Abstract
Epidemiological studies on multiple sclerosis (MS) carried out in Southern Europe in the last years have shown a significant increase in the disease frequency. Previous surveys conducted in the Republic of San Marino, Northern Italian peninsula, identified that the population is at high risk for MS, with a prevalence of 51.6 per 100,000 population in 1982 and of 166.7 in 2005 and with a mean annual incidence of 7.9 per 100,000 for the period 1990–2005. The present work is a community-based intensive prevalence and incidence survey, by a complete enumeration approach, to update the prevalence and incidence of MS in the Republic of San Marino. The mean annual incidence for the period 2005–14 was 7.7 (95% CI 4.9–11.4) per 100,000, 3.3 (95% CI 1.1–7.6) for men and 11.9 (95% CI 7.2–18.6) for women. On 31 December 2014, 67 patients (19 men and 48 women), suffering from definite or probable MS and living in the Republic of San Marino, yielded a crude prevalence of 204.3 (95% CI 158.4–259.5) per 100,000, 117.8 (95% CI 70.9–183.7) for men and 288.2 (95% CI 212.4–383.3) for women. Our study has confirmed San Marino is an area at high risk for MS, in line with epidemiological data from continental Italy. The marked increase in MS prevalence over time in this population can be ascribable to increased survival and improved ascertainment, in the presence of a substantially stable, yet high, incidence rate.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Epidemiological studies of multiple sclerosis (MS) carried out in Europe over the last few decades, including those conducted in Italy, have shown significant increase of the disease prevalence and incidence [1,2,3,4,5,6,7]. The rather heterogeneous distribution of MS, especially in Southern Europe, has led to surmount the gradient-by-latitude theory of MS geographic distribution proposed by Kurtzke [8].
In the most recent studies, the estimated incidence rate of MS in Italy varied from 4 to 6 per 100,000/year, with an incremental trend in several geographical areas [9, 10], while the disease prevalence is on average higher than 100 per 100,000 population, with high prevalence outbreaks in Sardinia and Sicily [6, 11,12,13,14]. Previous epidemiological studies carried out in the Republic of San Marino between 1982 and 2007 [15, 16] showed that this is a high prevalence area for MS. In particular, Granieri et al. reported a prevalence rate of 166.7 per 100,000 (95% CI 123.7–220.0) and an incidence rate of 7.9 per 100,000/year (95% CI 5.3–11.1) in the period 1990 to 2005 [16]. This study aimed to update incidence and prevalence of MS in the Republic of San Marino.
Methods
Area of investigation
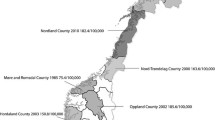
The Republic of San Marino is a little state in Southern Europe located within the northern Italian peninsula, lying near the Adriatic coast and completely surrounded by the Italian territory, i.e., Emilia-Romagna and Marche regions. San Marino is one of the smallest nations in the world, with a territorial extension of 61.2 km2, a population of 32,876 inhabitants, 16,176 men and 16,700 women as of 31 August 2015 [17], and a population density of 537.3 inhabitants/km2. During the study period, the population increased from 29,999 inhabitants in 2005 to 32,789 in 2014. The population is predominantly Caucasian, almost exclusively composed by natives in San Marino (85%) and Italians (10%) (Fig. 1).
The geographical, political, and socio-economical characteristics of the Republic of San Marino have been described in detail in previous epidemiological studies [15, 16]. Health care is free for all residents, whether citizens or not. San Marino has agreements with foreign hospitals and health care structures for the public health services which cannot be delivered within the territory. The public health system allows a wide availability of data, from both paper and computerized administrative records. San Marino State Hospital provides first- and second-level medical and surgical care, comprises a neurological unit with day-hospital, outpatient services, and relies on neuroimaging (MRI) and laboratory facilities for cerebrospinal fluid (CSF) analyses, in collaboration with the neurological units of nearby cities such as Rimini, Bologna, and Ferrara.
Case ascertainment and diagnostic criteria
The present study builds on 43 cases of definite or probable MS identified in previous studies carried out in the same area in 1984 [15] and in 2007 [16]. The main sources for case ascertainment were represented by medical records of the State Hospital Neurological Unit and administrative data based on hospitalization discharge codes (ICD9-CM 340), and files at the units of neuroradiology and neuropsychology and of laboratory tests. Data from public or private hospitals in neighboring areas were also scrutinized as well as death certificates. All diagnoses were validated by a team of neurologists at the State Hospital Neurological Unit. Demographic information was obtained by consulting the Civil Status appropriate registers.
All paper records of patients diagnosed with MS, demyelinating disease, optic neuritis, neuraxitis, encephalomyelitis, myelitis, myelopathy, paraparesis, and ataxia were scrutinized, and other clinical conditions ruled out. Only subjects with a definition of definite or probable MS according to Poser et al. criteria [18] were included in the study. Patients’ disability was assessed by using the Expanded Disability Status Scale (EDSS) [19].
Statistical analysis
An incidence case was defined as any individual with clinical presentation and diagnosis of clinically definite or probable MS [18] in the period 2005–14. Sex- and age-specific incidence rate was calculated based on the number of new cases for the incidence period (numerator) over the general population for the period (denominator) according to latest census (November 2010).
A prevalence case was defined as any individual residing in the study area who, on prevalence day 31 December 2014, showed signs or symptoms later classified as MS (onset-adjusted prevalence) or as any individual with a diagnosis of MS [18]. Sex- and age-specific crude prevalence was computed as the ratio between MS cases (numerator) and the general population in San Marino on 31 December 2014 (denominator) obtained from country official statistics. Prevalence was standardized to the 2011 Italian population [20] and to the standard European population [21] by the direct method.
95% confidence intervals (95% CI) were calculated around prevalence and incidence estimates using the Poisson distribution [22]. Students’ t test was used to compare means. Probability was calculated on two tails and the established significance was p < 0.05. The statistic significance of temporal incidence trends was estimated with the Armitage test for linear trends [23].
Results
Incidence
In the period 1 January 2005 to 31 December 2014, 24 patients were identified (5 men and 19 women) living in the Republic of San Marino, who had showed the first symptoms of MS, later diagnosed as definite or probable. In the same period, the general population increased from 29,999 to 32,789 inhabitants, with a mean of 31,269 (15,343 men and 15,926 women). The annual crude incidence rate was therefore 7.7 per 100,000 (95% CI 4.9–11.4), 3.3 (95% CI 1.1–7.6) for men and 11.9 (95% CI 7.2–18.6) for women, with a statistically significant difference between genders (p < 0.01). The female/male ratio was 3.8.
Sex- and age-specific crude mean annual incidence rates are reported in Table 1. The highest rates were observed for the age groups 20–29 years (19.8/100,000/year) and 40–49 years (12.6). Among men and among women, the highest rates were for the age groups 40–49 years (15.0) and 20–29 years (32.7), respectively.
The incidence rates adjusted to the Italian population were 7.5 per 100,000 (95% CI 4.8–11.2), 3.2 (95% CI 1.0–7.5) for men and 11.4 (95% CI 6.9–17.8) for women, respectively.
The incidence rates adjusted to the European population were 8.2 per 100,000 (95% CI 5.3–12.2), 3.0 (95% CI 1.0–7.1) for men and 13.2 (95% CI 8.0–20.6) for women, respectively.
The mean annual incidence during the period 2005 to 2009 was 9.2 per 100,000 (95% CI 5.0–15.5), 2.7 (95% CI 0.3–9.6) for men and 15.3 (95% CI 7.9–26.8) for women; it was 6.2 (95% CI 2.3–11.4), 3.8 (95% CI 0.8–11.1) for men and 8.5 (95% CI 3.4–17.6) for women, respectively, in the period from 2010 to 2014.
The mean age (SD) of onset was 33.2 (10.8) years for the total population, 30.8 (11.0) years for men and 34.0 (10.7) for women, respectively, with no statistically significant difference between the two genders. The mean (SD) age at onset was 30.5 (9.0) years in the relapsing-remitting form and 41.6 (12.0) years in the primary-progressive form (p < 0.05).
The clinical onset was a monosymptomatic way in 79.2% and a plurisymptomatic way in 20.8% patients. The most frequent symptom at onset was retrobulbar optic neuritis representing 29.2% of the monosymptomatic onsets.
The mean (SD) time period between the clinical onset and diagnosis for the patients with onset between 2005 and 2014 was 14.3 (23) months (range 4.2–39.3 months). The mean (SD) lag time between clinical onset and diagnosis was 8.7 (15.7) months for the relapsing-remitting form and 31.3 (33.5) months in the progressive forms.
Prevalence
On prevalence day 31 December 2014, 67 patients (19 men and 48 women) with definite or probable MS resided in San Marino, with a total population of 32,789 inhabitants (16,133 men and 16,656 women). The estimated total crude prevalence was 204.3 per 100,000 (95% CI 158.4–259.5), 117.8 (95% CI 70.9–183.7) for men and 288.2 (95% CI 212.4–383.3) for women, (p = 0.02). The female/male ratio was 2.5. The adjusted estimates for the Italian population were 203.0 per 100,000 (95% CI 157.3–257.8), 112.1 (95% CI 67.5–174.8) for men and 281.4 (95% CI 207.4–377.3) for women. The standardized estimates for the European population were 181.6 (95% CI 140.8–230.7), 101.5 (95% CI 61.1–158.3) for men and 259.5 (95% CI 191.3–344.5) for women. Crude age- and sex-specific prevalence estimates are reported in Table 2.
The highest estimates were reported for the age group 60–69 years in the total population (361.0 per 100,000) and among women (491.3) and for the age group 40–49 years among men (241.6). The mean (SD) age of study participants was 49.6 (13.0) years (range 17–82 years), 50.3 (10.2) years for men and 49.3 (14.0) for women (p = ns).
Fifty (74.6%) prevalent cases showed an EDSS score between 0 and 3; 8 (12%) cases had an EDSS score between 3.5 and 5.5, 4 (6%) had a score between 6 and 6.5, and 5 (7.5%) between 7 and 8.5.
The mean (SD) duration of the disease was 16.5 (10.1) years (range 1–45 years) for the total population, 20.3 (11.4) among men and 15 (9.5) among women (p = ns). The distribution of the clinical course [24] by prevalent cases was relapsing-remitting in 65.5%, primary-progressive in 15%, progressive-relapsing in 1.5%, and secondary-progressive in 18% of the cases. The most frequent symptoms among prevalence MS patients in 2014 were pyramidal disorders (38.8%) and sensitive disorders (52.0%). Familial occurrence considered up to relatives of third biological relationship was reported for a couple of brothers, a couple of sisters, one mother-daughter, and four patients with a family history of MS.
Discussion
By means of complete enumeration approach of a defined area [9], we report a mean annual MS incidence rate of 7.7 per 100,000 for the period 2005–14 and a prevalence of 204.3 per 100,000 in 2014 in the Republic of San Marino. These figures are among the highest reported in Italy and in Southern Europe [3, 7], by means of similar methodology. A prevalence of 121 per 100,000 was reported for the Republic of San Marino in 2005 [16], and an incidence of 4.4 per 100,000/year for the province of Ferrara in the Emilia-Romagna Region, lying ca. 200 km north-west of the current study site [4]. Between 2005 and 2014, no statistically significant difference in the incidence distribution was observed in San Marino, as well as for the previously studied period 1990–2005 (Table 3) [16].
As compared to those obtained from other areas in previous years, these higher estimates could be ascribed to the small size of the study population (wide 95% CI) and to more accurate case ascertainment. Epidemiological studies in smaller populations offer the advantage of minimizing the risk of failing the identification of all patients, facilitating the assessment of individual cases and their follow-up over time.
On the other hand, quite high prevalence and incidence were observed in studies carried out in neighboring areas such as in the province of Ferrara [4] benefitting from multiple ascertainments of MS over a long time period.
The current MS prevalence estimate of 204.3 per 100,000 (95% CI 158.4–259.5) in San Marino is significantly higher than that of 51.6 (95% CI 25.7–92.3) reported for 1984 [15] and, although not significantly, than that of 166.7 (95% CI 123.7–220.0) reported for 2005 [16].
The high MS prevalence burden identified in this study is consistent with most recent observations showing a sustained increase of MS prevalence in Italy [1, 5, 25], in Scotland [26, 27], in Northern Ireland [28], and in Norway [29]. Such increased burden of MS can be ascribed to increased raised life expectancy [30] both in the general population and among people with MS patients. Indeed, in the present study, the highest prevalence estimate was found in the age group 60 to 69 years, as compared to 50–54 years in previous study [16], with a mean age of MS patients at study time of 49.6 years as compared to 45.7 years. The mean disease duration has increased from 14.7 to 16.5 years. Increased prevalence can also be related to a detection of benign forms or cases at an early stage of the disease due to improved diagnostic procedures and awareness.
The proportion of patients identified without any or with a mild disability (i.e., EDSS of 0 to 3.5) is 74.6% and is higher than that in previously reported (53% in [16]), in line with a compared earlier detection of the disease in the general population.
With regard to the distribution of prevalent cases for disease course, 65.5% of the study subjects feature a relapsing-remitting disorder. Compared to the previous study, the secondary-progressive forms increased from 10 to 18% of prevalent cases, a possible expression of the increased life expectancy of people with MS.
A decreasing trend of diagnostic delay has been observed over time from 18 months in 1990 to 14 months in the present study. Similar trends have been observed in Iceland [31], Netherlands [32], Sardinia, insular Italy [12], and Ferrara, northern Italy [4].
High prevalence estimates can be explained by increased disease incidence. In the previous San Marino study [16], an increasing incidence was assumed although such distribution did not reach statistical significance and no previous data was available for comparison. A recent study carried out in the Hordaland county in Norway [29] showed similar epidemiological evidences, with a high and increasing prevalence of MS (211 per 100,000) and a high, but stable, annual incidence rate (8.5 per 100,000).
Finally, a key feature which may have strongly influenced the present results is that only patients with a definite or probable MS (according to Poser’s criteria) [18] were included in the study. Had current diagnoses of clinically isolated syndrome (CIS) been also included; the mean annual incidence rate would have risen to 10.2 per 100,000.
In this study, the female/male ratio was 2.5 for prevalence and 3.8 for incidence, in line with the ratios observed in Italian and European studies in recent years [3, 7] and with the evidence that not only MS is more frequent among women, but that such disparity is increasing. The role of environmental risk factors behind this gender-specific trend should not be overlooked [33].
Conclusions
Epidemiological descriptive studies of MS conducted in the Republic of San Marino over the past 35 years confirm this a high-risk area for the disease. Improvement of diagnostic facilities and awareness for the disease both among health operators and in the general population may account for such trends. However, the literature on incidence studies emphasizes the action of differently distributed exogenous, infectious, and/or lifestyle factors on the fluctuations of disease incidence over a relatively short time span [34,35,36,37].
References
Pugliatti M, Sotgiu S, Solinas G, Castiglia P, Pirastru MI, Murgia B, Mannu L, Sanna G, Rosati G (2001) Multiple sclerosis epidemiology in Sardinia: evidence for a true increasing risk. Acta Neurol Scand 103:20–26
Kurtzke JF (2005) Epidemiology and etiology of multiple sclerosis. Phys Med Rehabit Clin N Am 16:327–349
Pugliatti M, Rosati G, Carton H, Riise T, Drulovic J, Vecsei L, Milanov I (2006) The epidemiology of multiple sclerosis in Europe. Eur J Neurol 13:700–722
Granieri E, Economou NT, De Gennaro R et al (2007) Multiple sclerosis in the province of Ferrara: evidence of an increasing trend. J Neurol 254:1642–1648
Benito-Leon J (2011) Multiple sclerosis: is prevalence rising and if so why? Neuroepidemiology 37:236–237
Nicoletti A, Patti F, Lo Fermo S, Messina S, Bruno E, Quattrocchi G, Laisa P, Cilia S, Mostile G, Marziolo R, Scillieri R, Maimone D, Zappia M (2011) Increasing frequency of multiple sclerosis in Catania, Sicily: a 30-year survey. Mult Scler 17:273–280
Kingwell E, Marriott JJ, Jetté N, Pringsheim T, Makhani N, Morrow SA, Fisk JD, Evans C, Béland SG, Kulaga S, Dykeman J, Wolfson C, Koch MW, Marrie RA (2013) Incidence and prevalence of multiple sclerosis in Europe: a systematic review. BMC Neurol 13:128
Kurtzke JF (1980) The geographical distribution of multiple sclerosis—an update with special reference to Europe and the Mediterranean region. Acta Neurol Scand 62:65–80
Granieri E, Casetta I, Tola MR (1995) Epidemiology of multiple sclerosis in Italy and in southern Europe. Acta Neurol Scand 161:60–70
Trojano M, Lucchese G, Graziano G, Taylor BV, Simpson S, Lepore V, Grand’Maison F, Duquette P, Izquierdo G, Grammond P, Amato MP, Bergamaschi R, Giuliani G, Boz C, Hupperts R, van Pesch V, Lechner-Scott J, Cristiano E, Fiol M, Oreja-Guevara C, Saladino ML, Verheul F, Slee M, Paolicelli D, Tortorella C, D’Onghia M, Iaffaldano P, Direnzo V, Butzkueven H, MSBase Study Group and the New Zealand MS Prevalence Study Group (2012) Geographical variations in sex ratio trends over time in multiple sclerosis. PLoS One 7:e48078
Granieri E, Rosati G, Tola R, Pinna L, Carreras M, Manca M, Boldrini P (1983) The frequency of multiple sclerosis in Mediterranean Europe. An incidence and prevalence study in Barbagia, Sardinia, insular Italy. Acta Neurol Scand 68:84–89
Granieri E, Casetta I, Govoni V, Tola MR, Marchi D, Murgia SB, Ticca A, Pugliatti M, Murgia B, Rosati G (2000) The increasing incidence and prevalence of MS in a Sardinian province. Neurology 55:842–848
Savettieri G, Salemi G, Ragonese P, Aridon P, Scola G, Randisi G (1998) Prevalence and incidence of multiple sclerosis in the city of Monreale, Italy. J Neurol 245:40–43
Grimaldi LM, Palmeri B, Salemi G, Giglia G, D’Amelio M, Grimaldi R, Vitello G, Ragonese P, Savettieri G High prevalence and fast rising incidence of multiple sclerosis in Caltanissetta, Sicily, southern Italy(2007) Neuroepidemiology 28:28–32
Morganti G, Naccarato S, Ellan M et al (1984) Multiple sclerosis in the Republic of San Marino. J Epidemiol Community Health 38:23–28
Granieri E, Monaldini C, De Gennaro R et al (2007) Multiple sclerosis in the Republic of San Marino: a prevalence and incidence study. Mult Scler 00:1–5
Statistics Office of the Republic of San Marino (2015) Demographic balance (movement of the resident population), www.statistica.sm/on-line/en/home/statistics/docCat.14000847.1.10.1.html. Accessed 30 Sept 2015
Poser CM, Paty DW, Scheinberg L, McDonald WI, Davis FA, Ebers GC, Johnson KP, Sibley WA, Silberberg DH, Tourtellotte WW (1983) New diagnostic criteria for multiple sclerosis: guidelines for research protocols. Ann Neurol 13:227–231
Kurtzke JF (1983) Rating neurologic impairment in multiple sclerosis: an expanded disability status scale (EDSS). Neurology 33:1444–1452
Italian National Institute of Statistics (2011) Population Census. http://dati-censimentopopolazione.istat.it/Index.aspx?lang=en. 2012, Accessed 30 Sept 2015
Waterhouse JAH, Muir CS, Correa P et al (eds) (1976) Cancer incidence in five continents, vol 3. IARC, Lyon, p 456
Schoenberg BS (1983) Calculating confidence intervals for rates and ratios: simplified methods utilizing tabular values based in the Poisson distribution. Neuroepidemiology 2:257–265
Armitage P (1995) Tests for linear trends in proportions and frequencies. Biometrics 11:375–386
Lublin FD, Reingold SC (1996) Defining the clinical course of multiple sclerosis: results of an international survey. Neurology 46:907–911
Ranzato F, Perini P, Tzintzeva E, Tiberio M, Calabrese M, Ermani M, Davetag F, de Zanche L, Garbin E, Verdelli F, Villacara A, Volpe G, Moretto G, Gallo P (2003) Increasing frequency of multiple sclerosis in Padova, Italy: a 30 year epidemiological survey. Mult Scler 9:387–392
Forbes RB, Wilson SV, Swingler RJ (1999) The prevalence of multiple sclerosis in Tayside, Scotland: do latitudinal gradients really exist? J Neurol 246:1033–1040
Handel AM, McLaughlin R, Fries A et al (2011) The epidemiology of multiple sclerosis in Scotland: inferences from hospital admissions. PLoS One 6:e14606
McDonnell GV, Hawkins SA (1998) An epidemiologic study of multiple sclerosis in Northern Ireland. Neurology 50:423–428
Grytten N, Aarseth JH, Lunde HMB et al (2015) A 60-year follow-up of the incidence and prevalence of multiple sclerosis in Hordaland County, Western Norway. J Neurol Neurosurg Psychiatry 0:1–6
Govoni V, Casetta I, Granieri E, Vernonesi V, Malagù S, Tola MR, Paolino E, Fainardi E, Monetti VC, Aiello I (1993) Mortality study on multiple sclerosis in the province of Ferrara, northern Italy, 1968 through 1989. Acta Neurol 15:161–176
Benedikz J, Magnésson H, Guòmundsson G (1994) Multiple sclerosis in Iceland, with observations on the alleged epidemic in the Faroe Islands. Ann Neurol 36:S175–S179
Kramer MA, Van der Maas NAT, Van Soest EM et al (2012) Incidence of multiple sclerosis in the general population in the Netherlands, 1996–2008. Neuroepidemiology 39:96–102
Alonso A, Hernán M (2008) Temporal trend in the incidence of multiple sclerosis. Neurology 71:129–135
Casetta I, Granieri E (2000) Clinical infections and multiple sclerosis: contribution from analytical epidemiology. J Neuro-Oncol 6:S147–S151
Pugliatti M, Riise T, Sotgiu A et al (2006) Evidence of early childhood as the susceptibility period in multiple sclerosis: space-time cluster analysis in a Sardinian population. Am J Epidemiol 164:326–333
Ascherio A, Munger KL (2010) 99th Dahlem conference on infection, inflammation and chronic inflammatory disorders: Epstein-Barr virus and multiple sclerosis: epidemiological evidence. Clin Exp Immunol 160:120–124
Simon KC, Van der Mei I, Munger KL et al (2010) Combined effects of smoking, anti-EBNA antibodies, and HLA-DRB1*1501 on multiple sclerosis risk. Neurology 74:1365–1371
Acknowledgements
The authors thank Eva Sjolin for her help in revising the translation of the text.
Funding
This work is supported by Ferrara University (Fondo di Ateneo per la Ricerca).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
Ethics approval for the study was obtained.
Rights and permissions
About this article
Cite this article
Caniglia-Tenaglia, M., Guttmann, S., Monaldini, C. et al. Multiple sclerosis in the Republic of San Marino, Italian peninsula: an incidence and prevalence study from a high-risk area. Neurol Sci 39, 1231–1236 (2018). https://doi.org/10.1007/s10072-018-3402-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-018-3402-6