Abstract
Purpose
The aim of this study was to evaluate using quilting sutures in a prospective randomized controlled manner the decrease in the incidence of seroma formation among patients subjected to ventral hernia repair.
Methods
The study was a prospective randomized controlled study. 370 patients with large ventral hernias were randomly distributed among two groups. Group A (control group) included 180 patients in whom the repair was done without quilting sutures. Group B (quilting group) included 190 patients, all performed with quilting. Method of dissection was unified as far as possible. All cases had an attached closed suction drain that was removed after two successive days of output ≤ 50 cc. The output of the suction drain was recorded; accumulation of clinically detected seroma after 1, 2 and 4 weeks of removal of the drain was monitored.
Results
There was no statistical difference between both groups as regards the demographic data and the hernia characteristics. There was significantly smaller amount of output of the drains in every day of the first five postoperative days as well as the total amount of the output before drain removal in favor of the quilting group. Drains were removed earlier in group B. The incidence of clinically detected seroma was less in group B as well.
Conclusions
Quilting sutures is an effective and easy technique to reduce post-ventral hernia seroma accumulation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Among the most common surgical interventions is ventral hernia repair, which involves dissecting skin and subcutaneous tissue from the underlying sheath and muscle in an amount that varies depending on the hernia’s size and the state of the abdominal wall musculature. A common complication of ventral hernia repair is seroma formation, which surgical drains can reduce but cannot prevent [1].
The amount of seroma formed is directly proportionate to the surface area dissected [2]. Small seromas can be managed conservatively, whereas large ones may require multiple aspirations with subsequent risk of introducing infection that can be highly hazardous in the presence of synthetic mesh [1, 2]. Decreasing or obliterating the dead space created during hernia repair has long been considered a means to reduce seroma formation. Methods used to that end include inserting drains, injecting sclerosing material, using external compression, quilting sutures, or employing a combination of these procedures [3,4,5,6,7,8]. The concept of quilting sutures has effectively reduced seroma formation following other surgeries involving flap dissection with subsequent creation of dead space (e.g. latissimus dorsi flap harvesting) [9].
Aim
The aim of our prospective randomized controlled trial was to assess the effectiveness of quilting sutures in decreasing seroma accumulation in a large sample of patients subjected to ventral hernia repair, some of whom underwent abdominoplasty.
Patients
The study included 370 patients treated for ventral hernias, including paraumbilical hernias and incisional hernias, from February 2015 to January 2018 in the Surgical Oncology Unit and Plastic Surgery Unit within the Faculty of Medicine at Alexandria University. All participants were candidates for elective hernioplasty or abdominoplasty involving mesh fixation and had dissected flaps more than 15 cm × 15 cm (> 225 cm2) in area, determined easily by the size of the mesh. To reduce the presence of other factors with possible role in seroma formation, the sample excluded patients with diabetes, with BMIs equal to or greater than 30, or who required emergency treatment.
Methods
The required approvals from the Ethics Committee at Alexandria University were obtained. Each participant signed an informed written consent form before enrolling in the study. We randomly distributed participants into two groups according to the closed envelope technique, which blinded them as to which group they represented.
Group A, ultimately consisting of 180 participants, received an intervention involving the standard technique without quilting, whereas group B, with 190 participants, received quilting sutures to reduce seroma formation.
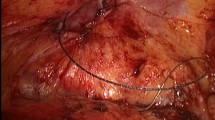
All cases were done by “onlay” mesh repair, which generally entails dissecting the skin and subcutaneous tissues to expose the anterior rectus sheath and external oblique (Fig. 1). All interventions were performed by one of the contributing surgeons, using the same technique of flap dissection involving electrocoagulation with a combination of coagulation and cutting. Once the hernial sac was dissected and excised, the contents were reduced. Partial omentectomy was performed in some cases. No case indicated a need for bowel resection. Closure of the hernia defect involved using nonabsorbable sutures. Cases of abdominal wall weakness or divaricated recti (e.g., rectus muscle diastasis) required keel repair to reinforce the abdominal wall.
Consequently, a combined polyglecaprone and polypropylene mesh “ULTRAPRO®” was fixed by interrupted 2/0 non-absorbable “polypropylene” sutures. Cases involving abdominoplasty also entailed the excision of redundant skin and subcutaneous fat. Liposuction was not used in any of the cases.
After the surgeon inserted a closed negative suction 14F drain into each participant, interventions by group diverged. Whereas participants in group A experienced the closure of subcutaneous tissue and skin, participants in group B experienced the obliteration of dead space. This was performed by application of multiple interrupted absorbable sutures between the subcutaneous tissue on one side and the underlying sheath and fixed mesh on the other side at a distance between the quilting sutures of 5–7 cm (Fig. 2). Thereafter, the surgeon closed the subcutaneous tissue and skin of participants in group B following the same method used in group A.
We monitored participants in both groups to assess the amount of daily drain output, the timing of drain removal, and the clinical detection of seromas 1, 2, and 4 weeks after removal. The attached drain was removed when the output was ≤ 50 cc for 2 days. We managed cases of seroma accumulation with frequent aspirations. Aspirated fluid was sent to culture and microbiological examination only if turbid and/or if infection was suspected.
Following surgery, we advised each participant to wear an abdominal binder for 6 weeks, reduce vigorous activity, and avoid straining factors.
Statistical analysis
Data analysis involved the use of the Statistical Package for the Social Sciences version 20.0 (IBM, Armonk, NY, USA). Qualitative data included number counts and percentages, whereas quantitative data included ranges (i.e., minimum to maximum), means and standard deviations, and medians. We set significance to 5%. Tests used included a Chi-square test to compare categorical variables between the groups, Student’s t test to compare normally distributed quantitative variables between the groups, and Mann–Whitney U test to compare abnormally distributed quantitative variables between the groups.
Results
Table 1 presents the characteristics of the sample. Factors that might have contributed to seroma formation, including BMI, smoking, the use of steroids, and the use of oral anticoagulants, made no statistically significant difference. Next, Table 2 presents the characteristics of hernias treated and their repair. Neither table indicates a statistically significant difference between groups A and B except regarding the type of hernia repaired. In particular, group A comprised mostly cases of de novo hernias (n = 95, 52.8%)—that is, paraumbilical hernias and epigastric hernias with or without divarication of the recti muscles—whereas group B had only 57 such cases (30%, p < .001) but a significant number of incisional (p = .044) and recurrent hernias (p = .002). Among other possible sources of difference, group A represented more cases of abdominoplasty than group B, although the difference was not significant nor was the between-group difference in the incidence of complications other than seromas (Table 2).
Seroma-related factors compared between group A and group B included daily monitoring of the output in drains or their removal during the first 5 days (i.e., whichever occurred first), the total amount of drain output before removal, the timing of removal, and the clinical detection of seromas 1, 2, and 4 weeks following removal (Table 3). During the first 5 days, when many participants were candidates for drain removal, group B not only indicated significantly less daily output than group A (Fig. 3) but also significantly less drain output before removal as well. Unsurprisingly, in terms of the timing of drain removal, group B also had an earlier median time of removal (4.2 ± 1.1 days) than group A (7.6 ± 1.6 days). Although group B additionally exhibited more seromas 1, 2, and 4 weeks after drain removal than group A, the difference was statistically significant only after a week.
Discussion
Often occurring after hernioplasty for ventral hernias, seromas contain fluid of mostly serum, liquefied fat, and lymphatic fluid [10]. Although the etiology of seromas remains poorly understood, many factors clearly contribute to their occurrence, including the patient’s body size (i.e., BMI) and comorbidities, the technique of dissection, field hemostasis, tissue handling, hernia size, and the surgeon’s volume [1, 10].
Other factors include the surface area of dissected flaps and potential dead space created as a result. This is possibly due to more tissue injury or the disruption of minor lymphatics given the enlarged area of dissection, which increases the accumulation of liquefied fat, serum, and fluid [1, 2, 10].
To assess seroma accumulation, we performed clinical examinations but did not use radiology. Because ultrasound is highly sensitive to seroma accumulation, with a diagnostic yield of more than 90%, such subclinical seromas are liable to increase the incidence of unnecessary interventions (i.e., aspirations) and, in turn, the risk of infection [11]. Alternatively, factors suggesting seroma were the presence of abnormal bulging over the dissected area, fluid thrill, patient discomfort, stretched skin, and/or sense of skin tension.
Following surgery, we advised each participant to wear an abdominal binder during daily activity for the first 6 weeks to alleviate pain and enhance ambulation. Another advantage of abdominal binders is their capacity to reduce seroma formation and recurrence [12]. Worth mentioning here is that we instructed participants to not wear binders tightly—just fitting—given their possible role in reducing lung function and increasing the risk of DVT [12].
We sought to unify the mode of dissection using diathermy, which combined the cutting mode (i.e., dissection and elevation of flaps) and the coagulation mode (i.e., for hemostasis), to not influence seroma formation due to the use of different methods of flap elevation [13, 14]. Although other authors have described how dissection on a subfascial plane (i.e., superficial to the scrape’s fascia) can decrease seroma formation by minimizing the major lymph trunk injury [15], this was not the standard technique adopted by us [15].
Pollock and Pollock retrospectively reviewed the use of “progressive tension sutures” in nearly 600 cases of abdominoplasty and ultimately advised against using surgical drains in cases of abdominoplasty, even if liposuction was performed [16, 17]. Antonetti and Antonetti [18] made a similar suggestion following their large retrospective study of more than 500 abdominoplasties.
In their prospective study with 21 female patients indicated for abdominoplasty and quilting sutures, Nahas et al. attached drains only for the first 48 h post-surgery and used ultrasound to detect the occurrence of seroma. Ultimately, they also recommended using quilting sutures to decrease seroma formation [19], as have Khan et al. and Baroudi and Ferreira in other similar studies [20,21,22].
One of the few prospective randomized trials was that done by Andrades et al. on 60 female patients divided into 4 equal groups [23]. They indicated no significant difference in the incidence of seroma formation between quilted groups without drains, the non-quilted group with drains attached, and the quilted group with drains attached.
Other researchers have examined the use of sclerosing or sealant material to decrease the incidence of seroma accumulation after ventral hernia repair with encouraging results [24,25,26,27]. Other studies combined the use of a sealant material together with the quilting for preventing seroma after latissimus dorsi flap dissection with good results [28]. On the other hand, a comparative study by Bercial et al. reported a higher incidence of seroma in the sealant group than in the quilted group [29]. Yet, the commercial availability, as well as the cost of the sealant material, is to be questioned at my institution (same issue raised by Azoury et al.) [30].
Conclusions
The results of our prospective randomized controlled trial with a relatively large group of patients safely suggest using quilting sutures, an unsophisticated technique requiring no special materials or supplementary tools, during ventral hernia repair.
References
Shermak MA, Rotellini-Coltvet LA, Chang D (2008) Seroma development following body contouring surgery for massive weight loss: patient risk factors and treatment strategies. Plast Reconstr Surg 122(1):280–288
Dayton MT (2004) Surgical complications. In: Townsend CM, Beauchamp RD, Evers BM, Mattox KL (eds) Sabiston textbook of surgery: the biological basis of modern surgical practice, 17th edn. Saunders, Philadelphia, pp 297–332
Lehr SC, Schuricht AL (2001) A minimally invasive approach for treating postoperative seromas after incisional hernia repair. J Soc Laparoendosc Surg 5(3):267–271
Morales-Conde S (2012) A new classification for seroma after laparoscopic ventral hernia repair. Hernia 16(3):261–267
Janis JE, Khansa L, Khansa I (2016) Strategies for postoperative seroma prevention: a systematic review. Plast Reconstr Surg 138(1):240–252
Klima DA, Belyansky I, Tsirline VB, Lincourt AE, Lipford EH, Getz SB et al (2012) Application of subcutaneous talc after axillary dissection in a porcine model safely reduces drain duration and prevents seromas. J Am Coll Surg 214(3):338–347
Berkoff DJ, Kanaan M, Kamath G (2013) Fibrin glue as a non-invasive outpatient treatment for post-arthroscopic knee seromas. Knee Surg Sports Traumatol Arthrosc 21(8):1922–1924
Moritz RK, Reich-Schupke S, Altmeyer P, Stucker M (2013) Polidocanol foam sclerotherapy of persisting postoperative seromas after varicose vein surgery: a series of six cases. Phlebology 28(7):341–346
Rossetto LA, Garcia EB, Abla LE, Ferreira LM (2014) Seroma and quilting suture at the donor site of the TRAM flap in breast reconstruction: a prospective randomized double-blind clinical trial. Ann Plast Surg 72(4):391–397
Read RC, Yoder G (1989) Recent trends in the management of incisional herniation. Arch Surg 124(4):485–488
Smereczynski A, Starzynska T, Kolaczyk K, Kladny J (2014) Role of sonography in assessing complications after laparoscopic cholecystectomy. J Ultrason 14(57):152–162
Hall AB, Northern D (2012) Effect of abdominal binders on pulmonary mechanics with implications for the military surgical population. J Surg Educ 69(1):34–36
Valenca-Filipe R, Martins A, Silva A, Vasconez LO, Amarante J, Costa-Ferreira A (2015) Dissection technique for abdominoplasty: a prospective study on scalpel versus diathermocoagulation (coagulation mode). Plast Reconstr Surg Glob Open 3(1):e299
Marsh DJ, Fox A, Grobbelaar AO, Chana JS (2015) Abdominoplasty and seroma: a prospective randomised study comparing scalpel and handheld electrocautery dissection. J Plast Reconstr Aesthet Surg 68(2):192–196
Le Louarn C (1996) Partial subfascial abdominoplasty. Aesthet Plast Surg 20(2):123–127
Pollock H, Pollock T (2000) Progressive tension sutures: a technique to reduce local complications in abdominoplasty. Plast Reconstr Surg 105(7):2583–2586 (discussion 7–8)
Pollock TA, Pollock H (2012) Progressive tension sutures in abdominoplasty: a review of 597 consecutive cases. Aesthet Surg J 32(6):729–742
Antonetti JW, Antonetti AR (2010) Reducing seroma in outpatient abdominoplasty: analysis of 516 consecutive cases. Aesthet Surg J 30(3):418–425
Nahas FX, Ferreira LM, Ghelfond C (2007) Does quilting suture prevent seroma in abdominoplasty? Plast Reconstr Surg 119(3):1060–1064 (discussion 5–6)
Baroudi R, Ferreira CA (1996) Contouring the hip and the abdomen. Clin Plast Surg 23(4):551–572 (discussion 72–73)
Baroudi R, Ferreira CA (1998) Seroma: how to avoid it and how to treat it. Aesthet Surg J 18(6):439–441
Khan S, Teotia SS, Mullis WF, Jacobs WE, Beasley ME, Smith KL et al (2006) Do progressive tension sutures really decrease complications in abdominoplasty? Ann Plast Surg 56(1):14–20 (discussion—1)
Andrades P, Prado A, Danilla S, Guerra C, Benitez S, Sepulveda S et al (2007) Progressive tension sutures in the prevention of post abdominoplasty seroma: a prospective, randomized, double-blind clinical trial. Plast Reconstr Surg 120(4):935–946 (discussion 47–51)
Toman N, Buschmann A, Muehlberger T (2007) Fibrin glue and seroma formation following abdominoplasty. Chirurg 78(6):531–535
Chevrel JP (1979) The treatment of large midline incisional hernias by “overcoat” plasty and prothesis (author’s transl). Nouv Presse Med 8(9):695–696
Lee JC, Teitelbaum J, Shajan JK, Naram A, Chao J (2012) The effect of fibrin sealant on the prevention of seroma formation after postbariatric abdominoplasty. Can J Plast Surg 20(3):178–180
Kohler G, Koch OO, Antoniou SA, Lechner M, Mayer F, Emmanuel K (2014) Prevention of subcutaneous seroma formation in open ventral hernia repair using a new low-thrombin fibrin sealant. World J Surg 38(11):2797–2803
Bailey SH, Oni G, Guevara R, Wong C, Saint-Cyr M (2012) Latissimus dorsi donor-site morbidity: the combination of quilting and fibrin sealant reduce length of drain placement and seroma rate. Ann Plast Surg 68(6):555–558
Bercial ME, Sabino Neto M, Calil JA, Rossetto LA, Ferreira LM (2012) Suction drains, quilting sutures, and fibrin sealant in the prevention of seroma formation in abdominoplasty: which is the best strategy? Aesthet Plast Surg 36(2):370–373
Azoury SC, Rodriguez-Unda N, Soares KC, Hicks CW, Baltodano PA, Poruk KE et al (2015) The effect of TISSEEL fibrin sealant on seroma formation following complex abdominal wall hernia repair: a single institutional review and derived cost analysis. Hernia 19(6):935–942
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors of this manuscript certify that they have NO affiliations with or involvement in any organization or entity with any financial interest or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Ethical approval
This study was approved by the ethical committee of Faculty of Medicine, University of Alexandria.
Human and animal rights
The study including human participants has been performed in accordance with the ethical standards of the Declaration of Helsinki and its later amendments.
Informed consent
Informed written consent was signed and obtained from all individual patients before being enrolled in the study.
Rights and permissions
About this article
Cite this article
Alhussini, M.A., Awad, A.T. & Kholosy, H.M. Using quilting sutures in decreasing seroma formation after managing large ventral hernias: a comparative study. Hernia 23, 717–722 (2019). https://doi.org/10.1007/s10029-018-1850-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-018-1850-9