Abstract
This study aims to investigate the effect of different energy densities provided by low-level laser therapy (LLLT) on the morphology of scar tissue and the oxidative response in the healing of secondary intention skin wounds in rats. Twenty-four male adult Wistar rats were used. Skin wounds were made on the backs of the animals, which were randomized into three groups of eight animals each as follows, 0.9% saline (control); laser GaAsAl 30 J/cm2 (L30); laser GaAsAl 90 J/cm2 (L90). The experiment lasted 21 days. Every 7 days, the wound contraction index (WCI) was calculated and tissue from different wounds was removed to assess the proportion of cells and blood vessels, collagen maturation index (CMI), thiobarbituric acid reactive substance (TBARS) levels and catalase activity (CAT). On the 7th and 14th days, the WCI and the proportion of cells were significantly higher in groups L30 and L90 compared to the control (p < 0.05). At all the time points analyzed, there was a greater proportion of blood vessels and a higher CMI in group L90 compared to the other groups (p < 0.05). On the 7th and 14th days, lower TBARS levels and increased CAT activity were found in the L90 group compared to the control (p < 0.05). On the 7th day, a moderately negative correlation was found between TBARS levels and WCI, CMI and CAT in all the groups. LLLT may modulate the oxidative status of wounded tissue, constituting a possible mechanism through which the LLLT exerts its effects in the initial phases of tissue repair.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
It has been systematically shown that low-level laser therapy (LLLT) is able to modify the morphology of scar tissue in skin wounds due to the positive influence on the proliferation and differentiation of fibroblasts, neoangiogenesis, and synthesis of collagen and elastin [1–8]. Traditionally, these aspects have been used as important markers of the efficacy of LLLT, since they are directly involved in efficiency of tissue repair [1, 9–11]. Recently, some studies have rekindled interest in investigating the effects of LLLT on biochemical parameters associated with the healing process [4, 12–14]. Biomarkers of oxidative stress and antioxidant defense have been the target of recent studies on the effect of oxidative stress on the healing process of skin wounds [3, 14, 15]. There are reports that exposing cells to laser beams stimulates the electron transport chain, leading to an increase in the synthesis of adenosine triphosphate [13, 16] and reactive oxygen species (ROS) such as O −2 , OH−, NO, and H2O2 [17, 18]. Furthermore, the results of previous studies have shown that in the normal healing process, although ROS production increases, LLLT also enhances antioxidant enzyme activity, minimizing the occurrence of oxidative damage to the healing tissue [5, 11]. Therefore, the balance between ROS production and the effect of the antioxidant system is believed to be directly related to the healing time and the quality of the wound tissue [12, 18, 19]; however, this is a question that remains to be fully clarified. It has been suggested that LLLT, depending on the dose, duration of irradiation applied to the wound, and the energy density used, may alter ROS production and antioxidant defense mechanisms [3, 12]. Nevertheless, the data available up to the present time are inconclusive.
Previous studies have shown that gallium arsenide aluminum laser (GaAsA1 λ 830 nm), when used at an energy density of 1–20 J/cm2, is capable of promoting healing in skin wounds in humans and laboratory animals [2, 5, 6]. Nevertheless, with relation to this particular type of laser, data on the effect of energy densities >20 J/cm2 on healing response and the dose–response effect of this stimulation are sparse and conflicting. Therefore, the objective of this study was to investigate the effect of different energy densities provided by LLLT on the morphology of scar tissue and the oxidative response induced in the healing process of secondary intention skin wounds in rats.
Material and methods
Animals
Twenty-four male Wistar rats (Rattus norvegicus) weighing 325.38 ± 27.92 g, from the Federal University of Viçosa (UFV) were used. During the experiment, the animals were allocated in individual cages that were cleaned daily and maintained in a environment with temperature (22 ± 2°C), humidity (60–70%) and illumination (12 h light/dark cycles) controlled. Water and standard rat chow were provided ad libitum. All the procedures involved in the experimental protocol were approved by the Animal Ethics Committee of the UFV (registration 005/2008).
Experimental design
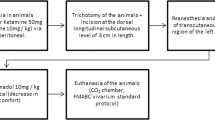
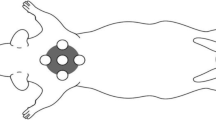
To create the wounds, the animals were anesthetized with ketamine and xylazine via intraperitoneal injection (60 mg/kg body weight). A trichotomy was performed on the dorsolateral region of all the animals and the area was thoroughly defatted using ethyl ether (Merck®, Rio de Janeiro, Brazil) followed by the use of 10% povidone–iodine for antisepsis (Johnson Diversey®, Rio de Janeiro, Brazil). Three circular secondary intention wounds of 12.5 mm in diameter were made by performing a surgical incision in the skin and subcutaneous cell tissue using a scalpel until exposure of the dorsal muscular fascia [7]. The animals were randomized into three treatment groups with eight animals in each group: Control, 0.9% saline solution; Group L30, GaAsA1 laser (λ 830 nm, 30 J/cm2); and Group L90, GaAsAl laser (λ 830 nm, 90 J/cm2). The laser used (Quasar®, Dentoflex, São Paulo, Brazil) has a power output of 90 mW, continuous wave, infrared spectrum (invisible), collimated beam with, area of the spot of 0.0035 cm2, and had been previously calibrated by the manufacturer. Both laser groups were treated at a power density of 0.073 W/cm2 on the wound surface. The laser light was applied during 410 s in the group L30 (energy density of 30 J/cm2) and 1,230 s in the group L90 (energy density of 30 J/cm2). The probe of the device positioned perpendicularly about 3 mm from the wound surface. The wounds were cleaned daily with 0.9% saline solution immediately prior to laser application. In all cases, treatment was initiated 6 h after the wounds were made and repeated once a day thereafter for the 21 days of the experiment [7].
Calculation of the area and the rate of wound contraction
The healing response of wound closure was evaluated by measuring the wound area every 7 days in digitized images with the dimensions of 320 × 240 pixels (24 bits/pixel) obtained using a digital video camera (W320, Sony, Tokyo, Japan). The wound areas were calculated by computerized planimetry using the Image Pro-Plus program version 4.5 (Media Cybernetics, Silver Spring, USA), previously calibrated. Wound contraction index (WCI) was calculated using the following ratio: initial area of the wound (Ao) − area on the day of measurement (Ai) / initial area of the wound (Ao) × 100 [20]. The third wound was selected for analysis of the progress of the healing process because it was from this wound that tissue was collected on the final day of the experiment (21st).
Stereology
Tissue fragments were collected from different wounds every 7 days, using a scalpel and the same anesthetic procedure previously described. Each fragment contained tissue removed from the center of the wound and the uninjured part of the tissue removed from a region adjacent to the border of the wound that did not receive laser radiation [7].
The fragments collected were fixed in Karnovsky’s solution, dehydrated in ethanol, cleared in xylol and embedded in paraffin. Semi-serial 4-μm-thick histological sections were obtained using a rotary microtome (Leica Multicut 2045®, Reichert-Jung Products, Germany), using one out of every ten sections to avoid repeating analysis of the same histological area. The sections were stained with hematoxylin and eosin for analysis of the fibroblasts and blood vessels. Sirius red (Sirius red F3B, Mobay Chemical Co., Union, New Jersey, USA) stain was used to differentiate the collagen fibers under polarizing microscopy [21]. The slides were visualized using a BX-60® light microscope (Olympus, São Paulo, Brazil) connected to a digital camera (QColor-3®, Olympus, São Paulo, Brazil). Using a ×20 objective lens, eight histological fields were selected at random on each slide, making a total tissue area of 5.37 × 106 μm2 submitted to stereological analysis. For this analysis, a grid containing 300 points within a standard test area (AT) of 73 × 103 μm2 was superimposed over each image. The stereological parameters of volumetric density (Vv) were calculated by counting the points that occurred over fibroblasts, blood vessels, type I and type III collagen, using the ratio: Vv = P P/P T; in which P P is the number of points occurring over the structure of interest and P T is the total number of points on the test system [22]. Analysis of the collagen was based on the birefringence properties of the collagen fibrils, since under polarization the thick collagen fibers (type I) appear in shades of bright color ranging from red to yellow, whereas thin reticular fibers (collagen type III) are shown in bright green. The collagen maturation index (CMI) was calculated using the ratio% collagen I / % collagen III. The length density (Lv) of blood vessels was estimated by the relationship, Lv [vessels] = 2Q A mm/mm3 where Q A is the number of blood vessels profiles in the AT, calculated by the relationship: Q A = Σ profiles/AT [7]. The stereological analysis was performed using the Image Pro-Plus program, version 4.5 (Media Cybernetics®, Silver Spring, USA).
Biochemical analysis
Fragments of tissue were collected from each wound, rapidly frozen (−196°C) in liquid nitrogen, and stored in a freezer at −80°C. Samples of these fragments were homogenized in phosphate-buffered saline and centrifuged at 5°C, the supernatant being used for analysis of catalase (CAT) and thiobarbituric acid reactive substances (TBARS), which are markers of lipid peroxidation. CAT activity was evaluated using the Aebi method [23] by measuring the decomposition rate of hydrogen peroxide (H2O2). TBARS measurement was performed in accordance with the protocol described by Gutteridge and Halliwell [24]. The biochemical data were normalized in relation to total protein levels in the supernatant, quantified according to the Bradford method [25].
Statistical analysis
The data were expressed as measures of central trend, means and standard deviations (mean ± S.D.). The morphological and biochemical data were subjected to Kruskal–Wallis test for multiple comparisons. The relationship between lipid peroxidation and morphological parameters of the scar tissue was investigated by Spearman correlation coefficient. In all analysis significance level of 5% was used. The tests were performed using the GraphPad Prism 5.0® statistical software program (GraphPad Software, Inc, California, USA).
Results
The reduction in the size of the wound on the 7th and 14th days was significantly greater in the irradiated groups compared to the control group. At these points, the best results were found in the group L90 (p < 0.05). On day 21, all animals in all groups had completely healed wounds (Table 1).
In all investigated time points, animals in the L90 group showed a proportion of fibroblasts (Vv [fibroblasts]), blood vessels (Vv [vessels]), length and density of blood vessels (Lv [vessels]) significantly higher compared to other groups (p < 0.05). On day 21, there were a significantly lower number of cells in the L90 group compared with the other two groups (Figs. 1a, b, d and 2). On days 7 and 14, there was a predominance of type III collagen fibers in all groups. At all times, the proportion of type I collagen fibers was higher in the L90 group compared to the other groups (p < 0.05; Fig. 1c). At the end of the experiment (day 21), type I collagen fibers were widely distributed in the scar tissue in the group L90. In the other groups, was observed high density of type III collagen (Fig. 1e). There was no significant difference in any morphological parameter in non-irradiated unharmed tissue from the different groups investigated.
Effect of high-energy density provided by low-level laser therapy on stereological parameters in skin wounds from Wistar rats (a–d). e Representative photomicrographs of the scar tissue at the end of the experiment (day 21; Sirius red staining under polarized light, bar 60 μm). Tissue fragments were collected every 7 days for 21 days of treatment. Control 0.9% saline solution, L30 laser 30 J/cm2, L90 laser 90 J/cm2. Day 0 represents the unwounded tissue. Data are reported as mean ± S.D. *†Statistical difference between groups (p < 0.05); *compared to the control group, †comparison between L30 and L90
Representative photomicrographs of histological sections of skin of rats stained with hematoxylin and eosin observed under light microscope. Tissue fragments were collected every 7 days for 21 days of treatment (bar 25 μm). Control saline 0.9%, L30 Laser 30 J/cm2, L90 90 J/cm2 laser. Day 0 represents the tissue unharmed
On the 7th and 14th days of treatment, TBARS levels were significantly lower and CAT activity was higher in the L90 group compared to the control group (p < 0.05). No significant differences were found in TBARS levels and CAT activity between the control and L30 groups at either of these time points. In non-irradiated unharmed tissues and on the 21st day, no statistically significant differences in TBARS and CAT were found between the three groups investigated (Fig. 3a, b).
Effect of high-energy density provided by low-level laser therapy on the levels of thiobarbituric acid reactive substances (TBARS) and catalase (CAT) activity in skin wounds from Wistar rats. Tissue fragments were collected every 7 days for 21 days of treatment. Control saline 0.9%, L30 Laser 30 J/cm2; L90 90 J/cm2 laser. Day 0 represents the tissue unharmed. Data are reported as mean ± S.D. *†Statistical difference between groups (p < 0.05); *compared to the control group, †comparison between L30 and L90
A moderate inverse correlation was found between TBARS levels in the wounded tissue and the CMI, WCI and CAT activity in all the study groups (Table 2).
Discussion
The findings of the present investigation contradict reports from previous studies indicating that LLLT stimulates tissue healing, principally at energy densities of 2–4 J/cm2, whereas higher energy densities may result in the opposite effect [2, 26]. Thus, the proportion of cells and blood vessels in the wounded tissue and the speed of the wound-healing process was greater in the group treated with the 90 J/cm2 density. Nevertheless, Gonçalves et al. [7] showed that the GaAsAl laser applied with an energy density of 60 J/cm2 was more effective in stimulating neoangiogenesis than 30 J/cm2. Furthermore, Corazza et al. [27] reported that a dose of 20 J/cm2 effectively increased the fibroblasts proliferation and the neoangiogenesis in skin wounds. Several mechanisms have been associated with the effects of LLLT, which include a reduction in tissue edema, enhanced synthesis in granulation tissue and the production of cytokines and growth factors such as tumor necrosis factor-alpha, insulin-like growth factor-I, and fibroblast growth factor by macrophages, T-lymphocytes, fibroblasts and keratinocytes, factors recognized to be involved in tissue repair [2, 4, 28, 29].
The extracellular matrix synthesis, particularly the collagen component, is an important participant in the wound healing process [5–7, 30, 31]. In the LLLT, an inversely proportional ratio between the wavelength and energy density has been reported to affect collagen production [32, 33], although this ratio remains controversial. In the present study, with a high wavelength and energy density of 90 J/cm2, LLLT was able to induce more effective collagen maturation. The enhanced maturation and rearrangement of the collagen in the healing tissue have important implications to the increased mechanical resistance of the newly formed tissue, which occurs throughout the collagen remodeling process as a consequence of the gradual substitution of type III for type I collagen fibers and the increased molecular interactions between the newly formed fibers [7, 34–37]. According to Meirelles et al. [11], enhanced collagen maturation may be seen on the 21st day of LLLT at an energy density of 20 J/cm2. Moreover, in the study conducted by Mendez et al. [33], use of a GaAlAs laser (λ 830 nm) at 50 J/cm2 successfully promoted intense collagen maturation in skin wounds in rats.
The present study confirmed previous findings [3, 12, 14] that trauma provoked a transitory rise in oxidative activity in the wounded tissue. Furthermore, LLLT was found to result in a marked reduction in lipid peroxidation (TBARS) and an increase in the activity of the antioxidant enzyme (CAT) in the scar tissue. In addition, a moderately negative correlation was found between lipid peroxidation and both the CMI and WCI on the 7th day in all the groups investigated, indicating a negative effect of the oxidative mediators on the wound-healing process.
Reports from previous studies that increased ROS levels in wounded tissue favors extracellular matrix synthesis [12, 35] should be interpreted with caution, since it may lead to an erroneous belief that ROS invariably promotes a better healing. In previous studies, increased ROS levels have been directly correlated with collagen deposition in the wounded tissue [19, 38]. However, there is sufficient evidence that oxidative stress constitutes an important pathogenic factor that leads to various degenerative diseases including tissue fibrosis in different organs such as the lungs, liver and kidneys [36, 39]. Under physiological conditions, the activity of the antioxidant enzymes neutralizes part of these ROS and reduces the oxidative lesion through tissue homeostasis. This mechanism determines the balance between pro-oxidant and antioxidant events, allowing the healing process to proceed normally [15]. However, under pathological conditions, the excess ROS increases the initial lesion through a cytotoxic mechanism, resulting in an abnormal healing that often leads to the occurrence of cell death, microvascular disorders and renders the inflammation chronic, characterized by a deceleration of tissue repair and fibrosis [19, 40].
It has been reported that LLLT is capable of modulating oxidative events in wounded tissue [3, 12, 14]. Two principal mechanisms are cited as being responsible for this modulation, the first resulting from a reduction in the migration and/or activity of inflammatory cells and consequently of ROS production, and the second from the stimulation of antioxidant enzyme synthesis and/or activity [3, 12, 14]. Indeed, the anti-inflammatory activity of LLLT has already been widely described [9, 14, 29]. In addition, the increased activity of antioxidant enzymes such as superoxide dismutase and CAT [18, 29] and regulation of the production of oxidative mediators such as the superoxide (O −2 ) and hydrogen peroxide (H2O2) radicals by LLLT has been associated with the control of collagen I and III gene expression [17, 29].
It is important to emphasize that in the present study, LLLT resulted in an increase in CAT activity, an event that was inversely correlated with lipid peroxidation biomarkers in the tissue samples collected from the wound on the 7th day. Interestingly, the wounds of the animals in the laser-treated groups also healed faster. Considering these findings, it is believed that the onset of the inflammatory reaction produced by the ROS and antioxidant activity is associated with the balance between destructive and repair processes, which may be profoundly affected by LLLT [3, 12]. Therefore, the present study admits the hypothesis that LLLT contributes towards achieving a balance between pro-oxidant and antioxidant events in such a way as to favor the healing process; hence it is not unrealistic to infer that both the down-regulation and up-regulation of ROS may hamper the healing process, since a surplus of these oxidative agents leads to tissue lesions [15, 19, 40]. On the other hand, however, depletion of these agents may block various cell-signaling pathways that directly or indirectly affect the healing process in the wounded tissue [37, 38].
There is sufficient evidence that the oxidative status of the tissue is controlled by a complex interaction between pro-oxidant and antioxidant mediators. Thus, although the present study has investigated the oxidation process by using a marker of lipid peroxidation (TBARS) and antioxidant status (CAT), the results of the effect of LLLT cannot be extended to the oxidation of proteins and nucleic acids, an issue that requires further investigation.
The results of the present study suggest that LLLT is able to stimulate the skin wound healing. Particularly, the highest energy density (90 J/cm2) proved to be potentially beneficial to the healing process through modulating the morphology and oxidative status of wounded tissue, representing an additional mechanism through which laser photobiostimulation exerts its effects, especially in the initial phases of the tissue repair process.
References
Woodruff LD, Bounkeo J, Brannon WM, Dawes KS, Barham CD, Waddell DL, Enwemeka CS (2004) The efficacy of laser therapy in wound repair: a meta-analysis of the literature. Photomed Laser Surg 22:241–247
Reddy GK (2004) Photobiological basis and clinical role of low-intensity lasers in biology and medicine. J Clin Photomed Laser Surg 23:289–294
Silveira PCL, Silva LA, Tuon T, Freitas TP, Streck EL, Pinho RA (2009) Effects of low-level laser therapy on epidermal oxidative response induced by wound healing. Braz J Phys Ther 13:281–287
Xavier M, David DR, Souza RA et al (2010) Anti-inflammatory effects of low-level light emitting diode therapy on achilles tendinitis in rats. Lasers Surg Med 42:553–558
Liu H, Dang Y, Wang Z, Chai X, Ren Q (2008) Laser induced collagen remodeling: a comparative study in vivo on mouse model. Lasers Surg Med 40:13–19
Gonçalves RV, Mezêncio JMS, Benevides GP, Matta SLP, Neves CA, Sarandy MM, Vilela EF (2010) Effect of gallium–arsenide laser, gallium–aluminum–arsenide laser and healing ointment on cutaneous wound healing in Wistar rats. Braz J Med Biol Res 43:350–355
Gonçalves RV, Novaes RD, Matta SLP, Benevides GP, Faria FR, Pinto MVM (2010) Comparative study of the effects of gallium–aluminum–arsenide laser photobiomodulation and healing oil on skin wounds in Wistar rats: a histomorphometric study. Photomed Laser Surg 28:597–602
Medrado AP, Pugliese LS, Reis SRA, Andrade ZA (2003) Influence of low level laser therapy on wound healing and its biological action upon myofibroblasts. Lasers Surg Med 32:239–244
Posten W, Wrone DA, Dover JS, Arndt KA, Silapunt S, Alam M (2005) Low-level laser therapy for wound healing: mechanism and efficacy. Dermatol Surg 31:334–340
Stadler I, Lanzafame RJ, Evans R, Narayan V, Dailey B, Buehner N, Naim JO (2001) 830-nm irradiation increases the wound tensile strength in a diabetic murine model. Lasers Surg Med 28:220–226
Meirelles GCS, Santos NJ, Chagas PO, Moura AP, Pinheiro ALB (2008) A comparative study of the effects of laser photobiomodulation on the healing of third-degree burns: a histological study in rats. Photomed Laser Surg 26:159–166
Fillipin LI, Mauriz JL, Vedovelli K, Moreira AJ, Zettler CG, Lech O, Marroni NP, González-Gallego J (2005) Low-level laser therapy (LLLT) prevents oxidative stress and reduces fibrosis in rat traumatized Achilles tendon. Lasers Surg Med 37:293–300
Silveira PC, Streck EL, Pinho RA (2007) Evaluation of mitochondrial respiratory chain activity in wound healing by low-level laser therapy. J Photochem Photobiol 86:279–282
Servetto N, Cremonezzi D, Simes JC, Moya M, Soriano F, Palma JA, Campana VR (2010) Evaluation of inflammatory biomarkers associated with oxidative stress and histological assessment of low-level laser therapy in experimental myopathy. Lasers Surg Med 42:577–583
Khodr B, Khalil Z (2001) Modulation of inflammation by reactive oxygen species: implications for aging and tissue repair. Free Radic Biol Med 30:1–8
Eells JT, Wong-Riley MT, VerHoeve J et al (2004) Mitochondrial signal transduction in accelerated wound and retinal healing by near-infrared light therapy. Mitochondrion 4:559–567
Kim YG, Pal SC, Lee SR (2000) Hairless mouse epidermal antioxidants and lipid peroxidation assessed by He–Ne laser. Lasers Surg Med 27:420–426
Karu T (1999) Primary and secondary mechanisms of action of visible to near-IR radiation on cells. J Photochem Photobiol 49:1–17
Poli G, Parola M (1997) Oxidative damage and fibrogenesis. Free Radic Biol Med 22:287–305
Agren MS, Mertz PM, Franzén LA (1997) Comparative study of three occlusive dressing in the treatment of full-thickness wounds in pigs. J Am Acad Dermatol 36:53–58
Junqueira LCU, Bignolas G, Brentani RR (1979) Picrosirius staining plus polarization microscopy, a specific method for collagen detection in tissue sections. Histochem J 11:447–455
Mandarim-de-Lacerda CA (2003) Stereological tools in biomedical research. Ann Acad Braz Sci 75:469–486
Aebi H (1984) Catalase in vitro. Meth Enzymol 105:121–126
Gutteridge JMC, Halliwel B (1990) The measurement and mechanism of lipid peroxidation in physiological systems. Trends Biochem 15:129–135
Bradford M (1976) A rapid and sensitive method for quantitation of microgram quantities of protein utilizing the principle of protein-dye-binding. Anal Biochem 72:248–254
Mester E, Mester AF, Mester A (1985) The biomedical effects of laser application. Lasers Surg Med 5:31–39
Corazza AV, Jorge J, Kurachi C, Bagnato VS (2007) Photobiomodulation on the angiogenesis of skin wounds in rats using different light sources. Photomed Laser Surg 25:102–106
Karu T (1987) Photobiological fundamentals of low-power laser therapy. IEEE J Quant Electron 23:1703–1717
Karu TI (2000) Mechanisms of low-power laser light action on cellular level. In: Simunovic Z (ed) Lasers in medicine and dentistry, 1st edn. Vitgraph, Rijeka, pp 97–125
Webb C, Dyson M (2003) The effect of 880-nm low level laser energy on human fibroblast cell numbers: a possible role in hypertrophic wound healing. J Photochem Photobiol 70:39–44
Steinstraesser L, Wehner M, Trust G et al (2010) Laser-mediated fixation of collagen-based scaffolds to dermal wounds. Lasers Surg Med 42:141–149
Nascimento PM, Pinheiro ALB, Salgado MAC, Ramalho LMP (2004) A preliminary report on the effect of laser therapy on the healing of cutaneous surgical wounds as a consequence of an inversely proportional relationship between wavelength and intensity: histological study in rats. Photomed Laser Surg 22:513–518
Mendez TMTV, Pinheiro ALB, Pacheco MTT, Nascimento PM, Ramalho LMP (2004) Dose and wavelength of laser light have influence on the repair of cutaneous wounds. J Clin Laser Med Surg 22:19–25
Saperia D, Gassberg E, Lyons RF, Abergel RP, Baneux P, Castel JC, Dwyer RM, Uitto J (1986) Demonstration of elevated type I and type III procollagen mRNA levels in cutaneous wounds treated with helium–neon laser. Biochem Biophys Res Commun 138:1123–1128
Reddy GK, Stehno-Bittel L, Enwemeka CS (1998) Laser photostimulation of collagen production in healing rabbit Achilles tendons. Lasers Surg Med 22:281–287
Polosukhin VV (1999) Ultrastructural study of the destructive and repair processes in pulmonary inflammation and following endobronchial laser therapy. Virchows Arch 435:13–19
Manoury B, Nenan S, Leclerc O, Guenon I, Boichot E, Planquois JM, Bertrand CP, Lagente V (2005) The absence of reactive oxygen species production protects mice against bleomycine-induced pulmonary fibrosis. Respir Res 6:1–12
Park SK, Kim J, Seomun Y et al (2001) Hydrogen peroxide is a novel inducer of connective tissue growth factor. Biochem Biophys Res Commun 284:966–971
Iglesias-De La Cruz MC, Ruiz-Torres MP, De Lucio-Cazana FJ, Rodriguez-Puyol M, Rodriguez-Puyol D (2000) Phenotypic modifications of human mesangial cells by extracellular matrix: the importance of matrix in the contractile response to reactive oxygen species. Exp Nephrol 8:97–103
Hensley K, Robinson KA, Gabbita SP, Salsman S, Floyd RA (2000) Reactive oxygen species, signaling and cell injury. Free Radic Biol Med 10:1456–1462
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gonçalves, R.V., Novaes, R.D., do Carmo Cupertino, M. et al. Time-dependent effects of low-level laser therapy on the morphology and oxidative response in the skin wound healing in rats. Lasers Med Sci 28, 383–390 (2013). https://doi.org/10.1007/s10103-012-1066-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-012-1066-7