Abstract
Objectives
To evaluate the effect of enhancement tools of intraoral digital radiographs on the assessment of vertical root fracture (VRF) and to quantify the resultant image noise.
Materials and methods
Thirty single-rooted human teeth (15 control and 15 fractured) were each radiographed in four intracanal conditions: no filling, gutta-percha, metal post, and fiberglass post, totaling 120 original images. Two filters were applied to the original images—Sharpen filter (SF) and Edge Enhancement filter (EE), and brightness and contrast were adjusted in four combinations (B&C1 to 4), resulting in 840 images. Five oral radiologists analyzed the images for VRF detection. Pixel intensity was obtained in two regions from the radiographs. Diagnostic values were calculated and compared by two-way ANOVA, and the SD values of pixel intensity values were compared by one-way ANOVA (α = 0.05).
Results
There were no significant differences in accuracy for VRF detection between the experimental groups (p > 0.05). Teeth with metal post presented the lowest sensitivity (p < 0.05) for all experimental conditions, except for SF and EE (p > 0.05). B&C2, B&C3, and B&C4 had higher specificity than SF (p ≤ 0.05) for all intracanal conditions. Analysis of pixel intensity showed that all enhanced images presented statistically significant higher noise compared to those of the original images (p ≤ 0.05).
Conclusion
Digital enhancement tools in digital radiography increase image noise; however, they can be used without compromising VRF detection.
Clinical relevance
The use of digital enhancement does not impair the detection of VRF and, therefore, can be applied for this purpose according to the observer preference.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Vertical root fracture (VRF) is a challenging clinical condition, and its diagnosis involves both clinical and imaging assessment. Clinically, the patient might present symptoms such as pain, swelling, deep probing defects, and tooth mobility [1] that can be misdiagnosed as a periodontal disorder. Radiographically, visualization of the fracture line is not always possible due to little or absent separation of the fragments and/or image overlapping [2]. This difficulty on the diagnostic task leads to a complex decision making situation when VRF is suspected. If VRF is confirmed, tooth extraction is indicated; otherwise, the investigation continues while patient keeps feeling discomfort and pain [3]. Many efforts have been directed towards developing and/or improving diagnostic tools for more accurate VRF diagnosis. Cone beam computed tomography (CBCT) has been extensively studied to improve VRF detection, but its accuracy remains low [3], especially in endodontically treated cases [1, 4,5,6] due to the presence of artifacts. In addition, VRF investigation requires higher resolution of CBCT scans, which results in an overall relatively higher radiation dose compared to intraoral radiography [2].
Intraoral digital radiography is widely used in dental practice. In addition to lower radiation cost, another advantage of digital radiology is the possibility of image enhancement [7]. Digital enhancement is widely performed in image visualization software programs in an attempt to improve image interpretation, and mostly comprises image filters, and brightness and contrast (B&C) adjustments.
Recent studies analyzed the influence of different levels of B&C adjustment on the assessment of proximal caries [8] and root resorptions [9] and did not find any significant impact on diagnostic performance. Unlike caries and root resorptions that are depicted on radiographs as gradients of shades of gray related to their etiopathogenesis, VRFs are expected to present high-contrast radiolucent fracture lines. The degree of separation of root fragments is variable, which affects the detection of those fracture lines [10]. The application of image filters and/or the variation of B&C could enhance the diagnosis of VRF. Previous studies have evaluated the influence of digital filters on the detection of VRF and recommended the use of “Sharpen” filter for this diagnostic task [11]. The enhancement of digital images has a direct impact on image pixels, modifying its original values to provide the expected result, whether it is a B&C adjustment or filter application [12]. The change in pixel values can result in an increase of image noise due to the high difference of surrounding pixels, which may affect image diagnosis [13, 14].
Considering the advances in imaging technology, it is of utmost importance to direct research into the use of the available enhancement tools that can act on the images to increase detection and early VRF diagnosis, without further exposures to the patient, following the ALADA (as low as diagnostically acceptable) principle [15]. In clinical practice, these digital enhancement tools are used according to the observers’ preferences, and their influence on the assessment of VRF in teeth with different intracanal materials has not been compared yet. Therefore, the aim of this study was to assess the effect of the post-processing enhancement tools of intraoral digital radiographs on the assessment of VRF with different intracanal materials, as well as to quantify the resulting image noise. The null hypothesis was that the use of digital enhancement does not influence the diagnostic accuracy of VRF or the image noise.
Materials and methods
Sample preparation
After local institutional ethics committee approval (protocol number #2.057.024), 30 single-rooted extracted human teeth were collected, cleaned, and disinfected to compose the study sample. Exclusion criteria consisted of teeth with endodontic treatment, pulp calcifications, incomplete root formation, or root resorptive lesions. Root canals were instrumented with Mtwo NiTi (VDW, Munich, Germany) through their full length with the sequence of instrumentation 30.05/35.04/40.04/25.07. With a low-speed bur no. 2 (Exacto, Angelus, Londrina, Brazil), two thirds of the root canal length was prepared for intracanal post placement. Teeth were decoronated at the cementoenamel junction using a diamond saw (Isomet 1000, Lake Bluff, IL, USA) to avoid memorization during radiographic evaluations. VRF was induced in half of the sample by introducing a conical metal tip of an Instron machine (Instron, Canton, MA, USA), set at 500 N and 1 mm/min, into the canal entrance. Teeth were placed in a 10-mm-diameter hole of an acrylic resin block, and the metal tip stopped automatically once the fracture occurred [6]. This technique leads to root fractures without displacement of the fragments.
Image acquisition
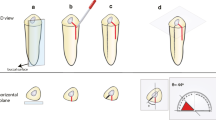
All teeth were individually placed in a socket of a dry human mandible section, and a custom-made acrylic device was used to maintain reproducible exposure geometry according to the paralleling technique. Images were acquired in a direct digital intraoral system with a size 2 CMOS sensor, DigoraToto (Soredex, Tuusula, Finland), X-rayed with Focus (Instrumentarium, Tuusula, Finland), at 70 kVp, 7 mA, and exposure time of 0.063 s. The focus-receptor distance was fixed at 40 cm, and an acrylic plate (25 mm thick) was placed between the X-ray tube and the teeth to simulate soft tissue scatter [16]. An aluminum step-wedge (eight steps with 2-mm-thick increments) was positioned adjacent to the mandible to standardize the gray values of the initial images, following the methodology proposed by Nascimento et al. (2018) [8].
Each tooth was radiographed in four different experimental intracanal conditions: no filling, gutta-percha, metal post (cobalt-chromium alloy), and fiberglass post (Exacto, Angelus, Londrina, Brazil). The intracanal materials were cautiously placed inside the root canal to keep the same radiographic geometry in all acquisitions. No root sealer was used in order to allow the replacement of intracanal materials between image acquisitions of the same tooth and to avoid filling the fracture line. Metal and fiberglass posts had the same dimensions. A total of 120 initial radiographs were acquired (30 teeth × 4 intracanal conditions).
Image preparation and assessment
Experimental groups were composed of the original images and each of the post-processing enhancement tools applied. The acquired images were displayed in the radiographic system software Digora for Windows 2.6 (Soredex, Tuusula, Finland) and exported in TIFF format, 8-bit depth, and with two image filters: Sharpen filter (SF) and Edge Enhancement (EE). Both filters were applied only once. Additionally, density and contrast of the original images were verified with aid of the aluminum step-wedge in ImageJ software (National Health Institute, Bethesda, MD, USA), and four controlled adjustments of B&C were performed (B&C1, − 30% brightness and + 30% contrast; B&C2, − 15% brightness and + 15% contrast; B&C3, + 15% brightness and − 15% contrast; and B&C4, + 30% brightness and − 30% contrast), according to a previous study [8] (Table 1). Thus, a total of 840 images were generated and divided into seven experimental groups: Original, SF, EE, B&C1, B&C2, B&C3, and B&C4 (Fig. 1).
Five oral and maxillofacial radiologists assessed the images. The observers were previously trained and calibrated regarding the VRF diagnosis. Images were randomized and assessed independently by the observers in JPEGView software (www.jpegview.sourceforge.net), which were blinded to the digital enhancements applied, on a 24.1-in. LCD display (1920 × 1080 pixels, MDRC-2124, Barco N.V., Courtray, Belgium) in a dimly lit room. For each image, observers had to evaluate the presence of VRF and score it in a 5-point scale as (1) absent, (2) probably absent, (3) uncertain, (4) probably present, and (5) present.
To avoid visual fatigue, the observers were asked to assess a maximum of 50 images per day and to maintain an interval of 3 days between sessions. Thirty days after the end of the evaluations, 30% of the sample was re-assessed to verify reproducibility.
An objective image quality evaluation was also performed to measure image noise after application of the digital enhancement tools. Standard deviation of pixel values (SD) has been used to measure the difference caused by the digital enhancement tools regarding image noise [13]. For that, images were imported into ImageJ software, and two 5 × 5 mm regions of interest (ROI) were registered and reproduced in the original and enhanced images. ROI 1 was placed in the fourth step (8 mm thick) of the aluminum step-wedge as a reference of a homogenous structure, and ROI 2 was placed in the alveolar bone (Fig. 2). The SD of the ROIs was measured and recorded for the experimental groups.
Statistical analysis
Data were analyzed in GraphPad Prism version 7.05 (GraphPad Software, La Jolla, CA, USA). Intra- and inter-observer agreement were calculated by the weighted Kappa test. The area under the ROC curve was performed for diagnostic accuracy (Az), sensitivity, and specificity values, which were compared by two-way ANOVA (enhancement tools × intracanal materials), with Tukey’s post hoc test. One-way ANOVA (enhancement tools) with Tukey’s post hoc test was used to compare the noise of the step-wedge and bone. The significance level adopted was 5% (α = 0.05). The power analysis was 0.75 based on the mean minimum differences among the groups and the mean standard deviation (Biostat software, v. 5.3, Instituto de Desenvolvimento Sustentável Mamirauá, Tefé, Amazonas, Brazil).
Results
The mean values of accuracy, sensitivity, and specificity for all intracanal conditions and experimental group variations are presented in Table 2. Teeth with intracanal fiberglass posts presented higher accuracy compared to teeth with no filling (p ≤ 0.05) for Original (0.64 vs 0.58, respectively) and SF (0.60 vs 0.47, respectively). No differences were found between the accuracy of the original (ranging from 0.58 to 0.64, depending on intracanal condition) and digitally enhanced images (ranging from 0.47 to 0.66) (p > 0.05); thus, the first null hypothesis was accepted. In general, metal post sensitivity was lower (ranging from 0.21 to 0.50) than that of the other intracanal conditions (p ≤ 0.05) for all experimental conditions, except for the image filters (SF = 0.47 and EE = 0.50, p > 0.05). The SF presented higher sensitivity (0.47–0.61) for VRF detection compared to B&C4 (0.21–0.45) in filled teeth (p ≤ 0.05). Specificity was higher for metal post in comparison to that of teeth with no filling (p ≤ 0.05) in all experimental groups. B&C2 (from 0.69 to 0.84), B&C3 (from 0.67 to 0.83), and B&C4 (from 0.71 to 0.88) had higher specificity than that of SF (ranging from 0.43 to 0.60) for all intracanal conditions (p ≤ 0.05).
The analysis of image quality showed that all digitally enhanced images presented statistically significant higher noise compared to the original images (p ≤ 0.05) for both ROIs; thus, the second null hypothesis was rejected. For ROI 1, placed at the aluminum step-wedge, EE presented the highest noise value, statistically different from B&C3, B&C4, and SF (p ≤ 0.05), while B&C3 presented the lowest value, different from all other groups, except for B&C4 (p > 0.05) (Fig. 3a). For ROI 2, the noise in B&C1, B&C2, and B&C3 was lower than in B&C4, SF, and EE (p ≤ 0.05) (Fig. 3b).
Graphs of the pixel intensity SD values according to the region of interest and experimental groups. a The SD values of pixel intensity on the aluminum step-wedge. b The SD values of pixel intensity on the alveolar bone. Different letters above the bars indicate a statistically significant difference between the experimental groups.
The mean intra-observer agreement values ranged from poor (0.24) to moderate (0.51), and the inter-observer agreement values ranged from poor (0.03) to reasonable (0.31), according to Landis and Koch [17].
Discussion
Detecting a fracture line on radiographs is not a straightforward task, as shown in our results: overall low mean sensitivity (0.43) and accuracy (0.58), as well as low mean intra-observer (0.35) and inter-observer agreements (0.2). Similar results have been found in previous studies that used digital periapical radiography for VRF detection, with sensitivity ranging from 0.09 to 0.68 and accuracy from 0.53 to 0.80 [1, 2, 4, 18,19,20,21]. Intra- and inter-observer agreements are also low, ranging from 0.20 to 0.38 and from 0.02 to 0.49, respectively [1,2,3, 19, 21]. Overall specificity in our study was somewhat higher than other diagnostic values (0.71), which is also similar to previous results (0.75 to 0.97) [1, 2, 4, 18,19,20,21].
Our first hypothesis was that the use of digital enhancement could positively influence diagnosis of VRF. However, there was no influence for either filters or B&C adjustments on the accuracy. In other words, the digital enhancement tools applied were not capable to overcome the limitations of periapical radiography in the detection of root fractures. Due to superimposition of anatomical structures inherent to the radiographic technique, the fracture line would only be detected if the X-ray beam was parallel to the fracture plane, especially in cases without separation of root fragments. Furthermore, the presence of intracanal material can mask the fracture line [1, 3, 19, 22, 23].
Some results may draw attention at first impression, such as the accuracy of the intracanal fiberglass posts being higher than that of the teeth with no filling for Original and SF groups. Mostly, the higher accuracy was an effect of the higher specificity in those cases (as observed statistically in the SF group). This can probably be associated with the fact that these posts do not have enough radiopacity to cover the fracture image or, in few cases, facilitate detection when the fracture line was located at its limits. In contrast, the greater specificity shown by metal post groups in comparison with groups with no filling can be attributed to the overlapping of images between the post (totally radiopaque) and the VRF, which possibly leads to the tendency of the “absence of VRF” response. This increases both the number of true negatives and false negatives, which reflects high specificity and low sensitivity, respectively, as observed in the metal post group.
Contrast reduction, as in B&C4, reduces differentiation between structures, which leads to lower sensitivity when compared to the SF in cases of filled teeth. In these cases, higher sharpness as a result of the SF may have facilitated the detection of the fracture line, even when a post or gutta-percha was present.
Concerning the use of digital enhancement, no previous study had assessed the EE filter for the VRF assessment. Barayan et al. [24] analyzed the effect of image filters (e.g., inversion, histogram equalization, and polynomial) on the diagnosis of horizontal root fractures in digital periapical radiographs and found that none of those influenced the diagnosis. Other studies assessed different filters in the diagnosis of VRF (e.g., reverse-contrast, colorization, sharpness, zoom-in-magnification, and pseudo-3D) [25, 26] and found no significant influence on the performance for VRF detection, corroborating with our results. Controversially, another study [11] assessed filters for VRF detection and found an increase on diagnostic accuracy for the Sharpen filter. This fact led us to compare the application of SF to the other digital enhancements; however, such improvement in VRF assessment was not observed in the present study. Unlike the present study, these authors [11] assessed only teeth without intracanal material, which may have led to the higher accuracy. Studies that have used digital subtraction radiography to evaluate the accuracy in the diagnosis of VRF [21, 27] verified that such image analysis technique offers an acceptable diagnostic accuracy and, therefore, can be considered when VRF is suspected. However, this technique was not able to improve the diagnostic accuracy. Additionally, the radiographs used for subtraction process must present the same features (brightness, contrast, and acquisition geometry) and are acquired in distinct moments. Therefore, limitations of periapical radiography regarding acquisition standardization in clinical practice affect the subtraction and may not be feasible as a daily routine [27].
Information on the effect of each filter on pixels is not provided by the manufacturer. However, as observed in this and previous studies, EE filter increases the contrast between structures along the outlines of the image while SF increases the contrast-to-noise ratio by grouping high-contrast pixels, thus increasing the contrast between structures and smoothing more homogeneous areas [11, 28]. All digital enhancements presented higher noise on both aluminum step-wedge and bone than original images. This means that the noise is increased when images are post-processed. In part, this result was expected since previous studies found an increase in noise as the sharpness was increased [13, 29]; however, surprisingly, B&C adjustments also affected image noise. While brightness influences the overall darkening (or brightening) of the image, contrast alters the nuances of gray values. Mostly, the contrast may have influenced the noise occurrence in the images because of its more direct impact in between adjacent structures; however, as these changes were applied jointly, it was not possible to assess their isolated effect on image noise. The changes in gray values were caused by contrast and brightness tools. Noise was higher in SF than in B&C adjustments. As SF specificity was lower for all intracanal conditions than that of B&C2, B&C3, and B&C4, it may be speculated that noise appearance in the image leads to false positive cases and, therefore, reduced specificity. Another factor observed was that the same filter or B&C adjustment resulted in different means of pixel intensity SD when different structures were evaluated. Thus, the effect of digital enhancement and noise in different structures and diagnostic tasks could be assessed in future studies.
When contrast is increased, all pixel values are shifted to the extremes of the gray scale, i.e., dark pixels get darker and bright pixels get brighter; thus, it changes the mean gray value of a ROI [12]. An increase in contrast results in the increase of the difference between the gray values of the fracture line and adjacent root dentin [12]. Furthermore, reduced brightness may also result in the enhancement of radiolucent areas, such as the fracture line. However, these features were not sufficient to have a positive impact on the diagnostic accuracy.
It is necessary to consider the individual visual perception of the observers, which results in personal preferences for different filters or levels of B&C of the images. Levels of B&C in this study were adjusted within a pre-set range and not freely chosen by the observers. Since no differences in diagnostic performance were found between the different post-processing enhancement tools, these tools can be applied according to the observers’ preference in clinical practice, without compromising diagnostic accuracy, for SF, EE, and within the limits of the tested levels for B&C (+ 30 to − 30%).
In vitro radiographic studies focus on the detection of the radiolucent fracture lines and do not reproduce the whole clinical scenario. Diagnosis of VRF involves the assessment of other clinical signs and symptoms (e.g., sinus tract, pain and/or swelling, and deep, narrow, isolated periodontal pocket) and indirect radiographic signs (e.g., radiolucent areas adjacent to the roots).
Conclusion
In conclusion, the diagnostic accuracy for VRF detection is low, and the use of enhancement tools in digital radiography increases image noise and does not aid or impair its detection. Therefore, it may be used according to the observer’s preference.
References
Patel S, Brady E, Wilson R, Brown J, Mannocci F (2013) The detection of vertical root fractures in root filled teeth with periapical radiographs and CBCT scans. Int Endod J 46:1140–1152. https://doi.org/10.1111/iej.12109
Bechara B, McMahan CA, Noujeim M et al (2013) Comparison of cone beam CT scans with enhanced photostimulated phosphor plate images in the detection of root fracture of endodontically treated teeth. Dentomaxillofac Radiol:42. https://doi.org/10.1259/dmfr.20120404
Brady E, Mannocci F, Brown J, Wilson R, Patel S (2014) A comparison of cone beam computed tomography and periapical radiography for the detection of vertical root fractures in nonendodontically treated teeth. Int Endod J 47:735–746. https://doi.org/10.1111/iej.12209
Khedmat S, Rouhi N, Drage N, Shokouhinejad N, Nekoofar MH (2012) Evaluation of three imaging techniques for the detection of vertical root fractures in the absence and presence of gutta-percha root fillings. Int Endod J 45:1004–1009. https://doi.org/10.1111/j.1365-2591.2012.02062.x
Talwar S, Utneja S, Nawal RR, Kaushik A, Srivastava D, Oberoy SS (2016) Role of cone-beam computed tomography in diagnosis of vertical root fractures: a systematic review and meta-analysis. J Endod 42:12–24. https://doi.org/10.1016/j.joen.2015.09.012
Gaêta-Araujo H, Silva de Souza GQ, Freitas DQ, de Oliveira-Santos C (2017) Optimization of tube current in cone-beam computed tomography for the detection of vertical root fractures with different intracanal materials. J Endod 43:1668–1673. https://doi.org/10.1016/j.joen.2017.04.003
Choi J-W, Han W-J, Kim E-K (2014) Image enhancement of digital periapical radiographs according to diagnostic tasks. Imaging Sci Dent 44:31–35. https://doi.org/10.5624/isd.2014.44.1.31
Nascimento EH, Gaêta-Araujo H, Vasconcelos KF et al (2018) Influence of brightness and contrast adjustments on the diagnosis of proximal caries lesions. Dentomaxillofac Radiol 47:20180100. https://doi.org/10.1259/dmfr.20180100
Nascimento EHL, Gaêta-Araujo H, Galvão NS, Moreira-Souza L, Oliveira-Santos C, Freitas DQ (2019) Effect of brightness and contrast variation for detectability of root resorption lesions in digital intraoral radiographs. Clin Oral Investig 23:3379–3386. https://doi.org/10.1007/s00784-018-2764-8
Makeeva IM, Byakova SF, Novozhilova NE, Adzhieva EK, Golubeva GI, Grachev VI, Kasatkina IV (2016) Detection of artificially induced vertical root fractures of different widths by cone beam computed tomography in vitro and in vivo. Int Endod J 49:980–989. https://doi.org/10.1111/iej.12549
Nascimento HAR, Ramos ACA, Neves FS, de-Azevedo-Vaz SL, Freitas DQ (2015) The ‘Sharpen’ filter improves the radiographic detection of vertical root fractures. Int Endod J 48:428–434. https://doi.org/10.1111/iej.12331
Güneri P, Lomçali G, Boyacioǧlu H, Kendir S (2005) The effects of incremental brightness and contrast adjustments on radiographic data: a quantitative study. Dentomaxillofac Radiol 34:20–27. https://doi.org/10.1259/dmfr/85029529
Brasil DM, Yamasaki MC, Santaella GM, Guido MCZ, Freitas DQ, Haiter-Neto F (2019) Influence of VistaScan image enhancement filters on diagnosis of simulated periapical lesions on intraoral radiographs. Dentomaxillofac Radiol 48:20180146. https://doi.org/10.1259/dmfr.20180146
Kal BI, Baksi BG, Dündar N, Şen BH (2007) Effect of various digital processing algorithms on the measurement accuracy of endodontic file length. Oral Surge Oral Med Oral Pathol Oral Radiol Endodontol 103:280–284. https://doi.org/10.1016/j.tripleo.2006.06.001
Bushberg JT (2015) Eleventh annual Warren K. Sinclair keynote address—science, radiation protection and NCRP: building on the past, looking to the future. Health Phys 108:115–123. https://doi.org/10.1097/HP.0000000000000228
Vasconcelos K d F, Rovaris K, Nascimento EHL et al (2017) Diagnostic accuracy of phosphor plate systems and conventional radiography in the detection of simulated internal root resorption. Acta Odontol Scand 75:573–576. https://doi.org/10.1080/00016357.2017.1359331
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Shintaku WH, Venturin JS, Noujeim M, Dove SB (2013) Comparison between intraoral indirect and conventional film-based imaging for the detection of dental root fractures: an ex vivo study. Dent Traumatol 29:445–449. https://doi.org/10.1111/edt.12041
Chavda R, Mannocci F, Andiappan M, Patel S (2014) Comparing the in vivo diagnostic accuracy of digital periapical radiography with cone-beam computed tomography for the detection of vertical root fracture. J Endod 40:1524–1529. https://doi.org/10.1016/j.joen.2014.05.011
Ferreira LM, Visconti MAPG, Nascimento HA, Dallemolle RR, Ambrosano GM, Freitas DQ (2015) Influence of CBCT enhancement filters on diagnosis of vertical root fractures: a simulation study in endodontically treated teeth with and without intracanal posts. Dentomaxillofac Radiol 44:2–7. https://doi.org/10.1259/dmfr.20140352
Queiroz PM, Nascimento HAR, Da Paz TDJ et al (2016) Accuracy of digital subtraction radiography in the detection of vertical root fractures. J Endod 42:896–899. https://doi.org/10.1016/j.joen.2016.03.003
Kambungton J, Janhom A, Prapayasatok S, Pongsiriwet S (2012) Assessment of vertical root fractures using three imaging modalities: cone beam CT, intraoral digital radiography and film. Dentomaxillofac Radiol 41:91–95. https://doi.org/10.1259/dmfr/49798768
Khasnis S, Kidiyoor K, Patil A, Kenganal S (2014) Vertical root fractures and their management. J Conserv Dent 17:103–110. https://doi.org/10.4103/0972-0707.128034
Barayan M, Nasseh I, Geha N, Noujeim M (2017) The effects of imaging enhancement tools in the detection of horizontal root fractures. J Clin Diagn Res 11:98–101. https://doi.org/10.7860/JCDR/2017/26775.10490
Tofangchiha M, Bakhshi M, Shariati M, Valizadeh S, Adel M, Sobouti F (2012) Detection of vertical root fractures using digitally enhanced images: reverse-contrast and colorization. Dent Traumatol 28:478–482. https://doi.org/10.1111/j.1600-9657.2012.01120.x
Kamburòlu K, Murat S, Pehlivan SY (2010) The effects of digital image enhancement on the detection of vertical root fracture. Dent Traumatol 26:47–51. https://doi.org/10.1111/j.1600-9657.2009.00841.x
Mikrogeorgis G, Eirinaki E, Kapralos V et al (2017) Diagnosis of vertical root fractures in endodontically treated teeth utilising digital subtraction radiography: a case series report. Aust Endod J. https://doi.org/10.1111/aej.12240
Belém MDF, Ambrosano GMB, Tabchoury CPM, Ferreita-Santos RI, Haiter-Neto F (2013) Performance of digital radiography with enhancement filters for the diagnosis of proximal caries. Braz Oral Res 27:245–251. https://doi.org/10.1590/S1806-83242013000300004
Clark JL, Wadhwani CP, Abramovitch K, Rice DD, Kattadiyil MT (2018) Effect of image sharpening on radiographic image quality. J Prosthet Dent 120:1–7. https://doi.org/10.1016/j.prosdent.2018.03.034
Funding
This study was financed in part by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior-Brasil (CAPES)-Finance Code 001.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in this study were conducted in accordance with the ethical standards of the institutional Research Ethics Committee of the Piracicaba Dental School, UNICAMP (#2.057.024) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gaêta-Araujo, H., Nascimento, E.H.L., Oliveira-Santos, N. et al. Effect of digital enhancement on the radiographic assessment of vertical root fractures in the presence of different intracanal materials: an in vitro study. Clin Oral Invest 25, 195–202 (2021). https://doi.org/10.1007/s00784-020-03353-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-020-03353-x