Abstract
A number of MRI studies have shown focal or diffuse cortical gray matter (GM) abnormalities in patients with post-traumatic stress disorder (PTSD). However, the results of these studies are unclear regarding the cortical regions involved in this condition, perhaps due to the heterogeneity of the PTSD population included or to the differences in the methodology used for the quantification of the brain structures. In this study, we assessed differences in cortical GM volumes between a selected group of 25 drug-naive PTSD patients with history of adulthood trauma and 25 matched non-traumatized controls. Analyses were performed by using two different automated methods: the structural image evaluation using normalization of atrophy (SIENAX) and the voxel-based morphometry (VBM), as we trusted that if these complementary techniques provided similar results, it would increase the confidence in the validity of the assessment. Results of SIENAX and VBM analyses similarly showed that cortical GM volume decreases in PTSD patients when compared to healthy controls, particularly in the frontal and occipital lobes. These decreases seem to correlate with clinical measures. Our findings suggest that in drug-naïve PTSD patients with a history of adulthood trauma, brain structural damage is diffuse, with a particular prevalence for the frontal and occipital lobes, and is clinically relevant.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Post-traumatic stress disorder (PTSD) is a chronic, debilitating psychiatric disorder that can occur following traumatic events, and that comprises re-experiencing, avoidance, and hyper-arousal symptoms. It has been recognized as a formal diagnosis since 1980. For many years, PTSD was associated with war experiences. In recent times, this disorder has attracted public attention following tragic events related to international terrorism. Several quantitative MRI studies investigated the pathophysiology of PTSD showing decreases in volume that either are localized in specific brain areas such as the limbic system and medial prefrontal cortex [1–8] or are diffusely present in the brain gray matter (GM) [9–14]. The latter seems to be the case in PTSD subjects who experienced the trauma during childhood [9–11], even though it was recently suggested that the same is also true in PTSD patients who experienced the trauma during adulthood [12–14]. The heterogeneity of the PTSD population included in the different studies, as well as the differences in the methodology used for the quantification of the brain structures might be, at least in part, the cause of these unclear results.
Among the many valid approaches to obtain MRI-based measures of brain volume changes, automated analysis methods have the advantage of providing good reproducibility and reducing reliance on time-consuming user intervention. The cross-sectional version of the structural imaging evaluation, using the normalization of atrophy method (SIENAX), part of the FMRIB Software Library (FSL, http:\\www.fmrib.ox.ac.uk) is an increasingly used method that automatically estimates global and regional brain tissue volumes normalized for subject head size [15]. Using this method, tissue-type segmentation with partial volume estimation is carried out in order to estimate volumes of specific GM regions. Regional measures of GM volume changes can also be obtained more indirectly by using the voxel-based morphometry (VBM) approach [16]. This is a widely used method, valuable for voxelwise comparisons of the local concentration of specific GM regions between two groups of subjects. Both methods have been extensively used in clinical studies to accurately assess global and regional volume loss [17, 18].
In a recent MR study of PTSD patients specifically selected for the absence of specific drug treatment and comorbidity conditions, we reported decreases in both hippocampal and cortical GM volumes. The latter, however, was a global measure that was not able to discriminate where in the cortex the decrease in volume was occurring. Thus, in the present study, we sought to investigate a similar population of PTSD subjects by using both SIENAX and VBM approaches in order to assess regional brain volume alterations and evaluate whether these alterations are specifically localized or attributable to a more widespread process. Finally, the use of two different methods for assessing brain volume measurement aimed at overcoming the conflicting results of previous studies, as we trusted that if two complementary techniques such as VBM and SIENAX provided similar results, it would have increased the confidence in the validity of the assessment.
Materials and methods
Subjects
The sample consisted of 25 PTSD subjects and 25 matched controls. PTSD subjects were recruited at the center for the diagnosis and treatment of PTSD, Department of Psychiatry, University of Siena. We initially screened 40 patients (25 females and 15 males, mean ± SD age 43.56 ± 12.75-year-old) who were diagnosed with PTSD from January 2004 to September 2007. Criteria of exclusion were history of traumas experienced during childhood, history of traumatic brain injury, presence of Axis I and Axis II psychiatric diagnoses other than PTSD and presence of neurological, endocrine, and degenerative disorders. On the basis of a structured clinical interview for DSM-IV (SCID), we selected 25 patients (17 females and 8 males, age mean ± standard deviation [SD] 38 ± 10 years) from the initial sample of 40 subjects. They were all drug-naïve, had experienced traumas during adulthood, and had a single diagnosis of PTSD without any other current or lifetime diagnosis. All patients underwent MRI scan before starting any type of treatment. For comparison, 25 healthy subjects were recruited from the general population of Siena. They were matched with the PTSD population in age and sex (17 females and 8 males, age mean ± SD: 38 ± 11 years), handedness and education. Exclusion criteria for the controls were presence of lifetime or current histories of psychiatric disorders, including alcohol and substance use disorders as determined by the SCID Non-Patient Version [19], traumatic brain injury, presence of neurological, endocrine and degenerative disorders, and previous or current use of any psychotropic medications. The study design was approved by the University of Siena Committee and was prepared in accordance with the ethical standards laid down in the Declaration of Helsinki. A written informed consent was obtained from all subjects who participated in the study after complete written and verbal descriptions of the study were provided.
Clinical assessments
All PTSD subjects were evaluated with the SCID for DSM-IV and the Clinician Administered PTSD Scale (CAPS) [20]. Diagnosis of PTSD was confirmed by the consensus of two clinicians (MT and SC). All patients had a single diagnosis of PTSD and had not had any other current or lifetime diagnoses on the basis of Axis I and Axis II interviews with SCID-I/P [21] and SCID-II/P [22]. This included alcohol or other substance use disorders. Furthermore, the Hamilton Depression Rating Scale (HAM-D) [23] and the Hamilton Anxiety Rating Scale (HAM-A) [24] were obtained from all PTSD subjects to evaluate the overlapping symptoms between PTSD, major depressive disorder, and state of anxiety.
Neuroimaging
Acquisition
Conventional MRI examinations of all subjects were performed at the University of Siena Magnetic Resonance Research Centre using an identical protocol. They were obtained in a single session on a 1.5 Tesla Philips Intera Machine (Philips Medical Systems, Best, The Netherlands). The data used for the present study were the T1-weighted FFE 1-mm-thick images of the entire brain (TE = 4.6 ms, TR = 30.00 ms, flip angle = 30.00°, FOV = 250 mm, matrix 256 × 256, slice number = 150), which were acquired in the axial plane parallel to the line connecting the anterior and posterior commissures.
SIENAX
Global and regional brain volumes were calculated on axial T1-FFE images through the SIENA package in its “cross-sectional” version (SIENAX, part of FSL 4.0) (http://www.fmrib.ox.ac.uk/fsl/), a previously described method to estimate the global brain volume normalized for head size [15]. In its latest version, SIENAX allows global measures of normalized brain parenchymal volume as well as selective measurement of normalized cortical volumes, including specific cortical regions on pre-definite standard space masks, as previously described [25, 26]. In this study, an improved brain extraction tool (BET) was used to perform a better separation of brain from non-brain tissue, avoiding manual correction [27]. Normalized volumes of total brain, total GM, cortical GM, insula, frontal, temporal, parietal and occipital lobes of both hemispheres were considered. The pre-definite standard space masks used for these localized measures were derived from the Harvard-Oxford Cortical Structural Atlas, as included in FSL 4.0 (http://www.fmrib.ox.ac.uk/fsl).
FSL-VBM
Axial T1-FFE images were also used to assess GM data as analyzed with a VBM-style analysis, which was carried out by using FSL tools [28]. First, images were brain-extracted as described above. Then, tissue-type segmentation was carried out using FAST [29], providing images representing partial volume estimates of GM, WM, and CSF. The resulting GM partial volume images were aligned with MNI152 standard space using the non-linear registration [30]. These images were then averaged to create a study-specific template (from GM images of the entire sample of PTSD patients and normal controls) in order to reduce the effect of inter-subject structural variability during the registration step, as described previously [31]. This template was used to non-linearly register the native GM images. Each voxel of these registered GM images was then divided by the Jacobian determinant of the warp field (modulation step). Each modulated-normalized cortical GM image was smoothed with an isotropic Gaussian kernel with a sigma of 2.5 mm (~5.75 mm FWHM). The final output was a series of 3D images in which the three indices were the spatial x, y, and z coordinates of voxels in the reference space, and each value of the matrix was proportional to the gray matter volume within each voxel. The output of each stage of the analysis was visually checked according to FSL-VBM guidelines. The Harvard-Oxford Cortical Structural Atlas, as included in FSL 4.0 (http://www.fmrib.ox.ac.uk/fsl) was used as an anatomical reference to assess the localization of significant differences of cerebral GM between the two groups.
Statistical analysis
The statistical analyses were performed using SPSS version 13.0 for Windows (SPSS Inc., Chicago, IL, USA). The distribution of data variables was assessed for normality using the Shapiro–Wilk test [32]. The Levene’s test [33] was used to assess the equality of variance of the data. Variables were compared using unpaired t tests when they were continuous and with the Mann–Whitney U test when they were non-normally distributed.
An ANCOVA for repeated measures was conducted to compare SIENAX regional outputs, using (1) two between-subject factors: group (PTSD subjects vs. healthy controls) and gender (female vs. male); (2) and two within-subject factors: side (left vs. right) and cerebral volumes (frontal, occipital, parietal, temporal, and insula), followed by post-hoc ANCOVAs.
In the VBM-style analysis, differences in cortical GM volume between PTSD patients and controls were assessed using an unpaired t test within the framework of the general linear model (GLM). Statistical inference was carried out using permutation testing [34], with 5,000 permutations as implemented in the “randomize” program, also part of FSL [35]. Cluster-size thresholding (t > 2.3) at p values <0.05, fully adjusted for multiple comparisons across space, was used.
Correlations between clinical, demographic, and volumetric variables (as measured by SIENAX and VBM-style analyses) were performed using two-tailed Spearman’s rho.
The level of 0.05 was used for all statistical tests. Bonferroni’s correction for multiple comparisons was used when appropriate.
Results
Sample characteristics
Patients and controls were right-handed and they did not differ for either age (t = −0.026; df = 48; p = 0.980), or education (U = 294.50; N = 50; p = 0.722); they were matched for sex. Table 1 provides information regarding illness duration; age when trauma occurred, PTSD severity (measured by CAPS), and depressive and anxiety symptoms (measured by HAM-D and HAM-A). In our sample, 14 patients had been exposed to a single traumatic event that caused PTSD, according to DSM-IV criteria, whereas 11 patients had been exposed to two traumatic events. No patients had experienced trauma-causing PTSD during childhood, according to DSM-IV criteria. According to the total score of the CAPS, all subjects were diagnosed with moderate to severe PTSD.
Volumetric results
SIENAX
The unpaired t test showed that between the two groups, there were no significant differences in normalized total brain volume (t = 0.93; df = 48; p = 0.35), while normalized volumes of the total GM (t = 3.31; df = 48; p = 0.002), and cortical GM (t = 2.70; df = 48; p = 0.01) were smaller in PTSD patients than in controls (Table 2). The ANCOVA with group and gender as the between-subject factors, and side and cerebral volumes (frontal, occipital, parietal, temporal and insula) as the within-subject factors showed that there was: (1) a significant difference between groups (F = 3.02; df = 5,42; p = 0.02); (2) no significant difference between genders (F = 1.051; df = 5,42; p = 0.207), and (3) a significant main effect for side (F = 73.07; df = 5,42; p < 0.001). No significant interactions among other factors were found.
The results also showed that there were significant differences between the two groups in frontal (7.3%) (F = 7.133; df = 1,46; p = 0.010) and occipital (8.2%) (F = 7.88; df = 1,46; p = 0.007) lobes (Fig. 1), with a trend toward significance in the insula (F = 4.14; df = 1,46; p = 0.04), but not in parietal (F = 2.70; df = 1,46; p = 0.10) and temporal lobes (F = 2.48; df = 1,46; p = 0.12).
Post-hoc ANCOVAs with diagnosis as between factors showed that PTSD subjects had smaller left (7.5%) (F = 8.05; df = 1,48; p = 0.007) and right (7.1%) (F = 7.78; df = 1,48; p = 0.008) frontal lobes, as well as smaller left (9.6%) (F = 12.18; df = 1,48; p = 0.001) and right (7.0%) (F = 7.59; df = 1,48; p = 0.008) occipital lobes (Table 2).
VBM
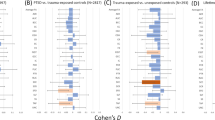
The VBM-style analysis revealed that PTSD subjects had lower GM volume compared to healthy controls. Specifically, lower GM volume was found in the left side of the frontal lobe (i.e., in the frontal pole, superior frontal gyrus, middle frontal gyrus, inferior frontal gyrus-pars triangularis, paracingulate gyrus, precentral gyrus, and in the postcentral gyrus). Bilaterally, lower GM volume was found in regions of the occipital lobes such as the posterior cingulate gyrus, intracalcarine cortex, lateral occipital cortex, lingual gyrus, occipital fusiform gyrus, occipital pole, precuneous cortex, supracalcarine cortex, and the temporal occipital fusiform cortex.
Finally, PTSD subjects had lower GM volume in the right inferior temporal gyrus (Fig. 2; Table 3).
Voxel-based morphometry analysis between the groups of healthy controls and PTSD patients. Red-yellow shows significant clusters of voxels (corrected for multiple comparisons across space at p < 0.05) with reduced gray matter volume in PTSD patients compared to healthy controls. Background image is the MNI152. All images are shown in radiological convention
Correlations
On SIENAX measurements, the cortical volumes did not correlate with age, years of education, duration of illness, and time since trauma. A significant negative correlation between cortical GM volumes and the score of re-experiencing subscale of CAPS (Spearman’s r = −0.494; p = 0.012) was found. Furthermore, the re-experiencing score was negatively correlated with PTSD cortical volumes on the frontal (r = −0.508; p = 0.010), and occipital (r = −0.400; p = 0.048) lobes. Results also showed that HAM-A total score was negatively correlated with volumes of cortical GM (r = −0.437; p = 0.029).
VBM-based measurements of the left frontal lobe appeared to be significantly negatively correlated with the score of re-experiencing subscale of CAPS (Spearman’s r = −0.412; p = 0.041). In contrast, no correlation between GM volume in left and right occipital lobes and clinical variables were found.
Discussion
PTSD is a psychiatric disorder, which was recognized as a formal diagnosis in 1980. For many years, PTSD was associated with war experiences. Recently this disorder has attracted public attention following tragic events related to international terrorism. However, the vast majority of PTSD cases are actually related to civilian traumas (i.e., personal violence, car accidents, robbery, rape), with a lifetime prevalence in the US population of 6.8% [36] and the annual prevalence of 3.5% [37]. With the advancement of the MR technique, several quantitative MRI studies have been performed to understand both structural and functional alterations in the brain related to PTSD with heterogeneous results [38, 39].
In the present study, by using two automated methods for assessing MRI-based measures of brain volume changes, we showed that PTSD patients, when compared to healthy controls, have smaller cortical GM and that this decrease in volume appears to be widespread in the brain cortex, largely involving the frontal and the occipital. Thus, our results add to previous data providing evidence that the structures located in the medial prefrontal cortex and in the limbic system may not be the only areas involved in PTSD, and suggest that the alterations in brain structure might be of a more global nature than the one often reported in the literature [1–7]. This seems to be particularly the case when the PTSD population is selected to have a single diagnosis of PTSD caused by trauma experienced during adulthood, is drug-naïve and other comorbidity conditions have been carefully excluded.
The two automated measures of brain volume changes used in our study independently showed that cortical decreases are more pronounced in large portions of the frontal lobes (see Tables 2, 3). The significant involvement of the frontal lobes appears to be in line with the hypothesis that PTSD may be associated with a global alteration in frontal lobe functions [40]. Several functional MRI studies involving both active task and resting paradigms suggest that PTSD subjects had altered functions in several frontal areas (i.e., medial prefrontal cortex, ventral and dorsal prefrontal cortex, orbitofrontal cortex, inferior frontal gyrus, middle frontal gyrus anterior and posterior cingulated cortex [41, 42]), involved in pain [43], memory [44], and extinction processes [45]. Moreover, it is particularly interesting to note that in both SIENAX and VBM analyses, frontal volume decreases were negatively correlated with the cluster B (re-experiencing) of PTSD symptoms, the cluster that is more closely related to conditioned fear, suggesting a clinical relevance of the volume decreases.
The cortical volume of both left and right occipital lobes also appeared to be significantly more decreased in our PTSD patients than in controls with both the SIENAX and the VBM-style analyses. The occipital lobes seem to be implicated in the dissociative responses of PTSD subjects [46] as well as in the emotive aspect of visual stimuli [47]. Thus, structural abnormalities of the occipital lobes found here and in a previous PTSD study of female victims of intimate partner violence [11] could be due to the role played by stress in the modification of this sensory brain area. However, it must be stressed that the role of occipital cortex in PTSD has not been studied enough to draw any specific conclusions and the possibility that the abnormalities found here could simply be due to a pancortical process cannot be excluded.
In the present study, the VBM analysis showed that PTSD subjects had lower GM volume in the right inferior temporal gyrus. This seems to agree with previous MRI studies [5, 12, 14, 49, 50], which provided additional evidence of the involvement of the temporal lobe in this disorder. In contrast, in the present study, we did not find a specific involvement of the anterior cingulate gyrus, although morphological alterations of this brain structure have been found in previous studies [4, 7, 51, 52]. Finally, our analyses did not show any differences in hippocampal and amygdala volume, brain structures previously indicated as involved in PTSD [53]. A reasonable explanation to this could be that significant involvement of hippocampi and amygdala was found in previous studies only when the volumetric analysis was specifically focused on these structures, either by a manual outline [1, 2, 13] or by a region-driven VBM analysis [7]. This was not the case in our study.
It should be noted that, in the present work, an effort was made to minimize potential sources of confounding factors that could influence the results. First, only subjects who had experienced trauma during adulthood were included in the study; therefore, the results cannot be explained by the influence of early traumas on neurodevelopment processes, as suggested by investigations performed with subjects with childhood traumas [9–11]. Second, we investigated patients with PTSD who had experienced heterogeneous types of civilian traumas rather than war traumas. Third, PTSD subjects with other psychiatric conditions or in treatment with any psychoactive drug were excluded from the study, while the group of non-PTSD subjects used for comparison was carefully selected to have similar sex, handedness, and years of education with that of PTSD patients. Finally, the two fully automated techniques deployed for the analysis allowed an objective and comprehensive assessment of the anatomical brain regions, avoiding the potential bias (i.e., within-subject variability) of manual intervention. In this context, the similar findings obtained with two complementary methods such as SIENAX and VBM-style increased our confidence in the validity of the analysis and ensured the accuracy and robustness of our results.
There were, however, limitations in our study. First, our sample size was relatively small and this might have affected our results. However, this was in the range of the previously published studies, with the above-mentioned peculiarity that our sample was carefully selected to be drug-naive with a history of adulthood trauma. Second, neuropsychological data (e.g., IQ, executive tasks, and working memory) were not collected in our study. Consequently we could not rule out whether lower IQ could be a risk factor for PTSD, as recently suggested [14, 54], or could be associated in patients with more decreased volumes [55, 56].
Even if the empirical evidence reported in the present study points towards a global nature of brain alterations in PTSD patients with a more pronounced involvement of frontal and occipital lobes, no definite explanations can be given to clarify the underlying mechanisms of this effect. Several factors may influence the structural brain damage found in the cortex of these patients. This may be due to a generalized neurotoxic effect caused by stress mediators (i.e., glucocorticoids) on brain structure [48, 57], but might also be related, at least in part, to the combination of both environmental and genetic factors [58, 59]. Longitudinal studies, providing a better understanding of the temporal relationships between brain morphological alterations and PTSD patients could be very useful in this context. These studies should consider the use of tissue-specific quantitative MR techniques such as MR spectroscopy and diffusion tensor imaging, able to investigate metabolic and micro structural changes of both gray and white matter abnormalities and potentially providing new insight into this interesting psychiatric disorder.
References
Lindauer RJ, Vlieger EJ, Jalink M, Olff M, Carlier IV, Majoie CB, den Heeten GL, Gersons BP (2004) Smaller hippocampal volume in Dutch police officers with posttraumatic stress disorder. Biol Psychiatry 56:356–363
Wignall EL, Dickson JM, Vaughan P, Farrow TFD, Wilkinson ID, Hunter MD, Woodruff PWR (2004) Smaller hippocampal volume in patients with recent-onset posttraumatic stress disorder. Biol Psychiatry 56:832–836
Corbo V, Clement MH, Armony JL, Pruessner JC, Brunet A (2005) Size versus shape differences: contrasting voxel-based and volumetric analyses of the anterior cingulate cortex in individuals with acute posttraumatic stress disorder. Biol Psychiatry 58:119–124
Woodward SH, Kaloupek DG, Streeter CC, Martinez C, Schaer M, Eliez S (2005) Decreased anterior cingulate volume in combat-relate PTSD. Biol Psychiatry 59:582–587
Karl A, Schaefer M, Malta LS, Dörfel D, Rohleder N, Werner A (2006) A meta-analysis of structural brain abnormalities in PTSD. Neurosci Biobehav Rev 30:1004–1031
Chen S, Xia W, Li L, Liu J, He Z, Zhang Z, Yan L, Zhang J, Hu D (2006) Gray matter density reduction in the insula in fire survivors with posttraumatic stress disorder: a voxel-based morphometric study. Psychiatry Res 146:65–72
Kasai K, Yamasue H, Gilbertson MW, Shenton ME, Rauch SL, Pitman RK (2008) Evidence for acquired pregenual anterior cingulate gray matter loss from a twin study of combat-related posttraumatic stress disorder. Biol Psychiatry 63:550–556
Nardo D, Högberg G, Looi JC, Larsson S, Hällström T, Pagani M (2010) Gray matter density in limbic and paralimbic cortices is associated with trauma load and EMDR outcome in PTSD patients. J Psychiatr Res 44:477–485
De Bellis MD, Keshavan NS, Shifflett H, Iyengar S, Beers SR, Hall J, Moritz G (2002) Brain structures in pediatric maltreatment-related posttraumatic stress disorder: a sociodemographically matched study. Biol Psychiatry 52:1066–1078
Carrion VG, Weems CF, Eliez S, Patwardhan A, Brown W, Ray RD, Reiss AL (2002) Attenuation of frontal asymmetry in pediatric posttraumatic stress disorder. Biol Psychiatry 50:943–951
Fennema-Notestine C, Stein MB, Kennedy CM, Archibald SL, Jernigan TL (2002) Brain morphometry in female victims of intimate partner violence with and without posttraumatic stress disorder. Biol Psychiatry 52:1089–1101
Geuze E, Westwenberg HGM, Heinecke A, de Kloet CS, Goebel R, Vermetten E (2008) Thinner prefrontal cortex in veterans with posttraumatic stress disorder. Neuroimage 41:675–681
Bossini L, Tavanti M, Calossi S, Lombardelli A, Polizzotto NR, Galli R, Vatti G, Pieraccini F, Castrogiovanni P (2008) Magnetic resonance imaging volumes of the hippocampus in drug-naïve patients with post-traumatic stress disorder without comorbidity conditions. J Psychiatr Res 42:752–762
Woodward SH, Schaer M, Kaloupek DG, Cediel L, Eliez S (2009) Smaller global and regional cortical volume in combat-related posttraumatic stress disorder. Arch Gen Psychiatry 66:1373–1382
Smith SM, Zhang Y, Jenkinson M, Chen J, Matthews PM, Federico A, De Stefano N (2002) Accurate, robust, and automated longitudinal and cross-sectional brain change analysis. Neuroimage 17:479–489
Ashburner J, Friston JK (2000) Voxel-based morphometry—the methods. Neuroimage 11:805–821
Honea R, Crow TJ, Passingham D, Mackay CE (2005) Regional deficits in brain volume in schizophrenia: a meta-analysis of voxel-based morphometry studies. Am J Psychiatry 162:2233–2245
De Stefano N, Battaglini M, Smith SM (2007) Measuring brain atrophy in multiple sclerosis. J Neuroimaging 17(Suppl 1):10S–15S
First MB, Spitzer RL, Gibbon M, Williams JB (1995) Structured clinical interview for Axis I DSM IV disorders, Non-patient edition (SCID-I/NP, version 2.0). Biometrics Research Department, New York State Psychiatric Institute, New York
Blake DD, Weathers FW, Nagy LM, Kaloupek DG, Gusman FD, Charney DS, Keane TM (1995) The development of a Clinician-Administered PTSD Scale. J Trauma Stress 8:75–90
First MB, Spitzer RL, Gibbon M, Williams JB (1996) Structured clinical interview for Axis I DSM-IV disorders-patient Edition (SCID-I/P, version 2.0). Biometrics Research Department, New York State Psychiatric Institute, New York
First MB, Spitzer RL, Gibbon M, Williams JB (1994) Structured clinical interview for axis II DSM IV disorders (SCID-II/P). Biometrics Research Department, New York State Psychiatric Institute, New York
Hamilton M (1960) A rating scale for depression. J Neurol Neurosurg Psychiatry 23:56–62
Hamilton M (1959) The assessment of anxiety states by rating. Br J Med Psychol 32:50–55
De Stefano N, Matthews PM, Filippi M, Agosta F, De Luca M et al (2003) Evidence of early cortical atrophy in MS. Neurology 60:1157–1162
Mazziotta J, Toga A, Evans A, Fox P, Lancaster J, Zilles K, Woods R, Paus T, Simpson G, Pike B, Holmes C, Collins L, Thompson P, MacDonald D, Iacoboni M, Schormann T, Amunts K, Palomero-Gallagher N, Geyer S, Parsons L, Narr K, Kabani N, Le Goualher G, Boomsms D, Cannon T, Kawashima R, Mazoyer B (2001) A probabilistic atlas and reference system for the human brain: International Consortium for Brain Mapping (ICBM). Philos Trans R Soc Lond B Biol Sci 356:1293–1322
Battaglini M, Smith SM, Brogi S, De Stefano N (2008) Enhanced brain extraction improves the accuracy of brain atrophy estimation. NeuroImage 40:583–589
Battaglini M, Giorgio A, Stromillo ML, Bartolozzi ML, Guidi L et al (2009) Voxel-wise assessment of progression of regional brain atrophy in relapsing–remitting multiple sclerosis. J Neurol Sci 282:55–60
Zhang Y, Brady M, Smith S (2001) Segmentation of brain MR images through a hidden Markov random field model and the expectation maximization algorithm. IEEE Trans Med Imaging 20:45–57
Rueckert D, Sonoda LI, Hayes C, Hill DLG, Leach MO, Hawkes DJ (1999) Non-rigid registration using free-form deformations: Application to breast MR images. IEEE Trans Med Imaging 18:712–721
Good C, Johnsrude I, Ashburner J, Henson R, Friston K, Frackowiak R (2001) A voxel-based morphometric study of ageing in 465 normal adult human brains. Neuroimage 14:21–36
Shapiro SS, Wilk MB (1965) An analysis of variance test for normality (complete samples). Biometrika 52:591–611
Levene H (1960) Robust tests for equality of variances. In: Olkin I, Ghurye SG, Hoeffding W, Madow WG, Mann HB (eds) Contributions to probability and statistics: essays in honor of Harold Hotelling. Stanford University Press, California, pp 278–292
Nichols TE, Holmes AP (2002) Nonparametric permutation tests for functional neuroimaging: a primer with examples. Hum Brain Mapp 15:1–25
Smith SM, Jenkinson M, Woolrich MW, Beckmann CF, Behrens TEJ, Johansen-Berg H, Bannister PR, De Luca M, Drobnjak I, Flitney DE, Niazy RK, Saunders J, Vickers J, Zhang Y, De Stefano N, Brady JM, Matthews PM (2004) Advances in functional and structural MR image analysis and implementation as FSL. Neuroimage 23:208–219
Kessler RC, Berglund P, Demler O, Jin R, Merikangas KR, Walters EE (2005) Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the national comorbidity survey replication. Am Med Assoc 62:593–602
Kessler RC, Chiu WT, Demler O, Walters EE (2005) Prevalence, severity and comorbidity of 12-month DSM-IV disorders in the national comorbidity survey replication. Am Med Assoc 62:617–627
Bremner JD (2007) Functional neuroimaging in post-traumatic stress disorder. Expert Rev Neurother 7:393–405
Nutt DJ, Malizia AL (2004) Structural and functional brain imaging in posttraumatic stress disorder. J Clin Psychiatry 65:11–17
Nemeroff CB, Bremner JD, Foa EB, Mayberg HS, North CS, Stein MB (2006) Posttraumatic stress disorder: a state-of-the-science review. J Psychiatr Res 40:1–21
Bremner JD, Vythilingam M, Vermetten E, Vaccarino V, Charney DS (2004) Deficits in hippocampal and anterior cingulate functioning during verbal declarative memory encoding in midlife major depression. Am J Psychiatry 161:637–645
Shin LM, Wright CI, Cannistraro PA, Wedig MM, McMullin K, Martis B, Mackiln ML, Lasko NB, Cavanagh SR, Krangel TS, Orr SP, Pitman RK, Whalen PJ, Rauch SL (2005) A functional magnetic resonance imaging study of amygdala and medial prefrontal cortex responses to overtly presented fearful faces in posttraumatic stress disorder. Arch Gen Psychiatry 62:273–281
Geuze E, Westenberg HG, Jochims A, de Kloet CS, Bohus M, Vermetten E, Schmahl C (2007) Altered pain processing in veterans with posttraumatic stress disorder. Arch Gen Psychiatry 64:76–85
Geuze E, Vermetten E, Ruf M, de Kloet CS, Westenberg HG (2008) Neural correlates of associative learning and memory in veterans with posttraumatic stress disorder. J Psychiatr Res 42:659–669
Phelps EA, Delgado MR, Nearing KI, LeDoux JE (2004) Extinction learning in humans: role of the amygdala and vmPFC. Neuron 43:897–905
Amaral DG, Price JL, Pitkanen A, Carmichael ST (1992) Anatomical organization of the primate amygdaloid complex. The amygdala neurobiological aspects of emotion. Memory and mental dysfunction. In: Aggleton W (ed) 1992. Wiley, New York, pp 1–66
Lanius RA, Bluhm R, Pain C (2006) A review of neuroimaging studies in PTSD: heterogeneity of response to symptom provocation. J Psichiatr Res 40:709–729
Hendler T, Rotshtein P, Yeshurun Y, Weizmann T, Kahn I, Ben-Bashat D, Malach R, Bleich A (2003) Sensing the invisible: differential sensitivity of visual cortex and amygdala to traumatic context. Neuroimage 19:587–600
Francati V, Vermetten E, Bremner JD (2007) Functional neuroimaging studies in posttraumatic stress disorder: review of current methods and findings. Depress Anxiety 24:202–218
Lindauer RJ, Booij J, Habraken JB, Uyling HB, Olff M et al (2004) Cerebral blood flow changes during script-driven imagery in police officers with posttraumatic stress disorder. Biol Psychiatry 56:853–861
Yamasue H, Kasai K, Iwanami A, Ohtani T, Yamada H, Abe O, Kuroki N, Fukuda R, Tochigi M, Furukawa S, Sadamatsu M, Sasaki T, Aoki S, Ohtomo K, Asukai N, Kato N (2003) Voxel-based analysis of MRI reveals anterior cingulated gray-matter volume reduction in posttraumatic stress disorder due to terrorism. Proc Natl Acad Sci USA 100:9039–9043
Abe O, Yamuse H, Kasai K, Yamada H, Aoki S, Iwanami A, Ohtani T, Masutani Y, Kato N, Ohtomo K (2006) Voxel-based diffusion tensor analysis reveals aberrant anterior cingulum integrity in posttraumatic stress disorder due to terrorism. Psychiatry Res 146:231–242
McEwen BS (2008) Central effects of stress hormones in health and disease: understanding the protective and damaging effects of stress and stress mediators. Eur J Pharmacol 583:174–185
Yehuda R, Flory JD (2007) Differentiating biological correlates of risk, PTSD, and resilience following trauma exposure. J Trauma Stress 20:435–447
Frangou S, Chitins X, Williams SCR (2004) Mapping IQ and gray matter density in healthy young people. Neuroimage 23:800–805
Lange N, Froimowitz MP, Bigler ED, Lainhart JE et al (2010) Brain Development Cooperative Group. Associations between IQ, total and regional brain volumes, and demography in a large normative sample of healthy children and adolescents. Dev Neuropsychol 35:296–317
McEwen BS (2000) The neurobiology of stress: from serendipity to clinical relevance. Brain Res 886:172–189
Zhang H, Ozbay F, Lappalainen J, Kranzler HR, van Dyck CH, Charney DS, Price LH, Southwick S, Yang BZ, Rasmussen A, Gelernter J (2006) Brain derived neurotrophic factor (BDNF) gene variants and Alzheimer’s disease, affective disorders, posttraumatic stress disorder, schizophrenia, and substance dependence. Am J Med Genet B Neuropsychiatr Genet 141B:387–393
Beng-Choon H, Nancy CA, Jeffrey DD, Thomas HW (2007) Association between brain-derived neurotrophic factor Val66Met gene polymorphism and progressive brain volume changes in schizophrenia. Am J Psychiatry 164:1890–1899
Acknowledgments
The authors wish to thank all the subjects for their participation in the study. Institutional funds of the Department of Neuroscience, University of Siena.
Conflict of interest
All Authors have no biomedical financial or potential conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tavanti, M., Battaglini, M., Borgogni, F. et al. Evidence of diffuse damage in frontal and occipital cortex in the brain of patients with post-traumatic stress disorder. Neurol Sci 33, 59–68 (2012). https://doi.org/10.1007/s10072-011-0659-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-011-0659-4