Abstract
Previous studies suggest a different regulation of the hypothalamus–pituitary–adrenal axis (HPA-axis) with lower diurnal cortisol levels, especially in the morning, in children with attention-deficit/hyperactivity disorder (ADHD) compared with controls. Since exposure to foetal and childhood psychosocial adversity has been associated with both ADHD and HPA-axis functioning, such exposures may explain these low cortisol levels in ADHD via early programming of the HPA-axis. Thus, our main aim was to retrospectively study foetal and early childhood exposures to psychosocial adversity in children with ADHD and to relate these exposures to cortisol levels. Saliva samples were collected during a regular weekday in children, 6–17 years old, with clinically confirmed ADHD (n = 197) and non-affected comparisons (n = 221) for radioimmunoassay analysis of cortisol. Parental rating scales were used for categorising subtypes of ADHD and degree of exposure to adversity. Children with ADHD had more reports of at least one rated foetal adversity (p = 0.041) and childhood adversity (p < 0.001) than comparisons. The association between low morning cortisol levels and ADHD-symptoms remained when analyses were adjusted for adversities, age, sex, sampling time and symptoms of oppositional defiant disorder. No relation was found between exposures to foetal/childhood adversity and cortisol levels except for a positive relation between childhood adversity and cortisol morning increase in children with ADHD. The hypothesis that early adversity may influence the HPA-axis, leading to lower cortisol levels in children with ADHD, was not supported by our findings.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Previous studies suggest a different regulation of the hypothalamus–pituitary–adrenal axis (HPA-axis) with lower diurnal cortisol levels in children with attention-deficit/hyperactivity disorder (ADHD) than in comparisons [1–3]. In a recent study, we found markedly lower cortisol levels in morning saliva samples in children with ADHD and slightly lower levels at bedtime [4]. The underlying mechanisms are not known. The general high heritability—especially in the morning—of cortisol levels [5] and the strong support for hereditary mechanisms underlying the development of ADHD [6, 7] suggest a genetic background. Since early adversity may constitute a risk factor for both ADHD [8] and dysregulation of the HPA-axis [9], a background of such exposures may be an alternative hypothesis to the HPA-dysfunction attributed to ADHD.
Foetal psychosocial adversity, often defined as maternal exposure to negative life events or maternal psychopathology, has in a number of studies been associated with subsequent emotional or cognitive problems in the child with ADHD-symptoms as a consistent adverse outcome [10–12]. Childhood psychosocial adversity—often defined as unfavourable family characteristics, socioeconomic disadvantage and parental psychopathology—has also been associated with ADHD-symptoms [6, 13]. Exposure to prenatal as well as early childhood psychosocial adversity has been associated mainly with HPA hyper-functioning in children [14–16]. However, different kinds of exposure to maltreatment seem to be associated with different cortisol regulation patterns [15, 17] and a down regulated HPA-axis with low diurnal cortisol levels has also been observed in association with early psychosocial adversity [17–21]. Furthermore, it has been argued that the observed alteration in cortisol levels observed early in life in the context of neglect and deprivation is not permanent [22].
The “programming theory” [12, 23, 24] is one of the most commonly proposed mechanisms that may explain how adverse exposures develop into behavioural symptoms. This theory means that exposure to a substantial amount and/or intensity of stressors during sensitive periods of development may lead to alterations in biological systems, which may in turn underlie deviating behaviour later in life. Particularly the brain regions involved in the regulation of the HPA-axis are susceptible to such environmental challenges [24, 25]. The HPA-axis is an important part of the neuroendocrine system. It has a number of effects, like mobilizing energy stores, potentiating the release of adrenaline, increasing cardiovascular tone, and inhibiting immune and inflammatory responses [23]. Animal studies have shown that maternal glucocorticoids cross the placenta, affecting foetal HPA development by modulations at the level of glucocorticoid receptors and mineralocorticoid receptors [26]. Such functional modulations may persist throughout life [26]. Also exposure to early childhood psychosocial adversity may affect the regulation of the HPA-axis. Animal studies have demonstrated that early exposure to substantial stressors may induce, e.g. attenuated development of glucocorticoid receptors and GABA-A receptors as well as changes in the structure of the brain [23], altered corticotrophin releasing factor (CRF) production and changed sensitivity of CRF receptors [27]. Teicher et al. [23] suggest that exposure to glucocorticoids exerts an organizing effect on the development, by facilitating subsequent adaptation to, e.g., deprivation or high levels of environmental stressors. Despite the quite extensive evidence from animal studies for HPA-axis programming theories, including behavioural consequences, human studies have not yet convincingly confirmed that similar processes are of importance also in humans [24, 25].
Thus, the main aim of this study was to retrospectively study foetal and early childhood exposures to psychosocial adversity in children with ADHD—also taking subgroup and sex into consideration—and to relate these exposures to cortisol levels. If exposure to psychosocial adversity explains or changes the strength of the relationship between ADHD-symptoms and cortisol levels it may shed light on the early programming theory in humans.
Methods
Subjects and procedure
Children/adolescents (6–17 years of age) of the ADHD group were recruited from four child psychiatry outpatient units in three Swedish counties. The ADHD-diagnosis refers to the last assessment by the clinically responsible child psychiatrist before inclusion in the study. The ADHD-diagnoses had been based on a clinical interview, a previous physical/neurological assessment and neuropsychological testing by a clinical psychologist (choice of tests adapted for the individual needs of the child and the degree of uncertainty about the diagnosis), as well as parental and teacher ratings (SNAP-IV). Written project information was presented at a regular examination or—in one county—by mail to the parents and to the child (an age-adapted version). After written informed consent from parents (and child when ≥15 years of age) questionnaires about psychosocial adversity, tubes for saliva samplings and instructions were mailed to the family. Clarifications were given by phone. Information about diagnosis/es and symptom ratings (Swanson, Nolan and Pelham ADHD symptom rating scale [SNAP-IV], see below) were collected from the medical record. All data were re-coded and all identifying information was destroyed, thereby implementing total anonymity. After exclusion of eight children reporting saliva sampling during a weekend or a holiday and exclusion of four children that lacked questionnaires on adversities, the ADHD group amounted to 197 children (148 boys and 49 girls; mean age: 11.9 years). The response rate was 35 %.
For the comparison group, children of the same ages and from schools in the same areas as the study persons were invited by mail or parental meetings, depending on the decision of the principal. In the written information, we clarified that children with verified or suspected ADHD should not participate. When the informed consent from parents (and child when ≥15 years of age) was returned, the following material was mailed to the family: questionnaires about psychosocial adversity, SNAP-IV, tubes for saliva sampling and sampling instructions. Clarifications were given by phone. The data were made anonymous as described above. After exclusion of three children reporting saliva sampling during a weekend or a holiday and seven children with indications of ADHD (six parental SNAP-IV items for any symptom cluster scored as “quite a bit” or “very much”) the comparison group amounted to 221 children. (92 boys and 129 girls; mean age: 11.9 years). The response rate was 30.5 %.
The study was approved by the Regional Ethical Review Board in Uppsala, no. 2009/034 and performed in accordance with the latest version of the Declaration of Helsinki. Informed consent of all participants was obtained after the nature of the procedures had been fully explained.
Questionnaires
Two questionnaires on adversities were administered to the parents, one concerning exposure to foetal psychosocial adversity (filled in by mothers) and one concerning psychosocial adversity during the first 6 years of life (filled in by any of the parents or both together). “Psychosocial Adversity” in this context means exposure to one or more negative life events.
The core of the items of the maternal questionnaire about foetal psychosocial adversity was the same as in a prospective study by Rosengren et al. [28]—reformulated to be used retrospectively—but the response alternatives (yes/no) were from a later adapted version of the same scale [29]. The 11 questions concern experiences during pregnancy of separation/divorce; relocation; change of employment; unemployment; insecurity at work; severe financial problems; legal sanctions; severe illness or accident (related to oneself or someone close); worries about someone close; death of someone close. The overall Cronbach’s Alpha in both groups was 0.62, specified in the ADHD group as 0.67 and in comparisons as 0.53.
The parental questionnaire about childhood psychosocial adversity during the first 6 years of life was based on general trauma items of The Early Trauma Inventory-Self Report (ETI-SR) Short Form [30]. This questionnaire has been confirmed to have good validity and reliability in another study on assessing childhood trauma in postpartum women [31]. The choice of using yes/no-items was made according to the author’s experiences with this scale [31]. Our original plan was to recruit patients during the—sometimes—critical referral phase (this approach was later changed due to practical obstacles). To avoid any negative influence on the referral process, we excluded items concerning potentially provocative issues (sexual/physical/emotional abuse), one item that may provoke feelings of guilt (separation of parents) and one item referring to an extremely unusual but emotionally repellent phenomenon (witness of murder). The number of items was, thus, reduced to nine concerning accidents; natural disasters; own, parental, siblings’ or friends’ severe injury/illness; parental psychiatric illness; substance abuse in the home environment; having witnessed violence. The overall Cronbach’s Alpha in both groups was 0.40, specified in the ADHD group as 0.44 and in comparisons as 0.23.
Parental ratings on SNAP-IV were used for estimating the severity of ADHD-symptoms and for excluding comparisons with high ADHD ratings [32]. Since the clinical diagnoses were ICD-based, these ratings were also used for identifying DSM-related subtypes of ADHD (predominantly inattention [ADHD-I], predominantly hyperactivity/impulsiveness [ADHD-HI], or combined [ADHD-C]). In the ADHD group 52 children were categorized as ADHD-I, 22 as ADHD-HI and 54 as ADHD-C. The version applied has 30 items [9 for inattention, 9 for hyperactivity/impulsivity, 8 for Oppositional Defiant Disorder (ODD), 4 control questions], scored by parents and teachers on a 4-point scale: 0 for “not at all”, 1 for “just a little”, 2 for “quite a bit” and 3 for “very much”. It has been psychometrically tested in a Northern American sample and has demonstrated “acceptable internal consistency and item selection and a factor structure consistent with the two-factor solution of ADHD-symptoms, and a third ODD factor” [33]. Normative data for Swedish children are not available. However, intercultural similarities and the firm basis in the DSM IV-criteria motivated this choice. The overall Cronbach’s Alpha was 0.97 in the ADHD group and comparison group together. Similar results were found in both groups. The alpha varied between 0.80 and 0.92 for the subscales. ODD was defined as at least four items scored as “quite a bit” or “very much”. In the ADHD group 84 children were categorized as having ODD.
Cortisol analyses
Cortisol was analyzed in saliva and expressed in nmol/L. Sampling was performed at home during one ordinary weekday (a school day) when waking up, 30 min after waking up, at 4 PM or when coming home from school and when going to bed. Information was given that the sampling should be done before brushing teeth, at least 30 min after eating or drinking and at least 1 h after sport activity. The sampling times were filled in by the families immediately after completing saliva sampling. Samples were collected by swabs (Salivette; Sarstedt Inc., Rommelsdorf, Germany), which the participants kept in their mouth 1–2 min until soaked with saliva. The swabs were placed in plastic sampling tubes. The tubes were centrifuged and stored at −70 °C until analyzed with radioimmunoassay technique using the Spectria Cortisol (125I) kit from Orion Diagnostica, Espoo, Finland [34]. In 89 % of the saliva samples the volume was large enough for carrying out analyses. There were no statistically significant (χ²) differences concerning the number of non-analyzable samples between the ADHD group and the comparison group for any of the sampling times. In addition to cortisol levels we analyzed “the morning increase” by calculating 30 min post awakening minus awakening value, i.e. the dynamic change in post wakening which is closely correlated to the area under the curve with reference to the first awakening [35]. Cortisol data for the comparison group and for a slightly different ADHD group (including four individuals lacking adversity data) has previously been published in Isaksson et al. [4].
Statistical analyses
All analyses were performed with the statistical software program SPSS (version 19). As data on cortisol and adversity ratings showed a skewed distribution, we used non-parametric statistical methods (Mann–Whitney and χ²) for calculating group differences and log-transformation of the saliva cortisol values. In the binary logistic model we used a reversed log scale since lower cortisol levels are associated with the outcome ADHD. The logistic regression was used to calculate the odds ratio of belonging to the ADHD group based on exposure to psychosocial adversity, sex, age (years) and cortisol levels. In this regression, we chose the cortisol awakening level since it was most clearly associated with ADHD-symptoms. As a consequence of the low internal consistency of the adversity questionnaires (especially childhood adversity) and with the intention of facilitating the interpretation of the results, exposures to adversity were transformed into categorical variables by severity: no reported adversity; one type of reported adversity; more than one type of reported adversity. Logistic regression does not have an equivalent to the R 2 that is found in OLS regression. However, Nagelkerke R 2 is a pseudo R 2 statistics which gives an estimation of the model fit. Interaction effects between sex and group belongingness on exposures to adversity were calculated with ANOVA. Associations between cortisol levels and ADHD-symptoms—adjusted for exposures to adversity, sex, age, sampling time and ODD-symptoms—were calculated with a linear regression. Analyses of adversity exposures in relation to cortisol levels were performed using Pearson correlation. Two-tailed test with p values <0.05 was considered significant.
Results
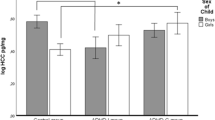
Parents of children in the ADHD group presented more reports of at least one rated foetal psychosocial adversity (55 and 44 %, respectively; p = 0.041), childhood psychosocial adversity (50 and 33 %, respectively; p < 0.001) or both foetal and childhood adversity (53 and 30 %, respectively; p < 0.001) than parents of comparisons. Frequencies of separate exposures and significant differences between both groups are presented in Table 1.
Data on cortisol levels on the different sampling occasions are presented in Table 2. Children with ADHD had lower cortisol levels at awakening, 30 min later and before going to bed. In a logistic regression model—adjusted for age, cortisol level at awakening and sex—more than one exposure of foetal and/or childhood psychosocial adversity remained a predictor of belonging to the ADHD group. Also, cortisol levels (lower levels increased the risk of belonging to the ADHD group) and sex (male sex increased the risk of belonging to the ADHD group) were significant predictors in the model (Table 3). The model explained 32 % of the variation of belonging to the ADHD group.
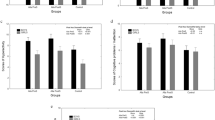
Reports of at least one foetal or childhood psychosocial adversity did not differ between subgroups (ADHD-I, ADHD-HI and ADHD-C; concurrent ODD-symptoms or not). As to sex differences, girls in the ADHD group had higher reported rates than female comparisons of at least one psychosocial adversity during pregnancy (66.7 and 43.3 %, respectively; p = 0.011) and childhood (49 and 32.6 %, respectively; p = 0.043), whereas boys in the ADHD group only had higher rates of childhood psychosocial adversity than male comparisons (50.7 and 33.7 %, respectively; p = 0.010). There was a significant interaction effect between sex and group belongingness for foetal adversity (f = 5.21; p = 0.023), but not for childhood adversity (not shown in tables).
There was a negative association between ADHD-symptoms and cortisol levels at awakening (b = −0.27; p < 0.001), 30 min after awakening (b = −0.24; p < 0.001) and at bedtime (b = −0.11; p = 0.027), as well as a trend in the afternoon sample (b = −0.092; p = 0.073). No association was found for the morning increase. The association between ADHD-symptoms and the two cortisol morning samples remained when adjusted for age, sex, foetal and childhood psychosocial adversity, sampling time and ODD-symptoms (b = −0.36; p < 0.001 and b = −0.25; p = 0.008, respectively), whereas the association between ADHD-symptoms and cortisol levels at bedtime disappeared. ODD-symptoms were not associated with cortisol levels in the adjusted models. There was no relation between foetal/childhood psychosocial adversity and cortisol levels on the four sampling occasions in the two groups, separately. However, there was a positive correlation in the ADHD group (not in the comparison group) between childhood adversity and morning increase (r = .19; p = 0.041).
Discussion
Children with clinically verified ADHD (n = 197) had to a higher degree been exposed to foetal and childhood psychosocial adversity than comparisons (n = 221). The previously reported association between low morning cortisol levels and ADHD-symptoms remained when adjusted for foetal and childhood psychosocial adversity as well as sex, age, sampling time and ODD-symptoms. No relation was found between exposures to psychosocial adversity and diurnal cortisol levels on any sampling point, but there was a positive correlation between childhood adversity and the cortisol morning increase in children with ADHD.
The high exposure of adversities in the ADHD group is in line with previous studies [6, 12]. This may hypothetically reflect a causal link. If so, an underlying mechanism could be the early programming of the HPA-axis [12, 23, 24]. However, the hypothesis that early psychosocial adversity (prenatal or postnatal) may have a programming effect on the HPA-axis, leading to a hyper- or hypocortisolism preceding psychiatric symptoms like ADHD, was not supported by our findings since there was no relation between adversity and diurnal cortisol levels in children with ADHD or in non-affected comparisons. However, there was a weak positive correlation between childhood adversity and the morning increase in children with ADHD. The morning increase is regarded as a distinct feature of the HPA-axis [36]. The function of this increase is not known, although it is hypothesized that a sharper increase is associated with chronic stress and/or anticipation of the upcoming day [36]. This is partly in line with our finding where the positive correlation in the ADHD group may reflect the greater extent of external stressors related to a higher degree of childhood adversity.
Although no previous studies have focused on the relation between early psychosocial adversity, cortisol and ADHD, there are some reports with a similar approach and a focus on “externalizing behaviour”, a concept that is overlapping ADHD. Externalizing behaviour has—just as ADHD—been associated with psychosocial adversity [37] as well as with lower cortisol levels [38]. In a study on the relation between salivary cortisol, aggressive behaviour and psychosocial adversity, hypocortisolism was the characteristic of children displaying relational aggression. The authors conclude that the cortisol dysregulation was related to the aggression in itself rather than to the exposure to stressors [39]. This is in line with the conclusions from a review on antisocial behaviour and its relation to the HPA-axis, where the authors conclude that “… pathways to antisocial behaviour involving early environmental adversity may be less related to the HPA-axis than has often been assumed” [38]. It has been discussed that lower cortisol levels in ADHD are particularly associated with comorbid ODD [40]. However, in our study ADHD was associated with lowered cortisol levels even after adjusting for ODD-symptoms. Furthermore, there were no association between ODD and cortisol levels in the adjusted model.
In a human research program aimed at testing each step of the programming theory [41], only a weak correlation was found between maternal anxiety and maternal plasma cortisol levels and no correlation was found between maternal anxiety on one side and the amniotic cortisol levels and amniotic testosterone levels on the other. In a following study, the authors found that amniotic cortisol levels predicted cognitive development and infant cortisol levels at approximately 17 months. However, neither maternal anxiety ratings nor maternal plasma cortisol levels were associated with infant cortisol or the child’s cognitive development [42, 43]. Accordingly, the findings so far from this research program also challenge the programming theory, i.e. in this case the hypothesis that cortisol mediates the effects of parental stress on the child’s development.
Notably, the link between psychosocial adversity and ADHD may be built up by various mechanisms, which may not necessarily be psychological or psycho-physiological in nature. For instance, psychosocial adversity may be related to malnutrition which seems to have an independent effect on the development of externalising behaviour, mediated by cognitive ability [44]. The higher rates of exposures to foetal and childhood psychosocial adversity among children with ADHD may also reflect a common genetic background, where some of the adversities may be seen as direct or indirect expressions of parental psychological and psychiatric symptoms. HPA-axis functioning—expressed as cortisol levels—may act as an independent variable, thereby rather suggesting a genetic background. Previous findings from our group [4] that foremost the morning cortisol levels—which seem to be more strongly influenced by genetic factors than afternoon and evening levels [5]—are lower in the ADHD group, are in line with a genetic explanation of the hypocortisolism in children with ADHD. Furthermore, as seen in this study, psychosocial adversity did not affect the relation between ADHD-symptoms and cortisol levels in the morning. Along the same line, a recent study showed that the link between prenatal stress and ADHD in the offspring was only present in biologically related mother–offspring pairs and, therefore, attributable to inherited factors [45].
Limitations
There is a risk of recall bias in case–control studies where the disease has already occurred when exposure information is obtained. Recall bias may distort the measure of association between exposure and disease by under-reporting or over-reporting. Parents may be prone to over-report when seeking for an explanation of the disease or when they have an assumption about its underlying cause [46].
Possibly, other types of stressors like exposure to sexual, physical and emotional abuse would have had a measurable impact on the cortisol levels. The instruments focused on “classical” traumatic experiences like accidents, illness or violence, just as the LITE-questionnaire [47]. Taking potentially stressful situations from other sectors of life into consideration—like the Coddington questionnaire [48] with its broader and more extensive life event approach—may have brought up other results.
The Cronbach Alpha values of the adversity questionnaires were low, especially for the Early Trauma Inventory, considerably lower than what has been previously reported by Bremner et al. [30]. To a certain degree this probably reflects the lower prevalence of all types of childhood trauma in our study and the lower number of items. However, it also reflects that the scores of the scales concerning foetal and childhood exposures cannot be directly considered and utilised as indices. They should rather be looked upon as a tentative approach to the task of elucidating the relations between psychological trauma and ADHD. To minimize the problem of low internal consistency we chose to perform our analyses using categorised trauma data instead of using mean scores.
The saliva sampling was performed during one regular weekday, limited to four occasions. For optimal cortisol measurement, it is advisable to collect saliva for more than 1 day also assessing participant’s adherence [35]. However, we wanted the sampling to be done on a regular school day since the day of cortisol assessment is crucial in psychoendocrinological stress studies [49]. We also assumed that the procedure with numerous collecting points would be too demanding and might increase attrition.
Subtypes of ADHD were defined by parental ratings and not diagnosis, thereby, reflecting symptoms rather than a psychiatric evaluation. However, all individuals in the ADHD group had undergone structured but individually adapted investigations at specialized teams and received an ADHD-diagnosis.
It is a delicate matter to choose statistical methods in a study where the outcome measures are on a skewed ordinal or interval scale. We used non-parametrical methods as well as log-transformations, according to the design of analysis. The procedure with non-parametrical statistical approaches will, on the one hand, avoid false findings according to outliers in the dependent variables (type I errors), however; on the other hand, reduce the power to detect small, but significant differences between groups (type II errors). We considered p < 0.05 significant, although several tests were done analyzing the data. An alternative would have been to use Bonferroni adjustments. However, this method has been criticized since the interpretations depend on the number of tests that are performed and the likelihood of type II errors is also increased [50]. Instead it is argued that the best approach is to describe what has been done and why [50]. However, the relation in our models was high, pointing at robust results.
In conclusion, children with ADHD had been exposed to foetal and childhood psychosocial adversity to a higher degree than comparisons. No relation was found between such exposures to foetal/childhood adversity and cortisol levels, but there was a positive correlation between childhood adversity and the morning increase in children with ADHD. The low cortisol levels in children with ADHD still stand out as a mystery.
References
King JA, Barkley RA, Barrett S (1998) Attention-deficit hyperactivity disorder and the stress response. Biol Psychiatry 44(1):72–74
Blomqvist M, Holmberg K, Lindblad F, Fernell E, Ek U, Dahllof G (2007) Salivary cortisol levels and dental anxiety in children with attention deficit hyperactivity disorder. Eur J Oral Sci 115(1):1–6
Ma L, Chen YH, Chen H, Liu YY, Wang YX (2011) The function of hypothalamus–pituitary–adrenal axis in children with ADHD. Brain Res 1368:159–162
Isaksson J, Nilsson KW, Nyberg F, Hogmark A, Lindblad F (2012) Cortisol levels in children with attention-deficit/hyperactivity disorder. J Psychiatr Res 46:1398–1405
Bartels M, de Geus EJ, Kirschbaum C, Sluyter F, Boomsma DI (2003) Heritability of daytime cortisol levels in children. Behav Genet 33(4):421–433
Biederman J, Faraone SV (2005) Attention-deficit hyperactivity disorder. Lancet 366(9481):237–248
Thapar A, Cooper M, Jefferies R, Stergiakouli E (2012) What causes attention deficit hyperactivity disorder? In: Archives of disease in childhood, vol 97. vol 3. England, pp 260–265
Banerjee TD, Middleton F, Faraone SV (2007) Environmental risk factors for attention-deficit hyperactivity disorder. Acta Paediatr 96(9):1269–1274
Maccari S, Morley-Fletcher S (2007) Effects of prenatal restraint stress on the hypothalamus–pituitary–adrenal axis and related behavioural and neurobiological alterations. Psychoneuroendocrinology 32(Suppl 1):S10–S15
Van den Bergh BR, Marcoen A (2004) High antenatal maternal anxiety is related to ADHD symptoms, externalizing problems, and anxiety in 8- and 9-year-olds. Child Dev 75(4):1085–1097
Rodriguez A, Bohlin G (2005) Are maternal smoking and stress during pregnancy related to ADHD symptoms in children? J Child Psychol Psychiatry 46(3):246–254
Talge NM, Neal C, Glover V (2007) Antenatal maternal stress and long-term effects on child neurodevelopment: how and why? J Child Psychol Psychiatry 48(3–4):245–261
Hjern A, Weitoft GR, Lindblad F (2010) Social adversity predicts ADHD-medication in school children—a national cohort study. Acta Paediatr 99(6):920–924
Lupien SJ, King S, Meaney MJ, McEwen BS (2000) Child’s stress hormone levels correlate with mother’s socioeconomic status and depressive state. Biol Psychiatry 48(10):976–980
Cicchetti D, Rogosch FA (2001) Diverse patterns of neuroendocrine activity in maltreated children. Dev Psychopathol 13(3):677–693
O’Connor TG, Ben-Shlomo Y, Heron J, Golding J, Adams D, Glover V (2005) Prenatal anxiety predicts individual differences in cortisol in pre-adolescent children. Biol Psychiatry 58(3):211–217
Gunnar MR, Frenn K, Wewerka SS, Van Ryzin MJ (2009) Moderate versus severe early life stress: associations with stress reactivity and regulation in 10–12-year-old children. Psychoneuroendocrinology 34(1):62–75
Carlson M, Earls F (1997) Psychological and neuroendocrinological sequelae of early social deprivation in institutionalized children in Romania. Ann N Y Acad Sci 807:419–428
Gunnar MR, Vazquez DM (2001) Low cortisol and a flattening of expected daytime rhythm: potential indices of risk in human development. Dev Psychopathol 13(3):515–538
Yehuda R, Engel SM, Brand SR, Seckl J, Marcus SM, Berkowitz GS (2005) Transgenerational effects of posttraumatic stress disorder in babies of mothers exposed to the World Trade Center attacks during pregnancy. J Clin Endocrinol Metabol 90(7):4115–4118
Bruce J, Fisher PA, Pears KC, Levine S (2009) Morning cortisol Levels in preschool-aged foster children: differential effects of maltreatment type. Dev Psychobiol 51(1):14–23
Gunnar MR, Quevedo KM (2008) Early care experiences and HPA axis regulation in children: a mechanism for later trauma vulnerability. In: Progress in brain research, vol 167. Netherlands, pp 137–149
Teicher MH, Andersen SL, Polcari A, Anderson CM, Navalta CP (2002) Developmental neurobiology of childhood stress and trauma. Psychiatr Clin N Am 25 (2):397–426, vii–viii
Lupien SJ, McEwen BS, Gunnar MR, Heim C (2009) Effects of stress throughout the lifespan on the brain, behaviour and cognition. Nat Rev Neurosci 10(6):434–445
Egliston KA, McMahon C, Austin MP (2007) Stress in pregnancy and infant HPA axis function: conceptual and methodological issues relating to the use of salivary cortisol as an outcome measure. Psychoneuroendocrinology 32(1):1–13
Kapoor A, Petropoulos S, Matthews SG (2008) Fetal programming of hypothalamic–pituitary–adrenal (HPA) axis function and behavior by synthetic glucocorticoids. Brain Res Rev 57(2):586–595
Van Voorhees E, Scarpa A (2004) The effects of child maltreatment on the hypothalamic–pituitary–adrenal axis. Trauma Violence Abuse 5(4):333–352
Rosengren A, Orth-Gomer K, Wedel H, Wilhelmsen L (1933) Stressful life events, social support, and mortality in men born in 1933. BMJ 307(6912):1102–1105
Rodriguez A, Waldenstrom U (2008) Fetal origins of child non-right-handedness and mental health. J Child Psychol Psychiatry 49(9):967–976
Bremner JD, Bolus R, Mayer EA (2007) Psychometric properties of the early trauma inventory-self report. J Nerv Ment Dis 195(3):211–218
Plaza A, Torres A, Martin-Santos R, Gelabert E, Imaz ML, Navarro P, Bremner JD, Valdes M, Garcia-Esteve L (2011) Validation and test-retest reliability of early trauma inventory in Spanish postpartum women. J Nerv Ment Dis 199(4):280–285
Swanson JM, Kraemer HC, Hinshaw SP, Arnold LE, Conners CK, Abikoff HB, Clevenger W, Davies M, Elliott GR, Greenhill LL, Hechtman L, Hoza B, Jensen PS, March JS, Newcorn JH, Owens EB, Pelham WE, Schiller E, Severe JB, Simpson S, Vitiello B, Wells K, Wigal T, Wu M (2001) Clinical relevance of the primary findings of the MTA: success rates based on severity of ADHD and ODD symptoms at the end of treatment. J Am Acad Child Adolesc Psychiatry 40(2):168–179
Bussing R, Fernandez M, Harwood M, Wei H, Garvan CW, Eyberg SM, Swanson JM (2008) Parent and teacher SNAP-IV ratings of attention deficit hyperactivity disorder symptoms: psychometric properties and normative ratings from a school district sample. Assessment 15(3):317–328
Hansen AM, Garde AH, Christensen JM, Eller NH, Netterstrom B (2003) Evaluation of a radioimmunoassay and establishment of a reference interval for salivary cortisol in healthy subjects in Denmark. Scand J Clin Lab Invest 63(4):303–310
Clow A, Hucklebridge F, Thorn L (2010) The cortisol awakening response in context. In: International review of neurobiology, vol 93. Elsevier Inc, United States, pp 153–175
Fries E, Dettenborn L, Kirschbaum C (2009) The cortisol awakening response (CAR): facts and future directions. Int J Psychophysiol 72:67–73
Deater-Deckard K, Dodge KA, Bates JE, Pettit GS (1998) Multiple risk factors in the development of externalizing behavior problems: group and individual differences. Dev Psychopathol 10(3):469–493
Hawes DJ, Brennan J, Dadds MR (2009) Cortisol, callous-unemotional traits, and pathways to antisocial behavior. Curr Opin Psychiatry 22(4):357–362
Murray-Close D, Han G, Cicchetti D, Crick NR, Rogosch FA (2008) Neuroendocrine regulation and physical and relational aggression: the moderating roles of child maltreatment and gender. Dev Psychol 44(4):1160–1176
Fairchild G (2010) Hypothalamic–pituitary–adrenocortical axis function in attention-deficit hyperactivity disorder. behavioral neuroscience of attention deficit hyperactivity disorder and its treatment, current topics in behavioral neuroscience 9. Springer Verlag, Berlin, pp 93–111
Sarkar P, Bergman K, O’Connor TG, Glover V (2008) Maternal antenatal anxiety and amniotic fluid cortisol and testosterone: possible implications for foetal programming. J Neuroendocrinol 20(4):489–496
Bergman K, Sarkar P, Glover V, O’Connor TG (2010) Maternal prenatal cortisol and infant cognitive development: moderation by infant–mother attachment. Biol Psychiatry 67(11):1026–1032
O’Connor TG, Bergman K, Sarkar P, Glover V (2012) Prenatal cortisol exposure predicts infant cortisol response to acute stress. Dev Psychobiol. doi:10.1002/dev.21007
Liu J, Raine A, Venables PH, Mednick SA (2004) Malnutrition at age 3 years and externalizing behavior problems at ages 8, 11, and 17 years. Am J Psychiatry 161(11):2005–2013
Rice F, Harold GT, Boivin J, van den Bree M, Hay DF, Thapar A (2010) The links between prenatal stress and offspring development and psychopathology: disentangling environmental and inherited influences. Psychol Med 40(2):335–345
Infante-Rivard C, Jacques L (2000) Empirical study of parental recall bias. Am J Epidemiol 152(5):480–486
Greenwald R, Rubin A (1999) Assessment of posttraumatic symptoms in children: development and preliminary validation of parent and child scales. Res Social Work Prac 9:61–75
Coddington RD (1972) The significance of life events as etiologic factors in the disease of children. J Psychosom Res 16:7–18
Schlotz W, Hellhammer J, Schulz P, Stone AA (2004) Perceived work overload and chronic worrying predict weekend–weekday differences in the cortisol awakening response. Psychosom Med 66(2):207–214
Perneger TV (1998) What’s wrong with Bonferroni adjustments. BMJ 316(7139):1236–1238
Acknowledgments
We are grateful to all children who volunteered and to their parents and schools in Uppsala, Enköping and Gävle who made it possible for us to recruit the children. We are also grateful to the child and adolescent Psychiatric units in Uppsala, Enköping, Gävle and Falun for contributions to the recruitment procedure. We also want to thank Hans Arinell for statistical assistance and Lars Holmberg for the cortisol analyses. The study was supported by Grants from Victoriafonden through the Swedish Brain Foundation, (Hjärnfonden), (no specific grant no.). The PhD position of Johan Isaksson was supported by Uppsala University Hospital Research Fund (ALF), (no specific grant no.). The research position of Frank Lindblad was financed by the Swedish Council for Working Life and Social Research, Grant No. 2006-0197.
Conflict of interest
The authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Isaksson, J., Nilsson, K.W. & Lindblad, F. Early psychosocial adversity and cortisol levels in children with attention-deficit/hyperactivity disorder. Eur Child Adolesc Psychiatry 22, 425–432 (2013). https://doi.org/10.1007/s00787-013-0383-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00787-013-0383-0