Abstract
This study presents the case of a patient with necrobiosis or necrosing fascitis of the inguinal region, secondary to a complicated Amyand’s hernia with a concomitant ipsilateral Richter’s hernia. The patient was treated with open trans-abdominal surgery and hernia repair through the pre-peritoneal approach, plus anti-microbians, and thrice-daily wound cleansing and dressings to the inguinal region. Evolution was satisfactory. There are no reports in the literature of a case such as this.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
An Amyand’s hernia is defined as an inguinal hernia where the vermiform appendix is also present in the hernial sac, and this may or may not be accompanied by an inflammatory process [1, 2]. The incidence of this type of hernia is less than 1%; and when there is accompanying acute appendicitis occurring in the hernial sac, the incidence drops to 0.13% [3, 4]. A Richter’s hernia is one where the antimesenteric surface of an intestinal loop is contained in the hernial sac, whether the hernia type is umbilical, inguinal, crural or even incisional. A Richter hernia classically contains an intestinal loop without causing mechanical intestinal occlusion [5, 6], but the hernia can sometimes become strangulated and lead to severe complications.
Although there are reports in the literature of an Amyand’s hernia and a Richter’s hernia occurring in isolates patients, what has not previously been published is the association of both an Amyand’s hernia and a Richter’s hernia occurring together within the same hernial sac. This article presents such a case, with the Amyand and Richter hernias both being found inside the one hernial sac, complicated in the case of our patient by an infectious process of the local region.
Clinical case
This 91-year-old female patient from a very low-income bracket, was seen at a rural hospital in Mexico depending of our hospital, complaining of a 9-day history of pain in the right inguinal region that had been increasing in intensity. On the second day she had developed associated aesthenia, adynamia and hyporexia, and on the fifth day an unquantified fever. She had also developed nausea, vomiting and a general worsening of his condition, together with a fetid odour, and this situation is what brought her to the hospital’s emergency department.
On admission, the patient was seen to be suffering from frank clinical malnutrition, and to be in poor physical condition overall. She had a blood pressure of 90/60 mm Hg, heart rate of 125 beats per minute, respiration rate of 35 per minute and a temperature of 101.3°F. The abdomen demonstrated guarding and generalized pain, but no frank indication of peritoneal irritation. There was, however, evident necrosis of the skin in the right inguinal region, with fetid fibrino-purulent membranes, erythema and oedema in the adjacent area, all accompanied by intense pain (Fig. 1).
Laboratory tests reported Hb 12.5 g/dl, haematocrit count 33%, leucocytosis 23,000 μl, neutrophilia 93%, and 6% band cells; glicemia of 124 g/dl, sodium 150 mEq/l, chloride 110 mEq/l and potassium 3.1 mEq/l.
Given the patient’s clinical condition, the decision was taken to intervene surgically to debride the necrotic tissue and clean the region. Because of the frank infection in the inguinal region, the abdominal cavity was opened through a median infra-umbilical line incision, clearly revealing that both the caecal appendix and terminal ileum were compromised.
Surgical revision began by freeing the ileum, which was found not to have any vascular compromise, and then appendectomy was performed, all without complication. Next, the deep inguinal orifice was repaired through the pre-peritoneal route, and the floor of the inguinal region was reinforced using N°1 Prolene sutures to unite the ileo-pubic tract to the conjoint area. The abdominal wound was then closed in layers, in the usual way.
Turning to the inguinal region, all the necrotic tissue was then debrided, removing skin, superficial fascia (Camper and Scarpa) and the aponeurosis of the major/greater oblique muscle and the round ligament (Fig. 2); finishing with a thorough lavage of the region. The inguinal wound was left open, to heal by itself.
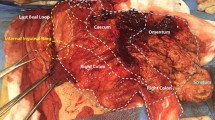
Trans-operative findings were necrosis of the soft tissue in the inguinal region with an indirect hernia of the caecal appendix in the hernial sac (Amyand’s hernia), the distal third of the appendix being necrosed, with perforation leading to seropurulent contents in the hernial sac and necrosis (Fig. 3). The same sac also contained the antimesenteric surface of the terminal ileum, but this was not necrosed (Fig. 4). Swabs of the purulent secretion were taken for culture, and the result on the third day was positive for Escherichia coli and Bacteroides fragilis.
Post-operative treatment consisted of an 8-day regime of intravenous antimicrobians, Cefotaxime 1 g every 8 h plus Clindamycin 600 mg every 6 h; wound cleansing thrice daily with soap and water, and the application of fresh gauze dressings; intravenous fluids; and analgesics.
Recovery was satisfactory. The patient began taking fluids by mouth on the second day, and was discharged from hospital on the tenth post-operative day. After 30 days, the inguinal wound was found to be clean, with granulating tissue developing (Fig. 5).
Discussion
The Amyand’s hernia owes its name to the British surgeon, Claudius Amyand (1680–1740), who in 1735 described the first case of perforated appendicitis in the sac of an inguinal hernia [1, 2]. The description of the caecal appendix appearing in the sac of a femoral hernia is attributed to the Parisian surgeon, Rene Jaques Croissant de Garengeot [7].
The Richter’s hernia, the antimesenteric surface of an intestinal loop being herniated but not necessarily in an inguinal hernia, owes its name to the German surgeon, August Gottlieb Richter (1742–1812). In 1785, he performed a revision of this type of hernia in the umbilicus, but also encountered hernias of the same type in the inguinal and femoral areas [5, 6].
As mentioned above, the Amyand’s hernia occurs in 1% of all hernias, and in 0.13% of hernias where associated acute appendicitis is also contained within the hernial sac [3, 4]. The Richter hernia is found in 5–15% of all strangulated hernias [5, 6]. The association of a hernia simultaneously containing both a perforated caecal appendix and the antimesenteric surface of an intestinal loop in the one sac, has not previously been reported.
The possible complication of the two types of hernia occurring together is the perforation of their contents, causing outflow of intestinal liquid into the inguinal region and secondary sepsis. The severity of the case described here was due to the delay in seeking medical help, because of the distance between the patient’s home in a remote rural area and the nearest hospital unit.
In our review of the available literature, we came across only one case of necrosis of the soft tissue secondary to an Amyand’s hernia, namely necrosing fascitis in part of the abdominal wall [8].
The clinical picture presented by our patient initially suggested a strangulated inguinal hernia with secondary necrosis to the structures in the inguinal region. This led to the decision to perform an exploratory laparotomy, in order to reduce the contents of the hernia with intestinal resection and anastomosis.
When an inguinal hernia is complicated by the strangulation of a loop of intestine, the surgical approach can be via the inguinal approach, with reduction and repair of the affected loop being conducted through the same incision [9, 10]. An alternative recommendation is via the pre-peritoneal approach [6, 11, 12]. A third option is open trans-abdominal surgery, which allows more detailed inspection of the condition of the intestinal loop involved, plus resection and anastomosis of the loop. This procedure can also be conducted laparoscopically.
In the case of our patient, the trans-abdominal approach was adopted because of the criteria mentioned above. Thus the contents of the hernial sac were clearly revealed, the suspected intestinal loop affected could be inspected closely, and there was unrestricted access for performing the necessary reconstruction. The surprise during operation was finding the type of hernia reported here.
In the event of the caecal appendix being found during inguinal hernia repair, even if the appendix is inflamed it is still possible to perform an appendectomy through the inguinal approach already opened [9, 10, 13] without any increase in morbidity.
However, in this instance the laparascopic approach was not possible; firstly because a laparoscope is not part of the standard equipment available at a rural hospital in Mexico, and secondly because hernia repair via the inguinal route could not even be considered given the septic and necrotic complications in the inguinal region that accompanied this case. The open abdominal approach adopted in this case allowed simultaneous treatment of all three conditions presented by our patient, namely: the Amyand’s hernia, the Richter’s hernia, and the inguinal hernia via the pre-peritoneal route. The infected conditions in the local region contra-indicated the use of a prosthetic mesh, added to the fact that rural hospitals in Mexico do not stock them anyway. Thus it was necessary to close the deep inguinal orifice and reinforce the floor of the inguinal region using the tension technique, via the pre-peritoneal route.
The regime of specific anti-microbian treatment combined with thrice daily cleansing and dressings to the inguinal wound, was sufficient to enable the patient to make a satisfactory recovery (Fig. 5).
Conclusion
Ipsilateral Amyand’s and Richter’s hernias in the same patient have not been reported previously, and the associated complication in this case of severe sepsis in the inguinal region required an integrated treatment that was both medical and surgical.
References
Hutchinson R (1993) Amyand’s hernia. J R Soc Med 86:104–105
Hiatt JR, Hiatt N (1988) Amyand’s hernia. N Engl J Med 318:1402
House MG, Goldin SB, Chen H (2001) Perforated Amyand’s hernia. South Med J 94:496–498
Gurer A, Ozdogan M, Ozlem N, Yildrim A, Kulacoglu H, Aydin R (2005) Uncommon content in groin hernia sac. Hernia 9:1–4
Tito WA, Allen WC (1989) Richter and Littre Hernia. In: Nyhus LM, Condon RE (eds) Hernia. J.B. Lippincott Company, Philadelphia, pp 305–310
Watkin D (2001) Groin hernia in the adult presenting as emergencies. In: Bendavid A (eds) Abdominal wall hernias principles and management. Springer, Berlin Heidelberg New York, pp 562–563
Akopian G, Alexander M (2005) De Garengeot hernia: appendicitis within a femoral hernia. Am Surg 71:526–527
Marron CD, Khadim M, McKay D, Mackle EJ, Peyton JW (2995) Amyand’s hernia causing necrotising fascitis of the anterior abdominal wall. Hernia 9:381–383
Kidmas AT, Iya D, Yilkudi MG, Nnadozie U (2004) Acute appendicitis in inguinal hernia: report of two cases. East Afr Med J 81:490–491
Breitenstein S, Eisenbach C, Wille G, Decurtins M (2005) Incarcerated vermiform appendix in a left-sided inguinal hernia. Hernia 9:100–102
Saggar VR, Singh K, Sarangi R (2004) Endoscopic total extraperitoneal management of Amyand’s hernia. Hernia 8:164–165
Logan MT, Nottingham JM (2001) Amyand’s hernia: a case report of an incarcerated and perforated appendix within an inguinal hernia and review of the literature. Am Surg 67:628–629
D’alia C, Lo Schiavo MG, Tonante A, Taranto F, Gagliano E, Bonanno L, Di Giuseppe G, Pagano D, Sturniolo G (2003) Amyand’s hernia: case report and review of the literature. Hernia 7:89–91
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Osorio, J.K., Guzmán-Valdivia, G. Ipsilateral Aymand’s and Richter’s hernia, complicated by necrosing fascitis. Hernia 10, 443–446 (2006). https://doi.org/10.1007/s10029-006-0120-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-006-0120-4