Abstract
To assess the goals of gout treatment from a patient perspective, a convenience sample of consecutive patients with doctor-diagnosed gout seen at a community-based outpatient clinic were invited. Sex-stratified nominal groups were conducted until saturation was achieved. Responses were collected verbatim, discussed, and rank-ordered by each participant. Thirty-six patients with doctor-diagnosed gout participated in 12 nominal groups: 6 male only, 5 female only, and 1 group with both. Mean age was 61.9 years (SD, 12.3); mean gout duration was 13.3 years (SD, 12.5); 53% were men, 64% African-American, 42% retired, 47% currently married, 87% were using either allopurinol and/or febuxostat, and 40% had had no gout flares in the last 6 months. The top 5 treatment goals accounted for 91% of all votes and included the following: (1) prevent and better manage flare-ups and improve function (25%), (2) eliminate flare-ups/disease remission (30%), (3) diet and activity modification/lifestyle change (13%), (4) patient education and public awareness (12%), and (5) medication management and minimization of side effects (11%). When examining the top-rated concern for each nominal group, the first two goals were nominated by four groups each, diet/activity modification and medication management by 1 group each, and patient education by 3 groups. There were no differences evident by sex in top-ranked treatment goal. People with gout identified and rank-ordered treatment goals relevant to them. Providers of gout care need to be cognizant of these goals. Disease management concordant with these treatment goals might lead to a more satisfied, informed patient.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Gout is the most common inflammatory arthritis in adults in the USA that affects 8.3 million Americans [1]. Numerous quality gaps in the care of gout are evident and have been documented in various health care settings [2,3,4,5,6,7], despite the availability of effective treatments, many of which are inexpensive and well-tolerated. Despite this, the medication adherence for gout was the lowest among seven chronic conditions [8]. Thus, there is an unmet need for improving gout management.
The increasing incidence and prevalence of gout in recent decades is partly due to the changes in dietary habits and lifestyles, medical care improvements, and increased life expectancy [9,10,11,12,13]. The incidence of gout in adults was 0.2% [14], and the 5-year incidence of gout in the elderly was 4.4% [15]. The mainstay of the treatment of gout is long-term urate-lowering therapy (ULT), in addition to the use of anti-inflammatory drugs for the treatment of gout flares [16]. Allopurinol, a purine hypoxanthine analog, is the drug of choice for the treatment of major manifestations of chronic hyperuricemia with deposit of crystals of uric acid/urate in joints, subcutaneous tissues (tophi), or affecting the kidney (urate renal calculi) [16]. Febuxostat is a non-purine selective xanthine oxidase inhibitor and is used in people with gout who are intolerant to (due to, for instance, hypersensitivity) or inadequately controlled with allopurinol [16]. Allopurinol monotherapy is cost-saving, and allopurinol dose escalation or allopurinol-febuxostat sequential therapy is cost-effective [17].
Low disease activity or disease remission is a treatment goal for rheumatoid arthritis (RA) [18], a condition similar to gout. Since the recent development of the American College of Rheumatology/European League Against Rheumatism (ACR/EULAR) definition of RA remission [19], the experts recognized the importance of the patient perspective of disease control [20, 21]. This led to an international effort to develop and validate a RA remission definition incorporating the patient perspective, which is currently underway [22]. In contrast to RA, the development and validation of a definition for gout remission criteria is at an early stage [23].
To our knowledge, there are no published reports that describe the patient’s perspective of important and meaningful goals of gout treatment. A better understanding of the patient perspective of treatment goals can make patient-physician discussion about treatment adherence more effective during a clinic visit, and also contribute to the development of the definition of disease remission and low disease activity in gout. Recently, the American College of Physicians (ACP) gout treatment guideline introduced a new concept of “treat-to-symptom” approach in gout [24], and did not endorse the “treat-to-target” (target being serum urate < 6 mg/dl, that is associated with improved gout outcomes, and is easy to monitor) approach, which has been recommended in the gout treatment guideline from the ACR and the other rheumatology societies worldwide. Interestingly, patient’s priorities regarding gout treatment goals are largely unknown. This is a major knowledge gap.
Our primary objective was to perform formative work to understand and define gout treatment goals from a patient perspective, using the nominal group technique (NGT). A secondary objective is to explore whether gout treatment goals differed by patient’s sex, since gout disease perception and/or disease experience may differ by sex.
Methods
Study sample
The study team invited consecutive patients with at least one visit to the community-based clinic at the University of Alabama at Birmingham (UAB) from January 2016 to August 2017 for gout for study participation, based on the presence of an International Classification of Diseases, ninth revision, common modification (ICD-9-CM) code, 274 for gout, a valid approach [4]. Each participant confirmed doctor-diagnosed gout before starting the nominal group discussion. African-Americans and women with gout were oversampled, since these groups are often under-represented in gout studies. Each participant was provided with free parking, refreshments during the session, and a $30 check for study participation. The Institutional Review Board (IRB) at the University of Alabama at Birmingham approved the study.
Nominal group technique (NGT) and analyses
The NGT has been used successfully in several medical conditions [25,26,27,28,29,30,31] and also in gout [32, 33]; details of the NGT methodology have been previously provided [32, 33]. The NGT, a variant of traditional focus group, allows an in-depth understanding of participant views and facilitates representation of the implicit views of the group, in response to a single question. NGT taps the experiences, skills, and views of the participants and promotes an even participation of all participants. An inclusive list of issues related to a specific question is developed, followed by soliciting participant feedback on the relative importance of this list using a rank-ordering or voting procedure [28, 34].
Sex-stratified patient nominal group sessions were conducted to understand patient perspective on gout treatment goals and to explore potential differences by patient sex. Each nominal group session was led by an experienced NGT moderator (J.A.S.) [32, 33] and lasted 1–1.5 h. Each participant gave brief introductions after providing informed consent. Each participant was provided with two study questions printed on top of two separate blank sheets of paper, which were also written on a two flipcharts: “Q1: Should doctors treat your gout as a chronic disease or just treat its symptoms as they occur?’ and “Q2: What should be the goals of gout treatment?” The first question was answered by a simple choice between disease and symptomatic treatment. Chronic disease was described akin to diabetes, hypertension, chronic lung disease, or coronary artery disease. Symptomatic treatment was described akin to symptoms that can occur or recur without an underlying chronic disease, i.e., nausea, loss of appetite, and lack of energy, For the second question, study participants independently generated as many word or short phrases as possible in response to the question on a sheet of paper. The NGT moderator (J.A.S.) collected each participant response in a round-robin fashion, and recorded it verbatim on a flip chart. Participants discussed and elaborated each response and combined responses similar to each other, where appropriate. All participants scored three top responses deemed the most important from 1 to 3 on index cards, 3 being the highest score. A rank order was created for each nominal group based on total score for each statement/theme, with the highest score corresponding to the top rank. The top-ranked and the top 3 ranked concepts/themes from each nominal group were examined, stratified by sex.
All discussions were recorded and transcribed verbatim (D.F.). The transcriptions were examined to identify discussion related to each response, which led to the creation of a comprehensive list of statements. Responses were compared to determine overlap and confirm theme saturation.
Data availability statement
We are ready to share the data with colleagues, after obtaining appropriate permissions from the University of Alabama at Birmingham (UAB) Ethics Committee, related to HIPAA and privacy policies.
Results
Study participant characteristics
Twelve nominal groups with 36 patients with gout were conducted, and theme saturation was achieved. Six male only nominal groups, five female only nominal groups, and one nominal group with both males and females were conducted. The mean age was 61.9 years (standard deviation, 12.3), and mean duration of gout was 13.3 years (standard deviation, 12.5) (Table 1). Of these, 53% were men, 64% were African-American, 42% were retired, and 47% were currently married (Table 1). Seventy-six percent of participants were using allopurinol (with/without colchicine, NSAIDs, or prednisone), and 14% were using febuxostat. Fifty-six percent were using one or more natural supplements for gout, with cherry extract or cherry juice being the most common supplement. Forty percent of participants had had no gout flares in the last 6 months, and 14% reported six or more gout flares in the last 6 months.
Gout: to treat as a disease or just symptomatically?
Ninety-five percent participants (34/36) wanted gout to be treated as a chronic disease, and 5% wanted it to be treated only symptomatically. Supplementary File 1 shows the number of people from each nominal group who made this choice. Only in 2 of the 12 nominal groups, one patient each voted for gout to be treated only symptomatically.
Themes from the NGT
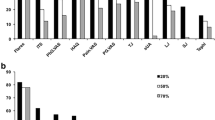
Nominal group participants brought up several ideas that mapped to nine key concepts, which are briefly described in the section below (Table 2). The nine top-voted themes are shown in Fig. 1 and listed in that order as follows. The top 5 themes (A to E) received 90% of the votes. Details of the key concepts/themes are provided in Supplementary File 2 that provides concept/themes followed by quotes.
-
A.
Prevent and better manage flare-ups and improve function: Four of the 12 nominal groups ranked this as their top concept/theme, and 8 of the 12 nominal groups ranked it among their top 3 concepts/themes. Several ideas mapped to this concept/theme, including the following: (1) prevent frequent gout flares by taking medications regularly, managing diet and other self-management actions; (2) prompt and effective treatment of gout flares and associated pain and joint swelling, using both pharmacologic and non-pharmacologic interventions; (3) shorten the duration of flares with the use of more effective medications; (4) allow return to normal activities, including self-care, recreational activities, sports, and the ability to work; and (5) allow participation in social activities with family and those in social settings including going to the church; and (6) availability of walking aids and special shoes for patients with gout.
-
B.
Eliminate flare-ups/remission: Four of the 12 nominal groups ranked this as their top concept, and 7 of the 12 nominal groups ranked it among their top 3 concepts. Participants wanted a total elimination of gout flares and indicated that elimination of flare-associated pain and functional limitation should be the goal. Some suggested a medication-free remission of gout, while others indicated disease remission on medication, preferably one medication. Participants wondered about the repair of bone/joint damage caused by gout. Some participants suggested that a gene therapy solution is needed for the cure of gout.
-
C.
Diet and activity modification/lifestyle change: One of the 12 nominal groups ranked this as their top concept, and 6 of the 12 nominal groups ranked it among their top 3 concepts. Several ideas mapped to this concept/theme as follows: (1) recognition that diet can contribute to flares; (2) set independent individualized goals for diet management with help from the healthcare provider team including a nutritionist; (3) identify the specific food to avoid and those to eat to avoid gout flares; (4) have activity and exercise goals specific for gout; (5) emphasize the role of obesity in gout and the importance of weight loss in reducing gout flares; (6) provide information on truths and myths of lifestyle and dietary changes needed for gout; and (7) advise about alcohol intake (type, amount, frequency) with regard to the risk of gout and gout flares. People were aware that eating fast food and low levels of activity was detrimental to gout. Participants realized that there was a lot of information about these aspects of gout management and they did not know what to trust and what not to. They preferred that their health care teams direct them to expert resources and provide this information directly to them, and that an “inter-disciplinary, multi-method” approach is needed to make this work. Only some patients had received such information to their satisfaction. This theme led to active discussion among the nominal group participants.
-
D.
Patient education and public awareness: Three of the 12 nominal groups ranked this as their top concept, and 5 of the 12 nominal groups ranked it among their top 3 concepts. Participants indicated that they needed reliable and trustworthy information about the following by the healthcare teams and/or resources (online, pamphlet, write down questions for nurse/doctor) that they are directed to (1) gout and its cause; (2) role of diet and exercise in gout management; (3) weight loss, obesity, and the risk of gout flares; and (4) importance of regular intake of gout medications in preventing flares. A variety of preferred settings including study groups, classes, and one-on-one and group sessions were suggested. Patients also expressed interest in having additional resources at hand such as support groups, smartphone “apps,” and online resources, vetted by the health care team. A patient helpline was also suggested as an important resource for patients with gout. A major barrier for patients was a lack of awareness of the general public about gout and its impact on people. This led to their illness not being understood by the family and friends, unlike heart disease or diabetes that everyone knew about and understood. Participants wanted general public awareness campaigns about gout, with more advertisement on the TV, media, and other communication resources.
-
E.
Medication management and minimization of side effects: One of the 12 nominal groups ranked this as their top concept, and 5 of the 12 nominal groups ranked it among their top 3 concepts. Several ideas mapped to this concept/theme as follows: (1) knowledge and discussion of potential medication side effects including drug-drug interactions before starting treatment, (2) recommendation of individualized gout therapy, (3) availability of alternate choices when the current therapy stops working, (4) making medications such as colcrys more affordable for an average patient, and (5) minimization of side effects of gout medications, by increasing the tolerability of the current medications and discovering less toxic alternative medications.
-
F.
Lowering the serum urate/uric acid: None of the 12 nominal groups ranked this as their top concept, and 3 of the 12 nominal groups ranked it among their top 3 concepts. Participants indicated that knowledge and monitoring of their serum urate/uric acid levels, which they were aware is the causative for joint manifestations of gout, would help reinforce the need for long-term treatment, as well as lifestyle choices. One suggestion was monthly laboratory monitoring. Participants wondered about an at-home urate test using either serum or urine, that they could use to get real-time feedback regarding lifestyle changes and their effects, as well as titrating their medication. Participants in these three groups understood the central role of serum urate in gout, and the need to keep the level below 6 or 5 mg/dl to avoid gout flares and continuing damage.
-
G.
Need for additional healthcare services: None of the 12 nominal groups ranked this as their top concept, and 2 of the 12 nominal groups ranked it among their top 3 concepts. Several ideas mapped to this concept/theme as follows: (1) need for family counseling services regarding the heritability of gout (i.e., next generation); (2) routine appointments for gout care; (3) get advice regarding gout via email, text, phone, linked through patient’s electronic health record; and (4) home health services to help treat and resolve acute flares at home, rather than with hospitalization.
-
H.
Address the emotional burden of flare-ups: None of the 12 nominal groups ranked this as their top concept, and 1 of the 12 nominal groups ranked it among their top 3 concepts. This issue was brought up by three nominal groups, but only received enough votes in one group. Participants indicated that the recognition and the treatment of the emotional burden of gout are important parts of gout management and treatment goals. They highlighted that minimization of the stress caused by flares should be a priority, preferably with a non-pharmacological intervention, by having an open dialog, and recognizing that gout flare is associated with one of the most severe pain episode most gout patients have, which often starts in the middle of the night.
-
I.
Comorbidity management: None of the 12 nominal groups ranked this as their top concept, and 1 of the 12 nominal groups ranked it among their top 3 concepts. Participants wondered if cardiovascular comorbidity is associated with gout, and whether gout treatment could lead to an extra-articular benefit, for example with their heart problems.
Sex differences in priority
No observable differences in ranking of themes by sex were noted, since similar themes were ranked highly by male vs. female only nominal groups. For the three top-ranked themes, an equal number of male vs. female groups ranked them as the top theme (Table 2).
Discussion
In this formative study with sex-stratified groups (except one), we used the NGT to understand the patient perspective of the goals of gout therapy. Patients ranked the themes, and a saturation of themes was achieved. Several treatment goals emerged that highlight the need for a multi-faceted approach to the health care of patients with gout. To my knowledge, this is among the first studies to elicit the patient goals of gout therapy. Several findings deserve further discussion.
Ninety-six percent patients considered gout to be chronic disease and preferred that gout should be treated as a chronic disease, rather than intermittently only symptomatically. This view is in contrast to the recent American College of Physicians (ACP) gout treatment guideline that proposed that ULT titration in patients with gout should be based on a treat-to-symptom approach rather than treat-to-target approach [24]. Undoubtedly, gout is a chronic disease associated with synovitis, bony erosions with intermittent flares, and chronic inflammation [35], where inflammation and crystal formation continue in periods between flares [36, 37], more often in gout patients not treated with ULT [38]. Treatment with ULT is associated with lowering of serum urate and total body urate burden that leads to a reduced frequency of gout attacks [39] and finally to the disappearance of urate crystals from synovial fluid in the asymptomatic gouty joints [40]. Additionally, studies have found ULT in gout to be cost-effective [38, 41]. Notably, ULT is cost-saving in people with gout, who have frequent attacks [42] or use allopurinol monotherapy [38], which is an uncommon/rare finding in chronic disease management, and therefore quite impressive. Thus, gout is similar to chronic conditions such as chronic obstructive pulmonary disease (COPD) and heart failure (HF) in that the disease course, disease symptoms, and outcomes including end-organ damage (joint damage due to gout) can vary from person to person. Therefore, based on pathology and evidence from studies, long-term management of gout with suppression of the underlying disease process, i.e., hyperuricemia, urate crystal formation, and chronic inflammation, is needed. This is what patients expect of the health care teams as well, according to our study.
It was clear that patients recognized gout as a chronic disease as a group. Despite this recognition, the top patient goals for gout treatment pertained to the reduction of gout flares and associated impact on patient’s function (as discussed below). This may reflect that health providers may be failing to explain the benefits of the gout treatment, i.e., prevention of joint damage and associated long-term irreversible disability, and the reduction of chronic systemic inflammation, with potential cardiovascular benefits, as have been shown in people with cardiovascular disease even without chronic inflammatory diseases [43]. Another possibility is that patients lack the knowledge of the serum urate goal or its importance [44] or may rank gout flares higher than long-term joint damage based on their experience of flares, while most were not aware of long-term joint damage.
Two treatment goals for gout tied for the top rank: (1) a reduction of gout flares and pain and improvement of flare-associated activity limitation and (2) elimination of gout flares completely or complete remission; both were the top voted theme in 4 out of 12 nominal groups each. These goals emphasize the importance of flare reduction or elimination and of disease remission to patients with gout. In qualitative studies, the effect of gout flare on daily life and severe pain were cited among the top concerns in several patient populations [32, 45,46,47]. Thus, our results extend the previous findings and are consistent with them. Severe gout with more flares was associated with poor health-related QOL and disability [48], and the use of pegloticase, a ULT, led to clinically important improvements in pain, function, and HRQOL [49]. An important part of these goals was the concept of gout remission and gout low disease activity that patients desired. A validated definition of gout remission for gout clinical trials is currently being developed [23]. It seems that a validated remission definition will also be relevant to patients.
Interestingly, lowering of serum urate was not selected as a top therapy goal by any of the 12 nominal groups. This is not surprising and is consistent with the lack of adequate patient knowledge of the central pathophysiologic mechanism in gout. High serum urate correlates with frequent gout flares [39], which was the most frequently chosen top goal of gout therapy. This implied that control of gout flares was patient’s top priority goal; however, the knowledge that this is achieved by optimal lowering of serum urate is mostly lacking among patients.
Patient education was ranked by three nominal groups as their top theme. A recent UK proof-of-concept study showed that patient education, when delivered comprehensively as a part of healthcare team-delivered program, can not only make gout patients more informed but also improve gout outcomes [50]. Our patient participants demanded reliable and trustworthy information vetted by the healthcare teams on several topics including the cause of gout; the role of obesity, diet, exercise, and weight loss in gout management; factors that increase or decrease the risk of gout flares; and reasons for adherence to urate-lowering therapy (ULT) and other gout medications, i.e., preventing flares or joint damage. They suggested various potential resources including pamphlets, reviewing questions with nurse/doctor, online resources, patient support groups, a gout helpline, etc. The use of current smart technology was also discussed as an opportunity for patient education. Participants indicated that most of them received little, if any gout education and had a high level of enthusiasm for participation in such activities. Patient education is a key recommendation in various gout treatment guidelines [51, 52]. Current patient education resources (information sheets, booklets, or webpages) available for gout have a wide range of readability, but were missing key messages about target serum urate and prophylaxis against flares [53]. Therefore, more comprehensive patient education materials for gout are needed, and should be provided in multiple settings and formats. Several groups discussed whether gout education was a goal for gout treatment or a process which helped patients achieve the main treatment goal, such as fewer flares, normal function, or feeling better or normal. This might explain why other themes related to flares and associated disability were chosen as top themes more often by patients.
One may debate the optimal content of patient education materials. According to the ACR/EULAR guidelines [51, 52], in addition to the treatment of acute flares, patient education materials would emphasize an adequate lowering of serum urate below 6 mg/dl as a key message, which can be achieved with regular use of adequately dosed ULT. This is based on its association with fewer gout flares, less cost, less productivity loss, and potentially less radiographic joint destruction. If education materials were based on the recent ACP guideline [24], treatment of gout flares and a treat-to-symptom approach rather than treat to target (no specification of which symptoms) would be emphasized; additionally, ULT would not be prescribed to all patients with recurrent gout attacks, but rather ULT risks, benefits, costs, and preferences will be discussed with the patient. These are two vastly different messages, and the healthcare providers must agree on the message, rather than confusing patients further, who demonstrate knowledge gaps about the treatment of gout. This study demonstrates that patients can define their knowledge needs to better understand what leads to gout which can then help them manage their gout with a better approach than the current approach, which is fragmented and confused at best. It is not only the patients who are confused about gout. The recent guideline debate shows that a large proportion of providers also have gross misperceptions about the chronicity of gout and the impact of associated chronic systemic and local inflammation on joints (leading to short- and long-term disability) and other vital organs (heart, kidneys, brain) as well.
Our study has an important message for gout trialists as well. Inclusion of gout flares and its impact should be considered a primary or secondary outcome in all trials of gout, not only those addressing treatment of flares. A validated definition of gout flares for clinical trials is available, which is easy to impliment, highly feasible, and incorporates patient input [54, 55]. Routine inclusion of flare assessment in most/all gout clinical trials can provide invaluable information about this patient-important outcome from gout trials, as in the ongoing allopurinol vs. febuxostat trial [56].
Medication management was a top theme in one nominal group, and 5 of the 12 nominal groups ranked it among their top 3 concepts. In a previous study, 60% of the nominal groups reported that medication-related issues negatively impacted their QOL [32]. Patients are often worried about medication side effects, potential side effects and have challenges taking their medications regularly, or taking them long-term/lifelong. We were encouraged that patients wanted to see this as a top treatment goal, which indicates their willingness and desire to be more adherent to their treatment regimen.
Our findings must be interpreted considering study limitations. We used a convenience sample from a community-based clinic. Our findings are only generalizable to patients with gout who are seeking health care at community and hospital clinics. We did not obtain the information, whether primary gout care was being provided by rheumatologist or another specialist of primary care provider. However, since we did not limit patient sample to a particular clinic, this sample represents all-comers to a community-based clinic. Since we performed sex-stratified nominal groups, we needed a larger number of nominal groups (n = 12) to achieve theme saturation within each sex. Theme saturation can sometimes be achieved with a smaller number of groups. A large proportion of study participants were on ULT (87%), which is higher proportion than that reported in previous gout studies, which indicates limited generalizability to people with low ULT prescription rates. However, many patients were not taking their ULT regularly, which makes them somewhat similar to other gout cohorts. Study findings need to be reproduced in other geographic and country settings. While we collected patient reported data on a limited set of demographic and clinical characteristics, we did not perform a detailed clinical examination for this formative study in accordance with ethics approval. Therefore, data on tophi, metabolic syndrome, and quality of life were not available. We did not perform age-stratified nominal groups (only sex-stratified); therefore, we were unable to determine whether goals of gout treatment may potentially differ by age. Future studies can examine this important issue. A future study that separates people with vs. without dietary restrictions or high vs. low medication adherence may provide additional insights, regarding goals of gout therapy.
Our study strengths were that we included African-Americans and women with gout that are typically under-represented in single- or multi-center gout studies. Therefore, findings are generalizable to most patients with gout, in the USA [1], although our cohort may have had a higher education level. Our study had a higher proportion of African-Americans with gout, as per the study design. We chose to include more African-Americans with gout, since this subgroup of patients is more difficult to recruit in clinical studies in the USA and therefore under-represented, not only in clinical studies of gout, but in clinical studies in general. We focused on a single question and achieved saturation of themes.
In conclusion, in nominal groups consisting of Caucasian and African-American men and women with gout, we assessed patient’s goals of the treatment of gout. The top treatment goals were the reduction/elimination of gout flares (and associated pain and functional limitation), disease remission, patient education, and medication management. These goals indicated the preferences of people with gout. These data must be carefully considered by the clinicians as they move forward with defining important outcomes for clinical care of gout, and perhaps even clinical trials in gout.
Abbreviations
- NGT:
-
Nominal group technique
- UAB:
-
University of Alabama at Birmingham
- ULT:
-
Urate-lowering therapy
References
Zhu Y, Pandya BJ, Choi HK (2011) Prevalence of gout and hyperuricemia in the US general population: the National Health and nutrition examination survey 2007-2008. Arthritis Rheum 63:3136–3141
Singh JA (2009) Quality of life and quality of care for patients with gout. Curr Rheumatol Rep 11:154–160
Singh JA, Hodges JS, Asch SM (2009) Opportunities for improving medication use and monitoring in gout. Ann Rheum Dis 68:1265–1270
Singh JA, Hodges JS, Toscano JP, Asch SM (2007) Quality of care for gout in the US needs improvement. Arthritis Rheum 57:822–829
Mikuls TR, Farrar JT, Bilker WB, Fernandes S, Saag KG (2005) Suboptimal physician adherence to quality indicators for the management of gout and asymptomatic hyperuricaemia: results from the UK General Practice Research Database (GPRD). Rheumatology (Oxford) 44:1038–1042
Sarawate CA, Brewer KK, Yang W, Patel PA, Schumacher HR, Saag KG, Bakst AW (2006) Gout medication treatment patterns and adherence to standards of care from a managed care perspective. Mayo Clin Proc 81:925–934
Edwards NL (2011) Quality of care in patients with gout: why is management suboptimal and what can be done about it? Curr Rheumatol Rep 13:154–159
Briesacher BA, Andrade SE, Fouayzi H, Chan KA (2008) Comparison of drug adherence rates among patients with seven different medical conditions. Pharmacotherapy 28:437–443
Kuo CF, Grainge MJ, Zhang W, Doherty M (2015) Global epidemiology of gout: prevalence, incidence and risk factors. Nat Rev Rheumatol 11:649–662
Brook RA, Forsythe A, Smeeding JE, Lawrence EN (2010) Chronic gout: epidemiology, disease progression, treatment and disease burden. Curr Med Res Opin 26:2813–2821
Choi HK (2005) Diet, alcohol, and gout: how do we advise patients given recent developments? Curr Rheumatol Rep 7:220–226
Choi HK (2010) A prescription for lifestyle change in patients with hyperuricemia and gout. Curr Opin Rheumatol 22:165–172
Roddy E, Choi HK (2014) Epidemiology of gout. Rheum Dis Clin N Am 40:155–175
Dehlin M, Drivelegka P, Sigurdardottir V, Svard A, Jacobsson LT (2016) Incidence and prevalence of gout in Western Sweden. Arthritis Res Ther 18:164
Hanly JG, Skedgel C, Sketris I, Cooke C, Linehan T, Thompson K et al (2009) Gout in the elderly—a population health study. J Rheumatol 36:822–830
Neogi T (2011) Clinical practice. Gout N Engl J Med 364:443–452
Jutkowitz E, Choi HK, Pizzi LT, Kuntz KM (2014) Cost-effectiveness of allopurinol and febuxostat for the management of gout. Ann Intern Med 161:617–626
Anderson J, Caplan L, Yazdany J, Robbins ML, Neogi T, Michaud K, Saag KG, O'dell JR, Kazi S (2012) Rheumatoid arthritis disease activity measures: American College of Rheumatology recommendations for use in clinical practice. Arthritis Care Res (Hoboken) 64:640–647
Felson DT, Smolen JS, Wells G, Zhang B, van Tuyl LH, Funovits J, Aletaha D, Allaart CF, Bathon J, Bombardieri S, Brooks P, Brown A, Matucci-Cerinic M, Choi H, Combe B, de Wit M, Dougados M, Emery P, Furst D, Gomez-Reino J, Hawker G, Keystone E, Khanna D, Kirwan J, Kvien TK, Landewé R, Listing J, Michaud K, Martin-Mola E, Montie P, Pincus T, Richards P, Siegel JN, Simon LS, Sokka T, Strand V, Tugwell P, Tyndall A, van der Heijde D, Verstappen S, White B, Wolfe F, Zink A, Boers M, American College of Rheumatology, European League Against Rheumatism (2011) American College of Rheumatology/European league against rheumatism provisional definition of remission in rheumatoid arthritis for clinical trials. Arthritis Rheum 63:573–586
van Tuyl LH, Hewlett S, Sadlonova M, Davis B, Flurey C, Hoogland W et al (2015) The patient perspective on remission in rheumatoid arthritis: ‘You've got limits, but you're back to being you again’. Ann Rheum Dis 74:1004–1010
van Tuyl LHD, Boers M (2017) Rheumatoid arthritis: remission—keeping the patient experience front and Centre. Nat Rev Rheumatol 13:573–574
Rasch LA, Boers M, Hill CL, Voshaar M, Hoogland W, de Wit M, Flurey C, Davis B, Hetland ML, Brahe CH, Gossec L, Wells GA, Tugwell P, Kuriya B, Goel N, Singh JA, Duarte C, da Silva J, van Schaardenburg D, Proudman S, van Tuyl L, Working Group on the Patients’ Perspective on Remission in Rheumatoid Arthritis (2017) Validating rheumatoid arthritis remission using the Patients' perspective: results from a special interest group at OMERACT 2016. J Rheumatol 44:1889–1893
de Lautour H, Taylor WJ, Adebajo A, Alten R, Burgos-Vargas R, Chapman P, Cimmino MA, da Rocha Castelar Pinheiro G, Day R, Harrold LR, Helliwell P, Janssen M, Kerr G, Kavanaugh A, Khanna D, Khanna PP, Lin C, Louthrenoo W, McCarthy G, Vazquez-Mellado J, Mikuls TR, Neogi T, Ogdie A, Perez-Ruiz F, Schlesinger N, Ralph Schumacher H, Scirè CA, Singh JA, Sivera F, Slot O, Stamp LK, Tausche AK, Terkeltaub R, Uhlig T, van de Laar M, White D, Yamanaka H, Zeng X, Dalbeth N (2016) Development of preliminary remission criteria for gout using Delphi and 1000Minds consensus exercises. Arthritis Care Res (Hoboken) 68:667–672
Qaseem A, Harris RP, Forciea MA, Clinical Guidelines Committee of the American College of P (2017) Management of acute and recurrent gout: a clinical practice guideline from the American College of Physicians. Ann Intern Med 166:58–68
Jefferson WK, Zunker C, Feucht JC, Fitzpatrick SL, Greene LF, Shewchuk RM, Baskin ML, Walton NW, Phillips B, Ard JD (2010) Use of the nominal group technique (NGT) to understand the perceptions of the healthiness of foods associated with African Americans. Eval Program Plann 33:343–348
Kleiner-Fisman G, Gryfe P, Naglie G (2013) A patient-based needs assessment for living well with Parkinson disease: implementation via nominal group technique. Parkinsons Dis 2013:974964
MacLachlan M (1996) Identifying problems in community health promotion: an illustration of the nominal group technique in AIDS education. J R Soc Health 116:143–148
Miller D, Shewchuk R, Elliot TR, Richards S (2000) Nominal group technique: a process for identifying diabetes self-care issues among patients and caregivers. Diabetes Educ 26:305–10 12, 14
Pastrana T, Radbruch L, Nauck F, Hover G, Fegg M, Pestinger M et al (2010) Outcome indicators in palliative care—how to assess quality and success. Focus group and nominal group technique in Germany. Support Care Cancer 18:859–868
Pena A, Estrada CA, Soniat D, Taylor B, Burton M (2012) Nominal group technique: a brainstorming tool for identifying areas to improve pain management in hospitalized patients. J Hosp Med 7:416–420
Redman S, Carrick S, Cockburn J, Hirst S (1997) Consulting about priorities for the NHMRC National Breast Cancer Centre: how good is the nominal group technique. Aust N Z J Public Health 21:250–256
Singh JA (2014) The impact of gout on patient's lives: a study of African-American and Caucasian men and women with gout. Arthritis Res Ther 16:R132
Singh JA (2014) Facilitators and barriers to adherence to urate-lowering therapy in African-Americans with gout: a qualitative study. Arthritis Res Ther 16:R82
Gallagher M, Hares T, Spencer J, Bradshaw C, Webb I (1993) The nominal group technique: a research tool for general practice? Fam Pract 10:76–81
Cavalcanti NG, Marques CD, Lins ELTU, Pereira MC, Rego MJ, Duarte AL et al (2016) Cytokine profile in gout: inflammation driven by IL-6 and IL-18? Immunol Investig 45:383–395
Bomalaski JS, Lluberas G, Schumacher HR Jr (1986) Monosodium urate crystals in the knee joints of patients with asymptomatic nontophaceous gout. Arthritis Rheum 29:1480–1484
Pascual E (1991) Persistence of monosodium urate crystals and low-grade inflammation in the synovial fluid of patients with untreated gout. Arthritis Rheum 34:141–145
Pascual E, Batlle-Gualda E, Martinez A, Rosas J, Vela P (1999) Synovial fluid analysis for diagnosis of intercritical gout. Ann Intern Med 131:756–759
Shoji A, Yamanaka H, Kamatani N (2004) A retrospective study of the relationship between serum urate level and recurrent attacks of gouty arthritis: evidence for reduction of recurrent gouty arthritis with antihyperuricemic therapy. Arthritis Rheum 51:321–325
Pascual E, Sivera F (2007) Time required for disappearance of urate crystals from synovial fluid after successful hypouricaemic treatment relates to the duration of gout. Ann Rheum Dis 66:1056–1058
Beard SM, von Scheele BG, Nuki G, Pearson IV (2014) Cost-effectiveness of febuxostat in chronic gout. Eur J Health Econ 15:453–63
Ferraz MB, O'Brien B (1995) A cost effectiveness analysis of urate lowering drugs in nontophaceous recurrent gouty arthritis. J Rheumatol 22:908–914
Ridker PM, Everett BM, Thuren T, MacFadyen JG, Chang WH, Ballantyne C, Fonseca F, Nicolau J, Koenig W, Anker SD, Kastelein JJP, Cornel JH, Pais P, Pella D, Genest J, Cifkova R, Lorenzatti A, Forster T, Kobalava Z, Vida-Simiti L, Flather M, Shimokawa H, Ogawa H, Dellborg M, Rossi PRF, Troquay RPT, Libby P, Glynn RJ, CANTOS Trial Group (2017) Antiinflammatory therapy with Canakinumab for atherosclerotic disease. N Engl J Med 377:1119–1131
Coburn BW, Bendlin KA, Sayles H, Hentzen KS, Hrdy MM, Mikuls TR (2016) Target serum urate: do gout patients know their goal? Arthritis Care Res (Hoboken) 68:1028–1035
Harrold LR, Mazor KM, Velten S, Ockene IS, Yood RA (2010) Patients and providers view gout differently: a qualitative study. Chronic Illn 6:263–271
Lindsay K, Gow P, Vanderpyl J, Logo P, Dalbeth N (2011) The experience and impact of living with gout: a study of men with chronic gout using a qualitative grounded theory approach. J Clin Rheumatol 17:1–6
Spencer K, Carr A, Doherty M (2012) Patient and provider barriers to effective management of gout in general practice: a qualitative study. Ann Rheum Dis 71:1490–1495
Becker MA, Schumacher HR, Benjamin KL, Gorevic P, Greenwald M, Fessel J et al (2009) Quality of life and disability in patients with treatment-failure gout. J Rheumatol 36:1041–1048
Strand V, Khanna D, Singh JA, Forsythe A, Edwards NL (2012) Improved health-related quality of life and physical function in patients with refractory chronic gout following treatment with pegloticase: evidence from phase III randomized controlled trials. J Rheumatol 39:1450–1457
Rees F, Jenkins W, Doherty M (2013) Patients with gout adhere to curative treatment if informed appropriately: proof-of-concept observational study. Ann Rheum Dis 72:826–830
Zhang W, Doherty M, Pascual E, Bardin T, Barskova V, Conaghan P, Gerster J, Jacobs J, Leeb B, Lioté F, McCarthy G, Netter P, Nuki G, Perez-Ruiz F, Pignone A, Pimentão J, Punzi L, Roddy E, Uhlig T, Zimmermann-Gòrska I, EULAR Standing Committee for International Clinical Studies Including Therapeutics (2006) EULAR evidence based recommendations for gout. Part I: diagnosis. Report of a task force of the standing Committee for International Clinical Studies Including Therapeutics (ESCISIT). Ann Rheum Dis 65:1301–1311
Khanna D, Fitzgerald JD, Khanna PP, Bae S, Singh MK, Neogi T, Pillinger MH, Merill J, Lee S, Prakash S, Kaldas M, Gogia M, Perez-Ruiz F, Taylor W, Lioté F, Choi H, Singh JA, Dalbeth N, Kaplan S, Niyyar V, Jones D, Yarows SA, Roessler B, Kerr G, King C, Levy G, Furst DE, Edwards NL, Mandell B, Schumacher HR, Robbins M, Wenger N, Terkeltaub R, American College of Rheumatology (2012) 2012 American College of Rheumatology guidelines for management of gout. Part 1: systematic nonpharmacologic and pharmacologic therapeutic approaches to hyperuricemia. Arthritis Care Res (Hoboken) 64:1431–1446
Robinson PC, Schumacher HR Jr (2013) A qualitative and quantitative analysis of the characteristics of gout patient education resources. Clin Rheumatol 32:771–778
Gaffo AL, Dalbeth N, Saag KG, Singh JA, Rahn EJ, Mudano AS, Chen YH, Lin CT, Bourke S, Louthrenoo W, Vazquez-Mellado J, Hernández-Llinas H, Neogi T, Vargas-Santos AB, da Rocha Castelar-Pinheiro G, Amorim RBC, Uhlig T, Hammer HB, Eliseev M, Perez-Ruiz F, Cavagna L, McCarthy GM, Stamp LK, Gerritsen M, Fana V, Sivera F, Taylor W (2018) Brief report: validation of a definition of flare in patients with established gout. Arthritis Rheumatol 70:462–467
Gaffo AL, Schumacher HR, Saag KG, Taylor WJ, Dinnella J, Outman R, Chen L, Dalbeth N, Sivera F, Vázquez-Mellado J, Chou CT, Zeng X, Perez-Ruiz F, Kowalski SC, Goldenstein-Schainberg C, Chen L, Bardin T, Singh JA (2012) Developing a provisional definition of flare in patients with established gout. Arthritis Rheum 64:1508–1517
NIH (2016) Gout: Allopurinol vs. Febuxostat. https://clinicaltrials.gov/ct2/show/record/NCT02579096. Bethesda, Maryland: Clinicaltrials.gov. A service of the U.S. National Institutes of Health
Acknowledgements
I am thankful to study team members, who assisted with various study administrative tasks: UAB student Sara Chirambo (S.C.) for her help in scheduling the patients and data entry; research assistant, Candace Green (C.G.), BS for scheduling the patients and providing administrative oversight and support for conducting the nominal groups; and administrative assistant, Diana Florence (D.F.) for transcribing the nominal group discussion. I thank several colleagues and patients who provided informal input into drafting the question for the nominal groups.
Funding
This material is the result of work supported by research funds from the Division of Rheumatology at the University of Alabama at Birmingham and the resources and use of facilities at the Birmingham VA Medical Center, Birmingham, Alabama, USA. The funding body did not play any role in design, in the collection, analysis, and interpretation of data; in the writing of the manuscript; and in the decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Contributions
JAS designed the study, developed the protocol, conducted the nominal sessions, analyzed the data, wrote the first draft of the manuscript and revised it, and made the decision to submit it.
Corresponding author
Ethics declarations
Conflict of interest
JAS has received research grants from Takeda and Savient pharmaceuticals and consultant fees from Savient, Takeda, Regeneron, Merz, Iroko, Bioiberica, Crealta/Horizon and Allergan pharmaceuticals, WebMD, UBM LLC, Medscape, Fidia pharmaceuticals, and the American College of Rheumatology. JAS serves as the principal investigator for an investigator-initiated study funded by Horizon pharmaceuticals through a grant to DINORA, Inc., a 501 (c) (3) entity. JAS is a member of the executive of OMERACT, an organization that develops outcome measures in rheumatology and receives arms-length funding from 36 companies; a member of the American College of Rheumatology’s (ACR) Annual Meeting Planning Committee (AMPC); Chair of the ACR Meet-the-Professor, Workshop and Study Group Subcommittee; and a member of the Veterans Affairs Rheumatology Field Advisory Committee. JAS is the editor and Director of the UAB Cochrane Musculoskeletal Group Satellite Center on Network Meta-analysis.
Ethics/IRB approval and consent to participate
The University of Alabama at Birmingham’s Institutional Review Board approved this study (X120404005), and all investigations were conducted in conformity with ethical principles of research. All patients involved in the study including consent to participate in the study.
Rights and permissions
About this article
Cite this article
Singh, J.A. Goals of gout treatment: a patient perspective. Clin Rheumatol 37, 2557–2566 (2018). https://doi.org/10.1007/s10067-018-4243-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-018-4243-7