Abstract
Thanks to today’s modern imaging examination techniques and especially to the common use of intracranial electrodes for localizing seizure foci, more and more patients with partial epilepsy can be treated microsurgically. The results of such neurosurgical therapies are very good, particularly in mesial temporal lobe epilepsy. In recent years, good results (60–70% seizure freedom) have also been achieved in extratemporal epilepsy surgery, so that such procedures can now be recommended for carefully selected patients. In this review, presurgical evaluations and the different surgical approaches are presented.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
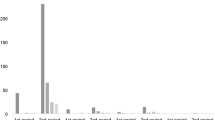
Epilepsy is one of the more common neurological diseases, with a prevalence of 0.5–1.0% and estimated lifetime cumulative incidence of 3% [79, 81]. It may arise from a constitutional predisposition or as a consequence of acquired cerebral pathology. Specific causes for epilepsy differ with geographic areas, but idiopathic/cryptogenic epilepsies are the most frequent type, accounting for two thirds of all new cases [79, 81]. In patients with identified etiology for epilepsy, cerebrovascular disease is the most common cause (accounting for 10.9% of new cases), followed by congenital diseases (8%), trauma (5.5%), neoplasms (4.1%), degenerative disorders (3.5%), and infections (2.5%) [81].
Approximately 40% of the patients suffer from generalized seizures and 60% from focal (partial) seizures [78]. About 55% of focal epilepsies in which seizures originate from a circumscribed cerebral region are temporal lobe epilepsies. Epilepsies of the frontal, parietal, or occipital lobe make up the remaining 45%. This heterogeneity in the causes and clinical syndromes of epilepsy is also reflected in the different therapeutic approaches, which mainly consist of antiepileptic medication and, in some cases, epilepsy surgery.
Complete seizure control and improvement of quality of life are the main goals of any treatment. Antiepileptic drugs are usually given as the first therapeutic step. However, fewer than 33% of all patients achieve full control of seizures for 1 year on monotherapy, and only 10–20% of the failures achieve full control of seizures with two-drug therapy [128, 129, 178, 194, 198, 206, 240].
Interestingly, the percentage of drug-resistant epilepsies has not diminished significantly, in spite of the new antiepileptic drugs [17, 115, 131, 174]. Overall, about 30–40% of all patients with epilepsy have medically intractable seizures, and 50% of these are candidates for epilepsy surgery [2, 20, 44, 53, 80, 196]. For the United States, it has been estimated that there are more than 100,000 candidates for surgical treatment, with 5,000–10,000 added annually [31, 32, 53]. Despite this large number of potential surgical candidates, only 2,000 surgical procedures were performed per year in the United States [53, 80]. This discrepancy in need and utilization may be explained by:
-
1.
Ignorance among primary care physicians of the recent advances in safety and efficacy of surgical epilepsy treatment
-
2.
The fact that some patients prefer to tolerate seizures and side effects rather than undergo surgery
-
3.
The lack of funding by third-parties for the expensive presurgical workup and surgical treatment, even though several studies have shown their cost effectiveness [18, 56]
In the last decade, however, epilepsy surgery has gained acceptance, and a large number of patients have been operated on throughout the world. This new interest can be explained by the advances in presurgical evaluation and improved surgical techniques. Modern presurgical workup includes noninvasive and invasive telemetric long-term EEG monitoring, quantitative magnetic resonance imaging (MRI), functional MRI, positron emission tomography (PET), single photon emission tomography (SPECT), MR spectroscopy (MRS), and magnetoencephalography (MEG).
New surgical techniques have made epilepsy surgery safer and more effective. For instance, the introduction of microneurosurgery has allowed more selective operations such as selective amygdalohippocampectomy [145, 255]. Furthermore, palliative surgical procedures such as multiple subpial transection and the formerly more common partial callosotomy have witnessed renewed interest [130, 138, 140, 179, 180, 209, 281]. Some centers have also evaluated new approaches such as radiosurgery for the treatment of partial epilepsy [170, 171, 172, 173, 227].
The extent to which today’s possibilities of epilepsy surgery have changed the neurologist’s daily routine can be illustrated best with the example of so-called mesial temporal lobe epilepsy, the most common form of focal epilepsy. In this type, seizures are generated in the amygdala and the hippocampal formation. Mesial temporal lobe epilepsy was long reputed to be incurable, and patients could only be abandoned to their fate. However, the currently available interventions, anterior 2/3 temporal lobectomy or the less crude selective amygdalohippocampectomy (specific resection of the two mesial temporal structures causing the seizures), lead to postsurgical freedom from seizures in about 80% of patients [54, 145, 200, 212, 255, 258]. These good operative results, reached over several decades, now make it clear why unsuccessful drug therapy for medically refractory mesial temporal lobe epilepsy should no longer be continued indefinitely. Rather, such patients should be operated on as soon as possible.
Whereas the treatment of mesial temporal lobe epilepsy has been significantly simplified by surgery, drug-resistant extratemporal epilepsies still constitute a major challenge to epileptologists and neurosurgeons. Until about 10 years ago, the results of major epilepsy centers with this category of patients were rather disappointing, and quite frequently only 40–50% of the patients showed postsurgical seizure-free outcomes; but also with extratemporal epilepsies, the development of imaging procedures has simplified precise seizure localization. Furthermore, improved neurosurgical techniques have increasingly led to very good operative results, so that surgical interventions must also be considered as a therapeutic option for drug-resistant extratemporal epilepsies.
Abnormal brain areas involved in interictal and ictal activity
When epilepsy surgery is considered, presurgical workup must define the different brain areas that either generate seizures or are involved in interictal and ictal epileptiform activity. Lüders proposed a theoretical concept that distinguishes six brain areas (Table 1) [121, 122, 184]. The identification of these areas allows neurosurgeons and neurologists not only to tailor the resection but also predict postoperative deficits to a certain extent. Therefore, it becomes clear that presurgical evaluation includes several different types of diagnostic studies.
Current indications for epilepsy surgery
Before an indication for the surgical treatment of epilepsy can be established, the tentative diagnosis of epilepsy must be verified. This may sound banal but, as the diagnosis sets the course for possible further diagnostic procedures, it has an important role. In epileptology, as elsewhere in clinical medicine, history is also one of the most important diagnostic tools, because exact observation allows the differentiation of epileptic seizures from nonepileptic ones, while an accurate history usually provides important clues to seizure origin. The typical seizure characteristics of partial epilepsies are summarized in Table 2 [12, 25, 55, 96, 186, 188, 189, 190, 201, 202, 260, 263, 268, 269, 270].
When the tentative diagnosis of partial epilepsy has been made on the basis of history and surgical treatment is considered because of drug-resistant seizures, the next step is to evaluate the patients as candidates for epilepsy surgery according to the following criteria set by Walker [249]:
-
1.
Progressive neurological disease (e.g., malignant brain tumor, cerebral vasculitis, multiple sclerosis, etc.) should be ruled out. Although patients with malignant tumors can also have epileptic seizures, operations relating to this cannot be considered epilepsy surgery (so-called epilepsy surgery sensu strictu), because primarily they do not represent treatment of epilepsy but rather of malignant tumors.
-
2.
The resistance to drug treatment has to be ascertained. Here it is particularly important to make sure that the formerly used antiepileptic drugs have been carefully administered up to the limit of “subjective intoxication.” This means not only that antiepileptic drugs should be given up to the limit within the therapeutic range but that individual differences in metabolism be considered and the drug be given to just below the blood level at which side effects set in (which may be far above the maximum therapeutic level). Furthermore, apart from at least two monotherapies, polytherapies also should have been tried.
-
3.
The duration of the disease has to be at least 1–2 years. However, exceptions are allowed in this respect (particularly with epilepsies due to structural lesions or with early-diagnosed mesial temporal lobe epilepsy).
-
4.
Patients have to be handicapped by the seizures, although this may of course differ significantly from individual to individual. Generally, however, the indication for surgery should be established rather cautiously when the seizures consist only of sensory phenomena without alteration of consciousness, even if they are frequent.
-
5.
The patients should be motivated for the presurgical workup and operation and aware, above all, that they must also take antiepileptic drugs postsurgically.
-
6.
An IQ below 70 strongly suggests diffuse brain disease, in which case the prospects of success of an epilepsy surgery intervention are poor and the surgical indication should be established with caution.
-
7.
Psychiatric diseases are also a contraindication to epilepsy surgery.
Stages of presurgical evaluation
If there are no contraindications to operative intervention on the basis of the aforementioned criteria, the patients normally need further evaluation. This presurgical workup of candidates for epilepsy surgery is comprised of noninvasive (phase I) and invasive (phase II) evaluation. Phase I consists of a detailed history including review of past treatment, neurological exam, neuropsychological testing, psychiatric and psychosocial evaluation, interictal and ictal EEG recording (including video EEG monitoring), MEG, structural CT and MRI, MRS, fMRI, SPECT, and PET.
This first phase of presurgical evaluation screens patients considered for surgery. If the epileptogenic focus (zone) can be identified during phase I, the recommendation may be made to proceed directly to epilepsy surgery. In some patients, however, phase I cannot accurately localize the epileptogenic zone, and an additional invasive evaluation (phase II) becomes mandatory. This includes video EEG recording by means of invasive depth, subdural, and/or epidural electrodes and, if necessary, further neuropsychological control with intra-arterial amobarbital tests. At the end of phase II, a final decision can be made whether a patient suffers from a surgically remediable epilepsy syndrome and thus whether surgery with or without intraoperative EEG monitoring (phase III) can be performed (Table 3) [40].
Noninvasive evaluations (phase I)
Scalp electroencephalogram
Scalp (surface) EEG in the waking and sleeping states with simultaneous video monitoring of seizures is one of the more important evaluations in phase I. Video EEG monitoring allows adequate observation not only of seizures but also of the simultaneously recorded EEGs, which enables conclusions to be drawn on the origin of the seizures (lateralization and localization).
Several studies have shown that the repeated incidence of interictal epileptiform potentials in the same cerebral region in multiple EEGs correlates very well with the origin of ictal discharges [5, 213]. Thus, interictal epileptiform discharges may be recorded in 50% of patients during routine awake EEG [103, 157, 163, 164, 197, 252]. In temporal lobe epilepsy, the diagnostic accuracy even increases up to 90% by recording a sleep EEG [29, 197, 252].
In mesial temporal lobe epilepsy, characteristically epileptiform potentials are found in basal areas of the frontal and temporal lobes [260], while in neocortical temporal lobe epilepsy the correlation with these potentials is of varying strength. In temporal lobe epilepsy, ictal surface EEG classically reveals rhythmic sinusoidal theta activity of high amplitude and low frequency [256].
While interictal and ictal surface EEG is very helpful in mesial temporal lobe epilepsy in terms of localization and lateralization of seizure origin, its value in extratemporal epilepsies is highly variable. In frontal lobe epilepsy, interictal and ictal surface EEG often reveals unspecific changes or is completely silent, i.e., abnormal EEG patterns can be observed in only about 10% of the patients [96, 163, 270]. The fact that, in frontal lobe epilepsy with its partially bizarre motor signs, EEG is often not very helpful makes the diagnosis even more difficult and explains frequent misdiagnoses of “hysteric,” “nonepileptic,” or “psychogenic” seizures.
In contrast to frontal lobe epilepsy, interictal as well as ictal epileptiform potentials are frequently observed in epilepsies of the occipital and parietal lobes [11, 202]. Thus parietal epileptiform potentials are found in approximately 65% of patients with parietal lobe epilepsy and occipital potentials in 79–97% of patients with occipital lobe epilepsy. At the same time, only 10% and 14% of patients with parietal and occipital lobe epilepsy, respectively, have normal EEGs [11, 202].
Magnetoencephalography
The basic concept underlying MEG is the measurement of extracranial magnetic fields generated by the electric activity of cortical pyramidal cells [3, 48, 136, 181, 193]. Unlike EEG, MEG is reference-free, as it measures magnetic fields rather than differences in potential.
Numerous studies of MEG in medically intractable epilepsy have shown that it can detect interictal and ictal epileptiform activity [3, 4, 49, 106, 182, 226, 229]. Many studies compared localization by MEG with “standard” localization of the epileptogenic zone as determined by scalp and invasive EEG as well as MRI [50, 106, 207]. Smith et al. performed MEG in 50 patients being evaluated for possible surgery [207]. Of them, 56% had complete agreement between MEG and standard localizations, partial agreement in 12%, no agreement in 10%, lack of spikes in MEG in 16%, and inadequate data in 6% [207]. In this study, MEG was more effective localizing epileptogenic zones involving the cerebral convexity rather than in the deep structures. Other studies led to similar findings, in particular for extratemporal epilepsies [104, 106, 134]. Thus, MEG has been shown to be effective for detecting interictal and ictal epileptiform discharges.
The primary clinical use of MEG includes neocortical epilepsies, cases with normal MRI, and patients with large MRI abnormalities. In these groups, MEG can eliminate the need for invasive EEG monitoring and thereby reduce costs and morbidity. However, since MEG is rather expensive and insurance companies are reluctant to cover the costs, its use in localizing the foci of epileptic seizures is mainly limited to scientific issues.
Structural imaging
The evaluation of patients with epilepsy has been revolutionized by the advent of MRI. It provides the best anatomic detail of any imaging modality and is the most sensitive tool for demonstrating large structural lesions. Because of its superior sensitivity and specificity compared with CT, MRI is the preferred imaging technique in the presurgical workup of patients with medically refractory epilepsy [221].
Usually, high-resolution MRI is performed according to a special epilepsy protocol [9, 22, 34]. In the last decade, this technique has led to the recognition of smaller, even tiny epileptogenic lesions. Thus, in addition to the tumors and vascular malformations that are most commonly diagnosed today (e.g., cavernous and arteriovenous malformations), very small abnormalities due to migration disorders (cortical dysplasia, polymicrogyria, hamartoma, etc.) can be detected. Apart from these structural abnormalities, MRI in patients with mesial temporal lobe epilepsy often reveals mesial temporal sclerosis, which is characterized by both hippocampal atrophy seen on T1-weighted images and increased hippocampal signal intensity seen on T2-weighted spin-echo images [8, 58, 92, 95, 113, 127, 242]. Although mesial temporal sclerosis can usually be diagnosed by visual inspection of the MRI, modern MRI-based quantitative volume measurement of the hippocampal formation has further improved its sensitivity of detection [23, 90, 114].
In 30–40% of patients with extratemporal epilepsies, epileptogenic tumors are found (ganglioglioma, low-grade astrocytoma, oligodendroglioma, etc.) [27]. Cortical migration disorders are found with the same frequency [27]. Rare structural lesions include Sturge-Weber syndrome, postnatal injuries (porencephalic cysts), scars, etc. Such intracerebral lesions nearly always match with the epileptogenic zones, and patients—provided the further results of noninvasive studies can be explained by the lesion—can be directly passed on to the neurosurgeon [37, 105, 231]. However, in approximately 20% of patients, the most modern MR techniques fail to detect any lesions. Although these surgical candidates are among the most difficult patients to treat, it has been found that epilepsy surgery may yield good seizure outcome in these cases as well [205].
New MRI techniques such as fluid attenuated inversion recovery (FLAIR) sequence and diffusion and perfusion MRI may further help to localize seizure origin [162]. The FLAIR MRI produces images in which parenchymal lesions have a high signal and CSF has a low signal [162]. Thus, FLAIR imaging improved the identification of hippocampal sclerosis and lesions but not of heterotopias [7, 265]. Diffusion-weighted imaging was initially implemented for the identification of acute cerebral infarcts but has also been reported to be sensitive enough for the detection of epileptogenic foci [42, 111, 266]. Though diffusion and perfusion MRI have been found to be very sensitive, their use in presurgical workup still has to be tested.
Functional magnetic resonance imaging
More recent applications of the magnetic resonance technique include fMRI and MRS [152, 191, 192]. The former provides high-resolution, noninvasive measurements of neural activity by means of a signal dependent on the blood oxygen level [63, 64, 87, 93, 239, 250]. Thus, fMRI can supply the neurosurgeon with information about cortical areas that must be spared in the planned resection and, if they are not to be spared, about the neurological deficits to be expected postoperatively. Even though some of the initial data are very encouraging, at present fMRI has not yet taken over the role of functional mapping with intracranial electrodes in presurgical evaluation for epilepsy surgery. Triggering by EEG may increase the use of this new technique [107, 230, 250].
Magnetic resonance spectroscopy
The only noninvasive technique capable of measuring chemicals within the body, MRS measures chemical changes in the examined cerebral areas by application of the principle that every chemically distinct nucleus in a compound resonates at a slightly different frequency [33, 191]. In patients with epilepsy, MRS performed in vivo has mainly examined the 31P and 1H nuclei. Conventional MRS software distinguishes short- and long-echo time acquisitions. The latter produces spectra including N-acetyl aspartate (NAA), choline-containing compounds (Cho), phosphocreatine plus creatine (Cr), and lactate [33, 191]. Short-echo time acquisitions include the same metabolites and, in addition, myoinositol, glutamate and glutamine, alanine, glucose, scylloinositol/taurine, and proteins/lipids [10, 28, 86, 137, 161].
Because NAA is located primarily inside neurons and precursor cells, its reduction indicates neuronal loss or dysfunction. Conversely, Cho and Cr are found in both neurons and glial cells. Yet, MRS has been performed mainly in patients with temporal lobe epilepsy, in 60–90% of whom lower NAA concentrations could be observed in the hippocampus [112]. In extratemporal lobe epilepsy, there are only a few studies on the localizing value of MRS. Stanley et al. reported on 20 patients with nonlesional extratemporal epilepsy in whom the relative NAA resonance intensities (i.e., NAA/Cr, NAA/Cho, and NAA/Cr+Cho) were all significantly reduced, particularly in the regions of seizure origin [225]. However, the usefulness of MRS in extratemporal epilepsy has not been confirmed yet.
Functional imaging
Aside from structural imaging for the detection of cerebral lesions, functional imaging constitutes a helpful extension of the presurgical diagnostic workup. Thus, SPECT and PET both exploit the circumstance that an epileptogenic focus in the interictal state receives a smaller blood supply (hypoperfusion in SPECT) and also metabolizes less glucose than normal brain tissue (hypometabolism in PET) [21, 72, 75, 76]. In the ictal state, the contrary applies, i.e., the epileptogenic focus receives a larger blood supply (hyperperfusion in SPECT) and metabolizes more glucose (hypermetabolism in PET) [21, 72, 75, 76].
The most commonly used tracers for both interictal and ictal SPECT are technetium 99m hexamethyl-propylene amine oxime (HMPAO) and technetium 99m ethylene cysteinate dimer (ECD). In ictal SPECT, the tracer is administered intravenously at the beginning of the clinical and/or electroencephalographic seizure onset. A physician or nurse who injects the tracer and video EEG surveillance are needed for this procedure [232]. Even though it appears very complicated and time-consuming, the usefulness of ictal SPECT examination is enormous and justifies the effort, especially in extratemporal epilepsy.
Interictal SPECT in temporal lobe epilepsy has a sensitivity of about 50% and is therefore only of limited value for presurgical workup [72, 232]. In extratemporal lobe epilepsy, its localizing accuracy is even lower [91, 126]. Conversely, ictal SPECT is a very useful tool in presurgical evaluation. In mesiotemporal lobe epilepsy, its sensitivity ranges from 90% to 97% [41, 84, 217]. In extratemporal lobe epilepsy, the localizing accuracy of ictal SPECT depends mainly on the injection delay. The sensitivity in extratemporal lobe epilepsy was 81–90% in various studies [45, 46, 47, 77, 83, 117, 125, 126]. The localizing value of SPECT can be notably improved by coregistration of the interictal and ictal SPECT images, which yields an “ictal difference image” that may be coregistered with a patient’s MRI [117, 147].
Interictal and (rarely performed) ictal PET have been carried out mainly with [18F] fluorodeoxyglucose and [11C] flumazenil [82, 110, 233, 234]. In temporal lobe epilepsy, interictal PET demonstrates hypometabolism in about 60–90% of patients and therefore can be used in presurgical diagnosis [82]. However, PET is less sensitive in extratemporal lobe epilepsies (about 45–60%) and provides few useful data in these forms of epilepsy [82]. For example, its role in localizing the epileptogenic focus in MRI-negative frontal lobe epilepsy is not well established. Although PET may detect frontal focal hypometabolism, the abnormality detected may not correspond to the epileptogenic focus. The hypometabolism may even be found in regions outside the frontal lobe [82].
Neuropsychological evaluation
Every patient with temporal or extratemporal epilepsy needs thorough preoperative neuropsychological examination. The following functions are generally tested: memory (mainly a function of the temporal lobe), learning, IQ, language lateralization, motor skills, visuoperceptive and visuoconstructive functions, attention and concentration, and verbal and nonverbal fluency [102, 154, 168]. Although the test batteries may vary from center to center, some, such as IQ testing with the Wechsler Adult Intelligence Scale, are generally accepted and established [97, 98, 251]. In addition, some tests are administered to find cognitive deficits of the lobe from which seizures originate. Tests for assessing frontal lobe functions include the Wisconsin Card Sorting, Design Fluency, Stroop, tower, trail-making, finger-tapping, and Purdue or Grooved Pegboard tests [19, 43, 69, 102, 118, 135, 158, 175, 224, 228, 235]. The Rey-Osterrieth Complex Figure Test and somatosensory tests such as two-point discrimination are used to assess parietal lobe function [71, 98, 118, 153, 177]. Memory tests focus on learning and retention of both verbal and nonverbal material. The most commonly administered test is the original or revised Wechsler Memory Scale [98]. Apart from word pairs and story recall, a list learning test such as the California or the Rey Auditory verbal learning tests is often used [98]. Tests for the assessment of language skills include the Western Aphasia Battery, Boston Diagnostic Aphasia Examination, and Boston Naming tests [98, 102, 236]. The last named is also used to assess function of the temporal neocortex [98, 99, 100, 102, 236].
Invasive evaluations (phase II)
If the seizure characteristics and results of phase I evaluations are concordant, patients can be directly passed on to neurosurgery. In the case of mesial temporal lobe epilepsy, this can be done more and more often, thanks to modern imaging procedures [37, 105, 231]. However, when noninvasive presurgical workup fails to delineate the epileptogenic zone adequately, invasive EEG may become necessary. In addition, if the side and site of seizure origin imply overlap with an eloquent speech and/or memory area, an amobarbital (Wada) test may become necessary.
Invasive electroencephalographic recording
The proportion of patients undergoing intracranial electrode implantation varies among epilepsy centers [148, 183, 216, 279]. The following indications for invasive monitoring are currently applied: lack of a potentially epileptogenic structural lesion as revealed by MRI, multiple putative epileptogenic lesions (zones), scalp EEG with multifocal or no interictal epileptiform discharges, surface EEG with indeterminate or multifocal seizure onset, discordant phase I findings, and seizure origin as identified by noninvasive procedures appearing diffuse or proximate to an eloquent area (e.g., perirolandic, Wernicke’s, or Broca’s area). Based on these indications, invasive EEG recording has been performed in 5–20% and 40–70% of temporal and extratemporal lobe epilepsy surgery patients, respectively [218].
If there is reason to assume that the seizures originate in mesiotemporal structures, intracranial EEG can be recorded by means of semi-invasive foramen ovale electrodes [257, 259, 261]. If phase I findings, however, point to an extratemporal or temporal neocortical seizure onset, invasive monitoring is performed by strip and/or grid electrodes and, less often, by depth electrodes. Strip and/or grid electrodes are laid under the dura subsequently to a small craniotomy, while depth electrodes are placed stereotactically by means of a small craniotomy [120, 148, 149, 216].
The accuracy of invasive electrodes depends not only on the type used but also on the cause of epilepsy and seizure origin. Spencer and Lee analyzed the accuracy of different electrodes in 53 patients with different types and causes of epilepsy (Table 4) [219]. In their study, localization accuracy for lesional and neocortical (in particular frontal) cases was higher with grids than with strip electrodes. The latter, however, localized seizure origin more precisely in nonlesional and mesial cases. These findings are in agreement with numerous other studies [176, 215, 216, 222].
The rate of morbidity when using intracranial electrodes is low (1–2%) and largely restricted to patients with wound infections or, more rarely, hematoma [57, 60, 215, 218]. Due to intracranial subdural electrodes and depth electrodes, the extratemporal origin of seizure can be determined in approximately 70–80% of implanted patients, who can then be considered for operation. Invasive re-evaluation is occasionally necessary after an unsuccessful first evaluation [204].
Amobarbital (Wada) test
Since 1960, intracarotid amobarbital testing (Wada test) has been part of the standard preoperative evaluation of candidates for epilepsy surgery in order to lateralize language and memory function [247]. The intra-arterial injection of sodium amobarbital into the carotid artery (global Wada test) or, more selectively, into the anterior choroidal artery (selective or superselective Wada test) may provide further information on dysfunctional hemispheres so that the risk of postoperative memory deficits can be assessed [223, 247, 262]. While the Wada test is a crucial tool in the presurgical evaluation of temporal lobe epilepsy (particularly when the operation is planned on the speech-dominant side), it does not play an important role in extratemporal epilepsy [101].
Surgical treatment of medically refractory epilepsies (phase III)
If a patient has undergone presurgical evaluation and, having met the criteria detailed above, is still a candidate for epilepsy surgery, the optimal neurosurgical intervention should be discussed in an interdisciplinary seizure conference including epileptologists, neuropsychologists, psychiatrists, and neurosurgeons. Epilepsy surgery interventions are generally divided into the following categories according to indications, underlying pathology, and method and extent of resection:
-
1.
Procedures are classified as causal or palliative. Causal operations (e.g., anterior 2/3 temporal lobectomy or resection of cavernous malformations) have the purpose of removing an epileptic focus so that seizure-free outcome can be achieved. Palliative procedures (e.g., callosal section), on the other hand, aim at either an interruption of seizure spread pathways or resection of secondary epileptogenic pacemakers. Surgical outcome is understandably not as good with palliative operations as with causal operations.
-
2.
On the basis of radiologic findings, a distinction is also made between lesional and nonlesional interventions. The former apply for the removal of radiologically detected structural lesions (so-called lesionectomies of, e.g., tumors, cavernous malformations, etc.), while the latter are performed in patients whose MRIs are normal or show only nonspecific pathology.
-
3.
Furthermore, epilepsy operations may be classified as either resective or nonresective (disconnective). In resective intervention, a variable amount of cerebral tissue is removed (as in lesionectomies or amygdalohippocampectomies). Nonresective (disconnective) operations include callosotomy and multiple subpial transection. The implantation of a vagal nerve stimulator is also a type of nonresective surgery.
-
4.
Finally, procedures are divided into those strictly limited to the removal of epileptogenic foci (individually tailored resections such as partial cortical frontal resection) and those involving more extensive, standard resection (e.g., standard anterior 2/3 temporal lobectomy) independent of the size of the epileptogenic focus. One clearly prefers to minimize the volume of brain resected—even though this means a few patients will require second operation because of unsatisfactory seizure outcome. The more common neurosurgical procedures for epilepsy and their associated seizure outcomes are discussed individually below.
Temporal lobectomy
Removal of the anterior temporal lobe is the most frequent and most successful type of epilepsy surgery. The most common version of this operation is standard anterior temporal lobectomy, which is, however, difficult to define because of subtle variations from center to center. Some neurosurgeons prefer the Falconer approach, which consists of en bloc resection of the temporal lobe (usually 4.5–6.5 cm from the temporal pole, depending on the side of operation, i.e., a smaller resection is performed on the speech-dominant hemisphere) including the amygdala and hippocampus [35, 59, 241, 248] (Fig. 1). Other surgeons remove variable amounts of the temporal lobe on the basis of intraoperative electrocorticographic findings [68, 237, 238].
The success rate for seizure control following standardized temporal lobectomy performed for strict indications is up to 80% [51, 52, 94, 95, 210, 212]. Surgical outcome in patients with neocortical temporal lesions may be complicated by the presence of dual pathology in as many as 30% [24, 116, 119]. Major operative complications from standard temporal lobectomy are rare. More common complications include subquadrantic or quadrantic visual field deficits (in >50% of patients), supraquadrantic or hemianopic visual field deficits (2–4%), transient or persistent hemiparesis (4% and 12%, respectively), infections (meningitis or abscess) and epidural hematoma (<0.5% each), transient III or IV nerve palsy (<0.1%), transient anomia for 4–7 days (>20%), persistent dysphasia (1–3%), global memory deficits (1%), and transient psychosis or depression (2–20%) [159, 160]. The mortality of standard anterior temporal lobectomy is <1% [159, 160].
Selective amygdalohippocampectomy
Seizure discharges in the most common form of focal epilepsies, mesial temporal lobe epilepsy, arise almost exclusively from the amygdala, the hippocampus, and, to some extent, the parahippocampal gyrus [256]. This fact immediately suggests that a resection limited to these structures might abolish the seizures. The first selective resections of these mesial temporal lobe structures go back to Paolo Niemeyer [145]. In 1958, he reported on the selective removal of the amygdala and hippocampus through a transcortical approach. Although the results were promising, this method of operation fell into oblivion because of other developments.
Then, in 1975, selective amygdalohippocampectomy by a trans-sylvian approach was developed in Zurich by the neurosurgeon Yasargil and the epileptologist Bemoulli, whose initial work was continued by Wieser [255] (Fig. 1). In this procedure, after removal of the amygdala, the anterior part of the hippocampus and part of the parahippocampal gyrus are removed. In addition to these mesial structures, the most important afferent pathway (entorhinal area) and the pathways of seizure spread (uncinate fasciculus, anterior commissure) are interrupted, which also contributes to the good postoperative results [200]. In a retrospective study of 369 patients with selective amygdalohippocampectomy followed up for at least 12 months (average 85.2), 67% were seizure-free or had auras only. A further 11% had no more than one or two seizures per year, and 15% showed reductions in seizure frequency of at least 90%; however, 8% obtained no substantial improvement [264]. Similar results have been reported in other studies analyzing seizure outcome after amygdalohippocampectomy with different approaches [85, 108, 150, 155, 156, 210, 278, 282]. Factors correlating with good outcome were the presence of a structural lesion (particularly severe hippocampus sclerosis), history of febrile convulsions, extensive resection of the hippocampus and especially of the parahippocampal gyrus, presurgical lack of contralateral epileptogenic foci, brief seizures (particularly with origin in the most anterior part of the mesial structures), and—in ictal discharges with contralateral propagation—late propagation to the contralateral hemisphere [199, 200, 259].
Extratemporal resections
In contrast to the commonly applied, standard, anterior 2/3 temporal lobectomy discussed above, complete removal of the frontal, parietal, or occipital lobes is nowadays hardly ever carried out (Fig. 1). The current surgical treatment of extratemporal epilepsy mainly includes partial cortical resection of the frontal, parietal, or occipital lobe and is limited to the epileptogenic focus [166].
In a large series of 75 patients operated on for frontal lobe epilepsy, 64% were postsurgically seizure-free, 12% had only rare seizures, 16% showed worthwhile reductions in seizure frequency, and 12% showed no worthwhile reduction [195]. The 26 patients with tumors (only two malignant) as the cause of seizures had the best results (81% seizure-free). In contrast, only 50% of the patients without lesions became seizure-free. Similar results have been reported by other centers [61, 62, 144, 187, 208, 253, 283].
In 39 patients with parietal lobe epilepsy surgery, 52% were postsurgically seizure-free and 30% had seizure frequencies reduced more than 90% [151]. Complications included transient sensorimotor deficits or mild aphasic syndromes (in 20% of the patients), permanent sensorimotor deficits (in 12%), and worsening of preoperative sensory deficits (in 15%) [189, 190]. Rare complications following parietal lobe surgery are transient lower quadrantal visual field deficits and right-left disorientation and a partial Gerstmann’s syndrome [189, 190].
In 30 patients with occipital lobe epilepsy, 71% were seizure-free after the operation, and 18% had seizure reduction of more than 90% [151]. Visual field deficit is the major complication following occipital lobe surgery [186]. Homonymous hemianopsia was present in 76% of cases, over two thirds of whom had partial visual field deficits preoperatively [186].
Compared with nonlesional cases, lesionectomies have a greater likelihood of producing seizure freedom, in particular if they include margin resection [16, 26, 203]. However, epilepsy surgery in patients with negative MR scans (nonlesional cases) may also yield good seizure outcome. In a study by Siegel et al., 20 of 25 patients with nonlesional neocortical, mainly extratemporal epilepsy became postsurgically seizure-free or had only rare seizures following cortectomy [205].
Callosotomy
Transection of the corpus callosum is probably the best example of a palliative operation. Callosotomy is intended to interrupt the pathways of seizure spread or interhemispheric synchronization [15]. Van Wagenen made the observation that epileptic patients who subsequently sustained a stroke involving the corpus callosum often had improvement in their seizure disorders; and in 1940 he and Herren reported a series in which the corpus callosum was intentionally divided for the treatment of intractable epilepsy [243]. In the early 1960s, Bogen reported a small series of similarly operated patients with encouraging results [12, 13, 14], and Luessenhop described comparable success in three of four children [123, 124]. In 1971, Wilson chose this procedure as an alternative to hemispherectomy in a 9-year-old boy with infantile hemiplegia and began compiling a series of 20 patients that ultimately revealed the efficacy of the procedure, warranting its wider application [74, 169, 271, 272, 273, 274, 275].
Callosal section may either be limited to the anterior half (or 2/3) of the corpus callosum or include some or all of the posterior half. Total callosotomy is rarely performed (in one- or two-stage operation) to avoid complications such as mutism, apraxia, and frontal lobe dysfunction [179, 180]. In the early years of callosotomy, division of additional structures important for interhemispheric seizure propagation, such as the anterior commissure, fornix, and posterior hippocampal commissure, was performed in the same operation [179, 180]. The indications for this palliative intervention are infantile hemiplegia, Lennox-Gastaut syndrome, Rasmussen’s encephalitis, and multifocal bilateral epilepsy [65, 66, 67, 179, 180, 211, 214, 280].
As far as seizure types, status epilepticus and drop attacks respond especially well to callosotomy. Our own study of 104 callosotomy patients at the Dartmouth-Hitchcock Medical Center, New Hampshire, USA found that 66% of patients with status epilepticus and 52% of those with drop attacks prior to surgery had none after the callosotomy [179, 180]. Complications of callosotomy included acute disconnection syndrome lasting days to weeks (in 90% of patients), sensory disconnection (>90%), split brain syndrome (30% transitory and 3% persistent), paresis or apraxia of the left arm or leg (about 15%), disorder of written language and/or mutism (6–15%), and cognitive deficits (about 10%) [159].
Hemispherectomy and multilobar resections
Further therapeutic options in patients with severe drug-resistant epilepsy and large multilobar or hemispheric epileptogenic lesions include multilobar resection and hemispherectomy. The latter is a surgical procedure in which a cerebral hemisphere is either anatomically removed or made nonfunctional by disconnection. Anatomic hemispherectomy involves a complete hemispheric corticectomy with or without removal of the basal ganglia, sparing both the hypothalamus and the diencephalon [109, 132, 245, 254, 276] (Fig. 1). Anatomic hemispherectomy has been performed both as a single operation and in multiple sittings [36, 70, 109, 146, 167]. After superficial cerebral hemosiderosis was recognized as a late, severe complication of anatomic hemispherectomy, other surgical techniques were developed [1, 39, 89, 165, 167, 244, 245, 277] (Table 5).
At present, porencephalic cysts and hemimegalencephaly, large cortical dysplasias, Rasmussen’s encephalitis, and the Sturge Weber syndrome are considered to be indications for multilobar resection and hemispherectomy. Furthermore, the latter is almost exclusively performed in patients who already have major preoperative deficits such as hemiplegia. In this subset of patients, seizure freedom can be achieved in over 90–95% of cases [245, 246, 277]. A series of 68 patients with hemispherectomies yielded very good results: 80% were postsurgically seizure-free (more than half no longer needed antiepileptic drugs) and 14% had seizure reduction of more than 90%. Despite these excellent results, the decision to perform such large resections should only be made cautiously. Furthermore, extensive presurgical evaluation must be carried out to lessen the likelihood of major postoperative deficit (e.g., pronounced hemiplegia).
Multiple subpial transection
Multiple subpial transection (MST) is a relatively new palliative surgical technique developed for medically refractory partial epilepsy emanating from an eloquent region such as the speech area or motor sensory cortex [88, 139, 140, 143]. The technique of MST requires a special knife-like instrument with which tangential intracortical fibers mediating seizure propagation are interrupted, while vertical afferent and efferent connections subserving essential cortical functions are preserved [139]. The MST can also be combined with cortical resection. In a series of 100 patients with MST, 48% were postsurgically seizure-free, 13% had only rare seizures, 20% had worthwhile improvement in their seizure situations, and 19% had no benefit. Other studies yielded similar results [88, 141, 143, 185, 220]. In 16 patients with Landau-Kleffner syndrome treated with MST and resective surgery, 75% became seizure-free and 44% had recovered age-appropriate language [143]. Predictors for good seizure outcome were the diagnosis of Landau-Kleffner syndrome and the combination of MST with simultaneous partial cortical resection [209, 281]. In a series of 97 patients, permanent complications occurred in 4% and included basal ganglia hemorrhage in one patient, hemorrhagic infarct with dysphasia in another, infarction of the precentral region in a third, and foot drop in a fourth. Transient complications occurred in 7% and included mild contralateral weakness in five patients, cortical sensory loss in one, and dyslexia in another [142].
Vagal nerve stimulation
The rationale of electric stimulation of the vagal nerve (VNS) for palliative epilepsy therapy is based on findings from animal experiments. Electric impulses are generated in a stimulator device, similar to a pacemaker, which is implanted underneath the clavicle and conducted through a wire electrode directly onto the vagal nerve in the neck [133, 267]. The VNS is indicated in patients with medically refractory partial epilepsy who are not good candidates for resective surgery. A large, multicenter study found that 37–43% of the patients had more than 50% reduction in seizures with VNS [30, 38, 133]. This technique seems to be particularly effective after prior callosotomy (Roberts and Siegel, unpublished data). Complications of VNS included voice alteration, increased coughing, paresthesia, dyspnea, dyspepsia, and laryngismus [6, 73].
Gamma knife radiosurgery
Stereotaxic radiosurgery using the gamma knife has been performed for the last 40 years in the treatment of vascular malformations and brain tumors. Recently, radiosurgery has also made an entrance in epilepsy surgery, particularly for mesial temporal lobe epilepsy syndrome. In the latter, gamma knife surgery delivers a focused dose of radiation to the mesial temporal structures. A recent study analyzed 25 patients treated with the gamma knife instead of open neurosurgical amygdalohippocampectomy [173]. Of the 16 patients with sufficient follow-up observation, 13 (81%) became seizure-free.
While gamma knife treatment might be useful in patients who would otherwise undergo mesial temporal lobe resection, it does not yet play an important role in the treatment of extratemporal epilepsy. Today, the gamma knife probably has its major application in the treatment of hypothalamic hamartoma, in which the postsurgical results of a multicentric study are very promising: 80% seizure freedom or improvement [173]. While the advantage of gamma knife—avoiding craniotomy—is obvious, its problem lies in the fact that seizure freedom or reduction usually does not set in till nearly a year after the procedure. This obviously makes it more difficult for the treating physician to recommend, as he must offer patients the choice between operation with usually instant reduction of or freedom from seizures and therapy avoiding craniotomy but after which the seizures persist for at least several months.
Conclusion
Thanks to today’s modern imaging examination techniques and especially to the common use of intracranial electrodes for localizing seizure foci, more and more patients with partial epilepsy can be treated microsurgically. The results of such neurosurgical therapies are very good, particularly with mesial temporal lobe epilepsy. In recent years, good results (60–70% seizure freedom) have also been achieved in extratemporal epilepsy surgery, so that such procedures can now be recommended for carefully selected patients.
References
Adams CBT (1983) Hemispherectomy—a modification. JNNP 46:617–619
Annegers JF, Hauser WA, Elveback LR (1979) Remission of seizures and relapse in patients with epilepsy. Epilepsia 20:729–737
Barth DS, Sutherling W, Engel J Jr, Beatty J (1982) Neuromagnetic localization of epileptiform spike activity in the human brain. Science 218:891–894
Barth DS, Sutherling W Engel J Jr, Beatty J (1984) Neuromagnetic evidence of spatially distributed sources underlying epileptiform spikes in the human brain. Science 223:293–296
Bengzon AR, Rasmussen T, Gloor P, Dussault J, Stephens M (1968) Prognostic factors in the surgical treatment of temporal lobe epileptics. Neurology 18:717–731
Ben-Menachem E, Manon-Espaillat R, Ristanovic R, et al (1994) Vagus nerve stimulation for treatment of partial seizures. I. A controlled study of effect on seizures. Epilepsia 35:616–626
Bergin PS, Fish DR, Shorvon SD, Oatridge A, Desouza NM, Bydder GM (1995) Magnetic resonance imaging in partial epilepsy—additional abnormalities shown with the fluid attenuated inversion-recovery (flair) pulse sequence. JNNP 58:439–443
Berkovic SF, Andermann F, Olivier A, Ethier R, Melanson D, Robitaille Y, Kuzniecky R, Peters T, Feindel W (1991) Hippocampal sclerosis in temporal-lobe epilepsy demonstrated by magnetic-resonance-imaging. Ann Neurol 29:175–182
Berkovic SF, Duncan JS, Barkovich A, Cascino G, Chiron C, Engel J, Gadian D, Jackson G, Kuzniecky R, McLachlan R, Meencke H, Palmini A, Reynolds EH, Sadzot B, Stefan H, Theodore W, Wolf P (1997) ILAE commission neuroimaging recommendations for neuroimaging of patients with epilepsy. Epilepsia 38:1–2
Birken DL, Oldendorf WH (1989) N-acetyl-L-aspartic acid: a literature review of a compound prominent in 1H-NMR spectroscopic studies of brain. Neurosci Biobehav Rev 13:23–31
Blume WT, Wiebe S (2000) Occipital lobe epilepsy. In: Williamson PD, Siegel AM, Roberts DW, Thadani VM, Gazzaniga MS (eds) Neocortical epilepsy. Advances in neurology, vol 84. Lippincott, Williams and Wilkins, New York, pp 173–188
Bogen JE, Vogel PJ (1962) Cerebral commissurotomy in man: preliminary case report. Bull Los Angeles Neurol Soc 27:169–172
Bogen JE, Fisher ED, Vogel PJ (1965) Cerebral commissurotomy: a second case report. JAMA 194:1328–1329
Bogen JE, Sperry RW, Vogel PJ (1969) Addendum: commissural section and propagation of seizures. In: Jasper HH, Ward Jr AA, Pope A (eds) Basic mechanisms of the epilepsies. Little, Brown, and Company, Boston, p 439
Bogen JE (1995) Some historical aspects of callosotomy for epilepsy. In: Reeves A, Roberts DW (eds) Epilepsy and the corpus callosum, 2nd edn. Plenum, New York, pp 107–122
Boon PA, Williamson PD, Fried I, Spencer DD, Novelly RA, Spencer SS, Mattson RH (1991) Intracranial, intraaxial, space-occupying lesions in patients with intractable partial seizures: an anatomoclinical, neuropsychological, and surgical correlation. Epilepsia 32:467–475
Boon P, Chauvel P, Pohlmann-Eden B, Otoul C, Wroe S (2002) Dose-response effect of levetiracetam 1000 and 2000 mg/day in partial epilepsy. Epilepsy Res 48:77–89
Boon P, D’Have M, Van Walleghem P, Michielsen G, Vonck K, Caemaert J, De Reuck J (2002) Direct medical costs of refractory epilepsy incurred by three different treatment modalities: a prospective assessment. Epilepsia 43:96–102
Bornstein RA (1985) Normative data on intermanual differences on three tests of motor performances. J Clin Exp Neuropsychology 8:12–20
Brorson LO, Wranne L (1987) Long-term prognosis in childhood epilepsy—survival and seizure prognosis. Epilepsia 28:324–330
Buck A, Frey LD, Bläuenstein P, Krämer G, Siegel AM, Weber B, Schubiger, PA, Wieser HG (1998) Monoamineoxidase B single-photon emission tomography with [123I]Ro 43–0463: imaging in volunteers and patients with temporal lobe epilepsy. Eur J Nucl Med 25:464–470
Cascino GD, Hirschorn KA, Jack CR, Sharbrough FW (1989) Gadolinium-DPTA-enhanced magnetic resonance imaging in intractable partial epilepsy. Neurology 39:1115–1118
Cascino GD, Jack CR Jr, Parisi JE, Sharbrough FW, Hirschorn KA, Meyer FB, Marsh WR, Obrien PC (1991) Magnetic resonance imaging-based volume studies in temporal lobe epilepsy: pathological correlations. Ann Neurol 30:31–36
Cascino GD, Clifford RJ Jr, Parisi JE, Sharbrough FW, Schreiber CP, Kelly PJ, Trenerry MR (1993) Operative strategy in patients with MRI-identified dual pathology and temporal lobe epilepsy. Epilepsy Res 14:175–182
Cascino GD, Hulihan JF, Sharbrough FW, Kelly PJ (1993) Parietal lobe lesional epilepsy: electroclinical correlation and operative outcome. Epilepsia 34:522–527
Cascino GD, Sharbrough FW, Trenerry MR, Marsh WR, Kelly PJ, So E (1994) Extratemporal cortical resections and lesionectomies for partial epilepsy: complications of surgical treatment. Epilepsia 35:1085–1090
Cascino GD (1998) Structural brain imaging. In: Engel J Jr, Pedley TA (eds) Epilepsy. A comprehensive textbook. Lippincott-Raven, Philadelphia, pp 937–946
Castillo M, Kwock L, Mukherji SK (1996) Clinical applications in proton MR spectroscopy. Am J Neuroradiol 17:1–15
Chabolla DR, Cascino GD (1996) Interpretation of extracranial EEG. In: Wyllie E (ed) The treatment of epilepsy: principles and practice. Williams and Wilkins, Baltimore, pp 264–279
Chadwick D (2001) Vagal-nerve stimulation for epilepsy. Lancet 357:1726–1727
US Department of Health, Education, and Welfare (1978) Commission for the control of epilepsy and its consequences: plan for nationwide action on epilepsy. National Institutes of Health issue no 78–311:314–343
Commission on Neurosurgery of Epilepsy (1997) ILAE commission report: a global survey on epilepsy surgery, 1980–1990: a report by the Commission on Neurosurgery of Epilepsy, The International League Against Epilepsy. Epilepsia 38:249–255
Constantinidis I (2000) MRS methodology. In: Henry TR, Duncan JS, Berkovic SF (eds) Functional imaging in the epilepsies. Advances in neurology, vol 83. Lippincott, Williams and Wilkins, New York, pp 235–246
Cook M, Sisodiya SM (1996) Magnetic resonance imaging evaluation for epilepsy surgery. In: Shorvon S, Dreifuss F, Fish D, Thomas D (eds) The treatment of epilepsy. Marston, Oxford, pp 589–604
Crandall PH (1987) Cortical resections. In: Engel J Jr (ed) Surgical treatment of the epilepsies. Raven, New York, pp 377–404
Dandy WE (1928) Removal of right cerebral hemisphere for certain tumors with hemiplegia. JAMA 90:823–825
de Bittencourt PRM, Araujo JC, Leite PJM, Moro MS, Pinna ER, Sandmann MC (1997) Epilepsy surgery without invasive EEG—early results of a new program. Arq Neuro-Psiquiat 55:542–546
De Giorgio CM, Schachter SC, Handforth A, Salinsky M, Thompson J, Uthman B, Reed R, Collins S, Tecoma E, Morris GL, Vaughn B, Naritoku DK, Henry T, Labar D, Gilmartin R, Labiner D, Osorio I, Ristanovic R, Jones J, Murphy J, Ney G, Wheless J, Lewis P, Heck C (2000) Prospective long-term study of vagus nerve stimulation for the treatment of refractory seizures. Epilepsia 41:1195–1200
Delalande O, Pinard JM, Basdevant C, Gauthe M, Plouin P, Dulac O (1992) Hemispherotomy: a new procedure for central disconnection. Epilepsia 33 [Suppl 3]:99–100
Devinsky O, Pacia S (1993) Epilepsy surgery. In: Devinsky O (ed) Epilepsy I: diagnosis and treatment. Neurologic clinic. Saunders, Philadelphia, pp 951–972
Devous MD, Thisted RA, Morgan GF, Leroy RF, Rowe CC (1998) SPECT brain imaging in epilepsy: a meta-analysis. J Nucl Med 39:285–293
Diehl B, Najm I, Ruggieri P, Foldvary N, Mohamed A, Tkach J, Morris H, Barnett G, Fisher E, Duda J, Luders HO (1999) Postictal diffusion-weighted imaging in a case with lesional epilepsy. Epilepsia 40:1667–1671
Djordjevic J, Piazzini A, Jones-Gotman M (1997) Two scoring systems for the Wisconsin Card Sorting Test: same or different measures? Epilepsia 38 [Suppl 8]:163
Dreifuss FE (1987) Goals of surgery for epilepsy. In: Engel J Jr (ed) Surgical treatment of the epilepsies. Raven, New York, pp 31–49
Duncan R, Patterson J, Roberts R, Hadley DM, Bone I (1993) Ictal postictal SPECT in the presurgical localization of complex partial seizures. JNNP 56:141–148
Duncan R (1997) The clinical use of SPECT in focal epilepsy. Epilepsia 38 [Suppl 10]:39–41
Duncan R, Biraben A, Patterson J, Hadley D, Bernard AM, Lecloirec J, Vignal JP, Chauvel P (1997) Ictal single photon emission computed tomography in occipital lobe seizures. Epilepsia 38:839–843
Ebersole JS (1997) Magnetencephalography/magnetic source imaging in the assessment of patients with epilepsy. Epilepsia 38 [Suppl 4]:S1–S5
Ebersole JS, Smith JR (1995) MEG spike modeling differentiates baso-mesial from lateral cortical temporal epilepsy. Electroencephalogr Clin Neurophysiol 95:20P
Eliashiv SD, Velasco AL, Wilson CL et al (1995) Magnetic source imaging as a predictor of invasive-electrode-defined irritative and ictal onset zones. Electroencephalogr Clin Neurophysiol 95:20P
Engel J Jr (1987) Outcome with respect to epileptic seizures. In: Engel J Jr (ed) Surgical treatment of the epilepsies. Raven, New York, pp 553–571
Engel J Jr (1992) Recent advances in surgical treatment of temporal lobe epilepsy. Acta Neurol Scand 86 [Suppl 5]:71–80
Engel J Jr, Shewmon DA (1993) Overview: who should be considered a surgical candidate? In: Engel J Jr (ed) Surgical treatment of the epilepsies, 2nd edn. Raven, New York, pp 23–34
Engel J Jr, Van Ness PC, Rasmussen TB, Ojemann LM (1993) Outcome with respect to epileptic seizures. In: Engel J Jr (ed) Surgical treatment of the epilepsies, 2nd edn. Raven, New York, pp 609–621
Engel J Jr, Williamson PD, Wieser HG (1997) Mesial temporal lobe epilepsy. In: Engel J Jr, Pedley J (eds) Epilepsy: a comprehensive textbook. Raven, New York, pp 2417–2426
Engel J Jr, Wieser HG, Spencer D (1998) Overview. In: Engel J Jr, Pedley TA, (eds) Epilepsy. A comprehensive textbook. Lippincott-Raven, Philadelphia, pp 1673–1676
Espinosa J, Olivier A, Andermann F, Quesney F, Dubeau F, Savard G (1994) Morbidity of chronic recording with intracranial depth electrodes in 170 patients. Stereotact Funct Neurosurg 63:63
Falconer M, Taylor D (1968) Surgical treatment of drug resistant epilepsy due to mesial temporal sclerosis. Arch Neurol 19:353–361
Falconer MA (1971) Anterior temporal lobectomy for epilepsy. In: Logue V (ed) Operative surgery. Neurosurgery, vol 14. Butterworths, London, pp 142–149
Fernandez G, Hufnagel A, Van Roost D, Helmstaedter C, Wolf HK, Zentner J, Schramm J, Elger CE (1997) Safety of intrahippocampal depth electrodes for presurgical evaluation of patients with intractable epilepsy. Epilepsia 38:922–929
Ferrier CH, Engelsman J, Alarcon G, Binnie CD, Polkey CE (1999) Prognostic factors in presurgical assessment of frontal lobe epilepsy. JNNP 66:350–356
Fish DR, Smith SJ, Quesney F, Andermann F, Rasmussen T (1991) Surgical treatment of children with medically intractable frontal or temporal lobe epilepsy: results and highlights of 40 years’ experience. Epilepsia 34:244–247
Forster BB, MacKay AL, Whittall KP, Kiehl KA, Smith AM, Hare RD, Liddle PF (1998) Functional magnetic resonance imaging: the basics of blood-oxygen-level dependent (BOLD) imaging. Can Assoc Radiol J 49:320–329
Gaillard WD, Bookheimer SY, Cohen M (2000) The use of fMRI in neocortical epilepsy. In: Williamson PD, Siegel AM, Roberts DW, Thadani VM, Gazzaniga MS (eds) Neocortical epilepsy. Advances in neurology, vol 84. Lippincott, Williams and Wilkins, New York, pp 391–404
Gates JR, Leppik IE, Yap J, Gumnit RJ (1984) Corpus callosotomy: clinical and electroencephalographic effects. Epilepsia 25:308–316
Gates JR, Mireles R, Maxwell R, Sharbrough F, Forbes G (1986) Magnetic resonance imaging, electroencephalogram and selected neuropsychological testing in staged corpus callosotomy. Arch Neurol 43:1188–1191
Gates JR, De Paola L (1996) Corpus callosum section. In: Shorvon S, Dreifuss F, Fish D, Thomas D (eds) The treatment of epilepsy. Marston, Oxford, pp 722–738
Gloor P (1975) Contributions of electroencephalography and electrocorticography to the neurosurgical treatment of the epilepsies. In: Purpura DP, Penry JK, Walter RD (eds) Advances in neurology, vol 8. Raven, New York, pp 59–105
Grant DA, Berg GA (1948) A behavioral analysis of degree of reinforcement and ease of shifting to new responses in a Weigl-type card-sorting problem. J Experimental Psychol 38:404–411
Griffith HB (1967) Cerebral hemispherectomy for infantile hemiplegia in the light of late results. Ann Roy Coll Surg Engl 41:183–201
Guerreiro C, Cendes F, Li L, Jones-Gotman M, Andermann F, Dubeau F, Piazzini A, Feindel W (1999) Clinical patterns of patients with temporal lobe epilepsy and pure amygdalar atrophy. Epilepsia 40:453–461
Hajek M, Siegel AM, Haldemann R, von Schulthess GK, Wieser HG (1991) Value of HM-PAO SPECT in the selective temporal lobe surgery for epilepsy. J Epilepsy 4:43–51
Handforth A, DeGiorgio CM, Schachter SC, Uthman BM, Naritoku DK, Tecoma ES, Henry TR, Collins SD, Vaughn BV, Gilmartin RC, Labar DR, Morris GL, Salinsky MC, Osorio I, Ristanovic RK, Labiner DM, Jones JC, Murphy JV, Ney GC, Wheless JW (1998) Vagus nerve stimulation therapy for partial onset seizures: a randomized active-control trial. Neurology 51:48–55
Harbaugh RE, Wilson DH, Reeves AG, Gazzaniga MS (1983) Forebrain commissurotomy for epilepsy: review of 20 consecutive cases. Acta Neurochir 68:263–275
Hartshorne MF (1995) Positron emission tomography. In: Orrison WW Jr, Lewine JD, Sanders JA, Hartshorne MF (eds) Functional brain imaging. Mosby Year Book 187, St Louis, p 212
Hartshorne MF (1995) Single photon emission computed tomography. In: Orrison WW Jr, Lewine JD, Sanders JA, Hartshorne MF (eds) Functional brain imaging. Mosby Year Book 187, St Louis, pp 213–238
Harvey AS, Hopkins IJ, Bowe JM, Cook DJ, Shield LK, Berkovic SF (1993) Frontal lobe epilepsy: clinical seizure characteristics and localization with ictal 99mTc-HMPAO SPECT. Neurology 43:1966–1980
Hauser WA, Kurland LT (1975) The epidemiology of epilepsy in Rochester, Minnesota: 1935 through 1967. Epilepsia 16:1–66
Hauser WA, Annegers JF, Kurland LT (1991) Prevalence of epilepsy in Rochester, Minnesota: 1940–1980. Epilepsia 32:429–445
Hauser WA (1992) The natural history of drug resistant epilepsy: epidemiologic considerations. In: Theodore WH (ed) Surgical treatment of epilepsy. (Epilepsy Res Suppl 5). Elsevier, Amsterdam, pp 25–28
Hauser WA (1998) Incidence and prevalence. In: Engel J, Pedley TA (eds) Epilepsy. A comprehensive textbook. Lippincott-Raven, Philadelphia, pp 47–57
Henry TR, Chugani HT, Abou-Khalil BW, Theodore WH, Swartz BE (1993) Positron emission tomography In: Engel J Jr (ed) Surgical treatment of the epilepsies, 2nd edn. Raven, New York, pp 211–232
Ho SS, Berkovic SF, Newton MR, Austin MC, McKay WJ, Bladin PF (1994) Parietal lobe epilepsy: clinical features and seizure localization by ictal SPECT. Neurology 44:2277–2284
Ho SS, Berkovic SF, McKay WJ, Kalnins RM, Bladin PF (1996) Temporal lobe epilepsy subtypes: differential patterns of cerebral perfusion on ictal SPECT. Epilepsia 37:788–795
Hori T, Tabuchi S, Kurosaki M, Kondo S, Takenobu A, Watanabe T (1993) Subtemporal amygdalohippocampectomy for treating medically intractable temporal lobe epilepsy. Neurosurgery 33:50–56
Howe FA, Maxwell RJ, Saunders DE, Brown MM, Griffiths JR (1993) Proton spectroscopy in vivo. Magn Reson Q 9:31–59
Howseman AM, Bowtell RW (1999) Functional magnetic resonance imaging: imaging techniques and contrast mechanisms. Philos Trans R Soc Lond Biol Sci 354:1179–1194
Hufnagel A, Zentner J, Fernandez G, Wolf HK, Schramm J, Elger CE (1997) Multiple subpial transection for control of epileptic seizures: effectiveness and safety. Epilepsia 38:678–688
Ignelzi RJ, Bucy PC (1968) Cerebral hemidecortication in the treatment of infantile cerebral hemiatrophy. J Nerv Ment Dis 147:14–30
Jack CR Jr, Sharbrough FW, Cascino GD (1992) MRI-based hippocampal volumetry: correlation with outcome after temporal lobectomy. Ann Neurol 31:138–146
Jack CR, Mullan BP, Sharbrough FW, Cascino GD, Hauser MF, Krecke KN, Luetmer PH, Trenerry MR, Obrien PC, Parisi JE (1994) Intractable nonlesional epilepsy of temporal-lobe origin—lateralization by interictal SPECT versus MRI. Neurology 44:829–836
Jackson GD, Berkovic SF, Tress BM (1990) Hippocampal sclerosis can be reliably detected by magnetic resonance imaging. Neurology 40:1869–1875
Jackson GD, Connelly A, Cross JH, Gordon I, Gadian DG (1994) Functional magnetic resonance imaging of focal seizures. Neurology 44:850–856
Jensen I (1975) Temporal lobe surgery around the world: results, complications, and mortality. Acta Neurol Scand 52:354–373
Jensen I (1976) Temporal lobe epilepsy: etiological factors and surgical results. Acta Neurol Scand 53:103–118.
Jobst BC, Siegel AM, Thadani VM, Roberts DW, Williamson PD (2000) Intractable seizures of frontal lobe origin: clinical characteristics, localizing signs and results of surgery. Epilepsia 41:1139–1152
Jones-Gotman M (1991) Localization of lesions by psychological testing. Epilepsia 32 [Suppl 5]: 41–52
Jones-Gotman M, Smith ML, Zatorre RJ (1993) Neuropsychological testing for localizing and lateralizing the epileptogenic region. In: Engel J Jr (ed) Surgical treatment of the epilepsies, 2nd edn. Raven, New York, pp 245–261
Jones-Gotman M, Zattorre RJ, Cendes F, Olivier A, Andermann F, Staunton H, McMackin D, Siegel AM, Wieser HG (1997) Contribution of medial versus lateral temporal-lobe structures to human odor identification. Brain 120:1845–1856
Jones-Gotman M, Zattorre RJ, Olivier A, Andermann F, Cendes F, Staunton H, McMackin D, Siegel AM, Wieser HG (1997) Learning and retention of words and designs following excision from medial or lateral temporal lobe structures. Neuropsychologia 35:963–973
Jones-Gotman M, Smith ML, Wieser HG (1998) Intra-arterial amobarbital procedure. In: Engel J Jr, Pedley TA (eds) Epilepsy. A comprehensive textbook. Lippincott-Raven, Philadelphia New York, pp 1767–1776
Jones-Gotman M (2000) Clinical neuropsychology and neocortical epilepsies. In: Williamson PD, Siegel AM, Roberts DW, Thadani VM, Gazzaniga MS (eds) Neocortical epilepsy. Advances in neurology, vol 84. Lippincott, Williams and Wilkins, New York, pp 457–462
Kaplan PW, Lesser RP (1996) Noninvasive EEG. In: Wyllie E (ed) The treatment of epilepsy: principles and practice. Williams and Wilkins, Baltimore MD, pp 976–987
King DW, Park YD, Smith JR, Wheless JW (2000) Magnetoencephalography in neocortical epilepsies. In: Williamson PD, Siegel AM, Roberts DW, Thadani VM, Gazzaniga MS (eds) Neocortical epilepsy. Advances in neurology, vol 84. Lippincott, Williams and Wilkins, New York, pp 415–423
Kilpatrick C, Cook M, Kaye A, Murphy M, Matkovic Z (1997) Noninvasive investigations successfully select patients for temporal lobe surgery. JNNP 63:327–333.
Knowlton R, Laxer K, Aminoff M, Roberts TPL, Wong STC, Rowley HA (1997) Magnetencephalography in partial epilepsy: clinical yield and localization accuracy. Ann Neurol 42:622–631
Krakow K, Woermann FG, Symms MR, Allen PJ, Lemieux L, Barker GJ, Duncan JS, Fish DR (1999) EEG-triggered functional MRI of interictal epileptiform activity in patients with partial seizures. Brain 122:1679–1688
Kratimenos GP, Pell MF, Thomas DG, Shorvon SD, Fish DR, Smith SJ (1992) Open stereotactic selective amygdalo-hippocampectomy for drug resistant epilepsy. Acta Neurochir 116:150–154
Krynauw RA (1950) Infantile hemiplegia treated by removing one cerebral hemisphere. JNNP 13:243–267
Kumlien E, Bergstrom M, Lilja A, Andersson J, Szekeres V, Westerberg CE, Westerberg G, Antoni G, Langstrom B (1995) Positron emission tomography with 11C-deuterium-deprenyl in temporal lobe epilepsy. Epilepsia 36:712–721
Lansberg MG, O’Brien MW, Norbash AM, Moseley ME, Morrell M, Albers GW (1999) MRI abnormalities associated with partial status epilepticus. Neurology 52:1021–1027
Laxer KD (2000) Magnetic resonance spectroscopy in neocortical epilepsies. In: Williamson PD, Siegel AM, Roberts DW, Thadani VM, Gazzaniga MS (eds) Neocortical epilepsy. Advances in neurology, vol 84. Lippincott, Williams and Wilkins, New York, pp 405–414
Lee DH, Gao FQ, Rogers JM, Gulka I, Mackenzie IRA, Parrent AG, Kubu CS, Munoz DG, McLachlan RS, Blume WT, Girvin JP (1998) MR in temporal lobe epilepsy: analysis with pathologic confirmation. Am J Neuroradiol 19:19–27
Lencz T, McCarthy G, Bronen RA, Scott TM, Inserni JA, Sass KJ, Novelly RA, Kim JH, Spencer DD (1992) Quantitative magnetic resonance imaging in temporal lobe epilepsy: relationship to neuropathology and neuropsychological function. Ann Neurol 31:629–637
Leppik IE (2002) Three new drugs for epilepsy: levetiracetam, oxcarbazepine, and zonisamide. J Child Neurol 17: S53–S57
Lévesque MF, Nakasato N, Vinters HV, Babb TL (1991) Surgical treatment of limbic epilepsy associated with extrahippocampal lesions: the problem of dual pathology. J Neurosurg 75:364–370
Lewis PJ, Siegel AH, Siegel AM, Studholme C, Sojkova J, Roberts DW, Thadani VM, Gilbert KL, Darcey TM, Williamson PD (2000) Does performing image registration and subtraction in ictal brain SPECT help localize neocortical seizures? J Nucl Med 41:1619–1626
Lezak MD (1995) Neuropsychological assessment, 3rd edn. Oxford University Press
Li LM, Cendes F, Andermann F, Watson C, Fish DR, Cook MJ, Dubeau F, Duncan JS, Shorvon SD, Berkovic SF, Free S, Olivier A, Harkness W, Arnold DL (1999) Surgical outcome in patients with epilepsy and dual pathology. Brain 122:799–805
Lüders H, Awad I, Burgess R, Wyllie E, Van Ness P (1992) Subdural electrodes in the presurgical evaluation for surgery of epilepsy. In: Theodore WH (ed) Surgical treatment of epilepsy. Elsevier, Amsterdam, pp 147–155
Lüders HO, Awad I (1992) Conceptual considerations. In: Lüders HO (ed) Epilepsy surgery. Raven, New York, pp 51–62
Lüders HO, Engel J Jr, Munari C (1993) General Principles. In: Engel J Jr (ed) Surgical treatment of the epilepsies, 2nd edn. Raven, New York, pp 137–153
Luessenhop AJ (1970) Interhemispheric commissurotomy: the split brain operation as an alternative to hemispherectomy for control of intractable seizures. Am Surg 36:265–268
Luessenhop AJ, de la Cruz TC, Fenichel GM (1970) Surgical disconnection of the cerebral hemispheres for intractable seizures. JAMA 213:1630–1636
Markand ON, Shen W, Park HM, Siddiqui AR, Wellman HH, Worth RM (1992) Single photon imaging computed-tomography (SPECT) for localization of epileptogenic focus in patients with intractable complex partial seizures. Epilepsy Res [Suppl 5]: 121–126
Marks DA, Katz A, Hoffer P, Spencer SS (1992) Localization of extratemporal epileptic foci during ictal single photon-emission computed-tomography. Ann Neurol 31:250–255
Mathieson G (1975) Pathology of temporal lobe foci. Adv Neurol 11:107–138
Mattson RH, Cramer JA, Collins JF, Smith DB, Delgado-Escueta AV, Browne TR, Williamson PD, Treiman DM, Mcnamara JO, McCutchen CB, Homan RW, Crill WE, Lubozynski MF, Rosenthal NP, Mayersdorf A (1985) Comparison of carbamazepine, phenobarbital, phenytoin and primidone in partial and secondarily generalized tonic-clonic seizures. N Engl J Med 313:145–152
Mattson RH (1992) Drug treatment of uncontrolled seizures. In: Theodore WH (ed) Surgical treatment of epilepsy. Elsevier, New York, pp 29–35
McInerney J, Siegel AM, Nordgren RE, Williamson PD, Thadani VM, Jobst BC, Reeves AG, Roberts DW (1999) Long-term seizure outcome following corpus callosotomy in preadolescent and adolescent children. Stereotact Funct Neurosurg 73:79–83
McKee PJW, Brodie MJ, Lamotrigine (1996) In: Shorvon S, Dreifuss F, Fish D, Thomas D (eds) The treatment of epilepsy. Marston, Oxford, pp 438–445
McKenzie KG (1938) The present status of a patient who had the right cerebral hemisphere removed. Proc Amer Med Ass Chicago 111:168
McLachlan RS (1997) Vagus nerve stimulation for intractable epilepsy: a review. J Clin Neurophysiol 14:358–368
Merlet I, Paetau R, Garcia-Larrea L, Uutela K, Granstrom ML, Mauguiere F (1997) Apparent asynchrony between interictal electric and magnetic spikes. Neuroreport 8:1071–1076
Milner B (1964) Some effects of frontal lobectomy in man. In: Warren JM, Akert K (eds) The frontal granular cortex and behavior. McGraw-Hill, New York, pp 313–334
Modena I, Ricci GB, Barbanera S, Leoni R, Romani GL, Carelli P (1982) Biomagnetic measurements of spontaneous brain activity in epileptic patients. Electroencephalogr Clin Neurophysiol 54:622–628
Moore GJ (1998) Proton magnetic resonance spectroscopy in pediatric neuroradiology. Pediatr Radiol 28:805–814
Morrell F, Hanbrey JW (1969) A new surgical technique for the treatment of focal cortical epilepsy. Electroenceph Clin Neurophysiol 26:120
Morrell F, Whisler W (1982) Multiple subpial transection for epilepsy eliminates seizures without destroying the function of the transected zone. Epilepsia 23:440
Morrell F, Whistler W, Bleck T (1989) Multiple subpial transection: a new approach to the surgical treatment of focal epilepsy. J Neurosurg 70:231–239
Morrell F, Whisler W (1993) Multiple subpial transection: technique, results and pitfalls. Jpn J Neurosurg 12:101–107
Morrell F, Whisler WW (1996) Multiple subpial transection. In: Shorvon S, Dreifuss F, Fish D, Thomas D (eds) The treatment of epilepsy. Marston, Oxford, pp 739–751
Morrell F, Kanner AM, de Toledo-Morell L, et al (1999) Multiple subpial transection. Adv Neurol 81:259–279
Mosewich RK, So EL, O’Brien TJ, Cascino GD, Sharbrough FW, Marsh WR, Meyer FB, Jack CR, O’Brien PC (2000) Factors predictive of the outcome of frontal lobe epilepsy surgery. Epilepsia 41:843–849
Niemeyer P (1958) The transventricular amygdalohippocampectomy in temporal lobe epilepsy. In: Baldwin M, Baily P (eds) Temporal lobe epilepsy. Thomas, Springfield, pp 461–482
Obrador A (1952) About the surgical technique of hemispherectomy in cases of cerebral hemiatrophy. Acta Neurochir 3:57–63
O’Brien TJ, So EL, Mullan BP, Hauser MF, Brinkmann BH, Jack CR, Cascino GD, Meyer FB, Sharbrough FW (1999) Subtraction SPECT co-registered to MRI improves postictal SPECT localization of seizure foci. Neurology 52:137–146
Olivier A, Gloor P, Quesney L, Andermann F (1983) The indications for and role of depth electrode recording in epilepsy. Appl Neurophysiol 46:33–36
Olivier A, Marchand E, Peters T, Tyler T (1987) Depth electrode implantation at the Montreal Neurological Institute and Hospital. In: Engel J Jr (ed) Surgical treatment of the epilepsies. Raven, New York, pp 595–602
Olivier A (2000) Transcortical selective amygdalohippocampectomy in temporal lobe epilepsy. Can J Neurol Sci 27 [Suppl 1]: 68–76
Olivier A, Bolding W (2000) Surgery of parietal and occipital lobe epilepsy. In: Williamson PD, Siegel AM, Roberts DW, Thadani VM, Gazzaniga MS (eds) Neocortical epilepsy. Advances in neurology, vol 84. Lippincott, Williams and Wilkins, New York, pp 533–576
Orrison WW Jr, Lewine JD, Sanders JA, Hartshorne MF (1995) Functional brain imaging. Mosby Year Book, St Louis
Osterrieth P (1944) Le test de copie d’une figure complexe. Arch Psychol 30:206–256
Oxbury S. Neuropsychological evaluation—children (1998) In: Engel J Jr, Pedley TA (eds) Epilepsy. A comprehensive textbook. Lippincott-Raven, Philadelphia, pp 989–1000
Park TS, Bourgeois BF, Silbergeld DL, Dodson WE (1996) Subtemporal transparahippocampal amygdalohippocampectomy for surgical treatment of mesial temporal lobe epilepsy. Technical note. J Neurosurg 85:1172–1176
Parrent AG, Blume WT (1999) Stereotactic amygdalohippocampotomy for the treatment of medial temporal lobe epilepsy. Epilepsia 40:1408–1416
Pedley TA (1990) Interictal epileptiform discharges: discriminating characteristics and clinical correlations. Am J EEG Technol 30:177–193
Perret E (1974) The left frontal lobe of man and the suppression of habitual responses in verbal categorical behaviour. Neuropsychologia 12:323–330
Pilcher WH, Rusynack WG (1993) Complications of epilepsy surgery. In: Silbergeld DL, Ojeman GA (eds) Epilepsy surgery. Neurosurgery Clinics of North America, Saunders, Philadelphia, pp 311–325
Pilcher WH, Roberts DW, Flanigin HHF, Crandall PH, Wieser HG, Ojemann GA, Peacock WJ (1993) Complications of epilepsy surgery. In: Engel J Jr (ed) Surgical treatment of the epilepsies, 2nd edn. Raven, New York, pp 565–581
Pouwels PJW, Frahm J (1998) Regional metabolite concentrations in human brain determined by quantitative localized proton MRS. Magn Reson Med 39:53–60
Prichard JW, Neil JJ (2000) Diffusion-weighted MRI: periictal studies. In: Henry TR, Duncan JS, Berkovic SF (eds) Functional imaging in the epilepsies. Advances in neurology, vol 83. Lippincott, Williams and Wilkins, New York, pp 279–284
Quesney LF, Gloor P (1985) Localization of epileptogenic foci. In: Gotman J, Ives JR, Gloor P (eds) Long-term monitoring in epilepsy. Elsevier, Amsterdam, pp 165–200
Quesney LF (1987) Extracranial EEG evaluation. In: Engel J Jr (ed) Surgical treatment of the epilepsies, 2nd edn. Raven, New York, pp 129–166
Rasmussen T (1973) Post-operative superficial hemosiderosis of the brain: its diagnosis, treatment and prevention. Am Neuro Assoc 98:133–137
Rasmussen T (1975) Cortical resection in the treatment of focal epilepsy. In: Purpura DP, Penry JK, Walter RD (eds) Neurosurgical management of the epilepsies. Advances in neurology, vol 8. Raven, New York, pp 139–154
Rasmussen T (1983) Hemispherectomy for seizures revisited. Can J Neurol Sci 10:71–78
Rausch R, Le MT, Langfitt JT (1998) Neuropsychological evaluation—adults. In: Engel J Jr, Pedley TA (eds) Epilepsy. A comprehensive textbook. Lippincott-Raven, Philadelphia, pp 977–988
Reeves AG, O’Leary PM (1985) Total corpus callosotomy for control of medically intractable epilepsy. In: Reeves AG (ed) Epilepsy and the corpus callosum. Plenum, New York, pp 269–280
Regis J, Peragut JC, Rey M, Samson Y, Levrier O, Porcheron D, Regis H, Sedan R (1994) First selective amygdalohippocampal radiosurgery for “mesial temporal lobe epilepsy”. Stereotact Funct Neurosurg 64 [Suppl 1]:191–201
Regis J, Roberts DW (1999) Gamma knife radiosurgery relative to microsurgery: epilepsy. Stereotact Funct Neurosurg 72 [Suppl 1]: 11–21
Regis J, Bartolomei F, Rey M, Genton P, Dravet C, Semah F, Gastaut JL, Chauvel P, Peragut JC (1999) Gamma knife surgery for mesial temporal lobe epilepsy. Epilepsia 40:1551–1556
Regis J, Bartolomei F, Hayashi M, Roberts D, Chauvel P, Peragut JC (2000) The role of gamma knife surgery in the treatment of severe epilepsies. Epileptic Disorders 2:113–122
Reife RA (1996) Topiramate. In: Shorvon S, Dreifuss F, Fish D, Thomas D (eds) The treatment of epilepsy. Marston, Oxford, pp 471–481
Reitan RM (1971) Trail making test results for normal and brain-damaged children. Percept Mot Skills 33:575–581
Resnick TJ, Duchowny MS, Alvarez LA, Jayakar P, Haller J (1989) Comparison of depth and subdural electrodes in recording interictal activity of children being evaluated for surgery. Epilepsia 30:659
Rey A (1942) L’examen psychologique dans les cas d’encephalopathie traumatique. Arch Psychol 28:112
Reynolds EH, Shorvon SD (1981) Monotherapy or polytherapy for epilepsy? Epilepsia 22:1–10
Roberts DW, Siegel AM (2001) Corpus callosotomy. In: Lüders HO, Comair Y (eds) Epilepsy surgery, 2nd edn. Lippincott, Williams and Wilkins, New York, pp 747–756
Roberts DW, Siegel AM (2001) Section of the corpus callosum for epilepsy. In: Schmidek HH (ed) Operative neurosurgical techniques. Saunders, Philadelphia
Rose DF, Smith PD, Sato S (1987) Magnetencephalography and epilepsy research. Science 238:329–335
Rose DF, Sato S, Smith PD, Porter RJ, Theodore WH, Friauf W, Bonner R, Jabbari B (1987) Localization of magnetic interictal discharges in temporal lobe epilepsy. Ann Neurol 22:348–354
Rosenbaum TJ, Laxer KD, Vessely M, Smith WB (1986) Subdural electrodes for seizure focus localization. Neurosurgery 19:73–81
Rosenow F, Lüders H (2001) Presurgical evaluation of epilepsy. Brain 124:1683–1700
Rougier A, Sundstrom L, Claveric B, Saint-Hilaire J-M, Labrecque R, Lurton D, Bouvier G (1996) Multiple subpial transection: report of 7 cases. Epilepsy Res 24:57–63
Salanova V, Andermann F, Olivier A, Rasmussen T, Quesney LF (1992) Occipital lobe epilepsy: electroclinical manifestations, electrocorticography, cortical stimulation and outcome in 42 patients treated between 1930 and 1991. Surgery of occipital lobe epilepsy. Brain 115:1655–1680
Salanova V, Quesney LF, Rasmussen T, Andermann F, Olivier A (1994) Reevaluation of surgical failures and the role of reoperation in 39 patients with frontal-lobe epilepsy. Epilepsia 35:70–80
Salanova V, Morris HH, Van Ness P, Kotagal P, Wyllie E, Lüders H (1995) Frontal lobe seizures: electroclinical syndromes. Epilepsia 36:16–24
Salanova V, Andermann F, Rasmussen T, Olivier A, Quesney LF (1995) Parietal lobe epilepsy. Clinical manifestations and outcome in 82 patients treated surgically between 1929 and 1988. Brain 118:607–627
Salanova V, Andermann F, Rasmussen T, Olivier A, Quesney LF (1995) Tumoural parietal lobe epilepsy. Clinical manifestations and outcome in 34 patients treated between 1934 and 1988. Brain 118:1289–1304
Sanders JA (1995) Magnetic resonance spectroscopy. In: Orrison WW Jr, Lewine JD, Sanders JA, Hartshorne MF (eds) Functional brain imaging. Mosby Year Book, St Louis, pp 419–467
Sanders JA, Orrison WW Jr (1995) Functional magnetic resonance imaging. In: Orrison WW Jr, Lewine JD, Sanders JA, Hartshorne MF (eds) Functional brain imaging. Mosby Year Book, St Louis, pp 239–326
Sato S, Smith PD (1985) Magnetencephalography. J Clin Neurophysiol 2:173–192
Schmidt D (1982) Two antiepileptic drugs for intractable epilepsy with complex partial seizures. JNNP 45:1119–1124
Schramm J, Kral T, Blümcke I, Elger CE (2000) Surgery of neocortical temporal and frontal epilepsy. In: Williamson PD, Siegel AM, Roberts DW, Thadani VM, Gazzaniga MS (eds) Neocortical epilepsy. Advances in neurology, vol 84. Lippincott, Williams and Wilkins, New York, pp 595–604
Shafer SQ, Hauser WA, Annegers JF, Klass DW (1988) EEG and other early predictors of epilepsy remission—a community study. Epilepsia 29:590–600
Sharbrough FW (1987) Commentary: extracranial EEG monitoring. In: Engel J Jr (ed) Surgical treatment of the epilepsies, 2nd edn, Raven, New York, pp 167–171
Shorvon SD (1996) Gabapentin. In: Shorvon S, Dreifuss F, Fish D, Thomas D (eds) The treatment of epilepsy. Marston, Oxford, pp 429–437
Siegel AM, Wieser HG (1989) Comparative pre- and postoperative interictal scalp EEG examinations in patients with selective amygdalohippocampectomy. J Epilepsy 2:65–72
Siegel AM, Wieser HG, Wichmann W, Yasargil MG (1990) Relationship between MR-imaged total amount of tissue removed, resection scores of specific mediobasal limbic subcompartments and clinical outcome following selective amygdalohippocampectomy. Epilepsy Res 6:56–65
Siegel AM, Williamson PD, Roberts DW, Thadani VM, Darcey TM (1999) Localized pain associated with seizure origin in the parietal lobe. Epilepsia 40:845–855
Siegel AM, Williamson PD (2000) Parietal lobe epilepsy. In: Williamson PD, Siegel AM, Roberts DW, Thadani VM, Gazzaniga MS (eds) Neocortical epilepsy. Advances in neurology, vol 84. Lippincott, Williams and Wilkins, New York, pp 189–199
Siegel AM, Roberts DW, Harbaugh RI, Williamson PD (2000) Pure lesionectomy versus tailored epilepsy surgery in treatment of cavernous angioma presenting with epilepsy. Neurosurg Rev 23:80–83
Siegel AM, Roberts DW, Thadani VM, McInerney J, Jost BC, Williamson PD (2000) The role of intracranial electrode reevaluation in epilepsy patients failing initial invasive monitoring. Epilepsia 41:571–580
Siegel AM, Jobst BC, Thadani VM, Rhodes CH, Lewis PJ, Roberts DW, Williamson PD (2001) Medically intractable, localization-related epilepsy with normal MRI: presurgical evaluation and surgical outcome in 43 patients. Epilepsia 42:883–888
Smith DB, Mattson RH, Cramer JA, Collins JF, Novelly RA, Craft B (1987) Results of a cooperative study nationwide Veterans Administration cooperative study comparing efficacy and toxicity of carbamazepine, phenobarbital, phenytoin, and primidone. Epilepsia 28 [Suppl 3]:S50–S58
Smith JR, Schwartz BJ, Gallen C, Orrison W, Lewine J, Murro AM, King DW, Park YD (1995) Utilization of multichannel magnetencephalography in the guidance of ablative seizure surgery. J Epilepsy 8:119–130
Smith JR, Lee MR, King DW, Murro AM, Park YD, Lee GP, Loring DW, Meador KJ, Harp R (1997) Results of lesional vs. nonlesional frontal lobe epilepsy surgery. Stereotact Funct Neurosurg 69:202–209
Smith MC, Byrne R (2000) Multiple subpial transection in neocortical epilepsy: part I. In: Williamson PD, Siegel AM, Roberts DW, Thadani VM, Gazzaniga MS (eds) Neocortical epilepsy. Advances in neurology, vol 84. Lippincott, Williams and Wilkins, New York, pp 621–634
Spencer DD, Spencer SS, Mattson RH, Williamson PD, Novelly RA (1984) Access to the posterior medial temporal lobe structures in the surgical treatment of temporal lobe epilepsy. Neurosurgery 15:667–671
Spencer DD, Spencer SS (1989) Corpus callosotomy in the treatment of medically intractable secondarily generalized seizures of children. Cleve Clin J Med 56:S69–S78
Spencer DD, Inserni J (1992) Temporal lobectomy. In: Lüders H (ed) Epilepsy surgery. Raven, New York, pp 533–545
Spencer SS, Williamson PD, Bridgers SL, Mattson RH, Cicchetti DV, Spencer DD (1985) Reliability and accuracy of localization by scalp ictal EEG. Neurology 35:1567–1575
Spencer SS, Gates JR, Reeves AG et al (1987) Corpus callosum section for uncontrolled epilepsy. In: Engel J Jr (ed) Surgical treatment of epilepsy. Raven, New York, pp 425–444
Spencer SS, Spencer DD, Williamson, Mattson R (1990) Combined depth and subdural electrode investigation in uncontrolled epilepsy. Neurology 40:74–79
Spencer SS (1992) Depth electrodes. In: Theodore WH (ed) Surgical treatment of epilepsy. Elsevier, Amsterdam, pp 135–145
Spencer SS (1994) The relative contributions of MRI, SPECT, and PET imaging in epilepsy. Epilepsia 35 [Suppl 6]: S72-S89
Spencer SS, Sperling MR, Shewmon DA (1998) Intracranial electrodes. In: Engel J Jr, Pedley TA (eds) Epilepsy. A comprehensive textbook. Lippincott-Raven, Philadelphia, pp 1719–1747
Spencer SS, Lee SA (2000) Invasive EEG in neocortical epilepsy: seizure onset. In: Williamson PD, Siegel AM, Roberts DW, Thadani VM, Gazzaniga MS (eds) Neocortical epilepsy. Advances in neurology, vol 84. Lippincott, Williams and Wilkins, New York, pp 275–286
Spencer SS, Schramm J, Wyler A, O’Connor M, Orbach D, Krauss G, Sperling M, Devinsky O, Elger C, Lesser R, Mulligan L, Westerveld M (2002) Multiple subpial transection for intractable partial epilepsy: An international meta-analysis. Epilepsia 43:141–145
Sperling MR, Wilson G, Engel J Jr, Babb TL, Phelps M, Bradley W (1986) Magnetic resonance imaging in intractable partial epilepsy: correlative studies. Ann Neurol 20:57–62
Sperling MR, O’Connor MJ (1989) Comparison of depth and subdural electrodes in recording temporal lobe seizures. Neurology 39:1497–1504
Sperling MR, Saykin AJ, Glosser G, Moran M, French JA, Brooks M, O’Connor MJ (1994) Predictors of outcome after anterior temporal lobectomy: the intracarotid amobarbital test. Neurology 44:2325–2330
Spreen O, Strauss E (1998) A compendium of neuropsychological tests, 2nd edn. Oxford University Press, New York
Stanley JA, Cendes F, Dubeau F, Andermann F, Arnold DL (1998) Proton magnetic resonance spectroscopic imaging in patients with extratemporal epilepsy. Epilepsia 39:267–273
Stefan H, Schneider S, Feistel H, Pawlik G, Schuler P, Abrahamfuchs K, Schlegel T, Neubauer U, Huk WJ (1992) Ictal and interictal activity in partial epilepsy recorded with multichannel magnetencephalography: correlation of electroencephalography/electrocorticography, magnetic resonance imaging, single photon emission computed tomography, and positron emission tomography findings. Epilepsia 33:874–887
Steiner L, Lindquist C, Steiner M (1992) Radiosurgery. In: Advances and technical standards in neurosurgery. New York, pp 20–102
Stroop JR (1935) Studies of interference in serial verbal reactions. J Exp Psychol 18:643–662
Sutherling WW, Barth DS (1989) Neocortical propagation in temporal lobe spike foci on magnetoencephalography and electroencephalography. Ann Neurol 25:373–381
Symms MR, Allen PJ, Woermann FG, Polizzi G, Krakow K, Barker GJ, Fish DR, Duncan JS (1999) Reproducible localisation of interictal epileptiform activity using functional MRI. Phys Med Biol 41:161–168
Thadani VM, Williamson PD, Berger R, Spencer SS, Spencer DD, Novelly RA, Sass KJ, Kim JH, Mattson RH (1995) Successful epilepsy surgery without intracranial EEG recording—criteria for patient selection. Epilepsia 36:7–15
Thadani VM, Siegel AH, Lewis PJ, Siegel AM, Gilbert KL, Darcey TM, Roberts DW, Williamson PD (2000) SPECT in neocortical epilepsies. In: Williamson PD, Siegel AM, Roberts DW, Thadani VM, Gazzaniga MS (eds) Neocortical epilepsy. Advances in neurology, vol 84. Lippincott, Williams and Wilkins, New York, pp 425–434
Theodore WH, Dorwart R, Holmes M, Porter RJ, Dichiro G (1986) Neuroimaging in refractory partial seizures: comparison of PET, CT, and MRI. Neurology 36:750–759
Theodore WH, Fishbein D, Dubinsky R (1988) Patterns of cerebral glucose metabolism in patients with partial seizures. Neurology 38:1201–1206
Tiffin J, Asher EJ (1948) The Purdue pegboard: norms and studies of reliability and validity. J Appl Psychol 32:234–247
Trenerry MR (1996) Neuropsychologic assessment in surgical treatment of epilepsies. Mayo Clin Proc 71:1196–1200
Tsai ML, Chatrian GE, Pauri F, Temkin NR, Holubkov AL, Shaw CM, Ojemann GA (1993) Electrocorticography in patients with medically intractable temporal-lobe seizures. I. Quantification of epileptiform discharges prior to resective surgery. Electroenceph Clin Neurophysiol 87:10–24
Tsai ML, Chatrian GE, Holubkov AL, Temkin NR, Shaw CM, Ojemann GA (1993) Electrocorticography in patients with medically intractable temporal-lobe seizures. II. Quantification of epileptiform discharges following successive stages of resective surgery. Electroenceph Clin Neurophysiol 87:25–37
Turner R, Howseman A, Rees GE, Josephs O, Friston K (1998) Functional magnetic resonance imaging of the human brain: data acquisition and analysis. Exp Brain Res 123:5-12
V.A. Cooperative Study 118 (1984) Newsletter for epilepsy. Issue 25:5
Van Buren JM, Ajmone-Marsan C, Mutsuga N, Sadowsky D (1975) Surgery of temporal lobe epilepsy. In: Purpura DP, Penry JK, Walter RD (eds) Neurosurgical management of the epilepsies. Advances in neurology, vol 8. Raven, New York, pp 155–196
Van Paesschen W, Connelly A, King MD, Jackson GD, Duncan JS (1997) The spectrum of hippocampal sclerosis: a quantitative magnetic resonance imaging study. Ann Neurol 41:41–51
Van Wagenen WP, Herren RY (1940) Surgical division of commissural pathways in the corpus callosum. Relation to spread of an epileptic attack. Arch Neurol Psychiatr 44:740–759
Villemure JG, Mascott C (1993) Hemispherotomy: the peri-insular approach. Technical aspects. Epilepsia 34 [Suppl 6]:48
Villemure JG (1996) Hemispherectomy. In: Shorvon S, Dreifuss F, Fish D, Thomas D (eds) The treatment of epilepsy. Marston, Oxford, 713–721
Vining EPG, Freeman JM, Brandt J, Carson S, Uematsu S (1993) Progressive unilateral encephalopathy of childhood (Rasmussen’s syndrome): a reappraisal. Epilepsia 34:639–650
Wada J, Rasmussen T (1960) Intracarotid injection of sodium amytal for the lateralization of cerebral speech dominance: experimental and clinical observations. J Neurosurg 17:266–282
Walker AE (1967) Temporal lobectomy. J Neurosurg 26:642–649
Walker AE (1974) Surgery for epilepsy. In: Vinken PJ, Bruyn GW (eds) Handbook of clinical neurology, vol 15. North-Holland, Amsterdam, pp 739–757
Warach S, Ives JR, Schlaug G, Patel MR, Darby DG, Thangaraj V, Edelman RR, Schomer DL (1996) EEG-triggered echo-planar functional MRI in epilepsy. Neurology 47:89–93
Wechsler D (1955) Wechsler adult intelligence scale. Psychological Corporation, New York
Westmoreland BF (1985) The electroencephalogram in patients with epilepsy. Neurol Clin Vol 3:599–613
Wetjen NM, Cohen-Gadol AA, Maher CO, Marsh WR, Meyer FB, Cascino GD (2002) Frontal lobe epilepsy: diagnosis and surgical treatment. Neurosurg Rev 25:119–138
White HH (1961) Cerebral hemispherectomy in the treatment of infantile hemiplegia. Confinia Neurol 21:1–50
Wieser HG, Yasargil MG (1982) Selective amygdalohippocampectomy as a surgical treatment of mesiobasal limbic epilepsy. Surg Neurol 17:445–457
Wieser HG (1983) Electroclinical features of the psychomotor seizure. Fischer-Butterworths, Stuttgart
Wieser HG, Elger CE, Stodieck SRG (1985) The foramen ovale electrode. A new recording method for the preoperative evaluation of patients suffering from mesiobasal limbic temporal lobe epilepsy. Electroenceph Clin Neurophysiol 61:314–322
Wieser HG, Siegel AM, Yasargil MG (1990) The Zürich amygdalo-hippocampectomy series: a short up-date. Acta Neurochirurgica Suppl (Wien) 50:122–127
Wieser HG, Siegel AM (1991) Analysis of foramen ovale electrodes recorded seizures: correlation with outcome following amygdalohippocampectomy. Epilepsia 32:838–850
Wieser HG, Siegel AM (1993) Symptomatische Epilepsie des Frontal-, Temporal-, Parietal- und Okzipitallappens. In: Fröscher W, Vassella F (eds) Die Epilepsien. De Gruyter, Berlin, pp 177–195
Wieser HG (1993) Stereoelectroencephalography and foramen ovale electrode recording. In: Niedermeyer E, Lopes da Silva F (eds) Electroencephalography. Basic principles, clinical applications, and related fields, 3rd edn. Williams and Wilkins, Baltimore, pp 679–693
Wieser HG, Müller S, Schiess R, Khan N, Regard M, Landis T, Bjeljac M, Buck A, Valavanis A, Yasargil G, Yonekawa Y (1997) The anterior and posterior selective temporal lobe amobarbital tests: angiographical, clinical, electroencephalographical, PET and SPECT findings, and memory performance. Brain Cogn 33:71–97
Wieser HG (2000) Semiology of neocortical temporal lobe epilepsy. In: Williamson PD, Siegel AM, Roberts DW, Thadani VM, Gazzaniga MS (eds) Neocortical epilepsy. Advances in neurology, vol 84. Lippincott, Williams and Wilkins, New York, pp 201–214
Wieser HG, Ortega M (2001) Kommentar zum “Vorschlag für eine neue Outcome-Klassifikation betreffend epileptische Anfälle nach Epilepsichirurgie” der Internationalen Liga gegen Epilepsie und Beispiel für deren Anwendung anhand der Zürcher Amygdala-Hippokampektomie-Serie. Akt Neurol 29:138–144
Wieshmann UC, Free SL, Everitt AD, Bartlett PA, Barker GJ, Tofts PS, Duncan JS, Shorvon SD, Stevens JM (1996) Magnetic resonance imaging in epilepsy with a fast FLAIR sequence. JNNP 61:357–361
Wieshmann UC, Symms MR, Shorvon SD (1997) Diffusion changes in status epilepticus. Lancet 350:493–494
Wilder BJ, Uthman BM, Hammond EJ (1991) Vagal stimulation for control of complex partial seizures in medically refractory epileptic patients. PACE 14:108–115
Williamson PD, Thadani VM, Darcey TM, Spencer DD, Spencer SS, Mattson RH (1992) Occipital lobe epilepsy: clinical characteristics, seizure spread patterns, and results of surgery. Ann Neurol 31:3–13
Williamson PD, Boon PA, Thadani VM, Darcey TM, Spencer DD, Spencer SS, Novelly RA, Mattson RH (1992) Parietal lobe epilepsy: diagnostic considerations and results of surgery. Ann Neurol 31:193–201
Williamson PD, Jobst BC (2000) Frontal lobe epilepsy. In: Williamson PD, Siegel AM, Roberts DW, Thadani VM, Gazzaniga MS (eds) Neocortical epilepsy. Advances in neurology, vol 84. Lippincott, Williams and Wilkins, New York, pp 215–242
Wilson DH, Culver C, Waddington M, Gazzaniga M (1975) Disconnection of the cerebral hemispheres: an alternative to hemispherectomy for the control of intractable seizures. Neurology 25:1149–1153.
Wilson DH, Reeves AG, Gazzaniga MS, Culver C (1977) Cerebral commissurotomy for control of intractable seizures. Neurology 27:708–715
Wilson DH, Reeves A, Gazzaniga M (1978) Division of the corpus callosum for uncontrollable epilepsy. Neurology 28:649–653
Wilson DH, Reeves A, Gazzaniga M (1980) Corpus callosotomy for control of intractable seizures. In: Wada JA, Penry JK (eds) Advances in epileptology. The Xth Epilepsy International Symposium. Raven, New York, pp 205–213
Wilson DH, Reeves AG, Gazzaniga MS (1982) “Central” commissurotomy for intractable generalized epilepsy: series two. Neurology 32:687–697
Wilson PJE (1970) Cerebral hemispherectomy for infantile hemiplegia. Brain 93:147–180
Winston KR, Welch K, Adler JR, Erba G (1992) Cerebral hemicorticectomy for epilepsy. J Neurosurg 77:889–895
Wurm G, Wies W, Schnizer M, Trenkler J, Holl K (2000) Advanced surgical approach for selective amygdalohippocampectomy through neuronavigation. Neurosurgery 48:456–457
Wyler AR, Walker G, Richey ET, Hermann BP (1988) Chronic subdural strip electrode recordings for difficult epileptic problems. J Epilepsy 1:71–78
Wyler AR (1992) Corpus callosotomy. In: Theodore WH (ed) Surgical treatment of epilepsy (Epilepsy Res Suppl 5). Elsevier, Amsterdam, pp 205–208
Wyler AR (2000) Multiple subpial transection in neocortical epilepsy: part II. In: Williamson PD, Siegel AM, Roberts DW, Thadani VM, Gazzaniga MS (eds) Neocortical epilepsy. Advances in neurology, vol 84. Lippincott, Williams and Wilkins, New York, pp 635–642
Yonekawa Y, Imhof HG, Taub E, Curcic M, Kaku Y, Roth P, Wieser HG, Groscurth P (2001) Supracerebellar transtentorial approach to posterior temporomedial structures. J Neurosurg 94:339–345
Zentner J, Hufnagel A, Ostertun B, Wolf HK, Behrens E, Campos MG, Solymosi L, Elger CE, Wiestler OD, Schramm J (1996) Surgical treatment of extratemporal epilepsy: clinical, radiologic, and histopathologic findings in 60 patients. Epilepsia 37:1072–1080
Author information
Authors and Affiliations
Corresponding author
Additional information
Commentaries on this paper are available at http://dx.doi.org/10.1007/s10143-003-0306-5 and http://dx.doi.org/10.1007/s10143-003-0307-4
Rights and permissions
About this article
Cite this article
Siegel, A.M. Presurgical evaluation and surgical treatment of medically refractory epilepsy. Neurosurg Rev 27, 1–18 (2004). https://doi.org/10.1007/s10143-003-0305-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-003-0305-6