Abstract
The heat-shock protein 70 gene (hsp70) has been exploited for Leishmania species identification in the New and Old World, using PCR followed by restriction fragment length polymorphism (RFLP) analysis. Current PCR presents limitations in terms of sensitivity, which hampers its use for analyzing clinical and biological samples, and specificity, which makes it inappropriate to discriminate between Leishmania and other trypanosomatids. The aim of the study was to improve the sensitivity and specificity of a previously reported hsp70 PCR using alternative PCR primers and RFLPs. Following in silico analysis of available sequences, three new PCR primer sets and restriction digest schemes were tested on a globally representative panel of 114 Leishmania strains, various other infectious agents, and clinical samples. The largest new PCR fragment retained the discriminatory power from RFLP, while two smaller fragments discriminated less species. The detection limit of the new PCRs was between 0.05 and 0.5 parasite genomes, they amplified clinical samples more efficiently, and were Leishmania specific. We succeeded in significantly improving the specificity and sensitivity of the PCRs for hsp70 Leishmania species typing. The improved PCR-RFLP assays can impact diagnosis, treatment, and epidemiological studies of leishmaniasis in any setting worldwide.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Leishmaniasis is one of the most neglected tropical diseases, with a major burden among the poorest segments of impoverished populations in Asia, Africa, South America and, in a lesser degree, Europe [1, 2]. It has been demonstrated that the clinical spectrum of the disease, prognosis, and response to treatment can vary according to the species [3–5]. Also epidemiological monitoring and vector and/or reservoir management rely on accurate parasite discrimination [6, 7]. Diagnosis of leishmaniasis currently focuses on parasite detection by microscopy, culture, and PCR. Molecular targets are either kinetoplast DNA (kDNA) [8] or genomic DNA (e.g. 18S rDNA [9]). Species discrimination requires species-specific PCRs, or PCR amplification followed by sequencing. Alternatively, digestion of the amplification product with a defined set of enzymes reveals restriction fragment length polymorphisms (RFLPs), which have been widely applied to discriminate Leishmania spp. from diverse geographical areas [10, 11].
Among the techniques used for both detection and typing, PCR amplification of the heat-shock protein 70 encoding gene (hsp70) has proven valuable [6]. However, it was initially used exclusively to analyze species of the L. (Viannia) subgenus, and the performance on other species, including those found in the Old World, had not been tested. Based on polymorphisms identified in a broad group of hsp70 Leishmania sequences [12], an RFLP strategy was designed to allow identification of most medically important species, including those of the subgenus L. (Leishmania) [13]. For its application, efficient amplification of all Leishmania species is crucial in order to obtain a sufficient amount of gene product for RFLP analysis from various environmental, clinical, and biological samples, which is not the case for the hsp70 protocol of García et al. [14] , in particular for the L. (Leishmania) subgenus. In addition, this PCR also amplifies other organisms (e.g. trypanosomes) that might be present in these specimen, which can interfere with the RFLP pattern.
The goal of the present study was to improve the sensitivity and specificity of the hsp70-PCR by using alternative primer sets, without compromising the discriminatory power of RFLP for identifying all medically important species worldwide. We also aimed at testing the new assays on DNA from reference strains and clinical samples, to determine their sensitivity and species discrimination potential.
Materials and methods
Strains and DNA
Table 1 lists the species and geographical origin of the 121 reference strains and isolates included in our study, representative of 14 Leishmania and two Trypanosoma species. A detailed listing is available in the supplementary Table ESM-1. From these, 114 Leishmania strains were tested in PCR-RFLP, while five were included only in the in silico analysis. As DNA was obtained from different sources, the reference species identification was based on various data such as zymodeme typing, RFLP analysis and gene sequencing. All DNAs were isolated from parasite cultures, and either parasites or DNA were obtained from the different institutes acknowledged at the end of this paper.
To test the analytical specificity of the PCRs, DNAs from clinical samples or cultures from various microorganisms and viruses were used: Plasmodium falciparum, Schistosoma mansoni, Trypanosoma cruzi, Trypanosoma rangeli, Trypanosoma brucei, Candida albicans, Candida parasilopsis, Cryptococcus neoformans, Haemophilus influenzae, Streptococcus pneumonia, Enterococcus, Mycobacterium tuberculosis, Mycobacterium habana, Epstein-Bar virus, Herpes zoster virus, Herpes simplex virus, Citomegalovirus, Staphylococcus epidermidis, Staphylococcus aureus, Pseudomonas aeroginosa, Escherichia coli, and Neisseria meningitides. These were obtained from various sources acknowledged at the end of the manuscript.
DNA from confirmed positive clinical samples was obtained from the centers mentioned in the acknowledgements section. Different diseases and sample types were represented, including biopsies, blood, scrappings, and aspirates. DNA was extracted using a variety of methods. All samples were taken according to the ethical guidelines of the respective institutes.
Primer design and in silico analysis of hsp70 coding sequences
Based on a previous alignment [12], three new PCR primer sets specific for the Leishmania genus were selected (Table 2). The fragments flanked by these primers contain polymorphisms for species differentiation already identified [13]. In silico RFLP analysis and prediction of the resulting fragments was performed with the software packages MEGA4 [15] and DNAMAN version 4.02 (Lynnon Biosoft, Quebec, Canada), as well as the online tools NEBcutter (tools.neb.com/NEBcutter2) and DistinctiEnz (www.bioinformatics.org/ydocreza/cgi-bin/restriction/DistinctiEnz.pl).
PCRs
Four hsp70-PCR protocols were performed (Table 2). PCR-G [14] was done according to previous reports [13]. PCR-F, PCR-N, and PCR-C were done in 50 μl total volume containing 1x Q solution; 1x standard PCR buffer; a total of 2.5 mM MgCl2; 0.8 μM of each primer; 200 μM of each deoxynucleoside triphosphate; and 1U HotStarTaq Plus DNA Polymerase (Qiagen, Hilden, Germany). Except when testing sensitivity or clinical samples, 10 ng of DNA was used. Concentrations were measured by spectrophotometry using the Nanodrop (ND1000, Thermo Scientific, Wilmington, DE, USA). Negative no-template controls were always included, along with a positive control consisting of 1 ng DNA from L. braziliensis strain MHOM/BR/75/M2903. The amplification conditions for the three new PCR variants were: denaturation at 95°C for 5 min; followed by 35 cycles of denaturation at 94°C for 40 sec, annealing at 61°C for 1 min (except PCR-C: 65°C), extension at 72°C for 1 min (except PCR-F: 2 min); and a final extension step of 10 min at 72°C. Thermal cycling was performed in either a PTC-150 (MJ Research, Waltham, MA, USA), a MyCycler™ (Bio-Rad, Foster City, CA, USA), or an iCycler (Bio-Rad). Analysis on a 2% agarose gel was used to verify the amplified product size.
Analytical sensitivity and specificity
The analytical sensitivity was determined for all four PCRs (Table 2) using several strains representing each species or species complex (Table ESM-1). Ten-fold DNA dilutions in water were tested, ranging from 10 fg to 10 ng/μl, whereby 1 μl was used for PCR. The presence of Leishmania DNA in the four lowest dilutions was confirmed by a diagnostic 18S rDNA-PCR [9]. The specificity of the PCRs was analyzed using the DNAs described above as template.
RFLP analysis
RFLP analysis was performed on amplicons from PCR-F, PCR-N, and PCR-C from 114 strains (Tables 1 and ESM-1). These are further referred to as RFLP-F, RFLP-N, and RFLP-C. Digests were performed in a total of 10 μl containing 5 μl of amplicon solution in 1x optimal buffer provided by the manufacturers, using 2U HaeIII (MBI Fermentas, St Leon-Rot, Germany); 2U BccI (New England Biolabs, Ipswich, MA, USA), 2U RsaI (MBI Fermentas), 2U MluI (MBI Fermentas); 2U BsaHI (MBI Fermentas); 2U BsaJI (MBI Fermentas), 2U HindII (MBI Fermentas), or 20U EcoRII (MBI Fermentas). For double digests with enzymes EcoRII and MluI, 10U and 20U were used respectively in buffer O, as the activity of MluI in this buffer is only 50%. Reactions were incubated overnight at 37°C, except for BsaJI (55°C). Subsequently, restriction patterns were analyzed by electrophoresis in a 3% small fragment agarose gel (Gentaur, Brussels, Belgium), running at 3.5 V/cm for 3 h. The GeneRuler™ 100 bp DNA Ladder (MBI Fermentas) was used as a size reference marker.
Results
For all 14 Leishmania species, the amplicon size for each PCR (data not shown) agrees with the in silico analysis (Table 2) and previous reports [13, 14]. A selection of results from the sensitivity study, showing one representative strain of each species or species complex, is depicted in Fig. 1. The 18S rDNA-PCR confirms the presence of Leishmania DNA in each dilution, down to 10 fg/μl. The hsp70 fragments amplified in all species. The detection limit of PCR-G differed according to the subgenus: whilst for L. (Viannia) parasites the procedure was able to detect between 10 (0.05 parasite genomes) and 100 (0.5 parasite genomes) fg of DNA, the detection limit for parasites belonging to subgenus L. (Leishmania) ranged from 0.1 to more than 1 ng. The overall sensitivity of PCR-F was better, detecting 10 fg of L. (Viannia) and 10–100 fg of L. (Leishmania). The detection limit of PCR-N and PCR-C was comparable for both subgenera, between 10 and 100 fg. When analyzing five clinical sample sets from different countries and diseases (Table 3), it was clear that PCR-F performed much better in amplifying Leishmania DNA as compared to PCR-G, as it amplified between two and ten times more samples. PCR-N and PCR-C performed only slightly better than PCR-F. With regard to the analytical specificity (figure available on request), no amplification was observed for PCR-F and PCR-N from species other than Leishmania. PCR-C showed an amplicon when DNA from M. tuberculosis was used, but its size differed from the Leishmania fragment. PCR-G amplified DNA from Leishmania, Trypanosoma cruzi, T. rangeli, and T. brucei.
Analytical sensitivity of the four PCRs (Table 2), compared to the 18S rDNA-PCR, as analyzed on agarose gel. Only the relevant part of the gels is shown. One representative isolate is depicted from each of the following Leishmania species: bra, L. braziliensis; per, L. peruviana; nai, L. naiffi; guy, L. guyanensis, pan, L. panamensis; lai, L. lainsoni; mex, L. mexicana species complex including L. garnhami and L. amazonensis; don, L. donovani; inf, L. infantum; aet, L. aethiopica; tro, L. tropica; maj, L. major. The DNA amount used per assay, ranging from 1 ng to 10 fg, is indicated on top
Nucleotide polymorphisms affecting restriction endonuclease recognition sites for differentiation of Leishmania species using PCR-F, PCR-N, and PCR-C, were identified in silico. Different schemes for discriminating medically important species from the New and Old World were designed, each relying on one to three digests for identification of all groups. They were applied on strains from all species from a diverse geographical origin (Table 1 and ESM-1, Fig. 2), which confirmed the in silico obtained results.
RFLP agarose gel patterns obtained from amplicons of the four PCRs in Table 2, and in different species and species complexes. Species abbreviation is as in Fig. 1, whereby bra* indicates isolates with a composite L. braziliensis – L. peruviana pattern. Per obtained pattern, only one representative image is depicted, in relation to the size markers (MM) on their left. This size marker is the GeneRuler™ 100 bp DNA Ladder (MBI Fermentas, St. Leon-Rot, Germany), showing fragments in multiples of 100 base pairs (bp), whereby some band sizes are indicated on the left in bp, and a grid across the figure is provided in the upper panels. a RFLP-F: the upper panel represents the groups as defined by digestion with HaeIII, the digests in the lower panel allow further separation within these groups. nai-1: MDAS/BR/79/M5533; nai-2: MDAS/BR/78/M5210. b RFLP-N: the upper panel digests allow a first separation of either Old World or New World species, which can be further distinguished using the digests below. c RFLP-C: HaeIII allows a first separation (upper panel), from which groups can be further typed using the digests in the lower panel. No intra-species variability was seen in any of the species when analyzing the isolates in Table 1 and ESM-1, except for L. braziliensis and L. naiffi, for which different patterns are shown next to each other in the relevant RFLPs
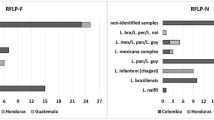
The discriminative power for each new RFLP analysis is as follows (Fig. 2). RFLP-F (Fig. 2a) typed five species from the Old World (L. major, L. tropica, L. aethiopica, L. donovani, L. infantum) and five from the New World (L. infantum, L. lainsoni, L. peruviana, L. guyanensis, L. panamensis). Of the 19 L. braziliensis isolates, ten shared the HaeIII pattern with L. naiffi MDAS/BR/79/M5533, while L. naiffi MDAS/BR/78/M5210 showed an extra faint band. In the RsaI digest, these 10 L. braziliensis isolates could not be distinguished from L. naiffi, but the remaining nine L. braziliensis showed a composite pattern with L. peruviana (indicated as bra* in Table 1 and ESM-1, and Fig. 2). Species from the L. mexicana complex (L. mexicana, L. amazonensis, L. garnhami) could not be separated, but the complex as a whole can be identified using HaeIII. RFLP-N (Fig. 2b) allowed differentiating four groups from the Old World (L. tropica/L. aethiopica, L. major, L. donovani, L. infantum) and seven from the New World (L. lainsoni, L. infantum, L. braziliensis/L. naiffi, L. peruviana, L. guyanensis/L. panamensis, L. mexicana complex, composite L. braziliensis bra*). Finally, RFLP-C (Fig. 2c) identified all five tested species from the Old World, as well as L. lainsoni from the New World. No intra-species differences were observed in any of the RFLPs, apart from the aforementioned cases of composite L. braziliensis (bra* in Table 1 and ESM-1, and Fig. 2) and L. naiffi.
Discussion
PCR-RFLP analysis of a 1422 bp hsp70 gene fragment (PCR-G) was already demonstrated to be valuable for discrimination of Leishmania species, both in the subgenera L. (Viannia) and L. (Leishmania) [6, 11, 13, 14]. However, sensitivity in the latter was poor. The new PCR variants (PCR-F, PCR-N, PCR-C) presented here showed an increased sensitivity of a factor 10,000 in L. (Leishmania), while sensitivity in the L. (Viannia) subgenus was comparable to PCR-G. In clinical samples however, we showed a significant improvement in amplification efficiency when comparing to PCR-G in both subgenera. This brings the typing potential of hsp70 to the same level for all Leishmania species, in view of the discriminative potential of the corresponding RFLPs. This was theoretically expected, as the new PCR primer sets were designed on the basis of all available Leishmania sequences, opposed to PCR-G having been developed specifically for L. (Viannia). An adequate sensitivity of the PCRs is of crucial importance for analyzing clinical and biological samples, which often contain a small number of parasites [16, 17]. It should be noted that in case the new PCRs show no or insufficient amplification from one PCR round, the new primer combinations can also be used in a (hemi-) nested PCR approach to further increase sensitivity, as was already applied in some clinical samples (data not shown). In such case either PCR-G or PCR-F can be used as the outer PCR.
The new PCR versions also showed an improved specificity for Leishmania. As already reported previously [14], our analysis confirmed the amplification of trypanosomatid species other than Leishmania with PCR-G, i.e. Trypanosoma cruzi, T. rangeli, and T. brucei. In the New World, T. rangeli, T. cruzi and Leishmania are sympatric in many areas [18, 19], emphasizing the importance of genus-specific PCRs. On the contrary, African trypanosome endemic areas are distinct from Leishmania foci, but in Uganda already both parasites occur [20], indicating a potential migration that could lead to both parasites being sympatric in certain regions in the future. None of the three newly designed PCRs amplified any of the trypanosomes. As for other organisms that potentially could cause mixed infections, such as bacteria, yeasts, and viruses, those included in the study did not amplify with any of the PCRs tested, except for an M. tuberculosis culture sample from which a product of different size as compared to Leishmania was amplified in PCR-C. These results highlight the potential of PCR-F, PCR-N, and PCR-C to be used as a first line molecular diagnostic tool to complement microscopy and simple serological tests where available, whereby a positive amplification is indicative of leishmaniasis. The amplified amplicon can then subsequently be digested in order to determine the species or species complex. It must be noted that for diagnostic purposes the PCRs should be evaluated in every specific setting, and negative PCRs must be confirmed with the most sensitive assays available, such as 18S rDNA [9] or kDNA PCR [21, 22].
The PCR-RFLP experiments on DNA from strains and isolates generally corroborated the results from in silico analysis. It should be emphasized that species discrimination for all RFLPs is based upon a step-wise approach, whereby a first digest (upper panels in Fig. 2) discriminates among broader groups, if needed followed by additional digests (lower panels in Fig. 2) to discriminate within these groups. Table ESM-2 gives an overview of the digests needed to discriminate all groups in the three RFLPs. Certainly upon implementation in a new setting, but also as a general practice, it is highly recommended to run all samples next to well-characterized references in order to compare fragment sizes on gel.
In the New World, identification is important for instance in the subgenus L. (Viannia), as some species can cause mucocutaneous disease, and a differential response to antimonial treatment has been documented [5, 23]. L. guyanensis, L. panamensis, L. lainsoni, L. peruviana, and L. infantum (syn. L. chagasi) can be discriminated using RFLP-F and RFLP-N, with the exception of L. guyanensis and L. panamensis being identical in RFLP-N (Table ESM-2). Species from the L. mexicana complex (L. mexicana, L. garnhami, L. amazonensis) can be distinguished as a group, but cannot be classified into their respective species. This is not surprising as also sequence analysis failed to cluster them accordingly [12], questioning their monophyly and species status. The discrimination of L. braziliensis and L. naiffi is not straightforward, as they often share the same pattern in RFLP-F and RFLP-N. For L. naiffi, the only exception is RFLP-F when using HaeIII, showing an additional fragment for one of the two tested isolates (Fig. 2a). Separating both species is necessary when sympatric transmission occurs, as in Brazil, where discrimination was suggested on the basis of PCR-G and restriction endonuclease BstUI [24]. However, not all L. braziliensis isolates are identical to L. naiffi, as almost half of them (9/19 bra* in Table 1 and ESM-1, see also Table ESM-2) displayed a mixed pattern, combining the L. braziliensis fragments with those of L. peruviana, being indicative of the presence of at least two hsp70 alleles. They originated from a wide geographical area (Bolivia and Peru), and may represent L. peruviana – L. braziliensis hybrids [25, 26], or genetic variation present within L. braziliensis. As yet, the clinical relevance of discriminating these parasites with both alleles is unclear. In conclusion, RFLP-F is recommended for species determination in the New World if L. guyanensis needs to be discriminated from L. panamensis. PCR-N has a slightly better analytical sensitivity as PCR-F (Fig. 1), and is expected to be less sensitive to PCR inhibitors because of its smaller size (Table 2), and can thus be used as an alternative. RFLP-C is of very limited use for separating New World species (Table ESM-2).
All medically important species from the Old World [27] can be identified by RFLP-F and RFLP-C, while in RFLP-N no distinction can be made between L. tropica and L. aethiopica. As RFLP-C is based upon a smaller PCR fragment, it may be less inhibited in clinical and biological specimen, and is therefore the method of choice. Taking into consideration the broad potential of RFLP-F across the entire globe, it might be a convenient option for travel clinics dealing with import Leishmania of unknown origin. In principle, L. major can be distinguished from L. donovani and L. infantum in RFLP-F after the first digest with HaeIII (Fig. 2a), but the size difference of the largest fragment is only 13 base pairs, often necessitating a second confirmation digest with HindII, as is the case in RFLP-C (Fig. 2c). Discriminating L. donovani from L. infantum requires yet an additional digest both in RFLP-F and RFLP-C.
Which one of the four now available PCRs (Table 2) is the most adequate, depends upon the particular situation. Origin of infection, sympatry of species, imported versus endemic pathology, clinical presentation, and type of samples, are determinants that will govern the choice of the most appropriate typing assay. Other studies have proposed PCR-based methods for distinguishing among neotropical and/or Old World Leishmania [24, 28–33]. Even though some of these included additional species as compared to those analyzed here, they generally focused on a more confined geographical representation of the genus. In addition, restriction digest schemes were often more complicated than those proposed here.
In conclusion, we have designed an adequate and flexible toolbox for diagnosing and typing most medically relevant Leishmania species worldwide. Specificity and sensitivity were significantly increased in relation to previously described hsp70 assays. The proposed methods can therefore be applied in an endemic context, as well as in travel clinics dealing with import leishmaniasis. Analysis of hsp70 can be advocated as a standardized analysis tool for Leishmania typing, whereby RFLP could also be replaced by sequencing of the proposed amplicons wherever available. Currently, validation of the technology in endemic and travel clinic settings is ongoing, and we anticipate that our method can contribute significantly to case management, and epidemiological as well as clinical studies.
References
Yamey G, Torreele E (2002) The world’s most neglected diseases. British Med J 325:176–177, Erratum British Med J 325:352
Alvar J, Yactayo S, Bern C (2006) Leishmaniasis and poverty. Trends Parasitol 22:552–557
Herwaldt BL (1999) Leishmaniasis. Lancet 354:1191–1199
Arévalo J, Ramírez L, Adaui V, Zimic M, Tulliano G, Miranda-Verástegui C, Lazo M, Loayza-Muro R, De Doncker S, Maurer A, Chappuis F, Dujardin JC, Llanos-Cuentas A (2007) Influence of Leishmania (Viannia) species on the response to antimonial treatment in patients with American tegumentary leishmaniasis. J Inf Dis 195:1846–1851
Llanos-Cuentas A, Tulliano G, Araujo Castillo R, Miranda-Verástegui C, Santamaría-Castrellon G, Ramírez L, Lazo M, De Doncker S, Boelaert M, Robays J, Dujardin JC, Arévalo J, Chappuis F (2008) Clinical and parasite species risk factors for pentavalent antimonial treatment failure in cutaneous leishmaniasis in Peru. Clin Infect Dis 46:223–231
García AL, Parrado R, De Doncker S, Bermúdez H, Dujardin JC (2007) American tegumentary leishmaniasis: direct species identification of Leishmania in non-invasive clinical samples. Trans R Soc Trop Med Hyg 101:368–371
Pérez JE, Veland N, Espinosa D, Torres K, Ogusuku E, Llanos-Cuentas A, Gamboa D, Arévalo J (2007) Isolation and molecular identification of Leishmania (Viannia) peruviana from naturally infected Lutzomyia peruensis (Diptera: Psychodidae) in the Peruvian Andes. Mem Inst Oswaldo Cruz 102:655–658
Ampuero J, Pereira Rios A, Carranza-Tamayo CO, Romero GAS (2009) Genus-specific kinetoplast-DNA PCR and parasite culture for the diagnosis of localized cutaneous leishmaniasis: applications for clinical trials under field conditions in Brazil. Mem Inst Oswaldo Cruz 104:992–997
Deborggraeve S, Laurent T, Espinosa D, Van der Auwera G, Mbuchi M, Wasunna M, El-Safi S, Al-Basheer AA, Arévalo J, Miranda-Verástegui C, Leclipeteux T, Mertensa P, Dujardin JC, Herdewijn P, Büscher P (2008) A simplified and standardized polymerase chain reaction format for the diagnosis of leishmaniasis. J Infect Dis 198:1565–1572
Gadisa E, Kuru T, Genet A, Engers H, Aseffa A, Gedamu L (2010) Leishmania donovani complex (Kinetoplastida, Trypanosomatidae). Comparison of deoxyribonucleic acid based techniques for typing isolates from Ethiopia. Exp Parasitol 126:203–208
Montalvo AM, Fraga J, Montano I, Monzote L, Marín M, Van der Auwera G, Dujardin JC, Vélez ID, Muskus C (2010) Differentiation of Leishmania (Viannia) panamensis and Leishmania (V.) guyanensis using BccI for hsp70 PCR-RFLP. Trans R Soc Trop Med Hyg 104:364–367
Fraga J, Montalvo AM, De Doncker S, Dujardin JC, Van der Auwera G (2010) Phylogeny of Leishmania species based on the heat-shock protein 70 gene. Infect Genet Evol 10:238–245
Montalvo AM, Fraga J, Monzote I, Montano I, De Doncker S, Dujardin JC, Van der Auwera G (2010) Heat-shock protein PCR-RFLP: a universal simple tool for Leishmania species discrimination in the New and Old World. Parasitology 137:1159–1168
García AL, Kindt A, Bermúdez H, Llanos-Cuentas A, De Doncker S, Arévalo J (2004) Culture-independent species typing of neotropical Leishmania for clinical validation of a PCR-based assay targeting heat shock protein 70 genes. J Clin Microbiol 42:2294–2297
Tamura K, Dudley J, Nei M, Kumar S (2007) MEGA 4: Molecular Evolutionary Genetics Analysis (MEGA) software version 4.0. Mol Biol Evol 24:1596–1599
Rodríguez N, Guzman B, Rodas A, Takiff H, Bloom BR, Convit J (1994) Diagnosis of cutaneous leishmaniasis and species discrimination of parasites by PCR and hybridization. J Clin Microbiol 32:2246–2252
Ramírez JR, Agudelo S, Muskus C, Alzate JF, Berberich C, Barker D, Vélez ID (2000) Diagnosis of cutaneous leishmaniasis in Colombia: the sampling site within lesions influences the sensitivity of parasitological diagnosis. J Clin Microbiol 38:3768–3773
Bastrenta B, Mita N, Buitrago R, Vargas F, Flores M, Machane M, Yacsik N, Torrez N, Le Pont F, Brenière F (2003) Human mixed infections of Leishmania spp. and Leishmania-Trypanosoma cruzi in a sub Andean Bolivian area: identification by polymerase chain reaction/hybridization and isoenzyme. Mem Inst Oswaldo Cruz 98:255–264
Mendes DG, Lauria-Pires L, Nitz N, Lozzi SP, Nascimento RJ, Monteiro PS, Rebelo MM, Rosa Ade C, Santana JM, Teixeira AR (2007) Exposure to mixed infections with Trypanosoma cruzi, Leishmania braziliensis and Leishmania chagasi in the human population of the greater Amazon. Trop Med Int Health 12:629–636
Mugasa CM, Deborggraeve S, Schoone GJ, Laurent T, Leeflang MM, Ekangu RA, El-Safi S, Saad AA, Basiye FL, De Doncker S, Lubega GW, Kager PA, Büscher P, Schallig HDFH (2010) Accordance and concordance of PCR and NASBA followed by oligochromatography for the molecular diagnosis of Trypanosoma brucei and Leishmania. Trop Med Intern Health 15:800–805
Bensoussan E, Nasereddin A, Jonas F, Schnur LF, Jaffe CL (2006) Comparison of PCR assays for diagnosis of cutaneous leishmaniasis. J Clin Microbiol 44:1435–1439
Romero GAS, Ferreira-Noronha E, Pirmez C, Silva-Pires FES, Fernandes O, Saad-Nehmec N, Cupolillo E, Firoozmand L, Cardoso da Graca G, Volpini A, Lopes-Santos S, Romanha AJ (2009) Sensitivity and reproducibility of a PCR assay for Leishmania detection using skin biopsy imprints on filter paper. Acta Trop 109:74–77
Arévalo J, Ramírez L, Adaui V, Zimic M, Tulliano G, Miranda-Verástegui C, Lazo M, Loayza-Muro R, De Doncker S, Maurer A, Chappuis F, Dujardin JC, Llanos-Cuentas A (2007) Influence of Leishmania (Viannia) species on the response to antimonial treatment in patients with American tegumentary leishmaniasis. J Inf Dis 195:1846–1851
da Silva LA, de Sousa CdS, da Graça GC, Porrozzi R, Cupolillo E (2010) Sequence analysis and PCR-RFLP profiling of the hsp70 gene as a valuable tool for identifying Leishmania species associated with human leishmaniasis in Brazil. Infect Genet Evol 10:77–83
Dujardin JC, Bañuls AL, Llanos-Cuentas A, Alvarez E, De Doncker S, Jacquet D, Le Ray D, Arévalo J, Tibayrenc M (1995) Putative Leishmania hybrids in the Eastern Andean valley of Huanuco, Peru. Acta Trop 59:293–307
Nolder D, Roncal N, Davies CR, Llanos-Cuentas A, Miles MA (2007) Multiple hybrid genotypes of Leishmania (Viannia) in a focus of mucocutaneous leishmaniasis. Am J Trop Med Hyg 76:573–578
Chappuis F, Sundar S, Hailu A, Ghalib H, Rijal S, Peeling RW, Alvar J, Boelaert M (2007) Visceral leishmaniasis: what are the needs for diagnosis, treatment and control? Nat Rev Microbiol 5:873–882
Cupolillo E, Grimaldi G, Momen H, Beverley SM (1995) Intergenic Region Typing (IRT) A rapid molecular approach to the characterization and evolution of Leishmania. Mol Biochem Parasitol 73:145–155
Marfurt J, Nasereddin A, Niederwieser I, Jaffe CL, Beck HP, Felger I (2003) Identification and differentiation of Leishmania species in clinical samples by PCR amplification of the miniexon sequence and subsequent restriction fragment length polymorphism analysis. J Clinic Microbiol 41:3147–3153
Marfurt J, Niederwiese I, Divine MN, Beck HP, Felger I (2003) Diagnostic genotyping of Old and New World Leishmania species by PCR-RFLP. Diag Microbiol Infect Dis 46:115–124
Rotureau B, Ravel C, Couppie P, Pratlong F, Nacher M, Dedet JP, Carme B (2006) Use of PCR-restriction fragment length polymorphism analysis to identify the main new world Leishmania species and analyze their taxonomic properties and polymorphism by application of the assay to clinical samples. J Clin Microbiol 44:459–467
Oshaghi MA, Ravasan NM, Hide M, Javadian EA, Rassi Y, Sedaghat MM, Mohebali M, Hajjaran H (2009) Development of species-specific PCR and PCR-restriction fragment length polymorphism assays for L. infantum / L. donovani discrimination. Exp Parasitol 122:61–65
Simon S, Veron V, Carme B (2010) Leishmania spp. identification by polymerase chain reaction-restriction fragment length polymorphism analysis and its applications in French Guiana. Diagn Microbiol Infect Dis 66:175–180
Acknowledgements
The authors would like to thank all colleagues and institutes who kindly donated the Leishmania reference strains or DNA: J. Arévalo (Instituto de Medicina Tropical Alexander von Humboldt, Lima, Peru); L. García (Centro Universitario de Medicina Tropical, Cochabamba, Bolivia); E. Cupolillo (Instituto Oswaldo Cruz, Rio de Janeiro, Brazil); G. Schönian (Institut für Mikrobiologie und Hygiene, Berlin, Germany); I. Mauricio and D. Evans (London School of Hygiene and Tropical Medicine, London, UK); P. Desjeux (Instituto Boliviano de Biología de Altura, La Paz, Bolivia); J.-P. Dedet and J.A. Rioux (Centre National de Référence des Leishmania, Montpellier, France); J.J. Shaw (University of São Paulo, São Paulo, Brazil); G. Schoone and A. El Harith (Royal Tropical Institute, Amsterdam, The Netherlands); Laboratorio de Biología Molecular (Departamento de Parasitología, Bacteriología y Virología, IPK, Havana, Cuba); and the LeishEpinetSA consortium (EU contract INCO-CT2005-015407). Clinical samples were provided by M. Gramiccia (Istituto Superiore di Sanità, Rome, Italy); A. Llanos (Instituto de Medicina Tropical Alexander von Humboldt, Lima, Peru); L. Campino (Instituto de Higiene e Medicina Tropical, Lisbon, Portugal); S. El Safi (University of Khartoum, Khartoum, Sudan); and A. Ben Salah (Institut Pasteur de Tunis, Tunis, Tunisia). We acknowledge Simonne De Doncker (ITM) for technical assistance. This work was funded by the third framework program of the Belgian Development Cooperation between ITM and IPK, which also provided salary support for GVDA.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Table ESM-1
Lists all reference strains and isolates used for the study, with WHO codes. Strains used for the wet and in silico analyses are indicated, as well as accession numbers of the hsp70 sequences (PDF 498 kb)
Table ESM-2
Gives a schematic overview of the recommended RFLP scheme for all identified groups (PDF 152 kb)
Rights and permissions
About this article
Cite this article
Montalvo, A.M., Fraga, J., Maes, I. et al. Three new sensitive and specific heat-shock protein 70 PCRs for global Leishmania species identification. Eur J Clin Microbiol Infect Dis 31, 1453–1461 (2012). https://doi.org/10.1007/s10096-011-1463-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-011-1463-z