Abstract
The major concerns related to transoral laser surgery (TLS) for T1a glottic carcinoma are disease control and postoperative voice. This study examines the efficacy of the excision and ablation strategy of TLS using the 532-nm pulsed potassium-titanyl-phosphate (KTP) laser as an alternative to the conventional carbon dioxide (CO2) laser in treating T1a glottis carcinoma. The tumor was excised using KTP laser, followed by circumferential ablation of the mucosa surrounding the surgical margin in a non-contact manner using the KTP laser. Local control was obtained in 22 of 24 patients (91.7 %). Mean scores on Voice-Related Quality of Life questionnaire (V-RQOL) and the Voice Handicap Index-10 (VHI-10) were 81.0 and 6.2, respectively. A highly significant correlation was observed between scores of V-RQOL and adjusted VHI-10 (r = 0.96). TLS with a KTP laser for early glottic carcinoma achieved acceptable local control and postoperative voice comparable to those with a CO2 laser reported in the literature, suggesting that the procedure based on an excision and ablation strategy can be considered oncologically and functionally acceptable for this lesion.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Radiotherapy (RT) is one of the most common treatment options for primary T1aN0M0 early glottic carcinomas. The 5-year local control rate for RT in such tumors reaches 93 % [1]. However, surgery can also be considered as an initial treatment because there is a possibility of radiation-induced cancer, especially in young patients, and because RT may be required for a second primary head and neck cancer in the future. Among several surgical procedures, transoral laser surgery (TLS) is an established treatment modality for primary T1a glottic carcinoma. The carbon dioxide (CO2) laser has been classically used for this purpose [2]. However, the 532-nm pulsed potassium-titanyl-phosphate (KTP) laser, another clinically available laser, is currently receiving attention because its selectivity for hemoglobin leads to ablation of aberrant neovascularity.
One of the major concerns of TLS for primary glottic carcinoma is disease control. Another major concern is voice quality, which might play a role in decisions about treatment strategies. The present prospective report documents the oncologic and vocal results of a TLS with KTP laser (TLS-KTP) to treat primary T1a glottic carcinoma.
Patients and methods
Patients
Twenty-four patients, including 23 males and 1 female, diagnosed as having primary T1a glottic squamous cell carcinoma, underwent TLS-KTP between 2002 and 2010 at Kanazawa University Hospital, Japan. Eligibility criteria for the surgery included clinically negative neck (cN0), adequate exposure of the glottic region, absence of contraindications to general anesthesia, the ability to understand and willingness to sign a written informed consent document, and absence of previous surgery or RT for laryngeal cancer. All patients in this series fulfilled these criteria. Eleven patients who did not agree to the surgical treatment were treated with radiotherapy.
Surgical procedure
Ipsilateral vestibulotomy was performed in all cases prior to cordectomy in order to evaluate the extension of the tumor (Fig. 1a). Then, dilated microvessels surrounding the tumor were ablated using the KTP laser (4.5 W, pulsed mode; Fig. 1b). Surgical procedures included 20 type II, namely, subligamental, cordectomies, and 4 type III, namely, transmuscular, cordectomies, according to the European Laryngological Society Working Committee [3]. Although the definition of transmuscular cordectomy includes resection of either superficial or deep muscle layer, all four procedures were the former. Tumor resection with a surgical margin of at least 2 mm was performed using the KTP laser (4.5 W; Fig. 2). Surgical resection was basically performed with pulsed mode; however, continuous mode was also used in an area where deep invasion was suspected. The resection margins and bed of each tumor were pathologically confirmed by examination of frozen sections. After removal of the tumor, the remaining microvessels surrounding the resection margin were further ablated using a KTP laser in a non-contact manner (4.5 W, pulsed mode; Fig. 3). The postoperative appearance of vocal cord became almost normal within a couple of months in most cases (Fig. 4).
Pre-cordectomy microlaryngoscopic image after ipsilateral vestibulotomy is shown (a). Arrowheads indicate the resection margin of vestibulotomy. Arrows indicate vascular dilatation around the glottic carcinoma. Gauze was introduced into subglottic space. Ablation of dilated microvessels was performed prior to resection of the tumor (b). Gauze was introduced into subglottic space
QOL questionnaires
The Voice-Related Quality of Life questionnaire (V-RQOL) is a ten-item self-administered validated voice outcome measure [4]. Scores are reported in two domains (social–emotional and physical functioning), and total score ranges from 0 to 100. A higher score indicates a better voice-related QOL. The Voice Handicap Index-10 (VHI-10) scale, a short form of the Voice Handicap Index, is a ten-item self-administered validated instrument that measures patient disability as a result of voice disorders [5]. Scores range from 0 to 40, in which a lower score indicates a better voice-related QOL. An adjusted VHI-10, ranging from 0 to 100, in which a higher index indicates a better voice-related QOL, was also calculated to assess the correlation with the V-RQOL score. Patients were asked to complete both questionnaires 6 months after TLS-KTP.
Results
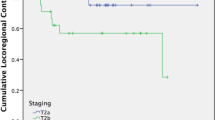
The mean and median ages of patients were 67.8 and 73 years, respectively (range, 41–82 years). The postoperative follow-up period for patients ranged from 12 to 84 months (mean, 40.6 months; median, 40 months). Of 24 patients, local control was obtained in 22 patients (91.7 %) after the initial TLS-KTP. The remaining two patients were rescued by the second TLS-KTP. There were two deaths due to lung cancer 14 and 20 months after the initial TLS-KTP without any sign of recurrent glottic cancer.
The surgical margin evaluated using resected tissue containing glottic tumor demonstrated a negative margin in 17 procedures. In the remaining seven procedures, tumor was close to, but not exposed to, the surgical margin, which was defined as a marginal margin. Both of the two recurrent cases had demonstrated a marginal surgical margin. Both recurrences developed contiguous to the anterior commissure.
Mean V-RQOL score (total) was 81.0 (Table 1). Mean social–emotional domain and physical functioning domain of V-RQOL scores were 84.4 and 78.8, respectively (Table 1). Mean VHI-10 score was 6.2 (Table 1). Unfortunately, this series does not contain a sufficient number of patients treated with either RT or TLS using CO2 laser (TLS-CO2) for comparison. A strong significant correlation was observed between V-RQOL and adjusted VHI-10 scores (r = 0.96 by Spearman’s rank correlation coefficient).
Discussion
Oncological outcome is the most important concern in the treatment of laryngeal cancer. TLS-CO2 provides a rate of local control comparable to that of RT for primary early glottic carcinoma as Gallo et al. reported that local control was achieved in 110 of 117 cases (94 %) [6]. Although the procedures for cordectomy were usually type IV (total cordectomy) in that study, Goor et al. also reported that local control for type I (submucosal) or type II cordectomy was achieved in 51 of 54 cases (91.4 %) of T1a glottic carcinoma [7], suggesting that total cordectomy is not necessarily required for all T1a lesions.
Lasers of different wavelengths produce energy that is absorbed by different substances within a tissue. Therefore, CO2 laser and KTP laser have different degrees of penetration, scatter and thermal effect in tissues [8]. CO2 laser has a wavelength in the infrared region (10,600 nm) and is absorbed primarily by water. It has been found in rat tongue epithelia to result in a microscopic damage zone with an average depth of 250 to 500 μm [9], suggesting less thermal damage to the surrounding tissues. This seems to be why the CO2 laser has been preferentially used in TLS for T1a glottic carcinoma.
KTP laser has a wavelength in the visible region (532 nm) and is absorbed by pigments containing its complementary colors, such as hemoglobin and melanin. Therefore, the KTP laser can be used for photoangiolysis (also known as microvascular ablation) based on the concept of selective photothermolysis [10]. It was previously reported that varices and ectasia of the vocal folds have been successfully treated with KTP laser [11]. Furthermore, laryngeal papillomatosis was recently shown to be successfully treated with KTP laser [12].
The versatility of KTP laser is shown by its use in treating dysplasia of the vocal cord [13]. However, there have been only a limited number of reports describing the availability of KTP laser for early laryngeal carcinoma [14]. It was emphasized that KTP laser is available for bilateral glottic carcinoma, which included conventional resection for the predominant side and laser photoangiolysis for the other less involved side. Photoangiolysis for neoplastic lesion is based on the concept of tumor angiogenesis process proposed by Folkman [15], implying that microinvasive carcinoma would be a good indication for the procedure; however, gross lesion itself would not be an indication. An experimental study using an established animal model demonstrated that complete resolution of mucosal squamous cell carcinoma in hamster cheek pouch following laser photoangiolytic treatments was observed in all lesions measuring less than 2 mm, in two of six lesions measuring between 2 and 5 mm, and in none of three lesions greater than 5 mm [16]. In the present study, we utilized a combination of KTP laser excision accompanied by photoangiolytic ablation of the circumferential microvessels for gross unilateral glottic carcinoma. Because certain removal of tumor by excision as well as diminished opportunity for angiogenesis by ablation is achieved, the excision and ablation strategy is rational and is expected to be widely used.
There were two recurrences in the present series, both of which occurred contiguously to the anterior commissure. This indicates that the ablation during TLS-KTP was not sufficient near the anterior commissure owing to hesitancy in performing vigorous treatment at the region in order to prevent glottic webbing. However, Burns et al. reported that none of the 51 patients with laryngeal papillomatosis who presented with anterior commissure involvement developed new webbing or synechia after KTP laser treatment [12], suggesting that further improvement of local control can be achieved with TLS-KTP.
Thus, oncological availability of TLS-KTP was demonstrated in the present study. Therefore, if the functional outcome of TLS-KTP is at least equal to that of TLS-CO2, the excision and ablation strategy in the present study may have further potential as an alternative to, or even a substitute for, TLS-CO2.
Functional outcome is another major concern during the treatment of laryngeal cancer. There are several ways to evaluate postoperative voice including auditory perceptual analysis and acoustic voice parameters; however, both correlate poorly with patient-perceived vocal outcome [17, 18]. How a patient regards voice impairment varies according to the individual; therefore, patient-based outcome assessments may have much greater importance. Several questionnaires could be used to assess posttreatment voice outcome in laryngeal cancer [19–24]. We attempted to evaluate voice-related QOL in T1a glottic carcinoma patients treated with TLS-KTP using two questionnaires, namely, VHI-10 and V-RQOL, both of which are also available in Japanese.
A meta-analysis review demonstrated that VHI, the original version of VHI-10, provides reliable assessment of posttreatment voice outcomes for early glottic carcinoma [25]. In addition, the development of VHI-10 provides a powerful representation of VHI that takes less time for the patient to complete without loss of validity, indicating that VHI-10 can replace VHI as an instrument to quantify the patient's perception of their voice handicap [5]. Rosen et al. reported that VHI-10 scores for control subjects, patients with Reinke edema, and patients with recurrent nerve paralysis were 3.38, 18.30, and 25.72, respectively [5]. Therefore, the mean VHI-10 score of patients obtained in the present study is considered acceptable.
The other questionnaire used in the present study, V-RQOL, has been reported to perform well in tests of reliability, validity, and responsiveness [4]. In that report, V-RQOL scores for voice-related patients and non-voice-related patients were 98.0 and 53.5, respectively. Furthermore, average V-RQOL scores for patients whose self-assessments of voice quality were poor/fair, good, and excellent/very good were 53.1, 83.1, and 95.0, respectively. Fung et al. reported that the V-RQOL scores for healthy volunteers and laryngeal cancer patients who had received chemoradiotherapy were 98.0 and 80.3, respectively [22]. Therefore, the mean V-RQOL score of patients obtained in the present study is also considered acceptable. Scores of adjusted VHI-10 and V-RQOL correlated well in the present study, suggesting that these two questionnaires could be used to evaluate postoperative voice after TLS-KTP.
Conclusions
The present data imply that TLS-KTP for early glottic carcinoma achieved acceptable local control and postoperative voice comparable to those with TLS-CO2 reported in the literature, suggesting that the excision and ablation strategy in the present study can be considered oncologically and functionally acceptable.
References
Cummings BJ (1994) Definitive radiation therapy for glottic cancer. In: Smee R, Bridger GP (eds) Laryngeal cancer. Elsevier, Amsterdam, pp 9–13
Vaughan CW, Strong MS, Jako GJ (1978) Laryngeal carcinoma: transoral treatment utilizing the CO2 laser. Am J Surg 136:490–493
Remacle M, Eckel HE, Antonelli A et al (2000) Endoscopic coredectomy. A proposal for a classification by the Working Committee, European Laryngological Society. Eur Arch Otorhinolaryngol 257:227–231
Hogikyan ND, Sethuraman G (1999) Validation of an instrument to measure voice-related quality of life (V-RQOL). J Voice 13:557–569
Rosen CA, Lee AS, Osborne J et al (2004) Development of and validation of the voice handicap index-10. Laryngoscope 114:1549–1556
Gallo A, de Vincentiis M, Manciocco V et al (2002) CO2 laser cordectomy for early-stage glottis carcinoma: a long-term follow-up of 156 cases. Laryngoscope 112:370–374
Goor KM, Peeters JGE, Mahieu HF et al (2007) Cordectomy by CO2 laser or radiotherapy for small T1a glottic carcinomas: costs, local control, survival, quality of life, and voice quality. Head Neck 29:128–136
Lesinski SG, Palmaer A (1989) Lasers in otosclerosis: CO2 vs. argon and KTP-532. Laryngoscope 99:1–8
Fleiner B, Plath T (1995) Histological evaluation of leukoplakia following CO2 laser excision: a clinical and experimental study. Adv Otorhinolaryngol 49:125–129
Anderson RR, Parrish JA (1981) Microvasculature can be selectively damaged using lasers: a basic theory and experimental evidence in human skin. Lasers Surg Med 1:263–276
Zeitels SM, Akst LM, Burns JA et al (2006) Pulsed angiolytic laser treatment of ectasias and varices in singers. Ann Otol Rhinol Laryngol 115:571–580
Burns JA, Zeitels SM, Akst LM et al (2007) 532nm pulsed potassium-titanyl-phosphate laser treatment of laryngeal papillomatosis under general anesthesia. Laryngoscope 117:1500–1504
Burns JA, Friedman AD, Lutch MJ et al (2010) Value and utility of 532 nanometre pulsed potassium-titanyl-phosphate laser in endoscopic laryngeal surgery. J Laryngol Otol 124:407–411
Zeitels SM, Burns JA, Lopez-Guerra G et al (2008) Photoangiolytic laser treatment of early glottis cancer: a new management strategy. Ann Otol Rhinol Laryngol 117(suppl 199):1–24
Folkman J (1971) Tumor angiogenesis: therapeutic implications. N Engl J Med 285:1182–1186
Burns JA, Lopez-Guerra G, Kobler JB et al (2011) Pulsed potassium-titanyl-phosphate laser photoangiolytic treatment of mucosal squamous cell carcinoma in the hamster cheek pouch. Laryngoscope 121:942–946
Rydell R, Schalen L, Fex S et al (1995) Voice evaluation before and after laser excision vs. radiotherapy of T1A glottic carcinoma. Acta Otolaryngol 115:560–565
Lehman JJ, Bless DM, Brandenburg JH (1988) An objective assessment of voice production after radiation therapy for stage I squamous cell carcinoma of the glottis. Otolaryngol Head Neck Surg 98:121–129
Loughran S, Calder M, MacGregor FB et al (2005) Quality of life and voice following endoscopic resection or radiotherapy for early glottic cancer. Clin Otolaryngol 30:42–47
Brondbo K, Benninger MS (2004) Laser resection of T1a glottic carcinomas: results and postoperative voice quality. Acta Otolaryngol 124:976–979
Peeters AJ, van Gouh CD, Goor KM et al (2004) Health status and voice outcome after treatment for T1a glottic carcinoma. Eur Arch Otorhinolaryngol 261:534–540
Fung K, Yoo J, Leeper HA et al (2001) Vocal function following radiation for non-laryngeal versus laryngeal tumors of the head and neck. Laryngoscope 111:1920–1924
Fung K, Lyden TH, Lee J et al (2005) Voice and swallowing outcomes of an organ-preservation trial for advanced laryngeal cancer. Int J Radiat Oncol Biol Phys 63:1395–1399
Oridate N, Homma A, Suzuki S et al (2009) Voice-related quality of life after treatment of laryngeal cancer. Arch Otolaryngol Head Neck Surg 135:363–368
Cohen SM, Garrett CG, Dupont WD et al (2006) Voice-related quality of life in T1 glottic cancer: irradiation versus endoscopic excision. Ann Otol Rhinol Laryngol 115:581–586
Conflict of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Murono, S., Endo, K., Kondo, S. et al. Oncological and functional outcome after transoral 532-nm pulsed potassium-titanyl-phosphate laser surgery for T1a glottic carcinoma. Lasers Med Sci 28, 615–619 (2013). https://doi.org/10.1007/s10103-012-1121-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-012-1121-4