Abstract
Clinical therapy incorporating femtosecond laser (FSL) devices is a quickly growing field in modern biomedical technology due to their precision and ability to generate therapeutic effects with substantially less laser pulse energy. FSLs have the potential to produce nonlinear optical effects such as harmonic generation (HG), especially in tissues with significant nonlinear susceptibilities such as the cornea. HG in corneal tissue has been demonstrated in nonlinear harmonic microscopy using low-power FSLs. Furthermore, the wavelength ranges of harmonic spectral emissions generated in corneal tissues are known to be phototoxic above certain intensities. We have investigated how the critical FSL parameters pulse energy, pulse repetition rate, and numerical aperture influence both second (SHG) and third harmonic generation (THG) in corneal tissue. Experimental results demonstrated corresponding increases in HG intensity with increasing repetition rate and numerical aperture. HG duration decreased with increasing repetition rate and pulse energy. The data also demonstrated a significant difference in HG between FSL parameters representing the two most common classes of FSL therapeutic devices.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Femtosecond laser (FSL) devices are rapidly emerging as unmatched tools for clinical optical therapeutics with respect to their precision and ability to generate therapeutic effects with substantially less energy [1–6]. The large impact that this advanced technology is having on the medical field is exemplified by its use in several of the most commonly performed surgical procedures in the world, specifically, LASIK, cataract surgery, and corneal transplantation [7–13]. In order to achieve optical breakdown, the predominant tissue cutting mechanism [14, 15], FSLs must generate very high intensities, which can also generate nonlinear optical effects (NOEs) such as second and third harmonic generation (SHG and THG, respectively) [16, 17]. NOEs cause a modification of the optical properties of a susceptible material due to an intense optical field, often generated by ultrashort pulsed lasers [18, 19]. Harmonic generation (HG) is an example of a NOE that could impact therapy efficacy and patient safety by changing the laser parameters responsible for the therapeutic effect and by generating phototoxic UV light and intense visible light. Coincidentally, corneal tissue, which has seen the largest application of FSL-based therapies, strongly generates NOEs due to its highly organized and oriented, dense collagen structure [20–22].
Harmonic generation is a frequency mixing process that occurs due to interactions between photons and materials with significant nonlinear susceptibilities. A harmonic frequency (2ω, 3ω, etc.) is generated as photon energy flows from the fundamental frequency, depending on the phase-matching conditions, to the harmonic field [23, 24]. SHG occurs only in non-centrosymmetric materials and results in photons with twice the frequency and energy, and half the wavelength. Similarly, THG results in photons with three times the frequency and energy, and one third the wavelength. However, THG does not require a lack of inversion symmetry and can occur in amorphous materials as well [18, 24].
HG-based nonlinear microscopy has been used to image the layers [25] and collagen structure [21, 26, 27] of corneal tissue. Further, Stoller et al. demonstrated experimentally that SHG signal intensity in corneal collagen is polarization dependent [28] and can be used to determine collagen fibril orientation. These previous studies regarding corneal tissue composition were accomplished using harmonic microscopy, a technique that uses low-power FSLs and photomultiplier tubes to amplify the relatively weak harmonic signals. Ophthalmic surgical procedures utilize FSLs with intensities three orders of magnitude higher than intensities used for imaging applications [29]. This enables the quantification of resulting HG without any amplification. In addition, unlike fluorescence, HG is a coherent process, resulting in more intense light and, therefore, more capable of causing unintended tissue damage. As nonlinear optical effects such as harmonic generation are greatly dependent on laser intensity, we believe that an investigation of the relationships between HG elicited by clinically important FSL parameters at these energy levels is warranted. Other nonlinear effects occurring also at significantly lower intensities, such as self-focusing and filamentation, have recently been studied using therapeutic FSL parameters [16, 17, 30]. SHG and THG have even been reported during photodisruption in corneal tissue [16, 17, 31], but no investigation to our knowledge has examined the relationship between laser parameters and HG characteristics at these energy levels.
Currently, FSLs can be grouped into two major categories. Conventional FSLs employ lower pulse repetition rates (kHz), longer pulse durations (>500 fs), and higher (μJ) pulse energies. In an attempt to further improve precision and reduce collateral effects, the new regime of FSLs employs higher repetition rates (MHz), shorter pulse durations (<500 fs), and lower (nJ) pulse energies, which allow for more precise and smooth tissue cutting [2, 29]. Since HG is dependent on laser intensity, which is largely determined by pulse duration, pulse energy, repetition rate, and numerical aperture (NA), different classes of FSLs may produce different amounts of HG in tissues.
Ophthalmic therapeutic FSLs emit near-infrared (NIR) light near 1.04 μm, producing SHG and THG in the green and ultraviolet A (UVA) spectral regions, respectively. Light in both of these regions can potentially cause photochemical damage in the retina [32–34]. In addition, UVA light increases the rate of cataract formation in the lens [35–37]. It is therefore important to minimize SHG and THG produced during FSL-based ophthalmic procedures. To our knowledge, no studies have quantified HG during optical breakdown in corneal tissue. In this work, we investigate the effect of the clinically relevant FSL parameters pulse energy, pulse repetition rate, and numerical aperture on HG intensity and duration induced in corneal tissue.
Materials and methods
HG quantification
To induce HG in corneal tissue and quantify the transmitted light, the setup illustrated in Fig. 1 was employed. A 1042-nm-wavelength, 300-fs-pulse-duration FSL (Spectra-Physics) was focused onto the cornea sample using single plano-convex lenses to avoid temporal pulse dispersion. Laser exposure and corneal sample position were controlled using an automated shutter and three-axis micro-positioning stage. Transmitted SHG and THG were separated from the fundamental wavelength using a dichroic long-pass filter (Edmund Optics) and collected using a fiber coupling lens (Thorlabs) and 600-μm-core-diameter fiber (Ocean Optics) attached to a spectrometer (Ocean Optics). A short-pass edge filter (Semrock) was used to remove any remaining background at the fundamental wavelength prior to fiber coupling.
Diagram of experimental setup used to produce and quantify second and third harmonic generation in corneal tissue (T) using a computer-controlled (CPU) femtosecond laser (FSL), shutter (S), translation stage (xyz), and spectrometer (Spec). M mirror; L1, L2 lens; D dichroic beam splitter; SP short-pass filter; F fiber
Tissue preparation
Freshly enucleated bovine globes were obtained from a local slaughterhouse and stored on ice. Immediately prior to testing, a 10-mm trephine was used to remove the central cornea. The corneal button was placed on a glass slide and positioned in front of the laser. Several drops of balanced salt solution were added to the slide to prevent corneal drying. For testing FSL repetition rate and pulse energy, specific combinations of laser parameters were randomly assigned to positions on a 1-mm spaced grid to ensure no locations were overlapped and to avoid effects of regionally specific tissue parameters, if present. Using 5 corneas, each combination of parameters was tested 20 times, 4 per cornea. For the effect of changing NA, each NA was tested at 13 locations on each of 2 corneas. Measurements were completed within 15 min of trephination of each cornea.
Experimental protocol
SHG and THG intensity and duration were measured for every combination of three FSL repetition rates (100 kHz, 500 kHz, and 1 MHz) and three pulse energies (0.38, 0.94, and 1.89 μJ). The FSL pulse energies are determined using the average power values measured after the focusing lens. In addition, SHG and THG intensities were measured for three different NAs (0.148, 0.169, and 0.233) by changing the focusing lens, while maintaining the pulse energy and repetition rate constant at 1.89 μJ and 100 kHz, respectively. A custom LabVIEW program automated the sample positioning, laser exposure (900 ms), and spectrophotometric measurements. High-speed spectrometer acquisition was started immediately prior to each laser exposure and ended after shutter closure. For this study, HG optical intensity is defined in arbitrary units as the highest achieved intensity during the laser exposure, and duration is defined as the time spent above a threshold set slightly above the noise level.
Data preparation
Data for each laser parameter combination or NA were averaged over all cornea samples and compared with each other using a Student’s t test assuming unequal variance to determine statistical significance. Differences were considered significant for p values <0.05. Ninety-five percent confidence intervals were calculated for each group with values stated as mean ± 95 % confidence bound.
Results
Repetition rate and pulse energy
In general, SHG was considerably more intense than THG. Figure 2 illustrates typical experimentally recorded SHG and THG signals which are plotted as intensity distribution as a function of time (Fig. 2a), as well as 3D (Fig. 2b) and 2D (Fig. 2c) signal distributions.
Mean SHG and THG intensities, grouped by pulse energy, are summarized in Fig. 3. For all pulse energies, SHG and THG intensities increased with repetition rate. Exposures using 1-MHz repetition rates produced some of the highest HG intensities. The 100-kHz repetition rates produced the largest variability.
Mean SHG and THG durations are summarized in Fig. 4. As the temporal resolution of the spectrometer was about 10 ms, HG intensity produced by the FSL pulse train is integrated over multiple pulses and appears as a continuous plot, despite the individual HG pulses having durations similar to the FSL pulses. As opposed to HG intensity, for each pulse energy, SHG duration decreased with increasing repetition rate. In the case of THG, duration for 100 kHz was substantially longer than 500 kHz and 1 MHz in the 0.38- and 0.94-μJ-pulse-energy groups. THG duration in the 1.89-μJ-pulse-energy group increased with increasing repetition rate. THG duration was shorter than SHG duration. In general, 1-MHz repetition rates generated the highest HG intensities but the shortest durations while 100-kHz repetition rates generated the lowest HG intensities and longest durations.
Numerical aperture
The resulting SHG and THG intensity for the three NAs tested is summarized in Fig. 5. There was a corresponding increase in SHG and THG intensity with increasing NA; however, increases in THG intensity were small in comparison with SHG.
Discussion
Repetition rate, pulse energy, and NA are important FSL parameters for achieving the desired tissue cutting therapeutic effect in many ophthalmic procedures employing FSLs. This study aims to evaluate the dependence of harmonic generation in corneal tissue on these key laser parameters that are similar to those used in current therapeutic applications. The results of this initial study do not include the exact replication of specific ophthalmic surgical procedures, which may involve some special scanning of the laser focus. Although not directly observed, the concurrence of photodisruption, the therapeutic effect, is predicted since the minimal intensity generated by the FSL parameters was approximately 8 × 1012 W/cm2, which is twice the threshold for optical breakdown [15]. This was confirmed experimentally by the presence of a microscopic bubble at each focal location on the cornea.
SHG occurs in non-centrosymmetric materials, such as the stromal collagen, while THG is strongest at interfaces between materials where there is a change in the nonlinear refractive index, such as the Bowman’s Layer-Stromal boundary [25, 38, 39]. This principle was used in this study to center the FSL focus in the stroma. This also explains why observed SHG intensities were higher than observed THG intensities (see Figs. 2 and 3). Further, since SHG and THG are second- and third-order nonlinear processes whose intensities vary with the square and cubic intensity of the incident laser [23], a weaker THG intensity would be expected even if all other factors were equal. The increase in HG intensity observed with increasing laser pulse repetition rate at a given pulse energy can be attributed to a higher number of FSL pulses, and therefore HG pulses, within the spectrometer’s integration period.
HG duration decreased with increasing repetition rate for most pulse energies (see Fig. 4). Shortening the period between pulses causes an increased rate of tissue destruction which shortens HG duration. Additionally, as the tissue is destroyed, more plasma absorption and scattering of HG away from the collecting fiber occur, which further reduces HG duration. A similar explanation can be made for the decrease in HG duration observed with increasing pulse energy. Higher pulse energy results in larger plasmas with higher free electron densities that destroy more tissue per pulse [15]. In clinical therapies, FSLs are rapidly scanned to produce a tissue cutting effect. This motion limits the laser exposure at any single location to periods much shorter than both the exposure time used and the HG durations observed in this experiment. However, since the highest HG intensity is generated instantaneously, rapid scanning of the laser constantly exposes fresh tissue which creates HG with constant peak intensity values.
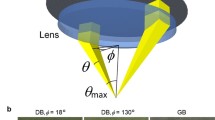
Changing the NA leads to changes in beam waist at the laser focus as well as changes in the Rayleigh length related to the beam depth of focus. Normally, these changes would tend to have opposite effects on HG. For example, decreasing the beam waist results in a higher intensity and correspondingly higher HG intensity, but decreasing the Rayleigh length decreases the volume of tissue interacting with an intense optical field resulting in a decrease in HG intensity. Experimentally, a significant increase in HG intensity was observed by increasing NA (see Fig. 5). Previous studies using harmonic microscopy to image the cornea have shown [25] that SHG signal intensity oscillates with tissue depth, with intensity peaks separated by approximately 100 μm. This effect may well be related to a varying degree of phase matching. The change in Rayleigh length associated with the tested NAs is approximately 35 μm. We suggest that since the laser focus is positioned in the stromal region by optimizing the SHG signal, extending the Rayleigh length 35 μm into low-efficiency SHG stromal regions will have a small effect on the overall SHG production. Therefore, changes in the beam waist will affect HG intensity more than changes in Rayleigh length.
Although some significant increases in THG were observed with increasing NA, they were minor in comparison to SHG. We believe that changes in optical field intensity in an already weak field, where most efficient THG occurs at the stromal interfaces, result in very small changes in THG intensity.
A large amount of variability was seen in HG which is likely a result of varying collagen orientations at different locations and depths within and across corneas [39, 40]. As we have previously shown, the orientation of collagen with respect to the laser polarization has a significant effect on HG efficiency. As previously noted, this is likely a result of different degrees of phase matching. Despite this variability, there were many significant differences in HG intensity and duration at all repetition rates. Many of the strongest differences occurred when comparing 1-MHz with 100-kHz repetition rates for intensity and duration measurements. The experimental groups that most closely represent current commercial therapeutic devices are (100 kHz, 0.94 μJ), (100 kHz, 1.89 μJ), and (1 MHz, 0.38 μJ) [29]. In this comparison, the 1-MHz repetition rate produced SHG intensities one and two orders of magnitude higher than the 100-kHz repetition rate at 0.94 and 1.89 μJ, respectively. The same comparison with respect to THG reveals no significant difference between (1 MHz, 0.94 μJ) and (100 kHz, 0.94 μJ) and a significantly higher 1-MHz THG intensity compared with (100 kHz, 1.89 μJ). Differences in SHG and THG duration were mostly not significant.
Laser parameters representing the newest generation of therapeutic FSLs may produce more intense SHG and THG than conventionally used FSLs. Since therapeutic FSLs allow the operator to adjust some of the laser parameters to customize the surgical procedure, and as both frequencies of light generated during SHG and THG have the potential to produce damaging effects to ocular tissues, future studies that determine HG irradiance at the crystalline lens and retina are warranted to determine if a safety concern exists.
References
Hoy CL, Ferhanoglu O, Yildirim M, Kim KH, Karajanagi SS, Chan KMC et al (2014) Clinical ultrafast laser surgery: recent advances and future directions, IEEE J Sel Top Quantum Electron 20
Ozulken K, Cabot F, Yoo SH (2013) Applications of femtosecond lasers in ophthalmic surgery. Expert Rev Med Devices 10:115–124
Strassl M, Wieger V, Brodoceanu D, Beer F, Moritz A, Wintner E (2008) Ultra-short pulse laser ablation of biological hard tissue and biocompatibles. J Laser Micro Nanoeng 3:30–40
Dutra-Correa M, Nicolodelli G, Rodrigues JR, Kurachi C, Bagnato VS (2011) Femtosecond laser ablation on dental hard tissues—analysis of ablated profile near an interface using local effective intensity. Laser Phys 21:965–971
Meesat R, Belmouaddine H, Allard JF, Tanguay-Renaud C, Lemay R, Brastaviceanu T et al (2012) Cancer radiotherapy based on femtosecond IR laser-beam filamentation yielding ultra-high dose rates and zero entrance dose. Proc Natl Acad Sci U S A 109:E2508–E2513
Chakravarty P, Qian W, El-Sayed MA, Prausnitz MR (2010) Delivery of molecules into cells using carbon nanoparticles activated by femtosecond laser pulses. Nat Nanotechnol 5:607–611
Binder PS (2010) Femtosecond applications for anterior segment surgery. Eye Contact Lens 36:282–285
Daukantas P (2010) Lasers in ophthalmology. Opt Photonics News 21:28
Farjo AA, Sugar A, Schallhorn SC, Majmudar PA, Tanzer DJ, Trattler WB et al (2013) Femtosecond lasers for LASIK flap creation: a report by the American Academy of Ophthalmology. Ophthalmology 120:e5–e20
Kymionis GD, Kankariya VP, Plaka AD, Reinstein DZ (2012) Femtosecond laser technology in corneal refractive surgery: a review. J Refract Surg (Thorofare, NJ: 1995) 28:912–920
Reddy KP, Kandulla J, Auffarth GU (2013) Effectiveness and safety of femtosecond laser-assisted lens fragmentation and anterior capsulotomy versus the manual technique in cataract surgery. J Cataract Refract Surg 39:1297–1306
Naranjo-Tackman R (2011) How a femtosecond laser increases safety and precision in cataract surgery? Curr Opin Ophthalmol 22:53–57
He L, Sheehy K, Culbertson W (2011) Femtosecond laser-assisted cataract surgery. Curr Opin Ophthalmol 22:43–52
Vogel A, Noack J, Hüttman G, Paltauf G (2005) Mechanisms of femtosecond laser nanosurgery of cells and tissues. Appl Phys B 81:1015–1047
Vogel A, Venugopalan V (2003) Mechanisms of pulsed laser ablation of biological tissues. Chem Rev 103:577–644
Heisterkamp A, Ripken T, Mamom T, Drommer W, Welling H, Ertmer W et al (2002) Nonlinear side effects of fs pulses inside corneal tissue during photodisruption. Appl Phys B-Lasers Opt 74:419–425
Harzic RL, Bückle R, Wüllner C, Donitzky C, König K (2005) Laser safety aspects for refractive eye surgery with femtosecond laser pulses. Med Laser Appl 20:233–238
Boyd R (2003) Nonlinear optics. Academic, San Diego
Hecht E (2002) Optics. Pearson, San Francisco
Meek KM, Boote C (2004) The organization of collagen in the corneal stroma. Exp Eye Res 78:503–512
Bueno JM, Gualda EJ, Artal P (2011) Analysis of corneal stroma organization with wavefront optimized nonlinear microscopy. Cornea 30:692–701
Daxer A, Fratzl P (1997) Collagen fibril orientation in the human corneal stroma and its implication in keratoconus. Invest Ophthalmol Vis Sci 38:121–129
Boyd R (2008) Nonlinear optics, 3rd edn. Academic, Burlington
New G (2011) An introduction to nonlinear optics. Cambridge University Press, Cambridge
Jay L, Brocas A, Singh K, Kieffer JC, Brunette I, Ozaki T (2008) Determination of porcine corneal layers with high spatial resolution by simultaneous second and third harmonic generation microscopy. Opt Express 16:16284
Olivier N, Aptel F, Plamann K, Schanne-Klein M-C, Beaurepaire E (2010) Harmonic microscopy of isotropic and anisotropic microstructure of the human cornea. Opt Express 18:5028–5040
Morishige N, Wahlert AJ, Kenney MC, Brown DJ, Kawamoto K, Chikama T et al (2007) Second-harmonic imaging microscopy of normal human and keratoconus cornea. Invest Ophthalmol Vis Sci 48:1087–1094
Stoller P, Reiser KM, Celliers PM, Rubenchik AM (2002) Polarization-modulated second harmonic generation in collagen. Biophys J 82:3330–3342
Lubatschowski H (2008) Overview of commercially available femtosecond lasers in refractive surgery. J Refract Surg 24:102–107
Nuzzo V, Savoldelli M, Legeais JM, Plamann K (2010) Self-focusing and spherical aberrations in corneal tissue during photodisruption by femtosecond laser. J Biomed Opt 15:038003
Nuzzo V, Plamann K, Savoldelli M, Merano M, Donate D, Albert O et al (2007) In situ monitoring of second-harmonic generation in human corneas to compensate for femtosecond laser pulse attenuation in keratoplasty. J Biomed Opt 12:064032
Glickman RD (2011) Ultraviolet phototoxicity to the retina. Eye Contact Lens 37:196–205
Glickman RD (2002) Phototoxicity to the retina: mechanisms of damage. Int J Toxicol 21:473–490
Wu J, Seregard S, Algvere PV (2006) Photochemical damage of the retina. Surv Ophthalmol 51:461–481
Zigman S, Vaughan T (1974) Near-ultraviolet light effects on the lenses and retinas of mice. Invest Ophthalmol 13:462–465
Varma SD, Hegde KR, Kovtun S (2008) UV-B-induced damage to the lens in vitro: prevention by caffeine. J Ocul Pharmacol Ther 24:439–444
Zigman S (1995) Environmental near-UV radiation and cataracts. Optom Vis Sci 72:899–901
Barad Y, Eisenberg H, Horowitz M, Silberberg Y (1997) Nonlinear scanning laser microscopy by third harmonic generation. Appl Phys Lett 70:922–924
Calhoun W, Kernik D, Beylin A, Weiblinger R, Ilev I (2013) Nonlinear optical frequency conversions of a femtosecond laser in cornea tissue, In SPIE Photonics West, San Francisco
Calhoun W, Ilev IK (2014) Effect of femtosecond laser pulse energy and repetition rate on laser induced second and third harmonic generation in corneal tissue, In CLEO: Applications and Technology, p. ATh3P. 5.
Acknowledgments
The mention of commercial products, their sources, or their use in connection with material reported here is not to be construed as either an actual or implied endorsement of such products by the U.S. Food and Drug Administration (FDA). This article does not contain any studies with animals performed by any of the authors.
Conflict of interest
The authors have no conflicts of interest to report.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Calhoun, W.R., Ilev, I.K. Effect of therapeutic femtosecond laser pulse energy, repetition rate, and numerical aperture on laser-induced second and third harmonic generation in corneal tissue. Lasers Med Sci 30, 1341–1346 (2015). https://doi.org/10.1007/s10103-015-1726-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-015-1726-5