Abstract
Croissant de Garengeot’s hernia is defined as the presence of an appendix in the femoral hernial sac. It is rare and occurs mostly in females. We report this hernia in a male patient along with the surgical management and review of literature.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The de Garengeot’s hernia is a rare and incidental finding occurring in 0.9% of femoral hernia repairs [1], and appendicitis is rarer still, with an incidence of 0.08–0.13% [2–4]. Since first described by Rene Jacques Croissant de Garengeot, an 18th-century Parisian surgeon [5], de Garengeot’s hernia remains primarily an intra-operative diagnosis. To date there are 82 reported cases of appendicitis in a femoral hernia with a predisposition in women (13:1, 93% in women), probably in keeping with the increased incidence of femoral hernia in females. We report a case of gangrenous appendicitis within an incarcerated femoral hernia presenting in a male patient.
Case report
A previously fit 80-year-old man presented with a 24-h history of sudden onset of right groin pain and a lump. He remained haemodynamically stable, and on clinical examination his abdomen was soft with minimal tenderness over the right groin lump. Local examination of the right groin revealed a firm, tender, 3 × 4 cm irreducible lump. He did not have any bowel obstruction clinically or radiologically on the abdominal X-ray. His laboratory findings were within normal limits. Clinically he was diagnosed to have strangulated right inguinal hernia.
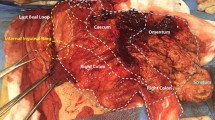
Considering the diagnosis of strangulated right inguinal hernia, open exploration via low inguinal approach was planned under general anaesthetic. Broad-spectrum antibiotic cover was provided at induction. Intra-operative findings were consistent with an inflamed and gangrenous appendix protruding through the femoral hernial sac (Fig. 1). The incision was extended laterally, and the external oblique, internal oblique and transversalis muscles were split, and the peritoneum exposed and incised to gain intra-peritoneal access. The caecum was identified, and the proximal end of the appendix was found to be engaged in the femoral ring. The appendix was reduced, and routine appendicectomy was performed. The femoral hernial sac was transfixed and excised intra-abdominally and the femoral defect was repaired using two interrupted prolene sutures between the inguinal and Cooper’s ligaments. Abdominal incision was closed in layers using absorbable sutures. The postoperative course was uneventful and the patient was discharged home on the second day after the procedure. The histological examination confirmed severely congested appendix with inflammatory changes consistent with acute appendicitis (Fig. 2a, b).
a Cut section of the distal appendix within the femoral hernial sac showing histological evidence of severe congestion in all layers of the appendix. There is fibrinoid necrosis of small vessels in the subserosal stromal tissues as well as mild inflammatory changes (×20 magnification). b Cut section of the appendix proximal to the neck of the hernia sac which was histologically normal (×20 magnification)
Discussion
Femoral hernias account for 4% of all groin hernias and have a higher incidence in post-menopausal women. A hernial sac can contain any of the intra-abdominal contents such as omentum, small bowel, colon, Meckel’s diverticulum or appendix. A pelvic appendix has the highest risk of entering a femoral hernial sac [6, 7]. In the largest series of herniation of appendix reported by Watson et al., out of 512 cases, 55% were inguinal and 40% were femoral hernia [8].
The evolution of inflammation in the appendix is thought to be secondary to its engagement in the hernial sac. The rigid femoral ring causes luminal obstruction resulting in congestion and ischemia distal to the site of constriction. This is followed by transmucosal inflammation and subsequent necrosis, perforation or abscess formation [9]. The rigid neck of the hernia may be responsible for limiting the intra-peritoneal spread of infection, minimising peritoneal irritation as was noted in this and previous cases of de Garengeot’s hernia [10, 11].
Although appendicitis in a hernia is mainly an intra-operative finding, CT and ultrasound have been successfully used for preoperative diagnosis [12–14]. A low-positioned caecum along with tubular structure within the hernial sac and stranding of nearby fat on CT have been reported to have 98% specificity and sensitivity for diagnosing or ruling out appendicitis within a hernial sac [15]. As this patient had a clinically strangulated hernia, further preoperative radiological refinement of the diagnosis would not have changed the decision to operate.
Alternative approaches such as Cooper’s ligament repair and a preperitoneal approach [6, 13] have been described in the literature, but the low inguinal approach adopted in this case provided adequate exposure for both the femoral canal exploration and intra-abdominal access. As the femoral hernial defect could be repaired with prolene sutures, this avoided a mesh in the presence of inflammation and infection.
Conclusions
The presence of appendicitis within a femoral hernia remains a rare and interesting diagnosis, particularly for a trainee surgeon, due to the lack of abdominal signs of appendicitis. Adhesion to the basic principles of management of a strangulated hernia though, still results in a timely diagnosis and appropriate management without incurring any delay for radiological imaging.
References
Wise L, Tanner N (1963) Strangulated femoral hernia appendix with perforated sigmoid diverticulitis. Proc R Soc Med 56:1105
Wakely CPG (1969) Hernia of the vermiform appendix. In: Maingot R (ed) Abdominal operations. Appleton-Century-Crofts, New York, p 1288
D’Alia C, Lo Schiavo MG, Tonante A et al (2003) Amyand’s hernia: case report and review of the literature. Hernia 7:89–91
Ryan WJ (1937) Hernia of the vermiform appendix. Ann Surg 105:135
Akopian G, Alexander M (2005) De Garengeot hernia: appendicitis within a femoral hernia. Am Surg 71:526–527
Carey LC (1967) Acute appendicitis occurring in hernias: a report of ten cases. Surgery 61:236–238
Guirguis EM, Taylor GA, Chadwick CDJ (1989) Femoral appendicitis: an unusual case. Can J Surg 32:380–381
Watson L (1924) Hernia. C. V. Mosby, St. Louis, p 527
Temple CL, Hunchcroft SA, Temple WJ (1995) The natural history of appendicitis in adults: a prospective study. Ann Surg 221:278–281
Nguyen ET, Komenaka IK (2004) Strangulated femoral hernia containing a perforated appendix. Can J Surg 47:68–69
D’ambrosio N, Katz D, Hines J (2006) Perforated appendix within a femoral hernia. AJR Am J Roentgeol 186:906–907
Bradley M, Morgan D, Pentlow B et al (2003) The groin hernia: an ultrasound diagnosis? Ann R Coll Surg Engl 85:178–180
Korenkov M, Paul A, Troidl H (1999) Color duplex sonography: diagnostic tool in the differentiation of inguinal hernias. J Ultrasound Med 18:565–568
Luchs JS, Halpern D, Katz DS (2000) Amyand’s hernia: prospective CT diagnosis. J Comput Assist Tomogr 24:884–886
Rao PM, Rhea JT, Novelline RA et al (1998) Effect of computed tomography of the appendix on treatment of patients and the use of hospital resources. N Eng J Med 338:141–146
Acknowledgments
Dr. J. Heald, FRCS (path), Department of Pathology, Huddersfield Royal Infirmary for providing the histological slides.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rajan, S.S., Girn, H.R.S. & Ainslie, W.G. Inflamed appendix in a femoral hernial sac: de Garengeot’s hernia. Hernia 13, 551–553 (2009). https://doi.org/10.1007/s10029-009-0472-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-009-0472-7