the hand” of surgeons step by step.
Ludwig Benes, Marburg, Germany
This is a well-presented paper on a transposition technique for microvascular decompression in patients suffering trigeminal neuralgia, hemifacial spasm, and glossopharyngeal neuralgia by an experienced writing group.
Although a variety of sling retraction techniques for securing vascular transposition have been previously published, this paper is focusing on the anatomical details especially on the preferred stitching point for effective vessel transposition.
To achieve a sufficient vessel transposition, the operative field has to be prepared by a tailored approach to offer all possibilities to the surgeon performing this technique.
I share the author’s opinion that the transposition method is more suitable in comparison with interposition techniques, e.g., with “Teflon” as long as the perforators are long enough for an adequate vessel management.
Meticulous care should be taken to prevent vessel kicking when utilizing the described sling retraction technique.
Volker Tronnier, Lübeck, Germany
Trigeminal neuralgia and other neurovascular compression syndromes as hemifacial spasm, glossopharyngeal neuralgia, and others still are puzzling with regard to their pathophysiology. Although a neurovascular conflict is considered to be the cause for these attack-like syndromes, several aspects as the intermittent clinical course, the usually excellent relief by sodium channel blockers, the instantaneous relief after microvascular decompression as well as the relief by lesioning or irradiating the nerve are not well understood. Meanwhile, the question is solved that microvascular decompression does not produce pain relief purely by surgical trauma or manipulation of the nerve. Careful neurological examination with quantitative sensory testing has revealed that patients with hypoesthesia due to trauma do not benefit to a higher extent regarding pain-free intervals than patients without any postoperative sensory deficit. Not yet solved is the question whether pure removal of a vessel wall from the nerve will give some benefit due to removal of nerve cell membrane depolarizing or exciting mediators or whether a pure mechanical pressure plays the most important role. However, it is well-known in cases of recurrent pain that scar tissue or granulomas by the interposition material can also cause typical tic-like symptoms.
Several neurosurgeons were looking for alternatives to the technique of interpositioning some material between nerve and vessel as originally favored by Jannetta and were looking to separate the vessel from the nerve without causing any trauma and fixing the vessel to the dura [1–3]. This technique soon became popular by other neurosurgeons as well [4–6].
It is well-known to neurosurgeons that the so-called sling retraction technique can be challenging depending on the anatomical site, the size of the cistern and the vascular variability, and finally the characteristics of the involved vessel. Especially in cases with large vertebral or basilar, partially calcified, vessels, it can be even difficult to hold these vessels with a microdissector away, so everybody will be happy if some material could be placed between the offending vessel and the compromised neural structures. On the other hand, the actual paper by Masuoka et al. [7] gives invaluable surgical hints and details how to dislocate and stitch the vessels to the surrounding dura in “normal” anatomical cases. They nicely detail in a small series the stitching points in the tentorium for separating the SCA from the trigeminal nerve sparing the sinuses, separating the AICA in a caudolateral direction, when the compression of the trigeminal nerve comes from underneath and how to separate the AICA from the seventh nerve as well as the PICA from the glossopharyngeal nerve. Their technique is underlined by intraoperative photographs and anatomical sketches. One has, however, to keep in mind the enormous anatomical variability in these areas. Sometimes the AICA cannot be displaced without harming the labyrinthine artery or the PICA cannot be displaced because of kinking perforators. The use of stitches is preferable to glue which can cause compression or adhesion to adjacent structures and cause recurrent compression.
In summary, this paper is very instructive to think of theses neurovascular conflicts and their treatment in a systematic anatomical way which might be very helpful for surgeons not dealing regularly with these syndromes. The authors are to be congratulated for their highly didactic publication.
References
1. Fukushima T (1986) Surgery for hemifacial spasm (in Japanese). Clin Neurosci 4:584–585
2. Rawlinson JN, Coakham JB (1988) The treatment of hemifacial spasm by sling retraction. Br J Neurosurg 2:173–178
3. Sindou M, Amrani F, Mertens P (1990) Microsurgical vascular decompression in trigeminal neuralgia. Comparison of 2 technical modalities and physiopathologic deductions. A study of 120 cases (in French). Neurochirurgie 36:16–25
4. Melvill RL, Baxter BL (1996) A tentorial sling in microvascular decompression for trigeminal neuralgia. J Neurosurg 84:127–128
5. Suzuki S, Tsuchita T, Kurokawa Y et al (1990) New method of MVD using a vascular tape for neurovascular compression involving the vertebrobasilar artery. Neurol Med Chir 30:1020–1023
6. Matsushima T, Yamaguchi T, Inoue K et al (2000) Recurrent trigeminal neuralgia after microvascular decompression using an interposing technique. Teflon felt and the sling retraction technique. Acta Neurochir 142:557–561
7. Masuoka J, Matsushima T, Kawashima M (2011) Stitched sting retraction technique for microvascular decompression. Procedures and techniques based on an anatomical viewpoint. Neurosurg Rev doi:10.1007/s10143-011-0310-0
Rights and permissions
About this article
Cite this article
Masuoka, J., Matsushima, T., Kawashima, M. et al. Stitched sling retraction technique for microvascular decompression: procedures and techniques based on an anatomical viewpoint. Neurosurg Rev 34, 373–380 (2011). https://doi.org/10.1007/s10143-011-0310-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-011-0310-0