Abstract
Objectives
Clinical and microbiological longitudinal changes in individuals with peri-implant mucositis (PM) with or without preventive maintenance therapy (PMT) have not been reported, especially in long periods of monitoring. This 5-year follow-up study aimed to assess the clinical and microbiological changes along time in individuals initially diagnosed with PM.
Materials and methods
Eighty individuals diagnosed with PM (T1) and followed during 5 years (T2) were divided into one group with PMT during the study period (GTP; n = 39) and another group without PMT (GNTP; n = 41). Full-mouth periodontal/peri-implant examinations were performed. Peri-implant microbiological samples were collected and analyzed through qPCR for Tannerella forsythia, Treponema denticola, Porphyromonas gingivalis, Prevotella intermedia, Fusobacterium nucleatum, and Actinomyces naeslundii at T1 and T2.
Results
GNTP presented higher incidence of peri-implantitis than GTP. Moreover, GNTP showed significantly higher total bacterial load and higher frequency of the evaluated orange complex bacteria than GTP. Individuals who progressed to peri-implantitis presented significantly higher total bacterial load and higher frequencies of P. gingivalis, T. denticola, and F. nucleatum.
Conclusions
The absence of regular appointments for PMT was associated with a higher incidence of peri-implantitis and a significant increase in total bacterial load.
Clinical relevance
Regular visits during PMT positively influenced subgingival microbiota and contributed to peri-implant homeostasis and clinical status stability during a 5-year monitoring period. Compliance with PMT programs should be reinforced among individuals rehabilitated with dental implants.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Peri-implant mucositis (PM) is a reversible inflammatory condition whose main clinical characteristic is bleeding on probing. Erythema, swelling, and/or suppuration may also be present. On the other hand, peri-implantitis (PI) is an irreversible plaque-associated pathological condition occurring in tissues around dental implants, characterized by inflammation in the peri-implant mucosa and subsequent progressive loss of supporting bone [1].
Regular appointments for preventive maintenance therapy (PMT) aim to maintain the health of peri-implant tissues in long term [2, 3]. In a systematic review of nine studies, no evidence of an appropriate frequency for PMT visits was determined [4]. However, regular appointments have been classified as those visits with intervals up to 1 year [5]. In recent studies, the lack of regularity in PMT visits was identified as a risk factor for the occurrence of PI [6,7,8,9]. Furthermore, the concept of reversibility of PM is still not fully clear. Experimental PM in men showed a healing time longer than 3 weeks to achieve pre-experimental levels of mucosal health after plaque control was reinstituted [10]. This topic underscores the need for PMT and rigorous plaque control for patients with PM or even peri-implant health.
Subgingival microbioma studies revealed that a group of bacteria, especially Tannerella forsythia, Treponema denticola, Porphyromonas gingivalis, Prevotella intermedia, Fusobacterium nucleatum, Campylobacter rectus, Prevotella nigrescens, Eubacterium nodatum, and Peptostreptococcus micros, have an important role in periodontitis (PE) [11,12,13].
Additionally, microbiological reviews have shown that the peri-implant microbioma, whether in health or disease, is similar to that around teeth [13,14,15,16,17]. Periodontal pathogens found in sites with PE are often found in implants with PI [16,17,18]. An increase in bacteria counts such as T. forsythia, T. denticola, P. gingivalis, P. intermedia, and F. nucleatum was identified in implants with PI [19,20,21,22]. Cross-sectional and case-control studies suggested that the microbiota around implants with PI is much more complex and diverse than that found in teeth with PE [17, 18, 23,24,25]. However, few longitudinal studies have assessed changes in peri-implant microbiota [26, 27]. It is important to notice that some assessments were performed only for short periods of time (up to 12 months).
Although some studies with different methodologies [24, 28, 29] reported findings on microbiological peri-implant diseases, to the best of our knowledge, clinical and microbiological longitudinal changes in individuals under PM in the absence or presence of PMT have not been reported, especially in long periods of time.
Hence, the objective of the present study was to evaluate, in a longitudinal period of 5 years, the peri-implant condition and the differences in the frequencies of T. forsythia, T. denticola, P. gingivalis, P. intermedia, F. nucleatum, and Actinomyces naeslundii in individuals initially diagnosed with PM in the presence and absence of PMT.
Materials and methods
Study design and sampling strategy
The sample for the present follow-up study was obtained from a previous study designed to identify the prevalence of peri-implant diseases and potential associated risk factors among partially edentulous individuals rehabilitated with dental implants [30]. In accordance with ethical principles, all participants were informed of their oral health and referred to the Federal University of Minas Gerais (UFMG), Brazil, for free treatment, or instructed to seek dental care elsewhere.
After a 5-year period, a large task force was employed for the recruitment of the 212 initial participants through direct approach, telephone calls, telegrams, emails, and/or text messages. Thus, 80 individuals who were diagnosed with PM at the initial examination (T1—year 2006) were recovered and underwent a new periodontal/peri-implant clinical examination and microbiological collection (T2—year 2011). These individuals were divided into two groups: one with preventive maintenance therapy during the study period (those carrying out regular PMT with dental visits at least once a year (GTP; n = 39)) and another one without preventive maintenance therapy (GNTP; n = 41). Individuals diagnosed with peri-implant health and peri-implantitis at T1 were not analyzed due to the lower recovery rate and insufficient sample size for analysis. By these means, this study is not a randomized clinical trial but a 5-year follow-up.
The sampling procedure, the inclusion and exclusion criteria, the data collection, the peri-implant, and the periodontal clinical examinations are summarily presented in study flowchart (Fig. 1) and were described in details elsewhere [6].
The present study was approved by the Research Ethics Committee from the UFMG, Brazil (protocol no. 05650203000-10).
Peri-implant clinical examination
The following clinical parameters for four peri-implant sites in each implant were evaluated according to the methodology proposed by Ferreira et al. [30]: suppuration, peri-implant probing depth (PDi), bleeding on probing (BOPi), and plaque index (PLI) around all implants.
Periodontal clinical examination
Also in accordance with Ferreira et al. [30], complete periodontal examinations were performed and included plaque index, periodontal probing depth (PD), clinical attachment level (CAL), and bleeding on periodontal probing (BOP) for four sites in each tooth.
All clinical parameters were measured at dental and peri-implant sites using manual periodontal probe (PCP-UNC 15, Hu-Friedy, Chicago, IL, USA).
Preventive maintenance procedures
During interviews at T2, special attention was given to the occurrence and frequency of periodontal and peri-implant preventive maintenance within the 5 years following T1. Frequency of PMT was determined by self-reported information and confirmed in dental records (GTP group: at least five dental visits during the evaluation period (mean 5.6 ± 0.3 visits); GNTP group: absence of dental visits during the evaluation period). During PMT visits, the following procedures were performed: (1) periodontal and peri-implant status assessment, (2) application of disclosing agents and oral hygiene instructions, and (3) coronal prophylaxis and non-surgical and surgical mechanical debridement, when necessary.
Diagnostic criteria
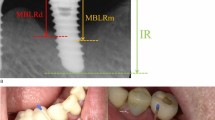
Peri-implant mucositis was defined as the presence of visual inflammation and BOPi. Peri-implantitis was defined as the presence of PDi ≥ 5 mm associated with BOPi and/or suppuration with peri-implant bone loss [30]. Cases where the radiographs did not confirm the peri-implant bone loss were diagnosed as PM. It should be noted that these definitions have been re-confirmed and updated according to the recent definition proposed in the recent World Workshop of American Academy of Periodontology and European Federation of Periodontology [1].
Microbiological collection and analyses
Subgingival samples were collected at T1 and T2 in eight peri-implant sites, two in each quadrant (the peri-implant sites with the higher PDi associated with BOPi were evaluated at both times), for each individual as previously reported [31].
Quantification of the total number of bacterial cells, A. naeslundii, P. gingivalis, T. forsythia, T. denticola, P. intermedia, and F. nucleatum was carried out by quantitative real-time polymerase chain reaction (qPCR) using TaqMan assay (TaqMan® Universal PCR Master Mix II, Life Technologies, Carlsbad, USA). The following primers/probes were designed using a primer software (software Primer3 online, Simgene, Hamilton, Canada) and were previously described [32]. A. naeslundii (forward: GTCTCAGTTCGGATCGGTGT; reverse: CCGGTACGGCTACCTTGTTA; probe: TACGTTCTCGGGCCTTGTAC), P. gingivalis (forward: ACCTTACCCGGGATTGAAATG; reverse: CAACCATGCAGCACCTACATAGAA; probe: VICATGACGATGGTGAAAACCGTCTTCCCTTCTAMRA), T. forsythia (forward: AGCGATGGTAGCAATACCTGTC; reverse: TTCGCCGGGTTATCCCTC; probe: 6FAMCACGGGTGAGTAACGTAMRA), T. denticola (forward: CCGAATGTG CTCATTTACATAAAGGT; reverse: GATACCCATCGTTGCCTTGGT; probe: 6FAMATGGGCCCGCGTCCCATTAGC TAMRA), P. intermedia (forward: 5′ AAT ACC CGA TGT TGT CCA CA 3′; reverse: 5′ TTA GCC GGT CCT TAT TCG AA 3′; probe: 5′ TGA CGT GGA CCA AAG ATT CAT CGG TGG A 3′), F. nucleatum (forward: GCAGCTTCAAATGATTCGAGTA; reverse: AAGCTTGGTAAAGGCTCTGAAG; probe TTGAAATAAAGAAGAAAAATGGAGG), and universal (forward: TGGAGCATG TGGTTTAATTCGA; reverse: TGCGGGACTTAACCCAACA; probe: VICCACGAG CTGACGACAAGCCATGCATAMRA) in an ABI 7500 Fast Real-Time PCR System® (Life Technologies, Carlsbad, USA) following manufacturer’s instructions in 20-μl reactions.
The absolute quantification of the target organism was determined by the plotting of the cycle threshold (Ct) value obtained from each clinical sample against a standard curve generated with a known concentration of gDNA of reference bacterial strains in 10-fold serial dilutions. Negative control (purified PCR-grade water instead of the DNA template) was included in all PCR.
Statistical analysis
A univariate analysis for all comparisons between GNTP and GTP groups was performed using chi-square, Fischer’s exact, Mann-Whitney, and Wilcoxon tests, when appropriate.
For the analyses of bacteria counts and bacterial complexes, natural logarithm (exponent) was used due to number size. This logarithm was used to evaluate bacterial frequency (by average and standard deviation) at the two examination times (T1 and T2) in the GTP and GNTP groups. Supplementary to that and following a normal data distribution, marginal linear models were performed to compare the bacterial counts and the bacterial complexes at T1 and T2, between groups and diagnostics (PM and PI), adjusting for the following potential confounders: smoking, diabetes, and plaque index.
The outliers were identified through the standardization of the results, so that the average of the variable was 0 and the standard deviation was 1. For this purpose, observations with standardized scores outside the range of 3.29 were considered outliers.
Statistical analyses were performed using the R software (Windows OS, version 3.2.0), and the results were considered statistically significant if p value < 0.05%.
Results
The characteristics of the sample at T1 and T2 are presented in Table 1. Individuals in the GNTP group had significantly higher values of plaque index when compared to GTP after 5 years (1.9 ± 0.5 vs. 1.4 ± 0.7; p = 0.001). Additional data on the periodontal/peri-implant clinical parameters in relation to variables of interest were previously reported by Costa et al. [6].
There was a significantly higher incidence of PI in GNTP (43.9%) than in GTP (18%) group. It is noteworthy that patients with PI in GTP, despite maintenance and necessary surgical treatment, still persisted with PI diagnosis in the final exam. All subjects (n = 12) who presented PM resolution at T2 were in the GTP group. There was an increase in the number of individuals with PE in GNTP when comparing T1 (22.0%) with T2 (41.5%) (Table 1).
Table 2 reports intra-group comparisons between T1 and T2 of the total bacterial load (TBL) and the isolated frequency of each pathogen, the frequency of the red complex (T. forsythia, P. gingivalis, and T. denticola), and the frequency of the two bacteria evaluated in the orange complex (sum of the counts of P. intermedia and F. nucleatum) in the unadjusted and adjusted models.
In the GTP group, there was a significant decrease in TBL, in the frequency of the bacteria analyzed in the orange complex, and in the isolated frequency of T. forsythia, P. gingivalis, P. intermedia, and A. naeslundii at T2 (unadjusted and adjusted models). Additionally, there was a significant increase in the isolated frequency F. nucleatum (unadjusted model) at T2 (Table 2).
In intra-group comparisons, there was a significant increase in TBL, in the frequency of the bacteria analyzed in the orange complex, and in the isolated frequencies of P. gingivalis, P. intermedia, and F. nucleatum in GNTP. There was an increase in the frequency (unadjusted model) of the red complex and A. naeslundii (Table 2).
Inter-group comparisons (adjusted for smoking, diabetes, and plaque index), as well as the changes in peri-implant diagnosis from T1 to T2, are presented in Figs. 2 and 3.
Comparisons of the frequency of T. forsythia, P. gingivalis, T. denticola, P. intermedia, F. nucleatum, and A. naeslundii: intra- and inter-group, and between diagnosis at each evaluation time, controlling for smoking, diabetes, and plaque index. PM peri-implant mucositis, PI peri-implantitis, GTP periodontal/peri-implant maintenance therapy group, GNTP no periodontal/peri-implant maintenance therapy group (marginal linear models)
Comparisons of total bacterial load, red complex, and two representative bacteria of the orange complex: intra- and inter-group, and between diagnosis at each evaluation time, controlling for smoking, diabetes, and plaque index. PM peri-implant mucositis, PI peri-implantitis, GTP periodontal/peri-implant maintenance therapy group, GNTP no periodontal/peri-implant maintenance therapy group (marginal linear models)
At T2, individuals diagnosed with PM and PI in the GNTP group presented a significantly higher TBL when compared to GTP. In both groups, individuals who progressed from PM to PI showed a significant increase in TBL. The GTP individuals who remained with PM showed a decrease in TBL (Fig. 3).
The analysis of the isolated frequencies of T. forsythia, P. gingivalis, T. denticola, P. intermedia, F. nucleatum, and A. naeslundii is presented in Fig. 2. Comparisons of total bacterial load, red complex, and two representative bacteria of the orange complex are presented in Fig. 3. The results showed that there were no significant differences between groups in the frequency of the red complex and in the isolated frequency of T. forsythia (Fig. 3). At T2, individuals with PM and PI in the GNTP group had a significantly higher frequency of P. gingivalis. Individuals who progressed from PM to PI showed a significant increase in the frequency of P. gingivalis in GNTP. The GTP individuals who remained with PM showed a decrease in the frequency of P. gingivalis. In the GTP and GNTP groups, individuals diagnosed with PI showed a higher frequency of P. gingivalis when compared to those diagnosed with PM at T2. Individuals with PI in the GNTP group presented a higher frequency of T. denticola at T2 when compared to individuals with PM (Fig. 2).
The frequencies of the bacteria analyzed in the orange complex (sum of P. intermedia and F. nucleatum) (Fig. 3) and P. intermedia (Fig. 2) were significantly lower in individuals with PM in the GTP group at T1 and T2, as in individuals with PI at T2. Individuals who remained with PM in GNTP showed a significant increase in the frequency of these bacteria in the orange complex, while in GTP, there was a significant decrease (Fig. 3). P. intermedia presented a significantly higher frequency in individuals with PI in GNTP (Fig. 2). The isolated frequency F. nucleatum analysis showed that, in both groups, individuals who developed PI showed higher frequencies of these bacteria. At T2, PI individuals in both groups showed an increase in the isolated frequency F. nucleatum when compared to individuals with PM (Fig. 2).
Among individuals diagnosed with PM at T2, the frequency of A. naeslundii was significantly lower in the GTP group. Individuals with PM at T2 and who performed periodontal/peri-implant maintenance (GTP group) showed a significant decrease in the frequency of A. naeslundii (Fig. 2).
Discussion
The results of the present study showed that individuals in the GNTP group presented higher incidence of PI, higher plaque index at T2, higher TBL, and higher counts of the majority of the evaluated bacteria. These findings should be highlighted and corroborate previous studies signaling that higher plaque index and absence of PMT [4, 21, 29, 33], and consequently a greater presence of pathogens for extended periods could collaborate for the increased incidence of PI [27, 34, 35]. Thus, the higher TBL and plaque index in GNTP can hypothetically suggest that the increase in the number of pathogens that could migrate to peri-implant sites can be a risk factor for the development of PI [13,14,15, 17].
Specifically, the increased frequency of the two pathogens evaluated in the orange complex and also some isolated species (P. gingivalis, P. intermedia, and F. nucleatum) in GNTP, and the reduction in TBL and in the frequencies of T. forsythia, P. gingivalis, and P. intermedia, in GTP, suggested that the absence of PMT can impact on the amount of pathogens found around implants. An important aspect of these findings also suggest that, in the present study sample, the quantitative characteristics of peri-implant microbiota appear to be more important than qualitative characteristics, confirming the results from previous studies [3, 25, 36]. However, surprising findings were also observed as a significant increase in the isolated frequency of F. nucleatum and a decrease in A. naeslundii in the GTP group.
The fact that all individuals who presented remission of PM were in the group that performed PMT also reinforces the importance of routine visits to peri-implant disease control, especially PM, since it is regarded as a pathological condition that is reversible only with clinical treatment [6, 37]. Additionally, as reported by Salvi et al. [10], PM may require a strict plaque control over 3 weeks for returning to levels of gingival and peri-implant mucosal health.
Results from the present study confirm data from the literature on the importance of regular PMT visits in the control of peri-implant diseases [7, 9, 37, 38]. The absence of PMT was also associated with increased risk of developing PI in recent systematic reviews [4, 37, 38].
Microbiological results from the present study were adjusted for potential confounders for periodontal and peri-implant diseases, such as smoking, diabetes, and plaque index. These confounding variables can, by themselves, affect the microbiological findings [12]. However, comparisons with other findings are limited because few studies have assessed these associations on dental implants [19, 29, 33].
Differences in TBL and in the isolated frequency of some pathogens were reported when comparing individuals diagnosed with PM and PI. Individuals who had a poorer peri-implant condition over time presented more TBL in both groups (GTP and GNTP), and also an increase in the frequency of P. gingivalis and F. nucleatum, supported by previous findings [19]. Conflicting results were reported in a study where levels of P. gingivalis and F. nucleatum were not associated with the presence of PI [28]. Findings from the present study showed no significant increase in the red complex bacteria among individuals who progressed to PI compared to individuals with PM. Nevertheless, when the pathogens were analyzed isolatedly, a higher frequency of P. gingivalis, T. denticola, and F. nucleatum was found in individuals with PI at T2. Similar results were described in studies with short periods of monitoring [13, 29, 39, 40].
While bacteria of the red and orange complexes are often associated with the presence of PE and the increase of probing depth, the blue complex has not been related to the presence of periodontal disease [11]. Healthy implants usually have a microbiota consisting of gram-positive bacteria, bacilli, and coccus [14, 34, 39, 41]. However, Renvert et al. [19] found no differences between the microbiota of teeth compared to healthy implants.
Recently, the steps of biofilm formation were reviewed [42]. Actinomyces species and the oral Streptococci are the primary bacteria to stick in the acquired film and interact with each other by favoring the colonization of both secondary colonizers as F. nucleatum and the red complex. Therefore, as the biofilm increases in thickness or in quantity, there is a gradual growth that later becomes constant for several species, including primary colonizers [43]. In teeth, for example, Actinomyces species may be most prevalent in both the supra and subgingival biofilm and both in health and periodontal disease [13, 44]. This could hypothetically explain the reduction of the A. naeslundii and increase of the F. nucleatum in the GTP group. However, there are great challenges in the interpretation of studies on subgingival biofilm in a multifactorial manner. Nevertheless, it is important to note that any change in the environment can have an impact on the microbiota (increase and/or reduction of species), which in turn is capable of inducing changes in the host’s response, generating an amplification loop of the periodontal disease process [45].
Hence, the present study showed that after 5 years, there was a trend of increased frequency of pathogens in implants that progressed to PI and in individuals with PM who were not regular in PMT. Despite that, there are great challenges in the interpretation of studies on subgingival biofilm in a multifactorial manner [45]. Therefore, PMT can be an important tool to generate positive impacts on the subgingival microbiota.
To the best of our knowledge, this is the first study on the frequency of different pathogens in the presence or absence of PMT in individuals diagnosed with PM accompanied during 5 years, which can be considered a long monitoring period. Few longitudinal studies on monitoring bacterial profile are found in the literature, and most monitoring periods and samples are short [10, 14, 15, 46,47,48,49].
The present study has the limitation of evaluating few bacterial species that are commonly associated with PE and related to PI. In this sense, other PI-related pathogens may have been overlooked, since there are reports of other bacterial species that are not commonly listed in the pathogenesis of PE, but were found in sites with PI [24]. However, the peri-implantitis microbiome is commensal-depleted and pathogen-enriched, harboring traditional and new pathogens. The core peri-implant microbiome harbors taxa from genera often associated with periodontal inflammation [48, 49]. Thus, additional clinical and microbiological longitudinal studies, since the installation of the implant, are required in order to verify the probable bacterial succession that occurs in implants that are subject to the development of PI and its association with different risk factors.
Conclusions
It might be concluded that there was a significant longitudinal increase in TBL, in the frequencies of P. gingivalis, P. intermedia, and the two pathogens evaluated in the orange complex in GNTP. On the other hand, these same pathogens and T. forsythia showed a reduction in GTP. Additionally, individuals who progressed from PM to PI showed significantly higher TBL and frequencies of P. gingivalis, T. denticola, and F. nucleatum. Consequently, it was observed a beneficial role of PMT in maintaining peri-implant clinical stability and homeostasis of the microbiological condition.
References
Berglundh T, Armitage G, Araujo MG, Avila-Ortiz G, Blanco J, Camargo PM, Chen S, Cochran D, Derks J, Figuero E, Hämmerle CHF, Heitz-Mayfield LJA, Huynh-Ba G, Iacono V, Koo KT, Lambert F, McCauley L, Quirynen M, Renvert S, Salvi GE, Schwarz F, Tarnow D, Tomasi C, Wang HL, Zitzmann N (2018) Peri-implant disease and conditions: consensus report of workgroup 4 of the 2017 World Workshop on the classification of periodontal and peri-implant disease and conditions. J Clin Periodontol 45:S286–S291. https://doi.org/10.1111/jcpe.12957
Salvi GE, Cosgarea R, Sculean A (2017) Prevalence and mechanisms of peri-implant diseases. J Dent Res 96:31–37. https://doi.org/10.1177/0022034516667484
Hultin M, Komiyama A, Klinge B (2007) Supportive therapy and the longevity of dental implants: a systematic review of the literature. Clin Oral Implants Res 18s:50–62. https://doi.org/10.1111/j.1600-0501.2007.01447.x
Monje A, Aranda L, Diaz KT, Alarcon MA, Bagramian RA, Wang HL, Catena A (2016) Impact of maintenance therapy for the prevention of peri-implant diseases: a systematic review and meta-analysis. J Dent Res 95:372–379. https://doi.org/10.1177/0022034515622432
Costa FO, Vieira TH, Cortelli SC, Cota LOM, Costa JE, Aguiar MCF, Cortelli JR (2018) Effect of compliance during periodontal maintenance therapy on levels of bacteria associated with periodontitis: a 6-year prospective study. J Periodontol 89:519–530. https://doi.org/10.1002/JPER.17-0173
Costa FO, Takenaka-Martinez S, Cota LO, Ferreira SD, Silva GL, Costa JE (2012) (2012) Peri-implant disease in subjects with and without preventive maintenance: a 5-year follow-up. J Clin Periodontol 39:173–181. https://doi.org/10.1111/j.1600-051X.2011.01819.x
Pjetursson BE, Helbling C, Weber HP, Matuliene G, Salvi GE, Bragger U, Schmidlin K, Zwahlen M, Lang NP (2012) Peri-implantitis susceptibility as it relates to periodontal therapy and supportive care. Clin Oral Implants Res 23:888–894. https://doi.org/10.1111/j.1600-0501.2012.02474.x
Aguirre-Zorzano LA, Estefania-Fresco R, Telletxea O, Bravo M (2015) Prevalence of peri-implant inflammatory disease in patients with a history of periodontal disease who receive supportive periodontal therapy. Clin Oral Implants Res 26:1338–1344. https://doi.org/10.1111/clr.12462
Monje A, Wang HL, Nart J (2017) Association of preventive maintenance therapy compliance and peri-implant diseases: a cross-sectional study. J Periodontol 88:1030–1041. https://doi.org/10.1902/jop.2017.170135
Salvi GE, Aglietta M, Eick S, Sculean A, Lang NP, Ramseier CA (2012) Reversibility of experimental peri-implant mucositis compared with experimental gingivitis in humans. Clin Oral Implants Res 23:182–190. https://doi.org/10.1111/j.1600-0501.2011.02220
Socransky SS, Haffajee AD, Cugini MA, Smith C, RLJr K (1998) Microbial complexes in subgingival plaque. J Clin Periodontol 25:134–144
Socransky SS, Haffajee AD (2002) Dental biofilms: difficult therapeutic targets. Periodontol 28:12–55
Gürlek Ö, Gümüş P, Nile CJ, Lappin DF, Buduneli NJ (2017) Biomarkers and bacteria around implants and natural teeth in the same individuals. J Periodontol 88:752–761. https://doi.org/10.1902/jop.2017.160751
Kumar PS, Mason MR, Brooker MR, O’Brien K (2012) Pyrosequencing reveals unique microbial signatures associated with healthy and failing dental implants. J Clin Periodontol 39:425–433. https://doi.org/10.1111/j.1600-051X.2012
Leonhardt A, Adolfsson B, Lekholm U, Wikstrom M, Dahlen G (1993) A longitudinal microbiological study on osseointegrated titanium implants in partially edentulous patients. Clin Oral Implants Res 4:113–120
Quirynen M, Alsaadi G, Pauwels M, Haffajee A, van Steenberghe D, Naert I (2005a) Microbiological and clinical outcomes and patient satisfaction for two treatment options in the edentulous lower jaw after 10 years of function. Clin Oral Implants Res 16:277–287. https://doi.org/10.1111/j.1600-0501.2005.01127.x
Quirynen M, Vogels R, Peeters, van Steenberghe D, Naert I, Haffajee A (2006) Dynamics of initial subgingival colonization of ‘pristine’ peri-implant pockets. Clin Oral Implants Res 17:25–37. https://doi.org/10.1111/j.1600-0501.2005.01194.x
Quirynen M, Vogels R, Pauwels M, Haffajee AD, Socransky SS, Uzel NG, van Steenberghe D (2005b) Initial subgingival colonization of ‘pristine’ pockets. J Dent Res 84:340–344
Renvert S, Roos-Jansaker AM, Lindahl C, Renvert H, Rutger Persson G (2007) Infection at titanium implants with or without a clinical diagnosis of inflammation. Clin Oral Implants Res 18:509–516. https://doi.org/10.1111/j.1600-0501.2007.01378.x
Cosyn J, Van Aelst L, Collaert B, Persson GR, de Bruyn H (2011) The peri-implant sulcus compared with internal implant and suprastructure components: a microbiological analysis. Clin Implant Dent Relat Res 13:286–295. https://doi.org/10.1111/j.1708-8208.2009.00220.x
Charalampakis G, Leonhardt A, Rabe P, Dahlen G (2012) Clinical and microbiological characteristics of peri-implantitis cases: a retrospective multicentre study. Clin Oral Implants Res 23:1045–1054. https://doi.org/10.1111/j.1600-0501.2011.02258.x
De Bruyn H, Bouvry P, Collaert B, De Clercq C, Persson GR, Cosyn J (2013) Long-term clinical, microbiological, and radiographic outcomes of Branemark implants installed in augmented maxillary bone for fixed full-arch rehabilitation. Clin Implant Dent Relat Res 15:73–82. https://doi.org/10.1111/j.1708-8208.2011.00359.x
Quirynen M, Van Assche N (2011) Microbial changes after full-mouth tooth extraction, followed by 2-stage implant placement. J Clin Periodontol 38:581–589. https://doi.org/10.1111/j.1600-051X.2011.01728.x
Koyanagi T, Sakamoto M, Takeuchi Y, Maruyama N, Ohkuma M, Izumi Y (2013) Comprehensive microbiological findings in peri-implantitis and periodontitis. J Clin Periodontol 40:218–226. https://doi.org/10.1111/jcpe.12047
Rakic M, Galindo-Moreno P, Monje A, Radovanovic S, Wang HL, Cochran D, Sculean A, Canullo L (2018) How frequent does peri-implantitis occur? A systematic review and meta-analysis. Clin Oral Investig 22:1805–1816. https://doi.org/10.1007/s00784-017-2276-y
De Waal YC, Winkel EG, Meijer HJ, Raghoebar GM, van Winkelhoff AJ (2014) Differences in peri-implant microflora between fully and partially edentulous patients: a systematic review. J Periodontol 85:68–82. https://doi.org/10.1902/jop.2013.130088
Renvert S, Quirynen M (2015) Risk indicators for peri-implantitis. A narrative review. Clin Oral Implants Res 26s:15–44. https://doi.org/10.1111/clr.12636.
Zhuang LF, Watt RM, Mattheos N, Si MS, Lai HC, Lang NP (2016) Periodontal and peri-implant microbiota in patients with healthy and inflamed periodontal and peri-implant tissues. Clin Oral Implants Res 27:13–21. https://doi.org/10.1111/clr.12508
Eick S, Ramseiser CA, Rothemberger K, Bragger U, buser D, Salvi GE (2016) Microbiota at teeth and implants in partially edentulous patientes. A 10-year retrospective study. Clin Oral Implants Res 27:218–225
Ferreira SD, Silva GL, Cortelli JR, Costa JE, Costa FO (2006) Prevalence and risk variables for peri-implant disease in Brazilian subjects. J Clin Periodontol 33:929–935. https://doi.org/10.1111/j.1600-051X.2006.01001.x
Cortelli JR, Cortelli SC, Jordan S, Haraszthy VI, Zambon JJ (2005) Prevalence of periodontal pathogens in Brazilians with aggressive or chronic periodontitis. J Clin Periodontol 32:860–866. https://doi.org/10.1111/j.1600-051X.2005.00777.x
Cortelli SC, Cortelli JR, Romeiro RL et al (2013) Frequency of periodontal pathogens in equivalent peri-implant and periodontal clinical statuses. Arch Oral Biol 58:67–74. https://doi.org/10.1016/j.archoralbio.2012.09.004
Canullo L, Penarrocha-Oltra D, Covani U, Botticelli D, Serino G, Penarrocha M (2016) Clinical and microbiological findings in patients with peri-implantitis: a cross-sectional study. Clin Oral Implants Res 27:376–382. https://doi.org/10.1111/clr.12557
Heitz-Mayfield LJ (2008) Peri-implant diseases: diagnosis and risk indicators. J Clin Periodontol 35:292–304. https://doi.org/10.1111/j.1600-051X.2008.01275.x.
Schou S (2008) Implant treatment in periodontitis-susceptible patients: a systematic review. J Oral Rehabil 35s:9–22. https://doi.org/10.1111/j.1365-2842.2007.01830.x.
Hultin M, Gustafsson A, Hallstrom H, Johansson LA, Ekfeldt A, Klinge B (2002) Microbiological findings and host response in patients with peri-implantitis. Clin Oral Implants Res 13:349–358
Jepsen S, Berglundh T, Genco R et al (2015) Primary prevention of peri-implantitis: managing peri-implant mucositis. J Clin Periodontol 42:S152–S157. https://doi.org/10.1111/jcpe.12369
Atieh MA, Alsabeeha NH, Faggion CM Jr, Duncan WJ (2013) The frequency of peri-implant diseases: a systematic review and meta-analysis. J Periodontol 84:1586–1598. https://doi.org/10.1902/jop.2012.120592.
Mombelli A (2002) Microbiology and antimicrobial therapy of peri-implantitis. Periodontol 28:177–189
Maximo MB, de Mendonca AC, Renata Santos V, Figueiredo LC, Feres M, Duarte PM (2009) Short-term clinical and microbiological evaluations of peri-implant diseases before and after mechanical anti-infective therapies. Clin Oral Implants Res 20:99–108. https://doi.org/10.1111/j.1600-0501.2008.01618.x
Kocar M, Seme K, Hren NI (2010) Characterization of the normal bacterial flora in peri-implant sulci of partially and completely edentulous patients. Int J Oral Maxillofac Implants 25:690–698
Aruni AW, Dou Y, Mishra A, Fletcher HM (2015) The biofilm community-rebels with a cause. Curr Oral Health Rep 2:48–56. https://doi.org/10.1007/s40496-014-0044-5
Thurnheer T, Bostanci N, Belibasakis GN (2016) Microbial dynamics during conversion from supragingival to subgingival biofilms in an in vitro model. Mol Oral Microbiol 31:125–135. https://doi.org/10.1111/omi.12108
Ximenez-Fyvie LA, Haffajee AD, Socransky SS (2000) Comparison of the microbiota of supra- and subgingival plaque in health and periodontitis. J Clin Periodontol 27:648–657
Loozen G, Ozcelik O, Boon N, De Mol A, Schoen C, Quirynen M, Teughels W (2014) Inter-bacterial correlations in subgingival biofilms: a large-scale survey. J Clin Periodontol 41:1–10. https://doi.org/10.1111/jcpe.12167.
Furst MM, Salvi GE, Lang NP, Persson GR (2014) Bacterial colonization immediately after installation on oral titanium implants. Clin Oral Implants Res 18:501–508. https://doi.org/10.1111/j.1600-0501.2007.01381.x.
Salvi GE, Furst MM, Lang NP, Persson GR (2008) One-year bacterial colonization patterns of Staphylococcus aureus and other bacteria at implants and adjacent teeth. Clin Oral Implants Res 19:242–248. https://doi.org/10.1111/j.1600-0501.2007.01470.x
Sanz-Martin I, Doolittle-Hall J, Teles RP, Patel M, Belibasakis GN, Hämmerle CHF, Jung RE, Teles FRF (2017) Exploring the microbiome of healthy and diseased peri-implant sites using Illumina sequencing. J Clin Periodontol 4:1274–1284. https://doi.org/10.1111/jcpe.12788.
Stokman MA, van Winkelhoff AJ, Vissink A, Spijkervet FK, Raghoebar GM (2017) Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study. Clin Oral Investig 21:717–724. https://doi.org/10.1007/s00784-016-1941-x
Acknowledgments
The authors thank Dr. Geraldo Lúcio Magalhães Silva, Dr. Satoschi Takenaka-Martinez, Dr. Eugenio José Pereira Lages, Mrs. Elizabeth Dohler, Mrs. Milene Aparecida Mendes da Rocha, and Ms. Wilciane Machado da Silva (private dental clinic, Belo Horizonte, Brazil) for their assistance with the re-calls, data collection, periodontal maintenance therapy visits, and monitoring of participants.
Funding
This study was supported by grants from Conselho Nacional de Desenvolvimento Científico e Tecnológico – CNPq Brazil (CNPq no. 402158/2016-4).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in the present study were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Costa, F.O., Ferreira, S.D., Cortelli, J.R. et al. Microbiological profile associated with peri-implant diseases in individuals with and without preventive maintenance therapy: a 5-year follow-up. Clin Oral Invest 23, 3161–3171 (2019). https://doi.org/10.1007/s00784-018-2737-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2737-y