Abstract
The aims of this study were to identify in what ways adolescents who cut themselves differ from those who take overdoses, and to investigate the role of contagion in these behaviours. Data from an anonymous self-report questionnaire survey of 6,020 adolescents in 41 schools were analysed. Comparison of 220 adolescents who reported self-cutting in the previous year with 86 who had taken overdoses in the previous year as the sole method of deliberate self-harm (DSH) showed that far more of those who cut themselves had friends who had also engaged in DSH in the same period (OR 2.84, 95% CI 1.5–5.3, P < 0.001), and fewer had sought help from friends before cutting (OR 0.5, 95% CI 0.3–0.9, P < 0.02). Self-cutting usually involved less premeditation. Analyses at both the individual and school level showed that the association between engaging in DSH and exposure to DSH amongst peers was largely confined to girls who cut themselves. There are important differences between adolescents who cut themselves and those who take overdoses. Contagion may be an important factor in DSH by adolescents, especially in girls who cut themselves. These findings are relevant to the design of prevention and treatment programmes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
A variety of terms and indeed concepts have been applied to self-poisoning and self-injury [34, 40]. In the UK the term ‘deliberate self-harm’ (DSH) has been used to encompass all acts of intentional self-poisoning and self-injury [20, 35], whereas in North America researchers often divide such behaviour into ‘attempted suicide’, where death is at least part of the intended outcome, and ‘non-suicidal self-injury’, where death is definitely not the intended outcome [40]. The rationale for the approach used in the UK is because, first, the motivation for an act of self-poisoning or self-injury is often mixed, both suicidal and non-suicidal intentions being involved in many acts [1, 27], secondly, suicidal intent is a dimensional rather than a unitary phenomenon [16], and thirdly, motives or intentions underlying some acts of self-poisoning and self-injury may be unclear. While pressure from user groups has lead some organisations and researchers to change the term ‘deliberate self-harm’ to ‘self-harm’ [22], we prefer to retain the full term ‘deliberate self-harm’ in order to indicate intentionality and thus distinguish the behaviour from accidental self-harm. Such an approach has also recently been adopted in a study of youth in the USA [32].
There is increasing recognition that DSH in adolescents represents a major problem [23]. Many studies have been conducted of adolescents who present to hospital following such behaviour, e.g. [2, 19, 29]. Most of these adolescents have taken overdoses. A growing body of research has shown that the levels of self-poisoning and self-injury in adolescents in the community are far greater than is apparent from hospital-based studies [9]. Furthermore, self-cutting is more common than self-poisoning amongst adolescents in the community [23, 30], with self-poisoning being the main factor likely to lead to presentation to clinical services following DSH [24, 45]. Also, self-cutting is likely to be repeated, often on many occasions [10].
There is growing interest in self-cutting among young people. Most previous research has been based on clinical samples [11, 33]. There is less understanding of self-cutting at the community level. This is important because only a small minority of adolescents who cut themselves may present to clinicians, and even fewer to hospitals. Thus, there is little information on the factors associated with self-cutting in adolescents and how those who cut themselves differ from those who take overdoses. Such information is likely to be important for the development of greater understanding of the development and maintenance of self-cutting and the design of prevention strategies.
We believe that comparing the characteristics of individuals involved in the two types of behaviour, self-cutting and self-poisoning, is important because these behaviours usually involve different levels of risk of fatality and there are known to be some marked differences in the motives associated with the acts [38]. There has been little research on self-cutting in males [21, 28], especially in adolescents, most attention having been focused on girls. It is known that there are some gender differences in the motives involved in the two behaviours [38], and there are important differences for suicidal and self-harming behaviours more generally [17].
One factor that may contribute to DSH by adolescents is exposure to the behaviour in other individuals [13, 44]. Reports from a multi-centre international study of DSH in adolescents, the Child and Adolescent Self-harm in Europe (CASE) Study [30], have highlighted this. Using the same methodology, investigators in six countries have found that one of the key factors associated with risk of DSH in adolescents is having peers who have carried out acts of DSH (and also DSH by family members) [6, 25, 46]. Other studies have also identified this as a significant factor [7]. Of further relevance to the possible influence of ‘contagion’ on DSH in adolescents is the extent to which they use peers as a source of help. In the investigation from the CASE Study carried out in England, friends were by far the most frequent individuals whom adolescents reported they had contacted for help, both before and after DSH [8]. In addition to providing a potential means of getting support and help, such contacts may also influence the potential spread of DSH. It is not known whether the influence of exposure to DSH by peers might differ between those who take overdoses and those who cut themselves.
Deliberate self-harm in adolescents is often related to life events and problems [22]. A range of other factors may contribute to vulnerability to DSH in adolescents [5, 22, 23], including depression and anxiety, impulsivity, low self-esteem and types of coping strategies adolescents employ [41]. Again, information is lacking on the extent to which these characteristics differ between those adolescents who cut themselves and those who take overdoses.
In the CASE Study the prevalence of DSH and associated factors were identified through a carefully developed and well-piloted self-report questionnaire completed by adolescents in schools [23, 30]. In the study carried out in England, DSH had occurred in 6.9% of adolescents in the previous year [25]. This figure is similar to that found in studies in other countries, although there may also be some international variations in prevalence [9, 30].
We have used the data from England in the present investigation. The main aim of this study was to identify factors which distinguish adolescents who cut themselves from those who take overdoses, including possible differences between the two genders. We have investigated the following characteristics: motives for the act, premeditation, previous DSH, types of problems adolescents were facing, drugs and alcohol use, depression, anxiety, impulsivity, self-esteem, coping styles and help-seeking before and after DSH. We have also conducted some preliminary analyses regarding the possible role of contagion through exposure to DSH by others, and whether this differs between those who cut themselves and those who take overdoses and also between the two genders. Our hypotheses were that there would be indications of less severe psychopathology in those who cut themselves and that evidence of possible contagion would be stronger for self-cutting and for females.
Materials and methods
Sample
The study was conducted in 41 schools in England in the counties of Oxfordshire and Northamptonshire, and the city of Birmingham. The schools were chosen to provide a representative sample in terms of gender, size, government or privately funded, single sex and co-educational, ethnic minorities, educational attainment and socio-economic deprivation. The pupils were in classes in which at least 90% were aged 15 and 16 years.
The target sample size was 5,000, based on a conservative estimate of prevalence of DSH in the preceding year of 4% [9].
Recruitment
All pupils in the identified classes were eligible for the study (N = 7,433). The parents of the pupils were informed of the study by letter and given the option to withdraw their child. Potential subjects could also withdraw if they wished. In total, 139 parents withdrew their child from the study and a further 23 pupils opted out. A total of 1,243 pupils were absent on the day of the survey, most of these absences being due to illness or involvement in external school activities. The eventual sample included 6,020 adolescents (3,186 males and 2,810 females; 24 gender unknown).
Data collection
Details of the study methodology have been reported elsewhere [23, 25]. The survey was conducted by means of an anonymous self-report questionnaire developed as part of an international collaboration, the CASE study [30]. Pilot testing of the questionnaire was conducted in two schools and an adolescent psychiatric unit.
The questionnaire included items on demographic information (gender, age, and ethnicity) and questions about lifestyle and problems. There were specific questions about episodes of DSH and thoughts of self-harm. Those adolescents who reported having harmed themselves were asked to describe this act (the most recent for repeaters) and to indicate whether or not they had presented to hospital (or other clinical services). The adolescents were also asked whether they had sought help beforehand or afterwards and if so, from whom. They were also asked to indicate which motive or motives from a list applied to this act, including if they had wanted to die. This list of motives was an adapted version of that developed by Bancroft and colleagues [1] and used in several other studies, e.g. [18, 27]. We have previously reported motives for self-harm acts as reported by adolescents who cut themselves and those taking overdoses [38] but included them in the present study for completeness.
All the adolescents in the study were asked whether they had experienced any of a series of problems, about alcohol and drug use, and about exposure to DSH and suicide involving peers and family members and who they turned to for help with problems.
Other measures of psychological functioning included in the questionnaire were:
Depression and anxiety
The hospital anxiety and depression scale (HADS), which is a 14-item self-report scale used to assess depression and anxiety in non-psychiatric populations [47]. It has been validated in adolescents [43].
Impulsivity
Six items from Plutchik Impulsivity Scale [36].
Self-esteem
A shortened 8-item version of the Self-Concept Scale, a well-validated measure of self-esteem [37]. The original author developed the shortened version [23] by selecting items from each factor within the full version of the scale that correlated most highly with overall scores on the scale.
Coping strategies
Participants were asked about the types of coping strategies they used when they were worried or upset. This measure was developed specifically for the project. Coping responses were divided into emotion-oriented items (blamed themselves for getting into the situation, got angry, stayed in their room, had an alcohol drink, tried not to think about what was worrying them) and problem-oriented items (talked to someone, thought about how they had dealt with similar situations, tried to sort things out).
The descriptions of the DSH episodes were analysed against a definition and specific guidelines in a manual (available from the first author and in Hawton and Rodham [23]) by three researchers independently. The definition of DSH was:
An act with a non-fatal outcome in which an individual deliberately did one or more of the following:
-
initiated behaviour (for example, self-cutting, jumping from a height), which they intended to cause self-harm
-
ingested medication in excess of the prescribed or generally recognised therapeutic dose
-
ingested a recreational or illicit drug in an act that the person regarded as self-harm
-
ingested a non-ingestible substance or object.
All adolescents who reported a DSH episode that involved self-cutting alone (i.e. not with another method) or self-poisoning alone in the year before the survey was conducted were included in the present study. Episodes that included self-cutting or self-poisoning along with another method of DSH, or other methods of DSH, were not included.
Ethical approval
The study had the approval of Oxford Psychiatric Research Ethical Committee.
Statistical analyses
Logistic regression analyses and Mann–Whitney tests were used to compare the adolescents who used self-cutting with those who used self-poisoning. Multiple stepwise logistic regression analysis was used to calculate adjusted odds ratios. For the investigation of the possible role of contagion at the school level, the percentage of adolescents in each school who reported self-cutting or self-poisoning and the percentage of adolescents in each of these groups in each school who reported having friends who had engaged in DSH were both calculated and then compared using Pearson’s r to assess the extent of correlation. The data were analysed with SPSS version 10 for Windows [42].
Results
The focus of this study was on those adolescents who reported either cutting OR poisoning. Of the 398 (6.9% of total) adolescents who described an episode of DSH in the preceding year meeting our study criteria, 220 (55.3%) had cut themselves and 86 (21.6%) had taken overdoses as the sole method of DSH (Table 1). We excluded those who reported using another single method (N = 42, 10.6%), or both cutting and poisoning in the same episode (N = 23, 5.8%), or use of other multiple methods (N = 27, 6.8%).
Comparison of characteristics of adolescents with self-cutting with those who self-poisoned
Deliberate self-harm was far less common in the boys than in girls. Of those with a history of DSH similar proportions of boys (49/61, 80.3%) and girls (171/245, 69.8%) had cut themselves (Table 2). Although there was no difference in the proportions of self-cutters and self-poisoners with a family history of DSH, the proportions were substantial in both groups of adolescents (approximately 40%). Adolescents who cut themselves were significantly more likely to have friends who had engaged in DSH in the preceding year. This was found for both those who indicated suicidal intent [14/74 (56.8%) vs. 16/48 (33.3%), χ2 = 6.41, P = 0.011] and those without suicidal intent [64/110 (58.2%) vs. 9/25 (36.0%), χ2 = 4.04, P < 0.05].
Far fewer of the adolescents who had cut themselves said that they had wanted to die at the time of DSH (Table 2). Self-cutting usually involved less pre-meditation than self-poisoning and was more often repeated. Repetition of DSH was more frequent in the adolescents who cut themselves with suicidal intent compared with those without such intention [54/74 (73.0%) vs. 54/110 (49.1%), χ2 = 10.41, P = 0.002] but not for those who took overdoses [23/49 (46.9%) vs. 10/25 (40.0%), χ2 = 0.32, P = 0.57]. There were no major differences between the two groups in terms of drug and alcohol use.
A smaller proportion of those who had cut themselves had sought help from a family member before their DSH, although few adolescents in either group had done so (Table 3). In contrast, many adolescents had sought help from friends before DSH, but once again, a significantly smaller proportion of those who cut themselves had done so. Very few in either group had sought help from a general practitioner, social worker, psychologist or psychiatrist, telephone helpline, or drop in/advice centre. Overall, fewer of those who had cut themselves than those who took overdoses had sought help from any source beforehand.
Fewer adolescents who cut themselves reported arguments between their parents in the preceding year (Table 3). The two groups of adolescents did not differ greatly with regard to other types of problems (the more frequent ones shown in Table 3). The two groups of adolescents also had similar scores on the measures of depression, anxiety, and both combined impulsivity, and self-esteem. Furthermore, their reported use of problem-orientated or emotion-focused coping strategies did not differ.
Comparison of the two groups of adolescents using multivariate logistic regression was conducted, using factors that were significant in the univariate analyses. Three factors then independently distinguished those who cut themselves from those who took overdoses. More of those who cut themselves had friends who had engaged in DSH (OR 2.84, 95% CI 1.5–5.3, P < 0.001), and fewer had sought help from friends before DSH (OR 0.5, 95% CI 0.3–0.9, P < 0.03) or had wanted to die (OR 0.46, 95% CI 0.3–0.9, P < 0.02).
Gender differences
As noted above, far more of those who cut themselves than those who took overdoses had friends who had self-harmed (Table 2). Whilst this difference was marked in the females (58.5 vs. 36.6%), there was a smaller but non-significant trend in the boys (40.8 vs. 27.3%) (Table 4).
Somewhat more of those who engaged in self-cutting said that they had friends who knew about their last episode of DSH, but this difference was small and non-significant for both genders (Table 4). Fewer of those who had cut themselves had tried to get help from a friend beforehand, although this difference was only significant for girls. The non-significant difference within boys may have been due to the relatively small number of boys who had taken overdoses.
While fewer of those who had cut themselves reported receiving help from a friend after the act of DSH, the difference was non-significant in both genders (Table 4). There was little difference between the self-cutters and the self-poisoners in terms of how many had ever told anyone that they were going to harm or kill themselves (Table 4).
Evidence of possible contagion within schools
Using only the co-educational schools (N = 32), we examined the correlation between the proportion of adolescents who reported an episode of DSH in the previous year and the proportion of those who said that they were aware of a friend having self-harmed. The analysis was focused on co-educational schools in order to provide a consistent basis for comparison between genders. There was a marked association between the level of DSH in schools and reporting of peers with DSH (Pearson’s r = 0.82, P < 0.001). This association was largely accounted for by a correlation between the two factors amongst girls (r = 0.69, P < 0.001). Amongst boys, the correlation was low and not significant (r = 0.20, P = 0.3). When the analysis was repeated for those who had cut themselves and those who took overdoses, the association was only found amongst those who had engaged in cutting (self-cutters, r = 0.69, P < 0.001; self-poisoners, r = 0.08, P = 0.7).
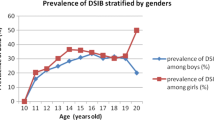
We then repeated the analysis by method of self-harm for girls and boys separately. The association between prevalence of self-harm and having peers who had self-harmed was strong when examined in females who cut themselves (r = 0.63, P < 0.001; Fig. 1), but was virtually absent in females who took overdoses (r = 0.10, P = 0.6). In the males, there was no significant association in either those who cut themselves (r = 0.14, P = 0.4; Fig. 1) or in those who took overdoses (r = 0.11, P = 0.5). It should be noted, however, that there were a relatively large number of schools in which no boys reported taking overdoses.
Discussion
We have used data from a large study of a representative population of school pupils to examine factors associated with the two main methods of DSH used by adolescents in the community, namely self-cutting and self-poisoning [25, 30]. The first aim was to compare the characteristics of adolescents who cut themselves with those who took overdoses. Interestingly, while the research literature on self-cutting is generally focused on females, in this study similar proportions of the DSH episodes by boys and girls involved self-cutting. However, in keeping with the overall prevalence of DSH, numerically there were far more self-cutting episodes in girls. A history of DSH by family members was equally common in the two groups of adolescents. We and other researchers have previously shown that a family history of DSH is a key independent factor associated with DSH [7, 25]. It is unclear, however, to what extent this association reflects transmission of the behaviour by biological [31, 39], social or psychological mechanisms, or is due to DSH being a marker of some other contributory factor such as family adversity [7].
Self-cutting was often more impulsive than self-poisoning, more of the adolescents who cut themselves saying that they had done it within an hour of first thinking about it. In keeping with this far fewer of those who cut themselves said they intended to die. As we have reported elsewhere, self-cutting, especially in girls, seems more often to be associated with relieving a distressed state of mind and with self-punishment [38]. Several investigators have emphasised the tension-reducing or affect-regulating function of many acts of superficial self-cutting [4, 33]. Perhaps because of this, and the apparent associated ‘addictive’ nature of self-cutting [33], this behaviour is often repeated and in this study this was so more often than for self-poisoning. We did not find any major differences between those who cut themselves and those who self-poisoned in terms of depression, anxiety, impulsivity, self-esteem and coping behaviours. Thus, there was no indication of differences in terms of possible psychopathology. However, we have previously shown that the adolescents with DSH in this study had higher scores than other adolescents for depression, anxiety and impulsivity, and lower scores for self-esteem [25].
Fewer of the adolescents who cut themselves had sought help from other people, including friends, beforehand. This might partly reflect the often impulsive nature of self-cutting. It might also be due to the private nature of many self-cutting acts. However, there was little difference between the two groups of adolescents in terms of the problems they were facing, except that fewer of those who cut themselves had been exposed to arguments between their parents.
One could question the distinction we have made in this study between two groups of adolescents who have engaged in DSH purely on the basis of specific methods used in the act, especially as it is known that some individuals who cut themselves may on another occasion take overdoses, or use both methods on the same occasion [25]. We believe, however, that the differences we have found between the two groups of adolescents have justified this approach and added new insights into the two phenomena.
The second aim of this study was to investigate the possible role of contagion in DSH. One indication that contagious influences may be more important in self-cutting was the fact that more of the adolescents who cut themselves had friends who had engaged in DSH (54.5 vs. 35.4%). This was especially true of the girls. Further evidence of the potentially contagious nature of self-cutting was provided by the school level analyses with the prevalence of self-cutting but not self-poisoning in schools being strongly correlated with reported exposure to DSH by peers. This association was only found in girls. This finding appears to provide evidence that contagion may be an important factor in self-cutting but that this primarily applies to girls. Of course there may be other explanations for the findings, including assortative selection of peer groups. However, it is unclear why this would selectively influence findings for self-cutting and not self-poisoning, and also why this should largely only apply to females. Contagion is well-recognised as an important factor in self-harming behaviour, including both suicide [14, 15] and non-fatal self-harm [13]. Contagion appears to be a particularly strong influence in young people [15, 26].
What mechanisms might be involved in the contagious nature of self-cutting? Several are possible. These include pressure to conform to peer group behaviour, sharing similar risk factors to peers, recognition of the potential psychological impact of self-cutting, and the normalisation of the behaviour through exposure to it in others. Further research is required to elucidate the relative importance of these possible explanations. In depth interviews with adolescents who cut themselves might be a useful way forward.
One of the limitations of this and similar studies of the community prevalence of DSH in adolescents is that it relies on self-reporting of DSH. However, we have gone further than most other investigations of this kind in that we obtained descriptions of the DSH episodes from the adolescents and only included as DSH those episodes for which a description was provided and where this met our criteria for DSH (see [23; pp. 28–29, 194–200], for more details). Another limitation of the study is that we did not have any information on the nature of the DSH episodes of the peers. Thus we do not know, for example, whether the DSH acts engaged in by peers involved the same methods as those used by the study participants. On the basis of the reported frequency of different methods of DSH, however, it is likely that the majority of the peers would have used self-cutting. A third limitation is that the precise timing of DSH episodes by both the adolescents in this study and their peers was not known, so that we cannot comment on possible clustering of DSH acts over time. A fourth limitation concerns absenteeism. As we have noted, the majority of absences recorded were due to illness or involvement in external school activities. However, we recognise that there is a possibility that some of those absent were deliberately avoiding participating in the survey. We do not know the potential effect of this on the prevalence of DSH, but recognise that DSH is more common amongst those who regularly truant [3]. Finally, in spite of including a relatively large sample of adolescents in the study statistical power was limited for certain analyses, especially those involving use of self-cutting versus self-poisoning in boys.
The findings of this study have shown that there are important differences as well as similarities between adolescents who cut themselves and those who take overdoses, especially in relation to premeditation and intention. The results have also provided some evidence for the role of contagion in DSH, but this appears to be more strongly related to self-cutting behaviour in girls. Studies involving a longitudinal research design are required to further investigate the nature of contagious influences and to examine how episodes might cluster in time in individual institutions such as schools. The often secretive nature of DSH and the fact that only a relatively small minority of DSH episodes in adolescents in the community (especially those involving self-cutting) come to clinical attention [25, 30, 45] mean that preventative efforts should primarily be based on population-based initiatives directed towards all adolescents. School-based initiatives seem most appropriate [12] and [23, pp. 117–131]. Such initiatives need to include attention to the factors differentially associated with self-cutting and self-poisoning, including the contagious aspects of self-cutting. These might include, for example, open discussion of peer influences, both generally and in relation to DSH, and of alternative methods of dealing with perceived pressure to follow the behaviour of peers.
References
Bancroft J, Hawton K, Simkin S, Kingston B, Cumming C, Whitwell D (1979) The reasons people give for taking overdoses: a further inquiry. Br J Med Psychol 52:353–365
Beautrais AL, Joyce PR, Mulder RT (1997) Precipitating factors and life events in serious suicide attempts among youths aged 13 through 24 years. J Am Acad Child Adolesc Psychiatry 36:1534–1551
Bjarnason T, Thorlindsson T (1994) Manifest predictors of past suicide attempts in a population of Icelandic adolescents. Suicide Life Threat Behav 24:350–358
Brain KL, Haines J, Williams CL (1998) The psychophysiology of self-mutilation: evidence of tension reduction. Arch Suicide Res 4:227–242
Bridge JA, Goldstein TR, Brent DA (2006) Adolescent suicide and suicidal behavior. J Child Psychol Psychiatry 47:372–394
De Leo D, Heller TS (2004) Who are the kids who self-harm? An Australian self-report school survey. Med J Aust 181:140–144
Evans E, Hawton K, Rodham K (2004) Factors associated with suicidal phenomena in adolescents: a systematic review of population-based studies. Clin Psychol Rev 24:957–979
Evans E, Hawton K, Rodham K (2005) In what ways are adolescents who engage in self-harm or experience thoughts of self-harm different in terms of help-seeking, communication and coping strategies? J Adolesc 28:573–587
Evans E, Hawton K, Rodham K, Deeks J (2005) The prevalence of suicidal phenomena in adolescents: a systematic review of population-based studies. Suicide Life Threat Behav 35:239–250
Favazza AR, Rosenthal RJ (1993) Diagnostic issues in self-mutilation. Hosp Community Psychiatry 44:134–140
Ghaziuddin M, Tsai L, Naylor M, Ghaziuddin N (1992) Mood disorder in a group of self-cutting adolescents. Acta Paedopsychiatr 55:103–105
Gould MS, Greenberg T, Velting DM, Shaffer D (2003) Youth suicide risk and preventive interventions: a review of the past 10 years. J Am Acad Child Adolesc Psychiatry 42:386–405
Gould MS, Petrie K, Kleinman MH, Wallenstein S (1994) Clustering of attempted suicide: New Zealand national data. Int J Epidemiol 23:1185–1189
Gould MS, Wallenstein S, Kleinman M (1990) Time-space clustering of teenage suicide. Am J Epidemiol 131:71–78
Gould MS, Wallenstein S, Kleinman MH, O’Carroll P, Mercy J (1990) Suicide clusters: an examination of age-specific effects. Am J Public Health 80:211–212
Harriss L, Hawton K, Zahl D (2005) Value of measuring suicidal intent in the assessment of people attending hospital following self-poisoning or self-injury. Br J Psychiatry 186:60–66
Hawton K (2000) Sex and suicide: gender differences in suicidal behaviour. Br J Psychiatry 177:484–485
Hawton K, Cole D, O’Grady J, Osborn M (1982) Motivational aspects of deliberate self-poisoning in adolescents. Br J Psychiatry 141:286–291
Hawton K, Hall S, Simkin S, Bale E, Bond A, Codd S, Stewart A (2003) Deliberate self-harm in adolescents: a study of characteristics and trends in Oxford, 1990–2000. J Child Psychol Psychiatry 44:1191–1198
Hawton K, Harriss L, Hall S, Simkin S, Bale E, Bond A (2003) Deliberate self-harm in Oxford, 1990–2000: a time of change in patient characteristics. Psychol Med 33:987–996
Hawton K, Harriss L, Simkin S, Bale E, Bond A (2004) Self-cutting: patient characteristics compared with self-poisoners. Suicide Life Threat Behav 34:199–208
Hawton K, James A (2005) Suicide and deliberate self harm in young people. BMJ 330:891–894
Hawton K, Rodham K (2006) By their own young hand: deliberate self-harm and suicidal ideas in adolescents. Jessica Kingsley Publishers, London
Hawton K, Rodham K, Evans E, Harriss L (2009) Adolescents who self harm: a comparison of those go to general hospital and those who do not. Child Adolesc Mental Health 14:24–30
Hawton K, Rodham K, Evans E, Weatherall R (2002) Deliberate self-harm in adolescents: self report survey in schools in England. BMJ 325:1207–1211
Hazell P (1993) Adolescent suicide clusters: evidence, mechanisms and prevention. Aust N Z J Psychiatry 27:653–665
Hjelmeland H, Hawton K, Nordvik H, Bille-Brahe U, De Leo D, Fekete S, Grad O, Haring C, Kerkhof A, Lönnqvist J, Michel K, Salander-Renberg E, Schmidtke A, Van Heeringen K, Wasserman D (2002) Why people engage in parasuicide: a cross-cultural study of intentions. Suicide Life Threat Behav 32:380–393
Horrocks J, Price S, House A, Owens D (2003) Self-injury attendances in the accident and emergency department: clinical database study. Br J Psychiatry 183:34–39
Kerfoot M, Dyer E, Harrington V, Woodham A, Harrington R (1996) Correlates and short-term course of self-poisoning in adolescents. Br J Psychiatry 168:38–42
Madge N, Hewitt A, Hawton K, de Wilde EJ, Corcoran P, Fekete S, Van Heeringen K, De Leo D, Ystgaard M (2008) Deliberate self-harm within an international community sample of young people: comparative findings from the Child and Adolescent Self-harm in Europe (CASE) Study. J Child Psychol Psychiatry 49:667–677
Mann JJ, Waternaux C, Haas GL, Malone KM (1999) Toward a clinical model of suicidal behavior in psychiatric patients. Am J Psychiatry 156:181–189
Mitchell KJ, Ybarra ML (2007) Online behavior of youth who engage in self-harm provides clues for preventive intervention. Prev Med. doi:10.1016/j.ypmed.2007.05.008
Nixon MK, Cloutier PF, Aggarwal S (2002) Affect regulation and addictive aspects of repetitive self-injury in hospitalized adolescents. J Am Acad Child Adolesc Psychiatry 41:1333–1341
O’Carroll PW, Berman AL, Maris RW, Moscicki EK, Tanney BL, Silverman MM (1996) Beyond the Tower of Babel: a nomenclature for suicidology. Suicide Life Threat Behav 26:237–252
O’Loughlin S, Sherwood J (2005) A 20-year review of trends in deliberate self-harm in a British town, 1981–2000. Soc Psychiatry Psychiatr Epidemiol 40:446–453
Plutchik R, van Praag HM (1986) The measurement of suicidality, aggressivity and impulsivity. Clin Neuropharmacol 9:380–382
Robson P (1989) Development of a new self-report questionnaire to measure self esteem. Psychol Med 19:513–518
Rodham K, Hawton K, Evans E (2004) Reasons for deliberate self-harm: comparison of self-poisoners and self-cutters in a community sample of adolescents. J Am Acad Child Adolesc Psychiatry 43:80–87
Roy A, Nielson D, Rylander G, Sarchiapone M (2000) The genetics of suicidal behaviour. In: Hawton K, Van Heeringen K (eds) The international handbook of suicide and attempted suicide. Wiley, Chichester, pp 209–221
Silverman MM, Berman AL, Sanddal ND, O’Carroll PW, Joiner TE Jr (2007) Rebuilding the tower of babel: a revised nomenclature for the study of suicide and suicidal behaviors. Part 2: suicide-related ideations, communications, and behaviors. Suicide Life Threat Behav 37:264–277
Speckens AEM, Hawton K (2005) Social problem-solving in adolescents with suicidal behaviour: a systematic review. Suicide Life Threat Behav 35:365–387
Inc SPSS (2000) SPSS base 10.0 users’ guide. Prentice-Hall, New Jersey
White D, Leach R, Sims R, Atkinson M, Cottrell D (1999) Validation of the hospital anxiety and depression scale for use with adolescents. Br J Psychiatry 175:452–454
Whitlock JL, Powers JL, Eckenrode J (2006) The virtual cutting edge: the internet and adolescent self-injury. Dev Psychol 42:407–417
Ystgaard M, Arensman E, Hawton K, Madge N, Van Heeringen K, Hewitt A, de Wilde EJ, De Leo D, Fekete S (2008) Deliberate self harm in adolescents: comparison between those who receive help following self harm and those who do not. J Adolesc 32(4):875–891
Ystgaard M, Reinholdt NP, Husby J, Mehlum L (2003) Deliberate self harm in adolescents. Tidsskr Nor Laegeforen 123:2241–2245
Zigmond AS, Snaith RP (1983) The hospital anxiety and depression scale. Acta Psychiatr Scand 67:361–370
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hawton, K., Harriss, L. & Rodham, K. How adolescents who cut themselves differ from those who take overdoses. Eur Child Adolesc Psychiatry 19, 513–523 (2010). https://doi.org/10.1007/s00787-009-0065-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00787-009-0065-0