Abstract
This review has been compiled to assess publications related to the clinical application of direct cerebral tissue oxygenation (PtiO2) monitoring published in international, peer-reviewed scientific journals. Its goal was to extract relevant, i.e. positive and negative information on indications, clinical application, safety issues and impact on clinical situations as well as treatment strategies in neurosurgery, neurosurgical anaesthesiology, neurosurgical intensive care, neurology and related specialties. For completeness’ sake it also presents some related basic science research. PtiO2 monitoring technology is a safe and valuable cerebral monitoring device in neurocritical care. Although a randomized outcome study is not available its clinical utility has repeatedly been clearly confirmed because it adds a monitoring parameter, independent from established cerebral monitoring devices. It offers new insights into cerebral physiology and pathophysiology. Pathologic values have been established in peer-reviewed research, which are not only relevant to outcome but are treatable. The benefits clearly outweigh the risks, which remains unchallenged in all publications retrieved. It is particularly attractive because it offers continuous, real-time data and is available at the bedside.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Methods
This review is based on a systematic “MEDLINE” literature search using the following search terms: “licox”, “neurotrend”, “brain tissue oxygenation”, “cerebral oxygenation” and “cerebral partial pressure of oxygen”. Only a few publications were not retrieved using this technique. They were, however, identified through personal communication with scientists in the field and meeting proceedings. This strategy provided sufficient certainty that relevant papers have not been missed. We excluded published or unpublished meeting abstracts or proceedings for this review. To address relevant matters, related to specific PtiO2 issues, we have included a few papers published in supplements only when no other peer-reviewed information was available.
Results
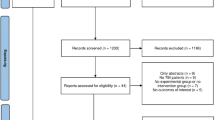
The MEDLINE search provided over 1,400 matches, which were sorted and then scanned. For this review we restricted the literature search to peer-reviewed publications from 2004, 2005 and up to May 2006. Only relevant publications and a few non-peer-reviewed publications published in supplements prior to 2004, which explicitly addressed or systematically examined the above issues, are included in this review and are listed in the reference section.
Indications and applications
Human
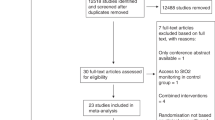
PtiO2 monitoring technology is largely used in neurosurgical and neurologic intensive care. The majority of publications are based on analysis of data from patients suffering from severe traumatic brain injury (TBI), which indicates that this condition represents the largest field of clinical application [11, 13, 16, 32, 44, 47, 50, 59, 66, 68, 74]. It is also used in patients with multiple extracranial injuries and TBI [20]. The second largest group of publications comprises aneurysmal subarachnoid haemorrhage (SAH) [9, 18, 29, 31, 36, 60, 64–66, 68] (Fig. 1). PtiO2 monitoring is also used intraoperatively during aneurysm surgery [33] and surgery of cerebral arteriovenous malformations [26] as well as during cerebral angiography [9]. A monitoring course of brain tissue oxygenation during cardiopulmonary resuscitation has been published on a case report basis [27].
This figure shows a patient suffering from aneurysmal subarachnoid haemorrhage. The small PtiO2 catheter is visible in the right-sided cerebral white matter, contralateral to the larger external ventricular drain. This scan was obtained after decreasing PtiO2 values with normal ICP values noted. Shortly thereafter the patient suffered a large right-sided cerebral infarct. Early signs of right-sided ischaemia can be appreciated
Animal
Direct brain tissue oxygenation (PtiO2) monitoring has also been used in animal models of spontaneous intracerebral haemorrhage [23] and malignant soft tissue tumours [4, 49]. In addition it is used to measure oxygen delivery to brain parenchyma in animal models [7, 10, 48]. It is also used in animal models to study cerebral oxygenation during postasphyxial seizures [19] and transfusion protocols [21].
Clinical applications
The majority of publications come from Germany, Italy, Spain, The Netherlands, the UK and the USA [1, 2, 4–6, 12, 13, 16, 18, 22, 23, 25–27, 31, 38, 44, 49, 54, 55, 58–60, 62, 66, 68, 70, 71, 74]. There is one publication each from Australia [46], China [32], Singapore [47] and Switzerland [50].
PtiO2 monitoring is almost exclusively used in combination with other cerebral non-invasive and invasive monitoring modalities, in particular intracranial pressure (ICP) monitoring [22, 29, 51, 65, 66], cerebral perfusion pressure monitoring [35, 38, 46, 47], jugular venous saturation (JvDO2) monitoring [70], cerebral microdialysis [8, 11, 36, 56, 57, 61], cerebral blood flow velocity measured by transcranial Doppler ultrasound (TCD) [38, 74], regional cerebral blood flow measurements (rCBF) [31], near infrared spectroscopy (NIRS) [6] and intracranial temperature measurements [32].
Oxygen monitoring technologies
Two monitoring devices are currently available, “Licox” and “Neurotrend” technology. Licox is manufactured by GMS-Integra (Kiel-Mielkendorf, Germany). Neurotrend is manufactured by Codman (Raynham, MA, USA).
The Neurotrend probe uses optical sensors. Measurements are obtained through a dye which is connected to a fiberoptic cable. The properties of the dye change along with gas concentrations and pH of adjacent tissues, which in turn reflects tissue partial pressure of oxygen. The Neurotrend probe contains four sensors; it measures PtiO2, PtiCO2, tissue pH and tissue temperature. Its sampling area is around 2 mm2.
The Licox probe uses a polarographic cell in which oxygen diffuses from the tissue through the catheter polyethylene wall into its inner electrolyte chamber. Oxygen is transformed at the electrode where it determines an electrical current. The electrical current reflects tissue PtiO2. Its sampling area is around 14 mm2, seven times the size of the Neurotrend probe.
The Neurotrend probe yields lower values compared to the Licox probe. This is a difference due to the probe’s monitoring techniques, which users must be aware of. It does not indicate measurement validity. Comparative studies are presented further on in the paper.
Catheter placement and sampling size
Catheters are generally placed in the right frontal lobe white matter in diffuse brain injury, or on the affected side in a hemispheric injury, and by and at large remain in situ for as long as ICP measurements are required [43, 73]. Although it is a local measurement, restricted to a small cerebral volume, its utility for reflecting hemispheric conditions has been demonstrated in studies where PtiO2 measurements were correlated with cerebral arteriovenous oxygen difference (AVDO2) and cerebral blood flow (CBF) measurements. Not only did they show a strong correlation but they also showed that PtiO2 measurements did pick up more ischaemic events than the global measurement [37, 52, 53].
The metabolic heterogeneity of different tissue types is well known because it affects sampling size considerations. It is important to factor in the heterogeneous nature of the brain when interpreting oximetry data. Early experiments on rats have demonstrated the differing PtiO2 within the cortex depending on the depth of probe placement [3]. It was proposed that the differing base levels relate to the metabolism, microcirculation and overall microstructure of each environment. Furthermore, depending on the probe’s relationship to the arterial microvessels, a gradient within the tissues can exist with oxygen levels decreasing over the space from arterial to venous circulation. The microenvironment is influenced by the cerebral blood flow velocity of each microenvironment, with low velocities showing the highest variability in terms of oxygenation differences [40].
This translates into a situation where spatial heterogeneity must be compensated for by a sufficiently large sensor sampling area to minimize the so-called random position error. This random position error will yield PtiO2 levels anywhere from 15 to 40 mmHg if the O2-sensitive area is limited to 1.4 mm in length. If the area is increased to 5.0 mm, the range is reduced to values between 25 and 30.
Impact on clinical situations and treatment strategies
There are numerous and most interesting findings which have been derived from about 10 years of research using PtiO2 technology. The following paragraphs summarize the important ones:
Normal PtiO2 values based on Licox technology are around 25–30 mmHg, based on animal research [41]. This was confirmed in patients with normal ICP and CPP [15, 37].
A study published in 1998 using Licox technology demonstrated that the likelihood of death increased with increasing duration of time at or below a PbtO2 of 15 mmHg (2.0 kPa) or with the occurrence of any PbtO2 values of < or = 6 mmHg (< or = 0.8 kPa) [72]. This study shows that PtiO2 technology has prognostic value in the treatment of patients with severe traumatic brain injury. This study has also helped to establish a generally accepted treatment threshold, which has been confirmed in other papers [9, 46].
Of interest is another paper, which has reported that “the presence of anaerobic cerebral metabolism probably depends on duration and severity of the hypoxic episode” [56]. This conclusion is relevant for clinical practice because it shows that (a) PtiO2 technology detects short episodes of cerebral hypoxia which are not picked up by other monitoring modalities and (b) magnitude and duration of cerebral hypoxia have prognostic relevance. One study also reports on the positive correlation and prognostic value of PtiO2 measurements and long-term neuropsychological outcome after severe traumatic brain injury [45].
A most recent study is of particular noteworthiness [67]. In a series of 53 TBI patients, 25 patients were treated using an ICP monitor alone while 28 patients had PtiO2-directed care, with comparable ICP and CPP levels for each group. The mortality rate was 44% for the first group and 25% for the second group, which was statistically significant. Although they were not exactly matched for age, 44 ± 14 years for the ICP/CPP group vs 38 ± 18 years for the PtiO2 group, the outcome difference was significant (p < 0.05). They conclude that “the use of both ICP and brain tissue PO2 monitors and therapy directed at brain tissue PO2 is associated with reduced patient death following severe TBI [67].
In 1996 and 2004 studies have addressed a long and much debated issue in neurocritical care: the role of hyperventilation for controlling intracranial hypertension. Hyperventilation constricts cerebral blood vessels, which in turn can cause hypoperfusion and ischaemia and lead to exacerbation of brain swelling. PtiO2 technology has the potential to guide the degree of hyperventilation because of its ability to indicate states of hypoperfusion and impending ischaemia [5, 12, 15]. This utility has also been demonstrated intraoperatively: “PtiO2 monitoring has a high reliability in the detection of intraoperative tissue hypoxia” [26]. Similar recommendations have previously been reported [62]. One paper, however, reports that in 3 of 17 TBI patients they noted an increase of PtiO2 on hyperventilation, which they called a “paradox reaction” [14]. This pattern was only seen in the early phase between days 0 and 3 after injury. It may represent flow-metabolic uncoupling, and it stresses the utility of multimodality monitoring for which other parameters are used as well.
PtiO2 technology has been used to address another much and long debated issue in neurocritical care: the role of head elevation. A study in 2004 using PtiO2 measurements has demonstrated that “routine nursing of patients with severe head injury at 30 degrees of head elevation within 24 hours after trauma leads to a consistent reduction of ICP (statistically significant) and an improvement in CPP (although not statistically significant) without concomitant deleterious changes in cerebral oxygenation” [47].
Two studies have recently addressed the utility of PtiO2 technology for timing of decompressive hemicraniectomy (DCH) in severe brain swelling [51, 68]. It has been shown that not only absolute PtiO2 values should be considered for the indication of DCH but also magnitude and the time course of monitoring trends [68]. Another study has concluded that “...ptiO(2) monitoring could be an important tool for timing craniectomy in the future” [51]. The effects of DCH, which represents a very invasive treatment option and which is considered an ultimate surgical treatment option, has also been studied: “DCH in the treatment of severe brain injury is associated with a significant improvement in brain oxygenation” [66]. In another, however small, series of patients it was pointed out that despite a rapid PtiO2 increase and ICP reduction from critical to normal values “the patients’ clinical status remained poor with two in a persistent vegetative state and one dead” [29]. This is in keeping with the long-standing and unresolved debate about the utility of DCH and its particular regard to outcome.
Two papers have addressed other long and much debated issues in neurocritical care: the effects of commonly used drugs in neurocritical care: nimodipine and mannitol. A paper published in 2005 has reported that “...although nimodipine use is associated with improved outcome following SAH, in some patients it can temporarily reduce brain tissue PO2” [65]. This report will again spark the academic discussion about whether nimodipine should be used in patients suffering from aneurysmal subarachnoid haemorrhage. The most valuable conclusion for daily neurocritical care practice which can be extracted from this study is that using PtiO2 technology will identify those patients in whom nimodipine has a negative effect [22]. With regard to mannitol it has been shown that although mannitol reduces ICP it has little effect on PtiO2. This is rather unexpected because it is expected that ICP reduction will improve PtiO2. The important clinical conclusion from this finding is that PtiO2 technology should be used in addition to ICP monitoring as the two monitoring parameters are not ultimately linked.
Vasopressors are commonly used in neurocritical care. There is currently debate whether dopamine or noradrenaline should be preferred. PtiO2 monitoring has been used to study the effects of both drugs in comparative studies. The authors report that “... CPP augmentation with norepinephrine, but not with dopamine, resulted in a significant reduction in arterial-venous oxygen difference (37 ± 11 vs 33 ± 12 ml/l) and a significant increase in brain tissue oxygen (2.6 ± 1.1 vs 3.0 ± 1.1 kPa). The CPP intervention did not significantly affect intracranial pressure. There were no significant differences between norepinephrine and dopamine on cerebral oxygenation or metabolism either at baseline or following a CPP intervention; however, the response to a CPP intervention with dopamine seemed to be more variable than the response achieved with norepinephrine” [35].
The effects of another commonly used sedative in neurocritical care, propofol, have also been studies using PtiO2 monitoring. Rather unexpectedly they found that burst suppression induced by propofol has no effect on cerebral oxygenation [34].
The fraction of inspired oxygen (FiO2) obviously affects cerebral PtiO2 levels. One study has recently addressed this issue, which is important in the interpretation of measured PtiO2 values [42]. The authors report a PtiO2 increase from a baseline of 30 ± 5 mmHg to 147 ± 36 mmHg when the FiO2 was increased from individual baseline values to 100%. When it was decreased to 0.6 FiO2, PtiO2 fell to 63 ± 6 mmHg. Another study of 52 TBI patients showed that normobaric hyperoxia treatment resulted in a significant improvement in biochemical cerebral markers [69]. Using simultaneous cerebral microdialysis they report increased glucose levels with significantly decreased glutamate and lactate levels. They also report lactate/glucose and lactate/pyruvate ratio decreases at comparable CPP levels. Outcome in the normobaric hyperoxia treatment group was improved. They concluded that: “...normobaric hyperoxia in patients with severe TBI improves the indices of brain oxidative metabolism. Based on these data further mechanistic studies and a prospective randomized controlled trial are warranted” [69].
The effects of packed red blood cell transfusion (RBCT) on brain tissue partial pressure of oxygen has also been studied. The authors report a graded response of local cerebral oxygenation in a combined group of TBI and SAH patients [63]. In 74% of patients they observed a PtiO2 increase but did not provide a suitable explanation why it fell in 26% of patients. Cerebral perfusion pressure, SaO2, and FiO2 were similar before and after RBCT.
One study reports on the utility of PtiO2 monitoring during cerebral angiography [9]. In their series of 14 patients, 4 patients showed a linear PtiO2 decrease which indicated cerebral hypoxia without ICP elevation when the cerebral catheter was advanced through cervical vessels. They also report significant correlations between severe intracranial angiographic arterial caliber reduction and reduced PtiO2 values, which was also reflected in an increased number of ischaemic lesions on computed tomography (CT) imaging [9].
More complex physiological matters, which have attracted much attention in neurocritical care, have also been addressed using PtiO2 technology: the role of cerebral autoregulation monitoring, i.e. the link between the mechanism of cerebral vascular regulation and cerebral oxygenation regulation. So far four studies have shown that the mechanisms are closely linked [24, 28, 38, 64]. One study has concluded that “assessment of ptiO2-autoregulation gives valuable information on which patient will benefit from an increase in CPP and which CPP should be achieved to do so” [64]. This finding is in keeping with the suggestion that CPP elevation may be beneficial for ICP control and PtiO2 management in selected patients after TBI, those with intact cerebral autoregulation [24, 39].
Safety issues and technical considerations
We retrieved three papers which have systematically addressed technical issues related to using PtiO2 technology [16, 17, 25]. It is assumed that the reader is familiar with the insertion of intracranial monitors using bolt or tunnelling techniques. Both Licox and Neurotrend sensors can be introduced using these techniques, which have been used for over 20 years for ICP monitoring.
In 1998 a comprehensive study addressed technical considerations and safety issues; 118 Licox catheters, which were used in 101 patients, were assessed [16]. This paper includes findings of a previous publication based on an assessment of 73 catheters [17]. The results are as follows:
-
1.
Small iatrogenic haematomas were observed for two patients (1.7%). This number compares favourably to what has been published for similar monitoring devices, e.g. intraparenchymal intracranial pressure monitoring. This number is much smaller than what has been published for external ventricular drains which are widely for treatment of TBI patients.
-
2.
No infection occurred after 6.7 ± 3.9 days. This number compares to what has been published (see 1 above)
-
3.
The technical complication (dislocation or defect) rate was 13.6%. This figure is higher than what has been published (see 1 above). It does, however, not translate into patients’ harm because it relates to technical malfunction. Such technical complications incur increased expenses because a fresh sensor is required.
-
4.
The mean adaptation time was 79.0 ± 51.7 min. This number relates to this particular monitoring technology.
-
5.
The greatest PO2 display errors were measured during the first 4 days of continuous monitoring. There are no comparable data to further comment on this number.
-
6.
The maximal probe display error was 1.07 ± 2.14%, tested at temperatures between 22 and 37° C and tested at oxygen pressures of 0, 44 and 150 mmHg. This number is low and is irrelevant for daily clinical practice.
-
7.
The zero display error was −0.21 ± 0.25 mmHg. This number is low and is irrelevant for daily clinical practice.
-
8.
Excluding the first 1 h after insertion, data are reliable, with almost 100% good data quality.
Formal comparison between sensors
In vitro accuracy, long-term drift and response time were addressed in a paper published in 2005 [25]. This paper also compared Licox and Neurotrend. The authors conclude that (1) both systems measure oxygen tension sufficiently, (2) Licox technology measures more accurately than Neurotrend, (3) Neurotrend sensors read significantly lower PtiO2 in 1% O2, (4) Neurotrend sensors show an increasing deviation with higher oxygen concentrations which was due to 2 of 12 probes and (5) a slight drift towards lower oxygen tension readings for both sensors, but more pronounced for the Neurotrend, does not impair long-term use.
Similar work was presented, although in a non-peer-reviewed paper, restricted to seven patients in whom PtiO2 was measured simultaneously using Licox and Neurotrend probes [30]. The authors report that PtiO2 measured with Neurotrend was approximately 7 mmHg lower compared to Licox measurements. They also report that only one Neurotrend sensor worked properly during the entire monitoring period and one did not work at all. They report no malfunction with a Licox sensor. Another group reports calibration-related problems with the Neurotrend probe in 4 of 14 monitored patients [9].
We did not find any negative reports about PtiO2 technology. We did not retrieve any reports which report serious complications using PtiO2 technology. We did not retrieve any reports which have challenged the risk-benefit ratio of PtiO2 technology. There are no reports that persons involved in direct care of the patients have been harmed or injured while using PtiO2 technology.
Critical appraisal
All evidence stresses the utility of this parameter for optimizing cerebral oxygenation in neurosurgical and neurologic critical care. All but one paper have failed to demonstrate that using this technology improves outcome. The outcome improvement was only reflected in a mortality reduction [67].
Although PtiO2 is an independent parameter which can predict the development of delayed cerebral ischaemia, there are episodes where it will fail to do so or where response patterns of apparently interconnected cerebral parameters do not follow the expected directions [36]. This fact once again stresses the utility of a multiparameter approach.
Conclusions
Based on this review it is concluded that PtiO2 technology is a safe and valuable cerebral monitoring device in neurocritical care. Its clinical utility has repeatedly been clearly confirmed because it adds a monitoring parameter, independent from established cerebral monitoring devices. It offers new insights into cerebral physiology and pathophysiology. Pathologic values have been established in peer-reviewed research, which are not only relevant to outcome but are treatable. The benefits clearly outweigh the risks, which remains unchallenged in all publications retrieved. It is particularly attractive because it offers continuous, real-time data and is available at the bedside.
This summary has been confirmed in virtually all studies retrieved, exemplified by two conclusions quoted here. The authors conclude that “...P(ti)O2 monitoring is a safe and reliable technique for monitoring cerebral oxygenation” [16]. A more recent study has once again confirmed this statement. “Cerebral oxymetry is confirmed safe in the patient with multiple injuries with TBI” [20]. PtiO2 monitoring might even have the potential to improve outcome [67].
Yet this technology represents an invasive cerebral monitoring modality which requires cranial access. It should only be used in units which have experience with comparable monitoring devices, e.g. intracranial pressure monitoring. It appears helpful to establish guidelines for safe practice which have recently been suggested [75].
References
Albano C, Comandante L, Nolan S (2005) Innovations in the management of cerebral injury. Crit Care Nurs Q 28:135–149
Alessandri B, Hoelper BM, Behr R, Kempski O (2004) Accuracy and stability of temperature probes for intracranial application. J Neurosci Methods 139:161–165
Baumgartl H, Lubbers DW (1983) Microaxial needle sensors for polarographic measurements of local O2 in the cellular range of living tissue. In: Gnaiger E, Foerstner H (eds) Polarographic oxygen sensors. Springer, Berlin Heidelberg New York, pp 37–65
Becker A, Kuhnt T, Liedtke H, Krivokuca A, Bloching M, Dunst J (2002) Oxygenation measurements in head and neck cancers during hyperbaric oxygenation. Strahlenther Onkol 178:105–108
Belda FJ, Aguilar G, Soro M, Maruenda A (2004) Ventilatory management of the severely brain-injured patient (in Spanish). Rev Esp Anestesiol Reanim 51:143–150
Brawanski A, Faltermeier R, Rothoerl RD, Woertgen C (2002) Comparison of near-infrared spectroscopy and tissue p(O2) time series in patients after severe head injury and aneurysmal subarachnoid hemorrhage. J Cereb Blood Flow Metab 22:605–611
Burger R, Bendszus M, Vince GH, Roosen K, Marmarou A (2002) A new reproducible model of an epidural mass lesion in rodents. Part I: characterization by neurophysiological monitoring, magnetic resonance imaging, and histopathological analysis. J Neurosurg 97:1410–1418
Carre E, Cantais E, Darbin O, Terrier JP, Lonjon M, Palmier B, Risso JJ (2004) Technical aspects of an impact acceleration traumatic brain injury rat model with potential suitability for both microdialysis and PtiO2 monitoring. J Neurosci Methods 140:23–28
Carvi y Nievas M, Toktamis S, Hollerhage HG, Haas E (2005) Hyperacute measurement of brain-tissue oxygen, carbon dioxide, pH, and intracranial pressure before, during, and after cerebral angiography in patients with aneurysmatic subarachnoid hemorrhage in poor condition. Surg Neurol 64:362–367; discussion 367
Cavus E, Dorges V, Wagner-Berger H, Stadlbauer KH, Steinfath M, Wenzel V, Bein B, Scholz J (2005) Changes of local brain tissue oxygen pressure after vasopressin during spontaneous circulation. Acta Neurochir (Wien) 147:283–290; discussion 290
Clausen T, Khaldi A, Zauner A, Reinert M, Doppenberg E, Menzel M, Soukup J, Alves OL, Bullock MR (2005) Cerebral acid-base homeostasis after severe traumatic brain injury. J Neurosurg 103:597–607
Clausen T, Scharf A, Menzel M, Soukup J, Holz C, Rieger A, Hanisch F, Brath E, Nemeth N, Miko I, Vajkoczy P, Radke J, Henze D (2004) Influence of moderate and profound hyperventilation on cerebral blood flow, oxygenation and metabolism. Brain Res 1019:113–123
Dings J, Jager A, Meixensberger J, Roosen K (1998) Brain tissue pO2 and outcome after severe head injury. Neurol Res 20(Suppl 1):S71–S75
Dings J, Meixensberger J, Amschler J, Hamelbeck B, Roosen K (1996) Brain tissue pO2 in relation to cerebral perfusion pressure, TCD findings and TCD-CO2-reactivity after severe head injury. Acta Neurochir (Wien) 138:425–434
Dings J, Meixensberger J, Amschler J, Roosen K (1996) Continuous monitoring of brain tissue PO2: a new tool to minimize the risk of ischemia caused by hyperventilation therapy. Zentralbl Neurochir 57:177–183
Dings J, Meixensberger J, Jager A, Roosen K (1998) Clinical experience with 118 brain tissue oxygen partial pressure catheter probes. Neurosurgery 43:1082–1095
Dings J, Meixensberger J, Roosen K (1997) Brain tissue pO2-monitoring: catheter stability and complications. Neurol Res 19:241–245
Gelabert-Gonzalez M, Fernandez-Villa JM, Ginesta-Galan V (2002) Intra-operative monitoring of brain tissue O2 (PtiO2) during aneurysm surgery. Acta Neurochir (Wien) 144:863–866; discussion 866–867
Gonzalez H, Hunter CJ, Bennet L, Power GG, Gunn AJ (2005) Cerebral oxygenation during postasphyxial seizures in near-term fetal sheep. J Cereb Blood Flow Metab 25:911–918
Gracias VH, Guillamondegui OD, Stiefel MF, Wilensky EM, Bloom S, Gupta R, Pryor JP, Reilly PM, Leroux PD, Schwab CW (2004) Cerebral cortical oxygenation: a pilot study. J Trauma 56:469–472; discussion 464–472
Hare GM, Hum KM, Kim SY, Barr A, Baker AJ, Mazer CD (2004) Increased cerebral tissue oxygen tension after extensive hemodilution with a hemoglobin-based oxygen carrier. Anesth Analg 99:528–535, table of contents
Hartl R, Bardt TF, Kiening KL, Sarrafzadeh AS, Schneider GH, Unterberg AW (1997) Mannitol decreases ICP but does not improve brain-tissue pO2 in severely head-injured patients with intracranial hypertension. Acta Neurochir Suppl 70:40–42
Hemphill JC 3rd, Morabito D, Farrant M, Manley GT (2005) Brain tissue oxygen monitoring in intracerebral hemorrhage. Neurocrit Care 3:260–270
Hlatky R, Valadka AB, Robertson CS (2005) Intracranial pressure response to induced hypertension: role of dynamic pressure autoregulation. Neurosurgery 57:917–923; discussion 917–923
Hoelper BM, Alessandri B, Heimann A, Behr R, Kempski O (2005) Brain oxygen monitoring: in-vitro accuracy, long-term drift and response-time of Licox- and Neurotrend sensors. Acta Neurochir (Wien) 147:767–774
Ibanez J, Vilalta A, Mena MP, Vilalta J, Topczewski T, Noguer M, Sahuquillo J, Rubio E (2003) Intraoperative detection of ischemic brain hypoxia using oxygen tissue pressure microprobes (in Spanish). Neurocirugia (Astur) 14:483–489; discussion 490
Imberti R, Bellinzona G, Riccardi F, Pagani M, Langer M (2003) Cerebral perfusion pressure and cerebral tissue oxygen tension in a patient during cardiopulmonary resuscitation. Intensive Care Med 29:1016–1019
Jaeger M, Schuhmann MU, Soehle M, Meixensberger J (2006) Continuous assessment of cerebrovascular autoregulation after traumatic brain injury using brain tissue oxygen pressure reactivity. Crit Care Med 34:1783–1788
Jaeger M, Soehle M, Meixensberger J (2003) Effects of decompressive craniectomy on brain tissue oxygen in patients with intracranial hypertension. J Neurol Neurosurg Psychiatry 74:513–515
Jaeger M, Soehle M, Meixensberger J (2005) Brain tissue oxygen (PtiO2): a clinical comparison of two monitoring devices. Acta Neurochir Suppl 95:79–81
Jaeger M, Soehle M, Schuhmann MU, Winkler D, Meixensberger J (2005) Correlation of continuously monitored regional cerebral blood flow and brain tissue oxygen. Acta Neurochir (Wien) 147:51–56; discussion 56
Jia J, Lin YQ, Liu WF, Zhong TA, Zhang J, Ye Y, Xu YQ (2005) Study of the effects of mild hypothermia on cerebral PO2, PCO2 and pH and body temperature in patients with acute severe head injury. Chin J Traumatol 8:138–141
Jodicke A, Hubner F, Boker DK (2003) Monitoring of brain tissue oxygenation during aneurysm surgery: prediction of procedure-related ischemic events. J Neurosurg 98:515–523
Johnston AJ, Steiner LA, Chatfield DA, Coleman MR, Coles JP, Al-Rawi PG, Menon DK, Gupta AK (2003) Effects of propofol on cerebral oxygenation and metabolism after head injury. Br J Anaesth 91:781–786
Johnston AJ, Steiner LA, Chatfield DA, Coles JP, Hutchinson PJ, Al-Rawi PG, Menon DK, Gupta AK (2004) Effect of cerebral perfusion pressure augmentation with dopamine and norepinephrine on global and focal brain oxygenation after traumatic brain injury. Intensive Care Med 30:791–797
Kett-White R, Hutchinson PJ, Al-Rawi PG, Gupta AK, Pickard JD, Kirkpatrick PJ (2002) Adverse cerebral events detected after subarachnoid hemorrhage using brain oxygen and microdialysis probes. Neurosurgery 50:1213–1221; discussion 1221–1212
Kiening KL, Unterberg AW, Bardt TF, Schneider GH, Lanksch WR (1996) Monitoring of cerebral oxygenation in patients with severe head injuries: brain tissue PO2 versus jugular vein oxygen saturation. J Neurosurg 85:751–757
Lang EW, Czosnyka M, Mehdorn HM (2003) Tissue oxygen reactivity and cerebral autoregulation after severe traumatic brain injury. Crit Care Med 31:267–271
Lang EW, Lagopoulos J, Griffith J, Yip K, Yam A, Mudaliar Y, Mehdorn HM, Dorsch NW (2003) Cerebral vasomotor reactivity testing in head injury: the link between pressure and flow. J Neurol Neurosurg Psychiatry 74:1053–1059
Lubbers DW, Baumgartl H (1997) Heterogeneities and profiles of oxygen pressure in brain and kidney as examples of the pO2 distribution in the living tissue. Kidney Int 51:372–380
Maas AI, Fleckenstein W, de Jong DA, van Santbrink H (1993) Monitoring cerebral oxygenation: experimental studies and preliminary clinical results of continuous monitoring of cerebrospinal fluid and brain tissue oxygen tension. Acta Neurochir Suppl (Wien) 59:50–57
McLeod AD, Igielman F, Elwell C, Cope M, Smith M (2003) Measuring cerebral oxygenation during normobaric hyperoxia: a comparison of tissue microprobes, near-infrared spectroscopy, and jugular venous oximetry in head injury. Anesth Analg 97:851–856
Meixensberger J, Baunach S, Amschler J, Dings J, Roosen K (1997) Influence of body position on tissue-pO2, cerebral perfusion pressure and intracranial pressure in patients with acute brain injury. Neurol Res 19:249–253
Meixensberger J, Jager A, Dings J, Baunach S, Roosen K (1998) Multimodal hemodynamic neuromonitoring-quality and consequences for therapy of severely head injured patients. Acta Neurochir Suppl 71:260–262
Meixensberger J, Renner C, Simanowski R, Schmidtke A, Dings J, Roosen K (2004) Influence of cerebral oxygenation following severe head injury on neuropsychological testing. Neurol Res 26:414–417
Mulvey JM, Dorsch NW, Mudaliar Y, Lang EW (2004) Multimodality monitoring in severe traumatic brain injury: the role of brain tissue oxygenation monitoring. Neurocrit Care 1:391–402
Ng I, Lim J, Wong HB (2004) Effects of head posture on cerebral hemodynamics: its influences on intracranial pressure, cerebral perfusion pressure, and cerebral oxygenation. Neurosurgery 54:593–597; discussion 598
Okonkwo DO, Wagner J, Melon DE, Alden T, Stone JR, Helm GA, Jane JA Sr (2003) Trans-sodium crocetinate increases oxygen delivery to brain parenchyma in rats on oxygen supplementation. Neurosci Lett 352:97–100
Raabe A, Gottschalk A, Hommel M, Dubben HH, Strandl T (2005) No effect of the hemoglobin solution HBOC-201 on the response of the rat R1H tumor to fractionated irradiation. Strahlenther Onkol 181:730–737
Reinert M, Barth A, Rothen HU, Schaller B, Takala J, Seiler RW (2003) Effects of cerebral perfusion pressure and increased fraction of inspired oxygen on brain tissue oxygen, lactate and glucose in patients with severe head injury. Acta Neurochir (Wien) 145:341–349; discussion 349–350
Reithmeier T, Lohr M, Pakos P, Ketter G, Ernestus RI (2005) Relevance of ICP and ptiO(2) for indication and timing of decompressive craniectomy in patients with malignant brain edema. Acta Neurochir (Wien) 147:947–952
Rossi S, Balestreri M, Spagnoli D, Bellinzona G, Valeriani V, Bruzzone P, Maestri M, Stocchetti N (2000) Oxygen delivery and oxygen tension in cerebral tissue during global cerebral ischaemia: a swine model. Acta Neurochir Suppl 76:199–202
Rossi S, Stocchetti N, Longhi L, Balestreri M, Spagnoli D, Zanier ER, Bellinzona G (2001) Brain oxygen tension, oxygen supply, and oxygen consumption during arterial hyperoxia in a model of progressive cerebral ischemia. J Neurotrauma 18:163–174
Sarrafzadeh AS, Kiening KL, Bardt TF, Hartl R, Schneider GH, Unterberg AW (1997) Monitoring cerebral oxygenation: a methodological comparison (in German). Anasthesiol Intensivmed Notfallmed Schmerzther 32:S224–S230
Sarrafzadeh AS, Kiening KL, Bardt TF, Schneider GH, Unterberg AW, Lanksch WR (1998) Cerebral oxygenation in contusioned vs. nonlesioned brain tissue: monitoring of PtiO2 with Licox and Paratrend. Acta Neurochir Suppl 71:186–189
Sarrafzadeh AS, Kiening KL, Callsen TA, Unterberg AW (2003) Metabolic changes during impending and manifest cerebral hypoxia in traumatic brain injury. Br J Neurosurg 17:340–346
Sarrafzadeh AS, Kiening KL, Unterberg AW (2003) Neuromonitoring: brain oxygenation and microdialysis. Curr Neurol Neurosci Rep 3:517–523
Sarrafzadeh AS, Peltonen EE, Kaisers U, Kuchler I, Lanksch WR, Unterberg AW (2001) Secondary insults in severe head injury-do multiply injured patients do worse? Crit Care Med 29:1116–1123
Sarrafzadeh AS, Sakowitz OW, Callsen TA, Lanksch WR, Unterberg AW (2002) Detection of secondary insults by brain tissue pO2 and bedside microdialysis in severe head injury. Acta Neurochir Suppl 81:319–321
Sarrafzadeh AS, Unterberg AW, Lanksch WR (1998) Bedside-microdialysis for early detection of vasospasm after subarachnoid hemorrhage. Case report and review of the literature. Zentralbl Neurochir 59:269–273
Scheufler KM, Lehnert A, Rohrborn HJ, Nadstawek J, Thees C (2004) Individual value of brain tissue oxygen pressure, microvascular oxygen saturation, cytochrome redox level, and energy metabolites in detecting critically reduced cerebral energy state during acute changes in global cerebral perfusion. J Neurosurg Anesthesiol 16:210–219
Schneider GH, Sarrafzadeh AS, Kiening KL, Bardt TF, Unterberg AW, Lanksch WR (1998) Influence of hyperventilation on brain tissue-PO2, PCO2, and pH in patients with intracranial hypertension. Acta Neurochir Suppl 71:62–65
Smith MJ, Stiefel MF, Magge S, Frangos S, Bloom S, Gracias V, Le Roux PD (2005) Packed red blood cell transfusion increases local cerebral oxygenation. Crit Care Med 33:1104–1108
Soehle M, Jaeger M, Meixensberger J (2003) Online assessment of brain tissue oxygen autoregulation in traumatic brain injury and subarachnoid hemorrhage. Neurol Res 25:411–417
Stiefel MF, Heuer GG, Abrahams JM, Bloom S, Smith MJ, Maloney-Wilensky E, Grady MS, LeRoux PD (2004) The effect of nimodipine on cerebral oxygenation in patients with poor-grade subarachnoid hemorrhage. J Neurosurg 101:594–599
Stiefel MF, Heuer GG, Smith MJ, Bloom S, Maloney-Wilensky E, Gracias VH, Grady MS, LeRoux PD (2004) Cerebral oxygenation following decompressive hemicraniectomy for the treatment of refractory intracranial hypertension. J Neurosurg 101:241–247
Stiefel MF, Spiotta A, Gracias VH, Garuffe AM, Guillamondegui O, Maloney-Wilensky E, Bloom S, Grady MS, LeRoux PD (2005) Reduced mortality rate in patients with severe traumatic brain injury treated with brain tissue oxygen monitoring. J Neurosurg 103:805–811
Strege RJ, Lang EW, Stark AM, Scheffner H, Fritsch MJ, Barth H, Mehdorn HM (2003) Cerebral edema leading to decompressive craniectomy: an assessment of the preceding clinical and neuromonitoring trends. Neurol Res 25:510–515
Tolias CM, Reinert M, Seiler R, Gilman C, Scharf A, Bullock MR (2004) Normobaric hyperoxia-induced improvement in cerebral metabolism and reduction in intracranial pressure in patients with severe head injury: a prospective historical cohort-matched study. J Neurosurg 101:435–444
Unterberg AW, Kiening KL, Hartl R, Bardt T, Sarrafzadeh AS, Lanksch WR (1997) Multimodal monitoring in patients with head injury: evaluation of the effects of treatment on cerebral oxygenation. J Trauma 42:S32–S37
Unterberg AW, Sarrafzadeh AS, Lanksch WR (1999) Skull-brain injury in polytrauma-results of neurosurgery (in German). Anasthesiol Intensivmed Notfallmed Schmerzther 34(Suppl 1):S13–S19
Valadka AB, Gopinath SP, Contant CF, Uzura M, Robertson CS (1998) Relationship of brain tissue PO2 to outcome after severe head injury. Crit Care Med 26:1576–1581
van Santbrink H, Maas AI, Avezaat CJ (1996) Continuous monitoring of partial pressure of brain tissue oxygen in patients with severe head injury. Neurosurgery 38:21–31
van Santbrink H, Schouten JW, Steyerberg EW, Avezaat CJ, Maas AI (2002) Serial transcranial Doppler measurements in traumatic brain injury with special focus on the early posttraumatic period. Acta Neurochir (Wien) 144:1141–1149
Wilensky EM, Bloom S, Leichter D, Verdiramo AM, Ledwith M, Stiefel M, LeRoux P, Grady MS (2005) Brain tissue oxygen practice guidelines using the LICOX CMP monitoring system. J Neurosci Nurs 37:278–288
Author information
Authors and Affiliations
Additional information
Comments
Ignacio J. Previgliano, Buenos Aires, Argentina
Brain tissue oxygenation, as demonstrated in this complete systematic review by Lang et al., is a promising technology. I agree that it offers continuous, real-time data and is available at the bedside safely. The rapid correlation between the indicated treatment and the regional response allowed by the devices is stimulating.
Beyond the applications updated in the review there is a potential use in early brain death diagnosis that should be borne in mind as a matter of research. Estimation of the best cerebral perfusion pressure and hyperventilation therapy control are, in my opinion, among the most important applications.
Nevertheless, there are some important issues to highlight regarding this technology. The Neurotrend device has been dropped off the market by Codman, Johnson and Johnson, so Licox is the only device available. There are no papers assessing sensitivity, specificity, positive and negative value as well as positive or negative likelihood ratio and pre- or post-test odds for the method as a prognostic or diagnostic tool, according to the principles of evidence-based medicine. There are also controversies on which region should be monitored: non-injured tissue, penumbra area or injured tissue, as well as which are the normal values or the pathologic threshold. Another controversy is the one that confronts regional vs global monitoring systems.
Even though well conducted and serious, most of the research has been done in Germany where the Gesellschaft für Medizinische Sondentechnik (GMS) developed the polarographic cell device, as is noted in the review references.
In view of these critical considerations that should be taken into account, brain tissue oxygenation should be considered a new star in the neurocritical monitoring constellation in which none is more important than the other and all of them are still looking for their right place.
Comment
Alexander Brawanski, Regensburg, Germany
In their paper the authors review the development and clinical application of the registration of cerebral oxygenation (PtiO2). They reviewed the pertinent literature from 2004 to 2006 with the aim of collecting the relevant information on clinical applicability, safety issues and clinical usefulness. All in all 1,400 publications were scanned. Mostly PtiO2 monitoring was used in traumatic brain injury (TBI) followed by subarachnoid hemorrhage. Less commonly it was used intraoperatively during cerebrovascular surgery. Other rarer applications, like during cardiopulmonary resuscitation or cerebral angiography, are included in the review. The authors report that PtiO2 monitoring is mostly used clinically in conjunction with additional cerebral monitoring devices like intracranial pressure (ICP) monitoring, jugular venous saturation monitoring, cerebral microdialysis and near infrared spectroscopy, just to name a few. Two different devices are on the market based on different technology and giving slightly different data. The main results of this review are that this methodology is safe and has an impact on clinical treatment of the above-mentioned patient groups. A safety range of tissue oxygen levels could be established, below that the outcome of the studied patients was significantly worse. Thus PtiO2 monitoring has a prognostic value. Negative effects of hyperventilation were detected and it was applied more safely as hypoxic cerebral oxygen levels were avoided. The indication for decompressive craniectomy in severe brain swelling could be guided by cerebral oxygen monitoring more safely. PtiO2 has also been proven useful in monitoring the use of vasoactive drugs given in neurocritical care as well as in elucidating effects of nimodipine and mannitol. There were no severe side effects using PtiO2 in patients. Both available probes measure oxygen tension sufficiently. However, the Licox technology seems to be more accurate than the Neurotrend monitor. The often quoted disadvantage of the “locality” of the measuring devices—they measure an area of a few cubic millimeters—could be alleviated by several publications. These could show that there is a certain random positioning error. On the other hand these local measurements correlated well with more global methods like cerebral blood flow. The authors conclude that PtiO2 monitoring is safe, clinically useful, and it improves the treatment of ICU patients. They favor, however, a multiparameter approach, meaning that other “brain” parameters should be monitored in addition. All in all this is a very informative study giving relevant and up-to-date information about this important monitoring technique.
Rights and permissions
About this article
Cite this article
Lang, E.W., Mulvey, J.M., Mudaliar, Y. et al. Direct cerebral oxygenation monitoring—a systematic review of recent publications. Neurosurg Rev 30, 99–107 (2007). https://doi.org/10.1007/s10143-006-0062-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-006-0062-4