Abstract
Objectives
The purpose of the present study was to investigate the volume, surface, morphometric index (MI), and position of the condyle in a normal population by applying Mimics 17.0 software. Then, the difference between left and right sides, sex, and age can be explored, which will contribute to establish the reference value of condylar morphology and position in normal individuals, and help us to study characteristics of condylar morphology and position in abnormal individuals.
Materials and methods
Three-hundred subjects were enrolled in our study from the radiology department of Shanghai Jiao Tong University Affiliated Sixth People’s Hospital. They were divided into three groups according to the age: group 1 (18–24 years old), group 2 (25–34 years old), and group 3 (35–44 years old). Each group included 100 subjects (with 50 males and 50 females). They were examined using multislice computed tomography (MSCT) after that. All images of condyle were reconstructed by Mimics 17.0 software, so as to measure the volume, surface, and MI of condyle, and to analyze the position of condyle in the articular fossa by means of joint spaces.
Results
The differences of condylar volume, surface, and MI between left and right sides were not obvious (P > 0.05). The condylar volume and surface were greater in males than females (P < 0.05), while their condylar MI existed no difference (P > 0.05). No statistical differences were found in volume and surface among three age groups. However, the MI of group 1 was statistically lower than that of group 3 (P < 0.05). On the other hand, no significant differences were found between left and right condylar position (P > 0.05). Nevertheless, there were significant differences of condylar position regarding the gender and age (P < 0.05).
Conclusions
This study showed no significant differences in condylar morphology and position between left and right sides, but factors of gender and age were proven to have a certain influence on the morphology and position of the condyle. This information can be clinically useful in establishing the diagnostic criteria for condylar morphology and position in the normal Asian population.
Clinical relevance
Examination of condylar morphology and position is important for evaluating the abnormalities and bony changes that affect the temporomandibular joint (TMJ). So, this will be conducive to the diagnosis and the evaluation of therapeutic effect of temporomandibular joint diseases. Also, it is important to evaluate these indexes prior to commencing orthodontic treatment, because TMJ abnormalities play a critical role in orthodontic treatment planning.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The condyle is an important part of the temporomandibular joint (TMJ), which is the primary growth center of the mandible. It has the particular ability of multi-directional growth and adaptive remodeling. So, it can respond to the continuous stimuli adaptively through the bone remodeling process, thus affecting the final (or adult) dimension of the mandible. Therefore, condylar volume can be connected with the mandibular final dimension and the relationship between maxillary and mandibular bases as well. During the developmental period, the condyle manifests adaptability to functional stimulation, which plays an important role in the stability of long-term orthodontic and orthognathic treatment [1]. While during adulthood, the condyle is often suffered from remodeling process due to its adaptability, that is, flattening, sclerosis, erosion, osteophytes, and absorption, which could influence its volume and shape [2].
On the other side, the position of the condyle in the temporomandibular joint and its clinical significance have always been a matter of controversy. Many different researches have attempted to explore the position of condyle in the glenoid fossa and whether it is related to temporomandibular joint disorder (TMD), malocclusion, and other maxillofacial diseases or not. The means of evaluating condylar position was first proposed by Ricketts; that is, joint spaces between the mandibular condyle and the articular fossa were measured through radiological methods, and the condyle-fossa relationship was further assessed on the basis of this data [3].
As a digitized three-dimensional interactive medical image controlling system, Mimics software was first developed by Materialise Company in Belgium. It has the function of generating three-dimensional images, as well as editing and processing of medical images, with highly integrated and easily accessible features [4]. The accurate TMJ three-dimensional digital model can be reconstructed on the personal computer by Mimics, based on the imported two-dimensional computed tomography (CT) images of TMJ. Afterwards, the volume and surface of the condyle will be calculated automatically. Also, it allows us to measure the joint space quantitatively with the function of measuring various linear distances and angles.
While the volume, surface, and position of the condyle have been examined previously, the information on Asian populations is still rare, particularly on the factor of age. In the present study, 300 adults were included for the purpose of assessing the volume, surface, morphometric index (MI), and position of bilateral condyles by using multislice computed tomography (MSCT) and Mimics 17.0 software. The aim of this study was therefore to determine the effects of left and right sides, gender, and age on the condylar morphology and position, and to establish the reference value of these parameters in normal individuals in addition, as well as to study characteristics of condylar morphology and position in abnormal individuals.
Materials and methods
Subjects
Three-hundred Chinese patients of maxillary sinusitis who referred to the Department of Radiology in Shanghai Jiao Tong University Affiliated Sixth People’s Hospital for paranasal sinus CT scan were recruited for this study from June 2015 to July 2016, with 150 males and 150 females. The inclusion criteria are as follows: the subjects were aged between 18 and 44 years old, with approximately symmetrical maxillofacial structures, and with intact permanent dentition (except for the third molar). The individuals who had any evidence of TMD both in clinical and radiological examination, malocclusion, the history of surgery and trauma in TMJ, and prior orthodontic or orthognathic treatment were excluded from the present study. Moreover, the presence of any congenital abnormalities or any systemic diseases which could affect joint morphology such as rheumatoidarthritis and maxillary sinusitis caused by odontogenic infection were all excluded. Next, the subjects were divided into three groups according to the age: group 1 (18–24 years old), group 2 (25–34 years old), and group 3 (35–44 years old). Each group included 100 persons (50 males and 50 females).
Acquisition of CT images
The CT images were obtained (Siemens Definition AS +128 MSCT) with the following technical parameters: 120 kV, 100 mA, 0.5 s/rot, and 512 × 512 matrix. The subjects were supine and biting their teeth into maximum intercuspal position. Their heads were positioned with the Frankfort horizontal plane and the midsagittal plane of the head perpendicular to the floor. The fixation device was used to keep the head stationary during the scanning process. The CT images covered the whole maxilla and mandible. All the subjects were scanned by the same radiologist using the same machine. The acquired CT images were saved in the form of two-dimensional digital imaging and medical communication documents (DICOM).
Condylar 3D reconstruction
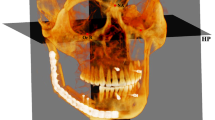
The 3D reconstruction of the condyle was conducted by reference to Schlueter et al. [5] and Tecco et al. [6],and our improved procedures are as follows: importing the saved DICOM images into Mimics 17.0 software(Materialize NV Technologielaan, Leuven, Belgium) and orientating the images at the same time. The images were visualized in the recommended range of bone density (range of gray scale from − 1024 to 1650). Each condyle was segmented using an adaptive threshold (226–3071), which was visually checked prior to reconstructing 3D condylar models. Then, the remaining surrounding structures of the condyle were progressively removed through the segmentation function of Mimics (Fig. 1).
The segmentation process was made on the axial views, and the superior and inferior bound of the condyle were standardized: On the axial view, the superior bound of the condyle was determined where the first radiopaque point was viewed in the image representing the synovial (Fig. 2a). The inferior bound was selected when the sigmoid area disappears, while scrolling the image from the upper to the lower region of the joint space (Fig. 2b).
ᅟThe segmentation process was made on the axial views, and the superior and inferior bound of the condyle were standardized. On the axial view, the superior bound of the condyle was determined where the first radiopaque point was viewed in the image representing the synovial (a). The inferior bound was selected when the sigmoid area disappears, while scrolling the image from the upper to the lower region of the joint space (b)
Analysis of condylar position
The axial view, on which the condylar process had the widest mediolateral diameter, was selected as the reference view for a secondary reconstruction. On this chosen reference view, a parallel line of the long axis of the condylar process was drawn, and lateral slices were reconstructed with 0.5-mm thickness using the “reslice” function. Joint spaces were measured on the central sagittal section after that.
The measurement method for condylar position used in the present study was described by Cohlmia JT et al. [7]. The landmarks used for analysis are illustrated in Fig. 3 and were established in the following manner: (1) line F which was parallel to the Frankfort horizontal plane was regarded as the baseline and line F′ was drawn tangent to the most superior point of the glenoid fossa (point a). (2) Lines were then drawn from point “a” tangent to the anterior and posterior aspects of the condylar process at the anterior condyle point (point b) and posterior condyle point (point c), respectively. (3) Perpendiculars to these tangents from points a and b intersected the articular fossa at point d anteriorly and point e posteriorly, respectively. (4) Anterior joint space (A) was the distance between point b and d, and posterior joint space (P) was the distance between point c and e.
Indexes for assessment
The reconstruction and measurement of the condyle were conducted by the same professional observer to avoid the measuring error from different persons. All images were revaluated over 3-week interval, and the averages were taken as the final values.
-
(1)
Condylar volume (V) and surface (S): This can be calculated automatically by Mimics.
-
(2)
Morphometric index (MI): MI = V/S.
-
(3)
Condylar position was expressed as \( \frac{\mathrm{P}\hbox{--} \mathrm{A}}{\mathrm{P}+\mathrm{A}}\times 100\% \). The position of the condyle was considered concentric if the ratio was within ± 12. The condylar position was considered anterior if the ratio was greater than + 12. While the ratio which was smaller than − 12 represented a posterior position.
Reproducibility of measurements
To assess the significance of any errors during measurement, 30 samples were re-evaluated with a 3-week interval by two observers. Intra-class correlation coefficients (ICCs) were used to determine the intra-observer and interobserver reliabilities, and the results were both greater than 0.9. Therefore, reproducibility of the evaluation method was found statistically acceptable.
Statistical analysis
The measurements were processed and analyzed using SPSS 21.0. The data presented as mean ± standard deviation were all normally distributed. The paired sample t test was used to calculate the statistically significant differences of volume, surface size, and MI between left and right sides, and the t test for independent samples was employed to calculate the statistically significant differences between the males and the females. An analysis of variance (ANOVA) was performed to do the analyses based on ages. Bonferroni method was used for comparison of two of the three age groups. As for the condylar position, McNemar test and Pearson chi-squared test were used to compare the condylar positions between TMJ sides and genders, respectively. Nevertheless, the comparison of different age groups was performed using the Pearson chi-squared test or the Kruskal-Wallis test depending on different purposes of the research. The level for significance was set at P < 0.05.
Results
Comparisons between left and right sides
No significant differences were found in condylar volume, surface, MI, and position between right and left sides (P > 0.05) (Tables 1 and 3).
Comparisons between males and females
For the condylar volume and surface, the differences according to genders were statistically significant (P < 0.05). Males showed a higher condylar volume and surface when compared with females. Although the MI of males was higher than that of the females, the difference was not significant (P > 0.05) (Table 1). There was also a significant gender difference in condylar position (P < 0.05). Females (62.1%) accounted for a greater proportion in posterior condylar position than males (37.9%), and the difference of gender distribution in posterior position was the most obvious among three kinds of condylar positions (Table 4).
Comparisons among different age groups
-
(1)
Differences of condylar morphology
There were no significant differences in volume and surface in accordance with ages (P > 0.05). Whereas significant differences were found in MI among three age groups (P < 0.05), and Bonferroni test was further used to assess the intergroup significances. It turns out that the difference between groups 1 and 3 was statistically significant (P < 0.05) (Tables 1 and 2).
-
(2)
Differences of the condylar position among different age groups
When differences of condylar position among three age groups were studied, the age can be regarded as a disorderly classified variable. And Pearson chi-squared test was used for statistical analysis. The results are summarized in Table 4. The distributions of condylar position in different age groups were significantly different (P < 0.05); thus, condylar positions may be affected by the factor of age.
-
(3)
The change of condylar position with age
The age was taken as an ordered variable to study whether there was some kind of changing tendency in condylar position with the growth of age. Kruskal-Wallis test was applied for this research purpose. However, no changing tendency was found in condylar position with age (P > 0.05) (Table 4).
Discussion
As one of the most important joints in the body, bilateral temporomandibular joints need to work together. The TMJ takes part in the composition of maxillofacial functional system together with the teeth, maxillofacial bones, masticatory muscles, nerves, and blood vessels. The assessment of anatomical structures of TMJ radiologically is an important way to study the morphology and function of TMJ, which will be conducive to the diagnosis, treatment, and evaluation of TMJ diseases. Various radiographic methods have been used in previous studies to analyze bony structures of TMJ quantitatively, such as conventional radiography [8], computed tomography (CT) [9], magnetic resonance imaging (MRI) [10], and cone beam computed tomography (CBCT) [11].
Conventional radiography is limited by projection angle and overlapped surrounding structures. And MRI is mainly used for soft tissues, which is regarded as the gold standard for diagnosis of temporomandibular joint disk displacement [12]. Whereas MSCT and CBCT are superior to MRI in observing hard tissues, they represent TMJ structures with high accuracy which produces submillimeter spatial resolution, and are increasingly used in clinical research. Zain-Alabdeen et al. [13] examined the differences between MSCT and CBCT in detecting bone changes of condylar surface, and they concluded that no significant differences existed in the accuracy. Moreover, relatively speaking, MSCT displays more soft tissues than CBCT [14]. Although articular disk displacement and perforation can be diagnosed by CBCT using arthrography, arthrocentesis is certainly traumatic and the direct images of the articular disk and other soft tissues cannot be shown clearly [15]. In addition, Hintze et al. [16] argued that no significant differences in diagnostic accuracy for the detection of bone changes in the condyle and articular tubercle were found between CBCT images and CT images, with the exception of bone defects in the articular tubercle examined on frontal views alone where the specificity with CT was significantly higher than that with CBCT. Consequently, in spite of the lower radiation dose, shorter scanning time, and lower cost of CBCT compared with CT [17], MSCT was selected for the present study in consideration of the sample source and previous studies simultaneously, so that the requirements of medical ethics and the reliability of research could be met at the same time.
The validation of condylar 3D reconstruction was mainly affected by the segmentation process and the observer. During the segmentation process, it was critical to identify the inferior bound of the condyle. The sigmoid notch, which is easy to be recognized and not affected by growth or surgical interventions, was taken as the landmark for the inferior bound of the condyle. So, the reconstructed condylar models would theoretically be highly reproducible. As for the measurement differences, the reconstruction and measurement of the condyle were conducted by the same professional observer to avoid the measuring error from different persons. Thirty samples were re-evaluated and intra-class correlation coefficients were calculated to assess the within observer difference. The results were all greater than 0.9. So, the reproducibility of the evaluation method was found statistically acceptable.
Differences in condylar morphology
The subjects enrolled in this study were approximately symmetrical in maxillofacial structures, with no symptoms of TMD. And no significant differences were found in condylar volume, surface, and MI between right and left sides, suggesting that the morphology of bilateral condyles was basically symmetrical, which was similar to previous studies [18]. But this finding contradicts that of Tecco et al. [6]. They found that the condylar volume in the right TMJ was significantly higher than in the left, as was the condylar surface. This contradiction perhaps results from the different inclusion criteria, since individuals with malocclusion were also included in their research. So, bilateral condylar morphology is generally symmetrical in the normal population.
In the light of our study, the condylar volume (1976.135 ± 356.940 mm3) and surface (963.084 ± 117.374 mm2) of males are significantly higher than those of females (1867.607 ± 389.225 mm3, 911.552 ± 155.171 mm2). The difference of condylar morphology in genders should be consistent with the difference of their skeletal characteristics, which was confirmed by Song et al. [19], who examined the female-to-male proportions of the head and face in Koreans; that is, both the frontal and lateral facial dimensions of males were larger than females.
It is reported that the most remarkable morphologic alterations and positioning asymmetries of TMJ structures are related to varieties of factors, such as the absence of teeth, dental abrasion, premature occlusal contact points, unilateral posterior crossbites, and functional mandibular deviations. The articular cartilage has been proven to respond to the degenerative changes and nonphysiological strain in the joint areas, by means of changing the thicknesses of single-cartilage layers and total layer thickness. And this will lead to a change in vertical dimensions and width [20]. What is more, the shape and linear dimensions of the mandibular condyle have been demonstrated to have high variability [21]. Instead of the volume and surface, MI could be a preferable indicator, because no significant differences are found according to TMJ sides and genders in the present study. This will serve to the judgment of the presence or absence of an abnormal condylar shape in clinic.
With regard to the condylar morphology among different age groups, no significant differences were found in condylar volume and surface. And there were no previous studies investigating the effect of age on condylar volume and surface. It is noteworthy that the maximum age of this study is 44 years old, so the condylar morphology in older individuals is likely to vary from younger individuals for the tendency of suffering from degenerative changes in the former. Thus, the reference value of condylar volume and surface could be established in a certain age range, which will surely help us to study characteristics of condylar morphology and position in abnormal individuals. Besides, group 1 (18–24 years old) and group 3 (35–44 years old) vary obviously in MI value, which was never reported before. Consequently, future studies with larger sample size and more age groups are required to confirm this.
The position of the condyle in the temporomandibular joint and its clinical significance have always been controversial. Some studies have suggested a relation between condylar position and TMD [22, 23]. While others failed to demonstrate the correlation between them [24]. Also, there have been many studies reporting nonconcentric condylar position in association with disk displacement [25], remodeling of the articular eminence and condyle [26], and osteoarthritic changes [27]. And this nonconcentric condylar position accounts for one third to one half of asymptomatic volunteers [28].
Differences in condylar position
The position of condyle in the articular fossa was investigated in 300 subjects, and differences based on TMJ sides, genders, and ages were compared. Similar to the condylar morphology, there is no difference in condylar position between left and right side (Table 3).
Unlikely, the distributions of condylar position in males and females are different. Females (62.1%) accounted for a greater proportion in posterior condylar position than males (37.9%), and the difference of gender distribution in posterior position was the most obvious among three kinds of condylar positions. Comparing mandibular condylar position patients with TMD and in healthy subjects, Paknahad et al. [29] stated that posterior condylar position was more frequently observed in females and anterior condylar position was more prevalent in males in the symptomatic group. Other authors have also reported an association between posterior condylar position and internal derangement [10, 25]. Accordingly, it can be speculated that preponderance of TMD and disk instability in women may result from the higher incidence of posterior condylar position in women.
When it comes to the comparison of condylar position according to ages, the age was first regarded as a disorderly classified variable to study differences of condylar position among three age groups. Pearson chi-squared test was used for statistical analysis. The results in Table 4 show that the distributions of condylar position in different age groups are significantly different (P < 0.05); thus, condylar positions may be affected by the age. Among them, posterior condyle in group 3 (35–44 years old) increases visibly. And according to an epidemiological analysis on patients with TMD, the majority of them are in the age group ranging from 26 to 40, with an average age of 35.6 [30]. Considering the association between posterior condylar position and internal derangement mentioned above, it may be assumed that the high incidence of posterior condylar in the age group ranging from 35 to 44 can be related to the susceptible age of TMD. However, when the age was taken as an ordered variable to study whether there was some kind of changing tendency in condylar position with the growth of age using Kruskal-Wallis test, no changing tendency was found in condylar position with age (P > 0.05). This may be related to the range of each age group, so it is necessary to narrow the age range for in the future study. Generally speaking, the relationship between condylar position and age should be further examined for the lack of related reports previously.
Conclusions
This study shows no differences of condylar volume and surface between left and right sides in normal population, but condylar volume and surface of males are significantly larger than females. For the studied age range (18–44), there is no difference concerning condylar morphology. But the MI in the age group of 35–44 is greater than that in the age group of 18–24. On the other hand, the condylar position manifests significant differences in genders and ages, but no significant differences in TMJ sides. In conclusion, there are no significant differences in condylar morphology and position between left and right sides, whereas factors of gender and age have been proven to have a certain influence on the morphology and position of the condyle. This information can be clinically useful in establishing the diagnostic criteria for condylar morphology and position in the normal Asian population.
References
Zane Krisjane IU, Krumina G, Bieza A, Zepa K, Rogovska I (2007) Condylar and mandibular morphological criteria in the 2D and 3D MSCT imaging for patients with class II division 1 subdivision malocclusion. Stomatologija 9(3):67–71
Alexiou KE, Stamatakis HC, Tsiklakis K (2009) Evaluation of the severity of temporomandibular joint osteoarthritic changes related to age using cone beam computed tomography. Dentomaxillofac Radiol 38(3):141–147. https://doi.org/10.1259/dmfr/59263880
Ricketts RM Variations of the temporomandibular joint as revealed by cephalometric laminagraphy. Am J Den 36:877–898
Kaya FN, Yavascaoglu B, Turker G, Yildirim A, Gurbet A, Mogol EB, Ozcan B (2010) Intravenous dexmedetomidine, but not midazolam, prolongs bupivacaine spinal anesthesia. Can J Anaesth 57(1):39–45. https://doi.org/10.1007/s12630-009-9231-6
Schlueter B, Kim KB, Oliver D, Sortiropoulos G (2008) Cone beam computed tomography 3D reconstruction of the mandibular condyle. Angle Orthod 78(5):880–888. https://doi.org/10.2319/072007-339.1
Tecco S, Saccucci M, Nucera R, Polimeni A, Pagnoni M, Cordasco G et al (2010) Condylar volume and surface in Caucasian young adult subjects. BMC Med Imaging 10:1471–2342
Cohlmia JTGJ, Sinha PK, Nanda RS, Currier GF (1996) Tomographic assessment of temporomandibular joints in patients with malocclusion. Angle Orthod 66(1):27–35. https://doi.org/10.1043/0003-3219(1996)066<0027:TAOTJI>2.3.CO;2
Menezes AV, de Almeida SM, Boscolo FN, Haiter-Neto F, Ambrosano GM, Manzi FR (2008) Comparison of transcranial radiograph and magnetic resonance imaging in the evaluation of mandibular condyle position. Dentomaxillofac Radiol 37(5):293–299. https://doi.org/10.1259/dmfr/31850388
Wu CK, Hsu JT, Shen YW, Chen JH, Shen WC, Fuh LJ (2012) Assessments of inclinations of the mandibular fossa by computed tomography in an Asian population. Clin Oral Investig 16(2):443–450. https://doi.org/10.1007/s00784-011-0518-y
Incesu L, Taşkaya-Yılmaz N, Öğütcen-Toller M, Uzun E (2004) Relationship of condylar position to disc position and morphology. Eur J Radiol 51(3):269–273. https://doi.org/10.1016/S0720-048X(03)00218-3
Shahidi S, Vojdani M, Paknahad M (2013) Correlation between articular eminence steepness measured with cone-beam computed tomography and clinical dysfunction index in patients with temporomandibular joint dysfunction. Oral Surg Oral Med Oral Pathol Oral Radiol 116(1):91–97. https://doi.org/10.1016/j.oooo.2013.04.001
Tasaki MMWP (1993) Temporomandibular joint: diagnostic accuracy with sagittal and coronal MR imaging. Radiology 186(3):723–729. https://doi.org/10.1148/radiology.186.3.8430181
Zain-Alabdeen EH, Alsadhan RI (2012) A comparative study of accuracy of detection of surface osseous changes in the temporomandibular joint using multidetector CT and cone beam CT. Dentomaxillofac Radiol. 41(3):185–191. https://doi.org/10.1259/dmfr/24985971
Barghan S, Merrill R, Tetradis S (2010) Cone beam computed tomography imaging in the evaluation of the temporomandibular joint. J Calif Dent Assoc 38:33–39
Tsiklakis K, Syriopoulos K, Stamatakis HC (2004) Radiographic examination of the temporomandibular joint using cone beam computed tomography. Dentomaxillofac Radiol 33(3):196–201. https://doi.org/10.1259/dmfr/27403192
Hintze H, Wiese M, Wenzel A (2007) Cone beam CT and conventional tomography for the detection of morphological temporomandibular joint changes. Dentomaxillofac Radiol 36(4):192–197. https://doi.org/10.1259/dmfr/25523853
Honey OB, Scarfe WC, Hilgers MJ, Klueber K, Silveira AM, Haskell BS, Farman AG (2007) Accuracy of cone-beam computed tomography imaging of the temporomandibular joint: comparisons with panoramic radiology and linear tomography. Am J Orthod Dentofac Orthop 132(4):429–438. https://doi.org/10.1016/j.ajodo.2005.10.032
Rodrigues AF, Fraga MR, Vitral RW (2009) Computed tomography evaluation of the temporomandibular joint in class I malocclusion patients: condylar symmetry and condyle-fossa relationship. Am J Orthod Dentofac Orthop 136(2):192–198. https://doi.org/10.1016/j.ajodo.2007.07.032
Song WC, Kim JI, Kim SH, Shin DH, Hu KS, Kim HJ, Lee JY, Koh KS (2009) Female-to-male proportions of the head and face in Koreans. J Craniofac Surg 20(2):356–361. https://doi.org/10.1097/SCS.0b013e3181843620
Fanghanel J, Gedrange T (2007) On the development, morphology and function of the temporomandibular joint in the light of the orofacial system. Ann Anat 189(4):314–319. https://doi.org/10.1016/j.aanat.2007.02.024
Solberg WK, Hansson TL, Nordstrom B (1985) The temporomandibular joint in young adults at autopsy: a morphologic classification and evaluation. J Oral Rehab 12(4):303–321. https://doi.org/10.1111/j.1365-2842.1985.tb01285.x
Weinberg LA (1979) An evaluation of occlusal factors in TMJ dysfunction-pain syndrome. J Prosthet Dent 41(2):198–208. https://doi.org/10.1016/0022-3913(79)90308-1
Blaschke DD, Solberg WK, Sanders B (1980) Arthorgraphy of the temporomandibular joint: review and current status. J Am Dent Assoc 100(3):388–395. https://doi.org/10.14219/jada.archive.1980.0094
Herbosa EG, Rotskoff KS, Ramos BF, Ambrookian HS (1990) Condylar position in superior maxillary repositioning and its effect on the temporomandibular joint. J Oral Maxillofac Surg 48(7):690–696. https://doi.org/10.1016/0278-2391(90)90051-3
Ikeda K, Kawamura A (2013) Disc displacement and changes in condylar position. Dentomaxillofac Radiol 42(3):84227642. https://doi.org/10.1259/dmfr/84227642
Scapino RP (1983) Histopathology associated with malposition of the human temporomandibular joint disc. Oral Surg Oral Med Oral Pathol 55(4):382–397. https://doi.org/10.1016/0030-4220(83)90193-7
Cho BH, Jung YH (2012) Osteoarthritic changes and condylar positioning of the temporomandibular joint in Korean children and adolescents. Imaging Sci Dent 42(3):169–174. https://doi.org/10.5624/isd.2012.42.3.169
White SC, Pharoah MJ. Oral Radiology: Principles and interpretation. Elsevier Health Science 2009; 6th edition
Paknahad M, Shahidi S, Iranpour S, Mirhadi S, Paknahad M. Cone-beam computed tomographic assessment of mandibular condylar position in patients with temporomandibular joint dysfunction and in healthy subjects. Int J Dent 2015; 2015:301796, 1, 6, DOI: https://doi.org/10.1155/2015/301796
Di Paolo CCG, Panti F, Rampello A, Falisi G, Pilloni A, Cascone P, Iannetti G (2013) Epidemiological analysis on 2375 patients with TMJ disorders: basic statistical aspects. Ann Stomatol (Roma) 4(1):161–169. https://doi.org/10.11138/ads.0161
Funding
We acknowledge the funding support from Project of Shanghai Municipal Commission of Health and Family Planning (Grant No. 201540177).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The research was approved by the local Ethical Committee of Shanghai Jiao Jong University Affiliated Sixth People’s Hospital (No. 2015-KY-003(T)).
Informed consent
All the participants took part voluntarily in this study, and the verbal consent from each of them was taken after being informed about the nature of the study detailedly.
Rights and permissions
About this article
Cite this article
Liu, Q., Wei, X., Guan, J. et al. Assessment of condylar morphology and position using MSCT in an Asian population. Clin Oral Invest 22, 2653–2661 (2018). https://doi.org/10.1007/s00784-018-2364-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2364-7