Abstract
Olfactory hypersensitivity may occur during migraine attacks and has been found to be very specific for this form of headache. Aim of this study was to investigate if migraineurs with ictal osmophobia have particular clinical features comparing to patients without ictal osmophobia. We recruited 200 consecutive migraineurs. Other primary headaches comorbidity and migraine prophylaxis were exclusion criteria. Each patient was interviewed following a structured questionnaire including general features about migraine, depression and anxiety symptoms. Migraine triggers both spontaneously and selecting from a specific list. Allodynia during the migraine attack was measured using the Allodynia symptoms check-list 12 (ASC-12). Eighty four (42 %) patients are non-osmophobic vs. 116 patients (58 %) who are osmophobic. After a logistic regression analysis, pain intensity (OR 1.391; p = 0.008) and anxiety (OR 1.099; p = 0.047) were significantly higher while aura (OR 0.421; p = 0.028) is less frequent in osmophobic migraineurs. We found significant differences in clinical features of osmophobic patients in respect to non-osmophobic ones. Ictal osmophobia seems being related to a broader sensorial hypersensitivity that could lead to a more florid clinical presentation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Migraine is a complex disorder and its pathogenesis is more complex than one thought in the past [1]. Beyond pain, sensation is altered during the migraine attack in which a general hyperaesthesia is a very common condition [2]. Although ictal osmophobia is not included between the classical diagnostic accompanying symptoms of migraine [3], olfactory hypersensitivity may occur during migraine attacks and it has been found very specific for this form of headache [4]. However, very few investigations have focused on the possible different clinical phenotype of migraine patients with osmophobia in respect to non-osmophobic migraineurs. Aim of this study was to investigate if migraineurs with ictal osmophobia have particular clinical features comparing to patients without ictal osmophobia.
Materials and methods
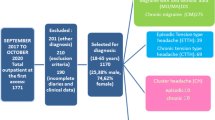
We performed a cross-sectional study in our outpatient headache clinic collecting data from a series of 200 consecutive patients which were evaluated by a neurologist with expertise in headache during the period February 2011–February 2013. A diagnosis of migraine with or without aura was made according to the criteria of the International classification of headache disorders-2nd edition (ICHD-II) [3]. Part of the population (120 migraineurs) and data collection methodology of this study have been described previously [5]. In brief, patients were interviewed following a structured questionnaire that included demographic characteristics, duration of migraine illness, duration of migraine attack, headaches per month, scoring of global intensity on a verbal numeric scale (VNS) from 0 (no pain) to 10 (extremely intense pain), quality of pain, site of pain, associated headache symptoms (the presence or not of photophobia, phonophobia, osmophobia, nausea/vomit, autonomic signs), headache triggers [5, 6]. Ictal allodynia was assessed with the allodynia symptoms check-list 12 (ASC-12) [7] with a cut-off of ASC-12 score of >2 defining allodynic patients. Anxiety and depression symptoms were measured in each patient by two brief self-reported scales: the generalized anxiety disorder 7-item scale (GAD-7) [8] assessing anxiety symptoms, and the Patient Health Questionnaire 9-item scale (PHQ-9) [9] evaluating depression symptoms.
Exclusion criteria were: (a) age <18 years; (b) recent onset of headaches (<6 months prior to study inclusion); (c) presence of other types of headaches (including medication overuse headache); (d) current or past prophylactic headache therapy; (e) recent use of hormonal contraception (<6 months); and (f) concurrent relevant medical condition including a previous psychiatric diagnosis. Informed written consent was obtained from each patient.
Statistical analysis
For calculations and statistical analyses SPSS version 16.0 for Windows was used. Our outcome was to find clinical differences in migraineurs with ictal osmophobia in respect to migraine subjects without ictal osmophobia. Continuous variables were expressed as mean ± standard deviation (SD). Categorical variables were expressed in terms of percentages frequency. Chi [2] test with continuity correction or Fisher’s exact test, when appropriate, was used for categorical variables to compare migraineurs without ictal osmophobia in respect to osmophobic migraineurs (for the multiple comparisons p < 0.01 was considered significant); for continuous variables a t test with Bonferroni correction for multiple comparisons was performed in the same two groups. Further, in a binary logistic regression model we divided the patients into those with no ictal osmophobia and those with ictal osmophobia. Thus, we tested the influences on the presence of ictal osmophobia of: sex (female/male), diagnosis (migraine without/with aura), allodynia (no/yes), unilateral pain (no/yes), photophobia (no/yes), phonophobia (no/yes), nausea/vomit (no/yes), autonomic signs (no/yes), throbbing pain (no/yes), headaches/month, migraine illness duration, VNS, triggers, GAD-7, PHQ-9, age, headaches per month, triggers (continuous variables). In this study, all p values were two tailed.
Results
Demographic and clinical characteristics
Detailed data about the migraine population were reported in a previous study and in supplementary materials. In our clinic population, of the 200 patients studied, 167 (83.5 %) were female, and mean age 38.49 years ± 11.44; 44 patients (22.0 %) had migraine with aura, 32 patients (16.0 %) had a chronic form of migraine. The mean migraine illness duration was 15.88 ± 12 years. The headaches per month were 6.68 ± 5.77 in the previous 3 months. The number of triggers was 7.0 ± 3.7. The mean intensity of migraine attacks on a VNS resulted 8.38 ± 1.37 points.
Ictal allodynia score measured with ASC-12 was 5.8 ± 4.2; ASC-12 score ≤2 identified 42 patients (21.0 %) as no allodynic, and ASC-12 score >2 identified 158 patients (79 %) as allodynic. Mean GAD-7 and PHQ scores were 8.5 ± 5.2 and 6.1 ± 4.2, respectively (Table 1).
Comparison between groups and logistic regression
Migraineurs osmophobic during the acute attack were 116 (58 %) vs 94 (42 %) that were non-osmophobic. Patients with osmophobia had significantly more severe attacks (p = 0.002) after correction for multiple comparisons (Tables 2, 3). The logistic regression model was statistically significant χ2 = 35.914, n = 200, p < 0.05. The model as whole was able to distinguish between 16.4 and 22.1 % of the variance and correctly classified 72 % of cases. Only aura, pain attack intensity (VNS) and anxiety symptoms (GAD-7) as independent variables made a unique statistical contribution to the model. In particular, on reporting ictal osmophobia: (a) aura an odds ratio of 0.421 (95 % CI 0.195–0.909; p = 0.028), (b) pain intensity expressed as a 0–10 points VNS indicating that for every additional point the odds ratio is 1.391 (95 % CI 1.089–1.776; p = 0.008) and (c) anxiety symptoms expressed as GAD-7 score indicating that for every additional point the odds ratio is 1.099 (95 % CI 1.001–1.207; p = 0.047) (Table 4).
Discussion
In our sample osmophobia is referred in the 58 % of migraineurs during the acute attack and this fits quite well with the literature data [4, 10, 11]. We found significant differences in clinical features of osmophobic patients in respect to non-osmophobic ones. Pain intensity is significantly higher in migraineurs presenting ictal osmophobia as well as anxiety. Only aura accompanying symptoms is a symptom less frequent in migraineurs with ictal osmophobia than in migraineurs without one. This last finding agrees with the results of a large previous study where a trend of a larger prevalence of osmophobia in migraineurs without aura (43.9 %) in respect to migraineurs with aura was reported (38.5 %). However, in general, osmophobic patients have a more florid clinical picture and more affective symptoms. Interestingly, it may be the significative association of ictal osmophobia with affective symptoms and in particular anxiety. Functional imaging studies during migraine attacks have revealed activation in areas related to pain matrix including limbic system, such as insula, thalamus, cingulate cortex [1, 11, 12]. In mood and anxiety disorders, several limbic areas have been found altered (e.g. amygdale, anterior cinguli, periacqueductal gray) [1]. Smell is innate related to limbic system. Olfactory hypersensitivity, anxiety and pain share common neural pathways and area activation, and a possible functional association and interaction one each other might be argued, basing both on imaging data and on the clinical experience that migraine is a complex disorder [1]. Moreover, we found that, as a trend, triggers susceptibility seems to be more elevated in osmophobic patients as well as number of headache days per month, attack duration, migraine disease duration, photophobia, phonophobia and allodynia occurrence. This is in line with a more broad concept of cortical hyperexcitability in migraine [4], as already reported for the visual and auditory systems [13]. Definitely, ictal osmophobia seems being related to a broader sensorial hypersensitivity that could lead to more long-lasting, more intense headaches and maybe further investigations should assess if it could be a risk factor for migraine transformation as well as it has been suggested for cutaneous allodynia [14]. In conclusion, we found that migraineurs with ictal osmophobia show different clinical features comparing to patients without ictal osmophobia and in particular more intensity of the pain during the attack, anxiety symptoms and less migraine with aura seems to be associated.
Abbreviations
- ASC-12:
-
Allodynia symptoms check-list 12
- BMI:
-
Body max index
- GAD-7:
-
Generalized anxiety disorder 7-item scale
- ICHD-II:
-
International classification of headache disorders-2nd edition
- PHQ-9:
-
Patient Health Questionnaire 9-item scale
References
Maizels M, Aurora S, Heinricher M (2012) Beyond neurovascular: migraine as a dysfunctional neurolimbic pain network. Headache doi:10.1111/j.1526-4610.2012.02209.x. [Epub ahead of print]
Burstein R, Jakubowski M, Garcia-Nicas E, Kainz V, Bajwa Z, Hargreaves R, Becerra L, Borsook D (2010) Thalamic sensitization transforms localized pain into widespread allodynia. Ann Neurol 68:81–91
Headache Classification Subcommittee of the International Headache Society (2004) The international classification of headache disorders, 2nd edn. Cephalalgia 24(Suppl. 1):1–160
Zanchin G, Dainese F, Trucco M, Mainardi F, Mampreso E, Maggioni F (2007) Osmophobia in migraine and tension-type headache and its clinical features in patients with migraine. Cephalalgia 27:1061–1068
Baldacci F, Vedovello M, Ulivi M, Vergallo A, Poletti M, Borelli P, Cipriani G, Nuti A, Bonuccelli U (2013) Triggers in allodynic and non-allodynic migraineurs. A clinic setting study. Headache 53(1):152–160
Baldacci F, Vedovello M, Ulivi M, Vergallo A, Poletti M, Borelli P, Nuti A, Bonuccelli U (2013) How aware are migraineurs of their triggers? Headache 53(5):834–837
Lipton RB, Bigal ME, Ashina S, Burstein R, Silberstein S, Reed ML, Serrano D, Stewart WF (2008) American Migraine Prevalence Prevention Advisory Group. Cutaneous allodynia in the migraine population. Ann Neurol 63(2):148–158
Spitzer RL, Kroenke K, Williams JB et al (2006) A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med 166:1092–1097
Kroenke K, Spitzer RL, Williams JB (2001) The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med 16:606–613
Sjöstrand C, Savic I, Laudon-Meyer E, Hillert L, Lodin K, Waldenlind E (2010) Migraine and olfactory stimuli. Curr Pain Headache Rep 14(3):244–251
Morillo LE, Alarcon F, Aranaga N, Aulet S, Chapman A, Conterno L et al (2005) Clinical characteristics and patterns of medication use of migraineurs in Latin America from 12 cities in 6 countries. Headache 45:118–126
Phan KL, Wager TD, Taylor SF, Liberzon I (2004) Functional neuroimaging studies of human emotions. CNS Spectr 9:258–266
Stankewitz A, May A (2011) Increased limbic and brainstem activity during migraine attacks following olfactory stimulation. Neurology 77(5):476–482
Bigal ME, Lipton RB (2008) Clinical course in migraine: conceptualizing migraine transformation. Neurology 71(11):848–855
Conflict of interest
In the past year, Ubaldo Bonuccelli has received fees for consultation from GSK and Eisai and for speeches from Novartis, GSK and Lundbeck. The remaining authors have nothing to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Baldacci, F., Lucchesi, C., Ulivi, M. et al. Clinical features associated with ictal osmophobia in migraine. Neurol Sci 36, 43–46 (2015). https://doi.org/10.1007/s10072-014-1903-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-014-1903-5