Abstract
Background
Although considered clinically effective, there is little systematic research confirming the use of Individual Psychodynamic Psychotherapy or Family Therapy as treatments for depression in children and young adolescents.
Aims
A clinical trial assessed the effectiveness of these two forms of psychotherapy in treating moderate and severe depression in this age group.
Methods
A randomised control trial was conducted with 72 patients aged 9–15 years allocated to one of two treatment groups.
Results
Significant reductions in disorder rates were seen for both Individual Therapy and Family Therapy. A total of 74.3% of cases were no longer clinically depressed following Individual Therapy and 75.7% of cases were no longer clinically depressed following Family Therapy. This included cases of Dysthymia and “Double Depression” (co-existing Major Depressive Disorder and Dysthymia). There was also an overall reduction in co-morbid conditions across the study. The changes in both treatment groups were persistent and there was ongoing improvement. At follow up six months after treatment had ended, 100% of cases in the Individual Therapy group, and 81% of cases in the Family Therapy group were no longer clinically depressed.
Conclusions
This study provides evidence supporting the use of focused forms of both Individual Psychodynamic Therapy and Family Therapy for moderate to severe depression in children and young adolescents.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Although considered clinically effective, there is little systematic research into the efficacy of Individual Psychodynamic Psychotherapy or Family Therapy in the treatment of depression in children and young adolescents. Most available evidence concerning psychological treatments is for Cognitive Behavioural Therapy (CBT) or Inter-personal Therapy [12]. While CBT is promising in the short-term, previous studies [4, 5, 35] have found high rates of relapse, suggesting the need for continuation or booster treatment. Psychodynamic psychotherapy holds the promise of effecting more lasting changes in childhood depression by improving the capacity to resolve internal and external conflicts over time [25].
With the serious nature of childhood/adolescent depression it is crucial that treatments with efficacy and more than transitory effects, and with the potential for a reduction in the cumulative risks, be provided promptly and skilfully.
There is some evidence to support the use of antidepressant medication in the treatment of childhood depression. Previous placebo-controlled studies have reported response rates to Fluoxetine monotherapy of 52% and 56% [13, 14] in cases of major depression. The TADS study [29] reported a response rate of 60.6% to Fluoxetine monotherapy for Major Depressive Disorder, and 71% when Fluoxetine was combined with CBT. However, the use of Selective Serotonin Re-uptake Inhibitors in the under 18 population is becoming more restricted because of the risk/benefit ratio [8]. It is therefore important to identify alternative treatment modalities for depression in children and young adolescents.
While CBT has been found to be superior to comparison interventions in the treatment of Major Depressive Disorder (MDD) in children/adolescents in 4 out of 6 randomised trials [18], some limitations have been identified: severe cases of depression have not been included, nor were cases with many co-morbid problems such as conduct disorder or repeated self-harm. A number of methodological limitations in the existing research to date were also identified in a review of the treatment research [19].
Muratori et al. [30] have shown that psychodynamic psychotherapy is effective in treating internalising disorders in routine outpatient care; the benefits of such treatment were manifest both immediately and with delayed onset (“sleeper effect”).
A number of factors suggest a place for Family Therapy in the treatment of depression in children. Parents can be important agents for behavioural change, as a positive parental attitude may be a powerful contributor to self-worth in childhood/adolescence [20, 27]. There is now much evidence that the family environment can contribute to childhood depression [11]. Depressed children who live in a confrontational environment also have higher rates of recurrence [2].
There is strong evidence of an association between depression in children and problems in family members, including dysfunctional family relationships [17]. Factors such as high parental criticism, family discord and poor communication between parent and child have been associated with the onset and course of juvenile depressive disorder. Goodyer et al. [16] concluded that psychosocial interventions with first-degree relatives and current close friendships should be considered as part of a treatment strategy for first episode Major Depressive Disorder in children/adolescents.
The aim of this study was to conduct a trial of two established but as yet unvalidated forms of psychotherapy for major depression in childhood/adolescence: (i) Focused Individual Psychodynamic Psychotherapy (“Individual Therapy”) with a focus on interpersonal relationships, life stresses and dysfunctional attachments based on the model of Malan [28] and Davenloo [10] who provide guidelines about psychodynamics, training and techniques in brief dynamic psychotherapy. (ii) Systems Integrative Family Therapy (“Family Therapy”) with a focus on family dysfunction, but without specific attention to unresolved intra-psychic conflicts and early childhood [6, 7, 34]. These treatments were compared in three culturally diverse settings, using a manualised approach.
It was hypothesised that Individual Therapy would be an effective treatment for depression and that improvement would be maintained and ongoing. Family therapy could also be effective in the treatment of depression. Based on the findings of Brent et al. [5] which demonstrated a 37.9% response rate for depression with Family Therapy, it was hypothesised that Family Therapy might not be as effective as Individual Therapy in the treatment of depression.
Further hypotheses were made with regard to the sequence of response (internal change vs social interaction) and predictors of response between the two therapy groups using other measures as well as changes of psychosocial functioning based on the Social Adjustment Scale for Children and the Family Assessment Device. These will be reported in subsequent papers.
Methods
A randomised control trial was conducted in London (Tavistock Clinic), Athens (Aghia Sophia Children’s Hospital) and Helsinki (Children’s Hospital), with 72 patients aged 9–15 years allocated to either Individual Therapy (FIPP) or Family Therapy (SIFT), based on standard randomisation methods. Caseness was the only factor considered at randomisation. Patients in each centre were randomly allocated to one of the two treatments [33].
Ethical approval for the study was obtained locally in each of the three centres. The use of placebo controls was ruled out on ethical grounds [21, 31].
Based on previous studies of therapy with maladjusted children [22, 23], a power calculation was done to detect a difference in outcome of 30% between the two treatment groups. Accordingly, it was expected that 44 patients per group would be required to detect a 30% difference with 80% power, using a 5% test of significance. Following difficulties with recruitment, a further power calculation was carried out based on another review of the literature; using the Brent et al. study [5] sample size as a guide, where there were 35–37 subjects in each treatment arm, the size of the treatment groups in this study was adjusted accordingly.
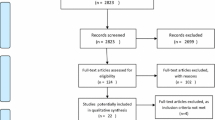
All participants were referred into the study from community Child Mental Health Services. The patients’ progress within the study is illustrated in the CONSORT diagram [3] in Fig. 1.
Entry to the trial followed screening using the Child Depression Inventory [26], a brief self-report measure. Children scoring >13 were included provided they subsequently met criteria for Major Depressive Disorder (MDD) and/or Dysthymia on the Kiddie-SADS [9], a standardised semi-structured diagnostic interview.
Children had to be living with at least one biological parent, and any antidepressants or other psychotropic medication had to have been stopped at least 4 weeks prior to commencement of therapy, to ensure the exclusion of confounding variables.
Exclusion criteria included: depressive disorders meriting urgent hospitalisation, Bipolar and Schizo-affective disorder, severe conduct disorder (considered likely to respond only moderately to psychotherapy) and parents with psychotic disorder or severe personality disorder.
Following screening, 24 cases entered into therapy in each country, divided equally between therapy types in London and Helsinki, with 11 in Individual therapy and 13 in Family therapy in Athens.
Treatment was conducted over a 9-month period and consisted of eight to fourteen 90 min sessions of Family Therapy (mean = 11), or sixteen to thirty 50 min sessions of Individual Therapy (mean = 24.7) plus Individual Parent sessions (one per 2 sessions of child’s psychotherapy) by a separate case worker. There were between 4 and 6 individual therapists, and 4 and 6 family therapists in each of the three centres. The therapists in Athens and Helsinki had received training from the London team prior to the commencement of the study. Treatment manuals were used to ensure comparability across all three centres, supplemented by cross-centre training.
Assessment took place prior to treatment (“Baseline”), at the end of therapy (“End of Therapy”, primary endpoint) and again 6 months later (“Follow up”, secondary endpoint). Patients “lost to follow up” were those who did not return for “End of therapy” or “Follow up” assessment. They had attended a variable number of therapy sessions.
An extensive battery of instruments was administered at each time point (full details available from the authors) collecting information about the child, the parents, their families, as well as relevant school measures. The findings of the following instruments are reported here:
-
1.
The Demography Interview [24]: a semi-structured interview.
-
2.
The Kiddie-SADS [9]: this semi-structured clinical interview provides a measure of Major Depressive Disorder and Dysthymia (based on DSM IV criteria), and psychiatric co-morbidity. These included anxiety disorders (Generalised, Phobias, Separation anxiety and Panic disorder), behavioural disorders (ODD, Conduct disorder), OCD, ADHD and Anorexia nervosa.
-
3.
The Childhood Depression Inventory (CDI) [26]: this 27 item self-report questionnaire indicates the number of depressive symptoms and has a cut off indicating the presence of depression. A score of 13 was used as the threshold for entry into the study, based on research by Garvin et al. [15] for use of the CDI in clinical settings.
-
4.
Moods & Feelings Questionnaire (MFQ, 1): this 16 item self-report questionnaire provides a measure of depression. A threshold of 8 or more defines high scorers.
-
5.
The Children’s Global Assessment Scale (C-GAS, [32]): this clinician rated scale provides a measure of overall impairment of child functioning (range of scores: 0 (lowest) to 100 (highest)).
Statistical analysis
Mixed Model Repeated Measures ANOVA was used to examine the extent of depression (as measured by the continuous instruments CDI, MFQ and C-GAS) at each of the three time points. χ 2 and Exact tests were used for the comparison of the presence/absence of depression using cut-offs and the Kiddie-SADS.
Due to the small sample size in each country, most of the analysis was done for the three countries combined.
With regards to the Kiddie-SADS data, results have been calculated for separate disorders, but since they are known to occur together it was deemed appropriate to adjust the significance level to control for this association. A significance level of P < 0.01 was used therefore instead of P < 0.05. Also the associations between these disorders are stated where applicable, and the significant results using these criteria are reported.
There were four “lost to follow up” cases (1 in Athens, 3 in London, all in the SIFT group). Intention-to-treat analysis principles were applied for these cases, with regard to the K-SADS scores, in order not to weaken the power of the sample size. Last available scores were carried forward. With regard to the CDI and MFQ, we used a “mean substitution” method for dealing with missing data, where feasible and appropriate. Means were calculated for each instrument splitting by centre, time point and therapy type and imputed. Analysis carried out on the pre- and post imputed data sets for each instrument confirmed that this did not change the statistical significance of any of the findings, other than to maintain the power of the sample.
A secondary analysis using Multi-level modelling (ML-WIN) on the pre-imputed data was also carried out on the CDI, MFQ and C-GAS data. The results of this (not presented here) confirmed the findings of the primary analysis. This also allowed us to examine factors related to improvement in each of the therapy groups.
Results
Characteristics of the sample
The mean age of participants was 12 years, almost two thirds (62%) were male, the majority were white and they represented all social class groups (see Table 1). Almost two thirds (62%) came from two-parent families (although not necessarily both biological parents). Just under half (44%) had a history of maternal psychiatric illness while 15% had a history of depression in their extended family (siblings, grandparents, aunts and uncles). Three quarters (76%) had been depressed for more than 6 months.
Overall, the sample characteristics were similar in each therapy type, except for a significantly higher percentage of males in the Individual therapy group (χ 2 = 4.036; df = 1; P < 0.05) and a significant higher prevalence of paternal psychiatric history in the Individual therapy group (χ 2 = 5.449; df = 1; P < 0.05). A possible explanation for these findings is that demographic factors were not taken into consideration at randomisation. These differences may have disappeared had the sample size been larger.
Prevalence of depressive disorders
The prevalence of cases of MDD and/or Dysthymia, only MDD, only Dysthymia and both MDD and Dysthymia (“double depression”) have been examined. This was done to examine any differences in treatment effects in these clinically distinct groups of patients.
Prevalence of Depression (Major Depressive Disorder and/or Dysthymia) before and after therapy based on the Kiddie-SADS
At baseline assessment all the participants were diagnosed as depressed, with either MDD and/or Dysthymia, based on the Kiddie-SADS. By the end of therapy, of those receiving Individual Therapy, 74.3% were no longer diagnosed as depressed and none were diagnosed as depressed at follow up, (see Table 2). Of those receiving Family Therapy, 75.7% of cases of depression had improved by the end of therapy and at follow up only 18.9% were still diagnosed as depressed.
The change in prevalence of depression over the 3 time points in the Individual Therapy group, was statistically significant (χ 2 = 77.537; df = 2; P < 0.001). Further 2 × 2 χ 2 were performed to confirm between which times points the significant changes had occurred. It was found that there was a statistically significant change in prevalence of depression from Baseline to End of Therapy (χ 2 = 41.364; df = 1; P < 0.001), from Baseline to Follow up (χ 2 = 70.00; df = 1; P < 0.001) and also from End of Therapy to Follow up. (χ 2 = 10.328; df = 1; P < 0.001).
The change in prevalence of depression over the 3 time points in the Family Therapy group, was also statistically significant (χ 2 = 60.953; df = 2; P < 0.001). The 2 × 2 χ 2 performed as above found that there was a statistically significant change in prevalence of depression from Baseline to End of Therapy (χ 2 = 45.043; df = 1; P < 0.001), from Baseline to Follow up (χ 2 = 50.455; df = 1; P < 0.001) but not from End of Therapy to Follow up.
The prevalence of depression in the two groups was similar at the end of therapy. At follow-up there were significantly more cases with depression in the Family Therapy group (χ 2 = 7.335; df = 1; P < 0.01). However, when the “lost to follow up” cases were excluded, the prevalence of depression in the Family Therapy group at End of Therapy was 13.4%, and at Follow up 8.1%. The comparison at Follow up between the therapy types was not statistically significant when the “lost to follow up” cases were excluded.
Prevalence of Major Depressive Disorder (MDD) before and after therapy based on the Kiddie-SADS
At the start of therapy more than 90% of the participants were diagnosed as having Major Depressive Disorder (see Table 2). By the end of therapy only 6 (17.1%) still had this diagnosis in the Individual Therapy group and by follow-up none received this diagnosis. In the Family Therapy group, the proportion with a diagnosis of MDD had dropped from 34 (91.9%) at baseline to 8 (21.6%) at the end of therapy and 7 (18.9%) at the follow-up contact.
The reduction in prevalence of MDD over the 3 time points in the Individual Therapy group was statistically significant (χ 2 = 71.595, df = 2; P < 0.001). Further 2 × 2 χ 2 were performed to confirm between which time points the significant changes had occurred. It was found that there was a statistically significant change in prevalence of MDD from Baseline to End of Therapy (χ 2 = 38.914; df = 1; P < 0.001), from Baseline to Follow up (χ 2 = 58.947; df = 1; P < 0.001) but not from End of Therapy to Follow up.
The change in prevalence of MDD over the 3 time points in the Family Therapy group was also statistically significant (χ 2 = 51.371; df = 2; P < 0.001). The 2 × 2 χ 2 performed as above found that there was a statistically significant change in prevalence of MDD from Baseline to End of Therapy (χ 2 = 37.220; df = 1; P < 0.001), from Baseline to Follow up (χ 2 = 39.871; df = 1; P < 0.001) but not from End of Therapy to Follow up.
The prevalence of MDD in the Individual Therapy group compared to the Family Therapy group at End of Therapy was not statistically significant. The prevalence of MDD in the Individual Therapy group compared to the Family Therapy group at Follow up was statistically significant (χ 2 = 7.335; df = 1; P < 0.01). However, this difference resulted from the inclusion of the 4 “lost to follow up” cases in the Family Therapy group (there were no “lost to follow up” cases in the Individual Therapy group). When the “lost to follow up” cases were excluded, the prevalence of MDD in the Individual Therapy group compared to the Family Therapy group at Follow up was not statistically significant.
Prevalence of Dysthymia before and after therapy based on the Kiddie-SADS
At the start of therapy more than 50% of the participants were diagnosed as having Dysthymia (see Table 2). By the end of therapy only 6 (17.1%) still gained a diagnosis of Dysthymia in the Individual Therapy group and by follow-up none received this diagnosis. In the Family Therapy group, the proportion with a diagnosis of Dysthymia had dropped from 20 (54.1%) at baseline to 7 (18.9%) at the end of therapy and 4 (10.8%) at the follow-up contact.
As shown in Table 2, the change in prevalence of Dysthymia over the 3 time points in the Individual Therapy group was statistically significant (χ 2 = 32.308; df = 2; P < 0.001). Further 2 × 2 χ 2 were performed to confirm between which time points the significant changes had occurred. It was found that there was a statistically significant change in prevalence of Dysthymia from Baseline to End of Therapy (χ 2 = 11.993; df = 1; P < 0.005), from Baseline to Follow up (χ 2 = 28.00; df = 1; P < 0.001) but not from End of Therapy to Follow up.
The change in prevalence of Dysthymia over the 3 time points in the Family Therapy group was also statistically significant (χ 2 = 19.425; df = 2; P < 0.001). The 2 × 2 χ 2 performed as above found that there was a statistically significant change in prevalence of Dysthymia from Baseline to End of Therapy (χ 2 = 9.855; df = 1; P < 0.005), from Baseline to Follow up (χ 2 = 15.787; df = 1; P < 0.001) but not from End of Therapy to Follow up.
The prevalence of Dysthymia in the Individual Therapy group compared to the Family Therapy group at End of Therapy was not statistically significant. This was also the case at Follow up.
Prevalence of “Double Depression” (Major Depressive Disorder and Dysthymia) before and after therapy based on the Kiddie-SADS
At the start of therapy 48.6% in the Individual Therapy group and 45.9% in the Family Therapy group were diagnosed as having double depression (see Table 2). By the end of therapy only 3 (8.6%) still gained a diagnosis of double depression in the Individual Therapy group and by follow-up none received this diagnosis. In the Family Therapy group, the proportion with a diagnosis of double depression had dropped from 17 (45.9%) at baseline to 6 (16.2%) at the end of therapy and 4 (10.8%) at the follow-up contact.
As shown in Table 2, the change in prevalence of double depression over the 3 time points in the Individual Therapy group was statistically significant (χ 2 = 30.512; df = 2; P < 0.001). Further 2 × 2 χ 2 were performed to confirm between which time points the significant changes had occurred. It was found that there was a statistically significant change in prevalence of double depression from Baseline to End of Therapy (χ 2 = 13.720; df = 1; P < 0.001), from Baseline to Follow up (χ 2 = 22.453; df = 1; P < 0.001) but not from End of Therapy to Follow up.
The change in prevalence of double depression over the 3 time points in the Family Therapy group was also statistically significant (χ 2 = 14.389; df = 2; P = 0.001). The 2 × 2 χ 2 performed as above found that there was a statistically significant change in prevalence of double depression from Baseline to End of Therapy (χ 2 = 7.633; df = 1; P < 0.01), from Baseline to Follow up (χ 2 = 11.236; df = 1; P < 0.005) but not from End of Therapy to Follow up.
The prevalence of double depression in the Individual Therapy group compared to the Family Therapy group at End of Therapy was not statistically significant, and this remained the case at Follow up.
Additional measures of depression:
Childhood Depression Inventory (CDI)
There was a significant difference in the mean CDI scores for both therapy groups at the different time points, with the scores going down for both types of therapy (see Table 3, P < 0.001, power > 99%). There was no significant difference between the Individual Therapy and Family therapy groups by Follow up. There was a slightly significant difference between the 2 therapy groups over time (P < 0.05, power < 80%).
In the Individual Therapy group, the mean drop in CDI score from Baseline to End of Therapy was 7.77, with a further drop of 5.49 from End of Therapy to Follow up (Total drop: 13.26). In the Family Therapy group, the mean drop in CDI score from Baseline to End of Therapy was 13.08, but with only a further mean drop of 1.18 from End of Therapy to Follow up. (Total drop: 14.26).
Secondary analysis using ML WIN confirmed the above findings.
Moods & Feelings Questionnaire (MFQ)
There was a significant difference in the mean MFQ scores for both therapy groups at the different time points, with the scores going down for both types of therapy (see Table 3, P < 0.001, power > 99%). There was a slightly significant difference between the Individual Therapy and Family therapy groups by Follow up (P < 0.05) but at low power (52%). There was also a slightly significant difference between the 2 therapy groups over time (P < 0.05).
In the Individual Therapy group, the mean drop in MFQ score from Baseline to End of Therapy was 6.21, with a further drop of 2.34 from End of Therapy to Follow up. (Total drop: 8.55) In the Family Therapy group, the mean drop in MFQ score from Baseline to End of Therapy was 9.95, but with only a further mean drop of 1.19 from End of Therapy to Follow up. (Total drop: 11.14)
Measure of impairment/level of functioning
Children’s Global Assessment Scale (C-GAS)
There was a significant difference in the mean C-GAS scores for both therapy groups at the different time points, with the scores increasing for both types of therapy (see Table 3, P < 0.001, power > 99%). There was no significant difference between the Individual Therapy and Family therapy groups by Follow up. There was also no significant difference between the 2 therapy groups over time, specifically at End of Therapy.
In the Individual Therapy group, the mean rise in C-GAS score from Baseline to End of Therapy was 16.13, with a further rise of 3.84 from End of Therapy to Follow up (Total rise: 19.97). In the Family Therapy group, the mean rise in C-GAS score from Baseline to End of Therapy was 17.05, with a further rise of 2.03 from End of Therapy to Follow up (Total rise: 19.08).
Secondary analysis using ML WIN confirmed the above findings.
Co-morbidity
The presence of co-morbid conditions was assessed using the Kiddie-SADS (based on DSM IV criteria).
The change in prevalence of cases with co-morbidity over the 3 time points in the Individual Therapy group, as depicted in Table 4, was statistically significant (χ 2 = 19.821; df = 2; P < 0.001). The change in prevalence of cases with co-morbidity over the 3 time points in the Family Therapy group was not statistically significant, because of the absence of any decrease from End of Therapy to Follow up. The prevalence of cases with co-morbidity in the Individual Therapy group compared to the Family Therapy group at each of the three time points, however, was not statistically significant.
Discussion
In this study the following was found:
In the Individual Therapy group, 74.3% of cases were no longer clinically depressed following therapy, and 100% of cases were no longer clinically depressed 6 months later. Individual therapy appears to have been effective in cases of Major Depressive Disorder, Dysthymia and “double depression”. This effectiveness appears to have been persistent, with no relapses 6 months following therapy. In addition, all remaining cases of depression (MDD, Dysthymia, and “double depression”) had resolved at the follow-up point. This suggests an ongoing response to therapy following completion, the sleeper effect.
In the Family Therapy group, 75.7% of cases were no longer clinically depressed following therapy, and 81% of cases were no longer clinically depressed 6 months later. Family therapy also appears to have been effective in cases of Major Depressive Disorder, Dysthymia and “double depression”. This effectiveness appears to have been persistent, with no relapses 6 months following therapy. In addition, further improvement in some of the remaining cases of depression (MDD, Dysthymia and “double depression”) was found at the follow-up point, particularly in cases of Dysthymia and “double depression”.
Response rates for depression in the Individual Therapy and Family Therapy groups were not significantly different by End of Therapy. While response rates appear to have been approximately 20% greater in the Individual Therapy group, compared to the Family Therapy group, at Follow up, this is very largely influenced by the inclusion of the four “lost to follow up” cases in the Family Therapy group, who were considered as unsuccessfully treated cases following therapy. Without these four cases, the differences in response rates between the two groups are not statistically significant.
In addition to improvement as measured by cases no longer meeting diagnostic criteria for Major Depressive Disorder or Dysthymia, similar improvement was found in both treatment groups in terms of level of impairment and level of functioning.
While final outcome appears to have been similar in the two groups in many respects, the results from the CDI and MFQ suggest a different pattern of response or improvement. With regard to the MFQ, the Family Therapy group had a lower score at End of Therapy, despite having had a higher score than the Individual Therapy group at Baseline. While the power of this test was low (<80%), it does reflect the slightly different “path” for each of the therapy groups.
The Family Therapy group appears to have made greater improvement, in some respects, by End of Therapy, compared to the Individual Therapy group. These differences, though, had disappeared by Follow up.
By Follow up, many of the Family Therapy trajectories appear to have plateaued, while the Individual Therapy group trajectories suggest the possibility of further, and possibly more rapid, improvement to follow.
The population groups in the three countries appear to have responded similarly to the treatment. Although not presented here, virtually no significant differences were found when similar analysis was done comparing the three treatment centres (London, Athens, Helsinki), in terms of response rates and patterns.
A significant number of cases in both therapy groups had co-morbid conditions. Almost a third of cases in the study had 3 or more co-morbid conditions. Following therapy, there was a decrease in co-morbid conditions, particularly anxiety disorders and conduct disorders, which are often associated with depressive disorders. This occurred in both therapy groups.
The results of this study suggest both Individual Therapy (response rate 74% by End of Therapy) and Family therapy (response rate 75% by End of Therapy) may be more effective in the treatment of depression than other forms of treatment. Previous studies have found a response rate in the region of 60% to CBT [5] and 52–56% to Fluoxetine [13, 14] and 71% to CBT and Fluoxetine combined [29]. A NNT analysis was undertaken using the End of Therapy results in this study. Using the Placebo data in the TADS study as a comparator, the NNT for both Individual Therapy and Family Therapy is 3. This compares favourably with the NNTs reported in the TADS study, where the NNT for Fluoxetine and CBT combined was 3, Fluoxetine was 4 and CBT was 12. In the absence of a control group in our study, a NNT analysis was also conducted using the Nondirective supportive therapy (NST) group from the Brent study [5] as an alternative comparator. The NNT for both Individual therapy and Family therapy was 6. It is important to note in both the Individual and Family therapy groups, further improvement was reported at Follow up. We would therefore expect to find lower NNTs at the Follow up point, were comparable data available.
The chronicity and severity of the depression in our study led us to believe that spontaneous remission was unlikely to have occurred in the vast majority of cases, particularly in light of the extent of co-existing dysthymia. Furthermore, the TADS study demonstrated a response rate of only 35% to placebo. The Brent/Birmaher study [4, 5] found that CBT did not confer any long-term advantage over family therapy or supportive therapy with regard to rates of remission, recovery, recurrence or level of functioning. In that study, the median onset of recurrence was 4 months after recovery, whereas in this study, there had been no recurrences, and ongoing improvement, 6 months post psychotherapy. Further research will explore which components of the therapy were significant.
Conclusions
Analysis has shown that both Focused Individual Psychodynamic Psychotherapy (with Parent support work) and Systems Integrative Family Therapy were both effective in treating moderate to severe depression in children and young adolescents in three countries.
This includes cases of dysthymia and “double depression” which are generally considered to be more difficult to treat. There has also been an overall reduction in co-morbid conditions across the study.
Clinical implications
-
1.
This study provides evidence supporting the use of both Individual Psychodynamic Therapy and Family Therapy in this age group.
-
2.
It may be possible for trained therapists, with the help of the manuals, to deliver effectively, these focused forms of therapy.
-
3.
Both treatments also appear to be exportable to wider settings in culturally diverse populations.
Limitations
-
1.
The study is limited by the sample size, which was influenced by recruitment difficulties. This becomes even more significant when comparing smaller sub-groups e.g. countries, and therapy groups within countries.
-
2.
The effect of the 4 “lost to follow up” cases is also significant, especially in relation to the total sample size, and more so, because all of them were in the Family Therapy group. Intention to treat analysis principles were used in order not to lessen the power of the study or over-rate the effect of the treatments.
-
3.
The absence of an “untreated” control group limits the study’s ability to prove with certainty the efficacy of the therapies provided.
Further research
Further analysis will be looking at whether differential predictors of response can be identified in the two therapy groups, and whether there are any significant differences across the three different cultural settings. Data from additional instruments about the child, his/her parents and family, and his/her environment will provide further insight into the current findings. It will also be important to establish if any specific components of the respective forms of therapy were likely to have contributed to the patients’ response. Further studies should take measures to counteract the limitations as discussed above. Other factors to consider would include gender distribution and family mental health history, as well as user preference for therapy type.
References
Angold A, Costello EJ, Pickles A, et al. (1987) The development of a questionnaire for use in epidemiological studies of depression in children and adolescents. Institute of Psychiatry, London University, London
Asarnow JR, Tompson M, Hamilton EB, et al. (1994) Family-expressed emotion, childhood-onset depression, and childhood-onset schizophrenia spectrum disorders: is expressed emotion a non-specific correlate of child psychopathology or a specific risk factor for depression? J Abnorm Child Psychol 22:129–146
Begg C, Cho M, Eastwood S, et al. (1996) Improving the quality of reporting of Randomised Controlled Trials. The CONSORT statement. JAMA 276:637–639
Birmaher B, Brent D, Kolko D, et al. (2000) Clinical outcome after short-term psychotherapy for adolescents with major depressive disorder. Arch Gen Psychiatry 57(1):29–36
Brent DA, Holder D, Kolko D, et al. (1997) A clinical psychotherapy trial for adolescent depression comparing cognitive, family, and supportive therapy. Arch Gen Psychiatry 54:877–885
Byng-Hall J (1995) Re-writing family scripts: improvisation and systems change. Guilford Press, New York & London
Byng-Hall J, Campbell DC (1981) Resolving conflicts in distance regulation: an integrative approach. J Marital Fam Ther 7:321–330
Committee on Safety of Medicines (CSM) (2003) Selective Serotonin Re-uptake Inhibitors (SSRIs): overview of regulatory status and CSM advice relating to major depressive disorder (MDD) in children and adolescents including a summary of available safety and efficacy data: http://medicines.mhra.gov.uk/ourwork/monitorsafequalmed/safetymessages/ssrioverview_101203.htm
Chambers W, Puig-Antich J, Hirsch M, et al. (1985) The assessment of affective disorders in children and adolescents by semi-structured interview: test–retest reliability of the Schedule for Affective Disorders and Schizophrenia for school-age children, present episode version. Arch Gen Psychiatry 42:696–702
Davenloo H (1978) Basic principles and techniques in short term dynamic psychotherapy. Spectrum Publications, New York
Diamond G, Serrano A, Dickey M, et al. (1995) Current status of family-based outcome and process research. J Am Acad Child Adolesc Psychiatry 35(1):6–16
Elkin I, Shea MT, Watkins JT, et al. (1989) National Institute of Mental Health treatment of depression collaborative research program, general effectiveness of treatment. Arch Gen Psychiatry 46:971–983
Emslie GJ, Rush AJ, Weinberg WA, et al. (1997) A double-blind, randomised placebo-controlled trial of fluoxetine in children and adolescents with depression. Arch Gen Psychiatry 54:1031–1037
Emslie GJ, Heiligenstein JH, Hoog S, et al. (2000) Fluoxetine for acute treatment of depression in children and adolescents: a placebo controlled, randomised clinical trial. Paper presented at 39th Annual Meeting of the American College of Neuropsychopharmacology, December 10–14, 2000, San Juan, Puerto Rico
Garvin V, Leber D, Kalter N (1991) Children of divorce: predictors of change following preventive intervention. Am J Orthopsychiatry 61(3):438–447
Goodyer IM, Herbert J, Secher SM, et al. (1997) Short-term outcome of major depression: I. Comorbidity and severity at presentation as predictors of persistent disorder. J Am Acad Child Adolesc Psychiatry 36:179–187
Harrington R, Dubicka B (2002) Adolescent depression: an evidence-based approach to intervention. Curr Opin Psychiatry 15:369–375
Harrington R, Whittaker J, Shoebridge P (1998a) Psychological treatment of depression in children and adolescents. A review of treatment research. Br J Psychiatry 173(10):291–298
Harrington R, Whittaker J, Shoebridge P, et al. (1998b) Systematic review of efficacy of cognitive behaviour therapies in childhood and adolescent depressive disorder. Br Med J 316:1559–1563
Harter S (1990) Causes, correlates and the functional role of global self-worth: a life-span perspective. In: Sternberg RJ, Kolligian J (eds) Competence considered. Yale University Press, New Haven, pp 67–97
Kazdin AE (1986) Comparative outcome studies of psychotherapy: methodological issues and strategies. J Consult Clin Psychol 54:95–105
Kolvin I, Garside RE, Nicol AR, et al. (1981/5) Help starts here: the maladjusted child in the ordinary school Tavistock Publications, London
Kolvin I, MacMillan A, Nicol AR, et al. (1988) Psychotherapy is effective. J R Soc Med 261–266
Kolvin I, Barrett L, Bhate SR, et al. (1991) The Newcastle child depression project: diagnosis and classification of depression. Br J Psychiatry 159(11):9–21
Kolvin I, Trowell J, Tsiantis J et al (1999) Psychotherapy for childhood depression. In: Maj M, Sartorius N (eds) Evidence and experience in psychiatry, WPA Series, vol 1. John Wiley & sons Ltd
Kovacs M (1981) Rating scales to assess depression in school aged children. Acta Paedopsychiatr 46:305–315
Kovacs M, Bastiaens LJ (1995) The psychotherapeutic management of major depressive and dysthymic disorders in childhood and adolescence, issues and prospects. In: Goodyer IM (ed) The depressed child and adolescent. Cambridge University Press, Cambridge
Malan DH, Osimo F (1992) Psychodynamics, training and outcome in brief psychotherapy. Butterworth, London
March J, Silva S, Petrycki JC, et al. (2004) Fluoxetine, Cognitive-Behavioural Therapy, and their combination for adolescents with depression. Treatment for Adolescents with Depression Study (TADS) Randomised Controlled Trial. J Am Med Assoc 292(7):807–820
Muratori F, Picchi L, Bruni G, et al. (2003) A two-year follow-up of psychodynamic psychotherapy for internalising disorders in children. J Am Acad Child Adolesc Psychiatry 42(3): 331–339
Parloff MB (1986) Placebo controls in psychotherapy research: a sine qua non or a placebo for research problems. J Consult Clin Psychol 54:79–87
Shaffer D, Gould MS, Brasic J (1993) A children’s global assessment scale (C GAS). Arch Gen Psychiatry 40:1228–1231
Tsiantis J, Kolvin I, Anastasopoulos D, et al. (2005) Psychotherapy for early adolescent depression (PEAD): a comparison of two psychotherapeutic interventions in three European countries. In: Hibbs ED, Jensen P (eds) Psychosocial treatments for child and adolescent disorders: empirically based strategies for clinical practice. American Psychological Association, Washington, DC, pp 267–293
Will D, Wrate RM (1985) Integrated Family Therapy. Tavistock Publications, London
Wood A, Harrington R, Moore A (1996) Controlled trial of brief cognitive behavioural intervention in adolescent patients with depressive disorders. J Clin Psychol Psychiatry 37:737–746
Acknowledgements
Members of the London project team: Anne Alvarez, Sarah Barratt, Vicky Bianco, Susan Bliss, David Campbell, Jane Cassidy, Lois Colling, Carol Desousa (statistician), Emilia Dowling, Elspeth Earle, Anna Fitzgerald, Henia Goldberg, Inge Gregorious, Agathe Gretton, Judith Loose, Ryan Lowe, Sue McNab, Gillian Miles, Renos Papadopoulos, David Pentacost, Maria Rhode, Margaret Rustin.
Members of the Athens project team: Alexandra Alexopoulou, Evi Athanassiadou, Maria Belivanaki, Vaso Chantzara, Stelios Christogiorgos, Kostas Francis, Dimitris Georgiadis, Georgios Gritzelas, Terpsi Korpa, Olga Lanara, Effie Lignos, Dimitris Magriplis, Maria Marangidi, Olga Maratos, Vasso Moula, Valeria Pomini, Eleni Stavrou, Marianna Tassi, Irene Tsanira, L. Tsarouhi.
Members of the Helsinki project team: Christina Bostrom, Taru Forst, Reija Graeffe, Susanne Friman, Kaarina Hastbacka, Liisa Hisinger, Eija Korpinen, Anna Kuikka, Sakari Lehtonen, Helena Lounavaara-Rintala, Kaija Mankinen, Pirkko Pingoud, Liisa Pirhonen, Marja Schulman, Esko Varilo, Leena Varilo, Maija von Fieandt, Pirjo Vuornos, Jan-Christer Wahlbeck, Hanna Westerinen.
We would also like to thank the young people and their families for their contribution to the study.
This study was partly funded by the European Community: Concerted action contract No. BMH4-CT98-3231 DG12-SSMI. Central co-ordination of the project took place at the Tavistock Clinic, London. Prof Kolvin was funded whilst developing the project by the Leverhulme Foundation.
Author information
Authors and Affiliations
Corresponding author
Additional information
Original lead researcher: Prof Issy Kolvin (deceased).
Rights and permissions
About this article
Cite this article
Trowell, J., Joffe, I., Campbell, J. et al. Childhood depression: a place for psychotherapy. Eur Child Adolesc Psychiatry 16, 157–167 (2007). https://doi.org/10.1007/s00787-006-0584-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00787-006-0584-x