Abstract
The prompt diagnosis of influenza enables the institution of antiviral therapy and adequate cohorting of patients, but scarce data are available to help clinicians correctly suspect influenza in children at the time of admission. This 16-year retrospective study assessed the main admission diagnoses of 401 children aged ≤16 years hospitalized with virologically confirmed influenza. The clinical data were derived from a systematic review of the medical records of the children. Sepsis-like illness was the main reason for admission in 52% of infants aged <6 months and in 7–16% of the older children. Respiratory symptoms accounted for 38% of admissions, and 15% of children were hospitalized due to acute neurologic conditions, primarily febrile convulsions. Wheezing or exacerbation of asthma was the primary reason for admission in 14% of children aged <3 years. No differences were observed in the admission diagnoses between children with influenza A and B infections. The main admission diagnoses vary widely in different age groups of children with influenza, and only a minority of children are hospitalized for respiratory symptoms. The leading role of sepsis-like illness in infants aged <6 months calls for increased efforts to find protective measures against influenza in this age group.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Annual influenza epidemics bring about a substantial disease burden on children, and influenza-related complications are frequent especially among the youngest patients [1–8]. Although the vast majority of children with influenza are treated as outpatients, the rates of influenza-associated hospitalizations are high in children, particularly among those younger than 2 years of age [1, 2, 7–10].
The clinical spectrum of influenza ranges widely from an asymptomatic infection to a life-threatening illness. Although the hallmark symptoms of influenza are high fever and cough, influenza may also manifest itself, e.g., as a severe form of croup, and, occasionally, febrile convulsion may be the first sign of influenza in young children [11–13]. Furthermore, the clinical features of influenza in children vary with age [14].
Few previous studies have assessed the clinical presentation of seasonal pediatric influenza at the time of hospital admission [15, 16]. Such information would be important for the clinician because the prompt identification of influenza-infected children enables the institution of early antiviral treatment and proper cohorting of patients on wards [17, 18]. We sought to determine the main admission diagnoses of children in different age groups who were hospitalized with laboratory-confirmed influenza during a 16-year study period.
Patients and methods
Study design and subjects
We conducted this retrospective study at the Department of Pediatrics, Turku University Hospital, Turku, Finland, during a period of 16 consecutive years from July 1, 1988, through June 30, 2004. Turku University Hospital is the only tertiary-care hospital in Southwestern Finland and the sole provider of acute pediatric hospital care for approximately 69,000 children ≤16 years of age. The study population consisted of all children aged ≤16 years who were hospitalized with virologically confirmed influenza during the study period.
Data collection and viral diagnosis
To identify all children who were hospitalized with influenza, we searched for data from three different sources: (1) the Department of Virology, University of Turku, which was the only laboratory that provided routine viral diagnostic services for our hospital; (2) the central database of Turku University Hospital; and (3) the files of the pediatric infectious diseases ward at our hospital. The medical records of all children with an International Classification of Diseases (ICD) code related to influenza (ICD-9: 4870A, 4871A, and 4878X; ICD-10: J10–J11) who were not found from the database of the Department of Virology were carefully examined to confirm or rule out the viral diagnosis of influenza. The files of the pediatric infectious diseases ward were examined to identify children who had tested positive for influenza by a rapid influenza test and from whom no additional viral specimens had, therefore, been obtained. Overall, we found 407 children who were hospitalized with virologically confirmed influenza. Six children were excluded from this analysis because the viral specimens had been obtained >2 days after admission, and, hence, nosocomial influenza infection could not be ruled out. The final analyses consisted of 401 influenza virus-infected children. The viral diagnosis was based on antigen detection [19] or viral culture in 372 (93%) cases and on rapid influenza testing (Directigen FluA+B, Becton Dickinson Diagnostic Systems, Sparks, MD, USA) in 29 (7%) cases. Seven children each were admitted twice due to influenza during the study period.
Classification of admission diagnoses and definitions
We categorized the primary reasons for admission into nine groups based on the presenting signs and symptoms and any additional information found in the medical records: (1) sepsis-like illness; (2) respiratory infection; (3) acute neurologic condition; (4) muscular symptoms; (5) abdominal symptoms; (6) general condition; (7) severe underlying condition; (8) social indication; and (9) other concomitant illness. The clinical data were collected by a systematic chart review, and, for consistency, the main reason for admission was determined by one investigator (H.S.) according to all of the available data. The primary admission diagnosis of a child could be different from the official discharge diagnosis recorded in the hospital central database. A few children had two or more apparent reasons for hospitalization; in these cases, the children’s medical charts were re-reviewed (by H.S. and T.H.) for consensus.
The diagnosis of pneumonia was based on radiological confirmation of the condition at admission. The admission diagnosis was recorded as upper respiratory tract infection if the child was hospitalized with a respiratory illness other than pneumonia, asthma/wheezing, laryngitis, tracheitis, or epiglottitis. Prolonged fever was defined as fever that had lasted ≥5 days. Vomiting was recorded as the main reason in case of repeated vomiting without signs of dehydration. Neurologic defects included severe, mainly congenital neurologic diseases, for example, cerebral palsy and tuberous sclerosis. The category “social indication” was used for children who were admitted mainly because of social problems and not because of the severity of the illness. Most children in the category “other concomitant illness” had a febrile respiratory illness, but the respiratory symptoms were not considered as the main reason for hospitalization.
Statistics
The Chi-square test and the Mann–Whitney U-test were used for comparisons between different groups of children. Two-sided p-values <0.05 were considered to be statistically significant. All statistical analyses were performed with StatsDirect (version 2.7.7) software.
Results
Study population
The median age of the 401 children in the study was 1.6 years (mean, 3.5 years; range, 1 week to 16 years). Eighty-eight (21.9%) children were <6 months of age; 169 (42.1%) were 0.5–2.9 years of age; 71 (17.7%) were 3.0–6.9 years of age; and 73 (18.2%) were 7.0–16.9 years of age. A total of 222 (55.4%) children were boys. One-hundred and five (26.2%) children had an underlying chronic illness, with asthma being the most common condition (7.2% of all children), followed by neurologic defects (6.7%) and malignancy or immunosuppression (4.2%). Influenza A virus was detected in 330 (82.3%) children and influenza B virus in 70 (17.5%) children; one child was infected with influenza A and B viruses simultaneously.
Primary admission diagnoses in different age groups
The primary admission diagnoses of children in different age groups are presented in Table 1.
In the entire child population, the most frequent reason for admission was respiratory illness, which accounted for 38% of all influenza-related admissions; approximately one-third of these children had pneumonia. Sepsis-like illness was the main reason for hospitalization in 52% of infants <6 months of age, but also in 7–16% of children in the older age groups. Wheezing or exacerbation of asthma was the primary reason for admission in 14% of infants and children <3 years of age. Twelve percent of all children were hospitalized due to febrile convulsion. Overall, 15% of the children were admitted because of acute neurologic symptoms and 10% because of dehydration.
Admission diagnoses in children with influenza A and B infections
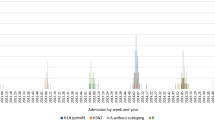
The rates of different admission diagnoses were further analyzed according to the type of influenza virus; one child with simultaneous infection with influenza A and B viruses was excluded from this analysis. Because the median ages of children with influenza A and B infections were significantly different (influenza A, 1.5 years; influenza B, 5.5 years; p < 0.001), the relative proportions of various admission categories were compared within each of the four different age groups (Fig. 1). No significant differences were observed in any categories between children with influenza A and B infections in any of the age groups.
Discussion
Our study demonstrates the wide spectrum of clinical conditions seen in influenza virus-infected children at the time of hospitalization. Furthermore, our results show that the main admission diagnoses vary substantially between different age groups of children. Although some previous studies have described the clinical features and outcomes in children hospitalized with seasonal influenza [15, 16], to our knowledge, this is the first study to assess and compare the admission diagnoses between different age groups of children who are being hospitalized with virologically confirmed influenza.
Perhaps the most striking finding in our study was that more than half of all infants under 6 months of age were admitted due to sepsis-like illness. In this age group, full-blown respiratory symptoms are often absent during the early phase of the illness, and the first manifestation of influenza may be an abrupt onset of high fever that imitates bacterial sepsis [7, 20–22]. Although the true incidence of serious bacterial co-infections in influenza virus-infected infants is low [22, 23], the presence of high fever in young infants usually leads to invasive examinations, hospitalization, and empirical antibiotic treatment [15]. Altogether, these procedures generate a notable burden on infants and their families, as well as substantial costs on society [24, 25]. In a recent US study of children <5 years of age with virologically confirmed influenza, hospitalized infants <6 months of age accounted for 45% of the total costs of influenza [25].
Although influenza is principally a respiratory infection, it was surprising that only 38% of the children were admitted mainly for respiratory symptoms. This finding is important, as it could be assumed that children with primarily non-respiratory clinical manifestations may easily remain undiagnosed and, subsequently, not receive adequate treatment for their influenza. The clinical importance of the early identification of influenza was underscored by our recent trial that demonstrated that oseltamivir treatment started within 24 h of the onset of influenza symptoms shortened the duration of illness by 3.5–4 days in young children with influenza A infection [18].
Compatible with earlier reports [26–30], pneumonia was the most frequent respiratory diagnosis leading to the hospitalization of children older than 6 months of age; one-sixth of all children in this age group were admitted due to suspected bacterial pneumonia. Although rhinoviruses and respiratory syncytial virus have been shown to be the most frequent etiologic agents in acute wheezing and exacerbation of asthma in young children [31], it is worth noting that acute expiratory wheezing was the primary reason for admission in approximately 14% of children <3 years of age, which suggests that the role of influenza viruses in triggering acute wheezing attacks in children is far from negligible. Furthermore, 5% of all influenza admissions were due to laryngitis, which is in agreement with a previous report indicating that laryngitis caused by influenza viruses is more severe than that caused by parainfluenza viruses [12].
Acute neurologic symptoms accounted for 15% of all influenza-related hospitalizations, which is a remarkably high percentage for a respiratory infection. This finding is, however, in good accordance with previous studies that have demonstrated an increased risk for influenza-related neurologic complications, mainly seizures, in young children [15, 32, 33]. Chiu et al. reported that influenza infections were associated with a higher incidence of febrile seizures than adenovirus or parainfluenza virus infections [13]. In our study, the rate of febrile convulsions was especially high among children aged 6 months to <3 years. Combined with other data evidencing that the total disease burden of influenza is greatest in children younger than 3 years of age, our findings corroborate the view that young children would substantially benefit from influenza vaccination [4, 34, 35].
It is generally thought that the clinical features of influenza A and B infections are different, with influenza A viruses causing more severe illnesses than influenza B viruses. While there are undoubtedly substantial differences in the overall virulence between different strains of influenza circulating in different years, it is possible that the conventional concept of an overall difference between A and B viruses is seriously confounded by age. In several studies, including the present one, children hospitalized with influenza B infections have been significantly older than those with influenza A infections [10, 16], and few studies have attempted to adjust the clinical features for the age of the children. In this study, in which we analyzed the admission diagnoses separately in different age groups, we could not demonstrate any significant differences between influenza A and B infections. This finding tends to agree with our earlier prospective study among outpatients, in which no differences were observed in any signs or symptoms between children with influenza A or B virus infections when analyzed within different age groups [14].
The main strengths of our study include the careful structured analysis of the medical records of all children and the 16-year observation period that balances any potential year-to-year variation in the results. There are also some limitations. Although obtaining viral specimens from hospitalized children was a routine procedure at our department during the period of this study, it is possible that some children with influenza had not been subjected to viral sampling. It is also possible that, especially with rapid diagnostic tests, some of the tests have remained false-negative. However, because of the generally high specificity of influenza rapid tests, we believe that, regardless of the viral diagnostic method used, all of the children in our analysis had true influenza, which is the most important issue for this study. In a few cases, the allocation of children into the different admission diagnosis categories was challenging due to the retrospective nature of the study. This was particularly true for children with underlying conditions, some of whom had two or more potential admission diagnoses available. Overall, however, we consider it very unlikely that any of these shortcomings could have introduced a significant bias to the results.
Infants younger than 6 months of age are an extremely vulnerable group in regard to seasonal influenza because neither vaccines nor antiviral treatments are currently available for them. Some recent studies have provided encouraging initial evidence for the safety and immunogenicity of a trivalent inactivated influenza vaccine in infants as young as 2 months of age [36, 37], but further studies in this area are clearly needed. In the meantime, readily available options to diminish the burden of influenza in the youngest infants include the immunization of mothers during pregnancy and the vaccination of all family members and close contacts of the infants [38–40].
In conclusion, we found that the clinical presentation of influenza varied widely in different age groups of children at the time of hospital admission. Our findings provide a challenge to clinicians who are responsible for the optimal treatment of these patients, and the results underscore the importance of clinicians’ awareness of the full spectrum of clinical manifestations of influenza in children. The leading role of sepsis-like illness in infants younger than 6 months of age is important, and further research into effective protective measures against influenza in this age group is clearly warranted.
References
Neuzil KM, Mellen BG, Wright PF, Mitchel EF Jr, Griffin MR (2000) The effect of influenza on hospitalizations, outpatient visits, and courses of antibiotics in children. N Engl J Med 342(4):225–231
Izurieta HS, Thompson WW, Kramarz P, Shay DK, Davis RL, DeStefano F, Black S, Shinefield H, Fukuda K (2000) Influenza and the rates of hospitalization for respiratory disease among infants and young children. N Engl J Med 342(4):232–239
Neuzil KM, Zhu Y, Griffin MR, Edwards KM, Thompson JM, Tollefson SJ, Wright PF (2002) Burden of interpandemic influenza in children younger than 5 years: a 25-year prospective study. J Infect Dis 185(2):147–152
Heikkinen T, Silvennoinen H, Peltola V, Ziegler T, Vainionpää R, Vuorinen T, Kainulainen L, Puhakka T, Jartti T, Toikka P, Lehtinen P, Routi T, Juven T (2004) Burden of influenza in children in the community. J Infect Dis 190(8):1369–1373
Poehling KA, Edwards KM, Weinberg GA, Szilagyi P, Staat MA, Iwane MK, Bridges CB, Grijalva CG, Zhu Y, Bernstein DI, Herrera G, Erdman D, Hall CB, Seither R, Griffin MR; New Vaccine Surveillance Network (2006) The underrecognized burden of influenza in young children. N Engl J Med 355(1):31–40
Tsolia MN, Logotheti I, Papadopoulos NG, Mavrikou M, Spyridis NP, Drossatou P, Kafetzis D, Konstantopoulos A; Outpatient Flu Study Group (2006) Impact of influenza infection in healthy children examined as outpatients and their families. Vaccine 24(33–34):5970–5976
Ploin D, Liberas S, Thouvenot D, Fouilhoux A, Gillet Y, Denis A, Chapuis F, Lina B, Floret D (2003) Influenza burden in children newborn to eleven months of age in a pediatric emergency department during the peak of an influenza epidemic. Pediatr Infect Dis J 22(10 Suppl):S218–S222
O’Brien MA, Uyeki TM, Shay DK, Thompson WW, Kleinman K, McAdam A, Yu XJ, Platt R, Lieu TA (2004) Incidence of outpatient visits and hospitalizations related to influenza in infants and young children. Pediatrics 113(3 Pt 1):585–593
Thompson WW, Shay DK, Weintraub E, Brammer L, Bridges CB, Cox NJ, Fukuda K (2004) Influenza-associated hospitalizations in the United States. JAMA 292(11):1333–1340
Silvennoinen H, Peltola V, Vainionpää R, Ruuskanen O, Heikkinen T (2011) Incidence of influenza-related hospitalizations in different age groups of children in Finland: a 16-year study. Pediatr Infect Dis J 30(2):e24–e28
Monto AS, Gravenstein S, Elliott M, Colopy M, Schweinle J (2000) Clinical signs and symptoms predicting influenza infection. Arch Intern Med 160(21):3243–3247
Peltola V, Heikkinen T, Ruuskanen O (2002) Clinical courses of croup caused by influenza and parainfluenza viruses. Pediatr Infect Dis J 21(1):76–78
Chiu SS, Tse CY, Lau YL, Peiris M (2001) Influenza A infection is an important cause of febrile seizures. Pediatrics 108(4):E63
Silvennoinen H, Peltola V, Lehtinen P, Vainionpää R, Heikkinen T (2009) Clinical presentation of influenza in unselected children treated as outpatients. Pediatr Infect Dis J 28(5):372–375
Quach C, Piché-Walker L, Platt R, Moore D (2003) Risk factors associated with severe influenza infections in childhood: implication for vaccine strategy. Pediatrics 112(3 Pt 1):e197–e201
Peltola V, Ziegler T, Ruuskanen O (2003) Influenza A and B virus infections in children. Clin Infect Dis 36(3):299–305
Whitley RJ, Hayden FG, Reisinger KS, Young N, Dutkowski R, Ipe D, Mills RG, Ward P (2001) Oral oseltamivir treatment of influenza in children. Pediatr Infect Dis J 20(2):127–133
Heinonen S, Silvennoinen H, Lehtinen P, Vainionpää R, Vahlberg T, Ziegler T, Ikonen N, Puhakka T, Heikkinen T (2010) Early oseltamivir treatment of influenza in children 1–3 years of age: a randomized controlled trial. Clin Infect Dis 51(8):887–894
Nikkari S, Halonen P, Kharitonenkov I, Kivivirta M, Khristova M, Waris M, Kendal A (1989) One-incubation time-resolved fluoroimmunoassay based on monoclonal antibodies in detection of influenza A and B viruses directly in clinical specimens. J Virol Methods 23(1):29–40
Dagan R, Hall CB (1984) Influenza A virus infection imitating bacterial sepsis in early infancy. Pediatr Infect Dis 3(3):218–221
Rojo JC, Ruiz-Contreras J, Fernández MB, Marín MA, Folgueira L (2006) Influenza-related hospitalizations in children younger than three years of age. Pediatr Infect Dis J 25(7):596–601
Bender JM, Ampofo K, Gesteland P, Sheng X, Korgenski K, Raines B, Daly JA, Valentine K, Srivastava R, Pavia AT, Byington CL (2010) Influenza virus infection in infants less than three months of age. Pediatr Infect Dis J 29(1):6–9
Byington CL, Enriquez FR, Hoff C, Tuohy R, Taggart EW, Hillyard DR, Carroll KC, Christenson JC (2004) Serious bacterial infections in febrile infants 1 to 90 days old with and without viral infections. Pediatrics 113(6):1662–1666
Ampofo K, Gesteland PH, Bender J, Mills M, Daly J, Samore M, Byington C, Pavia AT, Srivastava R (2006) Epidemiology, complications, and cost of hospitalization in children with laboratory-confirmed influenza infection. Pediatrics 118(6):2409–2417
Fairbrother G, Cassedy A, Ortega-Sanchez IR, Szilagyi PG, Edwards KM, Molinari NA, Donauer S, Henderson D, Ambrose S, Kent D, Poehling K, Weinberg GA, Griffin MR, Hall CB, Finelli L, Bridges C, Staat MA; New Vaccine Surveillance Network (NVSN) (2010) High costs of influenza: direct medical costs of influenza disease in young children. Vaccine 28(31):4913–4919
Wang YH, Huang YC, Chang LY, Kao HT, Lin PY, Huang CG, Lin TY (2003) Clinical characteristics of children with influenza A virus infection requiring hospitalization. J Microbiol Immunol Infect 36(2):111–116
Moore DL, Vaudry W, Scheifele DW, Halperin SA, Déry P, Ford-Jones E, Arishi HM, Law BJ, Lebel M, Le Saux N, Grimsrud K, Tam T (2006) Surveillance for influenza admissions among children hospitalized in Canadian immunization monitoring program active centers, 2003–2004. Pediatrics 118(3):e610–e619
Lahti E, Peltola V, Virkki R, Ruuskanen O (2006) Influenza pneumonia. Pediatr Infect Dis J 25(2):160–164
Coffin SE, Zaoutis TE, Rosenquist AB, Heydon K, Herrera G, Bridges CB, Watson B, Localio R, Hodinka RL, Keren R (2007) Incidence, complications, and risk factors for prolonged stay in children hospitalized with community-acquired influenza. Pediatrics 119(4):740–748
Dawood FS, Fiore A, Kamimoto L, Nowell M, Reingold A, Gershman K, Meek J, Hadler J, Arnold KE, Ryan P, Lynfield R, Morin C, Baumbach J, Zansky S, Bennett NM, Thomas A, Schaffner W, Kirschke D, Finelli L; Emerging Infections Program (EIP) Network (2010) Influenza-associated pneumonia in children hospitalized with laboratory-confirmed influenza, 2003–2008. Pediatr Infect Dis J 29(7):585–590
Jartti T, Lehtinen P, Vuorinen T, Österback R, van den Hoogen B, Osterhaus AD, Ruuskanen O (2004) Respiratory picornaviruses and respiratory syncytial virus as causative agents of acute expiratory wheezing in children. Emerg Infect Dis 10(6):1095–1101
Maricich SM, Neul JL, Lotze TE, Cazacu AC, Uyeki TM, Demmler GJ, Clark GD (2004) Neurologic complications associated with influenza A in children during the 2003–2004 influenza season in Houston, Texas. Pediatrics 114(5):e626–e633
Newland JG, Laurich VM, Rosenquist AW, Heydon K, Licht DJ, Keren R, Zaoutis TE, Watson B, Hodinka RL, Coffin SE (2007) Neurologic complications in children hospitalized with influenza: characteristics, incidence, and risk factors. J Pediatr 150(3):306–310
Heikkinen T, Booy R, Campins M, Finn A, Olcén P, Peltola H, Rodrigo C, Schmitt HJ, Schumacher F, Teo S, Weil-Olivier C (2006) Should healthy children be vaccinated against influenza? A consensus report of the Summits of Independent European Vaccination Experts. Eur J Pediatr 165(4):223–228
Heinonen S, Silvennoinen H, Lehtinen P, Vainionpää R, Ziegler T, Heikkinen T (2011) Effectiveness of inactivated influenza vaccine in children aged 9 months to 3 years: an observational cohort study. Lancet Infect Dis 11(1):23–29
Walter EB, Englund JA, Blatter M, Nyberg J, Ruben FL, Decker MD; GRC27 Study Team (2009) Trivalent inactivated influenza virus vaccine given to two-month-old children: an off-season pilot study. Pediatr Infect Dis J 28(12):1099–1104
Englund JA, Walter E, Black S, Blatter M, Nyberg J, Ruben FL, Decker MD; GRC28 Study Team (2010) Safety and immunogenicity of trivalent inactivated influenza vaccine in infants: a randomized double-blind placebo-controlled study. Pediatr Infect Dis J 29(2):105–110
Englund JA, Mbawuike IN, Hammill H, Holleman MC, Baxter BD, Glezen WP (1993) Maternal immunization with influenza or tetanus toxoid vaccine for passive antibody protection in young infants. J Infect Dis 168(3):647–656
Zaman K, Roy E, Arifeen SE, Rahman M, Raqib R, Wilson E, Omer SB, Shahid NS, Breiman RF, Steinhoff MC (2008) Effectiveness of maternal influenza immunization in mothers and infants. N Engl J Med 359(15):1555–1564
Benowitz I, Esposito DB, Gracey KD, Shapiro ED, Vázquez M (2010) Influenza vaccine given to pregnant women reduces hospitalization due to influenza in their infants. Clin Infect Dis 51(12):1355–1361
Acknowledgments
This study was supported by grants from the Turku University Hospital Foundation and the Finnish Medical Foundation (to Dr. Silvennoinen).
Conflict of interest statement
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Silvennoinen, H., Peltola, V., Vainionpää, R. et al. Admission diagnoses of children 0–16 years of age hospitalized with influenza. Eur J Clin Microbiol Infect Dis 31, 225–231 (2012). https://doi.org/10.1007/s10096-011-1297-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-011-1297-8